Abstract
Tendon tissue storage and preconditioning are often used in biomechanical experiments and whether this generates alterations in tissue properties is essential to know. The effect of storage and preconditioning on dense connective tissues, like tendons, is fairly understood. However, healing tendons are unlike and contain a loose connective tissue. Therefore, we investigated if storage of healing tendons in the fridge or freezer changed the mechanical properties compared to fresh tendons, using a pull-to-failure or a creep test. Tissue morphology and cell viability were also evaluated. Additionally, two preconditioning levels were tested. Rats underwent Achilles tendon transection and were euthanized 12 days postoperatively. Statistical analyzes were done with one-way ANOVA or Student’s t-test. Tissue force and stress were unaltered by storage and preconditioning compared to fresh samples, while high preconditioning increased the stiffness and modulus (p ≤ 0.007). Furthermore, both storage conditions did not modify the viscoelastic properties of the healing tendon, but altered transverse area, gap length, and water content. Cell viability was reduced after freezing. In conclusion, preconditioning on healing tissues can introduce mechanical data bias when having extensive tissue strength diversity. Storage can be used before biomechanical testing if structural properties are measured on the day of testing.
Similar content being viewed by others
Introduction
Biomechanical tests of various tissues are an essential part of experimental research to understand and improve connective tissue biology. However, these tests are not always possible to conduct straight after tissue collection, as transportation to test facilities or multiple collection time-points are sometimes needed. Therefore, storage of the samples at different temperatures (e.g. at 8 °C in the fridge or at − 18 °C in the freezer) is recurrently required. Tendon research often uses animal models to study the development of tendon healing and mechanical parameters are frequently the main outcomes1,2,3,4. Tendons heal through formation of a fibrovascular scar tissue by an orchestra of different biological mechanisms and the material and structural properties of the newly formed tissue are important to verify its function1,2,5. Hence, it is fundamental to understand how storage can affect various tissue properties. The effect of storage has been studied on intact tendons but not on healing tendons to our knowledge. Previous studies on intact tendons have somewhat diverging results. Freezing has been shown to alter some structural and mechanical parameters such as ultimate force, stress and modulus6,7. On the other hand, another study has shown that freezing or repeatedly freeze-thawing cycles did not affect intact tendons even on microscale level8. Although damage in the interfibrillar space was observed, the load-bearing collagen was not affected8.
Precondition of tendon specimens prior to biomechanical testing is a common laboratory routine, in order to normalize the load history of unequal samples9. This technique has been shown to influence the collagen fiber re-alignment in the intact tendon10. However, the advantage of preconditioning on intact tendons might not be the same for healing tendons as the tissue composition differs. Healing tendons are often weaker, contain more water and proteoglycans, are less stiff, and have more viscoelastic behavior4,11. Twelve days of healing in rat Achilles tendon corresponds to the proliferatory/early remodeling phase2 and samples collected at this stage display a large callus tissue that is hypercellular and contain disorganized collagen fibers12. Moreover, the healing tendons also comprise two types of tissue with different material properties; a dense intact/old tendon stump and a loose newly formed tissue2,13. Less is known about how preconditioning influences this newly formed connective tissue. This knowledge is an important issue for future studies and approaches.
Therefore, the objective of this study was to investigate if the elastic and viscoelastic properties of healing rat Achilles tendons were altered by short-term storage in the fridge or freezer. Furthermore, we also aimed to investigate how different levels of preconditioning influenced the mechanical properties of the healing Achilles tendons.
Results
The effect of storage in a pull-to-failure test (experiment 1)
No significant differences were seen for peak force, peak stress, energy uptake or stiffness between fresh samples and samples stored for 24 h at 8 °C in the fridge or after 7 days at − 18 °C in the freezer (Table 1). However, estimation of elastic modulus was increased by 48% after 1 week of storage in the freezer (p = 0.048), when compared with the fresh samples. Furthermore, when compared to the fresh samples, gap length was longer in the frozen samples (p < 0.001), while transverse area was larger in the refrigerated samples (p = 0.024).
The effect of storage on creep, water content and structural properties (experiment 2)
Viscoelastic properties, here measured by creep, were not altered by storage (Table 1). In contrast to experiment 1, there was no statistical difference in transverse area between the three groups, while gap length was decreased in the refrigerated samples compared to the fresh (p = 0.018). However, experiment 2 included structural measurements of the samples both before they were stored, and after storage, at the day of mechanical testing. Paired t-tests between these measurements showed an increased transverse area after storage, irrespective of temperature (fridge or freezer, p < 0.001 for both, Fig. 1). There was also an increased gap length between the pre and post storage measurement in the frozen samples but a decreased gap length in the refrigerated samples (p = 0.02 for both). There was a clear correlation between the pre and post measurement in the transverse area for the fresh (R2 = 0.949) and the frozen (R2 = 0.866) samples (p < 0.001 for both) but not for the refrigerated samples (R2 = − 0.099, p = 0.393). A significant correlation between the measurements of the gap length was seen in all groups (p < 0.02). The water content was increased after storage (p < 0.001; Table 1), primarily due to increased levels in the frozen samples (p < 0.001) but not in the refrigerated samples (p = 0.087).
Transverse area and gap length measurements from experiment 2. Measurements were done before samples were stored in the fridge or freezer and after storage, at the mechanical testing day (n = 10). The line represents the mean and the bars SD. Image created using GraphPad Prism software, version 8. https://www.graphpad.com/scientific-software/prism/.
The effect of preconditioning in a pull-to-failure test (experiment 1 and 2)
A high level of preconditioning with 5 cycles up to 5 N (Experiment 1) did not affect the peak force or the peak stress, but it resulted in an increased stiffness and estimated elastic modulus by 50–60% (p ≤ 0.007) compared to samples without any preconditioning (Fig. 2). A lower level of preconditioning with 5 cycles up to 2 N (Experiment 2) did not lead to any altered structural or material properties (Fig. 2).
Mechanical results from samples with or without preconditioning. Preconditioning in experiment 1 was performed with 5 cycles up to 5 N (n = 10) and preconditioning in experiment 2 was performed with 5 cycles up to 2 N (n = 9). The preconditioned samples were compared to control samples without any preconditioning. N = Newton; x = cycles. The line represents the mean and the bars SD. Image created using GraphPad Prism software, version 8. https://www.graphpad.com/scientific-software/prism/.
The effect of storage on tissue morphology and cell viability
Hematoxylin–Eosin staining showed regional variations in the healing tendons. There was overall more spacing between collagen fibers in both intact and healing tendons after storage in the freezer in comparison to fresh and refrigerated ones. Albeit, the spacing was more distinguishable in the intact tendons. Furthermore, the tissue appeared somewhat more disorganized in the refrigerated healing tendon compared to the fresh tendon. Both the MTT assay and the explant model demonstrated more live cells in fresh and refrigerated healing tendons compared to frozen tendons. The pattern was similar for the intact tendons, but with less intensity in the MTT assay due to less cells (Fig. 3).
Tissue morphology and cell viability. (A, B) Macroscopic and microscopic images from intact and healing tendons after storage. Microscopic images are stained with hematoxylin–eosin. Scale bar for intact tendons 50 µM and healing tendons 20 µM. (C) Images of 6-well plates after the dissolvement of formazan crystals in DMSO. Graph represents the MTT assay on intact and healing tendons, verified by absorbance (OD) measurements. The OD is normalized against tissue dry weight. The line represents the mean and the bars SD. (D) Explant culture with intact and healing tendons after two weeks. Notice the explants in the frozen samples, where no fibroblast growth was verified. Scale bar 200 µM. Images created by using the software cellsSens Entry (version 1.8.1, Olympus Corporation, www.olympus-sis.com), Dino Capture 2.0 (version 1.5.3.4, AnMO Eletronics Corporation, www.dino-lite.com), Zen 2 (blue edition, version 2.0.0.1, Zeiss, www.zeiss.com) and GraphPad Prism (version 8, https://www.graphpad.com/scientific-software/prism/).
Discussion
Biomechanical testing is an important resource used to analyze structural and material properties of different connective tissues. In this study, we compared if fresh healing rat Achilles tendons (tested straight after harvest) showed different mechanical proprieties compared to samples that have been stored either in the fridge (for 24 h) or in the freezer (for 1 week). Our results showed that peak force, peak stress, energy uptake, stiffness, and creep were all insensitive to storage. However, structural properties such as transverse area and gap length could indeed be altered by storage mainly through an increased water influx. These findings suggest that samples can be stored before mechanical testing, but measurements of structural properties should preferably be done at the day of testing, under equal conditions.
Our results are partly in line with previous studies on intact tendons. Studies using a single freeze–thaw cycle have also shown unaltered mechanical parameters when performing pull-to-failure or stress-relaxation tests8,14,15. On the other hand, it has been reported that the ultimate tensile failure can be altered in intact tendons after storage in the freezer7, and that repeated freeze/thaw cycles can lead to a reduced maximum load, maximum stress, and changes in collagen fibers alignment6. We observed a 48% increase in elastic modulus after the samples were stored in the freezer. This both contrast and corroborate with results from intact tendons where static or dynamic modulus have been shown to be either reduced or increased after a single or multiple freeze–thaw cycles7,14. Our measurements of static elastic modulus was done by normalization of the stiffness against transverse area and gap length, which were both altered by freezing. Taken together this suggests that elastic modulus is sensitive to freezing temperatures. Hence, the storage of samples should be chosen carefully when the elastic modulus is the main interest. Furthermore, healing tissues are morphologically different from the intact tendons, as seen in our macroscopic and microscopic images. Intact tendons contain a highly organized dense extracellular matrix, mainly composed of collagen type I and few cells16. On the other hand, injured tendons contain a disorganized loose connective tissue, with a higher water content, and show hypercellularity12. The tissue heals through formation of a fibrous scar tissue that forms a huge callus. The callus tissue will decrease in size over time when the matrix is replaced with a more functionally material4,5. The difference in extracellular matrix composition, cell number, and water content in these tissues could explain the differences between our study and previous ones.
An increased transverse area was found after storage in both the refrigerated and frozen samples compared to the fresh. Upon storage in either the fridge or freezer, samples were wrapped in gauze containing saline solution, and frozen samples were slowly thawed in the fridge overnight prior to the mechanical testing. This could explain why also the frozen samples absorbed more water and increased in size. In fact, frozen samples had significantly higher water content compared to fresh samples. Albeit not significant, the refrigerated samples also contained more water compared to fresh. The increased water content was also visualized in the microscopical images by spacing between the collagen fibers. An increased water content might be related to an larger extracellular area due to cell shrinkage, and this effect has been shown to be correlated with freezing time rather than temperature17. The storage time might therefore be an important factor to take into consideration. The time-points chosen in this study regarding storage condition were based on laboratory routines. When the use of fresh samples is unworkable, samples are instead stored for a maximum of 24 h in the fridge or 1 week in the freezer, and this can still be considered as a short-term storage. A prolonged storage time could potentially have more deleterious effects. Intact Achilles tendons respond differently to short or long-term storage in the freezer: long period (9 months) and repeatedly thawing (up to 5) lead to tissue deterioration while short periods (up to 3 months) and once or twice thawing do not have major effects on mechanical properties15.
The effect of long-term storage on healing tendons has not been studied here and might be important to evaluate in the future. Furthermore, we used pull-to-failure test or creep test while performing this study. The use of stress-relaxation tests or frequency sweeps in a dynamic protocol could reveal changes in for examples dynamic modulus or changes at different strain levels. Such protocol would provide a wider view of the viscoelastic properties of the healing tendon after different storage conditions and preconditioning levels. A previous study using a dynamic protocol on intact tendons showed changes in dynamic Young’s modulus after repeated freeze–thaw cycles, while no change in static Young’s modulus was observed14. However, healing tendons are weaker than intact tendons and the use of prolonged dynamic protocols could be complex. It has been shown that prolonged protocols on healing tendons can result in tendon failure before the final pull-to-failure test18. Another aspect to consider with healing tendons is the regional variation in matrix organization as seen in the histological evaluation in this study as well as in other studies18,19. Mechanical evaluation on regional differences in tendon properties might reveal even more insights in the effect of storage and preconditioning in the future.
The transverse area in experiment 1 was measured on the day of mechanical testing, hence, at different days for each group as all surgeries were performed on the same day. The different time-points of sample measurements can be considered as a limitation of this study. Therefore, in the second experiment, we performed the surgeries on different days to allow measurement and testing of all samples on the same day. To further clarify how the healing tendon tissue is affected by storage regarding structural properties, each sample was measured twice, first prior to the storage and thereafter straight before mechanical testing. Experiment 1 showed an increased transverse area in the fridge-stored samples but not in the frozen samples while experiment 2 showed no significant difference between the groups on the day of testing. However, paired t-tests of the measurements pre and post storage showed an increased transverse area after both storage conditions. On the other hand, we also observed that the gap length was affected differently depending on the storage condition in both experiment 1 and 2. Samples stored in the fridge had a decreased gap length whereas freezing increased the length. The changes in gap length might be linked to cell-mediated effects. Freezing tissues without cell protective actions leads to cell degradation as shown in frozen tendons and ligaments14,20 while short term storage at 4 °C normally protects cells. Our findings with the MTT assay and explant culture corroborate that cell viability is preserved when tendons are stored in the fridge but not in the freezer. Tendon cells in vitro can pull on the unloaded matrix21,22. Our tendons in the fridge are unloaded and therefore possibly subjected to cell-mediated extracellular matrix contraction during the storage time. This could perhaps explain the shorter gap length finding as well as the more disorganized appearance in the healing matrix after fridge storage compared to fresh and frozen samples. This contrast to the cells from frozen samples that die14, and possible instead release their tension to the extracellular matrix and perhaps have a disrupted cell-to-cell connection, which could explain the increased gap length. Frozen explants did not proliferate when cultured for 2 weeks, whereas refrigerated and fresh samples showed cell growth. Besides, frozen tissues also form ice crystals and the total tissue volume cannot contract due to this. Furthermore, sample storage in the freezer can trigger changes in morphological appearance, and together with the osmosis process, result in mechanical damage to the cellular structures17.
Another important finding with our study was the diverse response between the preconditioning levels in healing Achilles tendons. Five cycles up to 5 N lead to significantly stiffer tendons while five cycles up to 2 N showed no difference between the groups. This demonstrates the importance of knowledge on tissue strength prior to preconditioning execution. This might also limit the use of preconditioning in experiments where groups differ greatly in total strength, as the same protocol could potentially result in different strain levels. The strength of the healing tissue differs more compared to intact tendons depending on the treatment, such as loading conditions, drug exposure and the length of the healing period used in each study1,2,13,23,24. The 5 N of preconditioning corresponded to ~ 15% of the maximum force of the healing tendon, while 2 N corresponded to ~ 4% of the maximum force. The lack of an overall and a specific effect on peak force when using low preconditioning on healing tendons contrast to what has previously been shown on intact tendons. Preconditioning performed at ~ 1–3% of the ultimate failure load on intact tendons led to increased ultimate failure load and stress25.
In conclusion, there were no major effects on the peak force, stress, or viscoelastic properties of the healing tendon after different storage conditions or preconditioning levels. However, freezer storage has a major effect on cell viability, in contrast to fridge storage or fresh samples. Notwithstanding, different storage conditions should be carefully considered when elastic modulus, water content, transverse area, or gap length are the primary outcomes. It is also important to consider the strength of different groups (e.g. different treatment groups) when preconditioning is used. If the strength differs too much between groups, one might encounter unspecific differences due to the preconditioning level. Furthermore, it is essential to store all samples in an equivalent way and to perform measurements of structural properties (e.g. transverse area and length) on the day of mechanical testing and not straight after tissue collection.
Methods
Study design
In total, 103 female specific-pathogen free (SPF) Sprague–Dawley rats 10–11 weeks old (Janvier, Le Genest-Saint-Isle, France), weighing on average 252 g (SD20) were used in three separate experiments to study how elastic and viscoelastic properties of healing Achilles tendon are affected by different storage conditions and preconditioning levels.
Experiment 1
Achilles tendon transection was performed on 40 rats (all on the same day) and the animals were randomized to 4 different groups; Fresh/No preconditioning, Fridge, Frozen and Preconditioning high (Table 2). Sample collection was performed 12 days post-surgery (Fig. 4) and followed by mechanical testing (Fig. 5). Before the samples were subjected to a pull-to-failure test, the refrigerated samples were stored for 24 h at 8 °C and the frozen samples were stored for 7 days at − 18 °C. This test was therefore performed on different days for each group. The fresh, refrigerated, and frozen samples were all tested by a pull-to-failure test without preconditioning.
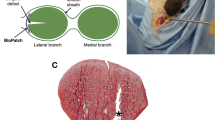
Experimental setup. (A) On day 0, a transversally skin incision was performed on the right hind limb and the tendon complex was exposed. The plantaris tendon was removed and the Achilles tendon was transected. (B) Animals were euthanized and tissue samples were collected 12 days post-surgery. (C) Samples were fixed in a metal clamp in the material-testing machine. Mechanical testing was performed according to each group.
Representative overview of the type of mechanical test and preconditioning level performed in each experiment. Graphs are from a fresh sample. (A, B) represents the preconditioning graph, where 5 cycles of 2 N (A) or 5 N (B) were applied. (C) Pull-to-failure test. (D) Creep test with a constant load of 8 N for 300 s. Graphs were obtained from the mechanical testing (100R; DDL INC., EDEN PRAIRIE, MN) software MtestW, version5.1.0 (ADMET). https://www.admet.com.
In the preconditioned high group, samples were fresh and subjected to 5 cycles of 5 N of preconditioning before the pull-to-failure test. This group was thereafter compared to the fresh samples with no preconditioning.
Experiment 2
48 rats were randomized to 5 different groups prior to the surgery; fresh, fridge, frozen, preconditioning low and no preconditioning. In contrast to experiment 1 (where we saw structural changes in the stored tendons), the Achilles tendon transection surgery was executed on different days to allow mechanical testing on the same day for all samples. Fresh, refrigerated, and frozen samples (n = 10/group) were all pre-conditioned with 5 cycles up to 2 N prior to a creep test. The transverse area and gap length were measured twice in experiment 2, straight after tissue collection and after storage (on the day of mechanical testing). The water content from the healing tendons was also measured in experiment 2, after the mechanical test. The two groups: preconditioning low and no preconditioning (n = 9/group) were subjected to a pull-to-failure test as in experiment 1, with or without a lower level of preconditioning of 5 cycles up to 2 N (as high preconditioning had an effect on stiffness and modulus in experiment 1).
Experiment 3
15 rats were randomized into three groups: fresh, fridge and frozen. Rat Achilles tendon was transected on different days and stored as the previous experiments. This enable data collection at the same time point. Both healing and intact tendons were used for histology (n = 1), MTT assay (n = 3), and explant culture (n = 1).
Animals and housing
The animals were kept in acrylic cages, in pairs, and placed on ventilated racks under controlled humidity (55%) and temperature (22 °C) with the light–dark cycle of 12 h each. Standard food pellets and water were given ad libitum. All cages were provided with shredded paper, wooden pegs and hiding places. The experiments adhered to the institutional guidelines for the care and treatment of laboratory animals. The Regional Ethics Committee for animal experiments in Linköping, Sweden, approved all the experiments (ID1424).
Tendon injury
All animals were anesthetized with isoflurane gas and laid in a prone position. The skin on the right leg was shaved and cleaned with chlorhexidine ethanol. Subcutaneously antibiotic injection was given once preoperatively (25 mg/kg oxytetracycline) and analgesics injections were given pre- and postoperatively every 8–12 h for a period of 48 h (0.045 mg/kg buprenorphine, subcutaneously). The surgery day was counted as day 0. A small skin incision, lateral to the Achilles tendon was made and the tendon complex was exposed (Fig. 4A). The plantaris tendon was removed and the Achilles tendon was cut transversely in the middle part, using a no.15 surgical blade mounted in a scalpel, and left unsutured. The skin was closed with 2 stitches using a 4/0 non-absorbable monofilament suture (DAFILON). This procedure was performed under aseptic conditions and has been described elsewhere1,2.
Sample collection and storage conditions
Twelve days after the surgery, the rats were euthanized with carbon dioxide and samples were collected (Fig. 4B). The right Achilles tendon, together with the calcaneal bone and calf muscle, was harvested and placed in gauze with 0.9% saline solution. The sagittal and transverse diameter of the midpart of the callus tissue was measured immediately after collection using a slide caliper, and the transverse area was calculated by assuming an elliptical geometry. The distance between the old tendon stumps was visualized through transillumination and the gap length was measured by a caliper. Fresh samples were tested mechanically the same day as the animals were euthanized. The remaining samples were either stored in the fridge (8 °C) for 24 h or in the freezer (− 18 °C) for 1 week. Frozen samples were thawed slowly, overnight in the fridge, before mechanical testing performance.
Mechanical testing
The major part of the muscle tissue was removed from the tendon, and the proximal part of the tendon was fixed in a metal clamp between two pieces of sandpapers. The calcaneal bone was fixed in a custom-made clamp at 30° dorsiflexion relative to the direction of traction in the material-testing machine (100R; DDL INC., EDEN PRAIRIE, MN) (Fig. 4C).
Preconditioning
Ten samples from experiment 1 and 38 samples from experiment 2 were preconditioned prior to the data recording test (pull-to-failure or creep test, Fig. 5). The preconditioning high group in experiment 1 was subjected to 5 cycles of 5 N (Fig. 5B) at a speed of 0.1 mm/s or and the preconditioning low group was subjected to 5 cycles of 2 N using the same speed (Fig. 5A). All groups subjected to the creep test in experiment 2 (fresh, fridge, and frozen samples) were preconditioned before the creep test (5 cycles of 2 N, Fig. 5A).
Pull-to-failure test
Samples were pulled at a constant speed of 0.1 mm/s until failure (Fig. 5C). Peak force at failure (N) and energy uptake until failure (N/mm) were measured by the machine software (MtestW, version5.1.0, ADMET). A linear portion of the elastic phase of the curve was marked by the investigator, for automated stiffness (N/mm) calculation by the machine software. Peak stress (MPa) and estimate of elastic modulus (MPa) were calculated assuming an elliptical cylindrical shape and homogeneous mechanical properties. Estimation of elastic modulus was calculated as stiffness × gap length/transverse area and peak stress as peak force/transverse area1,2.
Creep test
Samples were pulled to 8 N (2 mm/s) and thereafter kept under a constant load of 8 N for 300 s (Fig. 5D). The viscoelastic properties of the healing tendons were measured through the progressive deformation of the tissue and calculated as a percentage of the starting length.
MTT (colorimetric) assay
A MTT assay was used for quantification of cell viability after storage. The tendons were incubated for 3 h in DMEM/F-12 without phenol red (gibco) with 0.5 mg/mL MTT solution (3-4,5dimethylthiazol-2yl)-2,5-diphenyltetrazolium bromide), on an orbital shaker protected from light. The tendons were thereafter transferred to 7 mL DMSO and kept 1hour on an orbital shaker, protected from light. Purple formazan crystals were dissolved and 100 μL DMSO solution was used for absorbance reading. Absorbance was quantified at 550 nm with 680 nm as the reference wavelength. The darker the solution, the higher the number of active/viable cells. The absorbance value (OD) was normalized to the tissue dry weight.
Explant culture
Intact and healing tendons after storage were cleaned in PBS containing 1% penicillin–streptomycin (10.000 U/mL, gibco). Samples were cut into small pieces and placed in 25 cm2 cell culture flasks. Explants were kept for two weeks in culture with DMEM/F-12 containing l-glutamine, no phenol red and hepes (gibco), supplemented with 10% FBS (fetal bovine serum, heat inactivated, South American origin, gibco) and 1% penicillin–streptomycin (10.000 U/mL, gibco). After two weeks, fibroblast growth was confirmed by using a microscope (Axio Vert.A1 fluorescence microscope Carl Zeiss) with an N‐Achroplan 10 ×/0.25 objective (Carl Zeiss) and Axiocam 503 color camera (Carl Zeiss) Zen 2 (blue edition, version 2.0.0.1, Zeiss).
Histology
Intact and healing tendons were stored accordingly and thereafter fixed in 4% phosphate-buffered formaldehyde overnight, followed by dehydration and paraffin embedding (n = 1 for each group: fresh, refrigerated and frozen). Longitudinal sections (7 µM) were made and haematoxylin–eosin (HE) staining was performed. Images were captured using a light microscope (Olympus BX51) with an attached camera (Olympus DP73) and the software cellsSens (Entry version 1.8.1, Olympus Corporation). An UPlanFI 10 ×/0.30 objective lens was used for the healing tendons, while 20 ×/0.50 objective lens was used for the intact ones.
Water content measurement
Subsequently to the mechanical test performed in experiment 2, samples were weighted and then dried in a freeze-drying chamber (SAVANT, FDC206) for 24 h. Afterward, samples were weighted once more and the water content of each sample was calculated and normalized to the initial wet weight (%).
Statistics
GraphPad Prism software version 8 was used for data analyses. The primary variable outcome for the pull-to-failure and preconditioning test was peak force. For the creep test, the viscoelastic propriety of the healing connective tissue was considered the primary outcome. A one-way ANOVA was used to analyze differences between the three storage conditions (fresh, fridge or freezer) followed by a Dunnett’s multiple comparisons test where the two storage groups were compared to the fresh control group. A student’s t-test for independent samples was used to analyze the effect of preconditioning on fresh samples. A paired t-test and paired sample correlation analysis were used to investigate the measurements differences from before and after storage conditions (fridge and freezer) for transverse area and gap length.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Dietrich, F. et al. Effect of platelet-rich plasma on rat Achilles tendon healing is related to microbiota. Acta Orthop. 88, 416–421. https://doi.org/10.1080/17453674.2017.1293447 (2017).
Dietrich-Zagonel, F. et al. Stimulation of tendon healing with delayed dexamethasone treatment is modified by the microbiome. Am. J. Sports Med. 46, 3281–3287. https://doi.org/10.1177/0363546518799442 (2018).
Aspenberg, P. & Virchenko, O. Platelet concentrate injection improves Achilles tendon repair in rats. Acta Orthop. Scand. 75, 93–99. https://doi.org/10.1080/00016470410001708190 (2004).
Eliasson, P., Andersson, T. & Aspenberg, P. Rat Achilles tendon healing: Mechanical loading and gene expression. J. Appl. Physiol. 107, 399–407. https://doi.org/10.1152/japplphysiol.91563.2008 (2009).
Galatz, L. M., Gerstenfeld, L., Heber-Katz, E. & Rodeo, S. A. Tendon regeneration and scar formation: The concept of scarless healing. J. Orthop. Res. 33, 823–831. https://doi.org/10.1002/jor.22853 (2015).
Chen, L. et al. Effect of repeated freezing-thawing on the Achilles tendon of rabbits. Knee Surg. Sports Traumatol. Arthrosc. 19, 1028–1034. https://doi.org/10.1007/s00167-010-1278-y (2011).
Clavert, P. et al. Effects of freezing/thawing on the biomechanical properties of human tendons. Surg. Radiol. Anat. 23, 259–262. https://doi.org/10.1007/s00276-001-0259-8 (2001).
Lee, A. H. & Elliott, D. M. Freezing does not alter multiscale tendon mechanics and damage mechanisms in tension. Ann. N. Y. Acad. Sci. 1409, 85–94. https://doi.org/10.1111/nyas.13460 (2017).
Graf, B. K., Vanderby, R. Jr., Ulm, M. J., Rogalski, R. P. & Thielke, R. J. Effect of preconditioning on the viscoelastic response of primate patellar tendon. Arthroscopy 10, 90–96. https://doi.org/10.1016/s0749-8063(05)80298-1 (1994).
Miller, K. S., Edelstein, L., Connizzo, B. K. & Soslowsky, L. J. Effect of preconditioning and stress relaxation on local collagen fiber re-alignment: Inhomogeneous properties of rat supraspinatus tendon. J. Biomech. Eng. 134, 031007. https://doi.org/10.1115/1.4006340 (2012).
Wang, J. H. Mechanobiology of tendon. J. Biomech. 39, 1563–1582. https://doi.org/10.1016/j.jbiomech.2005.05.011 (2006).
Dietrich, F. et al. Platelet-rich fibrin promotes an accelerated healing of Achilles tendon when compared to platelet-rich plasma in rat. World J. Plast. Surg. 4, 101–109 (2015).
Hammerman, M., Dietrich-Zagonel, F., Blomgran, P., Eliasson, P. & Aspenberg, P. Different mechanisms activated by mild versus strong loading in rat Achilles tendon healing. PLoS ONE 13, e0201211. https://doi.org/10.1371/journal.pone.0201211 (2018).
Hochstrat, E. et al. Cryopreservation of tendon tissue using dimethyl sulfoxide combines conserved cell vitality with maintained biomechanical features. PLoS ONE 14, e0215595. https://doi.org/10.1371/journal.pone.0215595 (2019).
Quirk, N. P. et al. Effects of freeze-thaw on the biomechanical and structural properties of the rat Achilles tendon. J. Biomech. 81, 52–57. https://doi.org/10.1016/j.jbiomech.2018.09.012 (2018).
Rufai, A., Ralphs, J. R. & Benjamin, M. Structure and histopathology of the insertional region of the human Achilles tendon. J. Orthop. Res. 13, 585–593. https://doi.org/10.1002/jor.1100130414 (1995).
Schafer, A. T. & Kaufmann, J. D. What happens in freezing bodies? Experimental study of histological tissue change caused by freezing injuries. Forensic Sci. Int. 102, 149–158. https://doi.org/10.1016/s0379-0738(99)00043-2 (1999).
Khayyeri, H. et al. Diminishing effects of mechanical loading over time during rat Achilles tendon healing. bioRxiv https://doi.org/10.1101/2020.07.14.202077 (2020).
Sasaki, K., Yamamoto, N., Kiyosawa, T. & Sekido, M. The role of collagen arrangement change during tendon healing demonstrated by scanning electron microscopy. J. Electron. Microsc. 61, 327–334. https://doi.org/10.1093/jmicro/dfs057 (2012).
Woo, S. L., Orlando, C. A., Camp, J. F. & Akeson, W. H. Effects of postmortem storage by freezing on ligament tensile behavior. J. Biomech. 19, 399–404. https://doi.org/10.1016/0021-9290(86)90016-3 (1986).
Herchenhan, A., Dietrich-Zagonel, F., Schjerling, P., Kjaer, M. & Eliasson, P. Early growth response genes increases rapidly after mechanical overloading and unloading in tendon constructs. J. Orthop. Res. 38, 173–181. https://doi.org/10.1002/jor.24513 (2020).
Bayer, M. L. et al. Release of tensile strain on engineered human tendon tissue disturbs cell adhesions, changes matrix architecture, and induces an inflammatory phenotype. PLoS ONE 9, e86078. https://doi.org/10.1371/journal.pone.0086078 (2014).
Dietrich-Zagonel, F., Hammerman, M., Eliasson, P. & Aspenberg, P. Response to mechanical loading in rat Achilles tendon healing is influenced by the microbiome. PLoS ONE 15, e0229908. https://doi.org/10.1371/journal.pone.0229908 (2020).
Bernhardsson, M., Dietrich-Zagonel, F., Tatting, L., Eliasson, P. & Aspenberg, P. Depletion of cytotoxic (CD8+) T cells impairs implant fixation in rat cancellous bone. J. Orthop. Res. 37, 805–811. https://doi.org/10.1002/jor.24246 (2019).
Teramoto, A. & Luo, Z. P. Temporary tendon strengthening by preconditioning. Clin. Biomech. 23, 619–622. https://doi.org/10.1016/j.clinbiomech.2007.12.001 (2008).
Acknowledgements
The Swedish Research Council (VR2017-00990), the Swedish National Centre for Research in Sports (P2018-0140, P2019-0053), Linköping University and Östergötland Country Council (LIO-796831) for their funded for this study.
Funding
Open Access funding provided by Linköping University Library.
Author information
Authors and Affiliations
Contributions
F.D.Z and P.E designed the research; F.D.Z, M.H and M.B performed the research; F.D.Z and P.E analyzed data; F.D.Z and P.E wrote the paper. All authors have read and approved the final submitted manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Dietrich-Zagonel, F., Hammerman, M., Bernhardsson, M. et al. Effect of storage and preconditioning of healing rat Achilles tendon on structural and mechanical properties. Sci Rep 11, 958 (2021). https://doi.org/10.1038/s41598-020-80299-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-80299-w
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.