Abstract
Hand, foot, and mouth disease (HFMD), predominantly occurs among infants and children. Previous studies have shown that suitable, stable temperatures favor HFMD virus reproduction; however, temperature fluctuations also affect virus transmission, and there are, so far, no studies concerning the association between such fluctuations and the incidence of HFMD. The objective of this study was to map the spatial-temporal distribution of HFMD incidence and quantify the long-term effects of temperature fluctuations on HFMD incidence in children. HFMD cases in children under five, from January 2009 to December 2013, in Beijing, Tianjin, and Hebei provinces of China, were used in this study. The GeoDetector and Bayesian space-time hierarchy models were employed to explore the spatial-temporal association between temperature fluctuations and HFMD incidence. The results indicate that HFMD incidence had significant spatial stratified heterogeneity (GeoDetector q-statistic = 0.83, p < 0.05), and that areas with higher risk mainly appeared in metropolises and their adjacent regions. HFMD transmission was negatively associated with temperature fluctuations. A 1 °C increase in the standard deviation of maximum and minimum temperatures was associated with decreases of 8.22% and 11.87% in the risk of HFMD incidence, respectively. The study suggests that large temperature fluctuations affect virus growth or multiplication, thereby inhibiting the activity of the virus and potentially even leading to its extinction, and consequently affecting the spatial-temporal distribution of HFMD. The findings can serve as a reference for the practical control of this disease and offer help in the rational allocation of medical resources.
Similar content being viewed by others
Introduction
Hand, foot, and mouth disease (HFMD), a disease that predominantly occurring among infants and children. It is characterized by flu-like symptoms; a rash on hands, feet, and buttocks; mouth ulcers; poor appetite; and vomiting and diarrhea1,2. The disease is transmitted from person to person by direct contact with respiratory secretions, or through fecal-oral transmission. HFMD can be seriously life threatening, particularly in patients who rapidly develop neurological and systemic complications, which can be fatal1,2.
The primary viruses that cause HFMD are enteroviruses, of which enterovirus 71 (EV71) and Coxsackie virus A16 (CV-A16) are the most commonly reported2. EV71—a single-stranded RNA virus that belongs to the same category as poliovirus and was first diagnosed in California in 1967—is commonly related with the most severe symptoms, including central nervous system disorders and even the development of fatal pulmonary edema1. Over the past few decades, HFMD outbreaks have been reported worldwide, mainly in Asia-Pacific countries, including China, Singapore, Vietnam, Japan, and Malaysia3,4,5,6,7. In 2007 and early 2008, China experienced several large outbreaks of HFMD and promptly created a national enhanced surveillance system in response. Thereafter, on May 2, 2008, HFMD was listed as a category C infectious disease in China, and was made statutorily notifiable. Notably, breakouts of HFMD in many countries have continued to increase due to climate change, viral mutation, lack of comprehensive monitoring systems, and limited medical resources8.
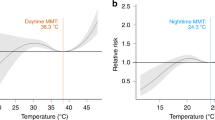
The survival of an organism has been affecting by several environmental factors, genetic composition, evolutionary trend, biological composition and so on. And Shelford’s law of tolerance states that an organism can exist and multiply in a suitable, stable environment, but if the variation of an environmental factor exceeds the tolerance of that organism, the species cannot survive, and may even become extinct9,10. This applies equally to enteroviruses, such as HFMD viruses (Fig. 1). Epidemiological evidences also show that the spread of HFMD viruses is elevated by meteorological factors3,5. For example, Liu et al. found that moderate temperatures promote the growth and transmission of the viruses that cause HFMD11 and Zhu et al. noted that higher temperature promote faster virus reproduction, contributing to increased risk of HFMD incidence12. Similarly, previous studies have demonstrated that, when the temperature is above 25 °C, the infectivity and activity of EV71 is restricted13, while an in vitro experiment found that enterovirus replication was enhanced at 39 °C14. Furthermore, in the broader study of virology, there is other evidence showing the temperature-sensitive nature of enteroviruses and other human enteric viruses15.
Although it is evident that HFMD virus reproduction and transmission is affected by meteorological conditions, such as temperature and humidity, there remain, to our knowledge, no studies concerned with the association between HFMD and temperature fluctuations that might disrupt the suitable, stable environment for the virus and directly affect its survival, and thus influence HFMD transmission12,13,14. Furthermore, against the background of global climate change, temperature variance has been continually intensifying16; thus assessing temperature fluctuations and their relationship to human health could provide novel evidence for policy makers and medical institutions to identify a focus for interventions and the optimal allocation of health resources.
The objective of our study was to 1) map the county-level spatial-temporal distribution of childhood HFMD incidence in the Beijing-Tianjin-Hebei area, China, from 2009 to 2013, and 2) quantify the long-term effects of temperature fluctuations associated with HFMD incidence, while controlling for other factors.
Results
Between January 1, 2009, and December 31, 2013, a total of 598,835 cases in five years of HFMD in 208 counties were reported in Beijing-Tianjin-Hebei area. There presented cyclical trend during the study period. The highest number of cases occurred in the late spring and summer (May to July), with a monthly incidence of 41.03 per 10,000 people. The lowest number of cases appeared in winter (December to February), with a monthly incidence of 1.56 per 10,000 people (Fig. 2).
The relative risk of HFMD varied across the study counties geographically; the GeoDetector q statistic value was 0.83 (p < 0.05), which indicates that there was significant spatial heterogeneity for HFMD risk. The high-risk areas mainly appear in large cities (e.g., Beijing and Tianjin) and their adjacent counties (Fig. 3).
Effect of potential driving factors on HFMD epidemics
In the study, the SD of temperature, used as the index of temperature fluctuation, and its effects on HFMD were analyzed using Bayesian space-time hierarchy model (BSTHM). The results showed that a 1 °C increase in the SD of maximum temperature was associated with a decrease of HFMD incidence of 8.22% (95% CI: −14.63 – −1.82), with a corresponding RR of 0.92 (95% CI: 0.86–0.98). The SD of minimum temperature also presented a similar relationship, with a 1 °C increase in SD of the minimum temperature associated with a decrease in HFMD incidence of 11.87% (95% CI: −19.55 – −4.18) and a corresponding RR of 0.89 (95% CI: 0.82–0.96). The effects of SD of average temperature were also assessed, but there was no significant association with the incidence of HFMD (Table 1).
In addition to the temperature variation factor, other risk factors, used as control variables (e.g., monthly average temperature, relative humidity, precipitation, and wind speed), were also analyzed and showed significant relationships with HFMD (Table 1).
A positive association was found between average temperature and HFMD incidence, which was different from the quantitative relationships between the SD of temperature and the disease. A rise in temperature of 1 °C was associated with an increase of 17.10% (97.5% CI: 14.84–19.38) in the incidence of HFMD; the corresponding RR was 1.19 (95% CI: 1.16–1.21). There was also a positive association between HFMD incidence and relative humidity—a 1% increase in relative humidity was associated with a 3.67% increase (95% CI: 3.05–4.30) in the incidence of HFMD, with a corresponding RR of 1.037 (95% CI: 1.03–1.04). Precipitation and wind speed showed negative correlations with HFMD—a 1 mm reduction in precipitation and a 1 m/s decrease in wind speed were associated with 0.15% (95% CI: −0.22 – −0.08) and 17.20% (95% CI: −26.82 – −7.75) decreases in the incidence of HFMD, respectively, with corresponding RRs of 0.86 (95% CI: 0.80–0.92) and 0.84 (95% CI: 0.77–0.93) (Table 1).
Discussion
HFMD has become an increasingly significant health problem among children in recent years. In this study, the spatial-temporal distribution and effects of temperature fluctuations on HFMD incidence were quantified for the Beijing-Tianjin-Hebei area, China. The study found that there was a significant spatial heterogeneity for HFMD risk, and that disease transmission had a negative association with temperature fluctuations.
Studies have indicated that there is a suitable, stable temperature for transmission of viruses related to HFMD3,6,12. Stantonet al. demonstrated that, compared with replication at 37 °C, enterovirus replication was inhibited by nearly 90% at 39 °C, greatly reducing the incidence of HFMD14. Onozuka et al., in Japan, found that the effect of temperature on HFMD cases peaked at 29 °C6. In the current study, it was indicated that temperature change was closely related to disease risk variant, which is similar to the previous studies. For examples, Zhang et al. found that, in Henan province of China, the disease of HFMD risk rise 4.09% with a 1 °C increase in temperature17. Moreover, Dung et al. demonstrated that in Vietnam the HFMD risk increase 7% with a 1 °C rise in temperature18. These studies suggest that if the temperature diverges too much from the suitable temperature, it can affect the transmission of HFMD.
To our knowledge, some studies have indicated that temperature fluctuation was a serious health risk factor for the infectious diseases. For examples, Joshi et al. showed that, in Korea, the aseptic meningitis has a closely association with temperature fluctuation19. Similarly, Beck et al. demonstrated that temperature fluctuation was significantly connected with malaria within the malaria transmission zone in sub-Saharan Africa20. Meanwhile, Abbas et al. found that, in Karachi, temperature fluctuation presented significantly association with dengue fever21. Additionally, Joshi et al. presented that, in Korea, temperature fluctuation closely related to hemorrhagic fever22.
The study found that the HFMD risks also were strongly related to temperature fluctuations, which presented different quantitative relationships compared with that between the disease and average temperature. It was indicated that a 1 °C increase in the SD of maximum and minimum temperatures was associated with decreased risk of HFMD incidence of 8.22% and 11.87%, respectively. The potential mechanism may be because HFMD virus growth and reproduction have adapted to the most suitable temperature, if a large temperature fluctuation occurs, this would exceed the tolerance of virus growth or multiplication and inhibit the activity of the virus or even cause its extinction9,10, ultimately affecting the incidence of HFMD.
Moderate and stable temperatures in the environment may be good for the survival of HFMD viruses, accelerating their transmission11,12, while large fluctuations of temperature may weaken the reproductive capacity of infectious pathogens and vectors, thus altering the survival of viruses in the physical environment and decreasing disease prevalence accordingly. This is reasonable according to experimental findings that indicate that, when the temperature is higher than 25 °C, the activity and infectivity of EV71 is restricted13. A study by Shelford also demonstrated that if the quantity (or quality) of a factor is insufficient or excessive for an organism to exist and multiply, the species cannot survive, and may even become extinct9,10. A further study demonstrated that serological antibodies in the human body may adjust according to temperature changes23, and thus environmental temperature fluctuations may be one of the major underlying factors influencing the incidence of this disease. To assess the influence of temperature fluctuations, other potential meteorological factors were used as control variables. A positive association was found between relative humidity and HFMD incidence, which is consistent with the results from previous studies. For example, one study indicated that every 1% increase in relative humidity was association with a 4.7% rise in HFMD, and found a threshold of humidity at 80%6; another study observed that increased relative humidity was related to a 13% increase in the risk of HFMD23.
The current study found that wind speed and precipitation were negatively correlated with HFMD incidence, which is also consistent with other studies. For example, a previous study in Hong Kong found a negative association between HFMD incidence and wind speed24, while a study in Singapore reported a negative relationship between precipitation and HFMD25, as heavy downpours can disrupt the survival environment of viruses26. Another study found that heavy rainfall is negatively related to physical activity27, thus significant precipitation could interrupt transmission by reducing social contact24.
The results from the BSTHM showed that the spatial distribution of HFMD risk was non-homogeneous. Notably, areas with the highest incidence were mainly concentrated in large cities and their adjacent areas. The areas with developed economies, high population density, and mixed socio-human environment (e.g. Beijing and Tianjin) were the main epidemic regions, which is consistent with previous studies. For instance, a previous study found that the HFMD incidence in economically developed areas, including Beijing, Tianjin, Shanghai, and Zhejiang, was higher than in less developed areas17,28,29,30. A further study found that the incidence of HFMD was higher in the provincial capital city of Chengdu than in other counties in Sichuan province, China31. A potential mechanism may be that, due to rapid economic development and urbanization in recent years, there is both higher population density and an increased floating population in large cities and their adjacent counties, thus inevitably promoting more frequent communication and contact with others, which is conducive to the transmission of HFMD.
There are some limitations to this study that should be mentioned. Spatial data at the county level was used, which could introduce an ecological fallacy. Spatial heterogeneity also exists within a county area; for example, populations in urban and rural areas may have different living conditions and healthcare, which would reflect on temperature variations differently. In future studies, data at a finer spatial scale (e.g., villages and towns) will be collected to analyze the relationship between HFMD and environmental factors. Furthermore, the data used in this study was from 2009 to 2013 in Beijing, Tianjin and Hebei province of China, although the findings and conclusions were applicable to the time period and region, in the future, the data covering more regions in recent years will be collected and analyzed to strengthen the study.
Conclusions
Temperature fluctuations play an important role in shaping HFMD spatiotemporal patterns. HFMD transmission is negatively associated with temperature variations, implying that the risk of HFMD decreases in temperature-unstable environments. These findings can serve as reference and basis for the surveillance and control of the disease in practice, and may be helpful in the rational allocation of medical resources.
Methods
Study area
The study region is located in the north of China; includes Beijing, Tianjin, and Hebei provinces; and is a typical semi-humid continental monsoon climate in the North Temperate Zone. It is hot and rainy in summer, and cold and dry in winter. The geographical location of the study area is shown in Fig. 4.
Beijing is the capital of China, a megalopolis, with an area of 16,400 km2 and a population of 20.7 million. Tianjin is a municipality directly governed by the central government, with an area of 11,900 km2 and a population of 14.1 million. Hebei province is located around Beijing and Tianjin, with a total area of 188,800 km2 and a population of 72.9 million.
Data
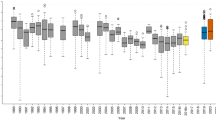
Data on HFMD cases in children under five, from January 2009 to December 2013, was obtained from the Chinese Center for Disease Control and Prevention (http://www.phsciencedata.cn). Monthly meteorological data was obtained for the same period from the China Meteorological Data Sharing Service System (http://data.cma.gov.cn/). Temperature fluctuations were measured by the monthly standard deviation (SD) of average temperature, calculated using the daily average, maximum, and minimum values. In addition to these factors indicating temperature fluctuations, referencing the previous studies, other meteorological factors, including monthly average temperature, relative humidity, precipitation, hours of sunshine and wind speed, were used as control variables in the model (Figs. 5 and 6).
GeoDetector
GeoDetector is a novel spatial variation analysis method, which can be used to explore the stratified heterogeneity of a responding variable, where phenomena within strata are more similar than between strata32,33,34. In this study, GeoDetector was used to quantify the heterogeneity of the temporal and spatial variations of HFMD risk.
The q value can be expressed as:
where q denotes the degree of stratified heterogeneity for the dependent variable. Its value ranges from 0 to 1—the larger the q value, the more significant the spatial heterogeneity from the target variable. N is the number of counties and σ2 expresses the variance across all the statistical units in the study area. The study area is stratified into L strata, presented by h = 1, 2,…, L, implemented through a discretization process. σh2 is the variance within stratum h in the study area.
Bayesian space-time hierarchy model
The BSTHM has been widely used in disease mapping with sparse data. This model can overcome, to a certain extent, the shortcomings of a small sample and the autocorrelation of spatial-temporal data. And it also can make full use of the overall information, sample information, and prior information to estimate the posterior distribution of spatial-temporal parameters.
In this study, we used the BSTHM to analyze the county-level spatial-temporal distribution of HFMD incidence from 2009 to 2013 and quantify its relationships with temperature variation, after controlling for other meteorological factors. A space-time hierarchy model with Poisson distribution was used to model the monthly cases of HFMD. Letting yit and ni represent the number of disease cases and the risk population, respectively, with county i = (1,…,208) and month t = (1,…,60), the disease cases can be modeled as:
where uit indicates the potential risk of HFMD in region i and month t. Among them, α is the overall log disease risk during a selected period in the study area. The spatial index, si, throughout the total study period, denotes the residual spatial distribution of disease risks across the study area; this was affected by some temporal relative stable factors in the study period, such as local geographic environment, economic conditions, and medical resources. Time span relative to the midpoint tmid over the study period is represented by t* = t − tmid. The calculated spatial-temporal variability in disease risk in this model is decomposed in the following way:
The temporal term, (b0t* + vt), indicates the overall time trend for all counties, defined as a linear trend, b0t*, and additional Gaussian noise, vt. Specifically, the term b1it* represents the departure from b0 for each county, which allows for each county to have its own trend, while b0 measures the overall temporal change in disease risk. For example, a positive estimate for b1i suggests that the local variation intensity is higher than the overall variation trend; conversely, a negative estimate for b1i reveals that the local variation intensity is lower than the overall variation trend.
The term xvit repressents the temperature variation variable for area i and month t, and βv is the corresponding regression coefficient. The term xnit represents the n-th of the other potential confounds; the regression coefficient of these explanatory variables is βn.
The Gaussian random noise variable is represented by ε1i, involving all the factors that are not considered in the model but affect the explanatory variable, which is assumed to follow a normal distribution. That is, the Gaussian noise εit is modeled as εit ~N (0, σε2), and the temporal noise as vt ~ N (0, σv2). As suggested by Gelman, in this model, the prior distribution of the SDs (e.g., σv, σε) of all the random variables is determined as a strictly positive half Gaussian distribution N+∞(0, 0.1).
In this study, the Besag, York, and Mollie (BYM) spatial model was introduced to determine the prior distribution of the parameters si and b1i35,36. It is a convolution of a spatially unstructured random effect and a spatially structured random effect, and can be expressed as follow:
where the ui represents unstructured random effects, and the vi represents spatially structured heterogeneity, f(ci) is the non-linear effect of acovariate ci.
And the conditional autoregressive (CAR) prior is used to enhance the random effect of spatial structure in BYM with a spatial adjacency matrix W. The CAR prior on the spatial random effect indicates that adjacent counties tend to have similar disease risks.
All parameters were implemented in WinBUGS37, a statistical software package that was designed specifically for Bayesian calculations. Posterior distributions of all parameters in the model were obtained through Markov chain Monte Carlo (MCMC) simulations.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Qiu, J. Enterovirus 71 infection: a new threat to global public health? Lancet Neurology. 7, 868 (2008).
Xing, W. et al. Hand, foot, and mouth disease in China, 2008–12: an epidemiological study. Lancet Infectious Diseases. 14, 308–318 (2014).
Xiao, X. et al. The exposure-response relationship between temperature and childhood hand, foot and mouth disease: A multicity study from mainland China. Environment International 100, 102–109 (2017).
Ang, L. W. et al. Epidemiology and Control of Hand, Foot and Mouth Disease in Singapore, 2001–2007. Annals Academy of Medicine Singapore 38, 106–112 (2009).
Huong Xuan, N. et al. Temporal and spatial analysis of hand, foot, and mouth disease in relation to climate factors: A study in the Mekong Delta region, Vietnam. Science of the Total Environment 581, 766–772 (2017).
Onozuka, D. & Hashizume, M. The influence of temperature and humidity on the incidence of hand, foot, and mouth disease in Japan. Science of the Total Environment 410, 119–125 (2011).
Chua, K. B. & Kasri, A. R. Hand foot and mouth disease due to enterovirus 71 in Malaysia. Virologica Sinica 26, 221–228 (2011).
Hosoya, M. et al. Genetic diversity of coxsackievirus A16 associated with hand, foot, and mouth disease epidemics in Japan from 1983 to 2003. Journal of Clinical Microbiology 45, 112–120 (2007).
Shelford, V. E. Physiological animal geography. Journal of Morphology 22, 551–618 (1911).
Shelford, V. E. B. Animal communities in temperate America: as illustrated in the Chicago region. Progress in Inverse Spectral Geometry 135, 133–173 (1997).
Liu, W. et al. Spatiotemporal Dynamics of Hand-Foot-Mouth Disease and Its Relationship with Meteorological Factors in Jiangsu Province, China. Plos One 10 (2015).
Zhu, L. et al. Assessment of temperature effect on childhood hand, foot and mouth disease incidence (0–5 years) and associated effect modifiers: A 17 cities study in Shandong Province, China, 2007–2012. Science of the Total Environment 551, 452–459 (2016).
Arita, M. et al. Temperature-sensitive mutants of enterovirus 71 show attenuation in cynomolgus monkeys. Journal of General Virology 86, 1391–1401 (2005).
Stanton, G. J., Langford, M. P. & Baron, S. Effect of interferon, elevated-temperature, and cell type on replication of acute hemorrhagic conjunctivitis viruses. Infection and Immunity 18, 370–376 (1977).
Kung, Y. H. et al. Introduction of a strong temperature-sensitive phenotype into enterovirus 71 by altering an amino acid of virus 3D polymerase. Virology 396, 1–9 (2010).
Parey, S., Dacunha Castelle, D. & Hoang, T. T. H. Mean and variance evolutions of the hot and cold temperatures in Europe. Climate Dynamics 34, 345–359 (2010).
Zhang, X. X., Xu, C. D. & Xiao, G. X. Space-time heterogeneity of hand, foot and mouth disease in children and its potential driving factors in Henan, China. Bmc Infectious Diseases 18, 638 (2018).
Dung, P. et al. Spatiotemporal variation of hand-foot-mouth disease in relation to socioecological factors: A multiple-province analysis in Vietnam. Science of the Total Environment 610, 983–991 (2018).
Joshi, Y. P. et al. Associations between meteorological factors and aseptic meningitis in six metropolitan provinces of the republic of Korea. International Journal of Environmental Research and Public Health 13, 1193 (2016).
Beck Johnson, L. M. et al. The importance of temperature fluctuations in understanding mosquito population dynamics and malaria risk. Royal Society Open Science 4, 160969 (2017).
Abbas, S. & Ilyas, M. Assessing the impact of EI Nino southern oscillation index and land surface temperature fluctuations on dengue fever outbreaks using ARIMAX(p)-PARX(p)-NBARX(p) models. Arabian Journal of Geosciences 11, 777 (2018).
Joshi, Y. P., Kim, E. H. & Cheong, H. K. The influence of climatic factors on the development of hemorrhagic fever with renal syndrome and leptospirosis during the peak season in Korea: an ecologic study. BMC Infectious Diseases 17, 406 (2017).
Guo, C. et al. Short-term effects of meteorological factors on pediatric hand, foot, and mouth disease in Guangdong, China: a multi-city time-series analysis. BMC infectious diseases 16, 524–524 (2016).
Wang, P., Goggins, W. B. & Chan, E. Y. Y. Hand, Foot and Mouth Disease in Hong Kong: A Time-Series Analysis on Its Relationship with Weather. Plos One 11 (2016).
Hii, Y. L., Rocklov, J. & Ng, N. Short Term Effects of Weather on Hand, Foot and Mouth Disease. Plos One 6 (2011).
Cheng, J. et al. Associations between extreme precipitation and childhood hand, foot and mouth disease in urban and rural areas in Hefei, China. Science of the Total Environment 497, 484–490 (2014).
Belanger, M., Gray-Donald, K., O’Loughlin, J., Paradis, G. & Hanley, J. Influence of Weather Conditions and Season on Physical Activity in Adolescents. Annals of Epidemiology 19, 180–186 (2009).
Zhu, Q., Hao, Y., Ma, J., Yu, S. & Wang, Y. Surveillance of Hand, Foot, and Mouth Disease in Mainland China (2008–2009). Biomedical and Environmental Sciences 24, 349–356 (2011).
Xu, C. D. & Xiao, G. X. Spatiotemporal risk mapping of hand, foot and mouth disease and its association with meteorological variables in children under 5 years. Epidemiology & Infection 145, 2912–2920 (2017).
Xu, C. D., Zhang, X. X. & Xiao, G. X. Spatiotemporal decomposition and risk determinants of hand, foot and mouth disease in Henan, China. Science of The Total Environment 657, 509–516 (2019).
Liu, L., Zhao, X., Yin, F. & Lv, Q. Spatio-temporal clustering of hand, foot and mouth disease at the county level in Sichuan province, China, 2008-2013. Epidemiology and Infection 143, 831–838 (2015).
Wang,J. F. & Xu, C. D. Geodetector: Principle and prospective. Acta Geographica Sinica (2017).
Wang, J. F., Zhang, T. L. & Fu, B. J. A measure of spatial stratified heterogeneity. Ecological Indicators 67, 250–256 (2016).
Wang, J. F. et al. Geographical Detectors-Based health risk assessment and its application in the neural tube defects study of the Heshun region, China. International Journal of Geographical Information Science 24, 107–127 (2010).
Besag, J., York, J. & Mollie, A. Bayesian image-restoration, with 2 applications in spatial statistics. Annals of the Institute of Statistical Mathematics 43, 1–20 (1991).
Lia, G., Haining, R., Richardson, S. & Best, N. Space–time variability in burglary risk: A Bayesian spatio-temporal modelling approach. Spatial Statistics 9, 180–191 (2014).
Lunn, D. J., Thomas, A., Best, N. & Spiegelhalter, D. WinBUGS - A Bayesian modelling framework: Concepts, structure, and extensibility. Stat Comput 10, 325–337 (2000).
Acknowledgements
The authors would like to acknowledge the following grants: National Science Foundation of China (41901331, 41601478, 41531179, 41971357), Innovation Project of LREIS (O88RA205YA, O88RA200YA), Henan Postdoctoral Science Foundation (CJ3050A0670196), a grant from State Key Laboratory of Resources and Environmental Information System.
Author information
Authors and Affiliations
Contributions
C.X. and J.L. conceived designed the study. X.Z. and J.L. performed the experiments. X.Z., G.X. and L.W. analyzed the data. C.X., X.Z. and Y.Z. wrote the paper. All Authors contributed to the final version of the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xu, C., Zhang, X., Wang, L. et al. Effects of temperature fluctuations on spatial-temporal transmission of hand, foot, and mouth disease. Sci Rep 10, 2541 (2020). https://doi.org/10.1038/s41598-020-59265-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-59265-z
This article is cited by
-
Extended Impact of Cold Air Invasions in East Asia in Response to a Warm South China Sea and Philippine Sea
Advances in Atmospheric Sciences (2023)
-
Estimating the influence of high temperature on hand, foot, and mouth disease incidence in China
Environmental Science and Pollution Research (2023)
-
Spatiotemporal associations between hand, foot and mouth disease and meteorological factors over multiple climate zones
International Journal of Biometeorology (2023)
-
The effect and its critical window for ambient temperature and humidity in pregnancy on term low birth weight
Environmental Science and Pollution Research (2022)
-
A five-year retrospective study on the epidemiology of hand, foot and mouth disease in Sabah, Malaysia
Scientific Reports (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.