Abstract
In natural cycle or minimal stimulation cycle IVF, buserelin acetate (buserelin), a gonadotropin-releasing hormone agonist, is often used as a maturation trigger; however, its effect on pregnancy outcomes remains unclear. Therefore, in the present study, we compared uterine receptivity in buserelin-administered mice with that in human chorionic gonadotropin (hCG)-administered mice during the peri-implantation period. Implantation, decidualisation, and term-pregnancy were impaired following hCG, but not buserelin administration. hCG stimulated the synthesis and secretion of progesterone and oestradiol, whereas ovarian steroidogenesis in the buserelin-treated group was comparable with that in the control group. Furthermore, similar to the observation in controls, the buserelin-treated group exhibited activation of progesterone receptor signalling and inhibition of oestrogen receptor signalling in the endometrial epithelium on the day of implantation. However, epithelial progesterone signalling was not detected, and a high expression of genes downstream to oestrogen was observed on day 4 following hCG administration. These results suggest that buserelin administration does not impact uterine receptivity as it did not affect ovarian steroidogenesis and endometrial steroid signalling. Therefore, buserelin is preferred as an oocyte maturation trigger to optimise uterine receptivity during treatments involving timed intercourse, intrauterine insemination, or fresh embryo transfer following in vitro fertilisation.
Similar content being viewed by others
Introduction
During the 1990s, gonadotropin releasing hormone (GnRH) agonists were introduced as an alternative to human chorionic gonadotropin (hCG) for inducing oocyte maturation1,2,3,4. Historically, hCG administration had been the primary method to induce oocyte maturation in fertility treatments, including timed intercourse, intrauterine insemination, and in vitro fertilisation (IVF). When administered in cycles coinciding with multiple follicular development, hCG triggers the formation of multiple corpora lutea while stimulating luteal function and generating supraphysiological oestradiol and progesterone levels5. In contrast to hCG, which induces an increase in only luteinising hormone (LH)-like activity, GnRH agonists activate GnRH receptors in the pituitary, inducing surges in both LH and follicle stimulating hormone (FSH)3,6,7. These surges promote nuclear maturation and corpus luteum formation6,8,9, similar to the natural cycle2,7. In addition, GnRH agonists have lower carbohydrate content than hCG, resulting in a shorter circulating half-life and reduced duration of LH receptor activity10,11,12,13. These characteristics lower the risk of ovarian hyperstimulation syndrome (OHSS)14,15,16,17,18. Furthermore, hCG exerts negative effects on endometrial receptivity19,20,21,22 and embryo quality23.
These disadvantages of hCG treatment are a major reason for the interest in GnRH agonists. Of these, buserelin appears to generate significantly more mature oocytes than hCG following ovulation induction5. However, buserelin also significantly lowers implantation and clinical pregnancy rates, while increasing early pregnancy loss. These negative outcomes are not universal as a previous study failed to find adverse effects on implantation or pregnancy after oocyte maturation was induced24. Unfortunately, few studies have compared pregnancy outcomes after hCG or GnRH-agonist administration, causing difficulties in determining which treatment is effective while minimising side effects. Thus, in the present study, we examined the effects of buserelin administration on implantation, decidualisation, and term pregnancy in mice. We also assessed effects on ovarian steroidogenesis and endometrial steroid signalling, as both processes are crucial for uterine receptivity.
Results
Buserelin did not impair implantation, decidualisation, and term pregnancy
To evaluate the uterine receptivity after administration of hCG or buserelin, blastocyst stage embryos were transferred to pseudo-pregnant mice that were primed with either hCG or buserelin, and analysis of blastocyst implantation on day 5 was performed. In the saline injected (control) group, we observed implantation sites (average number: 6.3 ± 0.4) in 83.9% of female mice after embryo transfer (Fig. 1A,B). We also observed a dose-dependent reduction in the number of mice with implantation sites (5 IU: 41.9%, 10 IU: 27.3%) and in the number of implanted blastocysts (3.5 ± 1.0, 2.9 ± 1.2; respectively) in hCG-treated groups. However, buserelin groups did not differ from control in terms of the percentage of mice with implantation sites (360 ng: 81.3%, 720 ng: 81.8%) and the number of implantation sites (6.8 ± 0.2, 6.9 ± 0.4, respectively).
Embryo implantation and formation of decidual tissue after hCG or buserelin administration in mice. (A) Representative uteri on day 5 of pregnancy. Arrowheads indicate implantation sites. (B) Number of implantation sites on day 5 of pregnancy. Ten blastocysts were transferred to uteri on day 4 of pseudopregnancy, and the number of implantation sites was assessed on day 5. Values above bars indicate the amount of pregnant mice over total number of mice. (C) Decidualisation in hyper-stimulated mice after intrauterine oil infusion of uterine right horn (left horn was control). (D) Fold-increase in uterine weight. Decidualisation extent was calculated as fold-change in uterine weight of oil-infused horns divided by change in non-infused horns. Values above bars indicate number of mice with decidualisation over total number of mice. Error bars represent standard error of the mean. Bars labelled with distinct letters are significantly different from each other (P < 0.05).
To determine the decidualisation ability in endometrium post implantation period, artificial decidualisation was induced by oil infusion into the uterine horn of hCG or buserelin treated pseudo-pregnant mice. Regardless of dosage, endometrial decidualisation was compromised in hCG-treated groups (5 IU: 2.5 ± 0.7, 10 IU: 1.6 ± 0.2) compared with that in control (12.4 ± 1.5) (Fig. 1C,D). By contrast, fold increase in uterine weight was similar across control and buserelin-treated groups (360 ng: 11.2 ± 1.8, 720 ng: 10.4 ± 1.3).
Furthermore, the effect of hCG and buserelin administration on post-implantation development and term pregnancy was examined by embryo transfer. Compared with the control group, hCG-treated groups had significantly lower pregnancy rates after blastocyst transfer (5 IU: P = 0.0004, 10 IU: P < 0.0001, Table 1), whereas rates in buserelin-treated groups did not differ (360 ng: P = 0.2482, 720 ng: P = 0.1570). Pup number and weight were also considerably lower among hCG-treated mice than among the control. Buserelin treatment did not result in significantly fewer pups than control, although there was a tendency toward lower pup rate in the former group (360 ng: P = 0.0706, 720 ng: P = 0.0595). Together, these results indicate that hCG hampered implantation and decidualisation more so than did buserelin, leading to decreased pregnancy rates.
Buserelin did not alter progesterone/oestradiol synthesis and secretion
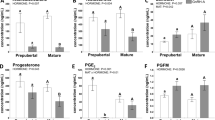
As a marker of progesterone synthesis, Hsd3b1 is responsible for transforming pregnenolone to progesterone. This gene was upregulated on day 3 in the control and buserelin-treated groups, but on day 1 in the hCG-treated groups (Fig. 2A). Cyp19a1 catalyses the conversion of testosterone to oestradiol; in the control group, its mRNA expression was high on day 1, then decreased on day 2 before increasing again on day 4 (Fig. 2B). Expression patterns were similar in the control and buserelin-treated groups, but higher on days 1–3 in hCG-treated groups.
Ovarian steroid-hormone synthesis and secretion during the pre-implantation period. (A) Hsd3b1 and (B) Cyp19a1 mRNA expression. Serum (C) progesterone and (D) oestradiol-17β levels. Error bars represent standard error of the mean. Bars labelled with distinct letters are significantly different from each other (P < 0.05).
Serum progesterone level increased starting from day 2 in the control and buserelin-groups (Fig. 2C). However, progesterone levels were already higher in the hCG-treated groups than in the control group on days 1–2, and levels were significantly lower than those in the control group on day 4. Control serum oestradiol decreased on day 2 before increasing again on day 4 (Fig. 2D). The hCG groups had notably higher oestradiol levels on days 1–3 before experiencing significant downregulation compared with those in the control on day 4. Buserelin-treated groups exhibited significantly higher oestradiol levels than control on day 1, but then did not differ from control on days 2–4. These results indicate that hCG dysregulated steroidogenic enzyme expression in ovaries through artificially inducing oocyte maturation. By contrast, buserelin administration did not affect the synthesis or secretion of ovarian steroid hormones during the pre-implantation period.
Buserelin does not adversely affect PR expression and downstream signalling
The expression of progesterone receptor (PR) and its downstream genes is associated with uterine receptivity in the endometrium during the pre-implantation period. In the control group, PR was detected in stromal cells from day 1 onward, as well as in the luminal epithelium on days 3 and 4 (Fig. 3A). Buserelin groups exhibited the same pattern. In contrast, hCG groups exhibited PR expression in stromal cells from day 1 onward, but not in the luminal epithelium. Thus, hCG, but not buserelin, altered the localisation of PR expression during pre-implantation, especially in luminal epithelium.
Endometrial PR signalling following oocyte maturation trigger. (A) Distribution of PR in endometrium during pre-implantation. Scale bars represent 100 μm. (B) Ihh, (C) Areg, and (D) Gata2 mRNA expression during pre-implantation. Error bars represent standard error of the mean. Bars labelled with distinct letters are significantly different from each other (P < 0.05).
The indian hedgehog (Ihh) acts downstream of epithelial PR25,26 and was expressed at low levels in all groups on days 1–3. Although Ihh expression notably increased on day 4 in the control and buserelin-treated groups, hCG groups exhibited lower Ihh expression than control (Fig. 3B). We further examined mRNA expression of amphiregulin (Areg)27,28 and GATA binding protein 2 (Gata2)29, two other genes downstream of epithelial PR. Both had substantially lower expression in the hCG-treated groups than in the control or buserelin-treated groups on day 4 (Fig. 3C,D). Therefore, hCG—but not buserelin—caused steroidogenic dysregulation that altered the expression of epithelial PR and its downstream genes.
Epithelial oestrogenic signalling was not adversely affected by buserelin administration
Immunohistochemistry detected oestrogen receptor (ER)α in the luminal epithelium of control mice on days 1–3, then tracked a substantial decrease on day 4 (Fig. 4A). Buserelin-treated groups exhibited similar ERα expression patterns throughout the pre-implantation period. However, some endometrium epithelial cells in the hCG-treated groups exhibited low ERα expression on days 1–4.
Endometrial ER signalling following oocyte maturation trigger. (A) Distribution of ERα in endometrium during pre-implantation. Scale bars represent 100 μm. (B) Muc1, (C) Ltf, and (D) Lif mRNA expression during pre-implantation. Error bars represent standard error of the mean. Bars labelled with distinct letters are significantly different from each other (P < 0.05).
Mucin 1 (Muc1) and lactotransferrin (Ltf) are both well-characterised genes that act downstream of epithelial ERα and are typically downregulated during the implantation period30,31,32. In the control and buserelin groups, Muc1 mRNA expression was detected on day 1, followed by a decrease in expression from day 2 onward (Fig. 4B). However, in hCG-treated groups, Muc1 mRNA expression was low on days 1–4. Immunohistochemical analysis showed that on day 4, MUC1 protein expression decreased on day 4 in all control and buserelin-treated mice, but only in 30.8% of hCG-treated mice (Supplemental Fig. 2A,B). High Ltf mRNA expression was also detected on day 1, but the level markedly decreased on days 2–4 in control and buserelin-treated groups, whereas it remained detectable on day 4 in the hCG-treated groups (Fig. 4C). Leukaemia inhibitory factor (Lif) is essential for uterine receptivity and implantation33,34. In control and buserelin groups, Lif mRNA expression was high on day 1, decreased on day 2, and increased again on day 4 (Fig. 4D). In hCG groups, however, Lif expression was low on day 4 (Fig. 4D).
Endometrial proliferation-differentiation switching was normally regulated after buserelin administration
Immunostaining revealed Ki67 expression in the luminal epithelium on day 1 for control and buserelin groups. Subsequently, the expression shifted to the stroma and increased on day 4 (Supplemental Fig. 2C,D). Similar to that in the control, the luminal epithelium in hCG-treated groups exhibited Ki67-positive cells on day 1. However, Ki67-positive cell localisation did not shift to the stroma and remained detectable in the luminal epithelium on day 4. These results suggest that buserelin, but not hCG, successfully inhibited estrogenic activity in the luminal epithelium during pre-implantation.
Discussion
This is the first report to compare the effects of hCG and buserelin-acetate-induced oocyte maturation on endometrial steroid signalling, a process crucial for uterine receptivity. We first determined that hCG administration substantially impaired blastocyst implantation in the endometrium, differentiation of endometrial stromal tissues to decidua, pregnancy rates, pup numbers, and pup weight in mice. Previous studies reported that ovarian stimulation using a combination of hCG and equine CG (eCG) reduced the number of embryos in the late stage of gestation that resulted in a lower number of full-term pups in rodent models. Furthermore, embryonic and foetal development was delayed after ovarian stimulation, and the formation of pinopodes was also affected35,36,37. These adverse effects have also been observed in mice treated with hCG alone, which had reduced number of pups due to failure in either implantation or early pregnancy21,38,39,40. Our results confirmed these previous findings that hCG administration impaired pregnancy outcomes after embryo transfer. Human chorionic gonadotropin acts in conjunction with LH through the hCG/LH receptor. However, LH has a far shorter circulating half-life (25–60 min)11,41 than hCG (24–37 h)12,42. Moreover, hCG remains detectable in serum and urine for 7–11 d after injection13. These differing biochemical characteristics of the two hormones suggest that hCG administration will affect the implantation window (4 d post-LH surge in mouse)43,44, but not buserelin administration.
Next, we examined the sustained effect of hCG and buserelin on ovarian steroidogenesis during the pre-implantation period. The secretion of FSH and LH from the pituitary regulates progesterone and oestrogen, both of which are essential for implantation initiation and optimal decidualisation44. In hCG-treated but not in buserelin-treated or control groups, we observed aberrant expression of Hsd3b1 and Cyp19a1, which are markers of progesterone and oestradiol production, respectively. Control and buserelin-treated groups also did not differ in progesterone and oestradiol secretion patterns, but hCG treatment disrupted their secretion. Therefore, hCG appears to exert prolonged effects on ovarian steroidogenesis during the implantation period, in line with a previous study demonstrating that this hormone stimulates progesterone/oestradiol production in luteal cells45. While buserelin elevated serum oestradiol on day 1, prolonged changes in ovarian steroidogenesis were not observed. Again, this difference in outcome is attributable to the shorter half-life of LH.
Progesterone and oestrogen regulate PR and ERα spatiotemporal expression in the uterus46,47,48. Critical for establishing and maintaining pregnancy49,50, PR is transiently expressed in luminal epithelium during the implantation period51,52. We confirmed this expression in control and buserelin-treated groups, but expression was inhibited throughout pre-implantation in hCG-treated groups. We further demonstrated that hCG administration inhibited Ihh, Areg, and Gata2 expression. These epithelial PR target genes play critical roles during initial implantation, regulating epithelial oestrogen signalling and the cell cycle26,53,54,55,56. In addition, Muc132,57,58 and Ltf30,31 epithelial oestrogen signalling remained high under hCG treatment on day 4, even though the process is normally inhibited during implantation, as observed in control and buserelin-treated groups.
Oestrogen-ER signalling promotes endometrial proliferation-differentiation switching, a marker of uterine receptivity59, while stromal PR signalling inhibits the process. Stromal proliferation is initiated on day 3 to prepare the uterus for implantation and decidualisation47,59,60,61,62. Furthermore, epithelial PR activity is essential for establishing uterine epithelial-stromal crosstalk and implantation63, but elevated oestrogen during pre-implantation inhibits PR64. We did not observe endometrial proliferation-differentiation switching in hCG-treated groups. Therefore, we speculate that when hCG stimulates oestradiol synthesis and secretion, PR signalling is inhibited, while ER signalling is stimulated in the luminal epithelium. In contrast, buserelin exerts no such effects, given that treatment with the GnRH agonist does not result in progesterone and oestradiol secretion patterns that differ from those of the control group. Our results demonstrate that buserelin administration is a method to trigger oocyte maturation that does not affect implantation, decidualisation, or subsequent term pregnancy. The drug does not affect ovarian steroidogenesis or endometrial steroid signalling during the pre-implantation period, whereas hCG clearly impaired uterine receptivity and pregnancy outcomes.
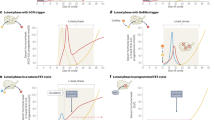
A previous study reported that the implantation process can be induced by exogenous LIF instead of oestrogen. Exogenous LIF induced implantation-associated events in the endometrium, such as closure of the uterine lumen, stromal decidualisation, and apoptosis of the luminal epithelium at the site of blastocyst attachment65. Therefore, we hypothesised that exogenous LIF administration could rescue the impairment of blastocyst implantation caused by hCG administration, as Lif expression was reduced in hCG treated mice. However, in contrast to our expectation, blastocyst implantation was not restored by LIF administration, although a slight improvement was observed in endometrial steroid signalling after the administration (Supplemental Fig. 3). Furthermore, we assessed the uterine receptivity after dual trigger with buserelin and hCG. Recent studies reported that dual trigger with GnRH agonist and hCG improved pregnancy outcomes compared to trigger with hCG only66,67. Although the effectiveness of dual trigger on uterine receptivity is still controversial as most recent study by Zhou et al. demonstrated that there are no differences in pregnancy outcomes between the dual and hCG only triggers68. Our results demonstrated that the dual trigger with low dose of buserelin and hCG tended to improve blastocyst implantation and endometrial steroid signalling (Supplemental Fig. 3), suggesting that the adverse effects of hCG administration on uterine receptivity may be dose-dependent and that the combination use of buserelin and low dose of hCG might be more likely to result in pregnancy outcomes after fresh embryo transfers.
While these results are promising, we note that human trials will be necessary to confirm whether the effects are carried over from the mouse model. Nevertheless, oestrogen and progesterone regulate uterine receptivity in both mice and humans43,69. Therefore, it is highly likely that hCG-induced hypersecretion of ovarian oestrogen and progesterone will alter epithelial PR and ER signalling in the endometrium and that these adverse effects are irreversible regardless of the treatment applied (whether recombinant LIF or dual trigger with buserelin). Our findings indicate that buserelin is preferable to hCG as an oocyte maturation trigger that can optimise uterine receptivity during fertility treatments.
Methods
Animals
ICR mice were obtained from Japan SLC Inc. (Shizuoka, Japan) and housed in a 12-h light/dark cycle. To induce oocyte maturation, 8-week-old female mice were divided into six treatment groups: 5 IU hCG, 10 IU hCG (Mochida Pharmaceutical, Tokyo, Japan), 360 ng buserelin acetate, 720 ng buserelin acetate (Sigma-Aldrich, St. Louis, MO, USA), and the low and moderate dose of dual trigger (low dose group, 2.5 IU hCG and 180 ng buserelin; moderate dose group, 5 IU hCG and 360 ng buserelin). Mice were injected intraperitoneally with the appropriate drug on the day of oestrus, as previously reported21,70, while a separate group of control mice were injected with saline. After injection, female mice were mated with 10–12-week-old vasectomised or intact ICR males to induce pseudopregnancy or pregnancy, respectively (day 1 = vaginal plug). Pseudopregnant females were subjected to the evaluation of decidualisation, as well as foetal development and implantation after embryo transfer. Pregnant females were evaluated for ovarian hormone synthesis and secretion, along with the expression of uterine steroid receptors and their downstream signalling. In some instances, 5 µg of recombinant LIF (Millipore, Burlington, MA, USA) was intraperitoneally injected into hCG-treated mice at 1600 h on days 3 and 4 of pregnancy or pseudopregnancy. All mouse work was conducted in accordance with the guideline of the institutional animal care and use committee of Kato Ladies Clinic which is based on Animal Welfare Act Regulations and the Guide for the Care and Use of Laboratory Animals. All animal experiments in this study were reviewed and approved by the institutional animal care and use committee of Kato Ladies Clinic (K011). All efforts were made to minimise the number of animals used and their suffering.
Embryo culture and transfer
Two-cell embryos were collected from the excised oviducts of donor mice on day 2 of pregnancy and cultured for 72 h until the blastocyst stage. The culturing medium was KSOM (potassium simplex optimised medium; Millipore, Billerica, MA, USA), and conditions were 37 °C in a 5% CO2/95% air atmosphere. Embryo transfers and caesarean sections were performed in all groups, as described previously21, to evaluate full-term development. Briefly, 12 blastocysts were transferred into uteri of pseudopregnant mice on day 4. On day 19, live foetuses were removed through caesarean sections to determine pregnancy rate.
Analysis of blastocyst implantation
Ten blastocysts were transferred into the uteri of pseudopregnant females on the fourth day after pregnancy initiation. On day 5, Chicago blue dye solution was intravenously injected into these pseudopregnant females or into naturally mated females71. The dye allowed for visual evaluation of implantation sites.
Induction of artificial decidualisation
Artificial decidualisation was induced as previously described72. Briefly, pseudopregnancy was induced in female mice through mating with vasectomised males. Sesame oil (25 µL) was infused into one side of the uterine horn to cause decidualisation. Wet weights of infused and non-infused uterine horns were recorded on day 8. Fold induction in uterine wet weights was used as the index for comparing artificial decidualisation.
Measurement of serum progesterone and oestradiol-17β
Serum was collected from 500 µL of blood per mouse. Serum progesterone and oestradiol levels were measured with enzyme immunoassay EIA kits (Cayman Chemical Company, Ann Arbor, MI, USA), following the manufacturer’s protocol.
Immunohistochemistry
Uterine sections were immunostained for PR, ERα, Muc1, Ki67, and pSTAT3 using previously described procedures with slight modifications21. Uterine horns were collected from female mice on days 1–4 of pregnancy and fixed in 10% neutral-buffered formalin to generate paraffin sections. Sections were deparaffinised in xylene, rehydrated using a graded ethanol series, and then blocked with 3% bovine serum albumin in Ca2+/Mg2+-free Dulbecco’s phosphate-buffered saline (PBS). Sections were incubated overnight at 4 °C with the following primary antibodies: mouse anti-PR antibody (1:300, LS-B5236; LifeSpan Biosciences, Seattle, WA, USA), rabbit anti-ERα antibody (1:300, sc-7207; Santa Cruz Biotechnology, Dallas, TX, USA), rabbit anti-Muc1 antibody (1:200, NB-120-15481; Novus Biologicals, Littleton, CO, USA), rabbit anti-Ki67 antibody (1:200, RM-9106; Thermo Scientific, Waltham, MA, USA), and rabbit anti-pSTAT3 antibody (1:200, ab76315; Abcam, Cambridge, UK). Sections were washed and then incubated with the following secondary antibodies: biotinylated goat anti-rabbit antibody (1:500, 111-065; Jackson ImmunoResearch, West Grove, PA, USA) to detect ERα, Muc1, Ki67, and pSTAT3, and biotinylated goat anti-mouse antibody (1:500, 62–6540; Life Technologies, Waltham, MA, USA) to detect PR. Next, sections were incubated with horseradish peroxidase-conjugated streptavidin (1:300, 43–4323; Life Technologies) and then with chromogen 3,3′-diaminobenzidine tetrahydrochloride (DAB, 00–2007; Life Technologies) to visualise antibody staining. Finally, sections were counterstained with haematoxylin to reveal immunoreaction sites (reddish deposits). A semiquantitative approach was used to evaluate Ki67 expression. Specifically, staining intensity (SI) per cell was classified as 0–3 (Supplemental Fig. 1) for calculating an H-score from the following formula: [1 × (% of cells with SI = 1) + 2 × (% of cells with SI = 2) + 3 × (% of cells with SI = 3)].
Quantitative RT-PCR analysis
Quantitative (q)RT-PCR assays were performed as previously described21,73. Ovaries and uterine horns were collected and stored at −80 °C until use. Total RNA was extracted using TRIzol reagent (Invitrogen, Carlsbad, CA, USA) and then further purified with the PureLink RNA mini kit (Life Technologies). Reverse transcription of RNA (5 μg) was performed using a high-capacity RNA-to-cDNA kit (Life Technologies). Next, mRNA levels of the following genes were quantified with TaqMan Gene Expression Assay (Life Technologies): Hsd3b1 (Mm01261921_mH), Cyp19a1 (Mm00484049_m1), Ihh (Mm00439613_m1), Areg (Mm01354339_m1), Gata2 (Mm00492301_m1), Lif (Mm00434762_g1), Muc1 (Mm00449604_m1), Ltf (Mm00434787_m1), and Foxa2 (Mm01976556_s1). The reaction mixture (20 μL) included the TaqMan Fast Universal PCR Master Mix (4352042; Life Technologies) and sequences were amplified in a StepOnePlus Real-time PCR System (Applied Biosystems, Foster City, CA, USA). Each sample was assayed in duplicate. Glyceraldehyde-3-phosphate dehydrogenase (Mm99999915_g1) was selected as the housekeeping gene. Relative gene expression was quantified according to the standard-curve method using StepOne version 2.1 (Applied Biosystems).
Statistical analysis
Significant differences in pregnancy rates, pup birth, and luminal Muc1-positive mice were determined via Chi-square tests, unless expected values were <5. In such cases, Fisher’s exact probability test was used for comparisons. Pup weight, placental weight, number of implantation sites, uterine weight fold-increase, serum progesterone and oestradiol levels, mRNA expression levels, as well as H-scores were all normally distributed. One-way analysis of variance and post-hoc multiple-comparison test were used to determine between-group differences and to separate means. Significance was set at P < 0.05.
References
Itskovitz, J. et al. Induction of preovulatory luteinizing hormone surge and prevention of ovarian hyperstimulation syndrome by gonadotropin-releasing hormone agonist. Fertility and sterility 56, 213–220 (1991).
Gonen, Y., Balakier, H., Powell, W. & Casper, R. F. Use of gonadotropin-releasing hormone agonist to trigger follicular maturation for in vitro fertilization. The Journal of clinical endocrinology and metabolism 71, 918–922, https://doi.org/10.1210/jcem-71-4-918 (1990).
Nakano, R. et al. “Triggering” of ovulation after infusion of synthetic luteinizing hormone releasing factor (LRF). Acta obstetricia et gynecologica Scandinavica 52, 269–272 (1973).
Segal, S. & Casper, R. F. Gonadotropin-releasing hormone agonist versus human chorionic gonadotropin for triggering follicular maturation in in vitro fertilization. Fertility and sterility 57, 1254–1258 (1992).
Humaidan, P. et al. GnRH agonist (buserelin) or hCG for ovulation induction in GnRH antagonist IVF/ICSI cycles: a prospective randomized study. Hum Reprod 20, 1213–1220, https://doi.org/10.1093/humrep/deh765 (2005).
Zelinski-Wooten, M. B., Hutchison, J. S., Hess, D. L., Wolf, D. P. & Stouffer, R. L. Follicle stimulating hormone alone supports follicle growth and oocyte development in gonadotrophin-releasing hormone antagonist-treated monkeys. Hum Reprod 10, 1658–1666 (1995).
Hoff, J. D., Quigley, M. E. & Yen, S. S. Hormonal dynamics at midcycle: a reevaluation. The Journal of clinical endocrinology and metabolism 57, 792–796, https://doi.org/10.1210/jcem-57-4-792 (1983).
Yding Andersen, C. Effect of FSH and its different isoforms on maturation of oocytes from pre-ovulatory follicles. Reproductive biomedicine online 5, 232–239 (2002).
Eppig, J. J. FSH stimulates hyaluronic acid synthesis by oocyte-cumulus cell complexes from mouse preovulatory follicles. Nature 281, 483–484 (1979).
Moyle, W. R., Bahl, O. P. & Marz, L. Role of carbohydrate of human chorionic gonadotropin in the mechanism of hormone action. The Journal of biological chemistry 250, 9163–9169 (1975).
Schalch, D. S., Parlow, A. F., Boon, R. C. & Reichlin, S. Measurement of human luteinizing hormone in plasma by radioimmunoassay. The Journal of clinical investigation 47, 665–678, https://doi.org/10.1172/JCI105762 (1968).
Faiman, C., Ryan, R. J., Zwirek, S. J. & Rubin, M. E. Serum FSH and HCG during human pregnancy and puerperium. The Journal of clinical endocrinology and metabolism 28, 1323–1329, https://doi.org/10.1210/jcem-28-9-1323 (1968).
Stenman, U. H., Unkila-Kallio, L., Korhonen, J. & Alfthan, H. Immunoprocedures for detecting human chorionic gonadotropin: clinical aspects and doping control. Clinical chemistry 43, 1293–1298 (1997).
Kol, S. Luteolysis induced by a gonadotropin-releasing hormone agonist is the key to prevention of ovarian hyperstimulation syndrome. Fertility and sterility 81, 1–5 (2004).
Engmann, L. et al. The use of gonadotropin-releasing hormone (GnRH) agonist to induce oocyte maturation after cotreatment with GnRH antagonist in high-risk patients undergoing in vitro fertilization prevents the risk of ovarian hyperstimulation syndrome: a prospective randomized controlled study. Fertility and sterility 89, 84–91, https://doi.org/10.1016/j.fertnstert.2007.02.002 (2008).
DiLuigi, A. J. et al. Gonadotropin-releasing hormone agonist to induce final oocyte maturation prevents the development of ovarian hyperstimulation syndrome in high-risk patients and leads to improved clinical outcomes compared with coasting. Fertility and sterility 94, 1111–1114, https://doi.org/10.1016/j.fertnstert.2009.10.034 (2010).
Lewit, N., Kol, S., Manor, D. & Itskovitz-Eldor, J. Comparison of gonadotrophin-releasing hormone analogues and human chorionic gonadotrophin for the induction of ovulation and prevention of ovarian hyperstimulation syndrome: a case-control study. Hum Reprod 11, 1399–1402 (1996).
Humaidan, P. et al. The luteal phase after GnRH-agonist triggering of ovulation: present and future perspectives. Reproductive biomedicine online 24, 134–141, https://doi.org/10.1016/j.rbmo.2011.11.001 (2012).
Forman, R. et al. Evidence for an adverse effect of elevated serum estradiol concentrations on embryo implantation. Fertility and sterility 49, 118–122 (1988).
Simon, C. et al. Increasing uterine receptivity by decreasing estradiol levels during the preimplantation period in high responders with the use of a follicle-stimulating hormone step-down regimen. Fertility and sterility 70, 234–239 (1998).
Ezoe, K. et al. Ovarian stimulation using human chorionic gonadotrophin impairs blastocyst implantation and decidualization by altering ovarian hormone levels and downstream signaling in mice. Molecular human reproduction 20, 1101–1116, https://doi.org/10.1093/molehr/gau065 (2014).
Bourgain, C. & Devroey, P. The endometrium in stimulated cycles for IVF. Human reproduction update 9, 515–522 (2003).
Valbuena, D. et al. Increasing levels of estradiol are deleterious to embryonic implantation because they directly affect the embryo. Fertility and sterility 76, 962–968 (2001).
Engmann, L. & Benadiva, C. GnRH agonist (buserelin) or HCG for ovulation induction in GnRH antagonist IVF/ICSI cycles: a prospective randomized study. Hum Reprod 20, 3258–3260; author reply 3260, https://doi.org/10.1093/humrep/dei190 (2005).
Lee, K. et al. Indian hedgehog is a major mediator of progesterone signaling in the mouse uterus. Nature genetics 38, 1204–1209, https://doi.org/10.1038/ng1874 (2006).
Matsumoto, H., Zhao, X., Das, S. K., Hogan, B. L. & Dey, S. K. Indian hedgehog as a progesterone-responsive factor mediating epithelial-mesenchymal interactions in the mouse uterus. Developmental biology 245, 280–290, https://doi.org/10.1006/dbio.2002.0645 (2002).
Lee, D. S., Yanagimoto Ueta, Y. & Suzuki, H. Expression of amphiregulin during the pre- and post-implantation period in the mouse reproductive tract. The Journal of reproduction and development 52, 781–787 (2006).
Das, S. K. et al. Amphiregulin is an implantation-specific and progesterone-regulated gene in the mouse uterus. Mol Endocrinol 9, 691–705, https://doi.org/10.1210/mend.9.6.8592515 (1995).
Rubel, C. A., Franco, H. L., Jeong, J. W., Lydon, J. P. & DeMayo, F. J. GATA2 is expressed at critical times in the mouse uterus during pregnancy. Gene expression patterns: GEP 12, 196–203, https://doi.org/10.1016/j.gep.2012.03.004 (2012).
Newbold, R. R. et al. Fluctuations of lactoferrin protein and messenger ribonucleic acid in the reproductive tract of the mouse during the estrous cycle. Biology of reproduction 47, 903–915 (1992).
Pentecost, B. T. & Teng, C. T. Lactotransferrin is the major estrogen inducible protein of mouse uterine secretions. The Journal of biological chemistry 262, 10134–10139 (1987).
Surveyor, G. A. et al. Expression and steroid hormonal control of Muc-1 in the mouse uterus. Endocrinology 136, 3639–3647 (1995).
Song, H., Lim, H., Das, S. K., Paria, B. C. & Dey, S. K. Dysregulation of EGF family of growth factors and COX-2 in the uterus during the preattachment and attachment reactions of the blastocyst with the luminal epithelium correlates with implantation failure in LIF-deficient mice. Mol Endocrinol 14, 1147–1161, https://doi.org/10.1210/mend.14.8.0498 (2000).
Stewart, C. L. et al. Blastocyst implantation depends on maternal expression of leukaemia inhibitory factor. Nature 359, 76–79, https://doi.org/10.1038/359076a0 (1992).
Ertzeid, G. & Storeng, R. The impact of ovarian stimulation on implantation and fetal development in mice. Hum Reprod 16, 221–225 (2001).
Van der Auwera, I. & D’Hooghe, T. Superovulation of female mice delays embryonic and fetal development. Hum Reprod 16, 1237–1243 (2001).
Rashidi, B., Soleimani Rad, J. I., Roshangar, L. & Alizadeh Miran, R. Evaluation of Pinopodes Expression on the Mouse Endometrium Immediately before Implantation by Treatment with HMG/HCG and Sildenafil Citrate Administration. Iranian journal of basic medical sciences 15, 1091–1096 (2012).
Walton, E. A., Huntley, S., Kennedy, T. G. & Armstrong, D. T. Possible causes of implantation failure in superovulated immature rats. Biology of reproduction 27, 847–852 (1982).
Fossum, G. T., Davidson, A. & Paulson, R. J. Ovarian hyperstimulation inhibits embryo implantation in the mouse. Journal of in vitro fertilization and embryo transfer: IVF 6, 7–10 (1989).
Ertzeid, G. & Storeng, R. Adverse effects of gonadotrophin treatment on pre- and postimplantation development in mice. Journal of reproduction and fertility 96, 649–655 (1992).
Yen, S. S., Llerena, O., Little, B. & Pearson, O. H. Disappearance rates of endogenous luteinizing hormone and chorionic gonadotropin in man. The Journal of clinical endocrinology and metabolism 28, 1763–1767, https://doi.org/10.1210/jcem-28-12-1763 (1968).
Damewood, M. D. et al. Disappearance of exogenously administered human chorionic gonadotropin. Fertility and sterility 52, 398–400 (1989).
Cha, J., Sun, X. & Dey, S. K. Mechanisms of implantation: strategies for successful pregnancy. Nature medicine 18, 1754–1767, https://doi.org/10.1038/nm.3012 (2012).
Dey, S. K. et al. Molecular cues to implantation. Endocrine reviews 25, 341–373, https://doi.org/10.1210/er.2003-0020 (2004).
Richardson, M. C. & Masson, G. M. Stimulation by human chorionic gonadotrophin of oestradiol production by dispersed cells from human corpus luteum: comparison with progesterone production; utilization of exogenous testosterone. The Journal of endocrinology 91, 197–203 (1981).
Das, S. K., Tan, J., Johnson, D. C. & Dey, S. K. Differential spatiotemporal regulation of lactoferrin and progesterone receptor genes in the mouse uterus by primary estrogen, catechol estrogen, and xenoestrogen. Endocrinology 139, 2905–2915 (1998).
Huet-Hudson, Y. M., Andrews, G. K. & Dey, S. K. Cell type-specific localization of c-myc protein in the mouse uterus: modulation by steroid hormones and analysis of the periimplantation period. Endocrinology 125, 1683–1690 (1989).
Tibbetts, T. A., Mendoza-Meneses, M., O’Malley, B. W. & Conneely, O. M. Mutual and intercompartmental regulation of estrogen receptor and progesterone receptor expression in the mouse uterus. Biology of reproduction 59, 1143–1152 (1998).
Fernandez-Valdivia, R. et al. A mouse model to dissect progesterone signaling in the female reproductive tract and mammary gland. Genesis 48, 106–113, https://doi.org/10.1002/dvg.20586 (2010).
Lydon, J. P. et al. Mice lacking progesterone receptor exhibit pleiotropic reproductive abnormalities. Genes & development 9, 2266–2278 (1995).
Spencer, T. E., Johnson, G. A., Burghardt, R. C. & Bazer, F. W. Progesterone and placental hormone actions on the uterus: insights from domestic animals. Biology of reproduction 71, 2–10, https://doi.org/10.1095/biolreprod.103.024133 (2004).
Tan, J., Paria, B. C., Dey, S. K. & Das, S. K. Differential uterine expression of estrogen and progesterone receptors correlates with uterine preparation for implantation and decidualization in the mouse. Endocrinology 140, 5310–5321 (1999).
Jeong, J. W. et al. Identification of murine uterine genes regulated in a ligand-dependent manner by the progesterone receptor. Endocrinology 146, 3490–3505, https://doi.org/10.1210/en.2005-0016 (2005).
Takamoto, N., Zhao, B., Tsai, S. Y. & DeMayo, F. J. Identification of Indian hedgehog as a progesterone-responsive gene in the murine uterus. Mol Endocrinol 16, 2338–2348 (2002).
Kurita, T., Lee, K. J., Cooke, P. S., Lydon, J. P. & Cunha, G. R. Paracrine regulation of epithelial progesterone receptor and lactoferrin by progesterone in the mouse uterus. Biology of reproduction 62, 831–838 (2000).
Franco, H. L. et al. Ablation of Indian hedgehog in the murine uterus results in decreased cell cycle progression, aberrant epidermal growth factor signaling, and increased estrogen signaling. Biology of reproduction 82, 783–790, https://doi.org/10.1095/biolreprod.109.080259 (2010).
Carson, D. D. et al. Mucin expression and function in the female reproductive tract. Human reproduction update 4, 459–464 (1998).
DeSouza, M. M. et al. MUC1/episialin: a critical barrier in the female reproductive tract. Journal of reproductive immunology 45, 127–158 (1999).
Haraguchi, H. et al. MicroRNA-200a locally attenuates progesterone signaling in the cervix, preventing embryo implantation. Mol Endocrinol 28, 1108–1117, https://doi.org/10.1210/me.2014-1097 (2014).
Li, Q. et al. The antiproliferative action of progesterone in uterine epithelium is mediated by Hand2. Science 331, 912–916, https://doi.org/10.1126/science.1197454 (2011).
Martin, L., Das, R. M. & Finn, C. A. The inhibition by progesterone of uterine epithelial proliferation in the mouse. The Journal of endocrinology 57, 549–554 (1973).
Martin, L., Finn, C. A. & Trinder, G. Hypertrophy and hyperplasia in the mouse uterus after oestrogen treatment: an autoradiographic study. The Journal of endocrinology 56, 133–144 (1973).
Franco, H. L. et al. Epithelial progesterone receptor exhibits pleiotropic roles in uterine development and function. FASEB journal: official publication of the Federation of American Societies for Experimental Biology 26, 1218–1227, https://doi.org/10.1096/fj.11-193334 (2012).
Ma, W. G., Song, H., Das, S. K., Paria, B. C. & Dey, S. K. Estrogen is a critical determinant that specifies the duration of the window of uterine receptivity for implantation. Proceedings of the National Academy of Sciences of the United States of America 100, 2963–2968, https://doi.org/10.1073/pnas.0530162100 (2003).
Chen, J. R. et al. Leukemia inhibitory factor can substitute for nidatory estrogen and is essential to inducing a receptive uterus for implantation but is not essential for subsequent embryogenesis. Endocrinology 141, 4365–4372, https://doi.org/10.1210/endo.141.12.7855 (2000).
Oliveira, S. A., Calsavara, V. F. & Cortes, G. C. Final Oocyte Maturation in Assisted Reproduction with Human Chorionic Gonadotropin and Gonadotropin-releasing Hormone agonist (Dual Trigger). JBRA assisted reproduction 20, 246–250, https://doi.org/10.5935/1518-0557.20160047 (2016).
Lin, M. H. et al. Dual trigger with gonadotropin releasing hormone agonist and human chorionic gonadotropin significantly improves live birth rate for women with diminished ovarian reserve. Reproductive biology and endocrinology: RB&E 17, 7, https://doi.org/10.1186/s12958-018-0451-x (2019).
Zhou, X. et al. Comparison of dual trigger with combination GnRH agonist and hCG versus hCG alone trigger of oocyte maturation for normal ovarian responders. International journal of gynaecology and obstetrics: the official organ of the International Federation of Gynaecology and Obstetrics 141, 327–331, https://doi.org/10.1002/ijgo.12457 (2018).
Chai, J., Lee, K. F., Ng, E. H., Yeung, W. S. & Ho, P. C. Ovarian stimulation modulates steroid receptor expression and spheroid attachment in peri-implantation endometria: studies on natural and stimulated cycles. Fertility and sterility 96, 764–768, https://doi.org/10.1016/j.fertnstert.2011.06.015 (2011).
Byers, S. L., Wiles, M. V., Dunn, S. L. & Taft, R. A. Mouse estrous cycle identification tool and images. PloS one 7, e35538, https://doi.org/10.1371/journal.pone.0035538 (2012).
Paria, B. C., Huet-Hudson, Y. M. & Dey, S. K. Blastocyst’s state of activity determines the “window” of implantation in the receptive mouse uterus. Proceedings of the National Academy of Sciences of the United States of America 90, 10159–10162 (1993).
Lim, H. et al. Multiple female reproductive failures in cyclooxygenase 2-deficient mice. Cell 91, 197–208 (1997).
Takehara, Y. et al. The restorative effects of adipose-derived mesenchymal stem cells on damaged ovarian function. Laboratory investigation; a journal of technical methods and pathology 93, 181–193, https://doi.org/10.1038/labinvest.2012.167 (2013).
Acknowledgements
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
K.E. and A.Y. designed the experiments. K.E. and N.M. performed experiments. K.E. analysed the data. K.E., A.Y., T.K. and K.K. wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ezoe, K., Murata, N., Yabuuchi, A. et al. Evaluation of uterine receptivity after gonadotropin releasing hormone agonist administration as an oocyte maturation trigger: a rodent model. Sci Rep 9, 12519 (2019). https://doi.org/10.1038/s41598-019-48918-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-48918-3
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.