Abstract
School-aged children and adolescents have complex interactions with their food environments—the point of engagement of individuals with the food system—and are influenced by a diversity of individual, household and organizational factors. Although a wide range of methods have been proposed to define, monitor and evaluate food environments, few are tailored to school-aged children and adolescents. Here, we interrogate published literature on food metrics and methodologies for the characterization of food environments for school-aged children and adolescents living in low- and middle-income counties. We identify key priority actions and potential indicators for better monitoring and evaluation to galvanize policymaking to improve the healthiness of these interactions, which are so crucial to future adult well-being.
Similar content being viewed by others
Main
Prior to the COVID-19 pandemic, globally one in three children under five years experienced poor growth and development due to multiple forms of malnutrition, including stunting (144 million), wasting (47 million) and overweight (38.3 million), and at least 340 million children suffered from ‘hidden hunger’ and micronutrient deficiencies1,2,3,4. Over the past two decades, overweight and obesity have become more prevalent in children and adolescents, increasing the risk of non-communicable diseases (NCDs) in adulthood1,3. The persistence of food insecurity and malnutrition worldwide is in part attributed to dramatic changes over the past 50 years within global food systems, and subsequently, food environments—the spaces within which individuals interact to procure and consume food5,6,7. The aim of this Perspective is to identify priority actions and potential indicators for researchers and policymakers to monitor and evaluate food environments specific to school-aged children and adolescents in low- and middle-income countries (LMICs; Box 1).
Food environments and children and adolescents
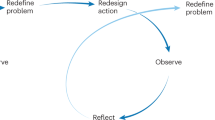
Several frameworks and models have been proposed to conceptualize this interaction and to capture its complexity and diversity, but they are rarely tailored to include or consider children and adolescents8,9,10,11,12,13,14. In 2019, the United Nations Children’s Emergency Fund (UNICEF) and the Global Alliance for Improved Nutrition adapted the High Level Panel of Experts on Food Security and Nutrition food system framework9 and food environment framework11, and introduced the Innocenti Framework on Food Systems for Children and Adolescents (Fig. 1)15,16.
The Innocenti Framework illustrates the influence of food system drivers (structural factors including demographic change, political and economic environment, technological advances, natural resource management and social and cultural norms), determinants (processes and conditions including food supply chains and food environments), influencers (individual factors including behaviours) and interactions (dynamic feedback loops) on the diets of children and adolescents. Figure reproduced with permission from ref. 16.
The Innocenti Framework conceptualizes and proposes the need to shape food systems as they relate specifically to children, adolescents and their caregivers. The framework depicts the dependency of agents, drivers and interactions within the food system that strongly influence and dictate how food moves from production to consumption, and how people interact with their surroundings to procure, prepare and consume food (external and personal food environments)14,15,16. These external (for example, community, retail and schools) and personal (for example, individual, family and household) food environments are the two main points of interaction with the food system for children and adolescents9,11. This framework also considers agency and one’s capacity to make food choices, which may depend on age, autonomy and opportunities, and broader social influencers, such as power dynamics, gender norms, wealth gaps and governance structures17,18,19.
An important caveat of this framework, however, is that food environments and their interactions are not static and uniform. Food environments, and more broadly the food systems and supply chains with which they are associated, are diverse and vary substantially in their typology (wild, cultivated, informal and formal)9,20,21, often with multiple typologies coexisting within the same country or region (for example, in the island countries of the Caribbean22) or differing environments (for example, urban, peri-urban or rural), which may substantially affect local actions to improve food environments3. This variability is more evident in LMICs where a large proportion of food is produced and sold through the informal sector9. Moreover, a lack of standardized metrics for food environments leads to unique challenges for assessment. For these reasons, the need to develop specific measures and indicators to assess food environments in the context of school-aged children and adolescents is critical for policy and programmatic responses to improve them11,23,24.
Evidence from LMICs on food environments for children and adolescents
So far, the majority of food environment research in school-aged children and adolescents has been conducted in high-income countries11,23,24,25,26, while most studies from LMICs have been conducted in upper-middle-income countries such as Brazil27,28,29,30, Chile31,32, China33, Guatemala34,35, Indonesia36, Mexico37,38 and South Africa39,40. Very few studies are from lower-middle-41,42,43,44,45,46 and low-income countries3,23,24. The limited evidence on children and adolescents may be owing to a lack of financial and human resources. Most studies applied an observational design11,23,25,47,48, with a limited number of intervention studies disaggregating data to isolate the effects of food environments on specific age groups47,49. Most research targeting children and adolescents in LMICs is conducted within the school environment;23,50,51 however, these studies do not account for the time spent outside school, and may miss a substantial proportion of those who do not or cannot attend school52. Furthermore, current research does not account for diverse community settings that may be important in LMICs, such as refugee settlements and urban slums. These unique settings may present different challenges in terms of food procurement and consumption, especially for migrant and internally displaced child and adolescent populations4. With regards to outcome indicators, most research has focused on anthropometric outcomes such as body mass index and weight status in response to the rising burden of obesity and overweight, and diet-related NCDs in this population3,11,23,50,53. Research efforts should consider micronutrient deficiencies, as these may coexist with other forms of malnutrition in the same household and community, and even within the same individual across their life cycle23,54.
Research limitations and recommendations
Based on this evidence, current designs, tools and indicators do not provide a complete picture of the food environment. Alternative study designs should be pursued to assess food environments that generate actionable results and support plausible causal inference by capturing repeated measures such as natural experiments, interrupted time series and longitudinal studies11,23,25,47,48,55. Qualitative methods, including ethnographic studies (for example, photovoice and intergenerational interviewing), which remain underutilized in this field, may provide additional insights into children’s, adolescents’ and their caregivers’ lived experiences of and perspectives about the food environment. This includes their views of food safety in their neighbourhood shops or the top priorities they consider when purchasing and consuming food, and the factors that underlie those priorities11,47,56. Mixed, integrated qualitative and quantitative methods and the triangulation of multiple data sources may provide a more comprehensive picture of children’s and adolescents’ perspectives and interactions with the food environment11,23,47,56.
In high-income settings, geographic information systems (GIS), global positioning systems (GPS) and shop audits are widely used to assess spatial indicators of food environments57,58,59,60. Food procurement by individuals, especially those in LMICs, however, may not be limited to geographic boundaries designated by GIS and GPS coordinates47. For example, shifts in daily activities (for example, commutes to and from school) contribute to the spatial and temporal uncertainty in identifying the relevant geographic area that exerts behavioural influence and exposure to various food environments. This has been raised as a major challenge in developing food environment metrics61. In some LMIC contexts, the informal nature of markets and mobile street stalls further complicates the accurate characterization of the food environment24,62. In addition, food choice behaviours of school-aged children and adolescents are influenced by objective features of the food environment, their perspectives about the food environment and purchasing decisions made by their caregivers. Proxy measures at the interface between personal and external food environment are contingent on consumer behaviour and relate to household affordability, including purchasing patterns (for example, frequency of fast-food/take-out purchases per month), purchasing power (for example, amount of pocket money given to children and adolescents to purchase food at school), spending patterns (for example, household income and budget share spent on fruits and vegetables) and perceived affordability.
There is also a widely recognized need for improved measurement and collection of dietary intake and diet quality data for children and adolescents in LMICs3,4. Available evidence linking diets to the food environment is inconsistent because few intervention studies measure dietary intake and quality, reported food choices and behaviours, and nutritional knowledge23,49,53. Especially in this age group, food choice and behaviour, and subsequently dietary intake, are influenced not only by objective features and personal perspectives of the food environment, but also by the purchasing decisions made by caregivers. The involvement and influence of caregivers in a child’s or adolescent’s food choice should be considered in the measurement dietary intake and behaviours. In addition, collection and interpretation of dietary intake data are inherently challenging due to a lack of standardization of methods, compositional data and metrics49,63,64. Furthermore, given that personal food environments are spaces that are rooted in and promote culture, norms and beliefs in food preparation and feeding practices, dietary intake data should sufficiently capture dietary patterns and the diversity and complexity of cultural, wild and traditional, and home-prepared foods49,63,64. To date, there exists no single, validated composite index or tool to effectively measure diet quality2. With a variety of rapid and inexpensive dietary assessment tools available, there is a strong tendency to use food frequency indicators as proxies for diet quality, in terms of dietary diversity and adequate nutrient content14,24,49.
Future research should also consider how this group makes food choice decisions and procures food in a variety of settings, such as the household, community, workplace and market environments. In the home environment, younger children’s food choice and behaviour may be strongly influenced by their caregivers, who make the primary decisions regarding food procurement3. As they transition into adolescence, children have greater freedom of choice and exposure to influences in food purchasing and consumption outside the home15,16,48. The role of personal factors (for example, nutrition literacy, appetite, preference and desirability) and the potential influences of conventional and digital advertisements (for example, social media and Internet marketing)65 to which this age group is exposed should be considered. This transition is influenced by greater autonomy, more independent travel, availability of pocket money and greater influence of peers15,48. The precise patterns of independence and agency will probably vary—perhaps substantially by child age, gender, culture and religion, social and economic status, and across geographic, political and built environmental contexts.
Given the current array of measures, indicators and assessment tools, a global food environment research agenda should aim to test and implement standardized methods, measures and indicators that accurately and reliably reflect the effects of the food environment on children and adolescents in LMICs11,14,23,24,48,50,56.
Standardized metrics and indicators
Food environment measures and indicators relevant to school-aged children and adolescents in LMICs should: (1) be specific, measurable, achievable, relevant and timely; (2) be applicable, valid and cross-context equivalent across diverse geographies to enable accurate comparisons across countries; (3) be translatable to drive policy action and implementation; and (4) help reveal gaps in current knowledge or practice relevant to public health priorities66. Examples of food environment measures and indicators, available tools, and suggested data collection methods in the context of school-aged children and adolescents in LMICs by domain, construct and survey type are presented in Table 1.
There are several methodological considerations in the development of food environment measures and indicators. First, agreement on standardized parameters for geographic range (proximity and density measures) is needed. Synthesizing food accessibility, availability and promotion using density measures depends on the definition of consistent reference points and buffer radial ranges (for example, 250, 500 or 750 m radius around a school). Second, while nutrient profiling models exist to dichotomize healthy versus unhealthy foods, especially for marketing to children, this classification system is not established for food retailers67. Criteria to distinguish foods, and to discriminate and categorize between healthy and unhealthy food access points (for example, retailers), would be useful. It may be necessary to determine whether such a dichotomy is appropriate or if a gradient in healthfulness is more effective. The classification of healthy versus unhealthy foods and retailers influences the inferences made about accessibility and availability, and may lead to spurious conclusions about causal relations of health outcomes with the food environment. Third, frequency measures that are applicable to food availability (for example, number of items available for sale) and food promotion (for example, television and Internet advertisement viewings) need to be standardized in terms of sampling frames, measurement units (timing) and other contextual information (channel type)68,69. At present, the International Network for Food and Obesity/Non-Communicable Diseases Research, Monitoring and Action Support (INFORMAS) has developed protocols for food retail, provision and promotion, but these are not specific to school-aged children and adolescents67,68,69.
Routine and market survey data
Routine national and sub-national surveys, such as the Multiple Indicator Cluster Survey, the Demographic and Health Survey, the Global School-Based Student Health Survey and Health Behaviour in School-Age Children, and large longitudinal studies such as Young Lives and Gender and Adolescence Global Evidence, may provide opportunities to assess representative populations and to extract information about personal and external food environments of school-aged children and adolescents14,70. For example, in areas where local infrastructure (for example, electricity, refrigeration and transportation) is inadequately developed, assessment of food acquisition (for example, proportion of food grown or purchased) and food preparation (proportion of food prepared or purchased ready-made) at the household level may explain the relative influence of personal versus external food environments13. In many LMICs, this interface becomes increasingly complex within modernized food environments, whereby the time burden of household food preparation competes with the cost and convenience of shop-bought prepared foods13.
Market and consumer surveys and tools71 developed both by the public (including the United Nations and non-governmental organizations) and private sectors are important to better understand the external food environment. These types of surveys have been widely used by the private sector to create industry benchmarks for sales and marketing, but these data are often proprietary or very expensive to purchase and use. Greater collaboration between the public and private sectors may enable researchers and policymakers to leverage available data sources to generate measures and indicators appropriate to school-aged children and adolescents in order to monitor the external food environment.
Collaboration with the private sector
Renewed efforts are needed to build an equity-sensitive, rights-based food systems agenda that promotes the basic human right to healthy, nutritious, affordable, safe and accessible food, and ultimately diets, with specific considerations to protect and promote the unique needs of children and adolescents14,64. Private sector and industry partners should be incentivized to produce and market healthier, safe and more sustainable food and beverage products, as well as to comply with international and national codes of conduct regarding production, packaging and labelling, and marketing and promotion to children and adolescents72,73. The private sector may help drive investments in technological innovation and advancement in agriculture and food manufacturing. For example, reformulation efforts to reduce levels of sodium and sugars, eliminate trans-fats, strengthen large-scale food fortification and increase availability of specially formulated foods for children and adolescents3.
Investing in evidence-based research and policy actions
Numerous global research institutions and non-governmental organizations have made strides in developing collaborative tools and platforms to monitor food environments globally, such as the Healthy Food Environment Policy Index by INFORMAS74, the Measurement, Evaluation, Accountability, and Leadership Support for NCDs75, the NCD Risk Factor Collaboration76 and, recently, the Food Systems Dashboard77. These concerted efforts by stakeholders are vital in streamlining and tracking progress of health goals, interventions and policy implementation in real time. However, systemic barriers within food systems will continue to hinder progress if left unaddressed. Societal inequities related to race, gender and socioeconomic status permeate food systems, exacerbate dietary inadequacies and result in intergenerational malnutrition15. Food consumption is affected by power imbalances that are influenced by the priorities and agendas of governments at all levels, the agricultural industry, transnational food and beverage corporations, international development policymakers, and donors78.
Governments, funding agencies and donors should seek to increase research spending to address evidence gaps regarding food environments of children and adolescents. Funding should be allocated towards strengthening capacity to identify innovative and cost-effective interventions and solutions to target health and nutrition in this population, with the consideration of local culture and practices3. Governments have the capacity to enact proactive interventions that target food environments and delivery platforms directed at school-aged children and adolescents to minimize inequities, support agency, and promote safe, affordable and healthy food. These may include taxes on unhealthy foods and beverages79, subsidy programmes, behavioural change and nutrition education programmes, and food environment interventions3. In addition, stronger governance is necessary to ensure that policies in food, agriculture and trade align with public health and nutrition targets, and do not compromise the cost and affordability of food consumed by children and adolescents. This may be achieved with robust legal and regulatory frameworks that can effectively monitor adherence and compliance among both public and private sector partners3,17.
Way forward
Beyond providing access to healthy, nutritious, affordable and safe food, food systems—including food environments—promote food culture, traditions and practices, and support the incomes and livelihoods of 1 billion people globally80. However, the rapidly changing landscape of food systems, including food environments, has also had negative consequences, including rising NCD rates, the climbing costs of food, food waste and unsafe food, that threaten global food security, nutrition and diets. In the current context of increased urbanization, climate change, ongoing humanitarian conflicts and disruptions due to the COVID-19 pandemic, food systems are at a crossroads2,17,81.
Global discourse around transforming food systems and a united agenda to create a resilient food system that prioritizes nutrition and diets particularly for the world’s children has intensified4,82. For this reason, we propose three mutually reinforcing priority actions and research efforts required to develop and test standardized food environment measures and indicators that directly inform policies and programming, and allow monitoring of progress of school-aged children and adolescents in LMICs (Box 1). Global public mobilization and actionable commitments from all stakeholders to invest in diverse ways to make food systems inclusive, climate-smart, resilient and supportive of sustainable peace is needed82. Furthermore, stronger collaboration among stakeholders will be vital to enable policy action and investments to promote food security and nutrition for future generations. Finally, policies and context-specific strategies must be developed and promoted in a manner that embraces the interdependence between the food system and other societal subsystems (health, environment and climate, social protection, education and water, and sanitation and hygiene), as well as democratizing food systems to restore food-related freedom of choice and sovereignty.
References
The State of Food Security and Nutrition in the World 2018: Building Climate Resilience for Food Security and Nutrition (FAO, IFAD, UNICEF, WFP, WHO, 2018).
The State of Food Security and Nutrition in the World 2020: Transforming Food Systems for Affordable Healthy Diets (FAO, IFAD, UNICEF, WFP, WHO, 2020).
2020 Global Nutrition Report: Action on Equity to End Malnutrition (Development Initiatives, 2020).
State of the World’s Children 2019: Children, Food and Nutrition: Growing Well in a Changing World (UNICEF, 2019).
Afshin, A. et al. Health effects of dietary risks in 195 countries, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 393, 1958–1972 (2019).
Baker, P. & Friel, S. Food systems transformations, ultra-processed food markets and the nutrition transition in Asia. Glob. Health 12, 80 (2016).
Popkin, B. M. & Reardon, T. Obesity and the food system transformation in Latin America. Obes. Rev. 19, 1028–1064 (2018).
Swinburn, B. et al. INFORMAS (International Network for Food and Obesity/Non-Communicable Diseases Research, Monitoring and Action Support): overview and key principles. Obes. Rev. 14, 1–12 (2013).
Nutrition and Food Systems: A Report by the High Level Panel of Experts on Food Security & Nutrition of the Committee on World Food Security (HLPE CFS, 2017).
Glanz, K., Sallis, J. F., Saelens, B. E. & Frank, L. D. Healthy nutrition environments: concepts and measures. Am. J. Health Promot. 19, 330–333 (2005).
Turner, C. et al. Concepts and critical perspectives for food environment research: a global framework with implications for action in low- and middle-income countries. Glob. Food Secur. 18, 93–101 (2018).
Global Nutrition Report 2017: Nourishing the SDGs (Development Initiatives, 2017).
Herforth, A. & Ahmed, S. The food environment, its effects on dietary consumption, and potential for measurement within agriculture-nutrition interventions. Food Secur. 7, 505–520 (2015).
Hawkes, C., Fox, E., Downs, S. M., Fanzo, J. & Neve, K. Child-centered food systems: reorienting food systems towards healthy diets for children. Glob. Food Secur. 27, 100414 (2020).
Food Systems for Children and Adolescents: Working Together to Secure Nutritious Diets (UNICEF Innocenti, 2018).
Raza, A. et al. Conceptual framework of food systems for children and adolescents. Glob. Food Secur. 27, 100436 (2020).
Food Security and Nutrition: Building a Global Narrative Towards 2030 (HLPE CFS, 2020).
Peter, F. Gender and the foundations of social choice: the role of situated agency. Fem. Econ. 9, 13–32 (2003).
Engler-Stringer, R., Le, H., Gerrard, A. & Muhajarine, N. The community and consumer food environment and children’s diet: a systematic review. BMC Public Health 14, 522 (2014).
Downs, S. M., Ahmed, S., Fanzo, J. & Herforth, A. Food environment typology: advancing an expanded definition, framework, and methodological approach for improved characterization of wild, cultivated, and built food environments toward sustainable diets. Foods https://doi.org/10.3390/foods9040532 (2020).
Fanzo, J. Healthy and sustainable diets and food systems: the key to achieving Sustainable Development Goal 2? Food Ethics 4, 159–174 (2019).
Haynes, E. et al. Food sources and dietary quality in small island developing states: development of methods and policy relevant novel survey data from the Pacific and Caribbean. Nutrients https://doi.org/10.3390/nu12113350 (2020).
Carducci, B., Oh, C., Keats, E. C., Roth, D. E. & Bhutta, Z. A. Effect of food environment interventions on anthropometric outcomes in school-aged children and adolescents in low- and middle-income countries: a systematic review and meta-analysis. Curr. Dev. Nutr. 4, nzaa098 (2020).
Turner et al. Food environment research in low- and middle-income countries: a systematic scoping review. Adv. Nutr. 11, 387–397 (2020).
Pineda, E., Swinburn, B. & Sassi, F. Effective school food environment interventions for the prevention of childhood obesity: systematic review and meta-analysis. Lancet https://doi.org/10.1016/s0140-6736(19)32874-0 (2019).
Downs, S. & Demmler, K. M. Food environment interventions targeting children and adolescents: a scoping review. Glob. Food Secur. https://doi.org/10.1016/j.gfs.2020.100403 (2020).
Correa, E. N., Rossi, C. E., das Neves, J., Silva, D. A. S. & de Vasconcelos, F. A. G. Utilization and environmental availability of food outlets and overweight/obesity among schoolchildren in a city in the south of Brazil. J. Public Health 40, 106–113 (2018).
de Assuncao Bezerra, M. K. et al. Health promotion initiatives at school related to overweight, insulin resistance, hypertension and dyslipidemia in adolescents: a cross-sectional study in Recife, Brazil. BMC Public Health 18, 223 (2018).
Motter, A. F., Vasconcelos Fde, A., Correa, E. N. & Andrade, D. F. Retail food outlets and the association with overweight/obesity in schoolchildren from Florianopolis, Santa Catarina State, Brazil. Cad. Saude Publica 31, 620–632 (2015).
Rossi, C. E., Patricia de Fragas, H., Correa, E. N., das Neves, J. & de Vasconcelos, F. A. G. Association between food, physical activity, and social assistance environments and the body mass index of schoolchildren from different socioeconomic strata. J. Public Health 41, e25–e34 (2019).
Dillman Carpentier, F. R., Correa, T., Reyes, M. & Taillie, L. S. Evaluating the impact of Chile’s marketing regulation of unhealthy foods and beverages: pre-school and adolescent children’s changes in exposure to food advertising on television. Public Health Nutr. 23, 747–755 (2020).
Rebolledo, N., Reyes, M., Corvalan, C., Popkin, B. M. & Smith Taillie, L. Dietary intake by food source and eating location in low- and middle-income Chilean preschool children and adolescents from southeast Santiago. Nutrients https://doi.org/10.3390/nu11071695 (2019).
An, R., He, L. & Shen, M. J. Impact of neighbourhood food environment on diet and obesity in China: a systematic review. Public Health Nutr. 23, 457–473 (2020).
Pehlke, E. L., Letona, P., Hurley, K. & Gittelsohn, J. Guatemalan school food environment: impact on schoolchildren’s risk of both undernutrition and overweight/obesity. Health Promot. Int. 31, 542–550 (2016).
Chacon, V., Letona, P., Villamor, E. & Barnoya, J. Snack food advertising in stores around public schools in Guatemala. Crit. Public Health 25, 291–298 (2015).
Umberger, W. J., He, X., Minot, N. & Toiba, H. Examining the relationship between the use of supermarkets and over-nutrition in Indonesia. Am. J. Agric. Econ. 97, 510–525 (2015).
Barrera, L. H., Rothenberg, S. J., Barquera, S. & Cifuentes, E. The toxic food environment around elementary schools and childhood obesity in Mexican cities. Am. J. Prev. Med. 51, 264–270 (2016).
Soltero, E. G. et al. Characterization of the school neighborhood food environment in three Mexican cities. Ecol. Food Nutr. 56, 139–151 (2017).
Okeyo, A. P. et al. The food and nutrition environment at secondary schools in the Eastern Cape, South Africa as reported by learners. Int. J. Environ. Res. Public Health https://doi.org/10.3390/ijerph17114038 (2020).
Moodley, G., Christofides, N., Norris, S. A., Achia, T. & Hofman, K. J. Obesogenic environments: access to and advertising of sugar-sweetened beverages in Soweto, South Africa, 2013. Prev. Chronic Dis. 12, E186 (2015).
Khonje, M. G., Ecker, O. & Qaim, M. Effects of modern food retailers on adult and child diets and nutrition. Nutrients https://doi.org/10.3390/nu12061714 (2020).
Laar, A. et al. Implementation of healthy food environment policies to prevent nutrition-related non-communicable diseases in Ghana: national experts’ assessment of government action. Food Policy 93, 101907 (2020).
El-Ammari, A., El Kazdouh, H., Bouftini, S., El Fakir, S. & El Achhab, Y. Social-ecological influences on unhealthy dietary behaviours among Moroccan adolescents: a mixed-methods study. Public Health Nutr. 23, 996–1008 (2020).
Debela, B. L., Demmler, K. M., Klasen, S. & Qaim, M. Supermarket food purchases and child nutrition in Kenya. Glob. Food Secur. https://doi.org/10.1016/j.gfs.2019.100341 (2020).
Nadeem Gill, F. An assessment of adolescent eating habits in public schools of Chak Shahzad, Islamabad. Int. J. Nutr. Food Sci. 5, 304–309 (2016).
Rathi, N., Riddell, L. & Worsley, A. Food environment and policies in private schools in Kolkata, India. Health Promot. Int. 32, 340–350 (2017).
Caspi, C. E., Sorensen, G., Subramanian, S. V. & Kawachi, I. The local food environment and diet: a systematic review. Health Place 18, 1172–1187 (2012).
Williams, J. et al. A systematic review of the influence of the retail food environment around schools on obesity-related outcomes. Obes. Rev. 15, 359–374 (2014).
Kirkpatrick, S. I. et al. Dietary assessment in food environment research: a systematic review. Am. J. Prev. Med. 46, 94–102 (2014).
Driessen, C. E., Cameron, A. J., Thornton, L. E., Lai, S. K. & Barnett, L. M. Effect of changes to the school food environment on eating behaviours and/or body weight in children: a systematic review. Obes. Rev. 15, 968–982 (2014).
Foster, G. D. et al. A policy-based school intervention to prevent overweight and obesity. Pediatrics 121, e794–e802 (2008).
One in Five Children, Adolescents and Youth is Out of School (UNESCO Institute of Statistics, 2018).
Osei-Assibey, G. et al. The influence of the food environment on overweight and obesity in young children: a systematic review. BMJ Open 2, e001538 (2012).
Burchi, F., Fanzo, J. & Frison, E. The role of food and nutrition system approaches in tackling hidden hunger. Int. J. Environ. Res. Public Health 8, 358–373 (2011).
Taillie, L. S. et al. Best practices for using natural experiments to evaluate retail food and beverage policies and interventions. Nutr. Rev. 75, 971–989 (2017).
Pitt, E., Gallegos, D., Comans, T., Cameron, C. & Thornton, L. Exploring the influence of local food environments on food behaviours: a systematic review of qualitative literature. Public Health Nutr. 20, 2393–2405 (2017).
Cetateanu, A. & Jones, A. How can GPS technology help us better understand exposure to the food environment? A systematic review. SSM Popul. Health 2, 196–205 (2016).
Lytle, L. A. & Sokol, R. L. Measures of the food environment: a systematic review of the field, 2007-2015. Health Place 44, 18–34 (2017).
Wilkins, E. L., Morris, M. A., Radley, D. & Griffiths, C. Using geographic information systems to measure retail food environments: discussion of methodological considerations and a proposed reporting checklist (Geo-FERN). Health Place 44, 110–117 (2017).
McKinnon, R. A., Reedy, J., Morrissette, M. A., Lytle, L. A. & Yaroch, A. L. Measures of the food environment: a compilation of the literature, 1990-2007. Am. J. Prev. Med. 36, S124–S133 (2009).
Liu, B., Widener, M., Burgoine, T. & Hammond, D. Association between time-weighted activity space-based exposures to fast food outlets and fast food consumption among young adults in urban Canada. Int. J. Behav. Nutr. Phys. Act. 17, 62 (2020).
Spires, M. et al. Snapshots of urban and rural food environments: EPOCH-based mapping in a high-, middle-, and low-income country from a non-communicable disease perspective. Nutrients https://doi.org/10.3390/nu12020484 (2020).
Keats, E. C. et al. The dietary intake and practices of adolescent girls in low- and middle-income countries: a systematic review. Nutrients https://doi.org/10.3390/nu10121978 (2018).
Kupka, R., Siekmans, K. & Beal, T. The diets of children: overview of available data for children and adolescents. Glob. Food Secur. https://doi.org/10.1016/j.gfs.2020.100442 (2020).
Tatlow-Golden, M. & Garde, A. Digital food marketing to children: exploitation, surveillance and rights violations. Glob. Food Secur. https://doi.org/10.1016/j.gfs.2020.100423 (2020).
Frongillo, E. A., Baranowski, T., Subar, A. F., Tooze, J. A. & Kirkpatrick, S. I. Establishing validity and cross-context equivalence of measures and indicators. J. Acad. Nutr. Diet 119, 1817–1830 (2019).
L’Abbe, M. et al. Monitoring foods and beverages provided and sold in public sector settings. Obes. Rev. 14, 96–107 (2013).
Kelly, B. et al. Monitoring food and non-alcoholic beverage promotions to children. Obes. Rev. 14, 59–69 (2013).
Ni Mhurchu, C. et al. Monitoring the availability of healthy and unhealthy foods and non-alcoholic beverages in community and consumer retail food environments globally. Obes. Rev. 14, 108–119 (2013).
Wilson, I., Huttly, S. R. A. & Fenn, B. A case study of sample design for longitudinal research: young lives. Int. J. Soc. Res. Methodol. 9, 351–365 (2006).
Glanz, K., Sallis, J. F., Saelens, B. E. & Frank, L. D. Nutrition environment measures survey in stores (NEMS-S): development and evaluation. Am. J. Prev. Med. 32, 282–289 (2007).
White, M. et al. What role should the commercial food system play in promoting health through better diet? Brit. Med. J. 368, m545 (2020).
Fanzo, J., Shawar, Y., Shyam, T., Das, S. & Shiffman, J. Challenges to establish effective public-private partnerships to address malnutrition in all its forms. Int. J. Health Policy Manag. https://doi.org/10.34172/ijhpm.2020.262 (2021).
Swinburn, B. et al. Monitoring and benchmarking government policies and actions to improve the healthiness of food environments: a proposed government healthy food environment policy index. Obes. Rev. 14, 24–37 (2013).
Measuring the Healthiness of Ghanaian Children’s Food Environments to Prevent Obesity and Non-communicable Diseases (MEALS4NCDs, 2020); https://www.meals4ncds.org/en/
NCD Risk Factor Collaboration Website (NCD-RisC, 2017); http://ncdrisc.org/index.html
Fanzo, J. et al. The Food Systems Dashboard is a new tool to inform better food policy. Nat. Food 1, 243–246 (2020).
Bene, C. et al. Global drivers of food system (un)sustainability: a multi-country correlation analysis. PLoS ONE 15, e0231071 (2020).
Du, M., Tugendhaft, A., Erzse, A. & Hofman, K. J. Sugar-sweetened beverage taxes: industry response and tactics. Yale J. Biol. Med. 91, 185–190 (2018).
Mbow, C. et al. in Special Report on Climate Change, Desertifcation, Land Degradation, Sustainable Land Management, Food Security, and Greenhouse Gas Fluxes in Terrestrial Ecosystems (eds Shukla, P. R. et al.) Ch. 5 (IPCC, Cambridge Univ. Press, 2019).
Willett, W. et al. Food in the Anthropocene: the EAT-Lancet commission on healthy diets from sustainable food systems. Lancet 393, 447–492 (2019).
Food Systems Summit 2021 (United Nations, 2020); https://www.un.org/sustainabledevelopment/food-systems-summit-2021/
Acknowledgements
We gratefully acknowledge the following individuals for their technical expertise during the workshop: A. Samuels, A. Demaio, A. Laar, C. Corvalan, C. Hayashi, C. Jalal, D. Tschirley, E. Nsosie, E. Kamau-Mbuthia, E. Keats, G. Kennedy, G. Hallen, H. Danton, J. Leroy, J. Tench, J. Rivera, K. Engesveen, K. Lichtner, L. Olson, M. Arabi, M. Corradini, M. Spires, M. Bloem, M. Woldt, P. Vos, R. Egan, R. Kupka, S. Hanck, S. Pedersen, S. de Pee, S. Downs, S. Sundberg, S. Barquera, S. Namaste, S. Nordhagen, S. Kadiyala, T. Nguyen and Z. Leung. A special thanks to A. Laar, E. Nsosie, H. Danton, K. Engesveen, M. Corradini, M. Spires, M. Woldt, R. Kupka, S. Pedersen, S. de Pee, S. Downs, S. Nordhagen and T. Nguyen for their review of the first draft of the manuscript. We thank G. Belayneh and C. McPherson for their administrative support for the workshop. The Centre for Global Child Health, Hospital for Sick Children, Joannah and Brian Lawson Centre for Child Nutrition, University of Toronto and the Global Alliance for Improved Nutrition co-funded the technical workshop.
Author information
Authors and Affiliations
Contributions
This Perspective is the result of discussions from a two-day technical workshop (January 2020), co-hosted by the Centre for Global Child Health, the Hospital for Sick Children, the Lawson Centre for Child Nutrition (University of Toronto) and the Global Alliance for Improved Nutrition. B.C., C.O., D.E.R., L.M.N., J.F., M.R.L., D.W.S. and Z.A.B. planned the workshop. B.C., C.O., D.E.R., L.M.N., D.W.S. and Z.A.B. facilitated the workshop. B.C. and C.O. wrote the first draft of the manuscript with substantive input from E.A.F. and A.H. All authors provided input, contributed to the revisions and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Nature Food thanks Christopher Turner, Ahmed Raza and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Table 1.
Rights and permissions
About this article
Cite this article
Carducci, B., Oh, C., Roth, D.E. et al. Gaps and priorities in assessment of food environments for children and adolescents in low- and middle-income countries. Nat Food 2, 396–403 (2021). https://doi.org/10.1038/s43016-021-00299-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s43016-021-00299-5
This article is cited by
-
Food environment research in Canada: a rapid review of methodologies and measures deployed between 2010 and 2021
International Journal of Behavioral Nutrition and Physical Activity (2024)
-
A Proposed Research Agenda for Promoting Healthy Retail Food Environments in the East Asia–Pacific Region
Current Nutrition Reports (2021)