Abstract
Invasive meningococcal disease (IMD) due to serogroup Y Neisseria meningitidis emerged in Europe during the 2000s. Draft genomes of serogroup Y isolates in Sweden revealed that although the population structure of these isolates was similar to other serogroup Y isolates internationally, a distinct strain (YI) and more specifically a sublineage (1) of this strain was responsible for the increase of serogroup Y IMD in Sweden. We performed single molecule real-time (SMRT) sequencing on eight serogroup Y isolates from different sublineages to unravel the genetic and epigenetic factors delineating them, in order to understand the serogroup Y emergence. Extensive comparisons between the serogroup Y sublineages of all coding sequences, complex genomic regions, intergenic regions, and methylation motifs revealed small point mutations in genes mainly encoding hypothetical and metabolic proteins, and non-synonymous variants in genes involved in adhesion, iron acquisition, and endotoxin production. The methylation motif CACNNNNNTAC was only found in isolates of sublineage 2. Only seven genes were putatively differentially expressed, and another two genes encoding hypothetical proteins were only present in sublineage 2. These data suggest that the serogroup Y IMD increase in Sweden was most probably due to small changes in genes important for colonization and transmission.
Similar content being viewed by others
Introduction
The Gram-negative encapsulated bacterium Neisseria meningitidis is a common commensal found exclusively in the human nasopharyngeal mucosa. It is the leading cause of epidemic meningitis and sepsis1. Invasive meningococcal disease (IMD) is mainly caused by meningococci expressing specific capsular groups (i.e. serogroups) and belonging to particular hyperinvasive lineages2,3, which have a changing global distribution over time. An increase in IMD due to serogroup Y occurred in the United States in the 1990s, and from the end of the 2000s this was also the case in Europe4,5. This serogroup was the most prevalent cause of IMD in Sweden between 2010 and 2015, representing 53% of all IMD in 20156. Characterization by multilocus sequence typing (MLST) and sequencing of the antigens FetA, FHbp, PenA, PorA, and PorB, revealed that three serogroup Y strain types were responsible for IMD in Sweden, in particular those with the genotype Y: P1.5-2, 10-1: F4-1: ST-23 clonal complex 23 (cc23) along with PorB allele 3–36, FHbp allele 25, and PenA allele 22, referred to as strain YI7. Illumina whole genome sequencing (WGS) of 185 serogroup Y genomes from Sweden showed that the majority of those causing IMD clustered with strain YI, belonging to the WGS lineage 23.18. Analysis of genes core to the meningococcus (cgMLST) revealed that this cluster, although antigenically identical, contained an average of 100 core loci with allelic differences, delineating it into sublineages 1 and 28. Analysis on a limited selection of 177 loci hypothesized to play a role in meningococcal virulence showed that 10 of these loci differed between the two sublineages. Because 213 core loci were incompletely assembled in at least one isolate in the draft genomes, the genetic analysis was only based on 1,241 completely assembled genes. However, the study showed that the temporal distribution of the two sublineages in Sweden coincided with an increase in serogroup Y IMD due to one of the sublineages, appearing in Sweden after 2006.
Single molecule real-time (SMRT) PacBio sequencing also includes data on DNA methylation in the form of N6-methyladenine (m6A), N4-methylcytosine (m4C) and C5-methylcytosine (m5C), only poorly at best. Enzymes that methylate (MTases) are part of the restriction-modification (RM) system, which acts as a defence mechanism against the invasion of foreign DNA in prokaryotes9. The restriction endonucleases (REases) cleave double stranded DNA with specific patterns, and methyl groups are added by MTases to specific motifs in order to prevent degradation by the REases. There are four types of RM systems, three of which have been found in Neisseria10,11. Type I systems consist of three subunit proteins: R (restriction), M (modification), and S (specificity). Type II systems consist of individual RM enzymes that bind to and cleave at the same position, or close to that sequence. Type III systems are composed of two protein subunits, Mod and Res that recognize non-palindromic motifs12. Although DNA methylation is best known for its role in prokaryotic defence, and is important for genetic flux, it has also been shown to have roles in gene expression13,14, DNA replication initiation15,16, virulence17 and are often phase variable11.
The aim of this study was to robustly identify all genetic alterations and differences in methylation between sublineage 1 (responsible for the serogroup Y increase in Sweden) and sublineage 2 using high-quality PacBio-derived finished genomes, thereby enhancing our understanding of how invasive meningococci may emerge over time.
Materials and Methods
Isolate collection and genome sequencing
Eight isolates belonging to YI sublineages 1 and 2 were chosen based on the phylogenetic clustering generated using Illumina-derived WGS of serogroup Y isolates from Sweden between 1995 and 20128 (Fig. 1). All isolates had the following designation: Y: P1.5-2,10-1,36-2: F4-1: ST-23 (cc23), and had PorB allele 3–36, FHbp allele 25, and PenA allele 22, except for isolate 98–182: FHbp allele 276, isolate 11–14: PorB allele 3–117, and isolate 12–176: PorA VR2 10–85. Sublineage 1 (n = 59) and sublineage 2 (n = 32) HiSeq genomes8 were used to confirm differences in presence/absence and premature stop codons of genes delineating the two sublineages. PubMLST Neisseria database identification numbers are shown in Supplementary Table 1.
Neighbour-net network based on the comparison of 1,605 Neisseria meningitidis core genome loci. Panel a shows strain YI from Sweden subclustered into sublineage 1 and sublineage 28. These two sublineages belong to sublineage 23.18, as shown in panel b of all clonal complex 23 genomes in the pubMLST Neisseria database (n = 1,576; accessed 20/01/10). Isolates from the present study are marked in blue. Isolate IDs for isolates belonging to sublineages 1 (n = 59) and 2 (n = 32) are provided in Supplementary Table 1. The scale bars denote the number of loci with allelic differences. This figure was generated using SplitsTree v 4.15.1 (http://www.splitstree.org/) and subsequently exported to Inkscape v0.92 (https://inkscape.org/) for additional edits.
Isolates were cultured on chocolate agar at 37 °C in a 5% CO2 enriched atmosphere overnight and archived at −70 °C. Genomic DNA was extracted using the Wizard Genomic DNA purification kit (Promega) according to the manufacturer’s instructions. Libraries were prepared using the Pacific Biosciences 10 kb library preparation protocol. Size selection of the final libraries was performed using BluePippin (Sage Science) or AMPure PB beads (PacBio). The libraries were sequenced on a Pacific Biosciences RS II sequencer using P4-C2 or P6-C4 chemistry with 1–3 SMRT cells each. One of the genomes (12–221) was sequenced with >1000x coverage in order to detect m5C motifs.
Genome assembly and annotation
Reads were assembled de novo using HGAP v3 (Pacific Biosciences, SMRT Analysis Software v2.3.0, smrtanalysis_2.3.0.140936.p5.167094). Sequencing and assembly metrics are shown in Supplementary Table 2. Quiver18 was used to correct sequencing errors in the assemblies by mapping the raw reads back to the PacBio assembly. Mimimus2 software from the Amos package19 was used to circularize the genomes. Illumina HiSeq 2000 100 bp reads from a previous study8 (ERR405856, ERR405873, ERR405911, ERR405968, ERR405969, ERR406012, ERR406017, and ERR406024) were filtered at Q30 and mapped onto the genomes obtained from the Pacific Biosciences RS II sequencer using CLC Genomics Workbench v8.0.1 (Qiagen) to detect any assembly and sequencing errors. To strengthen any corrections made, PacBio subreads were mapped onto the PacBio assemblies. All errors with >50% mapping frequency of the HiSeq reads and 9–28% of the mapped PacBio reads in agreement with the HiSeq reads were manually corrected. Thirty errors were found using these criteria; twenty-nine of the 30 corrections were single nucleotide insertions in homopolymeric tracts (5–9 nucleotides long) and one was in a repetitive region (Supplementary Table 3). The chromosome was adjusted so that the first base was upstream of the dnaA gene.
PacBio assemblies were annotated in two ways: (i) using the rapid bacterial annotation software Prokka20 and (ii) using the PubMLST Neisseria database (http://pubMLST.org/neisseria/) where genome data have been deposited. Genes were labelled using the locus tag prefix “NEIS”. NEIS identifiers were linked to an alias table, enabling cross-linking with Prokka annotations. Alleles were automatically assigned to and annotated with the appropriate allele number within the PubMLST Neisseria database when these were a ≥98% match to previously defined loci in the database. New alleles ≤98% identical were manually curated and assigned. Allele frequency was determined using the allele designations field filter when browsing all genomes deposited in the PubMLST Neisseria database. All eight genomes have been deposited in NCBI under BioProject number PRJNA386981; the PubMLST Neisseria database identification numbers are shown in Table 1.
Genome analyses
Annotated genomes were compared using Artemis21, ACT22, Mauve23, and BRIG24. To identify variations in coding sequences (CDS) among sublineages, the Genome Comparator Tool, available in the PubMLST Neisseria database, was employed using a sublineage as a reference as described previously25. Briefly, the Genome Comparator Tool compares genomes using any number of predefined loci in the database or a reference genome. For each locus, the allele sequences, designated by allele numbers, are compared and used to generate a distance matrix based on the number of variable loci across a genome. Distance matrices can subsequently be visualized using the neighbour-net algorithm26. The Genome Comparator Tool output includes a list of loci that are: (i) identical; (ii) variable; (iii) missing/absent; and (iv) incomplete (partially present in the genome due to incomplete assembly).
Core and pan genome
A total of 1,605 loci have been identified as core to meningococci, as they are present in ≥95% N. meningitidis isolates (cgMLST, v1.0)27. Neighbour-net diagrams were constructed using distance matrices generated by the PubMLST Genome Comparator Tool27 and visualized using SplitsTree428. Loci core to the whole genome based lineage 2327 were identified through the combined use of Prokka and Genome Comparator. Initially, all loci defined using Prokka were BLAST searched against all of the loci and associated alleles found in the PubMLST Neisseria database. This allowed identification of novel loci not yet defined in the PubMLST Neisseria database. All novel loci were subsequently verified using Artemis to ensure the correct start and stop codons had been annotated. These were then compared using Genome Comparator in all MLST cc23 isolates deposited in the PubMLST Neisseria database (978 cc23 isolates at the time of the study). A whole genome based lineage 23 core and pan genome scheme was then generated.
Methylation motifs
The RS_Modification_and_Motif_Analysis pipeline analysis platform SMRT Portal (Pacific Biosciences, SMRT Analysis Software v2.3.0, smrtanalysis_2.3.0.140936.p5.167094) was used for genome-wide analysis of modified motifs with quality value (QV) limit > 60. DNA methyltransferase genes associated with the different methyltransferase recognition motifs identified were searched using SEQWARE routines as described previously29, and deposited in the Restriction Enzyme Database REBASE30. Motif summary files have been deposited in the NCBI submission PRJNA386981 (see Supplementary Table 4 for a summary).
Enzymatic cleavage with MspJI and FspEI
MspJI and its homologue FspEI (New England Biolabs) was used to enzymatically verify the activity of predicted m5C methylations. These enzymes cleave at a fixed distance from the top-strand m5C (12 or 16 bases), leaving a 4-base 5′ overhang, and the resulting fragments were sequenced to determine the recognition site31. MspJI and FspEI cleavage was performed as previously described31. In short, 0.5 µg genomic DNA was digested with MspJI and FspEI (New England Biolabs) according to the manufacturer's instructions, and then separated on a 20% polyacrylamide gel electrophoresis (PAGE) in 0.5x TBE buffer and stained with SYBR GOLD. The 30–35 bp gel fragments were excised and purified using the NEB Monarch Nucleic Acid Purification Kit (New England Biolabs). Libraries were prepared for sequencing using the NEBNext Fast DNA Library Prep Set (New England Biolabs) according to the manufacturer’s instructions, except excluding the size selection and running only 12 cycles of PCR. The bioinformatics analysis was performed as previously described31.
Results
General genome features and comparative genomics
Eight N. meningitidis serogroup Y genomes were sequenced using PacBio RS II and each assembled into a single contiguous sequence. The median genome length was 2,167,932 nucleotides and the median number of predicted CDS was 2,149 (Table 1). The genomes had similar structure and gene synteny (Supplementary Figure 1), with dissimilarities between sublineages found mainly in transposases, hypothetical proteins and non-coding intergenic regions (IGRs) located between genes involved in metabolism, methyltransferases, and prophages (Fig. 2).
BLAST ring comparing N. meningitidis sublineages 1 (in blue; n = 5) and 2 (in purple; n = 2), with isolate 11–7 (sublineage 2) used as reference. The innermost circle shows the GC skew. The protein function of coding regions with low identity between the sublineages are indicated on the outermost circle. This figure was generated using BRIG v 0.95 (http://brig.sourceforge.net/) and subsequently exported to Inkscape v0.92 (https://inkscape.org/) for additional edits.
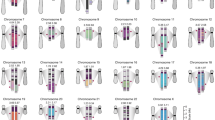
Gene-by-gene comparisons of all CDS identified allelic differences in 97 loci between isolates in the two sublineages (Fig. 3 and Supplementary Table 5). Of these loci, 73 had non-synonymous differences, including genes implicated in: adhesion (opcA); lipooligosaccharide (LOS) production (galE, galE2, lgtA, lgtB, lot, and yhbG); type IV pili production (pilI, pilQ, and pilX); and iron acquisition (NEIS0669). CRISPR-associated endonuclease Cas1 also differed in one amino acid residue (188 V→A) between sublineages 1 and 2 in all but two isolates among the collection of 91 draft genomes8.
Functions of loci that contained allelic differences resulting in synonymous or non-synonymous changes distinguishing the two sublineages. AA = amino acid change. Classification is according to the scheme in the PubMLST Neisseria database27. This figure was generated using Microsoft Excel 2016.
Among all CDS in isolates belonging to sublineages 1 and 2, only seven CDS with premature stop codons distinguished the sublineages (Table 2), encoding a hypothetical protein, DNA repair protein, metabolic protein, a RM protein, and inner and outer membrane proteins. Two of these were due to phase variability: NEIS2198 (opcA) and NEIS2535. OpcA, which is involved in adhesion to epithelial and endothelial cells important in the infection process32,33, has been shown to be phase variable and regulated by homopolymeric cytidine residues in the promoter sequence; ≤ 10 or ≥ 15 cytidine residues suppress expression, 12–13 cytidine residues lead to efficient expression, and 11 or 14 lead to intermediate expression34. Sublineage 2 isolates had ≤ 8 contiguous C residues and sublineage 1 isolates had ≥ 14, putatively leading to opcA being phase variable off in to both sublineages. Moreover, sublineage 1 had an insertion transposase inserted in NEIS2535 encoding the Type I restriction system specificity protein determining the specificity of the restriction and the modification reactions.
Only two genes were absent when comparing both sublineages. Genes NEIS0627 and NEIS2931 (both encoding hypothetical proteins) were absent in all sublineage 1 isolates but present in all sublineage 2 isolates (Table 2). The frequency of these genes in the larger collection of HiSeq genomes (Supplementary Table 1) is shown in Table 2. NEIS2931 was found to share sequence identity with a cornifin small proline rich (SPR) family protein that is strongly induced during differentiation of human epidermal keratinocytes35. NEIS0627 was highly prevalent among the 20,357 genomes deposited in the PubMLST Neisseria database (accessed 20/09/2019): only 985 of the 20,357 genomes lacked this locus. These 985 isolates were primarily cc23 isolates (167/985) and non-meningococcal isolates N. lactamica and N. gonorrhoeae (484/985). NEIS2931 was prevalent in cc23 isolates. Although a difference was observed in the number of genes absent or probably not expressed due to stop codons between sublineages 1 and 2 (7/1988 and 2/1975 respectively), this difference was not statistically significant (p=0.01).
A lineage 2327 pan genome was defined containing 1,757 core loci and 24 accessory loci. Accessory loci included genes encoding seven hypothetical proteins, a MafB toxin, and a Type I RM system protein (Supplementary Table 6). Of the 2,452 loci defined in the PubMLST Neisseria database, 466 were absent in all eight genomes in the present study, some of which putatively associated with pathogenic interactions (Supplementary Table 7).
Horizontal gene transfer
There were nine regions in which allelic differences were adjacent (2–5 genes in succession) and therefore putatively a consequence of horizontal gene transfer (HGT). These included genes implicated in capsule synthesis, metabolism, iron acquisition, antibiotic resistance, and LOS (Supplementary Table 5). Alleles from sublineage 1 in the putative HGT region including NEIS0625, NEIS0626, and NEIS0628 were unique to cc23 genomes, the majority of which were from Sweden (> 89%) (accessed 14/12/2017). Another putative HGT event included loci NEIS0667, NEIS0668, NEIS0669, NEIS0671, and NEIS0672, resulting in sublineage 2 isolates containing alleles more commonly found in Neisseria gonorrhoeae (> 96% for NEIS0667, NEIS0669, and NEIS0671). Alleles from sublineage 2 in the putative HGT event involving NEIS1901 (lgtB), NEIS1902 (lgtA), NEIS1903, and NEIS1904 were found in 80, 84, 70, and 80 isolates respectively; 55–64% of these were from Swedish cc23 genomes, and the remainder belonged to cc41/44. Isolate 12–330 (sublineage 1) had the shorter tbpB isotype characteristic of ST-11 meningococci36. Another three isolates belonging to sublineage 1 from the larger 185-isolate collection from our previous study8 had the same shorter tbpB isotype. The other sublineage 1 and 2 isolates had isotype II found among meningococci belonging to the hyper-invasive clonal complexes including ST-8, ST-18, ST-32, and ST-41/44 as well as N. gonorrhoeae isolates.
Methylome analysis
Eleven putative RM systems were identified (putative RM systems for isolate 12–221 are shown in Fig. 4). Initially, the genome-wide analysis of the methylomes identified two m6A and one m5C modified motif: GATC, CACNNNNNTAC, and GGNNCC (Table 3). CACNNNNNTAC was found exclusively in isolates belonging to sublineage 2; in sublineage 1, the specificity subunit of the candidate Type I RM system (NEIS2535) was disrupted by a transposase insertion. The motif CACNNNNNTAC was only found in one other meningococcal isolate in REBASE, belonging to cc23, suggesting that this may be a cc23 specific motif. Isolate 12–221 was sequenced with higher coverage (1266x) in order to detect m5C motifs that were potentially missed with lower sequencing depth due to the lower effect on delaying the polymerase during PacBio sequencing. Three additional motifs were discovered using higher coverage (Supplementary Table 4). Two of them (CGGCACGCNNNA and CGNGGTAACV) had low signal but were probable m5C motifs; however, no known enzymes could be assigned because the correct motifs could not be determined. The third motif found, a m6A: ACACC, has previously been described as methylated by the MTase encoded by the phase variable gene modA1237. modA12 was only putatively expressed by isolates 11–7, the remaining isolates with exception for 12–221 were switched off through translational phase variation by slipped strand mispairing due to a variable number of 5′-AGCC-3′ in the coding region of the gene38. Isolate 12–221, belonging to sublineage 1, had one less adenine residue at 1,505 bp resulting in a premature stop codon. This modA allele could not be found in any other isolates in the pubMLST Neisseria database indicating that this could be the result of a sequencing error. Furthermore, although modA12 in isolate 11–7 had ON status, the ACACC motif could not be detected in this isolate.
A circular view of the predicted restriction modification (RM) systems in the genome of N. meningitidis sublineage 1. ORF = open reading frame. This figure was generated in REBASE (http://rebase.neb.com/rebase/rebase.html) and subsequently exported to Inkscape v0.92 (https://inkscape.org/) for additional edits.
Five m5C genes were bioinformatically predicted from the sequences, but only three motifs (GCRYGC, GGNNCC, and CCAGR) were confirmed as methylated using MspJI and FspEI cleavage (Table 3). The apparent CCAGR motif may be the result of two MTases, one recognizing CCWGG and the other CCAGA.
Discussion
The increase in incidence of IMD caused by serogroup Y meningococci began in the 1990s and late 2000s in North America and Europe, respectively. In the United States, the increase in cc23 serogroup Y IMD was accompanied by an antigenic shift of the three outer membrane proteins: PorA, FetA, and PorB. The most prevalent serogroup Y strain in Sweden possessed the same antigenic profile; however, Illumina WGS analysis resolved this strain further into two distinct sublineages8. One of these sublineages was associated with patients with IMD after 2006, resulting in a marked increase in IMD in Sweden. Variations among the Illumina WGS could not be ruled out as being the result of incomplete genomes, and it was therefore not possible to distinguish robustly differences between these two sublineages, particularly in more complex regions such as IGRs, which are abundant in meningococci, or in the presence or absence of genes. In the present study, PacBio sequencing provides a single contiguous sequence for each genome, which were comprehensively annotated and enabled lineage 23 core and pan genomes to be determined.
Comparison of complete PacBio-derived genome sequences from sublineages 1 and 2 identified sequence differences, mostly limited to IGRs, transposases, and genes encoding hypothetical proteins (Fig. 2). Non-synonymous allelic differences were more abundant among genes encoding hypothetical and metabolic proteins but were also found among genes potentially associated with pathogenicity, such as those implicated in adhesion, LOS production, type IV pili production, and iron acquisition39. As with genes involved in pathogenicity, metabolic genes undergo high rates of HGT in meningococci40,41 and this is the most likely reason that such were dominant among the genes distinguishing the two sublineages. Nevertheless, functional genomic studies on meningococci during colonization and invasion have shown the importance of metabolic adaptation in the interaction with host cells42, which suggests that the differences in metabolic genes identified here may also have contributed to the difference in the emergence of sublineage 1. In contrast to the draft genomes generated by Illumina sequencing previously8, the complete PacBio genomes enabled comparison of presence and absence of genes. Only two CDS were absent in sublineage 1 but present in sublineage 2, and only seven were putatively differentially expressed due to premature stop codons, two of them through phase variation. Sequences obtained following WGS will be consensus sequences resulting from a population of colonies rather than a single colony. As a result, it is not possible to reliably infer expression and phase on or off status. Nevertheless, a pattern of phase variation was observed between sublineages 1 and 2. The absence of the hypothetical protein NEIS0627 in sublineage 1 was likely the result of HGT, as this locus was situated with other loci associated with HGT. Finally, the allelic similarities in putative HGT regions with other cc23 isolates and in some cases N. lactamica and N. gonorrhoeae suggests recombination mainly within cc23 but also potentially with other Neisseria species.
The present study revealed that sublineage 1 could not express the Type I restriction system specificity protein due to a transposon, which led to a difference in methylation between the two sublineages. RM systems are known to be located adjacently to mobility-related genes such as transposons in order to promote their own survival43,44,45 and truncation of Type I specificity proteins has been previously described46. No other motifs or predicted RM systems were associated with a particular sublineage. Four more m5C MTases were predicted than actually detected. The detection of m5C methylation is difficult using PacBio sequencing; however, deeper sequencing coverage did indicate that more m5C motifs were probably present. It is therefore possible that there are additional m5C motifs unique to a specific sublineage, although enzymatic digestions and ORF status of the predicted m5C MTases did not indicate any such association.
Genes specific to the Type I RM system as well as modB and modD, which encode phase variable DNA methyltransferases involved in the Type III RM system mediating epigenetic regulation11,38,47,48 were absent (Supplementary Table 7). modB and modD have been described to regulate biofilm formation, adherence and invasion of human epithelial cells as well as increased oxidative stress resistance14. These results are consistent with previous results showing that the compositions of different RM systems are clade-specific, suggesting that the population structure is dependent on the restriction of gene flow between clades caused by distinct RM systems49,50. This in turn suggests that the unique RM system of cc23 isolates consists of a different set of Type I and III RM systems, which will most likely result in a specific DNA methylation pattern unique to this particular cc, as has been shown in previous studies50.
In line with a study by Krauland et al.4, where pyrosequencing was used to complete the whole genomes of two cc23 strains responsible for the serogroup Y increase in the United States, the genomes in the present study lacked genes encoding the TspB, HmbR, NadA proteins, and the meningococcal disease associated (MDA) islands. These gene products are involved in adhesion, iron acquisition, bacterial immune system, endotoxin production, and mobile elements, and have been associated with meningococcal hyperinvasive lineages38,51,52,53,54,55,56. Their absence could therefore explain the particular clinical outcomes such as pneumonia commonly associated with serogroup Y disease57,58,59,60. Furthermore, CRISPR-associated genes cas1 and cas2, which were found among all cc23 genomes, have previously been shown to be associated with carriage isolates53. Notably, other genes were absent in all the serogroup Y genomes investigated in this study (Supplementary Table 7) and in Krauland et al.4; these have not been directly linked to virulence of the meningococcus, but are involved in RM, iron acquisition, and mobile elements that potentially play a role in pathogenicity. Shared differences were found between the early and late strain type in the Krauland et al. study and the sublineages in the present study, namely in the gene pilI involved in the type IV pili structure. None of the other differences in antigen profile or iron acquisition/uptake genes separating the early and late strain types in Krauland's study could be found among the two sublineages in this study; this suggests that the non-synonymous changes in type IV pili encoding genes may play an important role in the emergence of these serogroup Y strains.
Because many of the genes previously regarded as virulence genes have been found in commensal Neisseria species38,61, and the genomes of carrier and invasive strains are very similar62, differences in the presence or absence of genes cannot be the sole reason for the emergence of invasive disease. Instead, our results suggest that point mutations in genes involved in host cell interactions have led to a change in adhesion to epithelial cells, which may have improved colonization, in turn increasing transmission and resulting in expansion of this sublineage. This is also supported by a study showing that no significant differences were found in mortality or clinical outcome between the Swedish strain YI sublineages60. It is therefore probable that sublineage 1 has lower virulence but higher transmissibility; this may be due to either the genetic differences found in the present study or an immunologically-naïve host population. Increased transmission or carriage in connection with increased incidence of serogroup Y has been shown in the UK63,64 and the United States65, and preliminary data from an ongoing carriage study in Sweden indicate similar results but remain to be confirmed.
Conclusions
PacBio sequencing enabled a full comparison of all CDS, complex regions, IGRs, and methylation motifs among isolates belonging to two serogroup Y sublineages. The YI sublineages were distinguished by non-synonymous mutations in genes involved in metabolism, adhesion, iron acquisition, and endotoxin production, as well as differences observed in methylation motifs, which may have played a role in the emergence of sublineage 1. Additional omics approaches including transcriptomics will be needed to study the effects on gene expression.
References
Stephens, D. S., Greenwood, B. & Brandtzaeg, P. Epidemic meningitis, meningococcaemia, and Neisseria meningitidis. Lancet 369, 2196–2210, https://doi.org/10.1016/S0140-6736(07)61016-2 (2007).
Maiden, M. C. et al. Multilocus sequence typing: a portable approach to the identification of clones within populations of pathogenic microorganisms. Proc. Natl. Acad. Sci. USA 95, 3140–3145 (1998).
Yazdankhah, S. P. et al. Distribution of serogroups and genotypes among disease-associated and carried isolates of Neisseria meningitidis from the Czech Republic, Greece, and Norway. J. Clin. Microbiol. 42, 5146–5153, https://doi.org/10.1128/JCM.42.11.5146-5153.2004 (2004).
Krauland, M. G. et al. Whole genome sequencing to investigate the emergence of clonal complex 23 Neisseria meningitidis serogroup Y disease in the United States. PLoS One 7, e35699, https://doi.org/10.1371/journal.pone.0035699 (2012).
Broker, M. et al. Meningococcal serogroup Y emergence in Europe: high importance in some European regions in 2012. Hum. Vaccin. Immunother. 10, 1725–1728 (2014).
Eriksson, L. et al. Whole-genome sequencing of emerging invasive Neisseria meningitidis serogroup W in Sweden. J. Clin. Microbiol. 56, e01409–17, https://doi.org/10.1128/JCM.01409-17 (2018).
Hedberg, S. T., Toros, B., Fredlund, H., Olcen, P. & Molling, P. Genetic characterisation of the emerging invasive Neisseria meningitidis serogroup Y in Sweden, 2000 to 2010. Euro. Surveill. 16, 19885 (2011).
Toros, B. et al. Genome-based characterization of emergent invasive Neisseria meningitidis serogroup Y isolates in Sweden from 1995 to 2012. J. Clin. Microbiol. 53, 2154–2162, https://doi.org/10.1128/JCM.03524-14 (2015).
Vasu, K. & Nagaraja, V. Diverse functions of restriction-modification systems in addition to cellular defense. Microbiol. Mol. Biol. Rev. 77, 53–72, https://doi.org/10.1128/MMBR.00044-12 (2013).
Rotman, E. & Seifert, H. S. The genetics of Neisseria species. Annu. Rev. Genet. 48, 405–431, https://doi.org/10.1146/annurev-genet-120213-092007 (2014).
Srikhanta, Y. N., Fox, K. L. & Jennings, M. P. The phasevarion: phase variation of type III DNA methyltransferases controls coordinated switching in multiple genes. Nat. Rev. Microbiol. 8, 196–206, https://doi.org/10.1038/nrmicro2283 (2010).
Roberts, R. J. et al. A nomenclature for restriction enzymes, DNA methyltransferases, homing endonucleases and their genes. Nucleic Acids Res. 31, 1805–1812, https://doi.org/10.1093/nar/gkg274 (2003).
Srikhanta, Y. N., Maguire, T. L., Stacey, K. J., Grimmond, S. M. & Jennings, M. P. The phasevarion: a genetic system controlling coordinated, random switching of expression of multiple genes. Proc. Natl. Acad. Sci. USA 102, 5547–5551, https://doi.org/10.1073/pnas.0501169102 (2005).
Seib, K. L., Jen, F. E., Scott, A. L., Tan, A. & Jennings, M. P. Phase variation of DNA methyltransferases and the regulation of virulence and immune evasion in the pathogenic Neisseria. Pathog. Dis. 75, https://doi.org/10.1093/femspd/ftx080 (2017).
Braun, R. E., O’Day, K. & Wright, A. Autoregulation of the DNA replication gene dnaA in E. coli K-12. Cell 40, 159–169 (1985).
Yamaki, H., Ohtsubo, E., Nagai, K. & Maeda, Y. The oriC unwinding by dam methylation in Escherichia coli. Nucleic Acids Res. 16, 5067–5073 (1988).
Wion, D. & Casadesus, J. N6-methyl-adenine: an epigenetic signal for DNA-protein interactions. Nat. reviews. Microbiology 4, 183–192, https://doi.org/10.1038/nrmicro1350 (2006).
Chin, C. S. et al. Nonhybrid, finished microbial genome assemblies from long-read SMRT sequencing data. Nat. Methods 10, 563–569, https://doi.org/10.1038/nmeth.2474 (2013).
Treangen, T. J., Sommer, D. D., Angly, F. E., Koren, S. & Pop, M. Next generation sequence assembly with AMOS. Curr. Protoc. Bioinforma. 33, 11.8.1–11.8.18, https://doi.org/10.1002/0471250953.bi1108s33 (2011).
Seemann, T. Prokka: rapid prokaryotic genome annotation. Bioinforma. 30, 2068–2069, https://doi.org/10.1093/bioinformatics/btu153 (2014).
Rutherford, K. et al. Artemis: sequence visualization and annotation. Bioinforma. 16, 944–945 (2000).
Carver, T. J. et al. ACT: the Artemis Comparison Tool. Bioinforma. 21, 3422–3423, https://doi.org/10.1093/bioinformatics/bti553 (2005).
Darling, A. C., Mau, B., Blattner, F. R. & Perna, N. T. Mauve: multiple alignment of conserved genomic sequence with rearrangements. Genome Res. 14, 1394–1403, https://doi.org/10.1101/gr.2289704 (2004).
Alikhan, N. F., Petty, N. K., Ben Zakour, N. L. & Beatson, S. A. BLAST Ring Image Generator (BRIG): simple prokaryote genome comparisons. BMC Genomics 12, 402, https://doi.org/10.1186/1471-2164-12-402 (2011).
Jolley, K. A. & Maiden, M. C. BIGSdb: Scalable analysis of bacterial genome variation at the population level. BMC Bioinforma. 11, 595, https://doi.org/10.1186/1471-2105-11-595 (2010).
Bryant, D. & Moulton, V. Neighbor-net: an agglomerative method for the construction of phylogenetic networks. Mol. Biol. Evol. 21, 255–265, https://doi.org/10.1093/molbev/msh018 (2004).
Bratcher, H. B., Corton, C., Jolley, K. A., Parkhill, J. & Maiden, M. C. A gene-by-gene population genomics platform: de novo assembly, annotation and genealogical analysis of 108 representative Neisseria meningitidis genomes. BMC Genomics 15, 1138, https://doi.org/10.1186/1471-2164-15-1138 (2014).
Huson, D. H. & Bryant, D. Application of phylogenetic networks in evolutionary studies. Mol. Biol. Evol. 23, 254–267, https://doi.org/10.1093/molbev/msj030 (2006).
Murray, I. A. et al. The methylomes of six bacteria. Nucleic Acids Res. 40, 11450–11462, https://doi.org/10.1093/nar/gks891 (2012).
Roberts, R. J., Vincze, T., Posfai, J. & Macelis, D. REBASE—a database for DNA restriction and modification: enzymes, genes and genomes. Nucleic Acids Res. 43, D298–D299, https://doi.org/10.1093/nar/gku1046 (2015).
Cohen-Karni, D. et al. The MspJI family of modification-dependent restriction endonucleases for epigenetic studies. Proc. Natl. Acad. Sci. USA 108, 11040–11045, https://doi.org/10.1073/pnas.1018448108 (2011).
Virji, M., Makepeace, K., Ferguson, D. J., Achtman, M. & Moxon, E. R. Meningococcal Opa and Opc proteins: their role in colonization and invasion of human epithelial and endothelial cells. Mol. Microbiol. 10, 499–510, https://doi.org/10.1111/j.1365-2958.1993.tb00922.x (1993).
Virji, M. et al. Expression of the Opc protein correlates with invasion of epithelial and endothelial cells by Neisseria meningitidis. Mol. Microbiol. 6, 2785–2795, https://doi.org/10.1111/j.1365-2958.1992.tb01458.x (1992).
Sarkari, J., Pandit, N., Moxon, E. R. & Achtman, M. Variable expression of the Opc outer membrane protein in Neisseria meningitidis is caused by size variation of a promoter containing poly-cytidine. Mol. Microbiol. 13, 207–217, https://doi.org/10.1111/j.1365-2958.1994.tb00416.x (1994).
Gibbs, S. et al. Molecular characterization and evolution of the SPRR family of keratinocyte differentiation markers encoding small proline-rich proteins. Genomics 16, 630–637, https://doi.org/10.1006/geno.1993.1240 (1993).
Harrison, O. B., Maiden, M. C. & Rokbi, B. Distribution of transferrin binding protein B gene (tbpB) variants among Neisseria species. BMC Microbiol. 8, 66, https://doi.org/10.1186/1471-2180-8-66 (2008).
Seib, K. L. et al. Specificity of the ModA11, ModA12 and ModD1 epigenetic regulator N6-adenine DNA methyltransferases of Neisseria meningitidis. Nucleic Acids Res. 43, 4150–4162, https://doi.org/10.1093/nar/gkv219 (2015).
Srikhanta, Y. N. et al. Phasevarions mediate random switching of gene expression in pathogenic Neisseria. PLoS Pathog. 5, e1000400, https://doi.org/10.1371/journal.ppat.1000400 (2009).
Marri, P. R. et al. Genome sequencing reveals widespread virulence gene exchange among human Neisseria species. PLoS One 5, e11835, https://doi.org/10.1371/journal.pone.0011835 (2010).
Hao, W. et al. Extensive genomic variation within clonal complexes of Neisseria meningitidis. Genome Biol. Evol. 3, 1406–1418, https://doi.org/10.1093/gbe/evr119 (2011).
Joseph, B. et al. Comparative genome biology of a serogroup B carriage and disease strain supports a polygenic nature of meningococcal virulence. J. Bacteriol. 192, 5363–5377, https://doi.org/10.1128/JB.00883-10 (2010).
Schoen, C., Kischkies, L., Elias, J. & Ampattu, B. J. Metabolism and virulence in Neisseria meningitidis. Front. Cell. Infect. Microbiol. 4, 114, https://doi.org/10.3389/fcimb.2014.00114 (2014).
Naderer, M., Brust, J. R., Knowle, D. & Blumenthal, R. M. Mobility of a restriction-modification system revealed by its genetic contexts in three hosts. J. Bacteriol. 184, 2411–2419 (2002).
Dybvig, K., Sitaraman, R. & French, C. T. A family of phase-variable restriction enzymes with differing specificities generated by high-frequency gene rearrangements. Proc. Natl. Acad. Sci. USA 95, 13923–13928 (1998).
Antonenko, V., Pawlow, V., Heesemann, J. & Rakin, A. Characterization of a novel unique restriction-modification system from Yersinia enterocolitica O:8 1B. FEMS Microbiol. Lett. 219, 249–252, https://doi.org/10.1016/S0378-1097(03)00047-8 (2003).
Manso, A. S. et al. A random six-phase switch regulates pneumococcal virulence via global epigenetic changes. Nat. commun. 5, 5055, https://doi.org/10.1038/ncomms6055 (2014).
Seib, K. L. et al. A novel epigenetic regulator associated with the hypervirulent Neisseria meningitidis clonal complex 41/44. FASEB J. 25, 3622–3633, https://doi.org/10.1096/fj.11-183590 (2011).
Tan, A. et al. Distribution of the type III DNA methyltransferases modA, modB and modD among Neisseria meningitidis genotypes: implications for gene regulation and virulence. Sci. Rep. 6, 21015, https://doi.org/10.1038/srep21015 (2016).
Budroni, S. et al. Neisseria meningitidis is structured in clades associated with restriction modification systems that modulate homologous recombination. Proc. Natl. Acad. Sci. USA 108, 4494–4499, https://doi.org/10.1073/pnas.1019751108 (2011).
Nandi, T. et al. Burkholderia pseudomallei sequencing identifies genomic clades with distinct recombination, accessory, and epigenetic profiles. Genome Res. 25, 129–141, https://doi.org/10.1101/gr.177543.114 (2015).
Capecchi, B. et al. Neisseria meningitidis NadA is a new invasin which promotes bacterial adhesion to and penetration into human epithelial cells. Mol. Microbiol. 55, 687–698, https://doi.org/10.1111/j.1365-2958.2004.04423.x (2005).
Comanducci, M. et al. NadA, a novel vaccine candidate of Neisseria meningitidis. J. Exp. Med. 195, 1445–1454 (2002).
Joseph, B. et al. Virulence evolution of the human pathogen Neisseria meningitidis by recombination in the core and accessory genome. PLoS One 6, e18441, https://doi.org/10.1371/journal.pone.0018441 (2011).
Harrison, O. B. et al. Epidemiological evidence for the role of the hemoglobin receptor, hmbR, in meningococcal virulence. J. Infect. Dis. 200, 94–98, https://doi.org/10.1086/599377 (2009).
Muller, M. G., Moe, N. E., Richards, P. Q. & Moe, G. R. Resistance of Neisseria meningitidis to human serum depends on T and B cell stimulating protein B. Infect. Immun. 83, 1257–1264, https://doi.org/10.1128/IAI.03134-14 (2015).
Bille, E. et al. A chromosomally integrated bacteriophage in invasive meningococci. J. Exp. Med. 201, 1905–1913, https://doi.org/10.1084/jem.20050112 (2005).
Winstead, J. M., McKinsey, D. S., Tasker, S., De Groote, M. A. & Baddour, L. M. Meningococcal pneumonia: characterization and review of cases seen over the past 25 years. Clin. Infect. Dis. 30, 87–94, https://doi.org/10.1086/313617 (2000).
Racoosin, J. A., Whitney, C. G., Conover, C. S. & Diaz, P. S. Serogroup Y meningococcal disease in Chicago, 1991-1997. JAMA 280, 2094–2098 (1998).
Vossen, M., Mitteregger, D. & Steininger, C. Meningococcal pneumonia. Vaccine 34, 4364–4370, https://doi.org/10.1016/j.vaccine.2016.07.013 (2016).
Sall, O. et al. Clinical presentation of invasive disease caused by Neisseria meningitidis serogroup Y in Sweden, 1995 to 2012. Epidemiol. Infect. 145, 2137–2143, https://doi.org/10.1017/S0950268817000929 (2017).
Snyder, L. A. & Saunders, N. J. The majority of genes in the pathogenic Neisseria species are present in non-pathogenic Neisseria lactamica, including those designated as ‘virulence genes’. BMC Genomics 7, 128, https://doi.org/10.1186/1471-2164-7-128 (2006).
Schoen, C. et al. Whole-genome comparison of disease and carriage strains provides insights into virulence evolution in Neisseria meningitidis. Proc. Natl. Acad. Sci. USA 105, 3473–3478, https://doi.org/10.1073/pnas.0800151105 (2008).
Ala’Aldeen, D. A. A. et al. Carriage of meningococci by university students, United Kingdom. Emerg. Infect. Dis. 17, 1762–1763, https://doi.org/10.3201/eid1709.101762 (2011).
Bidmos, F. A. et al. Persistence, replacement, and rapid clonal expansion of meningococcal carriage isolates in a 2008 university student cohort. J. Clin. Microbiol. 49, 506–512, https://doi.org/10.1128/JCM.01322-10 (2011).
Kellerman, S. E. et al. Genotype-specific carriage of Neisseria meningitidis in Georgia counties with hyper- and hyposporadic rates of meningococcal disease. J. Infect. Dis. 186, 40–48, https://doi.org/10.1086/341067 (2002).
Acknowledgements
The sequencing service was provided by the Norwegian Sequencing Centre (http://www.sequencing.uio.no/), a national technology platform hosted by the University of Oslo and supported by the “Functional Genomics” and “Infrastructure” programs of the Research Council of Norway and the Southeastern Regional Health Authorities. This publication made use of the Neisseria Multi Locus Sequence Typing website (http://pubmlst.org/neisseria/) developed by Keith Jolley and hosted at the University of Oxford25. The development of this site was funded by the Wellcome Trust (Grant number 218205/Z/19/Z) and the European Union. This study was supported by grants from the Örebro County Council Research Committee and Nyckelfonden. MCJM and OBH are funded by the Wellcome Trust (Grant numbers: 218205/Z/19/Z and 214374/Z/18/Z). Open access funding provided by Örebro University.
Author information
Authors and Affiliations
Contributions
B.S.: Conceptualization, formal analysis, investigation, writing of the original draft. L.E.: Formal analysis, investigation. A.T.K.: Software, investigation, resources. O.B.H.: Formal analysis, validation, investigation, review & editing of the text. H.B.B.: Formal analysis, investigation, review & editing of the text. J.E.B.: Software. B.P.A.: Formal analysis, validation, resources, investigation, review & editing of the text. A.F.: Formal analysis, validation, resources, investigation. S.T.H.: Conceptualization, methodology, review & editing of the text. R.J.R.: Conceptualization, methodology, Investigation, review & editing of the text. M.C.J.M.: Conceptualization, methodology, review & editing of the text. P.M.: Conceptualization, methodology, funding acquisition, review & editing of the text.
Corresponding author
Ethics declarations
Competing interests
R.J.R., B.P.A. and A.F. work for New England Biolabs, a company that sells research reagents including restriction enzymes and DNA methyltransferases to the scientific community. The commercial affiliation of these authors does not alter our adherence policies on sharing data and materials. All other authors have no conflicts to declare.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Stenmark, B., Harrison, O.B., Eriksson, L. et al. Complete genome and methylome analysis of Neisseria meningitidis associated with increased serogroup Y disease. Sci Rep 10, 3644 (2020). https://doi.org/10.1038/s41598-020-59509-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-59509-y
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.