Abstract
Pathological principles governing early management of spinal cord trauma are:
1. The anatomical features of capacity, blood supply, and spinal cord structure.
2. The mechanisms by which the trauma is caused: flexion, extension and rotation, together with crushing, stretching and concussion.
3. The neural pathological pictures which emerge
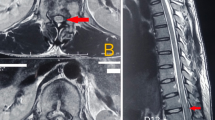
(i) Haematomyelia of the cord, with many manifestations caused by direct compression and direct interference with blood supply.
(ii) Gross crushing of the cord.
(iii) Subarachnoid and extra-dural haemorrhage.
(iv) Longitudinal manifestations of stretching and colliquative necrosis.
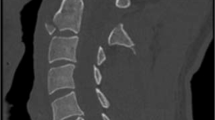
4. The bony patterns:
(i) The importance of the integrity of the neural canal after conservative management.
(ii) The absence of continuing bony compression.
In the later stages the final patterns that emerge are:
(i) Gross crushing.
(ii) Cysts.
(iii) Peri-neural and peri-dural fibrosis.
Applying these pathological principles, the author believes that a rational method of conservative treatment is, under most circumstances, the only method of management to be considered and explains the almost universal rejection of operative interference, since such interference can do little to affect the pathological state which has existed since the time of injury. Clinico-pathological facts which emerge are:
(a) That movement of the fracture site is minimal with proper nursing.
(b) Only a small percentage (7 per cent.) of a potentially unstable group of fractures in the cervical spine prove to be so after adequate management.
(c) Non-union is a rarity in lumbo-dorsal fractures and stability occurs early after the time of injury.
Similar content being viewed by others
Article PDF
References
Barnes, R (1948), J. Bone & Jt Surg. 30B, 234.
Beatson, T R (1963). J. Bone & Jt Surg. 45B, 21.
Bedbrook, G M (1963). Paraplegia, 1, 215.
Durbin, F C (1957). J. Bone & Jt Surg. 39B, 23.
Freeman, L W & Russell, J R (1955). J. Neurosurg. 12, 584.
Gillilan, L A, Crosby, E, Humphrey, T & Laver, E (1962). Correlative Anatomy of the Nervous System, Chap. 9.
Holdsworth, F (1963). J. Bone & Jt Surg. 45B, 6.
Hughes, J T (1964). Paraplegia, 2, 2.
Jefferson, G (1928). Proc. R. Soc. Med. 21, 625.
Nicol, E A (1949). J. Bone & Jt Surg. 31B, 376.
Scarff, J E (Revised 1960). In: Injuries of the Brain and Spinal Cord and their Coverings. Edit. S. Brock, 4th ed., p. 530. London: Cassell.
Schneider, R C, Cherry, G & Pantek, H (1954). J. Neurosurg. 11, 546.
Schneider, R C, Thompson, J M & Bebin, J T (1958). J. Neurol. Psychiat. 21, 216.
Windle, W F (1955). Regeneration in the Central Nervous System, p. 241. Springfield, Ill: C. C. Thomas.
Wolman, L (1964). Paraplegia, 1, 233.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bedbrook, G. Pathological principles in the management of spinal cord trauma. Spinal Cord 4, 43–56 (1966). https://doi.org/10.1038/sc.1966.5
Issue Date:
DOI: https://doi.org/10.1038/sc.1966.5