Abstract
Study design:
Literature review.
Objectives:
Update the global maps for traumatic spinal cord injury (TSCI) and incorporate methods for extrapolating incidence data.
Setting:
An initiative of the International Spinal Cord Society (ISCoS) Prevention Committee.
Methods:
A search of Medline/Embase was performed (1959-Jun/30/2011). Enhancement of data-quality 'zones' including individual data-ranking as well as integrating regression techniques to provide a platform for continued regional and global estimates.
Results:
A global-incident rate (2007) is estimated at 23 TSCI cases per million (179 312 cases per annum). Regional data are available from North America (40 per million), Western Europe (16 per million) and Australia (15 per million). Extrapolated regional data are available for Asia-Central (25 per million), Asia-South (21 per million), Caribbean (19 per million), Latin America, Andean (19 per million), Latin America, Central (24 per million), Latin America-Southern (25 per million), Sub-Saharan Africa-Central (29 per million), Sub-Saharan Africa-East (21 per million).
Discussion:
It is estimated that globally in 2007, there would have been between 133 and 226 thousand incident cases of TSCI from accidents and violence. The proportion of TSCI from land transport is decreasing/stable in developed but increasing in developing countries due to trends in transport mode (transition to motorised transport), poor infrastructure and regulatory challenges. TSCIs from low falls in the elderly are increasing in developed countries with ageing populations. In some developing countries low falls, resulting in TSCI occur while carrying heavy loads on the head in young people. In developing countries high-falls feature, commonly from trees, balconies, flat roofs and construction sites. TSCI is also due to crush-injuries, diving and violence.
Conclusion:
The online global maps now inform an extrapolative statistical model, which estimates incidence for areas with insufficient TSCI data. The accuracy of this methodology will be improved through the use of prospective, standardised-data registries.
Similar content being viewed by others
Introduction
Traumatic spinal cord injury (TSCI) is a catastrophic event that is sudden and unexpected and can be devastating and costly in human and social terms. TSCI in developed (high income) and developing countries primarily affects males aged 18–32 years, and in developed countries, due to an ageing population, males and females over the age of 65 years. Globally, information on the number of people living with TSCI (prevalence) as well as the number of new cases annually (incidence) is minimal, particularly in developing countries, hindering injury prevention, health care and other social planning. This paper updates the epidemiological information available primarily from published papers and reports, provides ranked data for statistical extrapolation and highlights issues relevant to decreasing the health-care burden of TSCI globally.1, 2 The high societal costs in developed countries, the high mortality rate in developing countries and the geographic spread in aetiology emphasise the importance of regionally targeted primary and secondary prevention programs.
Methods
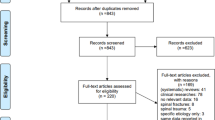
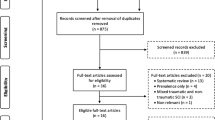
The literature search of Wyndaele3 was repeated from 1959 to June 30th 2011 without date or language restriction using search phrases (exploded): ‘Epidemiology of spinal cord injury’, ‘Prevalence of spinal cord injury’; ‘Incidence of spinal cord injury’ through Medline and Embase.3, 4, 5
World Health Organisation (WHO) global regions were utilised to allow epidemiologically similar regions to be compared.6 Regional data are now grouped into four broad (enhanced) zones with the addition of an Orange Zone to categorise appropriately extrapolated data (Box 1). The most representative studies were selected using the methods described by Cripps et al.2
Maps using TSCI incidence and aetiological data were developed for WHO global regions and countries within these regions using mapping and graphical techniques developed by Myriad Editions (http://www.myriadeditions.com/health).
Sources of data used were primarily from peer-reviewed journal articles and governmental publications and were prospective or retrospective studies using data from spinal registries, population registries, hospital data (admission and discharge data) and health survey data. Data sources from all cited references are summarised in Supplementary Table 1 http://www.iscos.org.uk/page.php?content=67 (online). Each paper’s quality of evidence is graded using the annotation (Box 2).
For TSCI there is a paucity of data available, with Green or Yellow Zone data only available for North America (USA and Canada), Australia and Western Europe (Denmark, Greenland, Iceland, Sweden, Ireland and Germany). These Green and Yellow Zone countries provided some national incidence data.7, 8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 18 There were larger numbers of regional-specific incidence data, however globally there were large regions without any published incidence data. To rectify this, regression modelling was developed and used to provide spinal cord injury (SCI) estimates of TSCI incidence using known countries’ TSCI incidence rates, populations at risk and a range of measured economic indicators. The formulae used for estimating TSCI incidence using population data within this paper is presented in Fitzharris et al.1 (in this issue).
The accompanying methods paper by Fitzharris et al.1 outlines a linear regression model using TSCI cases as the dependent variable and the population at risk as the single independent variable. Thirty-one studies (from 1990) were used in TSCI estimates. The ‘fit’ of the model was improved using fractional polynomials. A more advanced model for future iterations of the global mapping project is presented to give an example of how these data can be evaluated when data standardisation improves baseline study quality.19
These TSCI estimates are classified and mapped as Orange Zone data. Additional details of the modelling and detailed tables TSCI estimates (and ranges) are provided at Fitzharris et al.1 TSCI Prevalence will be extrapolatively modelled in a future iteration of the global maps.
Some of the data and issues discussed in this paper have been published in the previous global TSCI paper by Cripps et al.2
Results
The following information used median/average values and ranges for countries’ data within WHO global regions and reflects an iterative and methodological update of the 2010 global mapping project.2
Prevalence of TSCI globally
Detailed prevalence data for TSCI are summarised in Supplementary Table 2 http://www.iscos.org.uk/page.php?content=67 (online). The range of reported global prevalence is between 236 to 4187 per million. Missing prevalence data for major populations persists. Data for Asian countries are inadequate and may under-estimate prevalence within this region. No published data exist for Africa or South America. The differing methodologies used to derive prevalence have previously been noted.3
North America, high income
US data are unchanged (721–4187 per million, with a median of approximately 853 per million);9, 20, 21, 22, 23 however, statistical techniques were used by the Rick Hansen group to extrapolate a new Canadian prevalence of 1184 per million, which we have categorised as Orange Zone data.10, 24, 25
Other regional data
Regions of Asia South and SouthEast (236 to 464 per million TSCI26, 27), Australasia (370 in 1987 to 681 per million in 199828, 29, 30), Western Europe (280 per million31 and 316 per million15) are unchanged.2
Incidence and aetiology of TSCI globally
It is estimated that globally in 2007, there would have been between 133 and 226 thousand incident cases of TSCI from accidents and self-harm/violence.1 The most representative incidence statistic for each country within WHO global regions is presented in Supplementary Table 3 http://www.iscos.org.uk/page.php?content=67 (online). along with available aetiology data. Trends and statistical outliers in aetiology are identified.
Directly interpretable incidence data has not changed for the Green and Yellow Zone regions of North America, Western Europe and Australia.2 Four-wheeled road traffic accidents remain high in all three regions, higher violence/self-harm occurred in North America and high rates of falls were reported, particularly in Western Europe where the population is older.32 Median/average values for these data were calculated from information contained in Supplementary Tables 3 and Table 4 http://www.iscos.org.uk/page.php?content=67 (online). Map 1 (Figure 1) and Map 2 (Figure 2) illustrate WHO global regional and country incidence, aetiological, neurological and survival data.33
Orange Zone data derived through regression techniques outlined in the methods are presented for Africa, Caribbean and South America and, as an interim, may provide an alternative estimate of incidence and an improvement of Red Zone regional data, where the likelihood of maintaining a longitudinal registry is low.
Red Zone incidence data, although presented in the tables, are not analysed or interpreted, as comparisons between regions and countries are not supported and could be misleading.
Asia, East
Li and Ning34, 35 provided recent regional incidence data for mainland China (60.6 TSCI per million population per year in Beijing and 23.7 in Tianjin province). As previously reported,36 land transport accounted for 49% of TSCI in the Taiwanese population with 65% of these accidents associated with two-wheeled vehicles.36 Falls, particularly in Tianjin province, were higher than most developed countries. Although work-related TSCI was reported only for Tianjin province (0.8%), this is inaccurate as the proportion of falls that are work-related are not included in this figure, and the number of falls in this area is high (57%). It is important that future reports from this region parse out the number of work-related falls. A high incidence of TSCI in the aged with high rates of tetraplegia, predominantly due to low falls, was found in Taiwan.36
Asia, SouthEast
We have previously commented on high rates of land transport TSCI in Vietnam and Thailand, in particular motorcycles and other non-standard transport like jitneys.27, 37, 38 Contributing factors that increase the risk of accidents include transport of heavy loads, multiple passengers and poor road infrastructure.
Recent unpublished data from Vietnam (2010) using ASCoN SCI software (http://www.iscos.org.uk/page.php?content=20) in several spinal treatment centres, report that falls and land transport accounted for more than 75% of TSCI cases. Most falls occurred in the home (51%) while doing housekeeping and house maintenance. An additional 46% of falls occurred in the workplace. Thirty percent of the falls resulted in tetraplegia. Land transport continued to be the main cause of TSCI. Motorcyclists account for 70% of the land transport cases and 32% were complete paraplegic (highest in the 15–24-year age group). Trucks and bicycles each accounted for 10% of the TSCI cases, violence related 4% and sports 1%. (Unpublished data: Eric Weerts, Handicap International: ASCoN SCI registry software).
Australasia
Australia (updated) and New Zealand12, 39 have high rates of land transport TSCI (predominantly from four-wheeled vehicles) and growing numbers of falls, particularly in the elderly.2 Australia has high rates of water-related TSCI (9% of all TSCI reported in 2010). Sixty-three percent of these injuries were to the cervical spinal segments caused by diving into a body of water.40 In New Zealand, as reported previously, rugby was responsible for 8% of their sports-related injuries.
Europe, Eastern
New Estonian data are combined with regional data for Russia41, 42, 43 and show the main causes of TSCI in Estonia and Russia (Novosibirski and Saint Petersburg) were falls (median 40%) and land transport (median 25%).
Europe, Western
Reported rates are: Denmark (9.2 per million), Finland (13.8 per million), France 19.4 per million, Germany 10.7 per million, Greece 33.6 per million, Greenland 26 per million, Iceland 20 per million, Ireland 13.1 per million, Italy 19 per million, Israel 15.9 per million, Netherlands 7.5 per million, Norway 26.3 per million, Spain 12.1 per million, Switzerland 15 per million.2 The median calculated from these data for the Western Europe region is 16 per million. Median values were calculated from information contained in Supplementary Table 3.
New data are available for Spain (Aragon), which had a reported incidence rate of 12.1 per million, with land transport accidents accounting for 57% of TSCI. About one-quarter of cases were due to falls in this region and, for the period of this study (1972–2008), there was an increase in the proportion of TSCI related to falls in elderly people (older than 60 years).44
North Africa, Middle East
Land transport accidents were high in this region.45, 46, 47 As previously reported,5 Saudi Arabia and Qatar have the highest reported proportional rates of TSCI caused by land transport accidents in the world (85% and 72%, respectively).47, 48 TSCI from high falls were common in Turkey (37%). Accidental gunshot injuries were high in Jordan (26%). New data are available for fall-related TSCI in Iran, which was higher (42%) than in Qatar, which was very low (13%).49, 48 An estimated Middle Eastern incidence rate based on Jordanian, Qatari and Turkish incidence data is about 15 TSCI per million per year but this probably is an under-estimate and should be interpreted with caution.
North America, high income
A newly calculated national incidence rate reported for Canada was 35 per million per year in 2006,11 and an extrapolated value of 52.3 in 2010.10 Data for the USA are unchanged (30–40 per million per year, median 38.4).9, 23, 50, 51
Violence-related TSCI in the USA is high.51, 52 The most recent national rate for fall-related TSCI is 23%.51
As previously reported, Hawaii has a higher incidence of diving-related TSCI (12%), when compared to the rest of the USA.53 In other USA regional data reports, diving-related TSCI ranged from 3–6% of the TSCI cases.54, 55, 56, 57, 58, 59
Other regional data
Asia Pacific, high income; Asia, South; Europe, Central; Latin America, Tropical; Oceania; Sub-Saharan Africa, Southern; Sub-Saharan Africa, West are unchanged.2
Extrapolated data
Incidence rates were not available for many WHO global regions in Central and South America, the Caribbean and Africa due to lack of published TSCI data. Using regression modelling to estimate TSCI incidence rates, estimates and confidence intervals for the following WHO global regions are presented below and illustrated in Map 1 (Figure 1).
Fitzharris et al.1 has detailed tables for WHO geographical regions (a common format). We have re-aggregated these to reflect the WHO global region subgroups,33 which provides more detail:
Latin America, Andean (19 (13–24)); Latin America, Southern (25 (14–27)); Latin America, Central (24 (12–32)); Sub-Saharan Africa, Central (29 (13–39)); Sub-Saharan Africa, East (21 (16–26)) and Caribbean (19 (12–26)).
Survival of TSCI globally
(Supplementary Table 4) http://www.iscos.org.uk/page.php?content=67 (online).
Our ability to care for people with SCI is reflected in a number of survival statistics: the survival rate at 1 and 10 years after injury, and the life expectancy compared with the normal population.
Developing countries have the highest 1-year mortality rates (particularly Sub-Saharan Africa).60, 61, 62
Long-term longitudinal data (10-year mortality) are only available for those countries with established SCI registries: USA, – Southeast region63 16.2%; Canada, Manitoba region64 10.7% and Australia,65 14.3%.5
We have not performed a detailed literature review of life expectancy at this time. Newer data, confirming improved survival in developed countries, are available from Middleton et al.66 who projected from New South Wales (Australian) data that the estimated life expectancies (25–65 years; percentage of mean life expectancy) ‘ranged between 64%–69%, 74%–65%, 88%–91% and 97%–96% for C1-4 ASIA A-C, C5-8A-C, T1-S5 A-C and ASIA D lesions, respectively’.66
Discussion
The proportion of TSCI resulting from land transport (four-wheeled vehicles) is stable or decreasing in developed countries, but on the increase in developing countries. The relatively smaller proportion of TSCI due to land transport (Map 2) in developing countries belies the extent of the problem, owing to the growing number of people being (preventably) injured and poorer survival to hospital. The global status report on world safety outlined that 90% of fatal land transport accidents in 2004 occur in these low and middle income countries, representing only 48% of the worlds vehicles, and are the highest cause of death in people aged 15–29 years, the second highest in those aged 5–14 years and the third highest in the 30–44 year age group.67, 68
Developed countries have safer cars (energy absorbing body design, seat belt use and air bags), better road design, mandatory licensing and training as well as alternative transport implementation such as mass transit-rail. Developing countries in contrast have poor infrastructure, many non-standard vehicles, less regulation and enforcement due to cost, lack of resources and a poor safety culture. Relative TSCI land transport accident rates in areas like Asia will continue to increase as trends in transport use continue, transitioning from animal drawn vehicles and bicycles to motorcycles and to cars.67, 68 The Asia East region is particularly complex owing to a paucity of data and known diversity between rural and urbanised areas. This disparity is illustrated by life expectancy relative to income across, for example, China (www.gapminder.org: accessed Dec 2011) where a city, such as Shanghai, compares well with South Korea, Israel and New Zealand; whereas the provinces of Guizhou, Yunnan and Gansu compare with India, Pakistan and Yemen. TSCI statistics available for this country are far from representative and need to be interpreted with caution.
The global maps now include neurological data demonstrating that Japan in the Asia Pacific, high income region (Map 2) has the highest proportion of tetraplegia in the world due to the combination of an ageing population (more low falls), possibly worsened by genetic factors.32, 69, 70 In contrast, Map 2 also demonstrates a high proportion of paraplegia secondary to high falls in Asia, South (Pakistan, Bangladesh and Nepal) as well as a component of low falls (Bangladesh).71, 72, 73
Violence-related TSCI occurs in regions of conflict or high availability of weapons (gunshot wounds and stabbings).7, 46, 74 The Maps reveal a band of violence through North and South America into Southern Africa and the Middle East. High rates of gunshot injuries are present in the USA and Brazil and the world’s highest proportion in the country of South Africa.46, 51, 74, 75 Greenland (Western Europe) also has a high proportion of violence (self-harm), causing TSCI with high rates of attempted suicide.14 High suicide rates seem to predominate in Scandinavian countries.13, 16, 31
Demographic and economic differences between developed and developing countries affect the incidence of TSCI from low and high falls. Low falls (1-metre or less or on the same level (slips and trips) in elderly (often resulting in tetraplegia) are on the increase in developed countries with ageing populations.76 Tetraplegic survival rates in developed countries with ageing populations may start to decrease as the proportion of older people sustaining tetraplegia from low falls increases relative to those with other causes of TSCI. In developing countries, low falls resulting in TSCI occur while carrying heavy loads on head in young people.73, 80 TSCI due to crush factors from collapse of ceiling in poorly regulated mining activities is common in many developing countries.79 Diving into water of unknown depths results in high proportions of tetraplegia in rivers and coastal regions.40, 77
There is a need for optimal retrieval services and acute SCI care within the first 72 h after TSCI and ideally direct transfer to specialised spinal treatment centres to reduce complications and optimise treatment and long-term outcomes.81 Delayed admissions of over 1000 TSCI patients admitted to specialist centres in Italy and the United Kingdom resulted in more complications (pressure sores, heterotopic ossifications and urinary complications) and longer lengths of stay.82, 83
Most clinicians are aware of the need to report their local statistics for TSCI incidence and prevalence. This is mandatory in many developed countries and in some centres accreditation is linked to effective epidemiological and clinical data management. Other countries may lack training, tools or financial resources to undertake this task. Failure to refer patients with TSCI to a specialised centre, or lack of resources in the specialised centres to accept all referrals, makes this task more difficult unless national or regional reporting is routinely occurring using internationally accepted data standards through an injury registry. The absence of national reporting, illustrated by the many Red Zone areas in the global maps, makes it difficult to determine valid population denominators and even small area variation, helpful in determining prevention strategies.
Data presented in this paper from regression modelling extrapolates global data within a region of Red Zone data to try and get an estimate consistent with expectations based on the known cases of TSCI and the population at risk. Improving the quality of local data through the use of the International Classification of External Causes of Injury (ICECI) will improve these estimates of TSCI. As our future TSCI data improves, the ISCoS readership would be better served by the analysis of aetiology-specific incidence rates rather than proportional rates in conjunction with more sophisticated modelling to better cope with data inadequacies (Fitzharris–this issue).68
General deployment of the ISCoS prevention module, incorporating the ICECI will allow more accurate reporting of incidence by aetiology. The prevention module (http://www.iscos.org.uk/page.php?content=20) provides a platform to spread adoption of the ISCoS core data set as this is an integrated part of the ISCoS Prevention Committee data-tool to facilitate international data standardisation.
Future reviews of the global mapping project will refine the regression techniques presented for incidence and expand to provide more focus on the area of prevalence, survival and life expectancy. The current prevention module and core data set will also be translated to other languages as international partnerships are established. The ASCoN software is currently in English and will be available in Vietnamese and other translations and posted on the ISCoS website: http://www.iscos.org.uk/page.php?content=20.
Conclusions
This paper shows a correlation linking poor data quality and poor survival rates post TSCI in WHO global regions. It outlines how mandatory reporting is part of standard practice in some developed countries and makes the point that the epidemiological data system developed by the ISCoS Prevention Committee can serve as a reporting platform when such systems are unavailable. Establishing this platform in areas of data deficit will facilitate epidemiological and clinical data standardisation globally.
To continue to improve TSCI epidemiological data, the interim measure of epidemiological extrapolation of incident and prevalence data has been attempted by our group as well as others.11 As an interim method, it makes poorer quality data easier to compare. It is possible to enhance the methodology by exploring the addition of other appropriate variables such as human development index, urbanisation, employment and income, which in combination with better baseline data will continue to provide further refinement of regional estimates. As we get better quality data, it will become possible to provide separate reporting to assist analysis of small area variations within countries. In time, this will allow local areas to understand likely causes of TSCI in their regions, develop models or programs to address and compare the effect of prevention strategies as well as epidemiological and societal trends. At a crude level, given the Red Zone (low) quality of the majority of the extrapolated data, it may also give an estimate of resource requirement and cost-savings for TSCI service provision and prevention initiatives.
Extrapolation is a technique of limited utility in of itself and requires accurate and standardised reporting of the numbers and causes of TSCI at a local level. When we are concerned enough to report on an injury statistic, we should be concerned enough to reduce it. ISCoS offers a method for this to be done.
DATA ARCHIVING
Data tables are available at http://www.iscos.org.uk/sci-global-mapping.
References
Fitzharris M, Cripps RA, Lee BB . Estimating the global burden of traumatic spinal cord injury. Spinal Cord 2011 (in press).
Cripps R, Lee B, Wing P, Weerts E, Mackay J, Brown D . A global map for traumatic spinal cord injury epidemiology: towards a living data repository for injury prevention. Spinal Cord 2011; 49: 493–501.
Wyndaele M, Wyndaele JJ . Incidence, prevalence and epidemiology of spinal cord injury: what learns a worldwide literature survey? Spinal Cord 2006; 44: 523–529.
Ackery A, Tator C, Krassioukov AA . Global perspective on spinal cord injury epidemiology. J Neurotrauma 2004; 21: 1355–1370.
Blumer CE, Quine S . Prevalence of spinal cord injury: an international comparison. Neuroepidemiology 1995; 14: 258–268.
Harvard University, Institute for Health Metrics and Evaluation at the University of Wasington, Johns Hopkins University, University of Queensland, World Health Organization (WHO). Global Burden of Disease Operations Manual, final draft. WHO. 2009.
National Spinal Cord Injury Statistical Center. Spinal cord injury. Facts and figures at a glance. J Spinal Cord Med 2005; 28: 379–380.
Jackson AB, Dijkers M, DeVivo MJ, Poczatek RBA . Demographic profile of new traumatic spinal cord injuries: change and stability over 30 years. Arch Phys Med Rehabil 2004; 85: 1740–1748.
Lasfargues JE, Custis D, Morrone F, Carswell J, Nguyen T . A model for estimating spinal cord injury prevalence in the United States. Paraplegia 1995; 33: 62–68.
Farry A, Baxter D . The incidence and prevalence of spinal cord injury in canada: overview and estimates based on current evidence. Rick Hansen Institute and Urban Futures Institute, Canada. 2010 pp 1–49.
Rick Hansen Spinal Cord Injury Registry.. Spinal Cord Injury Facts and Statistics. Vancouver, British Columbia, Canada. 2006 pp 1–11.
Cripps R . Spinal cord injury, Australia, 2006–07. In. Injury Research and Statistics Series Number 48. Cat. no. INJCAT 119. Adelaide, AIHW. 2008.
Biering-Sorensen F, Pedersen V, Clausen S . Epidemiology of Spinal Cord Lesions in Denmark. Paraplegia 1990; 28: 105–108.
Pedersen V, Muller PG, Biering-Sorensen F . Traumatic Spinal Cord Injuries in Greenland 1965–1986. Paraplegia 1989; 27: 345–349.
Knutsdottir S . Spinal cord injuries in Iceland 1973–1989. A follow up study. Paraplegia 1993; 31: 68–72.
Divanoglou A, Levi R . Incidence of traumatic spinal cord injury in Thessaloniki, Greece and Stockholm, Sweden: a prospective population-based study. Spinal Cord 2009; 47: 1–6.
O'Connor RJ, Murray PC . Review of spinal cord injuries in Ireland. Spinal Cord 2006; 44: 445–448.
Exner G, Meinecke FW . Trends in the treatment of patients with spinal cord lesions seen within a period of 20 years in German centers. Spinal Cord 1997; 35: 415–419.
Lee B, Cripps RA, Woodman RJ, Biering-Sørensen F, Wing P, Campbell R et al Development of an international spinal injury prevention module: application of the international classification of external cause of injury to spinal cord injury. Spinal Cord 2010; 48: 498–503.
Harvey C, Rothschild BB, Asmann AJ . Stripling T. New estimates of traumatic sci prevalence: a survey-based approach. Paraplegia 1990; 28: 537–544.
Kurtzke JF . Epidemiology of spinal cord injury. Exp Neurol 1975; 48 (Part 2): 163–236.
DeVivo MJ, Fine PR, Maetz HM, Stover SL . Prevalence of spinal cord injury: a reestimation employing life table techniques. Arch Neurol 1980; 37: 707–708.
Stover SL, Fine PR . The epidemiology and economics of spinal cord injury. Paraplegia 1987; 25: 225–228.
Dryden DM, Saunders LD, Rowe BH, May LA, Yiannakoulias N, Svenson LW et al The epidemiology of traumatic spinal cord injury in Alberta, Canada. Can J Neurol Sci 2003; 30: 113–121.
Noonan V, Fingas M, Farry A, Baxter D, Singh A, Fehlings MG et al The incidence and prevalence of spinal cord injury in Canada: A national perspective. Neuroepidemiology 2012; 38: 219–226.
Razdan S, Kaul RL, Motta A, Kaul S, Bhatt RK . Prevalence and pattern of major neurological disorders in rural Kashmir (India) in 1986. Neuroepidemiology 1994; 13: 113–119.
Weerts E . Final reporting of project outcomes Spinal Cord Injury care and Orthopedic workshop, pp 1–3 ( Hanoi. 2009.
Walsh J . Costs of spinal cord injury in Australia. Paraplegia 1988; 26: 380–388.
O'Connor PJ . Prevalence of spinal cord injury in Australia. Spinal Cord 2005; 43: 42–46.
Yeo JD, Walsh J, Rutkowski SB, Soden RJ, Craven ML, Middleton JW . Mortality following spinal cord injury. Spinal Cord 1998; 36: 329–336.
Dahlberg A, Kotila M, Leppanen P, Kautiainen H, Alaranta H . Prevalence of spinal cord injury in Helsinki. Spinal Cord 2005; 43: 47–50.
United Nations: Department of Economic and Social Affairs/Population Division. World Population Ageing 2009. In. New York: United Nations. 2009.
World Health Organization. The global burden of disease: 2004 update. Geneva, Switzerland: World Health Organization. 2008.
Li J, Liu G, Zheng Y, Hao C, Zhang Y, Wei B et al The epidemiological survey of acute traumatic spinal cord injury (ATSCI) of 2002 in Beijing municipality. Spinal Cord 2011; 49: 777–782.
Ning G-Z, Yu T-Q, Feng S-Q, Zhou X-H, Ban D-X, Liu Y et al Epidemiology of traumatic spinal cord injury in Tianjin, China. Spinal Cord 2011; 49: 386–390.
Chen HY, Chen SS, Chiu WT, Lee LS, Hung CI, Hung CL et al A nationwide epidemiological study of spinal cord injury in geriatric patients in Taiwan. Neuroepidemiology 1997; 16: 241–247.
Kovindha A . A retrospective study of spinal cord injuries at Maharaj Nakorn Chiang Mai Hospital, during 1985–1991. Chiang Mai Med Bull 1993; 32: 85–92.
Pajareya K . Traumatic spinal cord injuries in Thailand; an epidemiologic study in Siriraj Hospital, 1989–1994. Spinal Cord 1996; 34: 608–610.
Dixon GS, Danesh JN, Caradoc-Davies TH . Epidemiology of spinal cord injury in New Zealand. Neuroepidemiology 1993; 12: 88–95.
Norton L Spinal cord injury, Australia 2007–08. Injury research and statistics series no. 52. Cat. no. INJCAT 128 Canberra: AIHW. 2010.
Sabre L, Linnamagi U, Derrik G, Rekand T, Asser T, Korv J . Traumatic spinal cord injuries in Estonia from 2003 to 2007. ISCoS. University of Tartu: Florence. 2009.
Silberstein B, Rabinovich S . Epidemiology of spinal cord injuries in Novosibirsk, Russia. Paraplegia 1995; 33: 322–325.
Kondakov EN, Simonova IA, Poliakov IV . The epidemiology of injuries to the spine and spinal cord in Saint Petersburg. Zh Vopr Neirokhir Im N N Burdenko 2002; 2: 50–53.
Van den Berg ME, Castellote JM, Mahillo-Fernandez I, De Pedro-Cuesta J . Incidence of traumatic spinal cord injury in Aragon, Spain (1972–2008). J Neurotrauma 2011; 28: 469–477.
Karacan I, Koyuncu H, Pekel O, Sumbuloglu G, Kirnap M, Dursun H et al Traumatic spinal cord injuries in Turkey: a nation-wide epidemiological study. Spinal Cord 2000; 38: 697–701.
Otom AS, Doughan AM, Kawar JS, Hattar EZ . Traumatic spinal cord injuries in Jordan–an epidemiological study. Spinal Cord 1997; 35: 253–255.
Alshahri S, Cripps RA, Lee BB . Traumatic spinal cord injury in Saudi Arabia: An epidemiological estimate from Riyadh. Spinal Cord 2012; 50: 882–884.
Quinones M, Nassal M, Al Bader KI, Al Muraikhi AE, Al Kahlout SR . Traumatic spinal cord in Qatar: An epidemiological study. Middle East Journal of Emergency Medicine 2002; 2: 1–5.
Chabok S, Safaee M, Alizadeh A, Dafchahi M, Taghinnejadi O, Koochakinejad L . Epidemiology of traumatic spinal injury: A descriptive study. Acta Med Iran 2010; 48: 308–311.
Ditunno JF . Formal CS. Chronic spinal cord injury. New Engl J Med 1994; 330: 550–556.
National Spinal Cord Injury Statistical Centre Birmingham Alabama. Spinal Cord Injury Facts and Figures at a Glance. Alabama, USA. 2008.
Burney RE, Maio RF, Maynard F, Karunas RB . Incidence, characteristics, and outcome of spinal cord injury at trauma ceners in North America. Arch Surg 1992; 128: 596–599.
Goebert DA, Ng MY, Varney JM, Sheetz DA . Traumatic spinal cord injury in Hawaii. Hawaii Med J 1991; 50: 44–50.
Griffin MR, O'Fallon WM, Opitz JL, Kurland LT . Mortality, survival and prevalence: traumatic spinal cord injury in Olmsted county, Minnesota, 1935–1981. J Chron Dis 1985; 38: 643–653.
Kraus JF, Franti CE, Riggins RS, Richards D, Borhani NO . Incidence of traumatic spinal cord lesions. J Chron Dis 1975; 28: 471–492.
Price C, Makintubee S, Herndon W, Istre GR . Epidemiology of traumatic spinal cord injury and acute hospitalization and rehabilitation charges for spinal cord injuries in Oklahhoma, 1988–1990. Am J Epidemiol 1994; 139: 37–47.
Acton PA, Farley T, Freni LW, Ilegbodu VA, Sniezek JE, Wohlleb JC . Traumatic spinal cord injury in Arkansas, 1980–1989. Arch Phys Med Rehabil 1993; 74: 1035–1040.
Thurman DJ, Burnett CL, Jeppson L, Beaudoin DE, Sniezek JE . Surveillance of spinal cord injuries in Utah, USA. Paraplegia 1994; 32: 665–669.
Calancie B, Molano MR, Broton JG . Epidemiology and demography of acute spinal cord injury in a large urban setting. J Spinal Cord Med 2005; 28: 92–96.
Nwadinigwe CU, Iloabuchi TC, Nwabude IA . Traumatic spinal cord injuries (SCI): A study of 104 cases. Niger J Med 2004; 13: 161–165.
Levy LF, Makarawo S, Madzivire D, Bhebhe E, Verbeek N, Parry O . Problems, struggles and some success with spinal cord injury in Zimbabwe. Spinal Cord 1998; 36: 213–218.
Key AG, Retief PjM . Spinal cord injuries: an analysis of 300 new lesions. Paraplegia, Tel-Aviv: Paraplegia 1968, 243–249.
Krause JS, Zhai Y, Saunders LL, Carter RE . Risk of mortality after spinal cord injury: An 8-year prospective study. Arc Phys Med Rehabil 2009; 90: 1708–1715.
Hu R, Mustard CA, Burns C . Epidemiology of incident spinal fracture in a complete population. Spine 1996; 21: 492–499.
O'Connor PJ . Survival after spinal cord injury in Australia. Arch Phys Med Rehabil 2005; 86: 37–47.
Middleton JW, Dayton A, Walsh J, Soden RJ, Leong G, Duong S . Life expectancy after spinal cord injury: a fifty-year study. Spinal Cord 2012; 50: 803–811.
World Health Organization In:. World report on road traffic injury prevention Peden M, Scurfield R, Sleet D, Mohan D, Hyder AA, Jarawan E, Mathers C (eds) Geneva. 2004.
World Health Organization. Global status report on road safety: time for action. Geneva: World Health Organization. 2009.
Shingu H, Ohama M, Ikata T, Katoh S, Akatsu T . A nationwide epidemiological survey of spinal cord injuries in Japan from January 1990 to December 1992. Paraplegia 1995; 33: 183–188.
Inamasu J, Guiot B, Sachs D . Ossification of the posterior longitudinal ligament: an update on its biology, epidemiology, and natural history. Neurosurgery 2006; 58: 1027–1039.
Raja IA, Viohra AH, Ahmed M . Neurotrauma in Pakistan. World J Surgery 2001; 25: 1230–1237.
Hoque MF, Grangeon C, Reed K . Spinal cord lesions in Bangladesh: an epidemiological study 1994–1995. Spinal Cord 1999; 37: 858–861.
Mukhida K, Sharma MR, Shilpakar SK . Pediatric neurotrauma in Kathmandu, Nepal: implications for injury management and control. Childs Nerv Syst 2006; 22: 352–362.
Hart C, Williams E . Epidemiologyof spinal cord injuries: a reflection of changes in South African society. Paraplegia 1994; 32: 709–714.
Barros F, Taricco MA, Oliveira RP, Greve JM, Santos LC, Napoli MM . Epidemiological study of patients with spinal cord injuries. Rev hosp Fac Med S Paulo 1990; 45: 123–126.
Ide M, Ogata H, Tokuhiro A, Takechi H . Spinal cord injuries in okayama prefecture: an epidemiological study '88-'89. J UOEH 1993; 15: 209–215.
Maharaj JC . Epidemiology of spinal cord paralysis in Fiji: 1985–1994. Spinal Cord 1996; 34: 549–559.
Masood Z, Wardug GM, Ashraf J . Spinal injuries: experience of a local neurosurgical centre. Pak J Med Sci 2008; 24: 368–371.
Wang D . The Prevention of Acute Traumatic Spinal Cord Injury (ATSCI) in China. ISCoS Workshop 111, 28th October: Delhi, India. 2010.
Bajracharya S, Singh M, Singh GK, Shrestha BP . Clinico-epidemiological study of spinal injuries in a predominantly rural population of eastern Nepal: a 10 years’ analysis. Indian J Orthop 2007; 41: 286–289.
Schiller MD, Mobbs RJ, Lee BB, Stanford RE, Marial O . Acute care for spinal cord injured patients at spinal injury units: the influence of early and direct admission on complications and length of stay. ANZCoS, Brisbane, Australia 2011.
Aito S, GruppoItaliano Studio EpidemiologicoMielolesioni GISEM Group. Complications during the acute phase of traumatic spinal cord lesions. Spinal Cord 2003; 41: 629–635.
Amin A, Bernard J, Nadarajah R, Davies N, Gow F, Tucker S . Spinal injuries admitted to a specialist centre over a 5-year period: a study to evaluate delayed admission. Spinal Cord 2005; 43: 434–437.
Acknowledgements
The members of the ISCoS prevention committee and the ISCoS membership for their continuing enthusiasm. Dr Lee and the Myriad Mapping were funded by the Prince of Wales Hospital Training, Education and Study Leave fund (New South Wales Department of Health, Australia). Many thanks to Hanan Youssef for helping us with reference coordination. In press data for this paper was made available by Vanessa Noonan, James Middleton, Anna Dayton and John Walsh.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest
Additional information
Supplementary Information accompanies this paper on the Spinal Cord website
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Lee, B., Cripps, R., Fitzharris, M. et al. The global map for traumatic spinal cord injury epidemiology: update 2011, global incidence rate. Spinal Cord 52, 110–116 (2014). https://doi.org/10.1038/sc.2012.158
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2012.158
Keywords
This article is cited by
-
The impact of COVID-19 and associated lockdowns on traumatic spinal cord injury incidence: a population based study
Spinal Cord (2024)
-
Characteristics of corticomuscular coupling during wheelchair Tai Chi in patients with spinal cord injury
Journal of NeuroEngineering and Rehabilitation (2023)
-
Spinal cord injury: molecular mechanisms and therapeutic interventions
Signal Transduction and Targeted Therapy (2023)
-
The prevalence and profile of spinal cord injury in public healthcare rehabilitation units in Gauteng, South Africa
Spinal Cord Series and Cases (2023)
-
Expression of transforming growth factor-β1 and autophagy markers in the bladder of rats with neurogenic lower urinary tract injury
Spinal Cord (2023)