Abstract
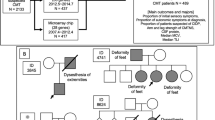
Polyneuropathy (PNP) has been reported to be a possible phenotypic feature in Gaucher disease type 1 (GD1), while less is known about PNP in type 3 (GD3). We performed a cross-sectional study, exploring PNP in a Swedish GD cohort. Clinical assessment and blood biochemistry were carried out in 8 patients with GD1 and 11 patients with GD3. In patients with symptoms or clinical findings indicative of PNP, nerve conduction studies and quantitative sensory testing were performed. Assessments were compared to historic controls. A subclinical small fiber neuropathy (SFN) was demonstrated in 2 of 8 patients in the significantly (p = 0,021) older GD1 cohort. A large fiber PNP was evident in an additional 3 GD1 patients but could not be ascribed as disease manifestation. No GD3 patients exhibited neurophysiological evidence of small or large fiber PNP attributed to GD3. Compared to historic controls, no significant group differences were evident with regard to neuropathy rating scores. In summary, our study does not support large fiber PNP as a prevalent manifestation of GD. SFN is a possible feature in GD1, although small sample size limits definite conclusions. Our study provides novel data, arguing against clinically significant small or large fiber PNP in GD3.
Similar content being viewed by others
Introduction
Gaucher disease (GD) is an autosomal recessive disease, caused by mutations in the GBA1 gene. This gene encodes the lysosomal enzyme glucocerebrosidase (GCase), which is essential for the metabolism of glycosphingolipids. Enzyme deficiency generates accumulation of its main substrate, glucosylceramide, considered central for disease pathogenesis. GD is thus characterized as a lysosomal storage disorder1.
GD is classified into three different forms with regard to phenotypic presentation. GD type 2 (GD2) is characterized by childhood-onset, with aggressive involvement of the central nervous system (CNS), often resulting in death within 2 years. GD type 3 (GD3) presents with a variable disease severity but a mandatory severe CNS involvement1,2,3. GD type 1 (GD1) has historically been viewed as a non-neuropathic phenotype, mainly presenting with symptoms secondary to visceral involvement2. However, it is now well-established that both homozygous and heterozygous GBA1 mutations also confer an increased risk of developing Parkinson’s disease (PD)4.
In recent years, retrospective, cross-sectional and prospective studies evaluating involvement of the peripheral nervous system (PNS) in GD1 have been conducted, showing an increased prevalence and incidence of polyneuropathy (PNP)5,6,7. PNP associated with GD1 has been described as axonal, engaging both motor and sensory nerve fibres7.
Cobalamin deficiency is a known cause of PNP8. The intracellular cobalamin pathways are dependent on the initial cellular uptake of cobalamin into the lysosome, from where further cellular processing ensues9,10,11. An increased susceptibility to functional cobalamin deficiency in GD, precipitated by disease associated lysosomal dysfunction, has been suggested12.
We conducted a cross-sectional study, exploring PNP and cobalamin status in a Swedish GD cohort.
Methods
Subjects
From November 2017 until August 2018, all adult patients attending regular clinical visits to the Dept. of Hematology, Karolinska University Hospital and the Dept. of Medicine, Sunderby Regional Hospital of Norrbotten County, were invited to participate in the study. All patients had a previously confirmed molecular and genetic diagnosis of GD1 or GD3.
All patients have signed an informed consent and the study was approved by the regional ethical board of Stockholm, Sweden (ref. nr 2016/19-31/1 and 2017/1957-32/1, Regionala Etikprövningsnämnden Stockholm). Patient related investigations were undertaken in accordance with the Helsinki Declaration.
Clinical assessment
Patients were evaluated by oral interview assessing current medication, disease history, smoking habits and a review of medical records. The presence of heavy alcohol consumption, as outlined by the Swedish National Board of Health and Welfare, was determined by oral history13. Standardized questions, with regard to symmetric symptoms compatible with a possible PNP, were undertaken including; “cold, pinching or burning pain-like sensations in extremities”, “electric shock-like pain or sensations in extremities”, “subjective muscle weakness” and “subjective impairment of sensation”. Clinical examination encompassed the Utah Early Neuropathy Scale (UENS) with the aim of detecting an early sensory predominant PNP14. GD3 patients were further evaluated with the modified Severity Scoring Tool (mSST)15.
Biochemistry
Non-fasting venous blood samples were collected for complete blood count, blood differential, creatinine, electrolytes, liver function test, s-electrophoresis, p/s-glucose and/or B-hemoglobin A1c (HbA1c). As part of the targeted assessment of cobalamin status, levels of p/s-homocysteine (Hcy), s-folic acid (folate), s-vitamin B12 (B12) and s-methylmalonic acid (MMA) were determined. Analyses were carried out according to established GMP approved clinical routines at Karolinska University Hospital, Sunderby County Hospital and University Hospital of Umeå.
Neurophysiology
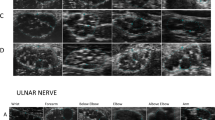
Patients describing symptoms compatible with PNP, or an UENS score ≥4, were scheduled for electrodiagnostic testing. UENS is considered sensitive in detecting small fiber neuropathy (SFN) and a cut-off value of >4 has been used in previous studies evaluating sensory predominant PNP in patients with PD14,16,17. Considering previous phenotypic descriptions of PNP in GD1, including SFN and axonal large fiber sensorimotor PNP, the cut-off value of ≥4 was chosen7,18. Testing was performed at three different sites (Stockholm, Sunderby and Umeå) and the protocol consisted of unilateral motor and sensory nerve conduction studies from the median, peroneal, tibial, ulnar and sural nerves. The parameters were carried out with Natus, Viking EDX (Cephalon A/S; Denmark) and compared to normal values corrected for age and/or height. Quantitative sensory testing (QST) was performed bilaterally in feet and unilaterally in hand. At the University Hospital of Umeå, QST was performed with Modular Sensory Analyzer Thermotest (Somedic; Sweden), at Karolinska University Hospital with Medusa, TSA II (Cephalon A/S; Denmark) and at Sunderby Regional Hospital with RollTemp (Somedic; Sweden).
Controls
Historic controls were used for comparison of UENS scores and biochemical measurements including MMA, B12, Hcy and folate. The controls are part of a previously published study which recruited control subjects aged 55–70 years with no previously known diagnosis of PNP, diabetes mellitus or alcohol overconsumption17. In order to generate a sample size comparable to the GD cohorts in the present study, the 11 youngest historic controls were used.
Statistical analyses
Categorical variables were compared with Fisher’s Exact Test. Non-parametric Mann-Whitney U-test was used for comparison of numerical variables. A two-tailed p-value of <0,05 was considered significant. All statistical analyses were carried out with IBM SPSS Statistics for Windows, version 25.0 (IBM Corp., Armonk, N.Y., USA).
Results
GD1 cohort
A summary of the characteristics of the GD1 cohort is shown in Table 1. One patient declined participation and the cohort (n = 8) had a median age of 54 years. Three of the patients (Pt 1, Pt 5, Pt 6) reported symptoms compatible with PNP, along with an UENS score ≥4. An additional two patients (Pt 2, Pt 8) had an UENS score ≥4 without reporting symptoms.
Patient 1 (Pt 1) was not assessed electrodiagnostically, since an established chemotherapy induced peripheral neuropathy due to lung cancer was present. Neurophysiological evidence of a symptomatic mild demyelinating motor PNP was found in Pt 5 and Pt 6. In Pt 5, an alcohol overconsumption was evident and the patient exhibited a mild folic acid deficiency. Pt 6 received treatment with miglustat and further investigation could not identify any other cause of PNP. The two asymptomatic patients with an UENS score ≥4, Pt 2 and Pt 8, both demonstrated findings on QST compatible with SFN (Table 1).
Mild Hcy elevations were seen in three patients, however none of the GD1 patients showed evidence of functional cobalamin deficiency, as reflected by normal MMA levels (Table 1). No patient demonstrated increased levels of HbA1c or visible monoclonal gammopathy.
GD3 cohort
A summary of the characteristics of the GD3 cohort is shown in Table 2. No patient declined participation and the cohort (n = 11) had a median age of 39 years. With the exception of Pt 19, all were classified as Norrbottnian GD3. Three of the patients (Pt 14, Pt 16, Pt 17) reported symptoms compatible with PNP of which one had an UENS score ≥4. An additional two patients (Pt 9, Pt 19) had an UENS score ≥4 without reporting symptoms.
Electrodiagnostic testing was performed in the three symptomatic patients, while Pt 9 declined testing and Pt 19 was considered ethically unsuitable due to cognitive impairment. A mild large fiber PNP was only demonstrated in Pt 16, who suffered from concurrent rheumatoid arthritis and polymyalgia rheumatica treated with prednisolone. QST revealed pathology in Pt 17, who suffered from severe kyphosis, however the distribution of findings was asymmetric and not deemed typical for SFN.
Only one patient, without symptoms or clinical findings, demonstrated an elevation of MMA, fitting with a functional cobalamin deficiency (Table 2). No monoclonal gammopathy was detected and none of the patients with neuropathic symptoms had elevated s-glucose.
Comparison to historic controls
The control group was matched to the two GD cohorts with regard to gender, but significantly older compared to the GD3 cohort (p < 0,05). No significant differences in UENS scores were seen when comparing controls to GD1 (p = 0,19) and GD3 (p = 0,49). None of the two GD groups had significantly higher MMA levels when compared to controls (Table 3).
Discussion
The present study, comprising 8 GD1 and 11 GD3 patients, demonstrated two cases interpreted as GD1 associated SFN and no clear case of GD1 or GD3 associated large fiber PNP.
In two GD1 patients with large fiber PNP (Pt 1, Pt 5), the underlying etiology was clouded by co-morbidities and the large fiber PNP found in the third GD1 patient (Pt 6) was confounded by exposure to miglustat. Since the initial treatment study from 2000, miglustat has been debated whether or not it could be causative of PNP19. The previously referenced study from 2010 challenged such association by demonstrating an increased prevalence and incidence of PNP in GD1 patients not receiving miglustat7. In the present study, we considered miglustat a potential confounder and the demonstrated PNP in Pt 6 was not interpreted as a disease manifestation.
Two GD1 patients exhibited clinical signs and findings on QST compatible with SFN with no other identified cause. Thus, we cannot exclude SFN as a possible phenotypic feature in GD1, although the current study lacks a sufficient sample size do draw firm conclusions. We note that the GD1 cohort tended to have a higher median UENS score compared to the older historic controls, although not significant (p = 0,19) and influenced by the other causes of PNP identified in the GD1 group (Table 3). The absence, in our GD1 cohort, of large fiber PNP as a clear disease manifestation differs from the previously referred study7. However, in that study, the sample size was larger and no neurophysiological assessment of SFN was carried out. Thus, we cannot exclude the possibility of co-existent SFN in the PNP cases reported there, which would be in agreement with the SFN cases detected in our study and the study by Devigili et al.18. A longitudinal follow-up of our GD1 cohort could discern whether patients with SFN are at risk of developing large fiber involvement over time.
Three of eleven patients in the GD3 cohort had symptoms compatible with PNP, of which none demonstrated neurophysiological evidence of SFN. Only one patient, Pt 16, showed evidence of mild large fiber PNP, but co-morbidities prevented the establishment of a causal relationship to GD3.
With regard to PNS involvement in GD3, previous studies are scarce. Eleven patients with Norrbottnian GD3 were evaluated in a study from 1980, including motor nerve conduction studies and electromyography, without signs of PNP. The majority of these patients were under the age of 20 and no assessment of small fiber function was carried out19. To our knowledge, no other systematic small and large fiber PNP evaluation has been performed in patients with GD3.
In the present study, a significant (p = 0,021) age difference is seen with a higher median age in the GD1 group compared to GD3. More specifically, the two GD1 patients with SFN were aged 55 and 61 at time of evaluation. Thus, SFN as a late-onset feature in GD1 is a possibility, similarly to what is seen with the development of PD in patients carrying GBA1 mutations4,20. A higher prevalence of PNP in GD3 could have been expected, considering the greater CNS involvement seen in this disease subtype compared to GD1. There are possible explanations to our surprising findings in this regard. As mentioned, the median age was lower in the GD3 cohort why the existence of late-onset SFN as a feature in GD3 cannot be excluded. Furthermore, the molecular mechanisms underlying peripheral neuropathy associated with GD are not well understood, why different pathways generating CNS and PNS pathology respectively are possible. In this context, it is worth mentioning the established association between the GBA1 variant E326K and PD, a variant that surprisingly does not cause GD in homozygous state21. Finally, it is possible that unknown factors attributed to the Norrbottnian form of GD3 are not present in the global GD3 population, thus our results are primarily representative of the Norrbottnian GD3 population.
Our study argues against cobalamin deficiency being a prevalent finding in GD, with only one asymptomatic patient exhibiting functional cobalamin deficiency (Tables 2 and 3). Thus, the study does not support an association between PNP and cobalamin deficiency in GD.
The main limitation of the present study is small sample size, which is attributed to the rarity of the disease. In the UK, a GD prevalence of 1 in 200 000 has been estimated22. However, since GD3 represents less than 10% of all GD patients, we believe the size of our GD3 cohort is a strength of our study1.
Confounding factors exist in the assessment of SFN with UENS and QST. QST is a subjective method and does not differentiate between peripheral and central sensory tracts, why myelopathy is a possible confounder even though we deemed symmetric findings as a requirement for SFN diagnosis. Furthermore, Pt 16 was examined with the less sensitive RollTemp instrument. Since this patient had other concurrent diseases, we do not believe the interpretation of our main findings would have changed if QST had revealed SFN. Moreover, we cannot exclude the presence of a subclinical PNP in Pt 9 and Pt 19, considering their mildly increased UENS scores. In this context, it is notable that Pt 19 was exposed to miglustat. Finally, electromyography was not part of the study protocol why a full assessment of potential lower motor neuron involvement was not obtained. Neuronal cell loss, including the spinal anterior horn, has previously been described in an infant with severe GD223.
In conclusion, the present study did not identify large fiber PNP as a prevalent feature in GD, but we cannot exclude SFN as a possible disease manifestation of GD1 as proposed in a previous study18. This concept is clinically relevant when assessing pain in GD1 patients, since the treatment for neuropathic pain differs from skeletal or inflammatory pain18. Furthermore, considering the absence of neurophysiological evidence of small or large fiber PNP attributed to GD3 in our cohort, our study questions whether a clinically significant PNP is evident in, at least, the Norrbottnian form of GD3, despite the pronounced level of CNS disease severity associated with this disease subtype.
Future studies, including objective measures of SFN such as corneal confocal microscopy and skin biopsies, in GD1 and GD3 patients and matched controls, could further discern the prevalence, severity and underlying pathophysiology of PNP in GD.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Cox, T. M. Gaucher disease: clinical profile and therapeutic developments. Biologics 4, 299–313, https://doi.org/10.2147/BTT.S7582 (2010).
Mercimek-Mahmutoglu, S. et al. Neurological and brain MRS findings in patients with Gaucher disease type 1. Mol Genet Metab 91, 390–395, https://doi.org/10.1016/j.ymgme.2007.03.009 (2007).
Pastores, G. M. Neuropathic Gaucher disease. Wien Med Wochenschr 160, 605–608, https://doi.org/10.1007/s10354-010-0850-x (2010).
Aflaki, E., Westbroek, W. & Sidransky, E. The Complicated Relationship between Gaucher Disease and Parkinsonism: Insights from a Rare Disease. Neuron 93, 737–746, https://doi.org/10.1016/j.neuron.2017.01.018 (2017).
Biegstraaten, M., van Schaik, I. N., Aerts, J. M. & Hollak, C. E. ‘Non-neuronopathic’ Gaucher disease reconsidered. Prevalence of neurological manifestations in a Dutch cohort of type I Gaucher disease patients and a systematic review of the literature. J Inherit Metab Dis 31, 337–349, https://doi.org/10.1007/s10545-008-0832-y (2008).
Cherin, P. et al. The neurological manifestations of Gaucher disease type 1: the French Observatoire on Gaucher disease (FROG). J Inherit Metab Dis 33, 331–338, https://doi.org/10.1007/s10545-010-9095-5 (2010).
Biegstraaten, M. et al. Peripheral neuropathy in adult type 1 Gaucher disease: a 2-year prospective observational study. Brain 133, 2909–2919, https://doi.org/10.1093/brain/awq198 (2010).
Saperstein, D. S. et al. Challenges in the identification of cobalamin-deficiency polyneuropathy. Arch Neurol 60, 1296–1301, https://doi.org/10.1001/archneur.60.9.1296 (2003).
Coelho, D. et al. Mutations in ABCD4 cause a new inborn error of vitamin B12 metabolism. Nat Genet 44, 1152–1155, https://doi.org/10.1038/ng.2386 (2012).
Zhao, H., Brunk, U. T. & Garner, B. Age-related lysosomal dysfunction: an unrecognized roadblock for cobalamin trafficking? Cell Mol Life Sci 68, 3963–3969, https://doi.org/10.1007/s00018-011-0861-9 (2011).
Hannibal, L. et al. Biomarkers and Algorithms for the Diagnosis of Vitamin B12 Deficiency. Front Mol Biosci 3, 27, https://doi.org/10.3389/fmolb.2016.00027 (2016).
Hannibal, L. et al. Hampered Vitamin B12 Metabolism in Gaucher Disease? Journal of Inborn Errors of Metabolism and Screening 5, 1–7, https://doi.org/10.1177/2326409817692359 (2017).
Danielsson, A. Alkoholberoende ett föränderligt tillstående av varierande grad. Läkartidningen 115, 115:E117ER (2018).
Singleton, J. R. et al. The Utah Early Neuropathy Scale: a sensitive clinical scale for early sensory predominant neuropathy. J Peripher Nerv Syst 13, 218–227, https://doi.org/10.1111/j.1529-8027.2008.00180.x (2008).
Davies, E. H. et al. Four-year follow-up of chronic neuronopathic Gaucher disease in Europeans using a modified severity scoring tool. J Inherit Metab Dis 34, 1053–1059, https://doi.org/10.1007/s10545-011-9347-z (2011).
Rajabally, Y. A. & Martey, J. Neuropathy in Parkinson disease: prevalence and determinants. Neurology 77, 1947–1950, https://doi.org/10.1212/WNL.0b013e31823a0ee4 (2011).
Andreasson, M., Brodin, L., Laffita-Mesa, J. M. & Svenningsson, P. Correlations Between Methionine Cycle Metabolism, COMT Genotype, and Polyneuropathy in L-Dopa Treated Parkinson’s Disease: A Preliminary Cross-Sectional Study. J Parkinsons Dis 7, 619–628, https://doi.org/10.3233/JPD-171127 (2017).
Devigili, G. et al. Chronic pain in Gaucher disease: skeletal or neuropathic origin? Orphanet J Rare Dis 12, 148, https://doi.org/10.1186/s13023-017-0700-7 (2017).
Dreborg, S., Erikson, A. & Hagberg, B. Gaucher disease–Norrbottnian type. I. General clinical description. Eur J Pediatr 133, 107–118 (1980).
Ran, C. et al. Strong association between glucocerebrosidase mutations and Parkinson’s disease in Sweden. Neurobiol Aging 45, 212 e215–212 e211, https://doi.org/10.1016/j.neurobiolaging.2016.04.022 (2016).
Duran, R. et al. The glucocerobrosidase E326K variant predisposes to Parkinson’s disease, but does not cause Gaucher’s disease. Mov Disord 28, 232–236, https://doi.org/10.1002/mds.25248 (2013).
Cox, T. M. & Schofield, J. P. Gaucher’s disease: clinical features and natural history. Baillieres Clin Haematol 10, 657–689 (1997).
Finn, L. S., Zhang, M., Chen, S. H. & Scott, C. R. Severe type II Gaucher disease with ichthyosis, arthrogryposis and neuronal apoptosis: molecular and pathological analyses. Am J Med Genet 91, 222–226 (2000).
Acknowledgements
The authors are grateful to the patients who participated in the study. The study was funded by the collaboration agreement between Karolinska Institutet and Stockholm County Council (ALF). Per Svenningsson is a Wallenberg Clinical Scholar. Open access funding provided by Karolinska Institute.
Author information
Authors and Affiliations
Contributions
Study concept and design: M.A. and P.S. Acquisition of data: M.A., P.S., C.K.B. and M.M. Analysis and interpretation of data: M.A., P.S., C.K.B. and M.M. Analysis and interpretation of neurophysiological data: G.S. Drafting the manuscript: M.A. Revision of the manuscript: M.A., P.S. and G.S.
Corresponding author
Ethics declarations
Competing interests
M.M., P.S. and C.K.B. have received honoraria for lecturing on Gaucher disease from Sanofi-Genzyme and Shire/Takeda. M.A. and P.S. are investigators in the MOVES-PD study sponsored by Sanofi-Genzyme. The other authors declare that they have no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Andréasson, M., Solders, G., Björkvall, C.K. et al. Polyneuropathy in Gaucher disease type 1 and 3 – a descriptive case series. Sci Rep 9, 15358 (2019). https://doi.org/10.1038/s41598-019-51976-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-51976-2
This article is cited by
-
Usefulness of the skin-wrinkling test in a patient with probable small fiber neuropathy and Gaucher disease
The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2023)
-
Clioquinol kills astrocyte-derived KT-5 cells by the impairment of the autophagy–lysosome pathway
Archives of Toxicology (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.