Abstract
To elucidate the molecular pathogenesis of pediatric germ cell tumors (GCTs), we performed DNA methylation array analysis, whole transcriptome sequencing, targeted capture sequencing, and single-nucleotide polymorphism array analysis using 51 GCT samples (25 female, 26 male), including 6 germinomas, 2 embryonal carcinomas, 4 immature teratomas, 3 mature teratomas, 30 yolk sac tumors, and 6 mixed germ cell tumors. Among the 51 samples, 11 were from infants, 23 were from young children, and 17 were from those aged ≥10 years. Sixteen of the 51 samples developed in the extragonadal regions. Germinomas showed upregulation of pluripotent genes and global hypomethylation. Pluripotent genes were also highly expressed in embryonal carcinomas. These genes may play essential roles in embryonal carcinomas given that their binding sites are hypomethylated. Yolk sac tumors exhibited overexpression of endodermal genes, such as GATA6 and FOXA2, the binding sites of which were hypomethylated. Interestingly, infant yolk sac tumors had different DNA methylation patterns from those observed in older children. Teratomas had higher expression of ectodermal genes, suggesting a tridermal nature. Based on our results, we suggest that KIT, TNFRSF8, and ERBB4 may be suitable targets for the treatment of germinoma, embryonal carcinomas, and yolk sac tumors, respectively.
Similar content being viewed by others
Introduction
Germ cell tumors (GCTs) are relatively rare in pediatric patients, and the incidence rates are 5.3 and 4.4 per million in girls and boys, respectively1. GCTs usually exhibit a bimodal age distribution with two peaks in infancy and young adolescence2. The survival rate of patients is excellent (>90%)1. However, in some cases, GCTs are refractory to treatment, including intensive chemotherapy3. Therefore, a novel treatment strategy should be established for chemotherapy-resistant GCTs. Additionally, a new approach of treatment may even be required for chemotherapy-sensitive GCTs. It has been found that survivors of pediatric cancer suffer from late complications induced by anticancer cytotoxic agents4. Therefore, we should elucidate the molecular pathogenesis of GCTs and develop novel therapies based on it.
GCTs develop from primordial germ cells (PGCs). PGCs develop in the yolk sacs of embryos during the embryonic period and migrate to gonads through the midline of the body5. As PGCs migrate to the gonads, they undergo DNA methylation erasure6. In this process, the KIT and CXCR4 pathways are associated with proliferation and migration, respectively7. After migration, PGCs reestablish their DNA methylation and differentiate into sperms or eggs depending on the sex of the individual8. Migrating PGCs are chromosomally unstable due to DNA hypomethylation and are prone to developing copy number abnormalities or mutations9. Although such aberrated PGCs are eliminated via apoptosis, a minority of aberrated PGCs survive and give rise to GCTs10. GCTs develop in the gonads and extragonads11, such as the central nervous system (CNS), mediastinum, or sacrococcygeal regions, which are thought to be the migration routes of PGCs. While GCTs include several subtypes, such as seminoma, yolk sac tumors (YSTs), or embryonic carcinomas (ECs), they are dependent on the differential stages of PGCs10.
In adults, the most common subtype of testicular GCTs is an immature type of GCT called seminoma12. Seminomas frequently exhibit an isochromosome of the short arm of chromosome 12 (isochromosome 12p) as well as mutations in KIT and RAS13. Because seminomas comprise neoplastic counterparts of PGCs, they exhibit global DNA hypomethylation14. Immature types of GCTs in the ovary and CNS are known as dysgerminomas and germinomas, respectively. In this study, dysgerminomas, seminomas, and CNS germinomas were all classified as germinomas. Because they also commonly retain global DNA hypomethylation, isochromosome 12p, and KIT or RAS mutations15,16,17,18, these tumors could have similar biological characteristics to seminomas. In fact, as isochromosome 12p is detected in adult GCTs regardless of their subtypes, it is considered to be one of the critical factors responsible for the development of GCTs. Additionally, DNA methylation aberrations could be associated with the development of GCTs owing to the dynamics of DNA methylation. In YSTs, several tumor-suppressor genes (such as RASSF1 or APC) are hypermethylated14,19. These reports suggest that DNA methylation aberrations, in addition to copy number abnormalities and mutations, contribute to the development of GCTs. Several studies have investigated genomic abnormalities in pediatric GCTs20,21; however, a comprehensive genomic analysis of pediatric GCTs has not been performed. Therefore, using 51 pediatric GCT samples, we performed a comprehensive genetic/epigenetic analysis including DNA methylation array, whole-transcriptome sequencing, single-nucleotide polymorphism (SNP) array, and targeted capture sequencing to obtain a better understanding of the molecular pathogenesis of pediatric GCTs.
Our comprehensive analyses profiled genetic and epigenetic characteristics in each subtype of pediatric GCTs. Germinomas showed upregulation of pluripotent genes and global hypomethylation. Pluripotent genes were also highly expressed in ECs. These genes may play essential roles in ECs given that their binding sites are hypomethylated. YSTs exhibited overexpression of endodermal genes, such as GATA6 and FOXA2, the binding sites of which were hypomethylated. Interestingly, infant YSTs had different DNA methylation patterns from those observed in older children. Teratomas had higher expression of ectodermal genes, suggesting a tridermal nature. Based on our results, we suggest that KIT, TNFRSF8, and ERBB4 may be suitable targets for the treatment of germinoma, ECs, and YSTs, respectively.
Results
A total of 51 patients with pediatric GCT (Table 1 and Supplementary Data 1) were enrolled in this retrospective study. All samples were collected from the University of Tokyo Hospital and associated hospitals. All patients received carboplatin-based chemotherapy at each hospital. Our cohort included 6 patients with germinomas, 2 with ECs, 4 with immature teratomas, 3 with mature teratomas, 30 with YSTs, and 6 with mixed germ cell tumors (MGCTs). Among these 51 samples, 16 developed in the extragonadal regions. The male-to-female ratio of our cohort was almost similar (26 males and 25 females). Among the 51 samples, 11 were from infants, 23 were from those aged 1 to <10 years, and 17 were from those aged ≥10 years. The ages ranged from 2 months to 19 years, with a median age of 2 years. The overall prognosis was excellent, with three recurrences and two deaths reported.
DNA methylation analysis
The density plot of each subtype revealed that germinomas were hypomethylated versus other subtypes (Supplementary Fig. 1). Consensus clustering of our cohort revealed that our samples were divided into two clusters: M1 and M2 (Fig. 1a and Supplementary Data 2). While the M1 cluster included several subtypes, the M2 cluster included almost all YSTs. MGCTs were clustered depending on the main subtypes. The two clusters were stable, and YSTs occupied two-third of our cohort. Actually, clustering based on the same probe sets (Supplementary Data 1) separated the open data22 of GCTs into YSTs and other subtypes (Supplementary Fig. 2). In a previous report14, differentially methylated regions (DMRs) between M1 and M2 showed that the tumor-suppressor genes, such as RASSF1, RUNX3, HIC1, or APC, were hypermethylated in M2, namely, in YSTs (Fig. 1b and Supplementary Data 3). Locus overlap analysis (LOLA) revealed that the binding sites of endodermal differential factors, particularly those of hepatic factors (e.g., FOXA2 and HNF4A), were hypomethylated (Fig. 1c and Supplementary Data 4). In addition, the binding sites of GATA6 were hypomethylated in M2. The open data of adult YSTs also showed hypomethylation of the binding sites of GATA6, FOXA2, and HNF4A23 (Supplementary Fig. 3).
a DNA methylation clustering in 51 GCT samples on unsupervised consensus clustering. Consensus clustering revealed that GCT samples were divided into two clusters: M1 and M2. While M1 included several subtypes except YSTs, M2 included almost all YSTs. MGCTs were clustered depending on the main subtypes. DNA methylation clusters, subtypes, age at onset, sex, primary developing sites, and types are shown by colors as indicated. MGCTs are also annotated by their main subtypes. b Volcano plot comparing significant delta–beta values between M1 and M2 clusters. Differentially methylated probes showing a delta–beta value >0.25 or <−0.25 and −log10 (q-value) >10 are colored in orange. Among these significant probes, the probes of the promoter regions of tumor-suppressor genes are colored in red. q-values are calculated using the Wilcoxon rank-sum test after adjusting by Benjamini–Hochberg correction. c The result of locus overlap analysis between M1 and M2 clusters. Colored dots represent ChIP-seq experiments for transcription factors. Dot size denotes the log-odds ratio. Among these dots, the dots of endoderm differentiation factors are colored in red. The binding sites of FOXA1, HNF4A, FOXA2, GATA6, EP300, ESR1, GATA3, and CEBPA were hypomethylated in the M2 (YST) cluster.
We performed a second consensus clustering of the M1 samples to determine the methylation profiles of the GCT subtypes in the M1 cluster as well as a second consensus clustering of the M2 samples so as to further classify the YST samples in the M2 cluster. The second consensus clustering of the M1 and M2 samples revealed that the M1 samples were divided into germinomas (M1A cluster) and other subtypes (M1B cluster), whereas the M2 samples were divided into two YSTs clusters: M2A and M2B (Fig. 2a and Supplementary Data 5 and 6). Consensus clustering revealed that methylation profiles depended on the histological subtypes, consistent with the findings of previous studies20,24. Thus comparing each subtype with other subtypes led to the detection of DMRs in each subtype. However, characteristic DMRs were not detected owing to hypomethylation of almost all genes of germinomas (M1A). While M1B included several subtypes, such as ECs, immature teratomas, and mature teratomas, DMRs were determined by each subtype. In ECs, the binding sites of pluripotency factors, such as NANOG, POU5F1, and SOX2, were hypomethylated (Fig. 2b and Supplementary Data 7). The open data of adult ECs also showed hypomethylation of the binding sites of NANOG, POU5F1, and SOX223 (Supplementary Fig. 4). We did not identify characteristic DMRs of teratomas compared with other subtypes and DMRs between mature and immature teratomas24. The M2 cluster was divided into two clusters: M2A and M2B. Comparison of M2A with M2B samples revealed slight hypermethylation in the latter (Supplementary Fig. 5). LOLA revealed that M2B samples had hypomethylation of the binding sites of EZH2 or RBBP5 in ES cells (Fig. 2c and Supplementary Data 8). This result suggests that M2B samples possess unique methylation patterns different from those observed in M2A samples.
a DNA methylation clustering in 21 samples of the M1 cluster (left panel) and in 30 samples of the M2 cluster (right panel) on unsupervised consensus clustering. A second consensus clustering revealed that M1 and M2 are further divided into two clusters. M1 cluster are separated into germinomas (M1A) and ECs and teratomas (M1B) clusters. M2 clusters are divided into adult-type (M2A) and infant-type (M2B) YSTs. DNA methylation clusters, subtypes, age at onset, sex, primary developing sites, and types are shown by colors as indicated. b Result of locus overlap analysis between embryonal carcinomas and other subtypes. Colored dots represent ChIP-seq experiments for transcription factors. Dot size denotes the log-odds ratio. Among these dots, those of pluripotency factors are colored in red. The binding sites of NANOG, POU5F1, SOX2, and CBFB were hypomethylated in embryonal carcinomas. c Result of locus overlap analysis between adult-type (M2A) and infant-type (M2B) YSTs. Colored dots represent ChIP-seq experiments for transcription factors. Dot size denotes the log-odds ratio. Among these dots, those of embryonic stem cells are colored in red. Infant-type YST has partially common methylation pattern with ES cells.
Expression analysis
Expression analysis showed that GCTs were divided into three clusters (Fig. 3a and Supplementary Data 9). The result of clustering based on expression also correlated with the histological subtypes. E1 included germinoma and EC samples, E2 included all teratoma samples, and E3 included all YSTs.
a Expression clustering in 49 GCT samples on unsupervised consensus clustering. Consensus clustering revealed that GCT samples are divided into three clusters: E1, E2, and E3. E1 included all germinomas and embryonal carcinomas. E2 included all teratomas. E3 included all yolk sac tumors. As with DNA methylation clustering, expression clustering correlated with histological subtypes. MGCTs were clustered dependent on the main subtypes. DNA methylation clusters, subtypes, age at onset, sex, primary developing sites, and types are shown by colors as indicated. b FPKM values of GATA6 in subtypes of GCTs and PGCs of the open data set. GATA6 is significantly highly expressed in YSTs than in PGCs. c Schematic representation of the MSH2–EPCAM fusion gene. The exon 4 of MSH2 is connected with the exon 7 of EPCAM. Because MSH2 loses MSH3/MSH6 interaction and MutL homologs interaction domains, MSH2 loses its function.
E1 was characterized by a higher expression of pluripotency factors, including POU5F1 or NANOG (Supplementary Fig. 6a), which was concordant with previous reports25,26. Expression analysis revealed that the EC samples were clustered with germinoma samples because they also exhibited higher expression of pluripotency factors. Notably, in DNA methylation clustering, EC samples were clustered with teratomas. Additionally, the MGCT sample including the EC component was also clustered into E1. Comparing ECs with germinomas in cluster E1, ECs overexpressed SOX2, GDF3, and TNFRSF827 (Supplementary Fig. 6b). In addition, DPPA3 and KIT were highly expressed in ECs28 and germinomas, respectively, although the difference was not significant due to the small sample size.
Mature teratomas, immature teratomas, and MGCTs, which included the teratoma component, were clustered into E2. Analysis of differential expression genes revealed that ectodermal genes, particularly the neuroectodermal genes, were highly expressed in teratomas (Supplementary Fig. 6c). Tumorigenic genes associated with the development of teratoma were not detected in genes exhibiting higher expression in E2. Comparison of immature teratomas with mature teratomas revealed that the former had higher SOX2 expression, suggesting their immaturity.
E3 included YSTs and MGCTs with the YST component; therefore, the expression characteristics of MGCT samples in cluster E3 were similar to those of YST. YST samples overexpressed endodermal induction genes, such as FOXA2 or HNF4A and GATA6 (Supplementary Fig. 6d)21. Actually, because the expression of GATA6 was not detected in the open data of PGC in fetuses29, the expression of GATA6 would be specific for YSTs (Fig. 3b). Pathway analysis revealed activation of the transforming growth factor-β signaling pathway in YSTs, similar to the findings of a previous report21, which was concordant with the hypermethylation of RUNX3 and APC (Supplementary Data 10). Additionally, ERBB4 was highly expressed in YSTs regardless of the regions of development or the age at onset. Analysis of differentially expressed genes between the M2A and M2B clusters in DNA methylation did not detect specific genes associated with pathogenicity. RNAseq also revealed that one YST sample carried the EPCAM–MSH6 fusion gene (Fig. 3c).
Copy number and mutational analyses
Copy number and mutational analyses revealed that each subtype had characteristic copy number alterations (Fig. 4) and mutations (Supplementary Data 11). In general, gaining of the long arms of chromosome 20 was the most frequently detected copy number alterations in 29 of the 51 GCT samples regardless of the histological subtypes, except teratomas. In addition to 20q, gaining of the short arms of chromosome 12 was also frequently detected in 20 of the 51 GCT samples. Among these 20 samples, 8 samples carried isochromosome 12p (Supplementary Fig. 7). All samples with isochromosome 12p belonged to children aged >10 years.
DNA methylation clusters, subtypes, age at onset, sex, primary developing sites, and types are shown by colors as indicated. Germinomas show chromosomal gains in nearly all chromosomes or KIT mutations. Two ECs have isochromosome 12p and gains of chromosome 7. Teratomas do not reveal specific mutations or copy number changes except global UPD in ovarian teratomas. YSTs exhibit gains of chromosome 1q, 12p, and 20q; losses of 1p, 4p, 6p, and 16; and partial UPD. Some YST samples possess KIT mutation; KRAS mutations; and NRAS mutation, TP53 mutations, or MDM2 amplifications.
While two germinoma samples showed chromosomal gains in nearly all chromosomes, other germinoma samples had fewer copy number alterations. Gains in chromosomes 1q, 7, 8, 10q, 12p, 20q, and 21q were detected in five of six germinoma samples. In our cohort, none of the germinoma sample possessed isochromosome 12p, which is often detected in adult germinomas30. Two germinoma samples had more than four copies of chromosome 12p, and these two germinoma samples did not have KIT mutations. In contrast, all germinoma samples with three or fewer copies of chromosome 12p carried activating mutation in KIT, which is one of the most frequently mutated genes detected in adult germinomas31. Two germinoma samples with more than four copies of chromosome 12p also gained the long arms of chromosome 4, which included KIT.
Although none of the EC samples carried mutations, they recurrently showed isochromosome 12p as well as gains of chromosome 7 and 8q. Expression analysis revealed that GDF3 and genes were highly expressed in ECs and were located in chromosome 12p23. Overexpression of these genes might be associated with gains of chromosome 12p.
Although teratomas did not exhibit characteristic copy number alterations or mutations, ovarian teratomas had global uniparental disomies (UPDs; Supplementary Fig. 8). Global UPD in ovarian teratomas was frequently found in adult ovarian teratomas32.
In 30 YST samples, gains of chromosome 1q (14 samples), 12p (nine samples), and 20q (23 samples); losses of 1p (17 samples), 4q (13 samples), 6q (13 samples), and 16 (13 samples)33; and partial UPD or uniparental trisomies (UPT) (11 samples) were frequently observed. There were several differences between the M2A and M2B cluster samples according to DNA methylation analysis. While the M2A cluster samples had more partial UPD or UPT, the M2B cluster samples had more 1q gains. Isochromosome 12p in YST samples was detected only in older children. Furthermore, two of the three YST samples with chromosomal gains in nearly all chromosomes developed in older children. While UPD or UPT was detected in the gonadal or extragonadal samples of male YST samples, only UPD was detected in the gonadal samples of female YST samples. In particular, ovarian YST samples showed global UPD similar to ovarian teratomas (Supplementary Fig. 9). In YST samples, KIT, KRAS, and NRAS mutations were detected in one, two, and one sample, respectively. These samples belonged to children aged >10 years. MGCT samples correlated with the mixture of several subtypes and possessed copy number alterations characteristic of each subtype.
Nonsynonymous TP53 mutations were detected in one YST (NM_001126114: p.C141Y) and one MGCT (NM_001126114: p.E11Q) sample belonging to children aged >10 years and developed in the mediastinum. The gains of MDM2 were detected in six YST samples, which highly expressed MDM2 versus other samples (Supplementary Fig. 10).
Discussion
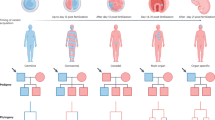
Our comprehensive analysis demonstrated that pediatric GCTs had characteristic genomic aberrations based on their developmental processes (Fig. 5).
PGCs develop in the yolk sacs of embryos in the embryonic period and migrate to gonads through the midline of the body. As PGCs migrate to gonads, they undergo DNA methylation erasure, including imprinting regions and basal methylation. With GCT core methylation and subtype-specific methylation, infant GCTs and type I GCTs develop from primed PGCs, which are partially demethylated PGCs. After migration and complete DNA demethylation, PGCs reestablish their DNA methylation and express pluripotent genes. PGCs expressing pluripotency genes gain additional genomic abnormalities, such as KIT mutation or 12p gain, and develop into germinomas. PGCs expressing pluripotent genes further reestablish DNA methylation and express DPPA3. PGCs expressing DPPA3 sometimes gain isochromosome 12p and develop into ECs. PGCs expressing DPPA3 further reestablish DNA methylation and differentiate into sperms or eggs dependent on each sex. On the way of differentiation, PGCs gaining additional genomic abnormalities develop into YSTs or teratomas. As type II EC, YST, and teratoma possessed sex-specific imprinting in the analysis of imprinting regions, these tumors are shown by each sex. This figure does not include type II GCTs developed in the extragonads.
As germinomas showed global hypomethylation and higher expression levels of pluripotency factors (e.g., POU5F1 or NANOG), they could develop from immature PGCs14,22. Although DNA methylation and expression analyses revealed that germinomas were uniform, copy number and mutational analyses could separate germinomas into two types. The first type possessed activating KIT mutations and fewer copy number alterations, suggesting that the activation of the KIT pathway was essential for some germinomas. The second type exhibited chromosomal gains in nearly all chromosomes without KIT mutations. These two types were mutually exclusive in our cohort. However, the expression levels of KIT were similar between the two types of germinomas. The karyotypes of the second type were near triploid or tetraploid, and these karyotypes were reported in adult GCTs34. Different from the germinomas in our cohort, most adult seminomas carried isochromosome 12p13, and some seminomas with isochromosome 12p retained activating KIT mutations, suggesting that the acquisition of isochromosome 12p precedes that of KIT mutations. In our cohort, five of the six germinoma samples had 12p gains. Among the five samples, two had more than four copies of 12p without KIT mutations. Therefore, a larger number of 12p copies may be able to cause the development of germinomas similar to that caused by KIT mutations; however, we did not identify any other causative genes except KIT. In this study, the outcome of germinomas was excellent; nevertheless, some adult germinomas are refractory to chemotherapy35. In pediatric intracranial germinomas, KIT-mutated cases were linked to worse prognosis22. The KIT inhibitor, avapritinib, is effective for the treatment of systemic mastocytosis with KIT D816 mutations36. Therefore, avapritinib may also be a promising therapeutic option for germinomas with KIT mutations.
ECs exhibited more methylated regions and higher expression of DPPA3 than germinomas; therefore, it was concluded that ECs developed from differentiated PGCs23. The observed overexpression of pluripotency factors and hypomethylation of their binding sites suggest that these factors play essential roles in ECs. The presence of the expression of pluripotency factors indicated the immature states of the ECs. Other cancers (e.g., renal cell carcinoma) with higher expression of pluripotency factors are linked to worse prognosis37. The worse prognosis of ECs in non-seminomas38 may also be associated with pluripotency factors. Because TNFRSF8 was highly expressed in ECs in our cohort, brentuximab may be a promising option for the treatment of refractory ECs. While copy number abnormalities induce the expression of TNFRSF839, other subtypes with complexed copy number abnormalities did not cause this effect. This finding suggests that TNFRSF8 expression is characteristic to ECs. Although ECs in our cohort did not possess mutations and adult ECs rarely have driver mutations13, most ECs carry isochromosome 12p23. Therefore, the present results imply that 12p gains may be indispensable for the development of ECs because 12p includes various genes associated with cancer (e.g., DPPA3, GDF3, KRAS, or CCND2).
Owing to the suppression of pluripotency factors, other nonseminomatous subtypes would be more differentiated than ECs. The teratomas in our cohort had similar DNA methylation and expression profiles. Compared with other subtypes, teratomas had higher expression of ectodermal genes, particularly of neuroectodermal genes, because they were tridermal tumors. In contrast, copy number analysis showed that only ovarian teratomas had global UPDs, suggesting the parthenogenetic development of ovarian teratomas40. Because teratomas had similar genomic profiles regardless of the presence or absence of UPDs, imprinting genes may play limited roles in the development of teratomas.
YSTs overexpressed endodermal genes (e.g., FOXA2 or HNF4A) and extraembryonic genes (e.g., GATA6)41. DNA methylation analysis revealed that the binding sites of these genes were hypomethylated; therefore, these genes would play fundamental roles in YSTs in a similar manner to pluripotency factors in ECs. GATA6 is particularly important among these genes because it is the master regulator of the differentiation of extraembryonic tissues and induces the differentiation of extraembryonic tissues, such as yolk sacs42 during the embryonic period. Pathway analysis showed activation of the transforming growth factor-β pathway in YSTs, which is associated with the overexpression of GATA6 and FOXA2 and the hypermethylation of tumor-suppressor genes (e.g., RASSF1, RUNX3, HIC1, or APC). Additionally, ERBB4 was also upregulated in YSTs. Because ERBB4 inhibition is effective for the treatment of breast cancer43, it may also be a promising therapeutic option against YSTs. The EPCAM–MSH6 gene fusion detected in one YST sample is one of the causative genes of Lynch syndrome, which may be a risk factor of the development of adult testicular GCTs44.
DNA methylation analysis divided the YST samples into two clusters: M2A and M2B; however, the expression profiles of these two types were similar. While the M2A cluster included almost all type II YST and mediastinal samples, the M2B cluster included all type I YST and sacrococcygeal samples. Generally, type I and type II GCTs are pediatric and adult types, respectively. In addition, all sacrococcygeal GCTs were of the infant type, and mediastinal GCTs were rare in children. Thus samples from the M2A and M2B clusters could be the so-called adult and infant GCTs, respectively. While infant GCTs developed from migrating PGCs undergoing DNA methylation erasure, adult GCTs developed from PGCs reestablishing DNA methylation. These results imply differences in DNA methylation between adult and infant GCTs. Consistent with this prediction, comparison between M2A and M2B samples revealed slight hypermethylation in the latter.
Copy number status was partly different between infant- and adult-type YSTs. In addition, ovarian YSTs showed global UPD similar to ovarian teratomas. Therefore, ovarian YSTs and teratomas may have the same origin because type I MGCTs (including YSTs and teratomas) were frequently detected in the pediatric type. Actually, a previous report identified the stem cells of type I GCTs45.
KIT, KRAS, and NRAS mutations were detected in one, three, and one YST sample, respectively. Although the frequency of gene mutations was low, mutations in these genes may be additional drivers for the development of YSTs.
Based on DNA methylation analysis, one YST sample was classified in the M1 cluster. While this particular sample showed higher expression of GATA6, FOXA2, or HNF4A and hypermethylation of RASSF1, RUNX3, HIC1, or APC, its methylation pattern was partially common to that of germinomas or ECs. Review of the pathological specimens of this particular sample showed that this particular sample contained syncytiotrophoblastic giant cells (STGCs) but not other histological components. Because STGCs are often detected in germinomas, germinomas may be incorporated into this particular YST sample. In addition to the histological involvement of STGCs, this sample possessed a TP53 mutation and was developed in the mediastinum of a patient aged >10 years. Such YSTs may have a unique profile. As MGCTs in older children also carries the TP53 mutation, mediastinal GCTs in older children exhibit a higher frequency of TP53 mutations (similar to adult GCTs46). Thus older children may be at a higher risk of mediastinal GCTs, similar to adults, because TP53-mutated GCTs are refractory to chemotherapy46.
Our study has some limitations. First, it was unclear whether we correctly characterized the genomic and epigenomic status of each subtype because the sample size was small, except for YSTs. In particular, the identification of the subtype refractory to convention chemotherapy remains unclear. TP53 mutations or EC subtypes might be refractory to conventional chemotherapy as discussed above. However, considering that TP53 mutations and EC subtypes are more common in adults, the worse prognosis of these subtypes in our cohort may be correlated with differences between pediatric and adult GCTs. Thus future larger-scale studies are needed to verify our speculations. Second, the genomic and epigenomic statuses of intracranial GCTs were also unclear as intracranial GCTs were not included in this study. However, analysis using the open data set of DNA methylation data of intracranial GCTs and testicular GCTs revealed that these GCTs had a similar DNA methylation pattern according to each subtype. Therefore, GCTs could have similar biological profiles according to each subtype regardless of the primary site. Third, although the reproducibility of our results could not be confirmed using the open data sets of GCTs, our analysis possesses a certain validity given that LOLA and clustering based on DNA methylation revealed that our cohorts and the open data set had similar results.
In conclusion, our comprehensive genomic/epigenomic analyses identified the characteristics of pediatric GCTs, and each subtype possessed unique characteristics. Although pediatric GCTs are associated with favorable prognosis, some pediatric GCTs such as TP53 mutations or EC subtype as shown in our analysis are refractory to conventional chemotherapy. For such cases, the molecular targets detected through our comprehensive genomic/epigenomic analyses may be promising therapeutic options. Therefore, additional studies are warranted to confirm the efficacy of these molecular targeted agents in patient-derived cell lines or xenograft models and to assess their effectiveness in clinical trials.
Methods
Patients and materials
All samples were collected from the University of Tokyo Hospital and associated hospitals. Tumor samples were collected after obtaining written informed consent from the legal guardians of the patients according to protocols approved by the Human Genome, Gene Analysis Research Ethics Committee of the University of Tokyo, and other participating institutions. All protocols conformed to the tenets of the Declaration of Helsinki. This retrospective study enrolled 51 patients with type I (infant-type) and type II (adult-type) extracranial GCTs (Supplementary Data 1)47. Moreover, dysgerminomas, seminomas, and CNS germinomas were all classified as germinomas.
Statistics
Statistical analyses were performed using the R software version 3.5.1 (https://www.R-project.org/).
DNA methylation analysis
Comprehensive DNA methylation analysis was performed using 51 samples of GCTs with the Infinium methylationEPIC Kit (Illumina, San Diego, CA, USA) according to the manufacturer’s instructions. Quality control, signal correction, and methylation beta value calculation were performed using the Bioconductor package ChAMP version 2.10.1. Differentially methylated CpG probes were ranked according to adjusted P values calculated by fitting linear models. For clustering, beta-values were corrected for probe design bias using a beta-mixture quantile normalization method48 and then converted to M-values49. Thereafter, the R package pcaMethods 1.68.0 was used to impute incomplete M-values, which were subsequently converted to beta-values. Imputed beta-values were later used for further analyses. For the determination of DNA methylation profiles, the following steps were adopted to select probes for unsupervised consensus clustering. Initially, we removed probes that were designed for sequences on the X and Y chromosomes. Subsequently, we selected probes annotated as promoter-associated CpG islands according to Illumina (Illumina, San Diego, CA, USA). We then performed unsupervised consensus clustering using the Ward’s method. Cluster stability was determined via consensus clustering with 1000 iterations using the R package ConsensusClusterPlus 1.40.0. Heat maps were generated using the R package pheatmap 1.0.7 using beta-value data. Statistical significance was assessed using Wilcoxon’s rank-sum test, and values were corrected by employing the Benjamini–Hochberg method. LOLA was performed using the R package LOLA 1.14.0.
Next-generation sequencing (NGS)
NGS was performed using the Illumina HiSeq 2000 or 2500 platform (Illumina, San Diego, CA, USA) with a standard 126-bp paired-end read protocol according to the manufacturer’s instructions.
RNA sequencing
High-quality RNA samples were isolated from 49 GCTs (RNA integrity number equivalent >5.5) using the Agilent TapeStation (Agilent Technologies, Santa Clara, CA, USA). These samples were used to prepare libraries for RNA sequencing using the NEBNext Ultra RNA Library Prep Kit for the Illumina platform (New England BioLabs, Ispwich, MA, USA). Fusion transcripts were detected using the Genomon version 2.5.3 (https://github.com/Genomon-Project/) and were filtered by excluding fusion mapping to repetitive regions, those with fewer than seven spanning reads, those occurring out of frame, or those with junctions not located at known exon–intron boundaries. Normalized count data obtained using the variance-stabilizing transformation function of the DESeq2 R package (1.16.1) were used for clustering analysis. For this analysis, we performed unsupervised consensus clustering using the Ward’s method. Heat maps were generated using the R package pheatmap version 1.0.7 using the variance-stabilizing transformation count data. Statistical significance was assessed using the Wilcoxon’s rank-sum test, and values were corrected by employing the Benjamini–Hochberg method.
Copy number analysis
DNA samples were processed via SNP array analysis using the Affymetrix GeneChip 250K Nsp or CytoScan HD (Affymetrix, Santa Clara, CA, USA) according to the protocol provided by the manufacturer. Informatics analysis of the SNP array data was conducted using the CNAG/AsCNAR software, which enables the accurate detection of allelic status without paired normal DNA, even in the presence of up to 70–80% normal cell contamination50. Isochromosome 12p was confirmed when a sample had two more copies of 12p than of 12q. To confirm the copy number abnormalities detected using the SNP array, NGS-based copy number analyses were also performed in all samples using the in-house pipeline, CNACS51, which enable digital karyotyping.
Targeted capture sequencing
The DNA isolated from 51 GCT samples was analyzed via targeted capture sequencing using a SureSelect XT Custom Kit (Agilent Technologies) according to the manufacturer’s protocol. Our custom bait library (U-Tokyo Onco-panel ver.1) was designed for mutation profiling of pediatric cancers, including 381 targeted genes and regions (Supplementary Data 12). Sequence alignment and detection of gene mutations and structural variations were performed using our in-house pipeline, Genomon v.2.5.3.
Mutational analysis
Gene mutations identified using the Genomon pipeline were first filtered to exclude sequencing/mapping errors and mutations of unknown significance using the following criteria: (i) including only exonic and splicing regions; (ii) excluding known variants listed in the 1000 Genomes Project (Nov 2010 release), National Center for Biotechnology Information SNP database (build 131), or National Heart, Lung, and Blood Institute Exome Sequencing Project 5400; (iii) excluding read depths <50; (iv) excluding unidirectional reads; (v) including variants with P value <10−60 through Empirical Bayesian mutation Calling52; and (vi) including variants showing “H,” “M,” or “L” in the MutationAssessor. Moreover, mapping errors were removed via visual inspection of the Integrative Genomics Viewer browser.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
All sequencing data supporting these findings, including DNA methylation arrays, RNA sequencing, targeted capture sequencing, and SNP arrays, were deposited in the DNA Data Bank of Japan and are accessible through accession number JGAS00000000204. All relevant data are available from the authors upon request.
References
Kaatsch, P., Häfner, C., Calaminus, G., Blettner, M. & Tulla, M. Pediatric germ cell tumors from 1987 to 2011: incidence rates, time trends, and survival. Pediatrics 135, e136–e143 (2015).
Poynter, J. N., Amatruda, J. F. & Ross, J. A. Trends in incidence and survival of pediatric and adolescent patients with germ cell tumors in the United States, 1975 to 2006. Cancer 116, 4882–4891 (2010).
Rashdan, S. & Einhorn, L. H. Salvage therapy for patients with germ cell tumor. J. Oncol. Pract. 12, 437–443 (2016).
Skinner, R., Wallace, W. H. B., Levitt, G. A. & UK Children’s Cancer Study Group Late Effects Group Long-term follow-up of people who have survived cancer during childhood. Lancet Oncol. 7, 489–498 (2006).
Fujimoto, T., Miyayama, Y. & Fuyuta, M. The origin, migration and fine morphology of human primordial germ cells. Anat. Rec. 188, 315–330 (1977).
Kim, S. et al. PRMT5 protects genomic integrity during global DNA demethylation in primordial germ cells and preimplantation embryos. Mol. Cell 56, 564–579 (2014).
Richardson, B. E. & Lehmann, R. Mechanisms guiding primordial germ cell migration: strategies from different organisms. Nat. Rev. Mol. Cell Biol. 11, 37–49 (2010).
Hirasawa, R. & Feil, R. Genomic imprinting and human disease. Essays Biochem. 48, 187–200 (2010).
Lee, A. S., Tang, C., Rao, M. S., Weissman, I. L. & Wu, J. C. Tumorigenicity as a clinical hurdle for pluripotent stem cell therapies. Nat. Med. 19, 998–1004 (2013).
Pierce, J. L., Frazier, A. L. & Amatruda, J. F. Pediatric germ cell tumors: a developmental perspective. Adv. Urol. 2018, 9059382 (2018).
Stang, A. et al. Gonadal and extragonadal germ cell tumours in the United States, 1973-2007. Int. J. Androl. 35, 616–625 (2012).
Rajpert-De Meyts, E., McGlynn, K. A., Okamoto, K., Jewett, M. A. & Bokemeyer, C. Testicular germ cell tumours. Lancet 387, 1762–1774 (2016).
Shen, H. et al. Integrated molecular characterization of testicular germ cell tumors. Cell Rep. 23, 3392–3406 (2018).
Rijlaarsdam, M. A. et al. Genome wide DNA methylation profiles provide clues to the origin and pathogenesis of germ cell tumors. PLoS ONE 10, e0122146 (2015).
Kraggerud, S. M. et al. DNA copy number changes in malignant ovarian germ cell tumors. Cancer Res. 60, 3025–3030 (2000).
Hersmus, R. et al. Prevalence of c-KIT mutations in gonadoblastoma and dysgerminomas of patients with disorders of sex development (DSD) and ovarian dysgerminomas. PLoS ONE 7, e43952 (2012).
Fukushima, S. et al. Mutually exclusive mutations of KIT and RAS are associated with KIT mRNA expression and chromosomal instability in primary intracranial pure germinomas. Acta Neuropathol. 127, 911–925 (2014).
de Bruin, T. W. et al. Isochromosome 12p-positive pineal germ cell tumor. Cancer Res. 54, 1542–1544 (1994).
Furukawa, S. et al. Yolk sac tumor but not seminoma or teratoma is associated with abnormal epigenetic reprogramming pathway and shows frequent hypermethylation of various tumor suppressor genes. Cancer Sci. 100, 698–708 (2009).
Williams, L. A. et al. Differences in DNA methylation profiles by histologic subtype of paediatric germ cell tumours: a report from the Children’s Oncology Group. Br. J. Cancer 119, 864–872 (2018).
Palmer, R. D. et al. Pediatric malignant germ cell tumors show characteristic transcriptome profiles. Cancer Res. 68, 4239–4247 (2008).
Fukushima, S. et al. Genome-wide methylation profiles in primary intracranial germ cell tumors indicate a primordial germ cell origin for germinomas. Acta Neuropathol. 133, 445–462 (2017).
Killian, J. K. et al. Imprints and DPPA3 are bypassed during pluripotency- and differentiation-coupled methylation reprogramming in testicular germ cell tumors. Genome Res. 26, 1490–1504 (2016).
Amatruda, J. F. et al. DNA methylation analysis reveals distinct methylation signatures in pediatric germ cell tumors. BMC Cancer 13, 313 (2013).
Santagata, S., Hornick, J. L. & Ligon, K. L. Comparative analysis of germ cell transcription factors in CNS germinoma reveals diagnostic utility of NANOG. Am. J. Surg. Pathol. 30, 1613–1618 (2006).
Skotheim, R. I. et al. Differentiation of human embryonal carcinomas in vitro and in vivo reveals expression profiles relevant to normal development. Cancer Res. 65, 5588–5598 (2005).
Dürkop, H. et al. Expression of the CD30 antigen in non-lymphoid tissues and cells. J. Pathol. 190, 613–618 (2000).
Wongtrakoongate, P., Jones, M., Gokhale, P. J. & Andrews, P. W. STELLA facilitates differentiation of germ cell and endodermal lineages of human embryonic stem cells. PLoS ONE 8, e56893 (2013).
Guo, F. et al. The transcriptome and DNA methylome landscapes of human primordial germ cells. Cell 161, 1437–1452 (2015).
Atkin, N. B. & Baker, M. C. Specific chromosome change, i(12p), in testicular tumours? Lancet 2, 1349 (1982).
Litchfield, K. et al. Whole-exome sequencing reveals the mutational spectrum of testicular germ cell tumours. Nat. Commun. 6, 5973 (2015).
Wang, W. C. & Lai, Y. C. Genetic analysis results of mature cystic teratomas of the ovary in Taiwan disagree with the previous origin theory of this tumor. Hum. Pathol. 52, 128–135 (2016).
Palmer, R. D. et al. Malignant germ cell tumours of childhood: new associations of genomic imbalance. Br. J. Cancer 96, 667–676 (2007).
Oud, P. S. et al. DNA cytometry of pure dysgerminomas of the ovary. Int. J. Gynecol. Pathol. 7, 258–267 (1988).
Rick, O. et al. High-dose chemotherapy as salvage treatment for seminoma. Bone Marrow Transplant. 30, 157–160 (2002).
Lübke, J. et al. Inhibitory effects of midostaurin and avapritinib on myeloid progenitors derived from patients with KIT D816V positive advanced systemic mastocytosis. Leukemia 33, 1195–1205 (2019).
Rasti, A. et al. Co-expression of cancer stem cell markers OCT4 and NANOG predicts poor prognosis in renal cell carcinomas. Sci. Rep. 8, 11739 (2018).
Huang, X., Zhang, R., Mao, Y. & Zhou, L. F. Modified grading system for clinical outcome of intracranial non-germinomatous malignant germ cell tumors. Oncol. Lett. 1, 627–631 (2010).
Herszfeld, D. et al. CD30 is a survival factor and a biomarker for transformed human pluripotent stem cells. Nat. Biotechnol. 24, 351–357 (2006).
Oliveira, F. G. et al. Evidence of parthenogenetic origin of ovarian teratoma: case report. Hum. Reprod. 19, 1867–1870 (2004).
Hwang, J. T. & Kelly, G. M. GATA6 and FOXA2 regulate Wnt6 expression during extraembryonic endoderm formation. Stem Cells Dev. 21, 3220–3232 (2012).
Wamaitha, S. E. et al. Gata6 potently initiates reprograming of pluripotent and differentiated cells to extraembryonic endoderm stem cells. Genes Dev. 29, 1239–1255 (2015).
Rauf, F. et al. Ibrutinib inhibition of ERBB4 reduces cell growth in a WNT5A-dependent manner. Oncogene 37, 2237–2250 (2018).
Huang, D., Matin, S. F., Lawrentschuk, N. & Roupret, M. Systematic review: an update on the spectrum of urological malignancies in Lynch syndrome. Bladder Cancer 4, 261–268 (2018).
Runyan, C., Gu, Y., Shoemaker, A., Looijenga, L. & Wylie, C. The distribution and behavior of extragonadal primordial germ cells in Bax mutant mice suggest a novel origin for sacrococcygeal germ cell tumors. Int. J. Dev. Biol. 52, 333–344 (2008).
Bagrodia, A. et al. Genetic determinants of cisplatin resistance in patients with advanced germ cell tumors. J. Clin. Oncol. 34, 4000–4007 (2016).
Looijenga, L. H., Van Agthoven, T. & Biermann, K. Development of malignant germ cells - the genvironmental hypothesis. Int. J. Dev. Biol. 57, 241–253 (2013).
Teschendorff, A. E. et al. A beta-mixture quantile normalization method for correcting probe design bias in Illumina Infinium 450 k DNA methylation data. Bioinformatics 29, 189–196 (2013).
Du, P. et al. Comparison of Beta-value and M-value methods for quantifying methylation levels by microarray analysis. BMC Bioinformatics 11, 587 (2010).
Yamamoto, G. et al. Highly sensitive method for genomewide detection of allelic composition in nonpaired, primary tumor specimens by use of affymetrix single-nucleotide-polymorphism genotyping microarrays. Am. J. Hum. Genet. 81, 114–126 (2007).
Yoshizato, T. et al. Genetic abnormalities in myelodysplasia and secondary acute myeloid leukemia: impact on outcome of stem cell transplantation. Blood 129, 2347–2358 (2017).
Shiraishi, Y. et al. An empirical Bayesian framework for somatic mutation detection from cancer genome sequencing data. Nucleic Acids Res. 41, e89 (2013).
Acknowledgements
This work was supported by Grants-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (KAKENHI; grant nos. JP17H04224, JP18K19467, and 20H00528 to J.T. and JP26221308 and JP19H05656 to S.O.); Project for Cancer Research and Therapeutic Evolution (P-CREATE; grant no. JP19cm0106509h9904 to J.T.), Project for Development of Innovative Research on Cancer Therapeutics (P-DIRECT; grant no. JP20cm0106501h0005 to S.O.), and Practical Research for Innovative Cancer Control (grant no. JP19ck0106468h0001 to J.T.) from Japan Agency for Medical Research and Development (AMED); Princess Takamatsu Cancer Research Fund (grant to J.T.); and Children’s Cancer Association of Japan (grant to Y Kubota). We are grateful to M. Matsumura, K. Yin, and F. Saito for their excellent technical assistance. We also wish to express our gratitude to M-J. Park (Gunma Children’s Medical Center), K. Koh (Saitama Children’s Medical Center), R. Hanada (Saitama Children’s Medical Center), C. Oyama (Shimane University), T. Taketani (Shimane University), and K. Kato (Ibaraki Children’s Hospital) for sample collection.
Author information
Authors and Affiliations
Contributions
Author contributions are as follows: Y.K., M.Y., and S.O. performed sequencing experiments. T.K., H.S., and K.H. performed DNA methylation analysis. Y.K., M.S., T.I., and K.Y. performed sequencing data analyses. K.K., Y.F., and S.O. performed SNP array analysis. M.S., S.K., K.W., and A.S.-O. designed custom targeted bait. Y.S., K.C., H.T., and S.M. developed bioinformatics pipelines. Y.K. and J.T. interpreted the results. Y.K. and J.T. generated figures and tables and wrote the manuscript. M.H., A.O., Y.H., S.O., Y.T., and J.T. co-led the entire project. All authors participated in discussions and interpretation of the data and results.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kubota, Y., Seki, M., Kawai, T. et al. Comprehensive genetic analysis of pediatric germ cell tumors identifies potential drug targets. Commun Biol 3, 544 (2020). https://doi.org/10.1038/s42003-020-01267-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s42003-020-01267-8
This article is cited by
-
A common deletion at BAK1 reduces enhancer activity and confers risk of intracranial germ cell tumors
Nature Communications (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.