Abstract
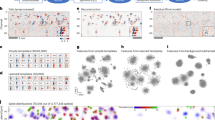
Various medical systems exist for monitoring people in daily life, but they typically require the patient to wear a device, which can create discomfort and can limit long-term use. Contactless vital-sign monitoring would be preferable, but such technology is challenging to develop as it involves weak signals that need to be accurately detected within a practical distance, while being reliably distinguished from unwanted disturbance. Here, we show that a radar-based sensor can be used to monitor the individual vital signs (heartbeat and respiration) of multiple people in a real-world setting. The contactless approach, which does not require any body parts to be worn, uses two antennas (one transmitter and one receiver) and algorithms for target tracking and rejection of random body movements. As a result, it is robust against moderate random body movements (limb movements and desk work) and can keep track of individual people during vigorous movement (such as walking and standing up).
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The data that support the plots within this paper and other findings of this study are available from the corresponding author upon reasonable request.
References
Scully, T. Demography: to the limit. Nature 492, 2–3 (2012).
Fontana, L., Kennedy, B. K., Longo, V. D., Seals, D. & Melov, S. Medical research: treat ageing. Nature 511, 405–407 (2014).
Hung, W. W., Ross, J. S., Boockvar, K. S. & Siu, A. L. Recent trends in chronic disease, impairment and disability among older adults in the United States. BMC Geriatr. 11, 47 (2011).
Gulley, S., Rasch, E. & Chan, L. If we build it, who will come? Working-age adults with chronic health care needs and the medical home. Med. Care 49, 149–155 (2011).
Abdelhafiz, A. H. Heart failure in older people: causes, diagnosis and treatment. Age Ageing 31, 29–36 (2002).
Global diffusion of eHealth: Making universal health coverage achievable. Report of the third global survey on eHealth (World Health Organization, 2016).
Soh, P. J., Vandenbosch, G. A. E., Mercuri, M. & Schreurs, D. Wearable wireless health monitoring: current developments, challenges and future trends. IEEE Microw. Mag. 55, 55–70 (2015).
Hao, Y. & Foster, R. Wireless body sensor networks for health monitoring applications. Physiol. Meas. 29, 27–57 (2008).
Patel, S., Park, H., Bonato, P., Chan, L. & Rodgers, M. A review of wearable sensors and systems with application in rehabilitation. J. Neuroeng. Rehabil. 9, 21 (2012).
Son, D. et al. Multifunctional wearable devices for diagnosis and therapy of movement disorders. Nat. Nanotechnol. 9, 397–404 (2014).
Gualandi, I. et al. Textile organic electrochemical transistors as a platform for wearable biosensors. Sci. Rep. 6, 33637 (2016).
Imani, S. et al. A wearable chemical-electrophysiological hybrid biosensing system for real-time health and fitness monitoring. Nat. Commun. 7, 11650 (2016).
Jung, S. et al. Wearable fall detector using integrated sensors and energy devices. Sci. Rep. 5, 17081 (2015).
Lobodzinski, S. S. & Laks, M. M. New devices for very long-term ECG monitoring. Cardiol. J. 19, 210–214 (2012).
Shafiq, G. & Veluvolu, K. C. Surface chest motion decomposition for cardiovascular monitoring. Sci. Rep. 4, 5093 (2014).
Pandian, P. S. et al. Smart vest: wearable multi-parameter remote physiological monitoring system. Med. Eng. Phys. 30, 466–477 (2008).
Bourke, A. K., O'Brien, J. V. & Lynos, G. M. Evaluation of a threshold-based tri-axial accelerometer fall detection algorithm. Gait Posture 26, 194–199 (2007).
Amelard, R. et al. Feasibility of long-distance heart rate monitoring using transmittance photoplethysmographic imaging (PPGI). Sci. Rep. 5, 14637 (2015).
Nomura, K. et al. A flexible proximity sensor formed by duplex screen/screen-offset printing and its application to non-contact detection of human breathing. Sci. Rep. 6, 19947 (2016).
Coronato, A. Uranus: a middleware architecture for dependable AAL and vital signs monitoring applications. Sensors 12, 3145–3161 (2012).
Partridge, L. Gerontology: extending the healthspan. Nature 529, 154 (2016).
National Research Council (US) Panel on a Research Agenda and New Data for an Aging World Preparing for an Aging World: The Case for Cross-National Research (US National Academies Press, 2001).
eHealth WHA58.28 (World Health Organization, 2005); https://www.who.int/healthacademy/media/WHA58-28-en.pdf
Korhonen, I. et al. Health monitoring in the home of the future. IEEE Eng. Med. Biol. Mag. 22, 66–73 (2003).
Levine, C. Home sweet hospital: the nature and limits of private responsibilities for home health care. J. Aging Health 11, 341–359 (1999).
Li, C. et al. Radar remote monitoring of vital signs. IEEE Microw. Mag. 10, 47–56 (2009).
Obeid, D., Zaharia, G., Sadek, S. & Zein, G. Microwave Doppler radar for heartbeat detection vs electrocardiogram. Microw. Opt. Technol. Lett. 54, 2610–2617 (2012).
Li, C. et al. A review on recent progress of portable short-range noncontact microwave radar systems. IEEE Trans. Microw. Theory Tech. 65, 1692–1706 (2017).
Mercuri, M. et al. Analysis of an indoor biomedical radar-based system for health monitoring. IEEE Trans. Microw. Theory Tech. 61, 2061–2068 (2013).
Su, B., Ho, K., Rantz, M. & Skubic, M. Doppler radar fall activity detection using the wavelet transform. IEEE Trans. Biomed. Eng. 62, 865–875 (2015).
Wang, F. K., Chou, Y. R., Chiu, Y. C. & Horng, T. S. Chest-worn health monitor based on a bistatic self-injection-locked radar. IEEE Trans. Biomed. Eng. 62, 2931–2940 (2015).
Morgan, D. R. & Zierdt, M. G. Novel signal processing techniques for Doppler radar cardiopulmonary sensing. Signal Process. 89, 45–66 (2009).
Mercuri, M. et al. Frequency-tracking CW Doppler radar solving small-angle approximation and null point issues in non-contact vital signs monitoring. IEEE Trans. Biomed. Circuits Syst. 11, 671–680 (2017).
Mercuri, M. et al. A direct phase-tracking doppler radar using wavelet independent component analysis for non-contact respiratory and heart rate monitoring. IEEE Trans. Biomed. Circuits Syst. 12, 632–643 (2018).
Mikhelson, I. V. et al. Remote sensing of patterns of cardiac activity on an ambulatory subject using millimeter-wave interferometry and statistical methods. Med. Biol. Eng. Comput. 51, 135–142 (2013).
Li, C. & Jenshan, L. Random body movement cancellation in Doppler radar vital sign detection. IEEE Trans. Microw. Theory Tech. 56, 3143–3152 (2008).
Peng, Z. et al. A portable FMCW interferometry radar with programmable low-IF architecture for localization, ISAR imaging and vital sign tracking. IEEE Trans. Microw. Theory Tech. 65, 1334–1344 (2017).
Hui, X. & Kan, E. C. Monitoring vital signs over multiplexed radio by near-field coherent sensing. Nat. Electron. 1, 74–78 (2018).
Adib, F., Kabelac, Z., Katabi, D. & Miller, R. C. 3D Tracking via body radio reflections. Proc. Usenix NSDI'14 (2014); http://witrack.csail.mit.edu/witrack-paper.pdf
Adib, F., Kabelac, Z. & Katabi, D. Multi-person localization via RF body reflections. Proc. Usenix NSDI'15 (2015); http://witrack.csail.mit.edu/witrack2-paper.pdf
Adib, F., Mao, H., Kabelac, Z., Katabi, D. & Miller R. C. Smart homes that monitor breathing and heart rate. Proc. ACM CHI https://doi.org/10.1145/2702123.2702200 (2015).
Su, B., Ho, K., Rantz, M. & Skubic, M. Doppler radar fall activity detection using the wavelet transform. IEEE Trans. Biomed. Circuits Syst. 62, 865–875 (2015).
Wang, F., Skubic, M., Rantz, M. & Cuddihy, P. E. Quantitative gait measurement with pulse-Doppler radar for passive in-home gait assessment. IEEE Trans. Biomed. Circuits Syst. 61, 2434–2443 (2014).
Taylor, J. D. Ultra-wideband Radar Technology (CRC Press, 2001).
http://www.gtec.at/Products/Hardware-and-Accessories/g.USBamp-Specs-Features
Acknowledgements
The authors thank all participating volunteers, and E. Hermeling, E. Wentink and B. Grundlehner for their consistent and prompt evaluation regarding the safety and ethical aspects of our experimental protocols.
Author information
Authors and Affiliations
Contributions
M.M. conceived and designed the systems and experiments, developed the range/Doppler profile methodology, analysed and interpreted the data, and wrote the paper. I.L. developed the range/Doppler profile and random body movement methodologies and processed, analysed, interpreted and plotted the data. Y.-H.L. provided technical expertise for the PLL implementation, measured the PLL phase noise and edited the manuscript. F.W. helped with designing the volunteer protocol for ethical approval, provided feedback on targeted medical applications as well as measurement validation and edited the manuscript. C.V.H. provided technical feedback, edited the manuscript and supervised the research. T.T. provided technical feedback, provided final editing of the manuscript and supervised the research.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Supplementary Information
Supplementary Figs. 1–3
Supplementary Video
The video shows the radar Doppler signal and the extracted heartbeat and respiration signals of a sitting subject at 2.6 m who performed four different random body movements: moving an arm (at about 18 s), crossing the legs (at about 55 s), moving the torso back and forth (at about 75 s), and moving an arm (at about 105 s). The extracted biomedical signals have been compared with gold standard references (PPG and respiration belt).
Rights and permissions
About this article
Cite this article
Mercuri, M., Lorato, I.R., Liu, YH. et al. Vital-sign monitoring and spatial tracking of multiple people using a contactless radar-based sensor. Nat Electron 2, 252–262 (2019). https://doi.org/10.1038/s41928-019-0258-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41928-019-0258-6
This article is cited by
-
Wide-range soft anisotropic thermistor with a direct wireless radio frequency interface
Nature Communications (2024)
-
Radar near-field sensing using metasurface for biomedical applications
Communications Engineering (2024)
-
A high-resolution handheld millimeter-wave imaging system with phase error estimation and compensation
Communications Engineering (2024)
-
Soli-enabled noncontact heart rate detection for sleep and meditation tracking
Scientific Reports (2023)
-
Photonic radar for contactless vital sign detection
Nature Photonics (2023)