Abstract
Study design:
Experimental, prospective study.
Objectives:
We evaluated the long-term clinical efficacy of transanal irrigation (TAI) and its effect on the quality of life of spina bifida children and their caregivers.
Setting:
Republic of Korea.
Method:
Forty-four spina bifida pediatric patients with constipation, fecal incontinence or both, underwent a TAI program at our spina bifida clinic between December 2010 and October 2013. The children and their caregivers were evaluated using a self-administered questionnaire before TAI and at 3 months and 3 years after initiation of the program.
Results:
Successful treatment outcome was achieved in 38 (86.4%) children after a mean follow-up duration of 33 months (range, 30–36). The mean number of fecal incontinence episodes per week, the number of diaper changes and the total time for bowel care per day before the program decreased at the latest follow-up examination from 7.3 to 0.4 (P<0.001), 1.6 to 0.2 (P<0.001) and 29.2 to 19.4 min (P=0.038), respectively. These results remained constant from short-term follow-up at 3 months to 3 years. Caregivers and children could go out more often (P=0.002), and the emotional impact of bowel care on caregivers decreased (P<0.001). The reported mean overall satisfaction with TAI was 8/10. The common adverse effect during TAI was abdominal discomfort (60.5%).
Conclusion:
We observed a sustained significant improvement in defecation symptoms and quality of life for 3 years in spina bifida children who underwent continuous TAI.
Similar content being viewed by others
Introduction
Spina bifida (SB) is a congenital impairment of neural tube closure that occurs between 24 and 26 days of gestation1 and affects the lower spinal cord with variable severity of neural symptoms that include neurogenic bladder and bowel dysfunction.2 Appropriate management often achieves urinary continence, but bowel continence is a major concern for patients with SB.3 More than 50% of children and adolescents with SB do not achieve full bowel continence;4 bowel dysfunction is a major obstacle to independence, activity, social integration and good quality of life (QoL).5 For some children with SB, bowel dysfunction is more distressing compared with their impaired motor function.6
Several methods are used to deal with constipation and fecal incontinence in children with SB, including conservative or pharmacological management, transanal irrigation (TAI) and surgical approaches. Different laxatives have been used with varying success; however, when the internal sphincter is not fully functional, fecal incontinence or soiling occurs.1 Therefore, a more aggressive management approach is needed for bowel continence in many cases. The Malone antegrade continence enema procedure is one of the most useful techniques for resolving fecal incontinence in SB children, but the downside of this procedure is the necessity for surgery.6 Therefore, conservative treatment should be first administered, and the efficacy of TAI may predict the efficacy of Malone antegrade continence enema on bowel management.7
TAI is a procedure that has been used for many years and has only recently been introduced for managing neurogenic bowel dysfunction.8 From the late 1990s, this method has been used in SB children and several researchers have reported its effectiveness and safety for neurogenic bowel management.6, 9, 10, 11, 12, 13, 14, 15, 16 These studies show that TAI reduces constipation and achieves fecal continence in children with SB, resulting in an improvement in independence and QoL. Up until the late 1990s, Malone antegrade continence enema was considered the last of all golden standards for bowel management in children with SB. Currently, however, TAI is suggested to be equivalent to Malone antegrade continence enema in the management of fecal continence.2 It is important to elucidate its long-term effectiveness in children, however, because much data on the use of TAI have been collected retrospectively, with limited long-term follow-up.9
We previously reported the short-term follow-up results for TAI.4 In this study, we evaluated the long-term clinical efficacy of TAI and its effect on the QoL of children with SB and their caregivers.
Materials and methods
The prospective research proposal was approved by the Institutional Review Board of Yonsei University Healthcare System. Each participant signed the informed consent form. Participants were told that they could withdraw from the study if they experienced any discomfort during the TAI bowel management program or completing the questionnaire. We certify that all regulations concerning the ethical use of human volunteers were followed during the course of this research.
Between December 2010 and April 2011, we enrolled 47 children with SB referred to the pediatric urology department of the SB clinic at Severance Children’s Hospital in Korea for our TAI bowel management program.
Inclusion criteria were patients with SB aged 3–18 years with chronic constipation or unsatisfactory bowel management defined as fecal incontinence, constipation or both. Fecal incontinence was defined as involuntary stool loss occurring more than once a week. Constipation was defined as the presence of one or more of the following: a stool frequency of <3 times a week; hard, large stools that were difficult and painful to pass; or the use of laxatives.6 Exclusion criteria included evidence of bowel obstruction or inflammatory bowel disease and a history of surgery for a congenital colorectal disorder.
Study design
Children and their caregivers were evaluated prospectively at baseline, the short-term follow-up examination and long-term follow-up examination in the bowel management program. The primary caregiver or patient (if the child could read and understand the survey questionnaire) completed the survey in an independent room in the clinic with guaranteed privacy. Most surveys were administered and completed in the clinic. We evaluated the short-term effects of TAI at 3 months and the long-term outcomes at 3 years. We assessed the clinical efficacy and QOL related to constipation and fecal incontinence in children with SB.
TAI procedure
Patients or their caregivers were instructed on how to run lukewarm tap water from a plastic bag into the bowel through an irrigation cone-based TAI system (Colotip, Coloplast, Humlebak, Denmark) or catheter-based TAI system (Peristeen anal irrigation system, Coloplast), depending on the child’s age. Using catheter-based TAI with its rectal balloon catheter is difficult in younger chidlren, who are less cooperative, because the procedure requires more cooperation from the child than that required for cone-based TAI. Therefore, we usually recommend cone enema for children younger than 6 years. Initially, enemas were administered daily. If successful, the frequency was reduced to once every 2–3 days.3 Enema volume was initially 300–500 ml but was increased to 500–700 ml depending on age and need. Retrograde large volume enemas clean only the distal part of the colon. To ensure that patients and caregivers received adequate knowledge about TAI, a specialized nurse practitioner provided training on its use. The methods for training included educational pocketbook, demonstration and practice by parents. During the trial, the nurse practitioner provided telephonic assistance within 2 weeks for evaluation of TAI program at least once and parents could call up nurse practitioner whenever required and inquired about the bowel management status.
Instruments
The survey questionnaire to assess the clinical efficacy of bowel management was developed on the basis of the literature related to bowel programs for children with SB and their caregivers.3, 4, 6, 17, 18, 19, 20, 21, 22 Clinical efficacy was based on parameters such as fecal continence/pseudo-continence, frequency of bowel movements, bowel care time (in minutes per day) and the number of diaper changes per day. Fecal continence was defined as no involuntary stool loss in the treatment with TAI alone, and pseudo-continence was defined as involuntary stool loss no more than once a week with the use of TAI treatment.3 Most items in the questionnaire for QoL were based on the study by Nanigian et al.,20 with the author’s permission, which assessed the fecal incontinence and constipation quality of life (FICQOL) in children with SB. To assess content validity and cultural approval of the questionnaire, six experts (two pediatric urologists, one pediatrician, one specialized nurse practitioner and two parents who have a child with SB) were consulted, and the items were revised accordingly. The questionnaire focuses on the aspects of daily life on which bowel incontinence and bowel care have a significant impact. It had a total of 40 items in three parts: part (1) 9 items on defecation symptoms and bowel management status; part 2) 21 items on QoL related to bowel management (8 items on travel and socialization; 6 items on caregiver support and emotional impact; 4 items on family relationships; and 3 items on financial impact; Appendix); and part 3) 10 items on general characteristics of the child and parent. Internal consistency of 21 items (excluding the defecation symptoms and bowel management status and the general characteristics) showed a Cronbach’s Alpha coefficient of 0.763. Higher scores indicate lower QoL. Patients who were no longer using TAI were asked to answer the item involving the description of reasons for stopping.
Statistical analysis
Statistical analysis was performed on the survey items at baseline and at short-term and long-term follow-up analysis with repeated analysis of variance and paired matched using a Wilcoxon signed-rank test. Data were analyzed using SPSS version 20.0 (SPSS, Seoul, Republic of Korea).
Results
All 47 children were evaluated at short-term follow-up examination; 3 children were lost to follow-up at the third year. Finally, we evaluated 44 children: 38 (86.4%) were active users, whereas the remaining 6 (13.6%) were nonusers at the long-term follow-up examination (Figure 1). Of these, 25 were born with meningomyelocele and the median age of the children was 5.3 (3.0–13.8) years at study initiation. The bowel program began with the use of a cone-based (34.1%) or catheter-based (65.9%) TAI (Table 1).
In patients still undergoing treatment, the mean grade of satisfaction with TAI was 8/10. The mean irrigation frequency was every 3 days, with a mean volume of 500 ml of water. Approximately 63% children needed 40–59 min for TAI and defecation after irrigation, and 79% of the children did not need additional treatments for defecation. The common adverse effect during TAI was abdominal discomfort (60.5%), and 39.5% of children had no adverse effects (Table 2). All the children were taken care of by their caregivers using TAI at baseline and short-term follow-up examination. However, 3 years later, 15 of 44 children used TAI by themselves and their mean age was 9.2 years.
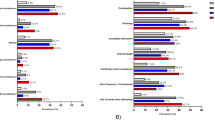
We observed a sustained improvement in defecation symptoms with TAI (Table 3). Comparing baseline and short-term and long-term results, fecal pseudo-continence improved from 35.1 to 91.9% and 89.2%, respectively, and the daily bowel care decreased from 29 to 17 and 19 min, respectively (P=0.022). The number of diaper changes and episodes of fecal incontinence significantly improved from baseline to short-term and long-term follow-up examinations (from 1.6 to 0.2 and 0.2, P<0.001; from 7.3 to 0.4 and 0.4, P=0.004; respectively). Children and caregivers reported a continuously improved and maintained QoL at the long-term follow-up examination. We observed a significantly improved effect on patient travel and socialization (from 13.1 to 7.5 and 8.8, P=0.001), caregiver support and emotional impact (from 13.0 to 8.5 and 9.1, P<0.001) and family relationships (from 3.8 to 2.0 and 2.3, P=0.028) in QoL (Table 3).
All six children who stopped treatment were using catheter-based TAI. The reasons for withdrawal of TAI were dislike of treatment by the children (four), unsatisfactory effect and burster/expulsion of the ballooned rectal catheter (two), high cost of the catheter (one), no reason (one) and normal defecation (two).
Discussion
TAI aims to improve and subsequently maintain regular bowel emptying combined with an improvement or resolution of constipation and fecal incontinence.13 Although TAI has been described as an effective treatment option,2, 14, 15, 16 our 33-month follow-up after TAI is the longest in a pediatric population, and our treatment compliance rate of 86.4% was the highest compared with adult studies. The rate of continuous TAI use at long-term follow-up was generally reported in the range of 34.6–62.5% in adult studies.23, 24, 25, 26 We surmise that the successful rate of a safe long-term use of TAI was because of the role of parents and specialized nurse practitioners. In studies of children, the role of parents is very important until they reach adolescence, and the caregivers are responsible for a child’s continence. If their child experiences fecal incontinence at school, it leads to sociopsychological difficulties and failure of successful developmental achievement.27 Furthermore, according to cultural differences, Korean parents take full responsibility for their child’s care because support programs for children with chronic condition in Korea are still very limited.28 For this reason, they seem to be more overprotective of their child and it led to be more proactive in the bowel management of their children comparing with adult/elderly population. It was essential that a designated specialized nurse practitioner provides structured follow-up of the children. It was also important that the patients know that they have open access back to the service in between scheduled contacts. Follow-up needs not be frequent or in-person but should ideally be with the same professional for each individual patient.29
After starting TAI, fecal incontinence significantly improved, with a decrease in bowel care time, the number of diaper changes and fecal incontinence episodes at the short-term follow-up examination. In addition, these improvements were maintained at the 3-year long-term follow-up examination. In our study, we evaluated not only the short-term and long-term clinical efficacies of TAI but also its effect on the QoL of children and their caregivers. We observed that these successful clinical results led to the improvement of QoL of children with SB and their caregivers. We surmise that children’s self-care ability can be increased with advancing years generally. However, if they cannot resolve their constipation and fecal incontinence, it cannot be improved with merely increasing the age of children. We have already confirmed the results of marked effectiveness in diaper use at short-term follow-up.14 Therefore, we believe that maintained bowel continence is the main cause of improved use of diapers rather than the increasing age of the children.
Our children and parent’s satisfaction was 8.0 after using TAI at the long-term follow-up examination (scale, 0–10). These results are similar to those obtained in other studies, where medium-to-high levels of satisfaction were reported in most cases.1, 3, 12, 14 However, until now, the single-scale numerical ratings of satisfaction may not have been sensitive enough to judge the impact of this procedure on the lives of SB children and their caregivers.2 Therefore, our evaluation of clinical efficacy, QoL and satisfaction following TAI for children with SB and their caregivers is more reliable compared with previous studies.
We have observed that the frequency of independent TAI use increased during the TAI program. Previous studies have reported independence ratios of 23.12 and 12.5%,3 but our result was 34.1%. Our higher success rate in terms of independence may result from the early introduction of TAI bowel management and the support program with a specialized nurse practitioner. In our clinic, we recommend starting TAI at the age of 4–6 years if the child cannot achieve fecal continence, despite behavioral modification and medication. Matsuno et al.2 reported that children could use the enema procedure with the help of their parents in their teenage years, if they have used TAI at a young age. However, the nurse practitioner should provide guidance on the transition timing and advice on attaining independence.
Regular and complete bowel movements have many social and psychological benefits,14 including the reduced likelihood of confinement to the house because of bowel care, decreased caregiver emotional stress and improved family relationships. However, in terms of travel and socialization, the QoL was decreased at the long-term follow-up examination compared with that at the short-term follow-up examination. We surmise that children encounter many chances to participate in various outdoor activities at school with advancing years, which could be burdensome, despite maintaining fecal continence using TAI. Because most children in Korean with SB do not reveal their SB condition and bowel problems, they cannot use TAI freely during outdoor activities, including camping. We can suppose that the change in life values as the child grew can be the suitable reason. About 70% of participants were preadolescents and adolescents at the long-term follow-up. In this developmental age, they think friends are the most important values.30 Therefore, participating in peer group activity is the very important for them, and they can have higher expectations about their fecal continence.
In this study, 11 out of 29 children who started catheter-based TAI changed to cone-based TAI after consultation with our team. In addition, all of the nonusers at the long-term follow-up had started with catheter-based TAI initially. Most experienced practical problems such as burster/expulsion of the rectal catheter and financial problems. These results were similar to those of Kim’s study26 that indicated practical problems with TAI in 63.5% of patients; in 48.1%, the problem was expulsion of the rectal catheter. Balloon burst and expulsion have already been reported previously in the literature (33–77%).9, 12 It is similar to a western study for adults, the practical problems and difficulties with catheter occurred in approximately one in three patients and was the cause of discontinuation in four patients.31 Financial burden is another problem, as TAI is not reimbursed by the Korean national health insurance program, meaning that participants had to cover all the expenses of the TAI device.26 Comparing two types of TAI in Korea, the price of the cone-based TAI is approximately 80 dollars, and it can be recycled for 1 year. However, the price of the catheter-based TAI system is approximately 300 dollars, and individual catheters, which cost 10 dollars each, cannot be used again. The differences in cost resulted in switching of the type of TAI in some cases. Therefore, we need to identify patients in whom a catheter-based TAI should be used and those in whom a cone-based TAI is better suited, depending on the child’s developmental stage, child’s and parents’ preference and socioeconomic status.
Over 60% of children experienced abdominal discomfort or pain during the TAI procedure, which is similar to that reported by previous studies.6, 10, 11, 15, 26 However, anorectal pain, nausea, headache and other symptoms were not reported in any case in this study. There are documented risks associated with TAI, which include systemic reactions to irrigation solutions and rectal perforation,9 but these adverse effects were not noted in our study. Complete evacuation of water and stool can be time-consuming. Further research should aim at finding methods to decrease this time; for example, decrease time by adding colon motility stimulation agents to the enema.
Limitations of this study include the use of non-validated questionnaires. Therefore, a reliable and validated QoL measure specifically designed to assess the impact of fecal incontinence and constipation on the lives of children with SB and their caregivers is needed. TAI is a safe method to improve long-term constipation and fecal incontinence in children with SB. Therefore, we recommend this simple therapeutic method as a safe and valid choice for the treatment of neurogenic bowel problems, especially from early childhood, if they do not achieve fecal continence with behavioral modification and medication.
Data archiving
There were no data to deposit.
References
Stevenson RE, Allen WP, Pai GS, Best R, Seaver LH, Dean J et al. Decline in prevalence of neural tube defects in a high-risk region of the United States. Pediatrics 2000; 106: 677–683.
Matsuno D, Yamazaki Y, Shiroyanagi Y, Ueda N, Suzuki M, Nishi M et al. The role of the retrograde colonic enema in children with spina bifida: is it inferior to the antegrade continence enema? Pediatr Surg Int 2010; 26: 529–533.
Vande Velde S, Van Biervliet S, Van Renterghem K, Van Laecke E, Hoebeke P, Van Winckel M . Achieving fecal continence in patients with spina bifida: a descriptive cohort study. J Urol 2007; 178: 2640–2644 discussion 2644.
Sawin KJ, Thompson NM . The experience of finding an effective bowel management program for children with spina bifida: the parent's perspective. J Pediatr Nurs 2009; 24: 280–291.
Krogh K, Lie HR, Bilenberg N, Laurberg S . Bowel function in Danish children with myelomeningocele. APMIS Suppl 2003; 109: 81–85.
Mattsson S, Gladh G . Tap-water enema for children with myelomeningocele and neurogenic bowel dysfunction. Acta Paediatr 2006; 95: 369–374.
Lemelle JL, Guillemin F, Aubert D, Guys JM, Lottmann H, Lortat-Jacob S et al. A multicentre study of the management of disorders of defecation in patients with spina bifida. Neurogastroenterol Motil 2006; 18: 123–128.
Christensen P, Kvitzau B, Krogh K, Buntzen S, Laurberg S . Neurogenic colorectal dysfunction - use of new antegrade and retrograde colonic wash-out methods. Spinal Cord 2000; 38: 255–261.
Bray L, Sanders C . An evidence-based review of the use of transanal irrigation in children and young people with neurogenic bowel. Spinal Cord 2013; 51: 88–93.
Cazemier M, Felt-Bersma RJ, Mulder CJ . Anal plugs and retrograde colonic irrigation are helpful in fecal incontinence or constipation. World J Gastroenterol 2007; 13: 3101–3105.
Liptak GS, Revell GM . Management of bowel dysfunction in children with spinal cord disease or injury by means of the enema continence catheter. J Pediatr 1992; 120: 190–194.
Eire PF, Cives RV, Gago MC . Faecal incontinence in children with spina bifida: the best conservative treatment. Spinal Cord 1998; 36: 774–776.
Lopez Pereira P, Salvador OP, Arcas JA, Martinez Urrutia MA, Romera RL, Monereo EJ . Transanal irrigation for the treatment of neuropathic bowel dysfunction. J Pediatr Urol 2010; 6: 134–138.
Choi EK, Shin SH, Im YJ, Kim MJ, Han SW . The effects of transanal irrigation as a stepwise bowel management program on the quality of life of children with spina bifida and their caregivers. Spinal Cord 2013; 51: 384–388.
Ausili E, Focarelli B, Tabacco F, Murolo D, Sigismondi M, Gasbarrini A et al. Transanal irrigation in myelomeningocele children: an alternative, safe and valid approach for neurogenic constipation. Spinal Cord 2010; 48: 560–565.
Neel KF . Total endoscopic and anal irrigation management approach to noncompliant neuropathic bladder in children: a good alternative. J Urol 2010; 184: 315–318.
Kanaheswari Y, Razak NN, Chandran V, Ong LC . Predictors of parenting stress in mothers of children with spina bifida. Spinal Cord 2011; 49: 376–380.
Lie HR, Lagergren J, Rasmussen F, Lagerkvist B, Hagelsteen J, Borjeson MC et al. Bowel and bladder control of children with myelomeningocele: a Nordic study. Dev Med Child Neurol 1991; 33: 1053–1061.
Rendeli C, Ausili E, Tabacco F, Caliandro P, Aprile I, Tonali P et al. Assessment of health status in children with spina bifida. Spinal Cord 2005; 43: 230–235.
Nanigian DK, Nguyen T, Tanaka ST, Cambio A, DiGrande A, Kurzrock EA . Development and validation of the fecal incontinence and constipation quality of life measure in children with spina bifida. J Urol 2008; 180: 1770–1773 discussion 1773.
Ok JH, Kurzrock EA . Objective measurement of quality of life changes after ACE Malone using the FICQOL survey. J Pediatr Urol 2011; 7: 389–393.
Rendeli C, Ausili E, Tabacco F, Focarelli B, Pantanella A, Di Rocco C et al. Polyethylene glycol 4000 vs. lactulose for the treatment of neurogenic constipation in myelomeningocele children: a randomized-controlled clinical trial. Aliment Pharmacol Ther 2006; 23: 1259–1265.
Faaborg PM, Christensen P, Kvitsau B, Buntzen S, Laurberg S, Krogh K . Long-term outcome and safety of transanal colonic irrigation for neurogenic bowel dysfunction. Spinal Cord 2009; 47: 545–549.
Christensen P, Krogh K, Buntzen S, Payandeh F, Laurberg S . Long-term outcome and safety of transanal irrigation for constipation and fecal incontinence. Dis Colon Rectum 2009; 52: 286–292.
Hamonet-Torny J, Bordes J, Daviet JC, Dalmay F, Joslin F, Salle JY . Long-term transanal irrigation's continuation at home. Preliminary study. Ann Phys Rehabil Med 2013; 56: 134–142.
Kim HR, Lee BS, Lee JE, Shin HI . Application of transanal irrigation for patients with spinal cord injury in South Korea: a 6-month follow-up study. Spinal Cord 2013; 51: 389–394.
Sanders C, Bray L . Examining professionals' and parents' views of using transanal irrigation with children: Understanding their experiences to develop a shared health resource for education and practise. J Child Health Care 2013; 18: 145–155.
Choi EK, Yoo IY . Resilience in families of children with Down syndrome in Korea. Int J Nurs Pract; e-pub ahead of print 22 April 2014.
Emmanuel AV, Krogh K, Bazzocchi G, Leroi AM, Bremers A, Leder D et al. Consensus review of best practice of transanal irrigation in adults. Spinal Cord 2013; 51: 732–738.
Burns CE . Pediatric primary care, 5th edn Elsevier: Philadelphia, PA. 2012.
Christensen P, Bazzocchi G, Coggrave M, Abel R, Hultling C, Krogh K et al. A randomized, controlled trial of transanal irrigation versus conservative bowel management in spinal cord-injured patients. Gastroenterology 2006; 131: 738–747.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Appendix
Appendix
Items on Quality of Life Questionnaire related bowel management
Items (number of items)
Travel and socialization (8)
Child’s bowel care prevents him/her from going out of the house.
Child’s bowel care prevents me from going out of the house.
I avoid traveling with my child.
My child is afraid to go out because of stool incontinence.
I worry about the smell of my child’s stool incontinence.
My child’s worries about the smell of stool incontinence.
My child’s stool incontinence affects his/her ability to socialize and meet friends.
My child’s stool incontinence affects his/her physical activities (walking, sports, etc).
Caregiver support and emotional impact (6)
My child’s bowel care bothers me.
My child’s bladder care bothers me.
My child’s bowel problems make me feel depressed.
My child’s bowel problems make me feel anxious.
If my child was continence of stool, this would change my life.
If my child was continence of stool, this would change his/her life.
Family relationships (4)
My child’s bowel problems affect his/her relationship with siblings.
My child’s bowel problems affect my relationship with my other children.
My child’s bowel incontinence affects my relationship with my partner.
Financial impact (3)
Are you employed?
If no, does your child’s bowel care prevent you from working?
If you do work, how much does your child’s bowel care affect your job?
Rights and permissions
About this article
Cite this article
Choi, E., Han, S., Shin, S. et al. Long-term outcome of transanal irrigation for children with spina bifida. Spinal Cord 53, 216–220 (2015). https://doi.org/10.1038/sc.2014.234
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2014.234
This article is cited by
-
Peristeen Transanal Irrigation System to Manage Bowel Dysfunction: A NICE Medical Technology Guidance
Applied Health Economics and Health Policy (2019)
-
Short versus mid-long-term outcome of transanal irrigation in children with spina bifida and anorectal malformations
Child's Nervous System (2018)
-
Management of Functional Constipation in Children: Therapy in Practice
Pediatric Drugs (2015)