Abstract
Dabigatran etexilate (DABE) is a direct oral anticoagulant (DOAC) and may be combined with ticagrelor, a P2Y12 inhibitor with antiplatelet effects. This combination of antiplatelet drugs and anticoagulants would increases the risk of bleeding in patients. In addition, the potential drug interaction may further increase the risk of bleeding. At present, there is scarce research to clarify the results of the interaction between the two. Therefore, we conducted this study to identify the potential impact of ticagrelor on the pharmacokinetics of DABE using physiologically based pharmacokinetic (PBPK) modeling. The models reasonably predicted the concentration-time profiles of dabigatran (DAB), the transformation form after DABE absorption, and ticagrelor. For pharmacokinetic drug-drug interaction (DDI), exposure to DAB at steady state was increased when co-administrated with ticagrelor. The Cmax and AUC0-t of DAB were raised by approximately 8.7% and 7.1%, respectively. Meanwhile, a stable-state ticagrelor co-administration at 400 mg once-daily increased the Cmax and AUC0-t of DAB by approximately 12.8% and 18.8%, respectively. As conclusions, Ticagrelor slightly increased the exposure of DAB. It is possible to safely use ticagrelor in a double or triple antithrombotic regimen containing DABE, only considering the antithrombotic efficacy, but not need to pay much attention on the pharmacokinetic DDI.
Similar content being viewed by others
Introduction
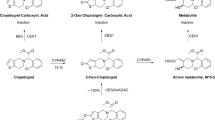
Previously referred to as new oral anticoagulants, the direct oral anticoagulants (DOACs) are a group of rapidly acting and directly clotting factors inhibiting anticoagulants. Current available DOACs include dabigatran etexilate (DABE), rivaroxaban, apixaban and edoxaban1. Among the DOACs, DABE is a particular Factor IIa (thrombin) inhibitor, used for (1) the prevention of stroke and systemic embolism in patients with nonvalvular atrial fibrillation (AF)2, (2) the treatment of acute venous thromboembolism and prevention of venous thromboembolism recurrence3, and (3) the prevention of venous thromboembolism after hip or knee replacement surgery4. DABE is a prodrug, which is converted to the active form dabigatran (DAB) after absorption. Both the prodrug and the metabolite are excreted via the renal route5, and not involved in the cytochrome P450 (CYP450) enzymes, regarding as an advantage over warfarin and many other DOACs. However, DABE, but not DAB, is a substrate for permeability glycoprotein (P-gp)2, which is an important efflux transporter protein, affecting the absorption of DABE6. Therefore, a P-gp inhibitor, such as amiodarone, verapamil, ketoconazole, clarithomycin, may increase the area under the plasma concentration–time curve (AUC) of DAB from about 50% to over 200%7. Besides, the P-gp mediated drug interactions between DABE and antibiotics, proton pump inhibitors, antiepileptic drugs or some new antiretroviral/antiproliferative drugs have also been reported8,9,10,11,12.
Ticagrelor is a novel, reversible, and direct oral adenosine diphosphate receptor P2Y12 inhibitor, and is applied in patients with acute coronary syndromes worldwide13,14,15. In the aspect of pharmacokinetics (PK), ticagrelor is both a P-gp substrate and a P-gp inhibitor that may affect substrates transported by the P-gp16.
The concomitant use of antagonist and antiplatelet agents can reduce the risk of all-cause death, myocardial infarction (MI), stroke and venous thrombosis in patients suffering from acute coronary syndrome (ACS)17,18, and has been extensively applied in patients with both AF and ischemic heart diseases, especially after percutaneous coronary intervention (PCI)19,20. As new antithrombotic drugs, DABE in combination with ticagrelor offers an additional option to substitute warfarin regimen, with the expectation of decreasing the bleeding risk and simultaneously maintaining the clinical effect21.
Thus, researchers have focused on the antithrombotic activation and effect of preventing cardiovascular events of DABE in conjunction with ticagrelor22,23, reaching conclusions that a triple therapy of DABE in combination with ticagrelor plus aspirin is as effective as warfarin triple regimen22, and dual therapy of DABE plus a P2Y12 inhibitor (clopidogrel or ticagrelor) is non-inferior to triple therapy of warfarin plus a P2Y12 inhibitor (clopidogrel or ticagrelor) and aspirin among patients with atrial fibrillation after PCI, and the risk of bleeding is lower23.
However, the potential P-gp induced drug-drug interaction (DDI) between DABE and ticagrelor, which may lead to an elevation of DAB plasma concentration, has not been accurately described. In addition, the indications for this dual therapy are still being explored. Our study aims to use a physiologically based pharmacokinetic (PBPK) model to predict PK profiles and to assess the P-gp mediated DDI of DABE when co-administered with multiple doses of ticagrelor.
Results
Physiologically based pharmacokinetic model and verification
We simulated blood concentration models of 150 mg dabigatran and 200 mg ticagrelor. Blood concentration data at each time point see Supplementary Table 1 and Supplementary Table 2.
The models reasonably predicted the concentration–time profiles of DAB (Cmax 0.11 μg/mL predicted vs. 0.11 μg/mL observed, Tmax 1.76 h predicted vs. 1.97 h observed, AUC0-t 0.69 μg·h/mL predicted vs. 0.70 μg·h/mL observed) and ticagrelor (Cmax 0.80 μg/mL predicted vs. 0.88 μg/mL observed, Tmax 2.28 h predicted vs. 1.92 h observed, AUC0-t 6.56 μg·h/mL predicted vs. 6.52 μg·h/mL observed).
The in vivo data were loaded to verify the predictive accuracy. The simulations and verifications of the plasma concentration–time curves for DAB at a dose of DABE 150 mg and ticagrelor at a dose of 200 mg were shown in Fig. 1a,b, respectively, revealing that the simulated profiles for both DAB and ticagrelor were qualitatively similar to the observed data.
The simulated plasma concentration–time profiles of DAB and ticagrelor corresponded well with the observed data obtained from literatures24,25. In addition, the predicted PK parameters were reasonably consistent (<2-fold error) with the observed values, which indicated that the models were successfully and accurately simulated the pharmacokinetic process of the two medications. The predicted and observed PK parameters with prediction accuracy were summarized in Table 2.
Drug-drug Interaction simulation with DABE and ticagrelor
A dynamic DDI simulation was performed to predict the effect of ticagrelor on the PK of DABE, using multiple doses in the PBPK model for 5 days (10 doses). The plasma concentration–time curves of DAB at baseline and following DDI were shown in Fig. 2, blood concentration data in Supplementary Table 3. The model-predicted ratios of DAB Cmax and AUC0-t with ticagrelor co-administration were 1.087 and 1.071 (Table 3).
In another DDI simulation, DABE were started after ticagrelor reaching stable state. The plasma concentration–time curves of DAB at baseline and following DDI after ticagrelor reaching stable state were drawn in Fig. 3, blood concentration data in Supplementary Table 4. The ratios of Cmax and AUC0-t values were ca. 1.128 and 1.188, respectively (Table 4). The result showed that the predicted ratio of DAB AUC0-t was higher than the ratios observed in the former regimen.
Discussion
DABE is a new oral anticoagulant used to reduce the risk of stroke and systemic embolism in non-valvular atrial fibrillation and to treat and prevent blood clots in veins. In the RE-DEEM trial26, DABE was given in addition to dual antiplatelet treatment (aspirin plus clopidogrel) in patients with a recent myocardial infarction at high risk of new ischaemic cardiovascular events. Ticagrelor is deemed as an alternative to clopidogrel in patients with acute coronary syndromes, especially with clopidogrel resistance27. Currently, concurrent medication with ticagrelor and different anti-coagulation agents has been paid great attention22,23,28,29,30,31, including DABE plus ticagrelor, which was not yet recommended a few years ago32. As mentioned, DABE is a prodrug that has a low oral availability of around 7%, for DABE is an intestinal P-gp substrate6. Whereas, in vitro studies have indicated that ticagrelor is a substrate and inhibitor of P-gp16. The current study was conducted to predict the potential interaction between DABE and ticagrelor, by comparing the pharmacokinetics of DAB alone and in combination with ticagrelor using PBPK modeling.
PBPK models are proved useful to integrate all the parameters which affect the pharmacokinetics, for example, the parameters associated with the properties of the drugs and the physiological parameters specific to the animal species. There are now many softwares available (such as GastroPlus, PKsim, Simcyp) which include the parameters, and equations describing the mechanisms involved in drug disposition, metabolism and excretion33. PBPK modeling and simulation were performed using the Simcyp Simulator in assessing potential DDIs between DABE and a P-gp inhibitor in renal impairment populations in Doki’s study34. GastroPlus was used to performed the PBPK models in the prediction of ticagrelor and its active metabolite in liver cirrhosis populations in Zhang's study35. Both PBPK models in Zhang’s and our study were performed and simulated using GastroPlus™. Although it is slightly different from Zhang’s modeling method, we validated the reliability of the model using data from clinical literature, which prompts the results are credible.
We designed two DDI simulations. One simulation was DABE 150 mg bid Day 1–5 + ticagrelor (180 mg loading dose followed by 90 mg bid) Day 1-5. Both doses were the maximum common doses currently used in clinical. As a result, a slight increase in DAB exposure at steady state was observed when co-administrated with ticagrelor - the Cmax and AUC0-t of DAB were raised by approximately 8.7% and 7.1%, respectively. As the DDI was small, we only validated 150 mg DABE dose, and did not put lower dosage into DDI simulation. In the other simulation, we designed a DABE 150 mg single dose after 5 days continuous use of ticagrelor 400 mg qd, which was higher than the approved 90 mg bid maintenance dose used clinically. This design was based on the previous study of the interaction between ticagrelor and digoxin36. In this dose regimen, ticagrelor increased the Cmax and AUC0-t of DAB by approximately 12.8% and 18.8%, respectively, indicating that there was limited influence of ticagrelor on the PK parameters of DAB, even at a relatively high ticagrelor level.
In a previous study, Weisshaar et al investigated the pharmacodynamic and pharmacokinetic effect of orally administered ticagrelor and aspirin in combination with DABE in healthy male subjects, compared with DABE alone22. As a result, the median DAB plasma concentration was increased 130% at 3 h after concomitant use of DABE, ticagrelor and aspirin, versus single-dose DABE alone. Besides, in the summary of product characteristics of DABE on European Medicines Agency (EMA), drug interaction data for DABE-ticagrelor showed a widely varied AUC and Cmax increase, which were higher than the change in our model prediction. We analyzed the possible reasons were as follows: First, the research population was different. The research population of our study was healthy young people with normal body weight, while the results listed in the EMA Summary of product characteristics may be the result of a combination of various population. Second, from a mechanistic perspective, ticagrelor is a weak P-gp inhibitor, which has a certain effect on drug transport, but the inhibitory effect is relatively weak. Compared with placebo, the AUCτ of digoxin, a substrate of renal and intestinal P-gp, was increased by approximately and 28 % when co-administration with ticagrelor36. Similarly, ticagrelor increased the Cmax and AUC0-inf of cyclosporine, another substrate of intestinal P-gp37, by approximately 5 % and 12 %, respectively38, proving ticagrelor is a weak inhibitor of intestinal P-gp. Therefore, our results were reasonable from the perspective of mechanism analysis.
With respect to efficacy, in patients with atrial fibrillation who had undergone PCI, the risk of bleeding was lower and non-inferior among those who receive dual therapy with DABE and ticagrelor (or clopidogrel), comparing to those who receive triple therapy with warfarin, ticagrelor (or clopidogrel) and aspirin, in RE-DUAL trail23. Regrettably, ticagrelor was not grouped separately, so that we were wondering whether the satisfactory efficacy was corresponding with the DDI between DABE and ticagrelor. Besides, further studies are in need of conducting to explore this dual therapy in the other indications for combination.
From another aspect, since both CYP3A4 and P-gp were involved in the disposition of rivaroxaban, apixaban and edoxaban39,40, clinical consequences may be affected when one of the three xabans was co-administrated with ticagrelor. In GEMINI-ACS-1 trial41, the frequency of TIMI non-CABG relevant bleeding for rivaroxaban plus ticagrelor was significantly increased compared to rivaroxaban plus clopidogrel. This result may partially blame on the DDI between rivaroxaban and ticagrelor. Therefore, it may be more secure to combine ticagrelor with DABE than other DOACs when using the routine dosage, for the pharmacokinetic changes of DABE are limited. Besides, it is possible to be a safety choice to use ticagrelor in a double or triple antithrombotic therapy with DABE.
Although the increases of DAB plasma concentration were considered unlikely to be of clinical significance, close clinical and laboratory monitoring was still highly recommended, referring to the higher rate of total bleeding at 33.3%/27.1% in patients receiving DABE 150 mg/110 mg plus ticagrelor (or clopidogrel)23, compared with the rate at 16.42%/14.62% with DABE 150 mg/110 mg alone42 or 16.1% with ticagrelor alone13, particularly in special populations such as elderly, renal dysfunction and other patients with high risk of bleeding. As DAB is mainly excreted by the kidneys, concomitant renal insufficiency may further increase DAB exposure when given together with P-gp inhibitors. This theoretically supports the findings of the literature, which found impaired renal function, co-medication with antiplatelet drugs or P-gp inhibitors are the risk factors for bleeding with DOACs43.
Overall, the results of this study fill in gaps in the effect of ticagrelor on the PK parameters of DAB, so as to provide support for the clinical application and further research of the combination of these two drugs.
There are several limitations to the current work. First, virtual Caucasian healthy male adults were simulated in the study, lacking for the evaluation on the other population like the elderly, female etc. A human study revealed that DAB exposure in female Caucasian healthy volunteers was about 25% higher than in males. This gender difference is most likely to be attributable to the lower body weight and lower creatinine clearance in females, which in turn results in lower drug clearance than males44. Second, the inhibitory effects of ticagrelor on other DOACs, i.e. rivaroxaban, apixaban, edoxaban, were not assessed, due to the limitation of published in vitro P-gp transporter study specifically designed to capture certain parameters that is required in the process of DDI predicting. Finally, the efficacy and safety of this co-administration therapy should be further verified by more clinical experience and experiments.
Conclusions
DABE and ticagrelor showed a pharmacokinetic interaction. At steady-state, DAB Cmax and AUC0–t were increased by 8.5% and 7.1%, respectively, in the presence of ticagrelor versus DABE alone. Meanwhile, after a 4-day loading of ticagrelor, DAB Cmax and AUC0–t were increased by 12.8% and 18.8%, respectively, versus DABE alone. Since the changes in pharmacokinetic parameters are limited, it is possible to safely use ticagrelor in a double or triple antithrombotic therapy with DABE. Based on these findings, it is recommended that DABE and ticagrelor can be used concomitantly, only considering the antithrombotic efficacy, but not need to pay much attention on the pharmacokinetic DDI.
Methods
The construction of PBPK models and the simulation of drug interaction were performed with GastroPlus v 9.0 (Simulations Plus Inc. Lancaster, CA). The models were constructed and refined to match the observed maximum plasma concentration (Cmax) and area under the plasma concentration–time curve (AUC) values from reported literatures. The Population Estimates for Age-Related (PEAR) human physiology model was used to assume that the typical study subjects were 30-year-old American healthy males weighing 78 kg.
Structure and validation of DAB and ticagrelor PBPK models
The PBPK models were developed via known physicochemical and PK parameters, which were initially required to run simulations with GastroPlus, including: formulation; molecular weight; partition coefficient (logP); the acid dissociation constant (pKa); fraction unbound in plasma (fup); aqueous solubility; blood/plasma concentration ratio (Rbp); effective permeability (Peff). These parameters were obtained from DrugBank (https://www.drugbank.ca/) or acquired from the ADMET Predictor (Simulations Plus Inc.) which is an inbuilt module within GastroPlus. Adjusted plasma fup values were used in the models. The P-gp and kinetic inputs such as maximum reaction velocity (Vmax) and Michaelis–Menten constant (Km) were obtained from the published literature24. All the parameters were listed in Table 1.
After the base PBPK models were constructed, simulations were conducted with an initial dose of DABE 150 mg or ticagrelor 200 mg. The predicted plasma concentration–time curves were validated using data from experimental human studies where volunteers received a single dose of DABE 150 mg or ticagrelor 200 mg. The overall accuracy of the predicted PK parameters was assessed by the fold-error (difference between predicted and observed in vivo values), and the prediction was considered successful if the fold-error was <245.
Quantitative prediction of drug-drug interaction
The DDI between DABE and ticagrelor in virtual healthy volunteers were simulated in the PBPK model, using GastroPlus, to predict the inhibitory effect of ticagrelor on the plasma concentration–time data of DAB.
The in vitro inhibition constant (Ki) of ticagrelor on human P-gp was calculated from Eq1 with published data24,36.
Dynamic simulations of DAB plasma concentration–time profiles taken with and without ticagrelor were run with the DDI Module within GastroPlus. The dose and dose interval of the substrate and inhibitor were set based on the US Food and Drug Administration (FDA) drug instructions.
All virtual subjects received oral DABE 150 mg twice-daily (Day 1–5). Besides, a loading dose of 180 mg and maintenance doses of 90 mg twice-daily ticagrelor was co-administered with DABE on Day 1-5, to determine the inhibitory activity.
The DDI was further evaluated in another PBPK model, in which, ticagrelor at 400 mg once daily36 was delivered on days 1-4, and then, DABE at 150 mg was added to the 5th dose of ticagrelor, when ticagrelor had reached stable state.
A number of PK parameters of DABE were predicted by the DDI models. These parameters included Cmax, time from last dosing to the maximum concentration of the analyte in plasma at steady state (Tmax) and area under the concentration-time curve at steady state over the simulated period (AUC0-t) and till infinite (AUC0-inf). In addition, DAB concentration-time curves for both models were depicted.
References
Gibson, C. M. & Finks, S. W. Edoxaban: How Does the Newest Agent Fit into the DOAC Landscape? The American journal of medicine 130, 900–906, https://doi.org/10.1016/j.amjmed.2017.02.048 (2017).
Blair, H. A. & Keating, G. M. Dabigatran Etexilate: A Review in Nonvalvular Atrial Fibrillation. Drugs 77, 331–344, https://doi.org/10.1007/s40265-017-0699-z (2017).
Greig, S. L. & McKeage, K. Dabigatran etexilate: a review of its use in the treatment of acute venous thromboembolism and prevention of venous thromboembolism recurrence. Drugs 74, 1785–1800, https://doi.org/10.1007/s40265-014-0304-7 (2014).
Burness, C. B. & McKeage, K. Dabigatran etexilate: a review of its use for the prevention of venous thromboembolism after total hip or knee replacement surgery. Drugs 72, 963–986, https://doi.org/10.2165/11209080-000000000-00000 (2012).
Stangier, J. Clinical pharmacokinetics and pharmacodynamics of the oral direct thrombin inhibitor dabigatran etexilate. Clinical pharmacokinetics 47, 285–295, https://doi.org/10.2165/00003088-200847050-00001 (2008).
Chin, P. K., Vella-Brincat, J. W., Barclay, M. L. & Begg, E. J. Perspective on dabigatran etexilate dosing: why not follow standard pharmacological principles? British journal of clinical pharmacology 74, 734–740, https://doi.org/10.1111/j.1365-2125.2012.04266.x (2012).
Delavenne, X. et al. A semi-mechanistic absorption model to evaluate drug-drug interaction with dabigatran: application with clarithromycin. British journal of clinical pharmacology 76, 107–113, https://doi.org/10.1111/bcp.12055 (2013).
Lippi, G., Favaloro, E. J. & Mattiuzzi, C. Combined administration of antibiotics and direct oral anticoagulants: a renewed indication for laboratory monitoring? Seminars in thrombosis and hemostasis 40, 756–765, https://doi.org/10.1055/s-0034-1381233 (2014).
Ollier, E. et al. In vitro and in vivo evaluation of drug-drug interaction between dabigatran and proton pump inhibitors. Fundamental & clinical pharmacology 29, 604–614, https://doi.org/10.1111/fcp.12154 (2015).
Stollberger, C. & Finsterer, J. Interactions between non-vitamin K oral anticoagulants and antiepileptic drugs. Epilepsy research 126, 98–101, https://doi.org/10.1016/j.eplepsyres.2016.06.003 (2016).
Kumar, P. et al. Differential Influence of the Antiretroviral Pharmacokinetic Enhancers Ritonavir and Cobicistat on Intestinal P-Glycoprotein Transport and the Pharmacokinetic/Pharmacodynamic Disposition of Dabigatran. Antimicrobial agents and chemotherapy 61, https://doi.org/10.1128/AAC.01201-17 (2017).
Hsyu, P. H., Pignataro, D. S. & Matschke, K. Effect of bosutinib on the absorption of dabigatran etexilate mesylate, a P-glycoprotein substrate, in healthy subjects. European journal of clinical pharmacology 73, 57–63, https://doi.org/10.1007/s00228-016-2115-0 (2017).
Wallentin, L. et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. The New England journal of medicine 361, 1045–1057, https://doi.org/10.1056/NEJMoa0904327 (2009).
James, S. et al. Ticagrelor versus clopidogrel in acute coronary syndromes in relation to renal function: results from the Platelet Inhibition and Patient Outcomes (PLATO) trial. Circulation 122, 1056–1067, https://doi.org/10.1161/CIRCULATIONAHA.109.933796 (2010).
Dhillon, S. Ticagrelor: a review of its use in adults with acute coronary syndromes. American journal of cardiovascular drugs : drugs, devices, and other interventions 15, 51–68, https://doi.org/10.1007/s40256-015-0108-5 (2015).
Teng, R. Ticagrelor: Pharmacokinetic, Pharmacodynamic and Pharmacogenetic Profile: An Update. Clinical pharmacokinetics 54, 1125–1138, https://doi.org/10.1007/s40262-015-0290-2 (2015).
Andreotti, F., Testa, L., Biondi-Zoccai, G. G. & Crea, F. Aspirin plus warfarin compared to aspirin alone after acute coronary syndromes: an updated and comprehensive meta-analysis of 25,307 patients. European heart journal 27, 519–526, https://doi.org/10.1093/eurheartj/ehi485 (2006).
Rothberg, M. B., Celestin, C., Fiore, L. D., Lawler, E. & Cook, J. R. Warfarin plus aspirin after myocardial infarction or the acute coronary syndrome: meta-analysis with estimates of risk and benefit. Annals of internal medicine 143, 241–250 (2005).
Cairns, J. A. & McMurtry, M. S. Oral antithrombotic therapy in atrial fibrillation associated with acute or chronic coronary artery disease. The Canadian journal of cardiology 29, S60–70, https://doi.org/10.1016/j.cjca.2013.04.006 (2013).
Dezsi, C. A., Dezsi, B. B. & Dezsi, D. A. Antithrombotic treatment in anticoagulated atrial fibrillation patients undergoing percutaneous coronary intervention. European journal of internal medicine 40, 1–7, https://doi.org/10.1016/j.ejim.2017.01.001 (2017).
Cannon, C. P. et al. Design and Rationale of the RE-DUAL PCI Trial: A Prospective, Randomized, Phase 3b Study Comparing the Safety and Efficacy of Dual Antithrombotic Therapy With Dabigatran Etexilate Versus Warfarin Triple Therapy in Patients With Nonvalvular Atrial Fibrillation Who Have Undergone Percutaneous Coronary Intervention With Stenting. Clinical cardiology 39, 555–564, https://doi.org/10.1002/clc.22572 (2016).
Weisshaar, S. et al. Antithrombotic triple therapy and coagulation activation at the site of thrombus formation: a randomized trial in healthy subjects. Journal of thrombosis and haemostasis : JTH 12, 1850–1860, https://doi.org/10.1111/jth.12726 (2014).
Cannon, C. P. et al. Dual Antithrombotic Therapy with Dabigatran after PCI in Atrial Fibrillation. The New England journal of medicine 377, 1513–1524, https://doi.org/10.1056/NEJMoa1708454 (2017).
Zhao, Y. & Hu, Z. Y. Physiologically based pharmacokinetic modelling and in vivo [I]/K(i) accurately predict P-glycoprotein-mediated drug-drug interactions with dabigatran etexilate. British journal of pharmacology 171, 1043–1053, https://doi.org/10.1111/bph.12533 (2014).
Teng, R., Oliver, S., Hayes, M. A. & Butler, K. Absorption, distribution, metabolism, and excretion of ticagrelor in healthy subjects. Drug metabolism and disposition: the biological fate of chemicals 38, 1514–1521, https://doi.org/10.1124/dmd.110.032250 (2010).
Oldgren, J. et al. Dabigatran vs. placebo in patients with acute coronary syndromes on dual antiplatelet therapy: a randomized, double-blind, phase II trial. European heart journal 32, 2781–2789, https://doi.org/10.1093/eurheartj/ehr113 (2011).
Samos, M. et al. Ticagrelor: a safe and effective approach for overcoming clopidogrel resistance in patients with stent thrombosis? Blood coagulation & fibrinolysis : an international journal in haemostasis and thrombosis 27, 117–120, https://doi.org/10.1097/MBC.0000000000000406 (2016).
Braun, O. O. et al. Concomitant use of warfarin and ticagrelor as an alternative to triple antithrombotic therapy after an acute coronary syndrome. Thrombosis research 135, 26–30, https://doi.org/10.1016/j.thromres.2014.10.016 (2015).
Lu, W. et al. Rationale and design of MANJUSRI trial: a randomized, open-label, active-controlled multicenter study to evaluate the safety of combined therapy with ticagrelor and warfarin in AF subjects after PCI-eS. Contemporary clinical trials 40, 166–171, https://doi.org/10.1016/j.cct.2014.12.002 (2015).
Gao, F. et al. Rationale and design of the RT-AF study: Combination of rivaroxaban and ticagrelor in patients with atrial fibrillation and coronary artery disease undergoing percutaneous coronary intervention. Contemporary clinical trials 43, 129–132, https://doi.org/10.1016/j.cct.2015.05.012 (2015).
Povsic, T. J. et al. A randomized trial to compare the safety of rivaroxaban vs aspirin in addition to either clopidogrel or ticagrelor in acute coronary syndrome: The design of the GEMINI-ACS-1 phase II study. American heart journal 174, 120–128, https://doi.org/10.1016/j.ahj.2016.01.004 (2016).
Di Minno, G., Russolillo, A., Gambacorta, C., Di Minno, A. & Prisco, D. Improving the use of direct oral anticoagulants in atrial fibrillation. European journal of internal medicine 24, 288–294, https://doi.org/10.1016/j.ejim.2013.01.021 (2013).
Gobeau, N., Stringer, R., De Buck, S., Tuntland, T. & Faller, B. Evaluation of the GastroPlusTM Advanced Compartmental and Transit (ACAT) Model in Early Discovery. Pharmaceutical research 33, 2126–2139, https://doi.org/10.1007/s11095-016-1951-z (2016).
Doki, K., Neuhoff, S., Rostami-Hodjegan, A. & Homma, M. Assessing Potential Drug-Drug Interactions Between Dabigatran Etexilate and a P-Glycoprotein Inhibitor in Renal Impairment Populations Using Physiologically Based Pharmacokinetic Modeling. CPT: pharmacometrics & systems pharmacology 8, 118–126, https://doi.org/10.1002/psp4.12382 (2019).
Zhang, M. et al. Prediction of Ticagrelor and its Active Metabolite in Liver Cirrhosis Populations Using a Physiologically Based Pharmacokinetic Model Involving Pharmacodynamics. Journal of pharmaceutical sciences 108, 2781–2790, https://doi.org/10.1016/j.xphs.2019.03.028 (2019).
Teng, R. & Butler, K. A pharmacokinetic interaction study of ticagrelor and digoxin in healthy volunteers. European journal of clinical pharmacology 69, 1801–1808, https://doi.org/10.1007/s00228-013-1543-3 (2013).
Lown, K. S. et al. Role of intestinal P-glycoprotein (mdr1) in interpatient variation in the oral bioavailability of cyclosporine. Clinical pharmacology and therapeutics 62, 248–260, https://doi.org/10.1016/S0009-9236(97)90027-8 (1997).
Teng, R., Kujacic, M. & Hsia, J. Pharmacokinetic interaction study of ticagrelor and cyclosporine in healthy volunteers. Clinical drug investigation 34, 529–536, https://doi.org/10.1007/s40261-014-0205-2 (2014).
Stollberger, C. Drug interactions with new oral anticoagulants in elderly patients. Expert review of clinical pharmacology 10, 1191–1202, https://doi.org/10.1080/17512433.2017.1370369 (2017).
Hodin, S. et al. In Vitro Comparison of the Role of P-Glycoprotein and Breast Cancer Resistance Protein on Direct Oral Anticoagulants Disposition. European journal of drug metabolism and pharmacokinetics 43, 183–191, https://doi.org/10.1007/s13318-017-0434-x (2018).
Ohman, E. M. et al. Clinically significant bleeding with low-dose rivaroxaban versus aspirin, in addition to P2Y12 inhibition, in acute coronary syndromes (GEMINI-ACS-1): a double-blind, multicentre, randomised trial. Lancet 389, 1799–1808, https://doi.org/10.1016/S0140-6736(17)30751-1 (2017).
Connolly, S. J. et al. Dabigatran versus warfarin in patients with atrial fibrillation. The New England journal of medicine 361, 1139–1151, https://doi.org/10.1056/NEJMoa0905561 (2009).
Pfeilschifter, W., Luger, S., Brunkhorst, R., Lindhoff-Last, E. & Foerch, C. The gap between trial data and clinical practice–an analysis of case reports on bleeding complications occurring under dabigatran and rivaroxaban anticoagulation. Cerebrovascular diseases 36, 115–119, https://doi.org/10.1159/000352062 (2013).
Hartter, S., Yamamura, N., Stangier, J., Reilly, P. A. & Clemens, A. Pharmacokinetics and pharmacodynamics in Japanese and Caucasian subjects after oral administration of dabigatran etexilate. Thrombosis and haemostasis 107, 260–269, https://doi.org/10.1160/TH11-08-0551 (2012).
Jones, H. M., Parrott, N., Jorga, K. & Lave, T. A novel strategy for physiologically based predictions of human pharmacokinetics. Clinical pharmacokinetics 45, 511–542, https://doi.org/10.2165/00003088-200645050-00006 (2006).
Author information
Authors and Affiliations
Contributions
Nan Wang. The main contributor to the research, accomplishing research design, article writing, charting and graphing. Lu Chen. Editing the article, providing support on PBPK modeling and interpretation of some literatures. Na Li. Structuring and validating PBPK models, predicting drug-drug interaction. Gaoqi Xu. Participating in research design. Fang Qi. Help with article writing. Liqin Zhu. Responsible for ideas of the research, providing research funding and platforms, supervising and guiding the entire process of the experiment and the publication of the article, responsible for the entire study. Wensheng Liu. Responsible for ideas of the research, supervising the entire process of the experiment and the publication of the article, responsible for the entire study.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wang, N., Chen, L., Li, N. et al. Predicted effect of ticagrelor on the pharmacokinetics of dabigatran etexilate using physiologically based pharmacokinetic modeling. Sci Rep 10, 9717 (2020). https://doi.org/10.1038/s41598-020-66557-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-66557-x
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.