Abstract
Humans are exposed to extreme environmental stressors during spaceflight and return with alterations in brain structure and shifts in intracranial fluids. To date, no studies have evaluated the effects of spaceflight on perivascular spaces (PVSs) within the brain, which are believed to facilitate fluid drainage and brain homeostasis. Here, we examined how the number and morphology of magnetic resonance imaging (MRI)-visible PVSs are affected by spaceflight, including prior spaceflight experience. Fifteen astronauts underwent six T1-weighted 3 T MRI scans, twice prior to launch and four times following their return to Earth after ~ 6-month missions to the International Space Station. White matter MRI-visible PVS number and morphology were calculated using an established, automated segmentation algorithm. We validated our automated segmentation algorithm by comparing algorithm PVS counts with those identified by two trained raters in 50 randomly selected slices from this cohort; the automated algorithm performed similarly to visual ratings (r(48) = 0.77, p < 0.001). In addition, we found high reliability for four of five PVS metrics across the two pre-flight time points and across the four control time points (ICC(3,k) > 0.50). Among the astronaut cohort, we found that novice astronauts showed an increase in total PVS volume from pre- to post-flight, whereas experienced crewmembers did not (p = 0.020), suggesting that experienced astronauts may exhibit holdover effects from prior spaceflight(s). Greater pre-flight PVS load was associated with more prior flight experience (r = 0.60–0.71), though these relationships did not reach statistical significance (p > 0.05). Pre- to post-flight changes in ventricular volume were not significantly associated with changes in PVS characteristics, and the presence of spaceflight associated neuro-ocular syndrome (SANS) was not associated with PVS number or morphology. Together, these findings demonstrate that PVSs can be consistently identified on T1-weighted MRI scans, and that spaceflight is associated with PVS changes. Specifically, prior spaceflight experience may be an important factor in determining PVS characteristics.
Similar content being viewed by others
Introduction
Spaceflight-induced physiological stressors have been well documented, including exposure to microgravity, ionizing radiation, and circadian disruption1,2. Astronauts returning to Earth after spaceflight exhibit structural brain changes, including an upward shift of the brain within the skull3,4,5, regional gray matter volume changes4,5,6,7, and altered white matter volume and microstructural integrity6,7,8. Spaceflight is also associated with alterations in cerebrospinal fluid (CSF) flow, evidenced by ventricular expansion3,5,6,7,9,10,11,12 and redistribution of CSF away from the top of the brain3,6,8. Clinically, approximately 33% of astronauts returning from long-duration spaceflight exhibit spaceflight associated neuro-ocular syndrome (SANS), a constellation of ocular structural changes including optic disc edema, choroidal folding, globe flattening, and hyperopic refractive error shifts13,14. The etiology of SANS remains unknown but could include fluid shifts, increased intracranial pressure, and/or altered CSF drainage with spaceflight13.
Brain CSF3,5,8,9,12, gray4,5, and white matter8,12 changes with spaceflight are associated with the number and duration of prior missions. Furthermore, some brain changes (particularly, lateral and third ventricular expansion) show only partial recovery at 6–12 months post-flight5,6,10,11; thus, astronauts who return to space may experience holdover effects from prior flights. For instance, our prior work5 reported that a shorter time between missions was associated with larger pre-flight lateral ventricles (even after correcting for age effects). Moreover, we found that experienced astronauts who exhibited larger pre-flight lateral ventricles also showed less lateral ventricular expansion in a subsequent flight compared to novice crewmembers5. Together, these findings highlight both frequency and duration of spaceflight as important factors for understanding how microgravity affects cranial fluid shifts and CSF drainage.
According to the classic model, CSF produced by the choroid plexus circulates to the subarachnoid space before exiting the brain via the arachnoid granulations. However, recent evidence suggests that CSF in the subarachnoid space also flows into the brain parenchyma through the periarterial spaces surrounding the penetrating arteries15. Once in the brain parenchyma, CSF exchanges with interstitial space fluid (ISF), eventually returning to the cisternal CSF along the perivenous pathway16. Interstitial and CSF solutes are cleared from the cranium in part through the cervical lymphatic system via dural lymphatic vessels located along the superior sagittal sinus, or near the cribriform plate17. This perivascular exchange of CSF and ISF along what has been termed the glymphatic pathway plays an important role in the removal of cerebral interstitial solutes and wastes18,19. Perivascular space (PVS) enlargement visible on MRI is proposed to represent a disruption of this process and has been observed in conditions associated with glymphatic dysfunction20,21,22,23,24,25.
To date, the effect of microgravity on perivascular CSF circulation remains unknown. We hypothesized that the upward brain shift resulting from microgravity exposure might compress the meningeal lymphatics running along the superior sagittal sinus, impairing CSF/ISF exchange, and/or impair CSF resorption in the arachnoid (Pacchioni) granulations. Disruption of fluid drainage would be evidenced by an increase in MRI-visible PVS number and/or size (i.e., enlargement of PVS volume, length, or width). In the present work, we examine PVS number and size in astronauts pre- and post-approximately 6-month-long International Space Station missions. Here we define PVS as the interstitial fluid-filled space surrounding the intracranial vessels in the brain parenchyma26, with a diametric measure of less than 3 mm27. Due to the high health standards set for astronauts, the MRI-visible loads exhibited by this population are likely PVSs and not manifestations of disease (i.e., small vessel disease) or brain injury. Although our original study design28 did not include PVS analysis, the literature that has emerged since this time19,20,22,25,29,30 led us to hypothesize that spaceflight would impact PVS number and morphology.
The objectives of this study included: (1) To define the effects of spaceflight on PVS characteristics. We predicted an increase in white matter PVS number, volume, length, and/or width after flight. (2) To explore the differences in PVS changes with flight for novice versus experienced astronauts. We predicted that novice astronauts would exhibit more changes in PVS number and size from pre- to post-flight. We also predicted that, within the experienced astronaut subgroup, there would be a correlation between a greater number of days previously spent in spaceflight and a higher number and larger size of PVSs at baseline. (3) To determine the relationship between ventricular expansion and PVS changes with spaceflight. We predicted that greater pre- to post-flight increases in the sum of lateral and third ventricular volume would be associated with an increase in PVS number and size. (4) To examine differences in PVS changes with flight for those who exhibited signs of SANS vs. those who did not (no-SANS). We predicted greater increases in PVS number and size from pre- to post-flight for the SANS versus no-SANS individuals.
Methods
Participants
This was a longitudinal cohort study. Fifteen astronauts and 16 ground-based controls provided their written informed consent to participate in this study. All flight participants completed the highly competitive astronaut selection process, which includes various health, fitness, and education requirements2. Astronauts were also screened for MRI contraindications prior to participation in this study. The ground-based control participants were employees at NASA Johnson Space Center who held at least a master’s degree in a science or engineering field and passed a minimum physical fitness standard (i.e., Air Force Class III equivalent physical examination). The University of Michigan, University of Florida, and NASA Institutional Review Boards approved all study procedures. All methods were performed in accordance with the relevant guidelines and regulations. This analysis was implemented as part of a larger NASA-funded project investigating brain5,31 and behavioral32 changes occurring with long-duration ISS missions28.
Experimental design
The astronauts completed approximately 6-month International Space Station missions (average mission duration: 167 days; Table 1), as well as MRI scans at six time points: approximately 180 and 60 days prior to launch (i.e., Launch-180 and Launch-60 days), as well as approximately 4, 30, 90, and 180 days after return to Earth (i.e., Return + 4, Return + 30, Return + 90, and Return + 180 days, respectively). One astronaut withdrew from the study before their Return + 180 days session; thus, we acquired data from 14 of 15 astronauts at this time point. Of note, this withdrawal did not affect any statistical analyses, which focused on pre- to post-flight changes and relationships of pre-flight PVS metrics with prior flight experience.
The controls completed the same MRI testing at 4 time points across 3 months (i.e., baseline and at approximately 10, 50, and 90 days following the baseline testing). Two controls dropped out before the final time point, so n = 14 subjects with MRI scans at these time points. Due to budget and time constraints, data from these control individuals were collected with the intention for use as control data for multiple spaceflight and spaceflight analog studies. That is, the data provide an estimate of stability over a 3-month period. Thus, the control testing timeline and demographics were not matched to the astronauts, which limited our ability to directly compare the controls to the astronauts. Rather, we leveraged the ground-based control group as converging evidence that PVS changes identified within the astronauts were due to spaceflight and not simply a function of test–retest reliability. There was a partial overlap between the MRI scan dates for the controls and the astronauts. Moreover, since we collected astronaut data at two pre-flight time points, we were able to test for pre-flight stability of our PVS metrics and the astronauts could serve as their own statistical controls. We have used a similar study design in our previous spaceflight analog work33,34, and such a study design is common in the longitudinal neuroimaging literature more broadly (e.g.35,36).
Structural MRI acquisition
All MRI scans were collected using the same 3.0 T Siemens Magnetom Verio MRI scanner using a 32-channel head coil at the University of Texas Medical Branch at Victory Lakes, TX. Recent evidence suggests that time of day can affect PVS metrics37; however, as all MRI scans for the current study were collected in the morning, our PVS measurements were likely not influenced by these timing effects. We collected a T1-weighted structural MRI scan using the following imaging parameters: magnetization-prepared rapid gradient-echo (MPRAGE) sequence, TR = 1.9 s, TE = 2.32 ms, TI = 900 ms, number of phase encoding steps = 255, phase oversampling = 0, slice oversampling = 18.2%, no parallel imaging, flip angle = 9°, FOV = 250 × 250 mm, slice thickness = 0.9 mm, 176 sagittal slices, matrix = 512 × 512, voxel size = 0.488 × 0.488 × 0.9 mm = 0.214 mm3.
Measurement of ventricular volume
We first processed all T1-weighted scans using the Computational Anatomy Toolbox (CAT12.6, version 1450)38,39 implemented within Statistical Parametric Mapping 12 (SPM12; version 7219)40 using MATLAB (R2016a, MathWorks Inc., Natick, MA). We implemented standard CAT12 preprocessing steps to segment the images by tissue type and to extract total intracranial and total white matter volumes. In addition, we extracted native space total lateral and third ventricular volumes for each participant and time point, as defined by the Neuromorphometrics volume-based atlas map (http://Neuromorphometrics.com). We used the sum of the total lateral and third ventricular volumes in all statistical models because extensive prior work has demonstrated substantial changes in both lateral and third (but not fourth) ventricular volume with spaceflight5,6,7,10,11. We refer to this sum as “ventricular volume” throughout the remainder of the manuscript.
Characterization of PVSs
PVS segmentation
White matter PVS identification was carried out using our previously-described algorithm that searches for hypointense structures that meet certain pre-specified morphological criteria29,41,42. Briefly, first, the 3D T1-weighted MRI images were skull-stripped using the Brain Extraction Tool (BET) from the FMRIB Software Library (FSL; Version 5.0). We then resliced the T1-weighted images and CAT12-produced white matter masks to 0.5 mm isotropic voxel size, dilated the white matter masks by two voxels, filled any holes, and, finally, eroded the corrected white matter masks by two voxels to avoid partial volume effects, as described by Promjunyakul et al.43. Each voxel was then subjected to a two-step morphological analysis as follows. First, a sphere with a 3 mm radius was constructed around each voxel within the eroded white matter mask, and the voxels within that sphere were ranked based on their intensity; each voxel was subsequently marked by its neighborhood rank. Another sphere with a 4 mm radius was constructed around each voxel. The average intensity difference between the voxel and the surrounding voxels was calculated and assigned to each voxel (3dLocalstat, AFNI). A voxel was considered for morphological analysis if: (a) the voxel resided in the eroded white matter mask; (b) the difference between the voxel’s intensity and the average intensity of the surrounding voxels was > 15%; (c) the voxel’s intensity fell in the bottom fifth percentile of its neighbors. Second, voxel clusters that were > 1 mm3 (3D corner-to-corner connectivity, 3dclust type 3, AFNI) were considered for morphologic constraint analysis. For each cluster, we calculated linearity, width, length, and total volume in MATLAB. Clusters that were (a) < 16.41 mm wide and (b) had a linearity of at least 0.8 were considered putative PVS and were manually verified by a trained rater (ML). Any identified false alarms (8.9% of total putative PVS across both the astronauts and controls) were removed from the final statistical analyses, as done in our prior work29,41; false alarms were largely due to a partial voluming of other structures (e.g., ventricle and basal ganglia). We then used custom MATLAB code to calculate five key outcome metrics, as done in our past work29,41,42. These outcomes included two metrics that describe total PVS load: (1) total PVS volume (i.e., the sum of the volumes in mL of each distinct PVS in the white matter), and (2) total PVS number (i.e., the total number of distinct PVS in the white matter). The remaining three metrics were characteristics of each distinct PVS: (3) volume (mm3), (4) length (mm), and (5) width (mm). For these three metrics, we then calculated the median volume, median length, and median width across all PVS clusters for each participant at each time point.
Image quality control
Out of the 89 total astronaut scans (i.e., 6 time points × 15 astronauts, with one astronaut who withdrew before the final post-flight scan) and 62 total control scans (i.e., 4 time points × 16 controls, with two individuals who withdrew before the final scan), we excluded 2 astronaut scans and 8 control scans in total from further analysis of PVS metrics. These excluded scans were degraded by motion, noise, or other artifacts, as determined by visual inspection by trained raters (ML, DS, and JP). The excluded astronaut scans included one pre-flight scan (i.e., Launch-60 days); for this participant, we calculated the pre- to post-flight change in PVS metrics using their single baseline scan (i.e., Launch-180 days). The other excluded astronaut scan was from a later post-flight timepoint (i.e., from Return + 180 days). For the control scans, we excluded the participant entirely if one of their four scans was excluded due to artifact; this left us with n = 11 complete control datasets.
Validation of PVS segmentation algorithm
In order to validate our PVS segmentation algorithm, we compared the results from the PVS detection pipeline to visual PVS inspection by two experienced raters (ML and JP). Briefly, these two experienced raters counted the number of PVS in a single slice in 50 randomly selected MRIs from this cohort. The raters were blinded to the number of PVS generated by the algorithm. The average PVS count between the two raters was then compared to the PVS counts generated by the algorithm using Pearson correlation coefficient.
Statistical analyses
We conducted all statistical analyses using R 4.0.044. Of note, no mathematical correction was made for multiple comparisons in any of the described statistical analyses. Instead, in each table in the main text and supplement, we report all individual p values and confidence intervals45,46.
Reliability of PVS metrics
We first tested for stability in the five PVS metrics and ventricular volume by calculating the intraclass correlation coefficient (ICC) between the two pre-flight scans for the astronauts, and across all four scans for the control group. As in our previous work33, we planned a priori to exclude from further statistical analyses any metric with an ICC(3,k) value below 0.5 (moderate reliability47).
PVS changes with spaceflight
We used five separate multivariate linear models to test for changes with spaceflight in each PVS metric and ventricular volume. We entered the difference between the PVS metric or ventricular volume from the last pre-flight time point (Launch-60 days) to the first post-flight time point (Return + 4 days) as the outcome variable. We were specifically interested in whether the intercept was statistically significant (p < 0.05), thereby indicating a change in the PVS metric or ventricular volume with spaceflight.
Next, we tested whether any covariates affected pre- to post-flight change in PVS or ventricular volume metrics. We entered the following covariates into the full model: sex, mean-centered age at launch, mean-centered flight duration, mean-centered time elapsed from landing to the Return + 4 days MRI scan, and novice versus experienced status. We then used stepAIC48 to produce a final model that retained only the best predictor variables; stepAIC uses a stepwise approach to select a maximal model based on the combination of predictors that produces the smallest Akaike information criterion (AIC).
To account for individual differences in total brain tissue volumes and allow for direct inter-subject comparison of PVS metrics, in the respective models we divided each participant’s total PVS volume (mm3) and total PVS number by their average pre-flight total brain white matter volume (cm3). These corrections are identical to those applied in our previous PVS work29,41. To account for individual differences in head size and allow for direct inter-subject comparison of ventricular volume, in the respective model we expressed each astronaut’s ventricular volume divided by their average baseline total intracranial volume5. A correction for head size was not necessary for the median PVS metrics29,41. We ensured that each model met the relevant assumptions (i.e., independence, outliers, linearity, and normality). We tested for normality using visual inspection of qqplots and the Shapiro test (p > 0.05).
Relationship between pre-flight PVS characteristics and previous flight experience
We then conducted an exploratory analysis on the subset of n = 6 experienced astronauts. We used stepwise multivariate linear regression to examine whether average baseline PVS metrics or ventricular volume associated with the total number of previous days spent in space (i.e., total days in space, not including the current mission). We first ran a reduced model including previous flight days as the only predictor. If there was a significant (p < 0.05) linear relationship between previous flight days and the respective PVS metric, we then planned to calculate a full model including sex and mean-centered age at launch as additional covariates. As above, we then planned to use stepAIC to produce a final model that retained only the best predictor variables, based on AIC. We ensured that each model met the relevant assumptions, and we tested for normality using visual inspection of qqplots and the Shapiro test (p > 0.05).
Relationship between spaceflight changes in PVS characteristics and ventricular volume
We also used stepwise multivariate linear regression to examine whether pre- to post-flight change in ventricular volume predicted changes in PVS characteristics. As there were no differences in ventricular volume changes with flight for the novice versus experienced astronauts, we conducted this analysis across the entire (n = 15) astronaut cohort. We first ran a reduced model including ventricular volume as the only predictor. If there was a significant (p < 0.05) linear relationship between ventricular volume and the respective PVS metric, we planned to calculate a full model including sex and mean-centered age at launch, total flight duration, and time elapsed from landing to the Return + 4 days MRI scan as additional covariates. Then, as above, we planned to use stepAIC to produce a final model that retained only the best predictor variables, based on AIC. We ensured that each model met the relevant assumptions (i.e., independence, outliers, linearity, and normality), and we tested for normality using visual inspection of qqplots and the Shapiro test (p > 0.05).
Differences in PVS changes for SANS versus no-SANS subgroups
We conducted a final exploratory analysis comparing a subset of astronauts who developed at least one symptom of spaceflight associated neuro-ocular syndrome (SANS, n = 6) to the subset of astronauts who did not experience any SANS symptoms (no-SANS, n = 6). SANS status was determined using pre- and post-flight ophthalmic exam results obtained from the NASA Lifetime Surveillance of Astronaut Health Repository. We were unable to obtain SANS data for three astronauts, resulting in a sample of 12 for our SANS analysis. As recently defined by Lee et al. 202013 an astronaut was determined to have SANS if they showed changes in the following measures in either eye from pre- to post-flight: optic disc edema (variable Frisén grades), choroidal folds, hyperopic refractive error shifts > 0.75 D, or globe flattening. We conducted identical analyses to those described above (“PVS changes with spaceflight”) to test for pre- to post-flight change in the PVS metrics and ventricular volume, but here we included SANS status as a predictor of interest instead of novice versus experienced status.
Results
The cohort consisted of 15 astronauts, 9 of whom had no prior flight experience (“novice” astronauts) and 6 of whom had completed at least one previous spaceflight mission (“experienced” astronauts). The experienced astronauts were, on average, older than the novice astronauts. No other novice versus experienced group differences emerged for sex, mission duration, or time between landing and the first post-flight MRI scan (Table 1). The control group consisted of 11 complete cases. There were no group differences in age or sex between the astronauts and controls (Table 1).
Identification of PVSs and validation of automated PVS algorithm
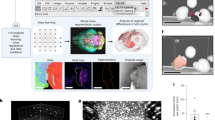
We identified PVSs in each astronaut and each control at each time point. PVSs were identified in the white matter in various regions across the centrum semiovale white matter (see exemplar participant, Fig. 1) (As described above, our algorithm searched for PVSs only within the white matter, and not within other tissue types).
PVSs identified on a single astronaut. Here we depict a binary mask of PVSs for a single astronaut at the last pre-flight time point (Launch-60 days), for illustrative purposes. PVSs are shown in red, overlaid onto this individual’s native space 3D-rendered white matter segment (left) as well as several sagittal slices of their skull stripped native space structural scan (right). The blue box shows a zoomed-in view of one PVS, inside the blue circle.
A Pearson correlation coefficient was computed to assess the linear relationship between total PVS numbers obtained with our automated algorithm and PVS counts obtained by visual ratings (average between two independent, blinded raters). There was a strong positive correlation between the two variables, r(48) = 0.77, p < 0.001 (Fig. 2).
Correlation of total PVS number obtained from automated algorithm and visual rating. Here we depict the strong positive correlation between the algorithm-generated total PVS number, and the average total PVS number (on the same slice for each participant), as counted by two blinded independent raters for 50 randomly selected MRI scans from this astronaut cohort. Note that points are jittered by x = 0.15 and y = 0.15, for ease of visual interpretation (as otherwise, many points would be overlapping with one another).
Reliability of PVS metrics
Four of the five PVS metrics, as well as ventricular volume, yielded ICC(3,k) values > 0.50 for both the astronauts and the controls. The ICC(3,k) values are presented in Table 2.
We excluded median width from further statistical analyses due to the low reliability of this measure in both the astronauts and controls.
Changes in PVS characteristics with spaceflight
Changes in PVS characteristics with spaceflight are summarized in Table S1, Table S2, Table 3, and Fig. 3. Table S1 presents PVS and ventricular volume descriptive statistics at each time point. Group mean PVS values reported here fall within the range identified previously by our group for a cohort of male veterans (mean age: 32 years; age range: 29–41 years) with a history of traumatic brain injury29. There were no statistically significant whole-group changes in any of the PVS characteristics from pre- to post-flight (p > 0.05; Table S2), though, across all astronauts, there was a trend towards pre- to post-flight increases in PVS median length (p = 0.069). The final model produced by the stepwise selection procedure for pre- to post-flight changes in total PVS volume included novice versus experienced status as a covariate. The novice astronauts showed a mean pre- to post-flight increase in total PVS volume, whereas the experienced astronauts showed a mean pre- to post-flight decrease in total PVS volume (p = 0.020; Table 3; Fig. 3). There was no statistically significant pre-to post-flight difference by novice versus experienced status for the other PVS characteristics, though total PVS number showed a trend (p = 0.068) similar to total PVS volume, in which the novice astronauts showed a mean pre- to post-flight increase in total PVS number, whereas the experienced astronauts showed a mean pre- to post-flight decrease in total PVS number. Ventricular volume showed a significant increase from pre- to post-flight for the whole group (p < 0.001; Table S2), though there was no effect of experience level on ventricular volume changes (p > 0.05; Table 3).
Changes in PVS metrics and ventricular volume from pre- to post-flight. Group average PVS characteristics are depicted for each of the four control group time points (gray, left panels) and for each of the six astronaut time points (right panels). The astronaut data are split into novice (green) and experienced (purple) subgroups. Bars represent standard error. The width of the green and purple boxes indicates the average flight duration for novice and experienced astronauts, respectively. *Indicates a statistically significant (p < 0.05) group difference between the novice and experienced astronauts for changes in total PVS volume with spaceflight. ***Indicates a statistically significant (p < 0.001) change in ventricular volume from pre- to post-flight. The second astronaut time point depicts group-average data for n = 8 (instead of 9) novice astronauts; the final astronaut time point depicts group-average data for n = 13 (instead of 15) experienced astronauts (see “Methods” for details on these missing data). We included only complete control group datasets, so n = 11 for all control time points. WM white matter, TIV total intracranial volume.
Correlation between past flight experience and baseline PVS characteristics
The correlations between past flight experience and baseline PVS characteristics are summarized in Table S3. Among the experienced astronauts (n = 6), there were no statistically significant relationships between past flight experience and baseline PVS characteristics (p > 0.05). However, each relationship was of large effect size (r = 0.60–0.71) and indicated that a greater number of previous flight days was associated with greater pre-flight PVS total volume (r(4) = 0.61; p = 0.201), total number (r(4) = 0.60; p = 0.208), median volume (r(4) = 0.71; p = 0.114), and median length (r(4) = 0.70; p = 0.121). These strong effect sizes remained similar when also controlling for age at launch (partial r = 0.69 to 0.77). There was no correlation between number of previous flight days and ventricular volume (r(4) = −0.08; p = 0.873).
Correlation between post-flight ventricular expansion and PVS characteristics
The correlations between post-flight ventricular expansion and PVS characteristics are summarized in Table S4. There was one relationship of moderate strength between greater pre- to post-flight change in ventricular volume and greater pre- to post-flight change in median PVS length, though this did not reach statistical significance (r(13) = 0.44; p = 0.100). There was no statistically significant correlation between ventricular volume changes and the other PVS characteristics (r = − 0.12 to − 0.25; p > 0.05).
No group differences by SANS status
There were no statistically significant changes in PVS metrics or ventricular volume at baseline from pre- to post-flight between those who did and did not experience one or more symptom(s) of SANS (Table S5).
Discussion
This is the first study to examine changes in MRI-visible PVS in the white matter with spaceflight, and to demonstrate that PVS metrics can be consistently identified on T1-weighted MRI scans using an automated algorithm. Our key findings included that novice astronauts exhibited increases in total PVS volume from pre- to post-flight, whereas experienced astronauts did not. Moreover, in experienced astronauts, the number of days spent in space prior to the current mission was associated with greater PVS load at the two pre-flight scan time points, though these relationships did not reach statistical significance. We also identified a moderate correlation between pre- to post-flight increases in PVS median length and pre- to post-flight increases in the sum of lateral and third ventricular volume, though this relationship also did not reach statistical significance. Finally, we did not find any significant differences in PVS characteristics between those who did and did not exhibit one or more symptom(s) of SANS.
We found that novice astronauts exhibited an increase in PVS volume from pre- to post-flight, whereas experienced flyers did not. This divergence between novice and experienced astronauts is consistent with the hypothesis that ventricular expansion with spaceflight is a compensatory response49. That is, Roberts and colleagues suggest that experienced flyers have larger pre-flight ventricular volume (i.e., lingering ventricular expansion from previous flights5,6,10,11), and therefore do not show as much ventricular volume increase with subsequent spaceflights, perhaps due to a loss of compliance with changes from previous flights. Whether the PVS findings observed here reflect pathophysiological or compensatory consequences of spaceflight remains unknown. Regardless, repeated spaceflight exposure appears to be a key determinant of brain fluid changes that should be further explored in the future. That is, these data suggest a cumulative and asymptotic effect on CSF spaces. As astronauts experience microgravity for longer cumulative durations, ventricles enlarge, and PVS size increases, eventually reaching a plateau, which potentially decreases the changes observed with each subsequent flight.
In line with this hypothesis, we also found that, among the experienced crewmembers, greater PVS load (i.e., total volume, total number, median volume, and median length) at baseline was correlated with more days previously spent in space (though these relationships did not reach statistical significance and should be interpreted with caution). This fits with previous work from our group and others, showing that alterations in gray matter4,5, white matter microstructure8, T2 hyperintensities12, free water distribution8, and ventricular volume3,5,9,12 depend on the frequency and/or duration of time spent in space. This finding also suggests that PVS changes with spaceflight may be long lasting. Indeed, previous spaceflight longitudinal analyses have suggested that several structural brain changes with flight (namely, ventricular expansion) are slow to recover, remaining elevated at 6 to 12 months post-flight for some individuals5,6,10,11. Therefore, as NASA’s goals shift towards longer-duration missions to Mars, it is becoming increasingly critical to study the mechanisms and consequences of PVS enlargement in future spaceflight or ground-based analog studies, ideally with larger samples.
Furthermore, we observed a moderate positive correlation between greater increase in ventricular volume with flight and greater increase in median PVS length (though this relationship did not reach statistical significance and thus we hesitate to over-interpret this result). However, it is worth noting that multiple previous studies have shown cranial fluid and brain position shifts following spaceflight3,5,6,8, and these shifts could compress the adjacent venous structures at the top of the head. This could then obstruct the arachnoid granulations positioned along the superior sagittal sinus and/or compress the dural lymphatic vessels, further impairing CSF reabsorption. Roberts et al.49 have suggested that the result of this CSF outflow obstruction is ventricular dilation similar to that observed in individuals with normal pressure hydrocephalus. Under this assumption, the moderate relationship between pre- to post-flight changes in PVS length and ventricular expansion could represent the result of CSF resorption obstruction in light of a fundamental venous cranial outflow obstruction due to cephalad fluid shift. It is worth noting that individuals with normal pressure hydrocephalus show both dilated PVS and glymphatic dysfunction represented by delayed clearance of intrathecally administered gadolinium contrast50,51,52.
In our cohort, we did not observe an association between changes in PVS characteristics and clinical manifestations of SANS. Headward fluid shifts leading to obstruction of CSF and intraorbital fluid and glymphatic dysfunction have been proposed as potential mechanisms underlying SANS13. There are several plausible explanations for the lack of relationship between PVS change and SANS symptoms. First, it may be that PVS function does not relate to SANS. Second, the role of PVS in CSF clearance remains unknown, and it is possible that impaired clearance still occurs in the absence of PVS enlargement19. Third, the absence of correlations between PVS and SANS symptoms could be a consequence of our small subgroup sizes.
Factors aside from long-duration microgravity exposure alone may also influence spaceflight effects on PVS. For instance, as suggested by evidence in subjects with traumatic brain injuries23,29, external mechanical forces (i.e., the high accelerations that occur with launch and landing) may contribute to PVS changes in astronauts. However, our recent case study in a single astronaut53 suggests that structural brain changes with spaceflight (i.e., fluid shifts within the brain and ventricular expansion) are more likely to be due to microgravity than to the accelerations of launch/landing (though we did not examine PVS in that study). Moreover, normal aging could influence longitudinal PVS changes. However, the pre-flight stability of the PVS metrics (over about 4 months), as well as the stability of the PVS metrics in the control group (over about 3 months) suggests that normal aging in our middle-aged astronauts did not substantially influence the observed longitudinal PVS changes. In addition, in the one case where we observed differences between novice and experienced astronauts, the older mean age of the experienced astronaut group likely did not affect these group differences. We showed that PVS total volume increased for the novice astronauts but decreased for the experienced astronauts from pre- to post-flight. This would be the opposite direction of what we would expect if we were only capturing normal aging changes in PVS metrics.
Parallel to what occurs with neurodegenerative disease (e.g., Alzheimer’s disease), PVS blockage and enlargement might suggest an inability to clear harmful metabolic waste (e.g., amyloid) from the draining pathway, leading to an accumulation of neurotoxic protein aggregates around the blood vessel54. This buildup is believed to result in a disruption to brain homeostasis and is associated with the pathogenesis of Alzheimer’s disease; however, the specific mechanisms driving PVS enlargement are unknown55. Recently in five cosmonauts, blood markers for amyloid-β (Aβ40 and Aβ42) proteins frequently linked with neurodegenerative disease and brain injury were identified to increase from pre- to post-spaceflight and remained elevated three weeks after return56. This post-flight amyloid-β elevation was described as a potential reparatory process, acting to restore the integrity of the blood–brain barrier56; the potential role of PVS clearance in this maintenance process should be examined in future spaceflight studies.
Our study has several limitations. Our original study design, developed over a decade ago, did not aim to examine PVS changes with spaceflight. However, recent reports of PVS changes in aging30,57, brain injury25,29, and neurologic disease populations19,20,22,55,58 led us to hypothesize that spaceflight might also cause changes in PVS number and morphology. Moreover, the number of people who travel to space is small, creating an inevitable obstacle in the efforts to study spaceflight-associated changes. To address the concern of sample size, a repeated measures design was implemented, thereby allowing each astronaut to serve as their own control. Given this limited sample size, the statistical analyses (and particularly, correlation results) should be interpreted with caution and replicated in future studies as more individuals travel to space.
Though we included a ground-based control group for comparison purposes, this control group was originally intended for use with multiple spaceflight and analog studies. As a result, the testing timeline and demographics for this control group were not specifically matched to the current study. Thus, here we leveraged the control group only to provide additional evidence that PVS metrics are stable over time when participants go about their daily lives on Earth. An additional limitation is that we did not have access to phantom data to perform our own quality controls on the data; however, the scans were all collected at the same, active clinical MRI facility, which regularly performs its own quality controls. There was also a delay between re-entry to Earth's gravitational field and the first post-flight MRI acquisition, ranging between one and six days after landing (average = 4.5 days). We used this value as a covariate in the full statistical models to mitigate its effect. Given that ventricular volume changes are still evident months post-flight5,6,10,11, this time offset is likely not a key factor in the current study. However, it could be that PVS and ventricular volume changes have different temporal dynamics and recovery patterns.
Another limitation is that the PVS algorithm we employed is tailored to white matter PVS segmentation and has not yet been optimized for identifying PVS in the gray matter; future studies should enhance the algorithm to incorporate other tissue types and anatomical regions. For example, future studies planning to characterize PVS changes with spaceflight should optimize acquisition protocols for PVS detection across the whole brain (e.g., by collecting structural images with isotropic voxels, instead of resampling to isotropic voxel sizes after acquisition59). Moreover, it is possible that the PVS segmentation algorithm is not sensitive enough to uncover subtle differences in PVS characteristics caused by spaceflight. However, despite large between-subject differences, ICCs between the two pre-flight MRIs and among the control participants met our a priori inclusion criteria for all but one (i.e., median width) PVS metric. Due to the resolution of the images available, we were not able to distinguish whether the quantified PVSs were arterial or venular. Moreover, although it is presumed that we identified MRI-visible PVSs, no quantitative delineation was instituted to rule out the presence of neuroanatomical anomalies (i.e., T1 hypointensities, small vessel disease, etc.). Lastly, while our algorithm is able to detect PVS in T1-weighted images, the absence of a T2-weighted scan prevents PVS from being compared with T2 white matter hyperintensities (i.e., T1 hypointensities). Despite finding a positive correlation between our PVS detection algorithm with the results of two experienced raters, future studies aimed at characterizing PVS changes with spaceflight will benefit from a more comprehensive imaging acquisition protocol that includes T2-weighted FLAIR sequences. The use of additional sequences such as T2 to confirm that findings on T1 are indeed PVS remains the preferred method for PVS characterization, particularly in older individuals. However, given that our sample comprises very healthy individuals, with a mean age in their mid-40s, we do not anticipate that T2 white matter hyperintensities posed a large problem for PVS identification in this cohort. For example, in a cohort of individuals ages 16–65 years, Hopkins et al.60 found that T2 white matter hyperintensities occurred in only 13 of these 243 individuals (i.e., 5.3% of the cohort). Moreover, those older than 55 years had a tenfold increase in hyperintensity prevalence compared to those ≤ 55 years. Thus, in this healthy astronaut cohort, we do not anticipate that T2 white matter hyperintensities were a substantial confounding factor in relation to the PVS metrics.
Conclusion
We found that at the group level, PVS was not affected by spaceflight. However, when we evaluated these changes separately between novice astronauts and those that had been to space before, we observed experience-dependent effects. First, novice astronauts had an increase in PVS with spaceflight, whereas experienced crewmembers did not. Second, those with prior spaceflight experience exhibited a correlation between more previous days in space and greater pre-flight PVS length (though this effect did not reach statistical significance). Our findings suggest that PVS changes with spaceflight are dependent upon prior microgravity exposure, similar to other brain structural changes we have reported5. Whether these changes in PVS represent a compensatory mechanism or could eventually lead to pathological manifestations remains unknown. Given the moderate (though not statistically significant) relationship we identified between greater increases in ventricular volume with flight and greater increases in PVS length, we suggest that our findings relate to CSF resorption obstruction caused by the fluid3,6,8 and upward brain position shifts3,5,6,8 observed with microgravity exposure. Moving forward, head-down tilt bed rest analog studies may provide further insights into PVS associations with spaceflight, as this environment also results in brain position and fluid shifts.
Data availability
The datasets included in this study will be made available through NASA’s Life Sciences Data Archive (https://lsda.jsc.nasa.gov), upon reasonable request and with permission of NASA.
References
Clément, G. R. et al. Challenges to the central nervous system during human spaceflight missions to Mars. J. Neurophysiol. 123, 2037–2063 (2020).
Hupfeld, K. E., McGregor, H. R., Reuter-Lorenz, P. A. & Seidler, R. D. Microgravity effects on the human brain and behavior: Dysfunction and adaptive plasticity. Neurosci. Biobehav. Rev. 122, 176–189 (2021).
Roberts, D. R. et al. Effects of spaceflight on astronaut brain structure as indicated on MRI. N. Engl. J. Med. 377, 1746–1753 (2017).
Koppelmans, V., Bloomberg, J. J., Mulavara, A. P. & Seidler, R. D. Brain structural plasticity with spaceflight. npj Microgravity 2, 1–8 (2016).
Hupfeld, K. E. et al. The impact of 6 and 12 months in space on human brain structure and intracranial fluid shifts. Cereb. Cortex Commun. 1, tgaa023 (2020).
Jillings, S. et al. Macro-and microstructural changes in cosmonauts’ brains after long-duration spaceflight. Sci. Adv. 6, eaaz9488 (2020).
Riascos, R. F. et al. Longitudinal analysis of quantitative brain MRI in astronauts following microgravity exposure. J. Neuroimaging 29, 323–330 (2019).
Lee, J. K. et al. Spaceflight-associated brain white matter microstructural changes and intracranial fluid redistribution. JAMA Neurol. 76, 412–419 (2019).
Roberts, D. R. et al. Prolonged microgravity affects human brain structure and function. Am. J. Neuroradiol. 40, 1878–1885 (2019).
Kramer, L. A. et al. Intracranial effects of microgravity: A prospective longitudinal MRI study. Radiology 295, 640–648 (2020).
Van Ombergen, A. et al. Brain ventricular volume changes induced by long-duration spaceflight. Proc. Natl. Acad. Sci. 116, 10531–10536 (2019).
Alperin, N., Bagci, A. M. & Lee, S. H. Spaceflight-induced changes in white matter hyperintensity burden in astronauts. Neurology 89, 2187–2191 (2017).
Lee, A. G. et al. Spaceflight associated neuro-ocular syndrome (SANS) and the neuro-ophthalmologic effects of microgravity: A review and an update. npj Microgravity 6, 1–10 (2020).
Lee, A. G., Mader, T. H., Gibson, C. R. & Tarver, W. Space flight-associated neuro-ocular syndrome. JAMA Ophthalmol. 135, 992–994 (2017).
Iliff, J. J. et al. Brain-wide pathway for waste clearance captured by contrast-enhanced MRI. J. Clin. Investig. 123, 1299–1309 (2012).
Iliff, J. J. et al. A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid β. Sci. Transl. Med. 4, 147ra111 (2012).
Louveau, A. et al. Structural and functional features of central nervous system lymphatic vessels. Nature 523, 337–341 (2016).
Bacyinski, A., Xu, M., Wang, W. & Hu, J. The paravascular pathway for brain waste clearance: Current understanding, significance and controversy. Front. Neuroanat. 11, 101 (2017).
Brown, R. et al. Understanding the role of the perivascular space in cerebral small vessel disease. Cardiovasc. Res. 114, 1462–1473 (2018).
Ramirez, J. et al. Visible Virchow–Robin spaces on magnetic resonance imaging of Alzheimer’s disease patients and normal elderly from the Sunnybrook Dementia Study. J. Alzheimers Dis. 43, 415–424 (2015).
Potter, G. M., Chappell, F. M., Morris, Z. & Wardlaw, J. M. Cerebral perivascular spaces visible on magnetic resonance imaging: Development of a qualitative rating scale and its observer reliability. Cerebrovasc. Dis. 39, 224–231 (2015).
Charidimou, A. et al. White matter perivascular spaces: An MRI marker in pathology-proven cerebral amyloid angiopathy?. Neurology 82, 57–62 (2014).
Inglese, M. et al. Clinical significance of dilated Virchow–Robin spaces in mild traumatic brain injury. Brain Inj. 20, 15–21 (2006).
Patankar, T. F. et al. Dilatation of the Virchow–Robin space is a sensitive indicator of cerebral microvascular disease: Study in elderly patients with dementia. Am. J. Neuroradiol. 26, 1512–1520 (2005).
Opel, R. A. et al. Effects of traumatic brain injury on sleep and enlarged perivascular spaces. J. Cereb. Blood Flow Metab. 39, 2258–2267 (2019).
Kwee, R. M. & Kwee, T. C. Virchow–Robin spaces at MR imaging. Radiographics 27, 1071–1086 (2007).
Wardlaw, J. M. et al. Neuroimaging standards for research into small vessel disease and its contribution to ageing and neurodegeneration. Lancet Neurol. 12, 822–838 (2013).
Koppelmans, V. et al. Study protocol to examine the effects of spaceflight and a spaceflight analog on neurocognitive performance: Extent, longevity, and neural bases. BMC Neurol. 13, 1–15 (2013).
Piantino, J. et al. Link between mild traumatic brain injury, poor sleep, and magnetic resonance imaging: Visible perivascular spaces in veterans. J. Neurotrauma 38, 2391–2399 (2021).
Bown, C. W., Carare, R. O., Schrag, M. S. & Jefferson, A. L. Physiology and clinical relevance of enlarged perivascular spaces in the aging brain. Neurology 98, 107–117 (2022).
Hupfeld, K. E. et al. Brain and behavioral evidence for reweighting of vestibular inputs with long-duration spaceflight. Cereb. Cortex 32, 755–769 (2021).
Tays, G. D. et al. The effects of long duration spaceflight on sensorimotor control and cognition. Front. Neural Circuits 15, 723504 (2021).
Koppelmans, V. et al. Brain plasticity and sensorimotor deterioration as a function of 70 days head down tilt bed rest. PLoS One 12, e0182236 (2017).
Koppelmans, V. et al. Intracranial fluid redistribution but no white matter microstructural changes during a spaceflight analog. Sci. Rep. 7, 1–12 (2017).
Iordan, A. D. et al. Neural correlates of working memory training: Evidence for plasticity in older adults. Neuroimage 217, 116887 (2020).
Iordan, A. D. et al. Age differences in functional network reconfiguration with working memory training. Hum. Brain Mapp. 42, 1888–1909 (2021).
Barisano, G., Sheikh-Bahaei, N., Law, M., Toga, A. W. & Sepehrband, F. Body mass index, time of day and genetics affect perivascular spaces in the white matter. J. Cereb. Blood Flow Metab. 41, 1563–1578 (2021).
Dahnke, R., Yotter, R. A. & Gaser, C. Cortical thickness and central surface estimation. Neuroimage 65, 336–348 (2013).
Gaser, C. & Kurth, F. Manual Computational Anatomy Toolbox-CAT12 (University of Jena, 2017).
Ashburner, J. et al. SPM12 Manual (Wellcome Trust Centre for Neuroimaging, 2014).
Piantino, J. et al. Characterization of MR imaging–visible perivascular spaces in the white matter of healthy adolescents at 3T. Am. J. Neuroradiol. 41, 2139–2145 (2020).
Schwartz, D. L. et al. Autoidentification of perivascular spaces in white matter using clinical field strength T1 and FLAIR MR imaging. Neuroimage 202, 116126 (2019).
Promjunyakul, N. et al. Characterizing the white matter hyperintensity penumbra with cerebral blood flow measures. NeuroImage Clin. 8, 224–229 (2015).
R Core Team. R: A Language and Environment for Statistical Computing (R Foundation for Statistical Computing, 2021).
Rothman, K. J. No adjustments are needed for multiple comparisons. Epidemiology 1, 43–46 (1990).
Saville, D. J. Multiple comparison procedures: The practical solution. Am. Stat. 44, 174–180 (1990).
Koo, T. K. & Li, M. Y. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J. Chiropr. Med. 15, 155–163 (2016).
Venables, W. N. & Ripley, B. D. Modern Applied Statistics with S-PLUS (Springer Science and Business Media, 2013).
Roberts, D. R. & Petersen, L. G. Studies of hydrocephalus associated with long-term spaceflight may provide new insights into cerebrospinal fluid flow dynamics here on earth. JAMA Neurol. 76, 391–392 (2019).
Ringstad, G., Vatnehol, S. A. S. & Eide, P. K. Glymphatic MRI in idiopathic normal pressure hydrocephalus. Brain 140, 2691–2705 (2017).
Ringstad, G. et al. Brain-wide glymphatic enhancement and clearance in humans assessed with MRI. JCI Insight 3, e121537 (2018).
Eide, P. K., Pripp, A. H., Ringstad, G. & Valnes, L. M. Impaired glymphatic function in idiopathic intracranial hypertension. Brain Commun. 3, fcab043 (2021).
McGregor, H. R. et al. Case report: No evidence of intracranial fluid shifts in an astronaut following an aborted launch. Front. Neurol. 12, 774805 (2021).
Ramirez, J. et al. Imaging the perivascular space as a potential biomarker of neurovascular and neurodegenerative diseases. Cell. Mol. Neurobiol. 36, 289–299 (2016).
Boespflug, E. L. et al. Targeted assessment of enlargement of the perivascular space in Alzheimer’s disease and vascular dementia subtypes implicates astroglial involvement specific to Alzheimer’s disease. J. Alzheimers Dis. 66, 1587–1597 (2018).
Zu Eulenburg, P. et al. Changes in blood biomarkers of brain injury and degeneration following long-duration spaceflight. JAMA Neurol. 78, 1525–1527 (2021).
Kress, B. T. et al. Impairment of paravascular clearance pathways in the aging brain. Ann. Neurol. 76, 845–861 (2014).
Donahue, E. K. et al. Global and regional changes in perivascular space in idiopathic and familial Parkinson’s disease. Mov. Disord. 36, 1126–1136 (2021).
Wardlaw, J. M. et al. Perivascular spaces in the brain: Anatomy, physiology and pathology. Nat. Rev. Neurol. 16, 137–153 (2020).
Hopkins, R. O. et al. Prevalence of white matter hyperintensities in a young healthy population. J. Neuroimaging 16, 243–251 (2006).
Acknowledgements
This work was supported by grants from the National Aeronautics and Space Administration (NASA NNX11AR02G) and the National Space Biomedical Research Institute (#NCC 9-58) to RS, AM, SW, and JB. During completion of this work, KH was supported by a National Science Foundation Graduate Research Fellowship under Grant no. DGE-1315138 and DGE-1842473, National Institute of Neurological Disorders and Stroke training grant T32-NS082128, and National Institute on Aging fellowship 1F99AG068440. DS was supported by the National Institute on Aging under Grant nos. R01AG056712 and P30AG008017. LS was supported by the National Institute on Aging under Grant no. P30AG066518. JP was supported by the National Heart Lung and Blood Institute under Grant no. K23HL150217-01. The authors also wish to thank all of the astronauts who volunteered their time, without whom this project would not have been possible.
Author information
Authors and Affiliations
Contributions
K.H. extracted ventricular volumes, conducted all statistical analyses, created all figures and supplemental material, and wrote the “Methods” and “Results”. K.H., S.B.R., R.S., and J.P. wrote the “Abstract”, “Introduction”, and “Discussion” sections. H.M. conducted the SANS versus no-SANS classifications and participated in manuscript preparation. D.S. designed the PVS analysis pipeline and processed the images to extract PVS metrics. M.L. visually checked the results of the automated PVS pipeline. N.B. and Y.D. collected and analyzed data. I.S. participated in project design and software development. R.R. facilitated data collection. S.W., J.B., A.M., L.S., J.I., R.S., and J.P. designed the project and led interpretation and discussion of the results. All authors participated in revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
NB, IK, YD, and AM were employed by the company KBR. The remaining authors (KE, SR, HM, DS, ML, RR, SW, JB, LS, JI, RS, and JP) declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hupfeld, K.E., Richmond, S.B., McGregor, H.R. et al. Longitudinal MRI-visible perivascular space (PVS) changes with long-duration spaceflight. Sci Rep 12, 7238 (2022). https://doi.org/10.1038/s41598-022-11593-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-11593-y
This article is cited by
-
Dynamic changes in perivascular space morphology predict signs of spaceflight-associated neuro-ocular syndrome in bed rest
npj Microgravity (2024)
-
A perspective on the evidence for glymphatic obstruction in spaceflight associated neuro-ocular syndrome and fatigue
npj Microgravity (2024)
-
Impacts of spaceflight experience on human brain structure
Scientific Reports (2023)
-
Methods for assessing change in brain plasticity at night and psychological resilience during daytime between repeated long-duration space missions
Scientific Reports (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.