Abstract
Chronic obstructive pulmonary disease (COPD) is a major cause of morbidity and death worldwide. Peroxynitrite, formed from nitric oxide, which is derived from inducible nitric oxide synthase, and superoxide, has been implicated in the development of emphysema, but the source of the superoxide was hitherto not characterized. Here, we identify the non-phagocytic NADPH oxidase organizer 1 (NOXO1) as the superoxide source and an essential driver of smoke-induced emphysema and pulmonary hypertension development in mice. NOXO1 is consistently upregulated in two models of lung emphysema, Cybb (also known as NADPH oxidase 2, Nox2)-knockout mice and wild-type mice with tobacco-smoke-induced emphysema, and in human COPD. Noxo1-knockout mice are protected against tobacco-smoke-induced pulmonary hypertension and emphysema. Quantification of superoxide, nitrotyrosine and multiple NOXO1-dependent signalling pathways confirm that peroxynitrite formation from nitric oxide and superoxide is a driver of lung emphysema. Our results suggest that NOXO1 may have potential as a therapeutic target in emphysema.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Data availability
Microarray data have been deposited at NCBI as GEO (accession number GSE112287). The data underlying all findings of this study are available from the corresponding author upon request and are provided as separate source data files. Source Data for Figs. 1–7 and Extended Data Figs. 1–8 are available online.
Change history
26 June 2020
A Correction to this paper has been published: https://doi.org/10.1038/s42255-020-0248-z
References
Barnes, P. J. et al. Chronic obstructive pulmonary disease. Nat. Rev. Dis. Primers 1, 15076 (2015).
Adeloye, D. et al. Global and regional estimates of COPD prevalence: systematic review and meta-analysis. J. Glob. Health 5, 020415 (2015).
Mercado, N., Ito, K. & Barnes, P. J. Accelerated ageing of the lung in COPD: new concepts. Thorax 70, 482–489 (2015).
Repine, J. E., Bast, A. & Lankhorst, I. Oxidative stress in chronic obstructive pulmonary disease. Oxidative Stress Study Group. Am. J. Respir. Crit. Care Med. 156, 341–357 (1997).
Barnes, P. J. Cellular and molecular mechanisms of chronic obstructive pulmonary disease. Clin. Chest. Med. 35, 71–86 (2014).
Seimetz, M. et al. Inducible NOS inhibition reverses tobacco-smoke-induced emphysema and pulmonary hypertension in mice. Cell 147, 293–305 (2011).
Weissmann, N. et al. Stimulation of soluble guanylate cyclase prevents cigarette smoke-induced pulmonary hypertension and emphysema. Am. J. Respir. Crit. Care Med. 189, 1359–1373 (2014).
Peinado, V. I., Pizarro, S. & Barbera, J. A. Pulmonary vascular involvement in COPD. Chest 134, 808–814 (2008).
Nathan, S. D. et al. Pulmonary hypertension in chronic lung disease and hypoxia. Eur. Respir. J. 53, 1801914 (2019).
Kharitonov, S. A. & Barnes, P. J. Nitric oxide, nitrotyrosine, and nitric oxide modulators in asthma and chronic obstructive pulmonary disease. Curr. Allergy Asthma Rep. 3, 121–129 (2003).
Szabo, C., Ischiropoulos, H. & Radi, R. Peroxynitrite: biochemistry, pathophysiology and development of therapeutics. Nat. Rev. Drug Discov. 6, 662–680 (2007).
Barnes, P. J. Inflammatory mechanisms in patients with chronic obstructive pulmonary disease. J. Allergy Clin. Immunol. 138, 16–27 (2016).
Kassim, S. Y. et al. NADPH oxidase restrains the matrix metalloproteinase activity of macrophages. J. Biol. Chem. 280, 30201–30205 (2005).
Lambeth, J. D., Kawahara, T. & Diebold, B. Regulation of Nox and Duox enzymatic activity and expression. Free Radic. Biol. Med. 43, 319–331 (2007).
Ris-Stalpers, C. Physiology and pathophysiology of the DUOXes. Antioxid. Redox. Signal. 8, 1563–1572 (2006).
Ambasta, R. K. et al. Direct interaction of the novel Nox proteins with p22phox is required for the formation of a functionally active NADPH oxidase. J. Biol. Chem. 279, 45935–45941 (2004).
Brandes, R. P., Weissmann, N. & Schroder, K. Nox family NADPH oxidases: molecular mechanisms of activation. Free Radic. Biol. Med. 76, 208–226 (2014).
Selemidis, S., Sobey, C. G., Wingler, K., Schmidt, H. H. & Drummond, G. R. NADPH oxidases in the vasculature: molecular features, roles in disease and pharmacological inhibition. Pharmacol. Ther. 120, 254–291 (2008).
Schroder, K., Weissmann, N. & Brandes, R. P. Organizers and activators: cytosolic Nox proteins impacting on vascular function. Free Radic. Biol. Med. 109, 22–32 (2017).
Ueyama, T., Lekstrom, K., Tsujibe, S., Saito, N. & Leto, T. L. Subcellular localization and function of alternatively spliced Noxo1 isoforms. Free Radic. Biol. Med. 42, 180–190 (2007).
Trocme, C. et al. Macrophage-specific NOX2 contributes to the development of lung emphysema through modulation of SIRT1/MMP-9 pathways. J. Pathol. 235, 65–78 (2015).
Vlahos, R. & Bozinovski, S. Role of alveolar macrophages in chronic obstructive pulmonary disease. Front. Immunol 5, 435 (2014).
Malczyk, M. et al. Classical transient receptor potential channel 1 in hypoxia-induced pulmonary hypertension. Am. J. Respir. Crit. Care Med. 188, 1451–1459 (2013).
Ball, M. K. et al. Regulation of hypoxia-induced pulmonary hypertension by vascular smooth muscle hypoxia-inducible factor-1α. Am. J. Respir. Crit. Care Med. 189, 314–324 (2014).
Kuwano, Y. et al. Tumor necrosis factor alpha activates transcription of the NADPH oxidase organizer 1 (NOXO1) gene and upregulates superoxide production in colon epithelial cells. Free Radic. Biol. Med. 45, 1642–1652 (2008).
Houghton, A. M. Matrix metalloproteinases in destructive lung disease. Matrix Biol. 44-46, 167–174 (2015).
Joo, J. H. et al. NADPH oxidase 1 activity and ROS generation are regulated by Grb2/Cbl-mediated proteasomal degradation of NoxO1 in colon cancer cells. Cancer Res. 76, 855–865 (2016).
Plataki, M. et al. Apoptotic mechanisms in the pathogenesis of COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 1, 161–171 (2006).
Yokohori, N., Aoshiba, K. & Nagai, A. & Respiratory Failure Research Group in Japan. Increased levels of cell death and proliferation in alveolar wall cells in patients with pulmonary emphysema. Chest 125, 626–632 (2004).
Barnes, P. J. Role of HDAC2 in the pathophysiology of COPD. Annu. Rev. Physiol. 71, 451–464 (2009).
Fredenburgh, L. E., Perrella, M. A. & Mitsialis, S. A. The role of heme oxygenase-1 in pulmonary disease. Am. J. Respir. Cell Mol. Biol. 36, 158–165 (2007).
Giordano, L. et al. Alternative oxidase attenuates cigarette smoke-induced lung dysfunction and tissue damage. Am. J. Respir. Cell Mol. Biol. 60, 515–522 (2019).
MacNee, W. Oxidative stress and lung inflammation in airways disease. Eur. J. Pharmacol. 429, 195–207 (2001).
Henricks, P. A. & Nijkamp, F. P. Reactive oxygen species as mediators in asthma. Pulm. Pharmacol. Ther. 14, 409–420 (2001).
Trojanek, J. B. et al. Airway mucus obstruction triggers macrophage activation and matrix metalloproteinase 12-dependent emphysema. Am. J. Respir. Cell Mol. Biol. 51, 709–720 (2014).
Shaykhiev, R. et al. Smoking-dependent reprogramming of alveolar macrophage polarization: implication for pathogenesis of chronic obstructive pulmonary disease. J Immunol. 183, 2867–2883 (2009).
Karch, A. et al. The German COPD cohort COSYCONET: aims, methods and descriptive analysis of the study population at baseline. Respir. Med. 114, 27–37 (2016).
Donko, A. et al. Urothelial cells produce hydrogen peroxide through the activation of Duox1. Free Radic. Biol. Med. 49, 2040–2048 (2010).
Sommer, N. et al. Mitochondrial complex IV subunit 4 isoform 2 is essential for acute pulmonary oxygen sensing. Circ. Res. 121, 424–438 (2017).
Savai, R. et al. Pro-proliferative and inflammatory signaling converge on FoxO1 transcription factor in pulmonary hypertension. Nat. Med. 20, 1289–1300 (2014).
Cortez-Retamozo, V. et al. Real-time assessment of inflammation and treatment response in a mouse model of allergic airway inflammation. J. Clin. Invest. 118, 4058–4066 (2008).
Waypa, G. B., Chandel, N. S. & Schumacker, P. T. Model for hypoxic pulmonary vasoconstriction involving mitochondrial oxygen sensing. Circ. Res. 88, 1259–1266 (2001).
Gentleman, R. C. et al. Bioconductor: open software development for computational biology and bioinformatics. Genome Biol. 5, R80 (2004).
Smyth, G. K. & Speed, T. Normalization of cDNA microarray data. Methods 31, 265–273 (2003).
Smyth, G. K. Linear models and empirical bayes methods for assessing differential expression in microarray experiments. Stat. Appl. Genet. Mol. Biol. 3, Article3 (2004).
Song, J. et al. Identification of genetic defects in pulmonary arterial hypertension by a new gene panel diagnostic tool. Clin. Sci. (Lond) 130, 2043–2052 (2016).
Richards, S. et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the american college of medical genetics and genomics and the association for molecular pathology. Genet. Med. 17, 405–424 (2015).
Rentzsch, P., Witten, D., Cooper, G. M., Shendure, J. & Kircher, M. CADD: predicting the deleteriousness of variants throughout the human genome. Nucleic Acids Res. 47, D886–D894 (2019).
R Core Team. R: A Language and Environment for Statistical Computing (R Foundation for Statistical Computing, 2019).
Douglas Bates, M. M. & Bolker, Ben. Steve walker fitting linear mixed-effects models using lme4. J. Stat. Softw. 67, 1–48 (2015).
Hothorn, T., Bretz, F. & Westfall, P. Simultaneous inference in general parametric models. Biom. J. 50, 346–363 (2008).
Acknowledgements
The authors thank I. Breitenborn-Müller, L. Fröhlich, S. Gräf-Höchst, C. Homberger, E. Kappes, K. Palfi, M. Wessendorf, N. Schupp, S. Lich and K. Quanz for technical assistance. We also thank S. Kostin for providing confocal microscopy and related quantifications for Fig. 4e,f and 5e; M. Szibor for providing the AOX mice and E. Dufour for the AOX constructs for Extended Data Fig. 8i,j; and S. Kuhnert for coordination of the COSYCONET study (Supplementary Tables 4 and 5). Portions of the doctoral thesis of M.S. and M.B. are incorporated into this report. This work was in part funded by the German Research Foundation (DFG) (project numbers: SE 2289/5-1 and 268555672; CRC 1213: project A06, A07 and CP02) and the Excellence Cluster Cardio-Pulmonary Institute (CPI). C. Mulligan and P. Overton (Beacon Medical Communications) provided editorial support, funded by the University of Giessen.
Author information
Authors and Affiliations
Contributions
Conceptualization, M.S., N.S., N.W.; Methodology, M.S., N.S., S.H., C.V., M.B., N.P., F.K., A.P., B.K., J.W., A.F., W.K., P.J., R.T.S., H.A.G., S.K., E.B-V., K.S., R.P.B., N.W., M.G., E.G., M.H., A.H., W.P., S.G., C.F.V., A.G.; Formal analysis, J.W.; Investigation, M.S., S.H., C.V., M.G., F.K., S.K., M.B., N.P., A.P., B.K., J.W., O.P., S.S., A.F., C.E., E.G., K.H., M.H., A.H., W.P., P.D., S.G., C.W., I.H., Z.I.K., N.M., F.R., G.B., I.W.; Resources, N.W., R.T.S., H.A.G., E.B.-V., R.P.B., W.S.; Data Curation, M.S., M.B., N.P., A.P., B.K., S.K., J.W., O.P., S.S., A.F., A.G., W.P., P.J., N.W., Writing (Original Draft), M.S.; Writing (Review and Editing), M.S., N.S., C.V., C.F.V., N.W., M.B., N.P, A.P., B.K., J.W., O.P., S.S., A.F., W.K., P.J., H.A.G., S.K., E.B-V., F.G., W.S.; Visualization, M.S., N.S., S.H., C.V., M.G., F.K., S.K., M.B., N.P., B.K., J.W., O.P., S.S., N.W.; Supervision, M.S., N.S., N.W.; Project Administration, M.S., N.S., N.W.; Funding Acquisition, M.S., N.S., R.T.S., H.A.G., R.B.P., F.G., W.S., N.W.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Primary Handling Editor: Elena Bellafante.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Lung functional and hemodynamic parameters in Nox2−/y mice after 8 months of room air or smoke exposure and in 2-month-old Nox2−/y mice compared with WT controls.
a–c, Quantification of lung functional parameters and blood pressure. a, Tidal volume, b, airway resistance, and c, systemic arterial pressure in WT and Nox2−/y mice after 8 months of smoke exposure (SE) compared with non-smoke-exposed (room air, RA), age-matched controls (n = 5 lungs each for WT and n = 6 lungs each for Nox2−/y). d, Right heart hypertrophy given as the ratio of right ventricular mass to left ventricular + septum mass (RV/(LV + septum)) from dried heart tissue in WT and Nox2−/y mice with and without 8 months of smoke exposure (n = 6 hearts each). Genotype and smoke exposure had no effect on LV mass. e–f, Expression of mRNA (e, n = 4 lungs each for WT and n = 5 lungs each for Nox2−/y) and protein (f, n = 5 lungs each) of iNOS in Nox2–/y lung homogenate of 8-month-old mice. g–m, Quantification of lung functional parameters and pulmonary haemodynamics in 2-month-old Nox2–/y mice (g, n = 8 mice for WT and n = 9 mice for Nox2−/y; h, n = 7 mice each; i-k, n = 8 lungs each; l: n = 6 mice for WT and n = 8 mice for Nox2−/y, m, n = 8 lungs for WT and n = 9 lungs for Nox2−/y). Statistical analysis: a–d: 2 × 2 factorial model on the log-transformed data; p-values are from two-sided t-tests. e: p-values are from two-sided t-tests comparing the ∆Ct values. f, g, i, k–m: p-values are from Tukey HSD tests using the log-transformed data. j: p-values are from Tukey HSD tests using the logit-transformed data. Data are represented as single value and mean ± s.e.m.
Extended Data Fig. 2 Expression of NADPH oxidase subunits in human lungs, NoxO1 expression in 2-month-old Nox2–/y mice and after smoke exposure, and late apoptosis and necrosis in PCLS of Duox1–/– mice.
a, qRT-PCR analysis of NADPH oxidase subunit expression in lung homogenate from patients with COPD compared with healthy controls (n = 5 lungs each). b, Protein expression of NoxO1 in lungs from 2-month-old Nox2–/y mice (n = 6 lungs each). c, Protein expression of NoxO1 3 months after re-exposure of 8-month smoke-exposed (SE) mice to room air (RA) (n = 5 in 8 m RA + 3 m RA and n = 6 in 8 m SE + 3 m RA group). d, NoxO1 protein expression in lungs explanted from healthy donors and patients with end stage emphysema/COPD quantified by densitometry (n = 5 Donor and n = 6 COPD lungs). e–g, Protein expression of DUOX1 (e, n = 6 lungs each), DUOX2 (f, n = 10 Donor and n = 9 COPD lungs, quantification from 2 parallel blots), and NADPH oxidase isoform NOX4 (g, n = 6 lungs each) in lungs explanted from healthy donors and patients with end-stage emphysema/COPD. h, Late apoptosis and necrosis in precision-cut lung slices (PCLS) of Duox1–/– mice after treatment with different concentrations of cigarette smoke extract (CSE) (n = 4 PCLS, except n = 3 PCLS for 10% CSE in Duox1–/– mice). Statistical analysis: a: one-factorial model on ∆Ct values; Benjamini-Hochberg corrected p-values are from two-sided tests using the pooled variance across the genes (for details please refer to Supplementary Methods). b–e, g: p-values are from Tukey HSD tests using the log-transformed data. f: One-factorial linear mixed model on log-transformed data using the membrane as random factor; p-values are from Chi-squared tests. h: Two-factorial linear mixed model on log-transformed data using the subject (mouse) as random factor; p-values are from Chi-squared tests. Data are represented as single value and mean ± s.e.m.
Extended Data Fig. 3 Parameters of emphysema after 3 and 8 months of smoke exposure in WT and Noxo1–/– mice.
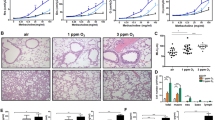
a, Quantification of septal wall thickness (alveolar morphometry; n = 9 lungs each for RA, n = 6 lungs for 8 m SE WT, n = 8 lungs for 8 m SE Noxo1–/–). RA, room air; SE, smoke exposure. b, Representative histologic images (stained with haematoxylin and eosin) of the lung parenchyma (n-number of stainings as given in (a)). c, Quantification of dynamic compliance (n = 12 lungs, except n = 11 lungs for 3 m SE Noxo1−/−). Statistical analysis: a,c 2 × 2 factorial models on log-transformed data; p-values are from 2-sided t-tests. Data are represented as single value and mean ± s.e.m.
Extended Data Fig. 4 In vivo and ex vivo characterization of parameters reflecting PH, right heart structure and function, and histology of the vasculature in WT and Noxo1−/− mice with and without smoke exposure.
a, Transthoracic echocardiography after 8 months of smoke exposure: i, Representative echocardiographic images, showing the short axis view of the right ventricle (RV), the four-chamber view demonstrating dilation of the RV (RV internal diameter: RVID), the pulmonary flow (pulmonary artery acceleration time: PAAT) which is inversely correlated to the RV systolic pressure (RVSP), and the tricuspid annular plane systolic excursion (TAPSE). ii–v, Quantitative analysis of PAAT (ii, n = 11 mice each for WT and n = 13 mice each for Noxo1−/−), right ventricular wall thickness (iii, RVWT, n = 10 mice for WT and n = 13 mice each for Noxo1−/− groups), RVID (iv, n = 10 mice each for WT and n = 13 mice each for Noxo1−/−) and TAPSE (v, n = 9 mice for 8 m RA WT, n = 10 mice for 8 m SE WT, n = 13 mice for 8 m RA Noxo1−/−, n = 11 mice for 8 m SE Noxo1−/− group). b–d, Parameters of PH after 3 months of smoke exposure. b, RVSP (n = 12 mice each, except n = 10 for 3 m SE Noxo1−/−) and c, Ratio of RV mass to left ventricular + septum mass (RV/(LV + septum). No changes in left ventricular mass were detectable among the different groups (n = 12 mice each, except n = 11 for 3 m SE Noxo1−/−). d, Vascular remodelling by quantification of muscularization degrees of small vessels, given as average of all muscularization, in lung sections co-stained against α-smooth muscle actin and von Willebrand factor (n = 4 lungs each). e, Representative histologic images from lung sections co-stained against α-smooth muscle actin and von Willebrand factor, demonstrating vascular remodelling after 8 months of smoke exposure. Statistical analysis: a, c: 2 × 2 factorial models on log-transformed data; p-values are from 2-sided t-tests. b: p-values are from Tukey HSD tests using the log-transformed data. d: 2 × 2 factorial models on logit-transformed data; p-values are from 2-sided t-tests. Data are represented as single value and mean ± s.e.m.
Extended Data Fig. 5 H2O2, nitrite/nitrate and NT in lungs of WT and Noxo1–/– mice after in vivo smoke exposure for different time periods.
a, Amplex® Red assay for quantification of hydrogen peroxide (H2O2) in ATII cells from WT and Noxo1−/− mice with and without 8 months smoke exposure (n = 3 cell isolations each). RA, room air; SE, smoke exposure. b, Quantification of nitrite (i, n = 5 lungs each, except n = 7 for 8 m SE WT) and nitrate (ii, n = 5 lungs each for RA, n = 7 lungs for 8 m SE WT, n = 4 lungs for 8 m SE Noxo1−/−) in bronchoalveolar lavage fluid (BALF) from WT and Noxo1−/− mice with and without 8 months smoke exposure. c, Quantification of NT staining after 3 months of in vivo smoke exposure (n = 8 lungs for 3 m RA WT, n = 7 lungs for 3 m SE WT, n = 9 lungs each for Noxo1−/−). d, NT staining after 2 weeks of high dose smoke exposure (500 mg/m3, 2 hours per day, 5 days per week) displayed as representative images (i, haematoxylin staining and NT staining in red colour) and quantification (ii, n = 3 lungs each). e, Picture of an isolated lung system (i, for details please refer to the methods section). NT staining after repetitive application of high dose cigarette smoke (3 times) over a period of 5 minutes once per hour (10 ml/minute, 3–4 seconds each breath) in the isolated lung by inhalation via the trachea (ii, representative images; iii, quantification). Lungs were collected 1 hour after the last cigarette smoke application (n = 3 lungs each group, except n = 4 for SE WT) f, Reactive nitrogen and oxygen species determined by detection of the CM ∙ radical with electron spin resonance using the spin probe CMH in the smoking chamber compared with room air (n = 6 for RA, n = 7 for smoking chamber). Statistical analysis: a–c: 2 × 2 factorial models on log-transformed data; p-values are from 2-sided t-tests. d, e: 2 × 2 factorial models on logit-transformed data; p-values are from 2-sided t-tests. f: p-values are from Tukey HSD tests using the log-transformed data. Data are represented as single value and mean ± s.e.m.
Extended Data Fig. 6 Effect of Noxo1 overexpression in vivo on lung function, haemodynamics and NT formation, as well as Noxo1–/– on chronic hypoxia-induced PH.
a–c, Effect of Noxo1 overexpression in vivo on dynamic compliance (a, n = 10 lungs for control AAV, n = 8 lungs for Noxo1 AAV), right ventricular systolic pressure (b, RVSP, n = 9 lungs for control AAV, n = 10 lungs for Noxo1 AAV) and NT formation (c i, representative images; c ii, quantification) in mouse lungs 6 weeks after application of Noxo1 by adeno-associated virus (AAV) in WT animals (n = 5 lungs each). d–f, Effect of Noxo1–/– in vivo on chronic hypoxia-induced PH. RVSP (d, n = 7 mice each, except n = 6 for normoxia Noxo1–/–), ratio of RV mass to left ventricular + septum mass (e, RV/(LV + septum), n = 7 mice each, except n = 6 for normoxia Noxo1–/–) and systemic arterial pressure (f). n = 7 mice each for WT and n = 6 mice each for Noxo1–/–. Statistical analysis: a, b, f: p-values are from Tukey HSD tests using the log-transformed data. c: p-values are from Tukey HSD tests using the logit-transformed data. d, e: 2 × 2 factorial models on log-transformed data; p-values are from 2-sided t-tests. Data are represented as single value and mean ± s.e.m.
Extended Data Fig. 7 Effects of smoke exposure on inflammation, cell proliferation, and apoptosis in WT and Noxo1−/− mice.
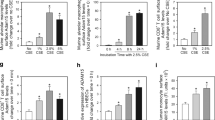
a, Quantification of inflammatory cells in cytospins of bronchoalveolar lavage fluid (BALF) from WT and Noxo1−/− mice with and without smoke exposure, visualized by Giemsa staining (BALF from n = 6 mice each). RA, room air, SE, smoke exposure. b, Proliferation of WT and Noxo1–/– PASMCs after in vitro cigarette smoke extract (CSE) exposure for 6 hours (n = 5 cell isolations each). c, Proliferation of PASMCs in presence of BALF from 8 months smoke- or room air-exposed WT or Noxo1–/– mice (n = 5 BALFs each). d, mRNA expression of depicted NADPH oxidase subunits in bone marrow derived macrophages (BMDM) compared with PASMCs and lung homogenate (LH). Data are from one experiment. e, Proliferation of ATII cells isolated from non-smoke-exposed WT and Noxo1−/− mice (n = 6 biologic replicates each for WT and n = 8 each for Noxo1−/− from 2–3 cell isolations). f, Suppression of proliferation by siRNA-mediated downregulation of Noxo1 is counteracted by lentiviral Noxo1 overexpression in PASMCs (n = 6 cell isolations, except n = 5 for siRNA Noxo1 and siRNA Noxo1 + Noxo1 vector). g, Glutathione-S-transferase activity in WT and Noxo1–/– lung homogenate (n = 12 lungs each). h, Apoptosis of PASMCs treated with siRNA for downregulation of Noxo1 and/or lentivirus for overexpression of Noxo1 (n = 3 cell isolations each, except n = 4 for Noxo1 vector, n = 5 cell for empty vector). i, Apoptosis of PASMCs isolated from non-smoke-exposed WT and Noxo1−/− mice (n = 8 biologic replicates each for WT, n = 7 biologic replicates each for Noxo1−/− from 2–3 cell isolations). Statistical analysis: a: 2 × 2 generalized linear model of the quasi-Poisson family with log-link; p-values are from Chi-squared tests. b, c: 2 × 2 factorial models on log-transformed data; p-values are from 2-sided t-tests. e–i: p-values are from Tukey HSD tests using the log-transformed data. Data are represented as single value and mean ± s.e.m.
Extended Data Fig. 8 Cigarette smoke extract (CSE)-induced apoptosis of ATII cells and in precision-cut lung slices (PCLS), and interaction of NoxO1 with mitochondria.
a, Apoptosis of WT ATII cells after CSE treatment in presence and absence of PEG superoxide dismutase (pSOD) (n = 7 biologic replicates from 3–4 cell isolations each). b, Late apoptosis and necrosis of WT and Noxo1–/– PCLS after CSE treatment in presence and absence of pSOD (n = 4 PCLS for Noxo1–/–, n = 5 PCLS each for WT from 4-5 mice). c, Apoptosis of WT and Noxo1–/– ATII cells after CSE treatment in presence and absence of potassium superoxide (KO2) (n = 7 biologic replicates from 3–4 cell isolations each). d, Late apoptosis and necrosis of WT and Noxo1–/– PCLS after CSE treatment in presence and absence of KO2 (n = 3 PCLS each, except n = 4 PCLS for Noxo1–/– from 3–4 mice). e, ROS production of WT Noxo1 and mutated Noxo1 determined by chemiluminescence with L-012 (n = 3 biologic replicates). f, Late apoptosis and necrosis of Noxo1–/– PCLS after CSE treatment after transfection with WT Noxo1 and mutated Noxo1 (n = 4 PCLS from 4 mice each). g, Volcano plot of genes regulated in septae of 8 months smoke-exposed (SE) Noxo1–/– mice compared with 8 months smoke-exposed WT mice, corrected for gene regulation in room air (RA) exposed Noxo1–/– mice compared with room air-exposed WT mice (n = 5 lungs each). h, Mitochondrial respiration in A549 cells treated with CSE after knockdown of NOXO1 by siRNA or application of control scrambled (scr) siRNA (n = 7 biologic replicates each for scr siRNA and n = –8 for siRNA NOXO1). Omy: Oligomycin, FCCP: Carbonyl cyanide-4-(trifluoromethoxy)phenylhydrazone i, Noxo1 mRNA level in PASMCs of WT and AOX expressing (Aoxtg) mice (n = 14 cell isolations each, except n = 13 for control Aoxtg) j, NOXO1 mRNA level in A549 cells expressing Aox or a non-functional mutated Aox plasmid (n = 3 biologic replicates). Statistical analysis: a, c, h: 2 × 2 factorial models on log-transformed data; p-values are from 2-sided t-tests. b, d: 3-factorial linear mixed model on log-transformed data using the subject (mouse) as random factor; p-values are from Chi-squared tests. e: one-factorial linear model on log-transformed data; p-values are from two-sample t-test f: 2-factorial linear mixed model on log-transformed data using the subject (mouse) as random factor; p-values are from Chi-squared tests. i, j: 2 × 2 factorial models on the ΔCt values; p-values are from two-sided t-tests. Data are represented as single value and mean ± s.e.m.
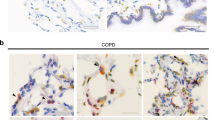
Extended Data Fig. 9 Co-staining of human lung tissue from donor lungs and COPD patients with anti-NoxO1 (light blue), anti-nitrotyrosine (red) and nuclear staining with hematoxylin (dark blue).
Arrows indicate alveolar structures, asterisks show vessels/bronchi; magnification 400×. n = 3 lungs each.
Supplementary information
Supplementary Information
Supplementary Discussion, Supplementary Methods and Supplementary Tables 1–6
Source data
Source Data Fig. 1
Statistical source data
Source Data Fig. 2
Statistical source data
Source Data Fig. 2
Unprocessed western blots
Source Data Fig. 3
Statistical source data
Source Data Fig. 4
Statistical source data
Source Data Fig. 5
Statistical source data
Source Data Fig. 5
Unprocessed western blots
Source Data Fig. 6
Statistical source data
Source Data Fig. 7
Statistical source data
Source Data Fig. 7
Unprocessed western blots and gels
Source Data Extended Data Fig. 1
Statistical source data
Source Data Extended Data Fig. 1
Unprocessed western blots
Source Data Extended Data Fig. 2
Statistical source data
Source Data Extended Data Fig. 2
Unprocessed western blots
Source Data Extended Data Fig. 3
Statistical source data
Source Data Extended Data Fig. 4
Statistical source data
Source Data Extended Data Fig. 5
Statistical source data
Source Data Extended Data Fig. 6
Statistical source data
Source Data Extended Data Fig. 7
Statistical source data
Source Data Extended Data Fig. 8
Statistical source data
Rights and permissions
About this article
Cite this article
Seimetz, M., Sommer, N., Bednorz, M. et al. NADPH oxidase subunit NOXO1 is a target for emphysema treatment in COPD. Nat Metab 2, 532–546 (2020). https://doi.org/10.1038/s42255-020-0215-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s42255-020-0215-8
This article is cited by
-
TRAIL protects the immature lung from hyperoxic injury
Cell Death & Disease (2022)
-
NADPH oxidase family proteins: signaling dynamics to disease management
Cellular & Molecular Immunology (2022)