Abstract
Study design:
Retrospective economic analysis.
Objectives:
To determine the total direct costs of publicly funded health care utilization for the three fiscal years 2003/04 to 2005/06 (1 April 2003 to 31 March 2004 to 1 April 2005 to 31 March 2006), from the time of initial hospitalization to 1 year after initial acute discharge among individuals with traumatic spinal cord injury (SCI).
Setting:
Ontario, Canada.
Methods:
Health system costs were calculated for 559 individuals with traumatic SCI (C1-T12 AIS A-D) for acute inpatient, emergency department, inpatient rehabilitation (that is, short-stay inpatient rehabilitation), complex continuing care (CCC) (i.e., long-stay inpatient rehabilitation), home care services, and physician visits in the year after index hospitalization. All care costs were calculated from the government payer′s perspective, the Ontario Ministry of Health and Long-Term Care.
Results:
Total direct costs of health care utilization in this traumatic SCI population (including the acute care costs of the index event and inpatient readmission in the following year after the index discharge) were substantial: $102 900 per person in 2003/04, $100 476 in 2004/05 and $123 674 in 2005/06 Canadian Dollars (2005 CDN $). The largest cost driver to the health care system was inpatient rehabilitation care. From 2003/04 to 2005/06, the average per person cost of rehabilitation was approximately three times the average per person costs of inpatient acute care.
Conclusion:
The high costs and long length of stay in inpatient rehabilitation are important system cost drivers, emphasizing the need to evaluate treatment efficacy and subsequent health outcomes in the inpatient rehabilitation setting.
Similar content being viewed by others
Introduction
Spinal cord injury (SCI) results in a variety of acute motor, sensory and autonomic impairments typically requiring tertiary care and rehabilitation to optimize patient outcomes. In the province of Ontario, advances in prehospital (critical), acute care and early surgical decompression1 have resulted in improved survival and an increasing number of persons with SCI seeking specialized rehabilitation services to augment their neurologic and functional recovery. Accompanying reduced acute care lengths of stay before inpatient rehabilitation admission are changing the required resource intensity and service provision models.2 After discharge from inpatient rehabilitation, individuals with SCI continue to be predisposed to multiple impairments, and an increased propensity for related secondary health complications.3
In the months and years after the initial acute care episode, previous research has demonstrated that increased risk of secondary complications is associated with frequent physician contact and hospitalizations.4, 5, 6, 7 This finding was recently supported by our research team in two studies on physician utilization and rehospitalization among adults with traumatic SCI in Ontario, Canada. We determined that the mean number of physician visits for traumatic SCI patients was 31.7 (median 26)8 with a rehospitalization rate of 27.5% 1 year after initial acute care discharge.9 The main reasons for rehospitalisation were (in descending order) musculoskeletal, respiratory, gastrointestinal and urological disorders.9 Beyond these medical complications, individuals who sustain a SCI frequently require assistance with personal care and activities of daily living.10 Thus, SCI results in significant initial and ongoing health care costs, which may escalate over time with advancing medical technology and increasing life expectancies among this population.11, 12 As such, accurate cost data are necessary for care planning and appropriate decision-making regarding resource allocation.
The existing literature on the direct costs of traumatic SCI in particular, including in Canada, is sparse and has been associated with methodological limitations. For example, some studies reflect the experiences of a subset of the SCI population, such as patients treated at a single health care centre13 or by a single service provider,11 or injury by a specific cause.14 Other studies have relied on patient recall to identify use of health services,4, 5 or estimated costs using secondary data sources such as government or trade association publications.13 Most recently, using information from the National SCI Statistical Centre in the United States, DeVivo et al.15 determined that overall mean first-year costs were $222 087 and that mean annual costs after 1 year were $68 815 (2009 US $). They reported mean initial acute care costs of $76 711 and mean rehabilitation costs of $68 543 (2009 US $). One Canadian population-based cohort study, on the direct health care costs after traumatic SCI, followed individuals who sustained a SCI in Alberta, Canada, from their date of injury to 6 years after injury.10 This study of 233 newly injured SCI patients determined that attributable health care costs in the first year after injury were $121 600 (2002 Canadian (CDN) $) per person with a complete SCI and $42 100 per person with an incomplete SCI. In the subsequent 5 years, annual attributable costs were $5 400 and $2 800 for persons with complete and incomplete SCI, respectively. The current study, also from Canada, includes more complete and recent health system data and a larger study population from Ontario, the most populous province in Canada. The primary objective of this study was to determine the direct costs of health care services for three fiscal years 2003/04 to 2005/06, for services provided among individuals with traumatic SCI from the time of initial hospitalization to 1 year after discharge.
methods
Study population
The initial population (n=936) consisted of men (n=694; 74.1%) and women (n=242; 25.9%) with incident cases of traumatic SCI between 2003/04 and 2006/07. SCI cases were identified by ICD-10 codes. The specific details of how cases of SCI were identified including the exclusion criteria have been described previously as well as in Figure 1.8, 9, 16
Inclusion and exclusion criteria to identify incident cases of traumatic SCI.Further exclusion were applied to the incident traumatic SCI cases in order to assemble the health care utilization cohort: (1) in-hospital mortality; (2) index discharge after 31 March 2006 (a minimum of 1 year was needed for follow-up of the 2005/06 cohort); and (3) died within 1 year after the index discharge (a minimum of 1 year was needed for follow-up). It should be noted that index discharge refers to discharge from the acute care center.
Overview of cost calculations
Health system costs were calculated for inpatient acute, emergency department (ED), inpatient rehabilitation, complex continuing care (CCC) (similar to Skilled Nursing Facilities in the US), home care services and physician visits from admission for an index SCI admission through to 1 year after index discharge. The Ontario Ministry of Health and Long-Term Care (MOHLTC) pays for all medically necessary institutional and community health care services. Although the government may seek recoveries from private auto and accident insurance where applicable, we include these services in our estimate of direct health care costs. Medication costs were not available for patients under age 65 and were not included in any cost calculations. Indirect costs to the patient, family or third party payers for other non-medically necessary services or services not funded by the Ministry were not included as there are no data sources applicable to the present study population. Total annual costs were calculated by summing per-patient case costs in each care setting. Costs were estimated from administrative data following recommended guidelines.17 Hospital and home care costs were based on costs reported to the Ontario government. Physician (that is, primary and specialist physicians) payment rates were based on the Ontario Health Insurance Plan (OHIP) fee schedule. For comparison purposes, all costs were converted to 2005 CDN $, using the consumer price indices (CPI) for the other health care services basket. CPI values were obtained from Statistics Canada CANSIM databases.18
Acute care
Each inpatient acute care discharge abstract database record includes the resource intensity weight associated with the hospital stay; the relative amount of hospital resources required to care for a patient. A resource intensity weight of 1.0 is equivalent to the average cost for a referent (equivalency) inpatient stay. We calculated the acute care cost by multiplying the resource intensity weight for each inpatient stay by the provincial average cost per weighted case obtained from the MOHLTC financial information management branch website.18
Inpatient rehabilitation
Cost weights per inpatient rehabilitation stay were assigned based on functional independence measurement rehabilitation cost groups validated for use in Ontario.18 Inpatient rehabilitation costs per weighted case were only available for 2004/05 and were extrapolated to other study years based on the rate of increase in acute hospital case costs. This estimate assumes that changes in rehabilitation hospital costs were the same as changes in acute hospital care costs, which is justified from a financial perspective as most inpatient rehabilitation hospital beds in Ontario are housed within acute hospitals.
Complex continuing care
Cost weights for CCC were based on the Resident Assessment Instrument-Minimum Data Set Resource Utilization Groups (RUG III),19 which represents the relative amount of hospital resources required to care for a patient each day in a CCC bed. We calculated the CCC case cost by multiplying the RUG-III weight for each patient by the average referent (equivalency) cost per day and multiplying this weighted per day cost by the patient′s length of stay. For residents not discharged within a year we only included costs to 365 days.
Outpatient and community-based care
ED costs were calculated by multiplying the number of ED visits by the average cost per ED visit. Physician costs were obtained based on the number of visits by type of visit (identified by the billing code in the OHIP record) and the associated fee code. Home care costs were based on the number of visits by type of service (nursing, personal support, rehabilitation professional by type) multiplied by the average provincial visit costs for each type of service.
Analyses
The primary objective of the study was to describe the total cost incurred in each sector in each year of study. We calculated total, mean and variance statistics for sector-specific and total spending in each year of study. We also developed a linear regression model to determine the incremental patient and utilization factors that were related to total patient-specific cost. Total costs were right-skewed so regressions were performed using the natural logarithm of total cost as the dependent variable. Quantile and residual plots support the validity of the linear model using the natural logarithm of costs. Independent variables included in the model included patient characteristics sex, age (70 or older), site of injury (cervical, thoracic, lumbar), Charlson comorbidity count20 (3 or more), concurrent brain injury (that is, traumatic brain injury) and rurality21 as well as utilization patterns of in-hospital complications, acute length of stay, discharge to inpatient rehabilitation and length of stay, and discharge to complex continuing care. To aid the reader in interpreting the parameter estimates from the regression, predicted costs were calculated using the intercept and the parameter estimate for each significant variable to re-transform the costs into dollars by exponentiating the parameter estimates arising from the linear regression. Incremental costs were estimated by subtracting the predicted baseline (intercept only) cost from the latter predicted cost estimates.
Privacy/ethics
This study was approved by the research ethics board at the Institute for Clinical Evaluative Sciences and Sunnybrook Health Sciences Centre.
Results
The sociodemographic and clinical characteristics of the cohort have been previously described.8, 9, 16 This health care utilization cohort was 76% male, with a mean overall age of 47 years.8
All costs were calculated from the government payer′s perspective, the MOHLTC, and are reported in 2005 CDN $. Both the average per patient and total direct costs of health care utilization for traumatic SCI increased between 2003 and 2005. The average patient cost rose from $102 900 in 2003/04 to $123 674 in 2005/06. After adjusting for inflation, average per patient care costs increased primarily due to increases in the intensity of acute and inpatient rehabilitation care. Most costs in the fiscal year 2004/05 were slightly lower or remained the same as the prior year and larger increases were observed in the final year (with the exception of costs for acute care readmissions, which were nearly double in 2004/05) (Tables 1, 2, 3). Costs associated with CCC were only reported in the total cost due to small cell sizes.
Both the average per-person and the total system costs (Table 4) associated with inpatient rehabilitation are higher than all other costs in the health system. Although the acute care costs for the index event increased from an average of $30 591 CDN per person in 2003/04 to an average of $35 654 CDN per person in 2005/06, direct costs of rehabilitation after the index discharge increased from an average of $112 317 CDN per person in 2003/04 to an average of $119 945 per person in 2005/06. Acute care inpatient readmission increased from an average of $13 744 CDN per person in 2003/04 to an average of $15 084 CDN per person in 2005/06.
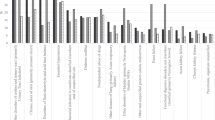
Across all of the institutional and community settings, the direct costs of rehabilitation after the index discharge were the highest, representing 58% of total costs of health care utilization, followed by inpatient acute care costs of the index event at 30%, and acute care inpatient readmission costs in the following year after index discharge at 4.5%. These trends were observed in each of the individual years. Complex continuing care contributed 3.5% (CCC not shown in tables due to small sample size), physician visits contributed 2.5%, home care in the following year after index discharge contributed 1.9% and ED visits in the following year after index discharge amounted to 0.17% of the total costs.
Results from the regression analyses are shown in Table 5. Significant patient characteristics related to total cost included sex, age and concurrent traumatic brain injury diagnosis. In-hospital complications reported in the hospital were associated with an average incremental cost of $5926 (parameter estimate=0.53694; 95% CI=0.40107, 0.67281). Treatment in an inpatient rehabilitation facility was associated with an incremental cost of $41 203 (parameter estimate=1.78198; 95% CI=1.62204, 1.94192) whereas treatment in complex continuing care was associated with an incremental cost of $61 501 (parameter estimate=2.12538; 95% CI=1.7467, 2.5043). Increases in length of stay (above the average length of stay) in acute and inpatient rehabilitation were each associated with incremental costs of only $63 (parameter estimate=0.00747; 95% CI=0.00545, 0.00949) and $39 per day (parameter estimate=0.00472; 95% CI=0.00357, 0.00587), respectively. The model fit the data very well with an adjusted R-square of 0.81.
Discussion
This population-based study examined the direct costs of health care utilization from the initial hospitalization to 1 year after discharge among individuals with traumatic SCI for fiscal years 2003/04 to 2005/06. Information on costs was comprehensive in that it included the inpatient acute care costs of the index event, the costs of inpatient rehabilitation after the index discharge, acute care inpatient readmission costs in the year following index discharge, as well as CCC, ED visits, home care visits and physician costs. The main results of this study revealed that (1) overall, the direct costs of health care utilization for traumatic SCI increased from the fiscal year 2003 to 2005; and, (2) across all of the institutional and community settings, the top three costs of health care utilization were for inpatient rehabilitation, initial inpatient acute care and acute care inpatient readmission in the year after the index discharge. Utilization and costs in early 2004/05 may be associated with lingering effects of the severe acute respiratory syndrome epidemic and a desire to reduce hospital utilization. The linear regression results also highlight the incremental individual-level costs associated with age, concurrent traumatic brain injury and both inpatient rehabilitation and complex continuing care hospitalizations. Although the latter costs are higher at the individual level, with very few such individuals, they constitute a small proportion of total health system costs.
Dryden et al.10 determined that hospitalizations were the highest category of expenditures ($7.3 million 2002 CDN$ or $8.4 million 2005 CDN $). Furthermore, and as previously mentioned, Dryden et al.10 found that the initial hospitalization (which included both the initial acute care and inpatient rehabilitation) costs for newly injured SCI patients were approximately $6.3 million (2002 CDN $) or $7.2 million (2005 CDN $), substantially lower than the costs reported in the present study. The present study separated the acute care inpatient index event and the inpatient rehabilitation costs, with the finding that the average total direct costs for rehabilitation are more than three times the average total costs for the acute care inpatient index event, in accordance with the longer length of stay in rehabilitation (mean 90.2 days±64.3)8 versus acute care (mean 21.7 days±31.4).8 Johnson et al.22 separated the average acute care and rehabilitation costs in the United States, but determined that the average costs in acute care were higher ($71 450 1992 USD; $88 219 1992 CDN) than in rehabilitation ($57 134 1992 USD; $70 543 1992 CDN) highlighting potentially different reimbursement and treatment patterns of institutional care across jurisdictions. It should be noted that these 1992 USD costs were converted to 1992 CDN using Purchasing Power Parities published by the OECD.23 The fact that rehabilitation costs after the index discharge constituted the largest proportion of health care utilization costs (that is, averaging 58% of the total costs from 2003 to 2005) may not be surprising. Progress in medical and rehabilitation treatment continues to improve survival among patients with the most complex needs,24 which undoubtedly keeps these costs high. This phenomenon contrasts with historical reductions in total rehabilitation utilization and reimbursement and pressures to reduce care costs in the United States.25 Until the second decade of 2000, Ontario had not seen such reductions, with a mean length of stay for the SCI population in Ontario rehabilitation hospitals of approximately 90.2 days±64.3 and a mean of 21.7±31.4 days in acute care.8
Our results also show that the highest proportion of total health care utilization costs after inpatient acute and rehabilitation was related to acute care inpatient readmission (totaling $2.8 million over 3 years in 2005 CDN $). As we have previously reported, the main causes of these readmissions were secondary complications including musculoskeletal, respiratory, gastrointestinal and urological disorders.9 Improving current care practices in preventing and managing secondary health complications could lead to not only improved quality of life in this population, but also reduced health care utilization and costs.
By comparison, disease entities that are also managed in a hospital setting have substantially lower per patient per year costs. For example, the per patient per year costs of cardiovascular disease have been reported as ranging from $3805 (2004 CDN $)26 to $27 772 (2004 CDN $).27 Similarly, a recent cost effectiveness study on heart failure clinics in Ontario, Canada determined that the per patient per year cost in standard clinics was $15 987 (2008 CDN $).28 Finally, Chang et al.29 determined the mean total costs per patient for cancer were $39 155 (2004 CDN $). Understanding the differences in the utilization requirements across the care continuum of the various diseases and populations is important for comparative costing.
This study, although rigourous in methodological approach, has some limitations. Cost calculations were limited to major health care services that were provided in the province of Ontario and paid for by the MOHLTC. Additional expenditures for pre-hospital care, diagnostic services, equipment and supplies to support activities of daily living and mobility in the community, and outpatient drugs are not included in the costs reported here. These can be substantial for some individuals with SCI depending on the nature and extent of disability. Indirect costs were also not captured such as societal costs from loss of work and family costs from caregiver absence from work. It was also not possible to determine the costs of health care utilization for out-of-province care or other services paid for through private sources. This results in an underestimate of total economic burden arising from traumatic SCI. Further, the data sources do not provide measures of severity such as the American Spinal Injury Association Impairment Scale, neurological outcomes or functional recovery of persons with SCI, which have been previously shown to be substantially associated with direct costs of health care utilization in traumatic SCI.10, 22
Despite these limitations, the current study has several strengths. This study has provided a comprehensive, recent estimate of the direct health care costs of SCI throughout the various stages of medical treatment—the initial acute care episode, inpatient rehabilitation and ED visits and/or hospital readmissions. It is one of the few population-based studies and is only the second Canadian study on the direct costs of health care utilization in traumatic SCI. Furthermore, it is the only study to use data from Ontario, which has a population of approximately 13 million people and represents 40% of the population of Canada. The current study also demonstrated that the total direct costs of rehabilitation are several times higher than the total costs of acute care. Finally, the use of administrative databases allowed population-based cost estimates. Thus, it is hoped that the current data can be used for informed health care planning and research, leading to not only improved health status and quality of life for patients but realistic costing of care for this population.
Conclusions
The largest cost driver in the health care system among SCI patients is inpatient rehabilitation care, where individual patients spend the majority of their time. Individuals with SCI require intensive therapeutic interventions to achieve optimal outcomes and therefore have long lengths of stay in inpatient rehabilitation. An undesirable effect of the current paper′s findings could be that length of stay in rehabilitation should be decreased in order to reduce costs. Instead, the investigators believe that future clinical and evaluative research should focus on the effects of creative strategies in rehabilitation such as novel service models or self-management programs as a potentially cost-effective strategy and that the link between understanding costs, service delivery and outcomes should be explored. These approaches would need to align with the potential for optimizing functional recovery for this population. Furthermore, we found that readmission costs were double in the year with the lowest inpatient rehabilitation costs. If costs were to be reduced in rehabilitation, a potential consequence might be increased ED visits, secondary health complication frequency and severity, and/or readmission rates to acute care. The costs reported in this study provide a baseline for evaluating the cost effectiveness of current and future treatment interventions. In future, looking at direct medical costs across the continuum of care will be critical for optimizing patient outcomes and using resources wisely.
Data archiving
There were no data to deposit.
References
Fehlings MG, Rabin D, Sears W, Cadotte DW, Aarabi B . Current practice in the timing of surgical intervention in spinal cord injury. Spine 2010; 35 (21 Suppl): S166–S173.
Verrier M, Ahn H, Craven C, Drew B, Fehlings M, Ford M et al. Ontario spinal cord injury informatics: informing practice research and innovation. Ontario Neurotrauma Foundation 2009, 1–64.
Paker N, Soy D, Kesiktaş N, Nur Bardak A, Erbil M, Ersoy S et al. Reasons for rehospitalization in patients with spinal cord injury: 5 years′ experience. Int J Rehabil Res 2006; 29: 71–76.
Berkowitz M . Assessing the socioeconomic impact of improved treatment of head and spinal cord injuries. J Emerg Med 1993; 11 (Suppl 1): 63–67.
Johnson RL, Gerhart KA, McCray J, Menconi JC, Whiteneck GG . Secondary conditions following spinal cord injury in a population-based sample. Spinal Cord 1998; 36: 45–50.
McKinley WO, Seel RT, Hardman JT . Nontraumatic spinal cord injury: incidence, epidemiology, and functional outcome. Arch Phys Med Rehabil 1999; 80: 619–623.
Dryden DM, Saunders LD, Rowe BH, May LA, Yiannakoulias N, Svenson LW et al. Utilization of health services following spinal cord injury: a 6-year follow-up study. Spinal Cord 2004; 42: 513–525.
Munce SEP, Guilcher SJT, Couris CM, Fung K, Craven BC, Verrier M et al. Physician utilization among adults with traumatic spinal cord injury in Ontario: a population-based study. Spinal Cord 2009; 47: 470–476.
Jaglal SB, Munce SEP, Guilcher SJT, Couris CM, Fung K, Craven BC et al. Health system factors associated with rehosptialisations after traumatic spinal cord injury: a population-based study. Spinal Cord 2009; 47: 604–609.
Dryden DM, Saunders LD, Jacobs P, Schopflocher DP, Rowe BH, May LA et al. Direct health care costs after traumatic spinal cord injury. J Trauma 2005; 59: 443–449.
DeVivo MJ, Stover SL . Long-term survival and causes of death. In: Stover SL, DeLisa JA, Whiteneck GG (eds). Spinal Cord Injury: Clinical Outcomes from the Model Systems. Aspen Publishers: Gaithersburg, MD, 1995: 289–316.
DeVivo MJ . Causes and costs of spinal cord injury in the United States. Spinal Cord 1997; 35: 809–813.
Tator CH, Duncan EG, Edmonds VE, Lapczak LI, Andrews DF . Complications and costs of management of acute spinal cord injury. Paraplegia 1993; 31: 700–714.
Smart CN, Sanders CR . The Costs of Motor Vehicle Related Spinal Cord Injuries. Insurance Institute for Highway Safety: Washington, DC, 1976: 1–114.
DeVivo MJ, Chen Y, Mennemeyer ST, Deutsch A . Costs of care following spinal cord injury. Top Spinal Cord Inj Rehabil 2011; 16: 1–9.
Couris CM, Guilcher SJT, Munce SEP, Fung K, Craven BC, Verrier M et al. Characteristics of adults with incident traumatic spinal cord injury (SCI) in Ontario, Canada. Spinal Cord 2010; 48: 39–44.
Jacobs P, Yim R . Using Canadian administrative databases to derive economic data for health technology assessments. Canadian Agency for Drugs and Technologies in Health: Edmonton, Alberta, 2009: 1–58.
Ministry of Health and Long-Term Care, Health Data Branch http://www.mohltcfim.com/cms/client_webmaster/login_a.jsp?rsectionID=website accessed 13 July 2011.
Fries BE, Schneider DP, Foley WJ, Gavazzi M, Burke R, Cornelius E . Refining a case-mix measure for nursing homes: resource utilization groups (RUG-III). Med Care 1994; 32: 668–685.
Deyo RA, Cherkin DC, Ciol MA . Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 1992; 45: 613–619.
Kralj B . Measuring ‘rurality’ for purposes of health-care planning: an empirical measure for Ontario. Ont Med Rev 2000; 67: 37–40.
Johnson RL, Brooks CA, Whiteneck GG . Cost of traumatic spinal cord injury in a population-based registry. Spinal Cord 1996; 34: 470–480.
OECD. PPPs and exchange rates. StatExtracts http://stats.oecd.org/Index.aspx?DataSetCode=SNA_TABLE4. accessed 15 January 2011.
Vaidyanathan S, Soni BM, Gopalan L, Sett P, Watt JW, Singh G et al. A review of the readmissions of patients with tetraplegia to the Regional Spinal Injuries Centre, Southport, United Kingdom, between January 1994 and December 1995. Spinal Cord 1998; 36: 838–846.
Waters RL, Apple DF, Meyer PR, Cotler JM, Adkins RH . Emergency and acute management of spine trauma. In: Stover SL, DeLisa JA, Whiteneck GG, (eds). Spinal cord injury: clinical outcomes from the model systems. Aspen Publishers, Inc: Gaithersburg, MD, 1995.
Garis RI, Farmer KC . Examining costs of chronic conditions in a Medicaid population. Managed Care 2002; 11: 43–50.
Sasser AC, Rousculp MD, Birnbaum HG, Oster EF, Lufkin E, Mallet D . Economic burden of osteoporosis, breast cancer, and cardiovascular disease among postmenopausal women in an employed population. Womens Health Issues 2005; 15: 97–108.
Wijeysundera HC, Machado M, Wang X, van der Velde G, Sikich N, Witteman W et al. Cost-effectiveness of specialized multidisciplinary heart failure clinics in Ontario, Canada. Value Health 2010; 13: 915–921.
Chang S, Long Sr, Kutikova L, Finley D, Crown WH, Bennett CL . Estimating the cost of cancer: results on the basis of claims data analyses for cancer patients diagnosed with seven types of cancer during 1999 to 2000. J Clin Oncol 2004; 22: 3524–3530.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Munce, S., Wodchis, W., Guilcher, S. et al. Direct costs of adult traumatic spinal cord injury in ontario. Spinal Cord 51, 64–69 (2013). https://doi.org/10.1038/sc.2012.81
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2012.81
Keywords
This article is cited by
-
Cost-effectiveness analysis of overground robotic training versus conventional locomotor training in people with spinal cord injury
Journal of NeuroEngineering and Rehabilitation (2023)
-
Use of professional home care in persons with spinal cord injury in Switzerland: a cross-sectional study
BMC Health Services Research (2023)
-
Incidence and mortality of spinal cord injury from 2008 to 2020: a retrospective population-based cohort study in the Piedmont Region, Italy
Spinal Cord (2023)
-
A geospatial examination of specialist care accessibility and impact on health outcomes for patients with acute traumatic spinal cord injury in New South Wales, Australia: a population record linkage study
BMC Health Services Research (2021)
-
Factors associated with discharge destination following inpatient functional rehabilitation in patients with traumatic spinal cord injury
Spinal Cord (2021)