Abstract
Data are limited on the prevalence and outcome of anemia and its risk on mortality among children under five years of age hospitalized for pneumonia/severe pneumonia. Thus, we conducted a secondary analysis of data extracted from Dhaka Hospital of International Centre for Diarrhoeal Disease Research, Bangladesh to address the evidence gap. Among 3468 children fulfilling the study criteria,1712 (49.4%) had anemia. If children aged ≤ 1.0, > 1.0 to 2.0, > 2.0 to < 6.0, and ≥ 6.0 to 59 months had blood hemoglobin (Hb) value of ≤ 10.7 g/dL, ≤ 9.4 g/dL, ≤ 9.5 g/dL, and ≤ 11 g/dl respectively; we considered them anemic. The trend of prevalence of anemia was found to be inversely related to increasing age (Chi-square for linear trend analysis was done to understand the relation of anemia with increasing age, which was = 6.96; p = 0.008). During hospitalization anemic children more often developed respiratory failure (7.2% vs. 4.4%, p < 0.001) and fatal outcome (7.1.0% vs. 4.2%, p < 0.001) than the children who did not have anemia. After adjusting for potential confounders, such as female sex, lack of immunization, abnormal mental status, severe acute malnutrition, dehydration, hypoxemia, severe sepsis, and bacteremia using multivariable logistic regression analysis, anemia was found to be independently associated with fatal outcome (OR = 1.88, 95% CI 1.23–2.89, p = 0.004). Thus, future interventional studies on the early management of anemia may be warranted to understand whether the intervention reduces the morbidity and deaths in such children.
Similar content being viewed by others
Introduction
Pneumonia has been the major infectious cause of global under-five deaths since the late eighties1. Each year, it accounts for an estimated 0.8 million under-five deaths globally2. More than 95% of these deaths occur in lower- and middle-income countries3. Pneumonia causes estimated 12,000 under-five deaths yearly in Bangladesh, making it the largest killer among this age group2. Globally, childhood pneumonia related mortality reduction was 54% from 2000 to 02184. Moreover, it is also important to note that after 2000, annual pneumonia related mortality declined significantly in Bangladesh, which potentially helped Bangladesh in attaining Millennium Development Goal. Data from the resource limited settings disclosed several risk factors for deaths from childhood pneumonia. Based on that, World Health Organization (WHO) emanated an endorsement that includes incorporating vaccines, appropriate antibiotics, oxygen therapy and other routine clinical care5. That helped lessen global pneumonia-related deaths between 2000 and 2018 by 54% among children under-five years of age4. We need to further bolster the reduction of pneumonia related mortality to attain the sustainable development goal. On the other hand, the prevalence of anemia was high, ranging from 10.2 to 56.6%, in children under five years of age, and the differences in prevalence occurred mainly due to the association of anemia with different co-morbidities among hospitalized children6,8,8. A number of co-morbidities were identified that affect the severity and outcome of anemic children that includes malnutrition6, pneumonia7,9, low birth weight7, poor socio-economic condition8, and intestinal parasitic infections8.
In a recent study9 presence of anemia in children hospitalized for pneumonia substantially increases the risk of severity of the disease and consequently was found to be one of the independent risk factors for deaths during hospitalization. If we are able to understand the role of anemia in pneumonia related mortality, especially in Bangladesh, that may help design potential future interventions and further help to achieve the sustainable development goal.. Thus, there is further need to have more conclusive evidence on the burden and role of anemia with other co-morbid conditions, including pneumonia and their potential outcome during hospitalization in Bangladesh. To further advocate the option of potential management of anemia in the early stage, we decided to investigate the prevalence of anemia and whether co-morbid conditions of anemia had any impact on the fatal outcome among children under five years of age hospitalized for pneumonia/severe pneumonia in Bangladesh.
Materials and methods
Study site
The study was performed in Dhaka Hospital of International Centre for Diarrhoeal Disease Research, Bangladesh (icddr,b), Dhaka, Bangladesh. The description of Dhaka Hospital has been provided somewhere else10.
Study population
Children aged 0–59 months with pneumonia/severe pneumonia, admitted to Dhaka Hospital of icddr,b between August’2013 and December’2017, whose hemoglobin (Hb) level was measured, constituted the study population.
Design
The data were extracted from electronic database of Dhaka Hospital of icddr,b. We stratified the study children into an anemic and non-anemic group. Anemia was defined if blood Hb values were ≤ 10.7 g/dL, ≤ 9.4 g/dL, ≤ 9.5 g/dL, and ≤ 11 g/dl among children aged ≤ 1.0, > 1.0 to 2.0, > 2.0 to < 6.0, and ≥ 6.0 to 59 months of age respectively11,12. The attending physician decided the selection for Hb investigation and was done in our icddr,b laboratory. An initial baseline comparison was made between the children who had anemia and those who did not have anemia. The final comparison was made between the study children who had a fatal outcome and those who survived during hospitalization.
Patient management
Study children received management according to standard treatment following hospital guideline that has been described elsewhere13.
Measurements
We have used pre-tested case report forms for initial acquisition of study relevant data from the electronic database before incorporating them in to a personal computer. We have evaluated baseline characteristics (Table 1) and outcome (Table 2) of children hospitalized for pneumonia/severe pneumonia with anemia compared to those without anemia. We further evaluated the characteristics (including anemia) of children who survived or expired after being hospitalized with pneumonia/severe pneumonia (Table 3).
Operational definition
Pneumonia/severe pneumonia, severe acute malnutrition, severe underweight, invasive diarrhea, dehydration, hypoxemia, bacteremia, and anemia were defined according to WHO guideline5. We have also used evidence-based definition of severe sepsis14. Respiratory failure was defined if the proportion of arterial oxygen saturation (measured by using a pulse oximeter) and fraction of inspired oxygen (SpO2/FiO2) was < 31515. Abnormal mental status was defined if a child had restlessness, or lethargy, or coma, or unconsciousness. These variables were shown in Tables 1, 2 and 3.
Statistical analysis
We analyzed the data using SPSS for Windows (version 20.0) and STATA(version 15.0). For initial baseline analysis (Table 1), anemia was the dependent variable whereas sex, lack of immunization, mental status, severe acute malnutrition, invasive diarrhea, dehydration, hypoxemia, bacteremia, and severe sepsis were the main independent variables. For the outcome table (Table 2) still anemia was the dependent variable whereas respiratory failure, duration of hospital stay and death were the independent variables. The dependent variable of our next analysis (Table 3) was death and main independent variables remained the same in addition to anemia. Normality test was done to understand the distribution of data. We have performed non-parametric test showing median (IQR), if data having continuous variables were not normally distributed. For normally distributed continuous variable we were intending to perform student ‘t’ test showing mean ± SD but we did not have any variable that require this test. We also performed frequencies and percentages for categorical variables. Differences in proportion for categorical variables were compared by the bivariate analysis. Those who had significant associations between the groups (study children who died compared to those who survived) by the bivariate analysis were put into multivariable logistic regression model. In the multivariable logistic regression model death (during hospital course) was the dependent variable and significantly associated factors (on admission) with death that includes anemia were the independent variables. We have also performed Chi-square for linear trend to understand the relation of anemia with increasing age. A p value of less than 0.05 was considered statistically significant. Strength of association was determined by calculating risk ratio (RR) (however, odds ratio [OR] for Table 3) and their 95% confidence intervals (CIs). Additionally, the power of the analysis (anemia vs. non-anemia for outcome of deaths) calculated by using Stata (version 15.0) was 96% with an effect size of 29%.
Institutional Review Board statement
The name of the ethics committee of icddr,b is “Ethical Review Committee”. All the study protocol was approved by the “Ethical Review Committee” of icddr,b following all methods in accordance with the relevant guidelines and regulations. The approval date of the project was 12 January 2020.
Informed consent
As it was a retrospective chart review where data were anonymous and no care-giver interview was required, thus, no informed consent was taken. It is important to note that “Ethical Review Committee” of icddr,b waived the need for informed consent of the study.
Results
Prevalence and associated factors of anemia
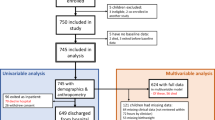
A total of 3468 children fulfilled the inclusion criteria during the study period, and among them,1712 (49.4%) had anemia (Fig. 1). Anemic children more often presented as male (95% CI 1.41–1.51, p < 0.001), had hypoxemia (95% CI 1.09–1.33, p < 0.001), severe acute malnutrition (95% CI 1.01––1.17, p = 0.042), and severe sepsis, compared to those without anemia (Table 1).
Outcomes of anemic children in the hospital
Anemic children more often developed respiratory failure (95% CI 1.24–2.15, p < 0.001) and fatal outcome (95% CI 1.28–2.26, p < 0.001) than their counterpart (Table 2). A total of 194 (5.6%) children with pneumonia/severe pneumonia had fatal outcome (Fig. 1).
Factors associated with deaths among study children
Initial bivariate analysis showed that the children with fatal outcome more frequently were female (95% CI 1.24–2.27, p < 0.001), had anemia (95% CI 2.71–3.43, p < 0.001), lack of immunization (95% CI 1.31–2.83, p < 0.001), abnormal mental status (95% CI 5.69–11.01, p < 0.001), severe acute malnutrition (95% CI 1.10–2.00, p = 0.008), dehydration (95% CI 1.38–2.58, p < 0.001), hypoxemia (95% CI 9.71–22.63, p < 0.001), severe sepsis (95% CI 18.30–36.16, p < 0.001), and bacteremia (95% CI 1.48–3.20, p < 0.001) compared with children who survived (Table 3). After adjusting with potential confounders using multivariable logistic regression analysis, we found that anemia (95% CI 1.23–2.89, p = 0.004) remained the independent risk factor for the fatal outcome (Table 3). In the same model, abnormal mental status (95% CI 1.52–3.75, p < 0.001), hypoxemia (95% CI 2.52–7.27, p < 0.001), severe sepsis (95% CI 5.07–12.16, p < 0.001), and bacteremia (95% CI 1.01–2.81, p = 0.047) were also found to be independently associated with fatal outcome (Table 3).
Relation of anemia with increasing age
The trend of prevalence of anemia was found to be inversely related to increasing age among children under five hospitalized for pneumonia/severe pneumonia (Chi-square for linear trend for anemia was = 6.96; p = 0.008) (Fig. 2).
Discussion
This study identified several important observations: the most important was higher case-fatality rate among the children with anemia compared to those who did not have anemia, and after adjusting for potential confounders anemia remained the independent risk factor for death among the children hospitalized for pneumonia/severe pneumonia. Other important findings includes almost half of the children were anemic, and the trend of anemia was inversely proportional to increasing age among children under five years of age hospitalized for pneumonia/severe pneumonia.
Although, the prevalence of anemia among hospitalized children without specification of pneumonia was found to be variable in a number of previous studies6,8,8, our study is the pioneer, which showed the high prevalence of anemia, specifically in pneumonic children. The prevalence of anemia among children with pneumonia in recent studies from other developing countries was found to be comparatively lower, ranging from 6 to 21.25%9,16,18,18. This observation might be due to the fact that our study children had a number of co-morbidities in addition to pneumonia/severe pneumonia, such as severe acute malnutrition, severe sepsis, and congenital heart disease. In addition, all the studies discussed above used different definitions of anemia, which might impact the variation. It is prudent to mention that the global prevalence of anemia (Hb < 11.0 gm/dl) in this age group of children without specifying the presence of pneumonia is shown to be almost similar (47.4%)19 to our study finding. Moreover, data analyzed from Bangladesh government repository found that the prevalence of anemia (without any specification of pneumonia) was 51.9% which is consistent with our study children. Thus, the prevalence of anemia among pre-school children, irrespective of the presence or absence of concomitant pneumonia, is alarmingly high and anemia in this age group demands more attention, especially with co-morbidity, such as with pneumonia/severe pneumonia due to its potentially fatal consequences.
The observation of the trend of prevalence of anemia to be inversely proportional to increasing age among children under five years of age hospitalized for pneumonia/severe pneumonia is really interesting. This might be due to the higher prevalence of severe illnesses, such as severe acute malnutrition20,21 and severe sepsis14 among infants compared to older children and these severe illnesses were associated with anemia. The observation is almost consistent with a study which evaluated the prevalence of anemia among children from 6 months to 15 years of age with pneumonia in Ecuador18.
We found that anemia was associated with abnormal mental status, hypoxemia, and severe sepsis. Simultaneously these three entities were also associated with fatal outcome in our same study population. A number of previous studies identified that abnormal mental status22, hypoxemia14, and severe sepsis23 resemble several pathways leading to fatal outcome of these illnesses. Pneumonic children with hypoxemia used to have a late presentation in the hospital and often suffer from ventilation-perfusion mismatch followed by reduced functional residual capacity of lungs leading to acute respiratory failure and fatal outcome. Children with severe sepsis and/or bacteremia usually present with impaired vaso-regulation as well as reduced cardiac function followed by poor peripheral perfusion24, which often leads to fatal outcomes25. Any of the above phenomena is found to be featuredwith abnormal mental status of the children5.
Thus, our observation of the independent association of anemia with deaths among the children hospitalized for pneumonia/severe pneumonia is explicable. This study had some inherent strengths that included large data set for long duration collected by trained staff. We have also used high quality icddr,b diagnostics for our lab tests. Simultaneously, we had also a number of limitations in this study that included potential selection bias in measuring anemia status, background characteristics were cross sectional in nature, and data collection were mainly done through the routine system.
Conclusion
Anemia has been shown to be the independent risk factor for deaths among these children during hospitalization. Thus, future studies focusing on anemia during hospitalization of children with pneumonia/severe pneumonia may explore novel interventions that can promote early and appropriate management to reduce morbidity and mortality burden in resource limited settings. The results of our study suggest that the prevalence of anemia was almost 50% and inversely proportional to increasing age among children hospitalized for pneumonia/severe pneumonia. Moreover, prevention of anemia in under-5 children through community-based interventions may reduce the overall burden of childhood pneumonia and severe pneumonia.
Data availability
De-identified data will be available upon request from the research administration of icddr, b.
References
McAllister, D. A. et al. Global, regional, and national estimates of pneumonia morbidity and mortality in children younger than 5 years between 2000 and 2015: A systematic analysis. Lancet Glob. Health 7(1), e47–e57. https://doi.org/10.1016/S2214-109X(18)30408-X (2019).
UNICEF, editor. The 30 High-Burden Countries Include 22 Countries with the Highest Absolute Number of Pneumonia Deaths and the top 14 Countries in Terms of Pneumonia-Specific Mortality Rates. UNICEF Analysis Based on WHO and Maternal and Child Epidemiology Estimation Group Interim Estimates Produced in September 2019, Applying Cause Fractions for the Year 2017 to UN Inter-Agency Group for Child Mortality Estimation Estimates for the Year 2018; WHO Global Health Observatory—Causes of Deaths 2017.
Collaborators GBDLRI. Quantifying risks and interventions that have affected the burden of lower respiratory infections among children younger than 5 years: An analysis for the Global Burden of Disease Study 2017. Lancet Infect. Dis. 2020;20(1):60–79. https://doi.org/10.1016/S1473-3099(19)30410-4
Fighting for Breath in Bangladesh. A Call to Action to Stop Children Dying from Pneumonia. Save the Children, UNICEF; 3rd Edition November 2019.
WHO. Pocket Book for Hospital Care of Children: Guidelines for the Management of Common Illness with Limited Resources. World Health Organization 2013.
Salami, A., Bahmad, H. F., Ghssein, G., Salloum, L. & Fakih, H. Prevalence of anemia among Lebanese hospitalized children: Risk and protective factors. PLoS ONE 13(8), e0201806. https://doi.org/10.1371/journal.pone.0201806 (2018).
Dos Santos, R. F. et al. Prevalence of anemia in under five-year-old children in a children’s hospital in Recife, Brazil. Rev. Bras. Hematol. Hemoter. 33(2), 100–104. https://doi.org/10.5581/1516-8484.20110028 (2011).
Kebede, D., Getaneh, F., Endalamaw, K., Belay, T. & Fenta, A. Prevalence of anemia and its associated factors among under-five age children in Shanan gibe hospital, Southwest Ethiopia. BMC Pediatr. 21(1), 542. https://doi.org/10.1186/s12887-021-03011-5 (2021).
Odeyemi, A. O., Odeyemi, A. O. & Musa, T. L. Determinants of outcome among under-five children hospitalized with pneumonia at a Tertiary Health Facility in South-West Nigeria. West Afr J Med. 38(2), 114–119 (2021).
Afroze, F. et al. The utility of bedside assessment tools and associated factors to avoid antibiotic overuse in an urban PICU of a Diarrheal Disease Hospital in Bangladesh. Antibiotics 10(10), 35. https://doi.org/10.3390/antibiotics10101255 (2021).
Sandoval C. Approach to the child with anemia. In: TWP, editor. UpToDate. UpToDate Inc. (2018).
World Health Organization. Vitamin and Mineral Nutrition Information System. Hemoglobin Concentrations for the Diagnosis of Anemia and Assessment of Severity. World Health Organization (2015).
Shahrin, L. et al. Intravenous amoxicillin plus intravenous gentamicin for children with severe pneumonia in Bangladesh: An open-label, randomized, non-inferiority controlled trial. Life https://doi.org/10.3390/life11121299 (2021).
Chisti, M. J. et al. Bubble continuous positive airway pressure for children with severe pneumonia and hypoxaemia in Bangladesh: An open, randomised controlled trial. Lancet 386(9998), 1057–1065. https://doi.org/10.1016/S0140-6736(15)60249-5 (2015).
Shaima, S. N. et al. Prevalence, predictive factors and outcomes of respiratory failure in children with pneumonia admitted in a developing country. Front. Pediatr. 10, 841–628 (2022).
Ginsburg, A. S. et al. Malawian children with chest-indrawing pneumonia with and without comorbidities or danger signs. J. Glob. Health 11, 04016. https://doi.org/10.7189/jogh.11.04016 (2021).
Ginsburg, A. S. et al. Malawian children with fast-breathing pneumonia with and without comorbidities. Pneumonia 13(1), 3. https://doi.org/10.1186/s41479-021-00081-y (2021).
Garrido, D. F. M., Garrido, S., Vivas, G. & Gutiérrez, M. Prevalence of anaemia in children diagnosed with pneumonia in a Tertiary Hospital in Quito, Ecuador. J. Nepal. Paediatr. Soc. 38(2), 102–109 (2018).
WHO. Worldwide Prevalence of Anaemia 1993–2005. WHO Global Database on Anaemia. World Health Organization; 2008.
Ahmed, T. et al. Mortality in severely malnourished children with diarrhoea and use of a standardised management protocol. Lancet 353(9168), 1919–1922. https://doi.org/10.1016/S0140-6736(98)07499-6 (1999).
Chisti, M. J. et al. Characteristics of severely malnourished under-five children hospitalized with diarrhoea, and their policy implications. Acta Paediatr. 96(5), 693–696. https://doi.org/10.1111/j.1651-2227.2007.00192.x (2007).
Sarmin, M., Ahmed, T., Bardhan, P. K. & Chisti, M. J. Specialist hospital study shows that septic shock and drowsiness predict mortality in children under five with diarrhoea. Acta Paediatr. 103(7), e306–e311. https://doi.org/10.1111/apa.12640 (2014).
Chisti, M. J. et al. Severe sepsis in severely malnourished young Bangladeshi children with pneumonia: A retrospective case control study. PLoS ONE 10(10), e0139966. https://doi.org/10.1371/journal.pone.0139966 (2015).
Carcillo, J. A. Reducing the global burden of sepsis in infants and children: A clinical practice research agenda. Pediatr. Crit. Care Med. 6(3 Suppl), S157–S164. https://doi.org/10.1097/01.PCC.0000161574.36857.CA (2005).
Chisti, M. J., Saha, S., Roy, C. N. & Salam, M. A. Predictors of bacteremia in infants with diarrhea and systemic inflammatory response syndrome attending an urban diarrheal treatment center in a developing country. Pediatr. Crit. Care Med. 11(1), 92–97. https://doi.org/10.1097/PCC.0b013e3181b063e1 (2010).
Acknowledgements
The governments of Bangladesh, Canada, Sweden and the UK provided support to icddr,b for their operations. We are grateful to the study staff for their commitment, as well as to the caregivers of the participating children.
Author information
Authors and Affiliations
Contributions
Conceptualization, M.J.C., C.A.K., and T.A.; Formal analysis, M.J.C., C.A.K., A.S.M.M.H.R., A.S.M.S.B.S., F.A., K.M.S., L.S., M.S., S.N., A.E.R., T.A. (Tahmina Alam), I.P., M.M.A., G.M.S.M., S.N.S., A.S.G.F., T.A. (Tahmeed Ahmed); Investigation, M.J.C.; Methodology, M.J.C., C.A.K., A.S.M.M.H.R., A.S.M.S.B.S., F.A., K.M.S., L.S., M.S., S.N., A.E.R., T.A. (Tahmina Alam), I.P., M.M.A., G.M.S.M., S.N.S., A.S.G.F., T.A. (Tahmeed Ahmed); Supervision, C.A.K., and T.A. (Tahmeed Ahmed); Writing–original draft, M.J.C.; Writing—review & editing, M.J.C., C.A.K., A.S.M.M.H.R., A.S.M.S.B.S., F.A., K.M.S., L.S., M.S., S.N., A.E.R., T.A. (Tahmina Alam), I.P., M.M.A., G.M.S.M., S.N.S., A.S.G.F., T.A. (Tahmeed Ahmed). All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chisti, M.J., Kawser, C.A., Rahman, A.S.M.M.H. et al. Prevalence and outcome of anemia among children hospitalized for pneumonia and their risk of mortality in a developing country. Sci Rep 12, 10741 (2022). https://doi.org/10.1038/s41598-022-14818-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-14818-2
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.