Abstract
Introduction:
Real spinal cord injury without radiologic abnormality (SCIWORA) is a rare clinical entity.
Case presentation:
The patient was a 13-year-old girl whose body was overturned anteriorly after crashing her bicycle into a curb. Following the accident, in which her neck and upper back hit the ground, she could not move due to paralysis. On arrival, she had paresis of the bilateral upper extremities and experienced a painful sensation when her upper extremities were touched. Cervical roentgenography and whole-body computed tomography revealed no traumatic lesions in either the intracranium or the cervical bone. Urgent spinal magnetic resonance imaging (MRI) showed no significant spinal cord lesions or spinal canal stenosis. She was put on complete bed rest with a cervical collar. On the 2nd hospital day (24 h after the accident), her motor weakness had almost completely subsided, and she felt only mild dysesthesia in both forearms. Roentgenography revealed no instability. Her motor weakness completely recovered on the third day after accident and she was diagnosed with spinal cord concussion.
Discussion:
The present case study, in which MRI was performed, showed that an immediate improvement was obtained in a patient who experienced real SCIWORA. The importance of not only spinal cord lesions, but also perispinal soft tissue injury on MRI has been emphasized for predicting patient outcomes. Accordingly, immediate MRI is essential for evaluating patients with signs and symptoms of spinal cord injury, even when plain neck roentgenography and cervical CT are negative.
Similar content being viewed by others
Introduction
Blunt injuries of the spinal cord without overt skeletal or ligamentous disruption account for a significant proportion of spinal cord injuries (SCIs) in children, and most commonly occur in children younger than 8 years of age.1,2 In some cases, SCIs occur without radiographic abnormalities; this condition is referred to as SCIWORA. The term ‘real SCIWORA’ is also used when the findings of all imaging modalities—including MRI—are negative.1,2 The incompletely ossified cervical spine of young children is characterized by horizontally oriented uncovertebral joints and facets, anterior vertebral body wedging, ligamentous laxity and weak nuchal musculature.1,2 Such characteristics produce a hypermobile spinal column that has a much greater propensity for dislocation than does fracture.1,2 Spinal cord concussion is defined as transient paralysis and/or sensory disturbance that subsides within 72 h.3–5 We herein report a case of real SCIWORA in a patient with spinal cord concussion.
Case presentation
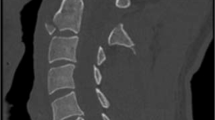
The patient was a 13-year-old girl whose body was overturned anteriorly after crashing her bicycle into a curb. Following the accident, in which her neck and upper back hit the ground, she could not move due to paralysis. She was transported to our department by an ambulance. On arrival, her vital signs were as follows: Glasgow Coma Scale, E4V5M6; blood pressure, 112/72 mm Hg; pulse rate, regular at 78 beats per minute; and respiratory rate, 20 breaths per minute. She had paresis of the bilateral upper extremities and she experienced a painful sensation when her upper extremities were touched. The details of her neurological deficits are shown in Table 1. She had no particular past history. A blood examination demonstrated no specific findings. Cervical roentgenography and whole-body computed tomography revealed no traumatic lesions in either the intracranium or cervical bone (Figure 1a). Urgent spinal magnetic resonance imaging showed no significant spinal cord lesions, spinal canal stenosis or perispinal soft tissue injury (Figure 1b). She was put on complete bed rest with a cervical collar. On the 2nd hospital day (24 h after the accident), her motor weakness had almost completely subsided and she felt only mild dysesthesia in both forearms. Roentgenography revealed no instability (Figure 2). She could stand, walk and use her hands to eat as usual. She was discharged on the 2nd hospital day. She completely recovered from the motor weakness on the 3rd day after the accident, but was diagnosed with spinal cord concussion.
Discussion
Real SCIWORA is associated with a favorable outcome.2 The present case study, in which MRI was performed, showed that an immediate improvement was obtained in a patient who experienced real SCIWORA. Other studies have shown similar findings. Mahajan et al.6 reported on 69 children who were diagnosed with SCIWORA, but who showed normal MRI findings (n=54), and noted that the clinical outcomes were substantially more favorable in comparison with those patients with cervical cord abnormalities as shown on MRI (n=15). However, their report did not show the timing of the patients’ improvement. In contrast, Nesnídal et al.7 reported on the timing in a retrospective study of 24 patients with spinal cord concussions who recovered from their symptoms within 76 h. The MRI scans of 21 (87.5%) of these patients showed no evidence of any traumatic spinal changes. All of the patients experienced a rapid resolution of their neurological deficits. The resolution occurred within 6 h after injury in 2 (8.4%) patients, within 12 h in 2 (8.4%) patients, within 24 h in 12 (50.0%) patients, within 48 h in 6 (25.0%) patients and after more than 48 h in 2 (8.4%) patients.7 However, the correlation between the presence/absence of lesions on MRI and the timing of improvement was not analyzed. Recently, the importance of both spinal cord lesions and perispinal soft tissue injury on MRI has been emphasized for predicting patient outcomes.8,9 These findings may suggest the instability of the vertebral column and may be correlated with the severity of spinal cord injury in comparison with intact perispinal soft tissue, through the temporal movement of the vertebral column, resulting in more severe spinal cord injury. In addition, the data of 1550 patients with negative CT scans following blunt trauma were subsequently evaluated by MRI.10 MRI detected abnormalities in 182 of the patients (12%). Among these patients, the management of 96 patients was changed, based on the MRI findings, in order to prevent secondary damage due to instability of the vertebral column. Accordingly, immediate MRI is essential for evaluating patients with signs and symptoms of spinal cord injury, even when plain neck roentgenography and cervical CT are negative.
The timing of MRI is also important. Performing an MRI examination after symptoms of spinal cord injury disappear is not clinically useful. Mahajan and Nesnídal did not describe when MRI was performed, but Maritnez-Perez performed MRI within 72 h, and Machino performed examinations at an average of 26.0 h after the traumatic incident.6–9 At our institute, MRI can be performed for patients with spinal cord injury at any time, so the present patient underwent MRI immediately after her CT examination. Specifically, she underwent the MRI study within 1 h after the accident. Such studies have never been reported. Because the present case had a normal cervical cord and soft tissue on MRI, rapid resolution of the neurological deficit could be predicted. Accordingly, the present case may not have required admission, stress roentgenography or complete bed rest with a cervical collar. Whether or not patients with normal MRI findings can safely return home without any treatment, even when those with spinal cord injury have symptoms, is a clinical question warranting further exploration.
Finally, this case presented with upper extremity paresis and a loss of sensation, but no lower extremity or bladder and bowel problems.10 This neurological dysfunction was compatible with a mild form of cervical central spinal cord injury as characterized by predominant upper extremity weakness and relatively little severe sensory and bladder dysfunction.11 In adults the occurrence of central spinal cord syndrome (50.2%) was higher than other injury patterns among patients with SCIWORA (not real SCIWORA). In pediatric SCIWORA, most studies have described neurological deficits using the Frankel or American Spinal Injury Association classifications. Hence, we were unable to investigate the frequency of cervical central spinal cord injury patterns among patients with SCIWORA.12,13 In case reports, Jung et al.14 reported a 7-year-old boy who complained of weakness in both arms (but not his lower extremities) after completing a standing high jump. This case showed no evidence of bone abnormalities on computed tomography of the cervical spine, but MRI revealed observable swelling with increased signal intensity at the C1-C4 levels. Ramírez et al.15 also reported a 15-year-old male patient who suffered cervical blunt trauma with a plastic tube. An evaluation showed that the patient had marked upper extremity weakness when compared with the lower extremities, corresponding to central spinal cord syndrome. MRI showed contusive changes in the C4-C7 central spinal cord. As both of these cases showed lesions on MRI, their symptoms did not recover quickly. However, the present case was unique as this was a case of pediatric cervical central spinal cord injury that subsided quickly, as predicted by an MRI study. As the present case had no history of psychiatric illness or neurological deficit compatible with cervical central spinal cord injury, the possibility of hysterical paralysis was low.16
Additional Information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Yucesoy K, Yuksel KZ . SCIWORA in MRI era. ClinNeurlNeurosurg 2008; 110: 429–433.
Dreizin D, Kim W, Kim JS, Boscak AR, Bodanapally UK, Munera F et al. Will the real SCIWORA please stand up? Exploring clinicoradiologic mismatch in closed spinal cord injuries. AJR Am J Roentgenol 2015; 205: 853–860.
Del Bigio MR, Johnson GE . Clinical presentation of spinal cord concussion. Spine 1989; 14: 37–40.
Zwimpfer TJ, Bernstein M . Spinal cord concussion. J Neurosurg 1990; 72: 894–900.
Nagoshi N, Tetreault L, Nakashima H, Nouri A, Fehlings MG . Return to play in athletes with spinal cord concussion: a systematic literature review. Spine J 2017; 17: 291–302.
Mahajan P, Jaffe DM, Olsen CS, Leonard JR, Nigrovic LE, Rogers AJ et al. Spinal cord injury without radiologic abnormality in children imaged with magnetic resonance imaging. J Trauma Acute Care Surg 2013; 75: 843–847.
Nesnídal P, Stulík J, Barna M . Spinal cord concussion: a retrospective study of twenty-four patients. Acta Chir Orthop Traumatol Cech 2012; 79: 150–155.
Martinez-Perez R, Munarriz PM, Paredes I, Cotrina J, Lagares A . Cervical spinal cord injury without computed tomography evidence of trauma in adults: magnetic resonance imaging prognostic factors. World Neurosurg 2017; 99: 192–199.
Machino M, Yukawa Y, Ito K, Nakashima H, Kanbara S, Morita D et al. Can magnetic resonance imaging reflect the prognosis in patients of cervical spinal cord injury without radiographic abnormality? Spine 2011; 36: E1568–E1572.
Schoenfeld AJ, Bono CM, McGuire KJ, Warholic N, Harris MB . Computed tomography alone versus computed tomography and magnetic resonance imaging in the identification of occult injuries to the cervical spine: a meta-analysis. J Trauma 2010; 68: 109–113.
Molliqaj G, Payer M, Schaller K, Tessitore E . Acute traumatic central cord syndrome: a comprehensive review. Neurochirurgie 2014; 60: 5–11.
Boese CK, Oppermann J, Siewe J, Eysel P, Scheyerer MJ, Lechler P . Spinal cord injury without radiologic abnormality in children: a systematic review and meta-analysis. J Trauma Acute Care Surg 2015; 78: 874–882.
Carroll T, Smith CD, Liu X, Bonaventura B, Mann N, Liu J et al. Spinal cord injuries without radiologic abnormality in children: a systematic review. Spinal Cord 2015; 53: 842–848.
Jung SK, Shin HJ, Kang HD, Oh SH . Central cord syndrome in a 7-year-old boy secondary to standing high jump. Pediatr Emerg Care 2014; 30: 640–642.
Ramírez NB, Arias-Berríos RE, López-Acevedo C, Ramos E . Traumatic central cord syndrome after blunt cervical trauma: a pediatric case report. Spinal Cord Ser Cases 2016; 2: 16014.
Baker JH, Silver JR . Hysterical paraplegia. J Neurol Neurosurg Psychiatry 1987; 50: 375–382.
Acknowledgements
This work received funding from a Ministry of Education, Culture, Sports, Science and Technology (MEXT)-Supported Program for the Strategic Research Foundation at Private Universities, 2015–2019. The title is [The constitution of total researching system for comprehensive disaster, medical management, corresponding to wide-scale disaster].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Nagasawa, H., Ishikawa, K., Takahashi, R. et al. A case of real spinal cord injury without radiologic abnormality in a pediatric patient with spinal cord concussion. Spinal Cord Ser Cases 3, 17051 (2017). https://doi.org/10.1038/scsandc.2017.51
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/scsandc.2017.51
This article is cited by
-
Spinal cord injury without radiologic abnormality: an updated systematic review and investigation of concurrent concussion
Bulletin of the National Research Centre (2023)