Abstract
To investigate synovitis’ influence on early knee osteoarthritis (EKOA) by serum biomarkers and magnetic resonance imaging (MRI) findings in Japanese women. We enrolled 255 women aged 30–70 without radiographic abnormalities (Kellgren–Lawrence grade ≥ 2). Knee injury, OA outcome scores (KOOS), clinical examinations, and standing radiograph were used for classification criteria of EKOA. Participants were classified into normal knee group and EKOA group. All participants underwent MRIs of their right knee. The amount of effusion-synovitis volume was quantified. We compared serum matrix metalloproteinases-3 levels (MMP-3), high-sensitivity C-reactive protein, interleukin-6, and adiponectin between the groups. The relationship between synovitis and EOKA was investigated using multiple linear regression. Fifty-four participants (21%) were classified as EKOA. Serum MMP-3 concentration and effusion-synovitis volume were higher in patients with EKOA (p = 0.025 and p = 0.001, respectively). Effusion-synovitis volume negatively correlated with all KOOS subscales and positively correlated with serum MMP-3 concentration. Serum MMP-3 concentration was associated with effusion-synovitis volume β = 0.60, p < 0.001). There was mildly active but definitive synovitis in EKOA. This was an observational study so that no conclusions can be drawn regarding cause-effect for synovitis and symptoms. Future studies should conduct follow-up of participants with synovitis to assess the progression of knee OA.
Similar content being viewed by others
Introduction
Knee osteoarthritis (OA) is a major joint disease that causes chronic pain, stiffness, and disability, especially in the aging population1,2. It requires high-cost treatment, such as arthroplasty, decreases productivity, and creates absence from work; therefore, knee OA imposes a substantial and growing burden on society3. Although early intervention or preventive approaches are needed, the timing and identifying methodology are not established, as conventional standard diagnosis and assessment are conducted mainly based on the Kellgren–Lawrence (KL) grading on radiographs4, thus making it difficult to detect early and minute changes.
Recently, new criteria for detecting early knee OA were proposed by the first international EKOA workshop (EKOA) without radiographic abnormalities5; they allow identification of people with moderate knee symptoms who have same risk factors as those with definitive knee OA. EKOA prevalence was 9.5% in men and 15.0% in women, and the highest prevalence was noted in middle-aged females6. Nevertheless, EKOA’s etiology has not been well studied.
Several biomarkers are frequently used to assess disease activity precisely and quantitatively. There are reports regarding the availability of serum biomarkers to evaluate synovitis at an early phase and to predict OA progression. Interleukin-6 (IL-6) and keratan sulfate levels increase in the early phase of knee OA accompanied by knee pain7,8. Magnetic resonance imaging (MRI) is a useful imaging biomarker for assessing early phase of knee OA. The Framingham osteoarthritis study suggested that the prevalence of any abnormality was seen in 89% of participants without radiographic abnormalities9. These findings suggest that MRI can detect features suggestive of knee osteoarthritis that cannot be visualized on conventional radiographs; nevertheless, the correlation between MRI findings and EKOA detected using the new criteria is unclear.
Synovitis is an important factor for determining the incidence and progression of knee OA10. Inflamed synovium secretes proteases such as MMP-3 and disintegrins and metalloproteinases with thrombospondin motifs (ADAMTSs), as well as cytokines such interleukin 1β and tumor necrosis factor α, all of which damage the cartilage matrix11. Evidence of synovitis using serum biomarkers8,12,13, MRI14,15,16, and arthroscopic findings9 are related to the rapid progression of knee OA; nevertheless, these examinations are contraindicated in clinical practice and large epidemiological studies because they are expensive and time-consuming. Some studies investigate the importance of biomarkers in those with early stage of knee OA in large sample cohort studies7,10. Elucidating the prevalence of synovitis in patients with symptomatic knees without radiographic abnormalities and diagnostic serum biomarkers may lead to a better understanding of the pathology and the potential for therapeutic intervention.
We focused on middle-aged women in our large sample cohort of the general Japanese population to identify those at high-risk for developing knee OA. We investigated relationships among serum biomarkers of synovitis and MRI findings. Furthermore, we compared serum biomarker concentrations and synovitis activity as evaluated by MRI between normal knees and EKOA in middle-aged women. We hypothesized that the presence of synovitis would be demonstrated in those with EKOA, and that the severity of symptoms would correlate with synovitis biomarkers, even in individuals without radiographic abnormalities.
Results
The number of participants with normal knee were 201(79%), and with EKOA were 54 (21%); the number of participants diagnosed with EKOA was 2 in the 30–39-year-old group, 14 in the 40–49-year-old group, 19 in the 50–59-year-old group and 12 in the 60–70-year-old group; the mean age was 54.5 ± 9.3 years, and the mean BMI was 22.1 ± 3.1 kg/m2; finally, age and BMI showed no significant difference between the normal and EKOA groups (p = 0.341 and p = 0.299, respectively) (Table 1).
The mean serum MMP-3 concentration was 32.5 ± 10.2 ng/ml in the normal group and 39.0 ± 38.3 ng/ml in the EKOA group (p = 0.025), while the other serum biomarkers showed no significant differences (Table 2). The serum MMP-3 concentration had a weak positive correlation with serum IL-6 concentration (r = 0.157, p = 0.040) and adiponectin concentration (r = 0.208, p = 0.025).
The mean synovial score was 0.2 ± 0.4 in the normal group and 0.6 ± 0.9 in the EKOA group; the mean effusion-synovitis volume was 2.0 ± 1.3 cm3 in the normal group and 3.5 ± 4.6 cm3 in the EKOA group. Both the synovial score and the effusion-synovitis volume in the EKOA group were significantly higher than those in the normal group (p = 0.003 and p = 0.001, respectively) (Fig. 1). There was a weak positive correlation between serum MMP-3 concentration and effusion-synovitis volume (r = 0.176, p = 0.003) (Table 3). The other serum concentrations were not correlated with effusion-synovitis volume (hs-CRP; p = 0.181, IL = 6; p = 0.203, adiponectin; p = 0.437). All KOOS subscales correlated negatively with effusion-synovitis volume (Fig. 2; Table 3). Multivariate regression analysis showed that effusion synovitis volume was associated with serum MMP-3 concentration (p < 0.001), but not associated with the other serum inflammation biomarkers (Table 4). According to the ROC analysis, the optimal effusion-synovitis volume cut-off value to detect EKOA (AUC = 0.578; odds ratio: 2.40; p = 0.013; Fig. 3) was 2.42 cm3. Using this cutoff value, 71 out of 250 patients (28%) demonstrated effusion-synovitis volume of more than 2.42 cm3. Among them, 35% of patients (25 of 71) were diagnosed with EKOA; sensitivity was 46% and specificity was 77%.
Synovial score and effusion synovitis volume in the normal and EKOA group. Mean values of synovitis score (a) and effusion synovitis volume (b) between normal and EKOA groups were compared using the Mann–Whitney U test. The error bars represent the standard deviation. A p-value below 0.05 was considered significant (*). EKOA early knee osteoarthritis.
Scatter gram of the effusion-synovitis volume and knee injury and osteoarthritis outcome scale subscales. The x-axis corresponds with each KOOS subscale, and the y-axis corresponds with effusion-synovitis volume (cm3) evaluated by magnetic resonance imaging. All subscales of KOOS were negatively correlated with effusion-synovitis volume. KOOS knee injury and osteoarthritis outcome scale.
Discussion
This is the first study to report the relationship between serum biomarkers and MRI evaluations in the general Japanese population with EKOA, which was diagnosed based on the new criteria proposed by Luyten et al. Both the mean serum MMP-3 concentrations and the effusion-synovitis volume were higher in the EKOA group than those in the normal group. Multiple regression analysis showed that serum MMP-3 concentration was associated with mild effusion-synovitis detected on MRI. These results suggest that, although not substantial, there is mildly active but definitive synovitis in EKOA. Effusion synovitis may play a role in the etiopathogenic events leading to knee OA and potentially contribute to further progression. MRI could be useful to assess a symptomatic knee joint with no radiographic abnormalities.
Early identification of changes to the knee at an early phase of OA may help prevent the progression to definitive OA. Although many studies had reported the features of early phase of knee OA1,6,17,18, there was no clear definition for early phase of knee OA; however, Luyten et al. defined the new criteria5. Whilst EKOA is solely diagnosed based on mild knee pain and disabilities, it can be clearly distinguished from both normal and symptomatically abnormal knees. In their cohort study, Sasaki et al. reported that the highest prevalence of EKOA was observed in females aged ≥ 50 years, who had reduced knee function and QOL; the risk factors for EKOA were age, female sex, obesity, and previous knee injury, similar to those of definitive knee OA6.
The association of serum biomarkers and EKOA has not been well established. Serum MMP-3 is a diagnostic biomarker for rheumatoid arthritis19, and its levels were shown to correlate with synovitis20. MMP-3 is produced by synovial membrane cells and chondrocytes in response to increasing mechanical stimulation and exposure to inflammatory cytokines21. Although not all investigators agree that there is significant increase in the serum MMP-3 concentrations in patients with OA, Pengas et al. reported that knee synovial MMP-3 concentrations correlated with serum MMP-3 concentrations concluding that serum MMP-3 concentrations could be used as a potential biomarker for knee osteoarthritis and possible disease predictor22. Here, the mean serum MMP-3 concentration was higher in the EKOA group than in the normal group.
Previous study demonstrated that serum hs-CRP as well as IL-6 levels increased with the progression of knee OA; the levels of IL-6, but not those of hs-CRP, significantly associated with pain severity23. In addition, IL-6 is produced by adipose tissue, which accompanies obesity24,25. In the present study, although the mean BMI of participants with EKOA was slightly higher than those with normal knees (p = 0.524), serum IL-6 and hs-CRP concentrations showed no significant differences. This might be due to EKOA entailing relatively mild knee joint inflammation. Obesity is a risk factor and onset for knee OA26,28. Sowers et al. suggested that the mechanism of knee OA in obese patients might be a simple increase of mechanical burden on the joints27. Adiponectin, a 28–30 kDa collagen-like protein, is not only one of the most abundantly secreted adipose tissue proteins but also the only adipokine identified thus far that is negatively correlated with obesity29. A recent study found there was a positive correlation between adiponectin concentration and KL grade26. On the other hand, a few studies found no statistical association between adiponectin levels and OA28,30. Yusuf et al. suggested that the serum adiponectin concentration negatively correlated with the radiographic severity of OA and might play a protective role in the pathogenesis of OA31. Our data showed a negative relationship between serum adiponectin concentration and effusion-synovitis volume. These results may support the notion that obesity might be a risk factor for knee joint inflammation.
To date, EKOA’s etiology and pathology remain unclear. Knee OA is a systemic disorder with a multifactorial origin. Previous studies reported MRI features of knee OA without radiographic abnormalities. Harkey et al. reported that the presence of degenerative ligaments, effusion-synovitis, and meniscal pathology served as pre-radiographic structural features, which identified an increased risk of knee OA development over the next 4 years32. They also concluded that patients with effusion-synovitis greater than 11.9 cm3 were about 3 times more likely to develop knee OA 2 years prior to disease development, with this likelihood increasing to ~ 5.2 times in the year prior to the onset of advanced-stage disease. The CHECK study reported associations between baseline MRI abnormalities and development of radiographic knee OA following 5 years18. In the study, cartilage lesions, osteophytes, bone marrow lesions and effusion detected on MRI had significant associations with the progression of definitive knee OA. We showed that effusion-synovitis volume was significantly higher in the EKOA group than that in the normal group, and correlated with all KOOS subscales negatively. From the ROC analysis, the sensitivity was relatively high for detecting EKOA using a cutoff point of 2.42 cm3. However, AUC was not high. These results suggested that relatively low active synovitis affects knee pain, and might play one of the important etiological roles of EKOA.
This study has several limitations. First, it was a single-center study, and therefore may be subject to selection bias. For this reason, we instituted strict inclusion and exclusion criteria. Multi-center studies are needed to validate our findings. Second, we assessed knee effusion-synovitis using non-contrast enhanced MRI even though contrast-enhanced MRI (CE-MRI) is considered the gold standard. However, CE-MRI is challenging to apply in large OA studies due to costs, practicality, and rare but possible, side-effects related to the contrast agent33. Third, our data showed that serum MMP-3 concentrations significantly correlated with effusion-synovitis volume, but the correlation was relatively weak. Other systemic biomarkers should be investigated. Longitudinal observation of patients with high concentrations of inflammation biomarkers should be performed. Fourth, all participants in this study were women, and the sample size was modest. We performed MRI only on middle-aged women because of the high cost of MRI and because they are the preferred candidates for OA and EKOA. Fifth, KL grade 1 may represent some radiographic abnormalities. A previous study reported that bone attrition, osteophyte formation, and meniscus extrusion were observed in the KL 1 knees8,17. However, commonly used radiographic abnormality (knee OA) in a clinical situation was defined by KL grade ≥ 2. In the EKOA group, participants with KL1 knees had a larger synovitis volume than patients with KL0 knees, but without significant difference (p = 0.794). Finally, the differences between symptoms of normal ageing and EKOA are controversial34. The normal aging process should be taken into consideration while discussing about EKOA. Further longitudinal validation studies are needed. To this end, we are conducting regular follow-ups with the participants of this study to confirm the prognostic power of the new criteria.
Despite these limitations, our study has several important findings that have important clinical relevance concerning intervention for knee pain. We showed the relationship between serum biomarkers and EKOA. The result of MRI and serum biomarkers suggest that synovitis is associated with EKOA.
Conclusion
The serum MMP-3 concentration, effusion-synovitis volume, and synovial score are valuable metrics for elucidating the characteristics of EKOA. MRI could be used to detect mild synovitis in knees with EKOA. Synovitis might be one of the key factors for intervention in EKOA.
Materials and methods
Participants
All participants volunteered for the Iwaki Health Promotion Project, a community-based preventative medicine program that aims to improve the average life expectancy by conducting general health checkups and prophylactic interventions, as previously described12,13,17,35. The ethics committee of the our hospital approved the study (reference number: 2017-026), and all of participants gave written informed consent prior to participation.
A total of 1,073 volunteers (441 men and 632 women) participated in the project in 2017. Participants answered questionnaires regarding their past and present medical history, lifestyle, occupation, family history, onset of menopause, health-related QOL, and disease-specific information, such as knee symptoms. We focused on female participants aged 30 to 70 years with no radiographic abnormalities because the prevalence of EKOA is higher in middle-aged women6. We excluded 15, 31, 10, 15, 14 and 428 participants who had undergone knee arthroplasty, who did not undergo radiographs, with history of knee ligament injury or fracture, diagnosed rheumatoid arthritis, with positive anti-cyclic citrullinated peptide antibody, and who were male participants, respectively. Finally, 255 women who underwent MRI with no radiographic abnormalities (KL glade 0/1) were included in the analysis (Fig. 4).
Knee injury and osteoarthritis outcome score
Subjective evaluations of knee symptoms were obtained using knee injury and osteoarthritis outcome scores (KOOS), the most frequently used tool that represents patient-based outcome scores36,37. KOOS consists of 42 knee-related items, and each item was scored from 0 to 4. Summed scores in 4 subscales (symptom, pain, ADL and QOL) were converted to 100 points as their best condition. Their reliability and internal congruence were high38.
Serum inflammation biomarkers
Blood samples were taken from all participants prior to breakfast in the early morning. Participants had a fasting restriction of 10 h or more prior to having their blood drawn. The serum concentrations of matrix metalloproteinases-3 (MMP-3, ng/mL, CLEIA; LSI Medience Corp., Tokyo, Japan), highly-sensitivity C-reactive protein (hs-CRP, mg/dL, CLEIA; LSI Medience Corp.), interleukin-6 (IL-6, pg/mL, CLEIA; LSI Medience Corp.), and adiponectin (μg/ml, LA; LSI Medience Corp.) were measured for the assessment of inflammation markers.
Radiographs
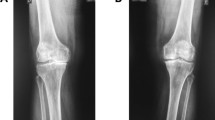
Knee radiographic examinations were performed using CXDI-40EG (Canon Inc. Tokyo, Japan). Experienced radiologic technicians and orthopedic surgeons obtained weight-bearing, full extension, and anterior–posterior radiographs of both knees with foot map positioning on the day of the check-up6,17. The beam was positioned parallel to the floor with no angle and aimed at the joint space, and the sequencing was set as 60 kV, 50 mA and 80 ms for all participants. A diagnosis of knee OA was defined by KL grade ≥ 2 in the most affected knee. All joints were graded by 2 orthopedic surgeons (DC and ES), and any discrepancy was resolved by mutual consultation. Only the participants showing no radiographic evidence of knee OA were included in this analysis.
Synovitis evaluated by magnetic resonance imaging
Synovitis on MRI was assessed in their right knee. Participants were positioned supine with their knees in full extension, and scanned with a rapid extremity coil and mobile magnetic resonance unit (1.5 T; ECHELON RX, Hitachi, Tokyo, Japan) within 1 week following other examinations. The scanning sequences were set including sagittal and coronal plane of T2-weighted fat-suppressed fast-spin echo (repetition time 5,000 ms; echo time 80 ms; field of view 16 cm; 288 × 288 matrix; slice thickness of 3 mm with a gap of 1.0 mm between slices). The image database was transferred to an independent computer workstation using the software program OsiriX (Newton Graphic, Inc., Hokkaido, Japan). According to the Whole-Organ MRI Scoring (WORMS) method39, synovia were semi-quantitatively graded from 0 to 3 in terms of the estimated maximal distention of the synovial cavity: 0 = normal; 1 = \(\le \hspace{0.17em}\)33% of maximum potential distention; 2 = 33–66% of maximum potential distention; 3 = \(\ge \) 66% of maximum potential distention. Furthermore, effusion-synovitis volume (cm3) was quantitatively measured at the suprapatellar fluid equivalent signal on MRI using the software program OsiriX. The ICC (1,1) of effusion synovitis volume was 0.984.
Classification criteria for early knee osteoarthritis
EKOA was defined according to the classification criteria proposed by Luyten et al.5. Classification criteria for EKOA were (A) patient-based questionnaires (KOOS)—2 of the following were required to score “positive” (i.e., ≤ 85%): pain (9 items), symptoms (7 items), activities of daily living (ADL) (short version, 7 items), and knee-related quality of life (QOL) (4 items). (B) Clinical examination—at least one of the following needs to be present: joint line tenderness or crepitus of the knee. (C) Radiographs: KL glade 0/1 at the standing, fixed flexion, and weight bearing positions. Participants were divided into normal knee group (i.e., without EKOA) and EKOA group.
Statistical analysis
Demographic data among normal and EKOA groups are expressed as mean ± standard deviation. The Chi-square test was performed for categorical variables and Mann–Whitney U test was performed for continuous variables to compare demographic data between groups, due to some demographic parameters not being normally distributed according to the Shapiro–Wilk test. The serum concentrations of inflammation biomarkers were compared using the Mann–Whitney U test. The correlations of serum concentrations of each of the inflammation biomarkers were analyzed using the Spearman rank correlation.
The synovial scores and effusion-synovitis volumes were compared using the Mann–Whitney U test; the relationship between serum concentrations of inflammation biomarker and effusion-synovial volume were analyzed using the Spearman rank correlation; to examine associations between knee symptoms and synovitis, Spearman rank correlation was performed between each KOOS score and effusion synovitis volume; to examine the associations between effusion-synovitis volume and inflammation biomarkers, multiple linear regression analyses were performed with effusion-synovitis volume as dependent variables, and serum inflammation biomarkers, age, and BMI as independent variables; finally, to estimate the predictive cutoff level of effusion-synovitis for diagnosing the EKOA, receiver operating characteristic (ROC) analysis was performed. The values of effusion-synovitis volume were used as a single variable in this analysis. A false positive fraction was plotted against the 1 true positive fraction, and the cutoff point was defined as the point of the maximum slope, i.e., the nearest point to true positive. The volume under the curve (AUC) was calculated to evaluate the validity of the ROC analysis. Data input and analysis were performed using SPSS version 25.0J (SPSS Inc., Chicago, IL, USA). A p value < 0.05 was considered statistically significant.
Ethical approval
All participants provided written informed consent, and the study was done in agreement with the 1964 Helsinki declaration and its later amendments or comparable ethical standards and conducted with the approval of the ethics committee of Hirosaki University Graduate School of Medicine.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable.
References
Guermazi, A. et al. Prevalence of abnormalities in knees detected by MRI in adults without knee osteoarthritis: population based observational study (Framingham Osteoarthritis Study). BMJ 345, e5339 (2012).
Yoshimura, N. et al. Prevalence of knee osteoarthritis, lumbar spondylosis, and osteoporosis in Japanese men and women: the research on osteoarthritis/osteoporosis against disability study. J. Bone Miner. Metab. 27, 620–628 (2009).
Hiligsmann, M. et al. Health economics in the field of osteoarthritis: an expert’s consensus paper from the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO). Semin. Arthritis Rheum. 43, 303–313 (2013).
Tubach, F. et al. Evaluation of clinically relevant states in patient reported outcomes in knee and hip osteoarthritis: the patient acceptable symptom state. Ann. Rheum Dis. 64, 34–37 (2005).
Luyten, F. P. et al. Toward classification criteria for early osteoarthritis of the knee. Semin. Arthritis Rheum. 47, 457–463 (2018).
Sasaki, E. et al. Early knee osteoarthritis prevalence is highest among middle-aged adult females with obesity based on new set of diagnostic criteria from a large sample cohort study in the Japanese general population. Knee Surg. Sport Traumatol. Arthrosc. 10, 1–1 (2019).
Golightly, Y. M. et al. Biomarkers of incident radiographic knee osteoarthritis: do they vary by chronic knee symptoms?. Arthritis Rheum. 63, 2276–2283 (2011).
Ishijima, M. et al. Relationships between biomarkers of cartilage, bone, synovial metabolism and knee pain provide insights into the origins of pain in early knee osteoarthritis. Arthritis Res. Ther. 1(13), R22 (2011).
Ayral, X., Pickering, E. H., Woodworth, T. G., Mackillop, N. & Dougados, M. Synovitis: a potential predictive factor of structural progression of medial tibiofemoral knee osteoarthritis–results of a 1 year longitudinal arthroscopic study in 422 patients. Osteoarthr. Cartil. 1(13), 361–367 (2005).
Scanzello, C. R. et al. Local cytokine profiles in knee osteoarthritis: elevated synovial fluid interleukin-15 differentiates early from end-stage disease. Osteoarthr. Cartil. 17, 1040–1048 (2009).
Sellam, J. & Berenbaum, F. The role of synovitis in pathophysiology and clinical symptoms of osteoarthritis. Nat. Rev. Rheumatol. 6, 625 (2010).
Inoue, R. et al. Knee osteoarthritis, knee joint pain and aging in relation to increasing serum hyaluronan level in the Japanese population. Osteoarthr. Cartil. 19, 51–57 (2011).
Sasaki, E. et al. Serum hyaluronic acid concentration predicts the progression of joint space narrowing in normal knees and established knee osteoarthritis—a five-year prospective cohort study. Arthritis Res. 17, 283 (2015).
Baker, K. et al. Relation of synovitis to knee pain using contrast-enhanced MRIs. Ann. Rheum. Dis. 69, 1779–1783 (2010).
Felson, D. T. et al. Synovitis and the risk of knee osteoarthritis: the MOST study. Osteoarthr. Cartil. 24, 458–464 (2016).
Roemer, F. W. et al. Presence of MRI-detected joint effusion and synovitis increases the risk of cartilage loss in knees without osteoarthritis at 30-month follow-up: the MOST study. Ann. Rheum. Dis. 70, 1804–1809 (2011).
Ota, S. et al. Symptomatic bone marrow lesions induced by reduced bone mineral density in middle-aged women: a cross-sectional Japanese population study. Arthritis Res. Ther. 21, 113 (2019).
van Oudenaarde, K. et al. Predictive value of MRI features for development of radiographic osteoarthritis in a cohort of participants with pre-radiographic knee osteoarthritis—the CHECK study. Rheumatology 56, 113–120 (2017).
Ma JD., et al. Serum matrix metalloproteinase-3 as a noninvasive biomarker of histological synovitis for diagnosis of rheumatoid arthritis. Mediators Inflamm. 2014, 2014 (2014).
Deveza, L. A. et al. Is synovitis detected on non-contrast-enhanced magnetic resonance imaging associated with serum biomarkers and clinical signs of effusion? Data from the Osteoarthritis Initiative. Scand. J. Rheumatol. 47, 235–242 (2018).
Fitzgerald, J. B. et al. Mechanical compression of cartilage explants induces multiple time-dependent gene expression patterns and involves intracellular calcium and cyclic AMP. J. Biol. Chem. 279, 19502–19511 (2004).
Pengas, I. et al. MMP-3 in the peripheral serum as a biomarker of knee osteoarthritis, 40 years following open total knee meniscectomy. J. Exp. Orthop. 5, 21 (2018).
Shimura, Y. et al. The factors associated with pain severity in patients with knee osteoarthritis vary according to the radiographic disease severity: a cross-sectional study. Osteoarthr. Cartil. 21, 1179–1184 (2013).
Nathan, C. Epidemic inflammation: pondering obesity. Mol. Med. 14, 485–492 (2008).
Vgontzas, A. N. et al. IL-6 and its circadian secretion in humans. NeuroImmunol. Modul. 12, 131–140 (2005).
Cuzdan, C. N., Ay, S., Evcik, F. D. & Oztuna, D. Adiponectin: is it a biomarker for assessing the disease severity in knee osteoarthritis patients?. Int. J. Rheum. Dis. 20, 1942–1949 (2017).
Sowers, M. R. & Karvonen-Gutierrez, C. A. The evolving role of obesity in knee osteoarthritis. Curr. Opin. Rheumatol. 22, 533 (2010).
Gabay, O., Hall, D. J., Berenbaum, F., Henrotin, Y. & Sanchez, C. Osteoarthritis and obesity: experimental models. Jt. Bone Spine 75, 675–679 (2008).
Honsawek, S. & Chayanupatkul, M. Correlation of plasma and synovial fluid adiponectin with knee osteoarthritis severity. Arch. Med. Res. 4, 593–598 (2010).
Tan, W. et al. High adiponectin and adiponectin receptor 1 expression in synovial fluids and synovial tissues of patients with rheumatoid arthritis. Semin. Arthritis Rheum. 38, 420–427 (2009).
Yusuf, E. et al. Association between leptin, adiponectin and resistin and long-term progression of hand osteoarthritis. Ann. Rheum. Dis. 70, 1282–1284 (2011).
Harkey, M. S. et al. Early pre-radiographic structural pathology precedes the onset of accelerated knee osteoarthritis. BMC Musculoskelet. Disord. 20, 241 (2019).
Hayashi, D. et al. Imaging of synovitis in osteoarthritis: current status and outlook. Semin. Arthritis Rheum. 41, 116–130 (2011).
Magnusson, K., Kumm, J., Turkiewicz, A. & Englund, M. A naturally aging knee, or development of early knee osteoarthritis?. Osteoarthr. Cartil. 26, 1447–1452 (2018).
Chiba, D. et al. Meniscal extrusion seen on ultrasonography affects the development of radiographic knee osteoarthritis: a 3-year prospective cohort study. Clin. Rheumatol. 36, 2557–2564 (2017).
Nakamura, N. et al. Cross-cultural adaptation and validation of the Japanese Knee Injury and Osteoarthritis Outcome Score (KOOS). J. Orthop. Sci. 16, 516 (2011).
Roos, E. M., Roos, H. P., Lohmander, L. S., Ekdahl, C. & Beynnon, B. D. Knee Injury and Osteoarthritis Outcome Score (KOOS)—development of a self-administered outcome measure. J. Orthop. Sports Phys. Ther. 28, 88–96 (1998).
Bekkers, J. E., de Windt, T. S., Raijmakers, N. J., Dhert, W. J. & Saris, D. B. Validation of the Knee Injury and Osteoarthritis Outcome Score (KOOS) for the treatment of focal cartilage lesions. Osteoarthr. Cartil. 17, 1434–1439 (2009).
Peterfy, C. G. et al. Whole-organ magnetic resonance imaging score (WORMS) of the knee in osteoarthritis. Osteoarthr. Cartil. 12, 177–190 (2004).
Acknowledgments
This study was supported in part by JST COI Grant Number JPMJCE1302, a Grant-in-Aid from the Japanese Society for the Promotion of Science (Nos. 21500676, 18K16606, 18K09091), Health Labor Sciences Research Grant, JOA-Subsidized Science Project Research from the Japanese Orthopedic Association, and Grant of Japan Orthopaedics and Traumatology Research Foundation (No. 421).
Author information
Authors and Affiliations
Contributions
All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ishibashi, K., Sasaki, E., Ota, S. et al. Detection of synovitis in early knee osteoarthritis by MRI and serum biomarkers in Japanese general population. Sci Rep 10, 12310 (2020). https://doi.org/10.1038/s41598-020-69328-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-69328-w
This article is cited by
-
Effusion detected by ultrasonography and overweight may predict the risk of knee osteoarthritis in females with early knee osteoarthritis: a retrospective analysis of Iwaki cohort data
BMC Musculoskeletal Disorders (2022)
-
Metabolomics with severity of radiographic knee osteoarthritis and early phase synovitis in middle-aged women from the Iwaki Health Promotion Project: a cross-sectional study
Arthritis Research & Therapy (2022)
-
Bone marrow lesion severity was associated with proximal tibial inclination in early knee osteoarthritis
Knee Surgery, Sports Traumatology, Arthroscopy (2022)
-
Extrusion, meniscal signal change, loss of shape, synovitis and bone marrow oedema are reliable scoring parameters to assess MRI appearance post meniscal transplant
Knee Surgery, Sports Traumatology, Arthroscopy (2022)
-
Reduced serum levels of anti-Mullerian hormone is a putative biomarker of early knee osteoarthritis in middle-aged females at menopausal transition
Scientific Reports (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.