Abstract
Zika virus (ZIKV) has emerged as one of the most medically relevant viral infections of the past decades; the devastating effects of this virus over the developing brain are a major matter of concern during pregnancy. Although the connection with congenital malformations are well documented, the mechanisms by which ZIKV reach the central nervous system (CNS) and the causes of impaired cortical growth in affected fetuses need to be better addressed. We performed a non-invasive, metabolomics-based screening of saliva from infants with congenital Zika syndrome (CZS), born from mothers that were infected with ZIKV during pregnancy. We were able to identify three biomarkers that suggest that this population suffered from an important inflammatory process; with the detection of mediators associated with glial activation, we propose that microcephaly is a product of immune response to the virus, as well as excitotoxicity mechanisms, which remain ongoing even after birth.
Similar content being viewed by others
Introduction
With the recent outbreak of ZIKV infection in Brazil in 2015 and 2016, followed by the intimate association between this infection and the increase in microcephaly, well-documented by case reports, public health authorities throughout the country assumed a state of alert that impacted the worldwide health community1,2. The neurotropism of ZIKV in adults and children has been studied in the last years, and viral pathogenesis is known to lead to autoimmune aggravations such as the Guillain-Barré syndrome3,4. Effects on infected pregnant women are even more devastating, as ZIKV is able to cross the placental and blood-brain barriers, causing disruptions in the developing brain of the fetus, impairing the growth of neural progenitor cells (NPCs), which ultimately lead to brain damage5,6,7. Furthermore, the role of ZIKV as a teratogen is strongly implicated from an epidemiological point of view, and the phenotypic spectrum of CZS has been accurately described and outlined by neuroimaging techniques8,9.
Studies detailing the pathophysiological effects and the cell machinery involved in ZIKV infection and proliferation are providing clearer information on the viral replication cycle, as research advances towards effective screening methods for viral detection in human fluids10. The mechanisms leading to neural underdevelopment in human NPCs, nonetheless, remain little known11. Recent literature reports rely on the hypothesis that ZIKV promotes impaired NPCs growth, with associated apoptotic events, exerting similar effects over the systems of both newborns and adults12. The idea of interfering in the replication of cells with high metabolic rate has even elicited a whole new line of studies where ZIKV was used in an oncolytic-like strategy to treat aggressive gliomas, with results showing important cytopathic effects of the virus over the tumors13,14.
The mechanisms by which flaviviruses migrate to the CNS, i.e. neurotropism, are still unresolved. Current literature describes three possible migration pathways: (i) through peripheral nerves after the mosquito bite, a mechanism that involves retrograde transportation through axons; (ii) through the bloodstream, crossing the blood-brain barrier (BBB) with altered permeability resulting from the presence of pro-inflammatory species; and (iii) carried by immune cells, a mechanism also known as ‘Trojan horse’ neuroinvasion15,16,17,18. Given this particular migratory behavior, and the trend to investigate the traces and effects of ZIKV infection using noninvasive biofluids, we hereby report the identification of three inflammatory mediators that were detected in the saliva of microcephalic infants after birth, all them from mothers that were diagnosed with Zika infection during pregnancy. Suggesting that CZS subjects overexpress inflammatory biomarkers in saliva is consistent with a status of ongoing neurological inflammation, and may be supported by the anatomical relationship of salivary glands and developing nerves, such as the trigeminal nerve19. Furthermore, our findings also support the utility of saliva sampling to monitor the status of this disease, corroborating the utility of this biofluid as a non-invasive approach for biomarker screening purposes, as recently demonstrated by Huan et. al in a contribution with Alzheimer’s Disease20.
Our hypothesis, therefore, is that the pathways associated with the biomarkers described are reflective of the anti-ZIKV infection cellular immune response, and that they may be involved with the neural damage that leads to microcephaly.
Metabolomics to Unravel Microcephaly-Related Biomarkers
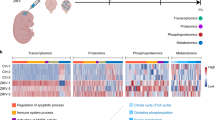
A statistical model using orthogonal partial least squares discriminant analysis (OPLS-DA) was applied to a high-resolution mass spectrometric dataset from saliva samples, assessing the differences between the metabolomic profile of two distinct groups of infants (n = 27 each): babies diagnosed with CZS upon birth, and healthy subjects with no clinical diagnosis of CZS. From the scores plot in Fig. 1, it is possible to visually assess the difference between groups in both ion modes, where control subjects and microcephalic patients cluster clearly differently in both positive and negative ion modes. Particularities of each group were addressed by a list of significant features generated by the variable importance in projection (VIP) scores from OPLS-DA, which provided a collection of 28 ions that are specific for the congenital microcephaly group. Out of the 28 features selected by OPLS-DA, we were able to identify three compound classes that make sense within the biochemical context of compromised neural development upon ZIKV infection.
OPLS-DA score plots indicating clear separation between the group of infants with congenital zika syndrome (green) and the control group (red). The statistical model was able to distinguish the high-resolution mass spectrometry-generated datasets from both the positive (A) and negative (B) ion modes, in a strong indication that the chemical composition of the two groups is different.
Inflammation as an Important Player in Impaired Neural Growth
Neuroinflammation has been proposed as one of the key factors that contribute to ZIKV-related microcephaly21, especially inflammatory processes mediated by glial cells. The series of molecules described in Table 1 compose a list of inflammatory mediators that participate directly in mechanisms associated with immune response, excitotoxicity, as well as physiological responses to minimize further damage to neural tissue. Their correlation with neuroinflammation is suggested by a series of seven elected isomeric prostaglandin analogues derived from PGD2, PGE1, PGE2, and PGI2. The role of these species and their derivatives in protecting the CNS is widely discussed in the literature, and it is known that they reflect an anti-inflammatory response to neuronal injuries22, contributing to neuroprotection in the CNS in the context of excitotoxicity23, which is a known contributor to acute brain injury24. Recently, Olmo, et al.25 described the increase in cytokines TNF-α and IL-1β, and glutamate in vitro, after infecting neuronal cells with ZIKV, demonstrating excitotoxicity induction as an important mechanism for the neurotoxic effects observed. Additionally, multiplex analyte-specific beads assays in serum samples have demonstrated that the production of immune mediators can modulate the clinical outcome after ZIKV infection, since the levels of IL-22, MCP-1, IP-10, and TNF-α are usually higher in patients with severe disease and neurological impairment26. Thus, our findings indicate that these mechanisms may be active in CZS, as the identified collection of prostaglandin metabolites are putatively overexpressed in response to the infection.
The abovementioned activation of the prostaglandin pathway due to excitotoxicity is reinforced by the identification of 15-deoxy-Δ-12,14-Prostaglandin J2 (15d-PGJ2) as a marker for the CZS group. This molecule is a non-enzymatic, end-metabolite of the PGD2 pathway, closely linked with microglial activation and neural tissue depletion, as observed in Fig. 2. Furthermore, 15d-PGJ2 is the natural agonist of the peroxisome proliferator-activated receptor-γ (PPAR-γ), a nuclear receptor that controls the activation of peroxisomes and, further downstream, negatively regulates microglial function27. The identification of 15d-PGJ2 as a biomarker for CZS is consistent with enhanced PGD2 metabolism, providing a neuroprotective response to reduce cytokine-driven excitotoxicity, as previously reported by Liang et al.23. The non-enzymatic metabolism of PGD2 intermediaries lead to an accumulation of 15d-PGJ2, which we propose directly activates PPAR-γ, driving changes of gene expression and eliciting the downregulation of microglial activation in spite of the proinflammatory environment associated with the driving of neural damage28.
A conception of metabolic pathways that are putatively activated in response to ZIKV pathogenesis, as suggested by the markers from OPLS-DA (in red). Arachidonic acid (AA) is the main precursor activated in this mechanism, with two main cascades unfolding upon activation: prostaglandin metabolism (and its derivatives), and hepoxilin metabolism. All highlighted mediators are linked with response to neural damage and show the organism attempting to attenuate nervous system deterioration. AA: arachidonic acid; 12(S)-HPETE: 12-hydroperoxyicosatetraenoic acid; 12- HPTEH: HxA3 and HxB3: hepoxilin A3 and B3; PTGS1: prostaglandin-endoperoxide synthase 1 (COX-1); PGG2: prostaglandin G2; PGH2: prostaglandin H2; PTGDS: prostaglandin-H2 D-isomerase; PGD2: prostaglandin D2; PGJ2: prostaglandin J2; Δ12-PGJ2: delta-12-prostaglandin J2.
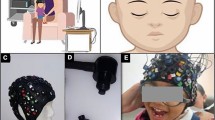
Among the biomarkers characterized in this study, we identified a particular class of endogenous metabolites of the lipoxygenase system, hepoxilins, namely two isomers: hepoxilins A3 and B3 (HxA3 and B3). These species have been described in the literature as signaling molecules associated with post-injury axonal repair mechanisms29, promotion of neurite regeneration30, as well as inducers of neutrophil extracellular traps (NETs)31. As ZIKV is able to trigger innate immune response in different cells types, such as dendritic cells, monocytes, and lymphocytes32, we decided to test whether ZIKV infection might induce NETs formation in human neutrophils in vitro. For this, we monitored the presence and concentration of extracellular DNA in human neutrophils after four treatments: a positive control (PMA), when NETs were induced by phorbol myristate acetate, a negative control (NCtrl), and when cells were infected with wild-type ZIKV or inactivated ZIKV by ultraviolet for 30 minutes (UV-ZIKV). As demonstrated in Fig. 3, extracellular DNA is not significantly increased in ZIKV-infected neutrophils after 6 hours post-infection. Thus, we hypothesize that hepoxilins are specifically acting as anti-inflammatory mediators in the aftermath of neural depletion, attempting to minimize the overall damage (Fig. 2). Furthermore, there is clinical evidence that ZIKV remains in the CNS even after birth, as Chimelli, et al.33 reported a case of ZIKV persistence after birth in an infant with CZS, evidenced by viral RNA presence in the urine at birth, and in the brain in postmortem tissue analyses. The findings from Arruza, et al.34 also provide support to the idea that neural damage provokes an integrated response, i.e. the effects and metabolites associated with inflammation may be present even in tissues that are distant from the actual threat. All these evidences are complementary, and consistent, therefore, with a condition of persistent neuroinflammation, in which hepoxilins and other prostaglandin derivatives are trying to counterbalance the action with anti-inflammatory processes.
Extracellular DNA quantification from ZIKV-infected human neutrophils. (A–C) Human neutrophils (1 × 105/300 μL) were stimulated with PMA (100 nM) or infected with ZIKV (MOI 2) for 6 hours in 8-chamber culture. Cells were stained for DNA with Hoechst 33342. Scale bars = 100 μm, Magnification = 20×. (D,E) Neutrophils (2 × 106/mL) were stimulated with ZIKV, UV-ZIKV or PMA or left unstimulated for 6 hours. Extracellular DNA (μg/mL) was quantified in culture supernatants and fold number of concentrations was evaluated using the negative control (NCrl) as reference. Data are representative of 2 independent experiments performed in triplicates and represent mean ± SD. Data were analyzed with Kruskal-Wallis test. *p < 0.05, **p < 0.01.
Our contention is that the broad spectrum of symptoms associated with congenital Zika syndrome affecting infants born to mothers infected with ZIKV are the result of viral induced microglial activation and excitotoxicity. The presence of the anti-inflammatory biomarkers in the saliva, even for longer periods after birth, indicate that the immune system remains active for an indefinite period. Therefore, in addition to the monitoring of cognitive development, which is the main focus of current public health policies for infants born with CZS, inflammation status and its relationship with the persistence of ZIKV after birth should also be investigated. Thus short- and long-term outcomes associated with ZIKV syndrome should be investigated using selected cohorts of CZS patients, especially at the molecular level, with care taken to control for other congenital infections which may additionally affect CNS development and/or elicit inflammatory responses. Finally, saliva emerges as a viable, non-invasive alternative to assess neural diseases, which is coherent due to the interactions between salivary glands and developing nerves; the use of this biofluid in prospective metabolomics studies is a current trend, and is being further explored in studies related to conditions that affect the nervous system35.
Methods
Metabolomics of saliva
Patient selection
Twenty-seven infants diagnosed with CZS according to an outlined phenotypic spectrum by neuroimaging36 were selected to participate in this study, which is approved by the Brazilian Research Ethics Committee under the number 61936216.9.0000.5404. The counterpart was a control group, composed of healthy individuals – 27 infants with no clinical signs and symptoms, nor neuroimaging diagnosis of CZS. Gender was not matched between groups, and the age limit for any group was 2 years of age; the choice to not homogenize groups was so that we would be able to assess the specificity of the proposed model in identifying disease-related molecules of interest. All experiments were performed in accordance with the guidelines provided by the Declaration of Helsinki. Since all individuals were under the age of 18 years, the written informed consent was obtained from their parents and/or legal guardians for sample collection and use within the scope of this research.
Sample collection and high-resolution mass spectrometry
Saliva samples were collected using the Oragene® DNA Self-Collection Kit (DNA Genotek Inc., Ontario, Canada) as per the manufacturer’s instructions. Samples were maintained frozen under −80 °C until analysis. 10 microliters of saliva were diluted in a methanol/water solution (1:1) to a final volume of 1 mL. The solution was homogenized under vortex, filtered through a PVDF membrane (0.22 µm); formic acid or ammonium hydroxide were added to a concentration of 0.1% to assist positive and negative ion formation, respectively. Final solutions were sent for analysis by high resolution mass spectrometry (ESI-LTQ-XL Orbitrap Discovery, Thermo Scientific, Bremen, Germany) both in positive and negative ion modes, in the mass range of 100–1000 m/z. Markers for the CZS group were determined with the assistance of online metabolomics platform METLIN (http://metlin.scripps.edu).
Statistical analysis
Spectrometric data were submitted to multivariate statistical analysis using Orthogonal Partial Least Squares Discriminant Analysis (OPLS-DA) in the online metabolomics-processing platform MetaboAnalyst37. Data were normalized with reference to the CZS group, with range scaling. Most relevant features elected by the variable importance in projection (VIP) scores were selected. One-hundred cross-validations (CV) were performed, and prediction accuracy during training was calculated using 1000 permutations for data from both ion modes (p = 0.001, data not shown) to assess significance and validate the proposed statistical model.
Assessment of NETs in vitro after neutrophil induction by ZIKV
Reagents
MEM (Minimum Essential Medium) and Dextran from Leuconostoc spp. were purchased from Sigma-Aldrich (St. Louis, MO). Qubit dsDNA HS assay kit was from Invitrogen (Carlsbad, CA). Ficoll-Paque PLUS was from GE Healthcare (Chicago, IL).
Human neutrophil isolation
Whole blood (20 mL) was collected from healthy volunteer donor into heparin-treated tubes. Neutrophils were purified by density gradient centrifugation using Ficoll-Paque PLUS (GE Healthcare, Chicago, IL)38. Erythrocytes were removed by dextran sedimentation followed by two rounds of hypotonic lysis. Purified neutrophils were re-suspended in MEM medium (Sigma-Aldrich, St. Louis, MO).
Stimulation of neutrophils and quantification of extracellular DNA
Neutrophils (2 × 106 cells/mL) were stimulated with PMA (100 nM), ZIKV or UV-inactivated ZIKV at an MOI of 2 for 6 hours at 37 °C under 5% CO2. After the stimulation period, culture supernatant was collected, and extracellular DNA was precipitated using 3 M sodium acetate and ethanol; the obtained pellet was then washed with 70% ethanol and resuspended in nuclease-free water. Isolated DNA samples were measured using either Quant-iT dsDNA or Qubit dsDNA HS kits (Invitrogen, Carlsbad, CA), following manufacturer’s instructions. The ZIKV strain was obtained and maintained according to the procedures by Melo et al.39.
Immunofluorescence
Neutrophils (1 × 105/300 μL) were seeded in 8-chamber culture slides and incubated with PMA (100 nM) or ZIKV (MOI 2) for 6 hours at 37 °C under 5% CO2. Cells fixed with 4% paraformaldehyde (PFA) and were stained with Hoechst 33342 (1:1000). Images were taken using 20x magnification in Cytation 5 (BioTek, Vermont).
Statistical analyses
Data were presented as mean ± SD. The results obtained were analyzed using GraphPad Prism (version 6.0, GraphPad Software, Inc., San Diego, CA) statistical software package. Comparisons between multiple groups were analyzed using nonparametric test with a posteriori Kruskal-Wallis test. The level of significance was set at p ≤ 0.05.
References
Tetro, J. A. Zika and microcephaly: causation, correlation, or coincidence? Microbes and Infection 18, 167–168, https://doi.org/10.1016/j.micinf.2015.12.010 (2016).
Mlakar, J. et al. Zika virus associated with microcephaly. N Engl J Med 2016, 951–958 (2016).
Lucchese, G. & Kanduc, D. Zika virus and autoimmunity: From microcephaly to Guillain-Barre syndrome, and beyond. Autoimmunity reviews 15, 801–808 (2016).
Brasil, P. et al. Guillain-Barré syndrome associated with Zika virus infection. The lancet 387, 1482 (2016).
Tang, H. et al. Zika Virus Infects Human Cortical Neural Progenitors and Attenuates Their Growth. Cell Stem Cell 18, 587–590, https://doi.org/10.1016/j.stem.2016.02.016 (2016).
Dang, J. et al. Zika Virus Depletes Neural Progenitors in Human Cerebral Organoids through Activation of the Innate Immune Receptor TLR3. Cell Stem Cell 19, 258–265, https://doi.org/10.1016/j.stem.2016.04.014 (2016).
Li, C. et al. Zika Virus Disrupts Neural Progenitor Development and Leads to Microcephaly in Mice. Cell Stem Cell 19, 120–126, https://doi.org/10.1016/j.stem.2016.04.017 (2016).
del Campo, M. et al. The phenotypic spectrum of congenital Zika syndrome. American Journal of Medical Genetics Part A 173, 841–857, https://doi.org/10.1002/ajmg.a.38170 (2017).
Schuler-Faccini, L. Possible association between Zika virus infection and microcephaly—Brazil, 2015. MMWR. Morbidity and mortality weekly report 65 (2016).
Melo, C. F. O. R. et al. Serum Metabolic Alterations upon Zika Infection. Frontiers in Microbiology 8, https://doi.org/10.3389/fmicb.2017.01954 (2017).
Faizan, M. I. et al. Zika virus-induced microcephaly and its possible molecular mechanism. Intervirology 59, 152–158 (2016).
Li, H., Saucedo-Cuevas, L., Shresta, S. & Gleeson, J. G. The Neurobiology of Zika Virus. Neuron 92, 949–958, https://doi.org/10.1016/j.neuron.2016.11.031 (2016).
Zhu, Z. et al. Zika virus has oncolytic activity against glioblastoma stem cells. Journal of Experimental Medicine 214, 2843–2857 (2017).
de O. Lima, E. et al. MALDI-Imaging detects endogenous Digoxin in glioblastoma cells infected by Zika virus – would it be the oncolytic key? Journal of Mass Spectrometry In press, n/a-n/a, https://doi.org/10.1002/jms.4058 (2017).
Neal, J. W. Flaviviruses are neurotropic, but how do they invade the CNS? Journal of Infection 69, 203–215, https://doi.org/10.1016/j.jinf.2014.05.010 (2014).
Perera-Lecoin, M., Meertens, L., Carnec, X. & Amara, A. Flavivirus entry receptors: an update. Viruses 6, 69–88 (2013).
Velandia, M. L. & Castellanos, J. E. In Viral Genomes - Molecular Structure, Diversity, Gene Expression Mechanisms and Host-Virus Interactions (ed Maria Garcia) Ch. 11, (InTech Open, 2012).
Suen, W., Prow, N., Hall, R. & Bielefeldt-Ohmann, H. Mechanism of West Nile Virus Neuroinvasion: A Critical Appraisal. Viruses 6, 2796 (2014).
Ferreira, J. N. & Hoffman, M. P. Interactions between developing nerves and salivary glands. Organogenesis 9, 199–205 (2013).
Huan, T. et al. Metabolomics Analyses of Saliva Detect Novel Biomarkers of Alzheimer’s Disease. Journal of Alzheimer’s Disease, 1–16 (2018).
Wen, Z., Song, H. & Ming, G.-l How does Zika virus cause microcephaly? Genes & development 31, 849–861 (2017).
Shi, J. et al. The Prostaglandin E2 E-Prostanoid 4 Receptor Exerts Anti-Inflammatory Effects in Brain Innate Immunity. The Journal of Immunology 184, 7207–7218, https://doi.org/10.4049/jimmunol.0903487 (2010).
Liang, X., Wu, L., Hand, T. & Andreasson, K. Prostaglandin D2 mediates neuronal protection via the DP1 receptor. Journal of Neurochemistry 92, 477–486, https://doi.org/10.1111/j.1471-4159.2004.02870.x (2005).
An, Y. et al. Prostacyclin mediates endothelial COX-2-dependent neuroprotective effects during excitotoxic brain injury. Journal of Inflammation Research 7, 57–67, https://doi.org/10.2147/JIR.S63205 (2014).
Olmo, I. G. et al. Zika Virus Promotes Neuronal Cell Death in a Non-Cell Autonomous Manner by Triggering the Release of Neurotoxic Factors. Frontiers in Immunology 8, https://doi.org/10.3389/fimmu.2017.01016 (2017).
Kam, Y.-W. et al. Specific Biomarkers Associated With Neurological Complications and Congenital Central Nervous System Abnormalities From Zika Virus–Infected Patients in Brazil. The Journal of Infectious Diseases 216, 172–181, https://doi.org/10.1093/infdis/jix261 (2017).
Bernardo, A., Levi, G. & Minghetti, L. Role of the peroxisome proliferator‐activated receptor‐γ (PPAR‐γ) and its natural ligand 15‐deoxy‐Δ12, 14‐prostaglandin J2 in the regulation of microglial functions. European Journal of Neuroscience 12, 2215–2223 (2000).
Bernardo, A. & Minghetti, L. PPAR-γ Agonists as Regulators of Microglial Activation and Brain Inflammation. Current Pharmaceutical Design 12, 93–109, https://doi.org/10.2174/138161206780574579 (2006).
Camara-Lemarroy, C. R., Gonzalez-Moreno, E. I., Guzman-de la Garza, F. J. & Fernandez-Garza, N. E. Arachidonic acid derivatives and their role in peripheral nerve degeneration and regeneration. The Scientific World Journal 2012 (2012).
Amer, R. K., Pace-Asciak, C. R. & Mills, L. R. A lipoxygenase product, hepoxilin A3, enhances nerve growth factor-dependent neurite regeneration post-axotomy in rat superior cervical ganglion neurons in vitro. Neuroscience 116, 935–946, https://doi.org/10.1016/S0306-4522(02)00764-9 (2003).
Douda, D. N., Grasemann, H., Pace-Asciak, C. & Palaniyar, N. A Lipid Mediator Hepoxilin A3 Is a Natural Inducer of Neutrophil Extracellular Traps in Human Neutrophils. Mediators of Inflammation 2015, 7, https://doi.org/10.1155/2015/520871 (2015).
O’Connor, M. A. et al. Early cellular innate immune responses drive Zika viral persistence and tissue tropism in pigtail macaques. Nature Communications 9, 3371, https://doi.org/10.1038/s41467-018-05826-w (2018).
Chimelli, L. et al. Persistence of Zika Virus After Birth: Clinical, Virological, Neuroimaging, and Neuropathological Documentation in a 5-Month Infant With Congenital Zika Syndrome. Journal of Neuropathology & Experimental Neurology 77, 193–198, https://doi.org/10.1093/jnen/nlx116 (2018).
Arruza, L. et al. Hypoxic–ischemic brain damage induces distant inflammatory lung injury in newborn piglets. Pediatric Research 79, 401, https://doi.org/10.1038/pr.2015.87 (2015).
Sapkota, S. et al. Alzheimer’s Biomarkers From Multiple Modalities Selectively Discriminate Clinical Status: Relative Importance of Salivary Metabolomics Panels, Genetic, Lifestyle, Cognitive, Functional Health and Demographic Risk Markers. Frontiers in Aging Neuroscience 10, https://doi.org/10.3389/fnagi.2018.00296 (2018).
Saúde, M. D. Vol. 1 (ed Secretaria de Atenção à Saúde) 46 (Ministério da Saúde, Brasília, 2016).
Xia, J., Sinelnikov, I. V., Han, B. & Wishart, D. S. MetaboAnalyst 3.0—making metabolomics more meaningful. Nucleic acids research 43, W251–W257 (2015).
Muraro, S. P. et al. Respiratory Syncytial Virus induces the classical ROS-dependent NETosis through PAD-4 and necroptosis pathways activation. Scientific Reports 8, 14166, https://doi.org/10.1038/s41598-018-32576-y (2018).
Melo, C. F. O. R. et al. A Lipidomics Approach in the Characterization of Zika-Infected Mosquito Cells: Potential Targets for Breaking the Transmission Cycle. Plos One 11, e0164377, https://doi.org/10.1371/journal.pone.0164377 (2016).
Acknowledgements
DNO would like to thank the Brazilian Ministry of Health (Plano Nacional de Enfrentamento ao Aedes aegypti e à Microcefalia [Brazilian Plan for Fighting Aedes aegypti and Microcephaly]) for the fellowship under process No. 88887.137889/2017-00 and PNPD No. 88882.305824/2013-01. DPC, JLPM and RRC thank CAPES/MEC, CNPq/MCTI and Decit/SCTIE/MS/FNDCT for grant No. 14/2016. Our group thanks the Coordination for the Improvement of Higher Level Personnel (CAPES) for the fellowships from EOL (PNPD: 1578388) and TMG (PROEX: 1489740). Finally, we acknowledge the São Paulo Research Foundation (FAPESP, Process Nos. 11/50400-0 and 18/14657-5 for RRC, and 16/17066-2 and 18/03321-6 for CFORM), as well as the financial support provided by the OCRC (Obesity Comorbidities Research Center) CEPID: CMPO - Centro Multidisciplinar de Pesquisa em Obesidade e Doenças Associadas, under FAPESP number 13/07607-8.
Author information
Authors and Affiliations
Contributions
D.N.O. idealized and performed experiments, analyzed data and wrote the manuscript. E.O.L., C.F.O.R.M., J.D. and T.M.G. analyzed data and revised the manuscript. R.G.M.R. and K.N.M. performed experiments and data collection. C.S. and G.P.M. performed sample collection and preparation and revised the manuscript. A.S., R.F.B., M.J.R.D. and P.S.S. performed patient selection and diagnosis, as well as pregnant mother’s monitoring. S.P.M., G.F.S. and A.V. performed human neutrophil isolation, infection, and extracellular DNA quantification for NETs. D.P.C., J.L.P.M. and R.R.C. coordinated the team, revised the manuscript and idealized all experiments.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
de Oliveira, D.N., Lima, E.O., Melo, C.F.O.R. et al. Inflammation markers in the saliva of infants born from Zika-infected mothers: exploring potential mechanisms of microcephaly during fetal development. Sci Rep 9, 13606 (2019). https://doi.org/10.1038/s41598-019-49796-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-49796-5
This article is cited by
-
Zika-exposed microcephalic neonates exhibit higher degree of inflammatory imbalance in cerebrospinal fluid
Scientific Reports (2021)
-
Minimally Invasive Biospecimen Collection for Exposome Research in Children’s Health
Current Environmental Health Reports (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.