Abstract
Study design:
Retrospective study based on a reference paper. Neurological outcome in patients who were managed surgically with closed traumatic cervical spine injury was evaluated using the ASIA motor scoring system and Frankel grading.
Objectives:
To assess the accuracy of motor charting and Frankel grading as tools to evaluate neurological outcome in closed traumatic cervical spine injury, and also to evaluate how the surgically treated patients fared in their neurological recovery by measurement tools as in the reference paper.
Setting:
National Spinal Injuries Centre, Stoke Mandeville Hospital, Aylesbury, UK.
Method:
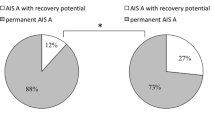
Fifty-seven patients were admitted within 2 days of the injury with closed traumatic cervical spine injuries (1997–2004). Thirty-seven (65%) met the inclusion criteria as per the referenced paper, that is, were treated surgically, were Frankel grade B and above and had at least 12 months follow up. The remaining 20 patients were not included as they did not meet the inclusion criteria. The breakdown of the 20 patients is given in Table 1. The mean recovery percentage (MRP) and mean deficit percentage (MDP) were calculated as per the referenced paper.
Results:
An evaluation of 37 patients surgically treated, who had follow up of at least 12 months, showed that preservation of pin prick below the level of lesion, and preservation of anal tone and perianal sensation were good prognostic indicators. There was no correlation between degree of encroachment of canal or the degree of kyphosis to MDP or MRP. The mean time from injury to mobilization was 7.6 days in 25 out of 37 patients. Twelve of the 37 patients had prolonged immobilization because of ITU stay or because they were initially treated conservatively. Three out of the 37 patients developed DVT/PE. Mean hospital stay was 6.4 months.
Conclusion:
The neurological outcome in surgically treated patients is comparable to the conservatively treated patients. The Frankel grading and ASIA motor charting combined is a powerful tool in assessing the neurological outcome in closed traumatic cervical spinal injured patients. Until now there has been no evidence to suggest that the obvious advantages of surgical management of closed cervical spine injuries (better alignment, easier manual handling and early mobilization) is traded for poorer neurological outcome.
Similar content being viewed by others
Introduction
There is a great deal of controversy in the management of traumatic closed cervical spine injuries.1 There is also a lack of efficient objective tools to measure the neurological outcome. Original Frankel grading and ASIA motor scoring have been used as tools to measure neurological outcome in conservatively treated cervical spine injuries.2, 3 This study looks into the neurological outcome in surgically treated patients with closed traumatic cervical spinal cord injury (SCI) following the same study design as in the reference paper.2 Stabilization within 72 h of injury in cervical spine injured patients is sufficient to improve neurological outcome.4 This is debatable, although in animal models there has been neurological improvement shown with early decompression.5, 6
Various investigators have also reported spontaneous neurological recovery in the conservatively managed group.7, 8, 9 Neurological deterioration following spinal surgery was observed in the past. This was because decompressive laminectomy was being performed without any stabilization of the cervical spine. The advances in spinal stabilization in the last two decades have provided better stability of the bony architecture, hence preventing further instability.10, 11 There is also controversy about early mobilization of the cervical spine injured group. Early mobilization in this group was thought to have worse outcomes on the neurology. In our study we did not find any such correlation.
Materials and methods
This was a retrospective study (1996–2004). Patients meeting the inclusion criteria were identified by looking at the admission list for the year. The individual case notes were scrutinized to get the data needed for the study. The inclusion criteria were as follows: traumatic closed cervical spine injury; patients admitted within 2 days of injury, treated surgically, Frankel B and above on admission; patients who had follow up of 12 months or longer. Following the inclusion criteria, 57 consecutive patients were admitted within 2 days of their injury, 37 (65%) of them were treated surgically, Frankel B and above and had at least 12 months follow up. The remaining 20 patients were excluded as they did not meet the inclusion criteria. Some of these patients were treated conservatively, some were Frankel A on admission although were treated surgically, and hence excluded. Some had no neurological deficit, hence excluded. The breakdown of these 20 patients is given in Table 1. We excluded double injuries of the spinal axis. The neurological examination was done as per the referenced papers protocol. Frankel classification and ASIA motor score were recorded from the notes in each patient. The last normal segment was defined as the distal segment with motor power greater than or equal to 3, provided all muscles supplied by the proximal myotome above had power grade 4 or 5.


The motor score was calculated by adding the strength of the five key muscles for upper limbs and lower limbs as per ASIA charting. The protocol for surgical management was as follows: patients with facet dislocations underwent attempted closed reduction. If this failed, we proceeded to posterior open reduction and anterior fixation at the same sitting. Patients who solely had anterior fixation were mobilized with a Philadelphia collar for 4 weeks. Both anterior and posterior fixations were mobilized without any orthosis.
Results
Men/women ratio of 43:14 (75.4% men and 24.6% women), mean age was 40.8 years (18–75), 18 patients were admitted on the day of injury, 20 patients were admitted one day after injury and 19 patients were admitted within 2 days of injury.
Causes of injury in the surgically treated patients were as follows: 13 road traffic accidents, 15 falls, 4 diving injuries, 2 rugby injuries and 2 assaults.
Timing of operation post-injury was as follows: 3 were operated on the same day, 10 on the first day, 4 on the second day, 5 on the third day, 9 were operated between 3–7 days and the remaining 6 were operated more than a week after the injury. There was no correlation between the timing of the operation and MRP (mean recovery percentage).
Level of skeletal injury is shown in Table 2.
Types of cervical injuries with MRP and MDP (mean deficit percentage) are shown in Table 3
The relation between MDP and MRP in all Frankel C patients is shown in Figure 1.
The P-value is >0.05.
No statistical significance was seen between the MDP and degree of encroachment of the canal.
AP Canal Diameter did not have any correlation with MRP.
Degree of kyphosis did not show any correlation to MRP.
Comparison of motor scores from admission to follow up for Frankel B patients (n=25) is shown in Figure 2.
Comparison of motor scores from admission to follow up for Frankel C patients (n=7) is shown in Figure 3.
Comparison of motor scores from admission to follow up for Frankel D patients (n=5) is shown in Figure 4.
Frankel grade at follow-up plotted against Frankel grade on admission is shown in Table 4.
Two patients deteriorated in their motor scores post-operatively. The first was C5B on admission with motor score of 14; post-operatively she had a motor score of 10, her motor score at the 12-month follow-up was 20. The second patient was C6C on admission with a motor score of 24; post-operatively his motor score was 20, and at the 12-month follow-up his motor score had gone up to 50.
Table 5 summarizes the patients who spent time in ITU. The data cannot prove or disprove the advantages or disadvantages of surgery in a cervical spine injured patient during the ITU phase because of its low number. However, there is enough evidence in the literature to suggest that patients who are initially admitted to ITU, intubated and ventilated, can be nursed without any restrictions to the neck once the cervical spine is stabilized surgically. This allows for easier nursing care and better management of the respiratory system, helping to wean these patients off the ventilator earlier.12, 13 Its agreeable that the comparison of patients treated conservatively requiring ITU treatment, with the group of patients who did not require ventilation before, but after surgery is a valuable tool to compare the influence of surgery in cervical spine injured patients. Unfortunately, the low numbers (one and three) of patients in the respective groups does not allow any comparison to be drawn. The reliability of neurological examination in the ventilated group is always questionable. In our group the patients who were sedated and ventilated on arrival were re-examined by the spinal team once they were awake. We realize that there is a lack of proper neurological examination documentation from the referring district general hospitals.
Controversies exist about the usage of methyprednisilone (MP) in acute SCI.14 Fifteen out of the 37 patients received MP. The MRP in this group was higher but not statistically significant. The institution the author belongs to discourages the use of MP in acute SCI. High dose MP cannot be justified as a standard treatment in acute SCI with current medical practice.15 High dose MP was being used in the earlier period of the study and some patients were started on it at the referring hospital, hence 15 patients received the drug.
The mean time between injury and mobilization was 7.6 days (2–16 days) in 25 out of 37 patients who were surgically treated. Twelve patients were excluded, as three were initially treated conservatively, and nine were admitted to ITU. The breakdown of the nine patients and three conservatively treated patients requiring ITU is given in Table 5. These nine patients were admitted to ITU in the first instance because of rising PCO2 and reduced vital capacity secondary to cervical SCI. Surgical intervention took place after they were intubated and ventilated.
The average hospital stay was 6.4 months or 192 days (37 patients), range (14–368 day). For Frankel B: 7.3 months 219 days (range 54–430), Frankel C: 5.2 months 156 days (range 38–282) and Frankel D: 2.1 months 63 days (range 29–85). The term ‘delayed discharge’ was coined in 2002 to mark patients who had achieved all the therapy goals, beyond that point they would receive maintenance physiotherapy and occupational therapy input. This group was staying beyond their agreed discharge dates on goal planning secondary to housing issues. Since 2002 there were 17 (out of 37) patients who met the inclusion criteria of the study. The average time from admission to completion of therapy goals in Frankel B (10 patients) was 172 days (range 35–230), average time from completion of therapy goals to actual discharge in Frankel B was 63 days (range 24–129). In Frankel C (4 patients) it was 93.5 days (range 44–154), overstay period was 47.25 days (range 23–80) and in Frankel D (3 patients) the average was 46 (range 18–96). There was no overstaying in Frankel D in the three patients. Only three of the nine patients treated conservatively fell in this group, that is, they were injured after 2002. Two Frankel C patients with an average rehabilitation time of 150 days (range 122–178) had an overstay period of 70 days (range 56–84). One Frankel B patient treated conservatively had an average stay of 190 days with no overstay. The numbers being small, it is difficult to draw comparisons between the surgically treated and conservatively treated group in their hospital stay. The social factors (mainly housing or lack of interim placement) were the key factors preventing patients going back into the community. The above data shows clearly that there is an overstay, with hospital bed days secondary to the social issues. Hence, actual rehabilitation time from admission to discharge when therapy goals are complete is much less compared to total hospital stay.
There is evidence in the literature that surgical intervention has helped in marginally cutting down the total hospital stay.1, 13 In our study, there was no significant statistical difference in the hospital stay when compared to the referenced paper.2
Out of 37 patients, 2 patients of Frankel B grading had deep vein thrombosis; both had prolonged immobilization because of ITU stay.
One patient of Frankel C grading had deep vein thrombosis and developed pulmonary embolus, he was initially conservatively treated. The protocol for DVT prophylaxis for the period of the study was TED stockings and low molecular weight heparin (Clexane) 40 mg s.c. for 3 months after injury in all patients. This protocol has been revised secondary to internal audit, where there was DVT/PE seen at an increasing rate in spite of prophylaxis. The current protocol is to give low molecular weight heparin (Fragmin), 125 mg kg−1 body weight as prophylaxis for 3 months after injury, along with TED stockings. The switch from Clexane to Fragmin is in line with the hospital protocol for anticoagulation, rather than any scientific evidence that one is better than the other. Low molecular weight heparin, when compared to unfractionated heparin, has better efficacy in reducing the deep vein thrombosis.16
Discussion
Surgical management is synonymous with early mobilization. There was no statistical significance in the duration of hospital stay, nor the neurological outcome compared to the reference paper.2 There was no statistical significance in the motor recovery rate and initial canal diameter, or degree of kyphosis at the time of admission and motor recovery rate, which is similar to the finding of the reference paper.1, 2
This was a retrospective study, involving a small number of patients, hence the question of statistical significance. Further studies (prospective and multi-centric) are overdue. The only prospective randomized trial to determine whether functional outcome is improved in traumatic cervical spinal cord injured patients is Vaccaro et al.17 The results of this study revealed no significant benefit if decompression and fixation is performed less than 72 h after injury (mean 1.8 days), as opposed to waiting longer than 5 days (mean 16.8 days).8 We found that Frankel grading in combination with ASIA motor scoring is a powerful tool for measuring neurological outcome. Both conservative and surgical management modalities should be discussed with patients before obtaining informed consent. In line with newer developments in stem cell research and olfactory ensheathing cell transplant,18, 19 the importance of well preserved cord, without any encroachment of the canal from bony fragments and in good alignment, may be the key in the success of any future treatment options to come. Resorption and remodeling of the canal do, however, occur naturally and without surgery.20 Until now, there is no evidence to suggest that the obvious advantages of surgical management in cervical SCI (better alignment, easier manual handling and early mobilization) are traded for poorer neurological outcome. The clinical value and cost benefits of better surgical alignment require further well-designed studies. It could also be argued that the objective of management should be patient centered and not centered on helping inexperienced nurses. Considering well-experienced nurses find it equally easy to nurse patients who undergo surgical and conservative management, surgery to help nursing should not be a key objective. The value of early mobilization also requires prospective, well-designed studies to evaluate any temporary neurological changes that occur during the early stages of mobilization.
References
Donovan WH, Cifu DX, Schotte DE . Neurological and skeletal outcomes in 113 patients with closed injuries to the cervical spinal cord. Paraplegia 1992; 30: 533–542.
Katoh S, El-Masry WS, Jaffray D, McCall IW, Eisenstein SM, Pringle RG et al. Neurological outcome in conservatively treated patients with incomplete closed traumatic cervical spinal cord injuries. Spine 1996; 21: 2345–2351.
Katoh S, El-Masry WS . Motor recovery of patients presenting with motor paralysis and sensory sparing following cervical spinal cord injury. Paraplegia 1995; 33: 506–509.
Mirza SK, Krengel III WF, Chapman JR, Anderson PA, Bailey JC, Grady MS et al. Early versus delayed surgery for acute cervical spinal cord injury. Clin Orthop Relat Res 1999; 359: 104–114.
Carlson GD, Gorden CD, Oliff HS, Pillai JJ, LaManna JC . Sustained spinal cord compression. Part 1: time-dependent effect on long-term pathophysiology. J Bone Joint Surg Am 2003; 85: 86–94.
Dimar II JR, Glassman SD, Raque GH, Zhang YP, Shields CB . The influence of spinal canal narrowing and timing of decompression on neurological recovery after spinal cord contusion in a rat model. Spine 1999; 24: 1623–1633.
Bedbrook GM . Spinal injuries with tetraplegia and paraplegia. J Bone Joint Surg Br 1979; 61: 267–284.
Bedbrook GM, Sakae T . A review of cervical spine injuries with neurological dysfunction. Paraplegia 1982; 20: 321–333.
Wilmot CB, Hall KM . Evaluation of the acute management of tetraplegia: conservative versus surgical management. Paraplegia 1986; 24: 148–153.
Botel U, Glaser E, Niedggen A . The surgical treatment of acute spinal paralysed patients. Spinal Cord 1997; 35: 420–428.
Fehling MG, Cooper PR, Errico TJ . Posterior plates in the management of cervical instability: long term results in 44 patients. J Neurosurg 1994; 81: 341–349.
Kerwin AJ, Frykberg ER, Schinco MA, Griffen MM, Murphy T, Tepas JJ . The effect of early spine fixation on non neurologic outcome. J Trauma 2005; 58: 15–21.
McKinley W, Meade MA, Kirshblum S, Barnard B . Outcomes of early surgical management versus late or no surgical intervention after acute spinal cord injury. Arch Phys Med Rehabil 2004; 85: 1818–1825.
Bracken MB, Holford TR . Effects of timing of Methylprednisolone or Naloxone administration on recovery of segmental and long tract neurological function in NASCIS 2. J Neurosurg 1993; 79: 500–507.
Short D . Is the role of steroids in acute spinal cord injury now resolved? Curr opin Neurol 2001; 14: 759–763.
Green D, Sullivan S, Simpson J, Soltysik RC, Yarnold PR . Evolving risk for thromboembolism in spinal cord injury (SPIRATE Study). Am J Phys Med Rehabil 2005; 84: 420–422.
Vaccaro AR, Daugherty RJ, Sheehan TP . Neurological outcome of early versus late surgery for cervical spinal cord injury. Semin Spine Surg 2002; 14: 174–181.
Lu J, Ashwell K . Olfactory ensheathing cells. Spine 2002; 27: 887–892.
Lima C, Pratas-Vital J, Escada P, Hasse-Ferreira A, Capucho C, Peduzzi JD . Olfactory mucosa autografts in human spinal cord injury: a pilot clinical study. Spinal Cord 2006; 29: 191–203; discussion 204-6.
Fidler MW . Remodelling of the spinal canal after burst fracture. JBJS 1988; 70b: 730–732.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Singhal, B., Mohammed, A., Samuel, J. et al. Neurological outcome in surgically treated patients with incomplete closed traumatic cervical spinal cord injury. Spinal Cord 46, 603–607 (2008). https://doi.org/10.1038/sc.2008.29
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2008.29