Abstract
Non-small cell lung cancer (NSCLC) is the most frequent cause of cancer-related death worldwide. Although many molecular-targeted drugs for NSCLC have been developed in recent years, the 5-year survival rate of patients with NSCLC remains low. Therefore, an improved understanding of the molecular mechanisms underlying the biology of NSCLC is essential for developing novel therapeutic strategies for the treatment of NSCLC. In this study, we examined the role of miR-130b in NSCLC. Our results showed that high expression of miR-130b in clinical specimens was significantly associated with poor overall survival in patients with NSCLC. Moreover, miR-130b expression was significantly increased in NSCLC clinical specimens from patients with vascular and lymphatic invasion. Consistent with this, overexpression of miR-130b promoted invasion and matrix metalloproteinase-2 (MMP-2) activity in A549 cells. Argonaute2 immunoprecipitation and gene array analysis identified tissue inhibitor of metalloproteinase-2 (TIMP-2) as a target of miR-130b. Invasion activity promoted by miR-130b was attenuated by TIMP-2 overexpression in A549 cells. Furthermore, TIMP-2 concentrations in serum were inversely correlated with relative miR-130b expression in tumor tissues from the same patients with NSCLC. Overall, miR-130b was found to act as an oncomiR, promoting metastasis by downregulating TIMP-2 and invasion activities in NSCLC cells.
Similar content being viewed by others
Introduction
Lung cancer is the most common cause of cancer-related death worldwide, causing an estimated 1.6 million deaths each year. Approximately 85% of patients with lung cancer have the histological subtype known as non-small cell lung cancer (NSCLC), in which lung adenocarcinoma and lung squamous cell carcinoma are the most common subtypes1,2. Although several therapeutic agents for NSCLC have been developed, the prognosis of patients with NSCLC is still poor, and the 5-year survival rate is less than 18%. This low survival rate may be explained by the observation that most cases are diagnosed as a late stage, when lung cancer cells have already metastasised to distant organs3,4,5.
To break away from the primary tumor and initiate the metastatic process, cancer cells must acquire the ability to migrate and invade6,7. Matrix metalloproteinases (MMPs) are proteases involved in extracellular matrix remodelling8. In particular, MMP-2 plays a key role in tumor invasion and metastasis by degrading type IV collagen, which is a major component of the basal membrane9. High expression of MMP-2 has been reported in several cancers and is a poor prognostic factor in patients with NSCLC10,11,12,13,14. Pro-MMP-2, an inactivated form of MMP-1, is activated on the cell surface by membrane-tethered membrane type 1-MMP (MT1-MMP), in a process regulated by tissue inhibitor of metalloproteinase (TIMP)-2. A complex of active membrane-tethered MT1-MMP and TIMP-2 binds to pro-MMP-2, enabling pro-MMP-2 to be activated by MT1-MMP15.
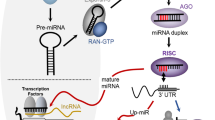
MicroRNAs (miRNAs) are small noncoding RNA molecules 20–25 nucleotides in length. These molecules regulate gene expression through translational repression or degradation of mRNA by binding to the 3′-untranslated region (3′-UTR) of target mRNAs16. Each miRNA typically targets approximately 200 genes17,18. Because 30–60% of human genes can be regulated by miRNAs19,20, these molecules have the potential to modulate various cellular processes, such as cell growth, migration, invasion, apoptosis, and angiogenesis21. Our previous study showed that the miR-130 family, including miR-130b, miR-301a, and miR-301b, is highly expressed in bladder cancer specimens and functions as an oncogenic miRNA family by promoting the migration and invasion of bladder cancer cells22. Moreover, miR-130 family-targeted LNA oligonucleotides were found to suppress tumor growth in an in vivo xenograft model23.
In this study, we evaluated the expression and roles of miR-130b in NSCLC. Our results provided important insights into the molecular pathogenesis of NSCLC and suggested that miR-130b may function as an oncogenic miRNA in NSCLC.
Results
High miR-130b expression was correlated with poor overall survival in patients with NSCLC
Using The Cancer Genome Atlas (TCGA) database, we first investigated the relationship between expression of the miR-130 family and prognosis of patients with NSCLC. Although there was no significant relationship between miR-130 family expression and the prognosis of patients with squamous cell carcinoma (Supplementary Fig. 1A–C), adenocarcinoma patients with high miR-130b expression had significantly poorer overall survival than those with low miR-130b expression (Fig. 1A). In contrast, there were no significant relationships between the expression of miR-301a or miR-301b and overall survival in patients with adenocarcinoma (Fig. 1B,C). Therefore, we focused on miR-130b in subsequent analyses. To confirm the expression of miR-130b in NSCLC clinical specimens, we performed real-time quantitative polymerase chain reaction (qPCR) analysis using matched pair samples of NSCLC tissues and normal adjacent lung tissues. We found that miR-130b expression was significantly higher in NSCLC tissues than in normal adjacent lung tissues (Fold-change 5.0, p < 0.001, Fig. 1D). miR-130b expression in NSCLC tissues tended to increase as the cancer stage increased (Fig. 1E). Interestingly, miR-130b expression was high in NSCLC tissues, regardless of histologic subtypes (Fig. 1F) and of the presence or absence of epidermal growth factor receptor gene mutation (Fig. 1G, Table 1) in adenocarcinoma specimens. These results suggested that miR-130b had an important role in NSCLC.
High miR-130b expression was correlated with poor overall survival in NSCLC clinical specimens. (A–C) TCGA database analysis of miR-130b, miR-301a, and miR-301b in patients with adenocarcinoma. Overall survival analysis in patients with high (copy number: 1) and low (copy number: −1) miR-130 family expression was analysed by Kaplan-Meier analysis with log-rank tests. The number of patients analysed is indicated in parentheses. miR-130b expression levels were measured by real-time qPCR and were compared among normal and tumor tissues (D) and tumor stages (E) in NSCLC clinical specimens, tumor subtypes in specimens with adenocarcinoma or squamous cell carcinoma (F), status of epidermal growth factor receptor gene mutation in specimens with adenocarcinoma (G). Relative miR-130b expression normalized to U6 snRNA is shown. Data are means ± standard deviations. **p < 0.01 and ***p < 0.001 for t-tests (D) and one-way analysis of variance (post-hoc Bonferroni multiple comparison tests) (E–G).
miR-130b promoted invasion activity in NSCLC cells
To investigate the biological functions of miR-130b, we first determined the expression level of miR-130b in NSCLC cell lines. Among 20 adenocarcinoma and squamous cell carcinoma cell lines, the lowest expression of miR-130b was found in A549 cells (Supplementary Fig. 2A). We then established A549 cells stably overexpressing miR-130b (Supplementary Fig. 2B) and examined the effects of miR-130b on tumor-promoting phenotypes in the cells. Although miR-130b overexpression had no significant effect on cell growth or migration (Supplementary Fig. 3A–C), invasion activity was upregulated in A549 cells stably overexpressing miR-130b (Fig. 2A). Next, we transfected the miR-130b mimic into A549 (not stably overexpressing miR-130b), NCI-H520 and NCI-H1975 cells, which show the lowest endogenous miR-130 expression, or miR-130b inhibitor into NCI-H1755 cells, which exhibit the highest endogenous miR-130 expression, of all NSCLC cell lines examined in this study (Supplementary Fig. 4A–D). Transfection with the miR-130b mimic markedly upregulated the invasion activity of A549 cells (Fig. 2B) and NCI-H520 cells (Supplementary Fig. 5), suggesting that miR-130b promotes cell invasion activity not only in adenocarcinoma cells but also in squamous cell carcinoma cells. In contrast, transfection with the miR-130b inhibitor downregulated the invasion activity of NCI-H1755 cells (Fig. 2C), without affecting cell proliferation (Supplementary Fig. 6). Importantly, primary cultured NSCLC cells with high miR-130b expression (No. 230) showed a more obvious invasive phenotype than cells with low miR-130b expression (No. 225) in the 3D invasion assay (Fig. 2D). Importantly, tumor samples from patients with vascular invasion, lymphatic invasion and pleura cancer cell invasion had higher miR-130b expression than those without invasion (Fig. 2E–G). Because high expression of MMP-2, which functions as a key enzyme in tumor cell invasion, has been reported as a prognostic factor in NSCLC12, we next examined the effects of miR-130b on MMP-2 activity in miR-130b-overexpressing A549 cells. Although MMP-2 mRNA levels were not altered (Fig. 2H), miR-130b-overexpressing A549 cells showed increased MMP2 activity in gelatine-zymography assays (Fig. 2I) and increased MMP-2 expression in western blot analysis using anti-MMP-2 antibodies (Fig. 2J) compared with that in mock-transfected A549 cells. The extracellular protein level was nearly identical between mock cells and miR-130b-overexpressing A549 cells (Supplementary Table 1). These results suggested that miR-130b promoted invasion in NSCLC cells via upregulation of MMP-2 activity.
miR-130b overexpression promoted invasion and MMP-2 activities in A549 cells. A549 cells stably overexpressing miR-130b or mock control (mock) (A), A549 cells transfected with the miR-130b mimic (130b) or negative control miRNA mimic (NC) (B), and NCI-H1755 cells transfected with the miR-130b inhibitor (130b) or negative control miRNA inhibitor (NC) (C) were subjected to invasion assays. The transfected cells were added to the upper chambers of Matrigel-coated transwell membrane inserts, and the lower chambers were filled with medium. Cells were cultured for 20 h (A549 cells), or 48 h (NCI-H1755). Fluorescence derived from invasive cells was measured. Data are means ± standard deviations of three independent experiments. *p < 0.05 and **p < 0.01 for t-tests. (D) miR-130b expression level was examined by real-time qPCR. Primary cultured NSCLC cells were seeded into Nunclon Sphera 96U-well plates and incubated for 48 h. The medium was replaced with that containing Matrigel and incubated for 72 h. The expression of miR-130b was compared in NSCLC specimens with or without vascular invasion (E), lymphatic invasion (F), and pleura cancer cell invasion (G). Relative expression normalized to U6 snRNA is shown (means ± standard deviations). *p < 0.05 for t-tests. (H) MMP-2 levels in A549 cells stably overexpressing miR-130b or control vector (mock) were analysed by real-time qPCR. The relative expression of MMP-2 normalized to GAPDH is shown (means ± standard deviations) from three independent experiments. Conditioned medium from A549 cells stably overexpressing miR-130b or control vector (mock) were subjected to gelatine-zymography (I) and western blotting analysis with anti-MMP-2 antibodies (J). Uncropped zymography and Western blot data is shown in Supplementary Fig. S9. Representative results from three independent experiments are shown. Data are means ± standard deviations from three independent experiments. *p < 0.05 and **p < 0.01 for t-tests.
miR-130b promoted invasion via targeting TIMP-2 in NSCLC cells
To identify target genes of miR-130b, we conducted an argonaute2 (Ago2) immunoprecipitation (IP) assay using A549 cells transfected with an empty vector or miR-130b expression vector (Supplementary Fig. 7A). mRNAs immunoprecipitated with anti-Ago2 antibodies were then subjected to gene array analysis. Candidate target genes of miR-130b were extracted by miRNA target prediction algorithms (miRbase, TargetScan, and miRWalk; Supplementary Table 2). Among the identified genes, we focused on TIMP-2, which functions as an inhibitor of MMP-2 activity, as a candidate miR-130b target gene in NSCLC cells.
To confirm whether TIMP-2 is a target gene of miR-130b, we transfected cells with a luciferase reporter vector harbouring a sequence containing the predicted miR-130b-binding site in the 3′-UTR of human TIMP-2 (wild-type TIMP-2) or that containing the mutated miR-130b-binding site (mutant TIMP-2) in A549 cells (Supplementary Fig. 7B). As shown in Fig. 3A, transfection with the wild-type TIMP-2 vector significantly decreased luciferase activity in miR-130b-overexpressing A549 cells compared with that in mock control A549 cells. In contrast, miR-130b overexpression had no significant effect on luciferase activity in mutant TIMP-2-transfected A549 cells (Fig. 3A). Although miR-130b overexpression had no significant effect on TIMP-2 mRNA levels (Fig. 3B), western blot analysis showed decreased protein levels of both extracellular and intracellular TIMP-2 in miR-130b-overexpressing A549 cells (Fig. 3C,D). Moreover, transfection with the miR-130b mimic decreased TIMP-2 protein levels in A549, NCI-H520 and NCI-H1975 cells (Supplementary Fig. 8A–D), while miR-130b mimic or inhibitor had no effect on TIMP-2 mRNA expression in the cells (Supplementary Fig. 9A–D). Conversely, transfection with a miR-130b inhibitor upregulated TIMP-2 protein expression in NCI-H1755 cells (Fig. 3E,F), indicating that TIMP-2 was a target of miR-130b in NSCLC cells.
miR-130b targeted TIMP-2 in NSCLC cells. (A) A549 cells stably overexpressing miR-130b were transfected with a luciferase reporter construct containing the predicted miR-130b-binding site (WT) or the mutated predicted miR-130b-binding site (mut) in the TIMP-2 3′-UTR. Data are means ± standard deviations of more than five independent experiments. *p < 0.05 for one-way analysis of variance followed by post-hoc Bonferroni multiple comparison tests. (B) A549 cells stably overexpressing miR-130b (130b) or control vector (mock) were subjected to real-time qPCR analysis of TIMP-2. Relative expression of TIMP-2 normalized to GAPDH is shown (means ± standard deviations) from three independent experiments. (C,D) A549 cells stably overexpressing miR-130b (130b) or control vector (mock) were subjected to western blotting with anti-TIMP-2 antibodies. Representative results from three independent experiments are shown. Representative results of three independent experiments are shown for (C). The numbers indicate the relative expression of TIMP-2 compared to that in NC, as analyzed by densitometry. *p < 0.05 for t-tests. Uncropped western blot data is shown in Supplementary Fig. 10. (E,F) NCI-H1755 cells were transfected with the negative control inhibitor (NC) or miR-130b inhibitor (130b) for 48 h, and whole-cell lysates were subjected to western blotting with anti-TIMP-2 antibodies. Representative results of three independent experiments are shown. The numbers indicate the relative expression of TIMP-2 compared to that in NC, as analysed by densitometry. *p < 0.05 for t-tests. Uncropped western blot data is shown in Supplementary Fig. 10.
Next, we examined whether promotion of invasion activity by miR-130b overexpression was related to a decrease in TIMP-2 expression. The effects of miR-130b on invasion activity were attenuated by TIMP-2 overexpression in A549 cells (Fig. 4A,B). Moreover, TIMP-2 overexpression blocked the effects of miR-130b on MMP-2 activity in A549 cells (Fig. 4C), suggesting that miR-130b promoted cell invasion activity by downregulating TIMP-2 protein expression and upregulating MMP-2 activity in NSCLC cells.
miR-130b promoted invasion by targeting TIMP-2 in A549 cells. Control (mock) or miR-130b-overexpressing A549 cells (130b) were transfected with the control vector (empty) or TIMP-2 expression vector (TIMP-2) for 48 h. Cells were then subjected to western blot analysis (A), invasion assays (B), and gelatine-zymography (C). Uncropped Western blot and zymography data are shown in Supplementary Fig. 10. Representative results from three independent experiments are shown. The numbers indicate the relative expression of TIMP-2 compared to that of control (mock/empty) A549 cells, as analyzed by densitometry (A,C). Data are the means ± standard deviations of three independent experiments in A, B, and C. *p < 0.05 for one-way analysis of variance followed by post-hoc Bonferroni multiple comparison tests.
Serum TIMP-2 concentrations were inversely correlated with tumor miR-130b expression levels in patients with NSCLC
Finally, we examined the relationship between TIMP-2 concentrations in the serum and miR-130b expression in tumor tissues from patients with NSCLC. Enzyme-linked immunosorbent assays (ELISAs) showed that TIMP-2 concentrations in the serum of patients with NSCLC were significantly lower in patients with stage II/III cancer than in patients with stage I cancer (Fig. 5A). Although no significant relationship was observed between the presence or absence of lymphatic invasion or pleura cancer cell invasion (Fig. 5C,D), TIMP-2 concentrations were significantly lower in serum from patients with NSCLC with vascular invasion of tumor cells than in those patients without invasion (Fig. 5B). Importantly, an inverse correlation was observed between TIMP-2 concentrations in serum and miR-130b expression levels in tumor tissues of the same patients with NSCLC (r = −0.3081, p = 0.0248; Fig. 5E). Moreover, the TIMP-2 concentrations were significantly higher in the sera of patients after operation than before operation (Fig. 5F).
TIMP-2 concentrations in serum were inversely correlated with miR-130b expression levels in tumor tissues from patients with NSCLC. Serum concentrations of TIMP-2 were compared according to tumor stage (A), with or without vascular (B), lymphatic (C), and pleura cancer cell invasion (D). (E) Correlations between TIMP-2 concentrations in serum and relative miR-130b expression in tumor tissues of patients with NSCLC were evaluated. (F) TIMP-2 concentration in serum was compared before or after operation. Data are means ± standard deviations. *p < 0.05 and **p < 0.01 for t-tests.
Discussion
In the present study, based on the significant correlation between high miR-130b expression and poor overall survival in patients with NSCLC, we demonstrated that miR-130b increased invasion activity by directly targeting TIMP-2 not only in adenocarcinoma cells but also in squamous cell carcinoma cells using loss-of function and gain-of function experiments. Moreover, we showed that miR-130b expression levels in tumor tissues and TIMP-2 concentrations in serum from the same patients were inversely correlated.
In this study, we found that TIMP-2 was a target of miR-130b using Ago2-IP assays, gene array analysis, and target prediction algorithms. TIMP-2 is a member of the TIMP family and functions as an inhibitor of MMP24. TIMP-2 characteristically inhibits MMP-2 activation by forming a complex with pro-MMP-2. Under normal physiological conditions, the expression of TIMP-2 is strictly controlled and prevents excessive extracellular matrix reorganisation by MMP-225. Conversely, in cancer tissues, including NSCLC, the expression of TIMP-2 is constantly low, thereby promoting the invasion of cancer cells26,27. Our data also indicated that the high expression of miR-130b activated MMP-2 by downregulating TIMP-2, leading to invasion of NSCLC cells in vitro.
Vascular invasion of lung cancer cells is often observed in low-stage tumors in patients with NSCLC28. Although metastasis via the lymphatic route usually takes a longer time for establishment of distant metastasis, tumor cell spreading via blood vessels occurs early during the metastatic process29. Our data showed that high expression of miR-130b was significantly upregulated in tumor tissues with vascular cancer cell invasion in patients with NSCLC. Moreover, a 3D gel invasion assay using primary cultured NSCLC cells revealed upregulated invasion activity when miR-130b expression was high (Fig. 2D). Therefore, high miR-130b expression may function to promote metastasis via targeting TIMP-2 expression and subsequent upregulation of the active form of MMP-2 during the early stages of NSCLC.
Increased TIMP-2 levels in tumor tissues are correlated with a favourable prognosis in patients with NSCLC30. TIMP-2 has various functions in addition to MMP-2 inhibition31. For example, TIMP-2 inhibits proliferation, migration, and angiogenesis of endothelial cells32,33,34,35. Moreover, TIMP-2 suppresses vascular permeability via the integrin α3β1/Shp-1/cAMP/protein kinase A pathway independently of MMP inhibition in human vascular endothelial cells36. Therefore, elevated miR-130b expression may increase the permeability of surrounding vascular endothelial cells via downregulation of TIMP-2 levels in the tumor microenvironment, leading to subsequent tumor cell intravasation in NSCLC. Furthermore, decreased TIMP-2 expression was shown to increase myeloid-derived suppressor cells in an A549 cell xenograft mouse model37. Therefore, high expression of miR-130b may affect the overall survival of patients with NSCLC by targeting TIMP-2, which in turn promotes cancer cell invasion and enhances the functions of endothelial cells and myeloid-derived suppressor cells in tumor tissues.
Our Ago2-IP analysis revealed over 300 candidate target genes of miR-130b, including phosphatase and tensin homolog deleted on chromosome 10 and FRZB (Supplementary Table 1). These genes have potential miR-130b binding sites within their 3′-UTRs. In our previous work, we reported that miR-130b promotes cell migration by targeting phosphatase and tensin homolog deleted on chromosome 10 in bladder cancer cells22. Frizzled-related protein, which functions as an antagonist of the Wnt pathway, exerts inhibitory effects on the epithelial-mesenchymal transition or migration activity in several cancers, including lung cancer38,39. Because miR-130b slightly promoted cell migration in A549 cells (Supplementary Fig. 3C), miR-130b may affect migration activity by targeting these genes in NSCLC cells. Recently, Tian et al. reported that miR-130b inhibition induces apoptosis in NSCLC cells via a peroxisome proliferator-activated receptor-γ/vascular endothelial growth factor A/BCL-2-mediated pathway40. Therefore, miR-130b may enhance the aggressiveness of lung cancer cells via targeting TIMP-2 or some other molecules in NSCLC cells.
SP1, which is reported as a transcriptional activator of TIMP-2 gene in breast cancer, was also found as a candidate target gene of miR-130b (Supplementary Table 1)41,42. Although miR-130b mimic nor inhibitor had no significant effect on TIMP2 expression at the mRNA level in NSCLC cells, miR-130b might affect TIMP-2 expression at the transcriptional level via targeting Sp1 transcriptional factor in other types of cancer such as breast cancer.
In summary, we demonstrated that TIMP-2 was an important target molecule of miR-130b in vitro and in clinical tumor tissues and serum samples from patients with NSCLC. High expression of miR-130b downregulated TIMP-2 expression and enhanced MMP-2 activity to promote the invasion of NSCLC cells. These findings indicated that miR-130b functioned as an oncogenic miRNA in NSCLC and could therefore facilitate the development of molecular-targeted therapeutic drugs for NSCLC.
Materials and Methods
Analysis of TCGA miRNA expression data
Clinical information and RNA-sequencing data for the miR-130 family in patients with adenocarcinoma (n = 122) and squamous cell carcinoma (n = 113) were obtained from TCGA database. Survival analysis was conducted by dividing patients into high (copy number: 1) and low (copy number: −1) groups based on miR-130b, miR-301a, and miR-301b expression. Overall survival rates for these two groups were evaluated by log-rank tests. The clinical information is presented in Table 2 (adenocarcinoma) and Supplementary Table 3 (squamous cell carcinoma).
Clinical specimens
Specimens of NSCLC tissues and adjacent noncancerous tissues were obtained from patients who had undergone primary curative resection of lung tumors at Kagoshima University Hospital (Japan). All enrolled patients were diagnosed by pathological examination and staged by specialised oncologists via the 7th edition of the International Association for the Study of Lung Cancer TNM Classification. Prior written informed consent was obtained from all patients at Kagoshima University Hospital, and the methods were carried out in accordance with approved guidelines. Experiments using clinical specimens were approved by the institutional review boards of Kagoshima University Hospital and the Graduate School of Pharmaceutical Sciences, Osaka University. Clinical and histopathological data related to the clinical specimens are presented in Tables 1, 2 and 3.
RNA extraction
Clinical tissue samples were immediately immersed in RNAlater (Qiagen, Valencia, CA, USA) after operation and stored at −80 °C until RNA extraction. miRNAs were purified from NSCLC or adjacent normal tissue samples using an miRNeasy mini kit (Qiagen). For cell line experiments, total RNA was isolated using TRIzol reagent (Thermo Fisher Scientific, MA, USA) according to the manufacturer’s instructions.
Real-time qPCR
cDNA was synthesised from total RNA (500 ng) in a 10-μl reaction volume using a PrimeScript RT-PCR Kit (TaKaRa, USA). Thermal cycling conditions included an initial step at 98 °C for 30 s, followed by 40 cycles at 95 °C for 5 s and 60 °C for 20 s. The following primers were used: MMP-2 forward, 5′-GATAACCTGGATGCCGTCGTG-3′; MMP-2 reverse, 5′-CAGCCTAGCCAGTCGGATTTG-3′; TIMP-2 forward, 5′-TACCAGATGGGCTGCGAGTG-3′; TIMP-2 reverse, 5′-CTGTGACCCAGTCCATCCAGAG-3′; and GAPDH forward, 5′-CCATCACCATCTTCCAGGAG-3′; GAPDH reverse, 5′-CCTGCTTCACCACCTTCTTG-3′.
The relative expression levels of mRNA were analysed using the 2−ΔΔCt method. For miRNA analysis, cDNA was synthesised using a miR-X miRNA first-strand synthesis kit (TaKaRa, Japan). Thermal cycling conditions included an initial step at 98 °C for 30 s, followed by 40 cycles at 95 °C for 2 s and 63 °C for 5 s. The following primers were used: miR-130b primer, 5′-CAGTGCAATGATGAAAGGGCAT-3′; mRQ 3′ primer (TaKaRa); and U6 snRNA-specific primer (TaKaRa) as an internal control.
Cell culture
A549 human lung cancer cells were maintained in Dulbecco’s modified Eagle’s medium (Wako, Japan) with 10% foetal bovine serum (FBS) and 100 mg/mL kanamycin. NCI-H520, NCI-H1755, NCI-H1975, 5637 and primary NSCLC cell lines were cultured in RPMI 1640 (Wako) with 10% FBS and 100 mg/mL kanamycin. HPL1D human lung epithelial cells were maintained in Ham’s F12 medium containing 10% FBS and 100 mg/mL kanamycin. Cells were cultured in an incubator at 37 °C in an atmosphere containing 5% CO2. A549 cells were purchased from Riken Cell Bank (Japan); NCI-H520, NCI-H1755, and NCI-H1975 cells were purchased from American Type Culture Collection (Manassas, VA, USA); and HPL1D and 5637 cells were kindly provided by the Department of Molecular Carcinogenesis, Nagoya University (Japan) and the Department of Urology, Osaka University (Japan), respectively.
Plasmid construction
To construct TIMP-2 reporter plasmids, the following oligonucleotides were used:
human TIMP-2 3′-UTR oligo sense, 5′-CTAGCGGCCGCTAGTCCCTTGGTAGGTATTAGACTTGCACTTG-3′; human TIMP-2 3′-UTR oligo antisense, 5′-TCGACAAGTGCAAGTCTAATACCTACCAAGGGACTAGCGGCCGCTAGAGCT-3′; mutated TIMP-2 3′-UTR oligo sense, 5′-CTAGCGGCCGCTAGTCCCAACGTTGGATATTGACAACGTCACG-3′; and mutated TIMP-2 3′-UTR oligo antisense, 5′-TCGACGTGACGTTGTCAATATCCAACGTTGGGACTAGCGGCCGCTAGAGCT-3′. The annealed products were digested with SacI and SalI and inserted into a pmirGLO dual-luciferase miRNA target expression vector (Promega, Madison, WI, USA). The primary hsa-miR-130b and the coding domain sequence of TIMP-2 were cloned from genomic DNA of 5637 cells and HPL1D cells, respectively, by PCR using KOD-FX (TOYOBO, Japan) and the following oligonucleotide primers: pri-hsa-miR-130b forward, 5′-TCGAAAGCTTTACCCAATTCGCTCCCTTCT-3′; pri-hsa-miR-130b reverse, 5′-TCGAGGATCCCACCCACCTGATCCTCTGAT-3′; hsa-TIMP-2 forward, 5′-CGGAAGCTTATGGGCGCCGCGGCC-3′; and hsa-TIMP-2 reverse, 5′-GGAGGCTCGAGTTATGGGTCCTCGATGTCG-3′. The PCR products were digested with HindIII and BamHI (hsa-miR-130b) or HindIII and XhoI (TIMP-2) and inserted into the pmR-ZsGreen1 miRNA expression vector (pmR-ZsGreen1/hsa-miR-130b) or pcDNA3.0 expression vector (pcDNA3.0/TIMP-2), respectively.
Establishment of A549 cell clones with stable miR-130b overexpression
The pmR-ZsGreen1/pri-hsa-miR-130b vector was transfected into A549 cells seeded at 3 × 104 cells/well in a 12-well plate using Lipofectamine 3000 (Invitrogen). At 24 h after transfection, culture medium was changed to new medium containing 1 mg/ml geneticin (Wako) to select transfected cells. The selected cells were subjected to a limited dilution method in 96-well plates (0.7 cells/well) to obtain a single colony. ZsGreen1-positive colonies were subjected to miRNA purification and then real-time qPCR to confirm the expression of miR-130b.
Cell invasion assay
A tumor invasion assay system with an 8.0-μm pore size FluoroBlok membrane (Corning, NY, USA) was used to analyse cell invasion in A549 and NCI-H1755 cells. The cells were reseeded into inserts in 96-well plates (1.25 × 104 cells/well) in serum-free conditions 24 h after transfection, and DMEM or RPMI1640 medium containing 10% FBS was added as a chemo-attractant in the base plate. A549 and NCI-H1755 cells were incubated for 20 and 48 h, respectively, at 37 °C in an atmosphere containing 5% CO2. After incubation, the cells were labelled with 4 μg/mL calcein AM (Dojindo, Japan), and the fluorescence intensity of the invaded cells was measured at wavelengths of 494/517 nm (excitation/emission) using an EnVision Multilabel Reader (PerkinElmer, USA).
3D invasion assay using primary NSCLC cells
We prepared neural stem/progenitor cells (NSC) medium containing DMEM/Ham’s F-12 (Wako), B-27TM Supplement (Thermo Fisher), fibroblast growth factor human recombinant animal-derived free (Wako), heparin sulfate sodium salt from bovine kidney (Sigma Aldrich) and antibiotic-antimycotic (Thermo Fisher). Primary cultured NSCLC cells were seeded into Nunclon Sphera 96U-well plates (2000 cells/well) and cultured for 48 h. Half of the medium was replaced with NSC medium containing Matrigel and then incubated for 72 h at 37 °C in an atmosphere containing 5% CO2. Images were acquired at 72 h after the medium change using an OLYMPUS IX71 fluorescence microscope (Tokyo, Japan).
Gelatine zymography
A549 cells were incubated at 37 °C in an atmosphere containing 5% CO2 in Dulbecco’s modified Eagle’s medium without foetal calf serum or antibiotics for 48 h. After incubation, conditioned medium was collected and concentrated using Amicon Ultra filters (Millipore, USA). Samples were mixed with Laemmli sodium dodecyl sulfate sample buffer without 2-mercaptoethanol and separated on 10% gelatine-containing gels. The gels were incubated in zymogram renaturing buffer (Invitrogen) at room temperature for 30 min and then in zymogram development buffer (Invitrogen) at 37 °C overnight. Gels were then washing and staining with Coomassie blue. Densitometric analysis was performed using NIH ImageJ software.
Western blot analysis
Whole-cell lysates were separated by sodium dodecyl sulfate-polyacrylamide gel electrophoresis and then transferred to polyvinylidene difluoride membranes (Millipore) using a semidry transfer system (Bio-Rad, Hercules, CA, USA). The membranes were probed with specific antibodies and then incubated with horseradish peroxidase-conjugated antibodies against mouse or rabbit immunoglobulin (Santa Cruz Biotechnology, Santa Cruz, CA, USA), followed by detection with enhanced chemiluminescence western blotting detection reagent (GE Healthcare, IL USA). An ImageQuant LAS4000 mini system (GE Healthcare) was used as a chemiluminescence detector. The following antibodies were used in this study: anti-TIMP-2 (1:1000; cat. no. SAB1400279; Sigma-Aldrich, St. Louis, MO, USA), anti-MMP-2 (1:2000; cat. no. 13132; Cell Signaling Technology, Danvers, MA, USA), and anti-β-actin (polyclonal; 1:50000; cat. no. A5316; Sigma-Aldrich). Densitometric analysis was performed using NIH Image J software.
Dual-luciferase assay
A pmirGLO dual-luciferase miRNA target expression vector was used for luciferase reporter assays (Promega). A549 cells were transfected with the reporter vector containing the predicted miR-130b binding site or mutated miR-130b binding site in the TIMP-2 3′-UTR (Supplementary Fig. 4B). After transfection for 24 h, dual-luciferase reporter assays were performed using a luminometer (Turner Biosystems 20/20 luminometer; Promega) according to the manufacturer’s protocol.
Transfection
MiRIDIAN miRNA mimic for hsa-miR-130b-3p (C-300660-05-000), miRNA mimic negative control (CN-001000-01-05), miRIDIAN miRNA hairpin inhibitor for hsa-miR-130b-3p (IH-300660-07-0005), and miRNA hairpin inhibitor negative control (IN-001005-01-05) were purchased from GE Healthcare. The miRNA mimic and the hairpin inhibitor were transfected at a concentration of 50 nM using Lipofectamine 3000 (Invitrogen). These transfection experiments were performed according to the protocol supplied by the manufacturer.
ELISA
A human TIMP-2 ELISA kit (Sigma-Aldrich) was used to detect TIMP-2 levels in the serum of patients with NSCLC according to the manufacturer’s protocol. Serum from patients with NSCLC was diluted 2000-fold before use, and colour intensity was measured at 450 nm using an Envision Multilabel Reader (PerkinElmer, MA, USA). Clinical information of specimens used for ELISA is presented in Table 3.
Statistics
F-test was preliminarily performed for verifying equality of variance. For all the other experiments, results were expressed as the mean ± standard deviation of the mean (S.D.) or median. Differences between values were statistically analysed using Student’s t-tests or one-way analysis of variance with Bonferroni post-hoc tests as appropriate (GraphPad Prism 5.0; GraphPad, USA). Differences with p values of less than 0.05 were considered statistically significant.
References
Chen, Z. et al. Non-small-cell lung cancers: a heterogeneous set of diseases. Nat Rev Cancer. 14, 535–46 (2014).
Herbst, R. S., Morgensztern, D. & Boshoff, C. The biology and management of non-small cell lung cancer. Nature. 553, 446–54 (2018).
Brugger, W. & Thomas, M. EGFR-TKI resistant non-small cell lung cancer (NSCLC): new developments and implications for future treatment. Lung Cancer. 77, 2–8 (2012).
Brahmer, J. et al. Nivolumab versus Docetaxel in advanced squamous-cell non-small-cell lung cancer. N Engl J Med. 373, 1627–39 (2015).
Zappa, C. & Mousa, S. A. Non-small cell lung cancer: current treatment and future advances. Transl Lung Cancer Res. 5, 288–300 (2016).
Friedl, P. & Wolf, K. Tumour-cell invasion and migration: Diversity and escape mechanisms. Nat Rev Cancer. 3, 362–74 (2003).
Friedl, P. & Alexander, S. Cancer invasion and the microenvironment: Plasticity and reciprocity. Cell. 147, 992–1009 (2011).
Page-mccaw, A., Ewald, A. J. & Werb, Z. Matrix metalloproteinases and the regulation of tissue remodelling. Nat Rev Mol Cell Biol. 8, 221–33 (2007).
Xu, X. et al. Matrix metalloproteinase-2 contributes to cancer cell migration on collagen. Cancer Res. 65, 130–6 (2005).
Liabakk, N. et al. Matrix metalloprotease 2 (MMP-2) and matrix metalloprotease 9 (MMP-9) type IV collagenases in colorectal cancer. Cancer Res. 56, 190–6 (1996).
Mori, M. et al. Analysis of MT1-MMP and MMP-2 expression in human gastric cancers. Int J Cancer. 74, 316–21 (1997).
Passlick, B. et al. Overexpression of matrix metalloproteinase 2 predicts unfavorable outcome in early-stage non-small cell lung cancer. Clin Cancer Res. 6, 3944–8 (2000).
Qian, Q. et al. The role of matrix metalloproteinase 2 on the survival of patients with non-small cell lung cancer: a systematic review with meta-analysis. Cancer Invest. 28, 661–9 (2010).
Alaseem, A. et al. Matrix Metalloproteinases: A challenging paradigm of cancer management. Semin. Cancer Biol. e-pub ahead of print 16 Nov 2017, https://doi.org/10.1016/j.semcancer.11.008 (2017).
Hernandez-Barrantes, S., Bernardo, M., Toth, M. & Fridman, R. Regulation of membrane type-matrix metalloproteinases. Semin Cancer Biol 12, 131–8 (2002).
Ha, M. & Kim, V. N. Regulation of microRNA biogenesis. Nat Rev Mol Cell Biol. 15, 509–24 (2014).
Reddy, K. B. MicroRNA (miRNA) in cancer. Cancer Cell Int. 15, 38 (2015).
Hayes, J., Peruzzi, P. P. & Lawler, S. MicroRNAs in cancer: biomarkers, functions and therapy. Trends Mol Med. 20, 460–9 (2014).
Bartel, D. P. MicroRNAs: Target Recognition and Regulatory Functions. Cell. 136, 215–33 (2009).
Friedman, R. C., Farh, K. K. H., Burge, C. B. & Bartel, D. P. Most mammalian mRNAs are conserved targets of microRNAs. Genome Res. 19, 92–105 (2009).
Esquela-Kerscher, A. & Slack, F. J. Oncomirs-microRNAs with a role in cancer. Nat Rev Cancer. 6, 259–69 (2006).
Egawa, H. et al. The miR-130 family promotes cell migration and invasion in bladder cancer through FAK and Akt phosphorylation by regulating PTEN. Sci Rep. 6, 20574 (2016).
Egawa, H. et al. Pharmacological regulation of bladder cancer by miR-130 family seed-targeting LNA. Integr Mol Med. 3, 457–63 (2016).
Stetler-Stevenson, W. G. & Gavil, N. V. Normalization of the tumor microenvironment: evidence for tissue inhibitor of metalloproteinase-2 as a cancer therapeutic. Connect Tissue Res. 55, 13–9 (2014).
Bernardo, M. M. & Fridman, R. TIMP-2 (tissue inhibitor of metalloproteinase-2) regulates MMP-2 (matrix metalloproteinase-2) activity in the extracellular environment after pro-MMP-2 activation by MT1 (membrane type 1)-MMP. Biochem J. 374, 739–45 (2003).
Wang, H. et al. MicroRNA-15b promotes proliferation and invasion of non-small cell lung carcinoma cells by directly targeting TIMP2. Oncol Rep. 37, 3305–12 (2017).
Bourboulia, D., Han, H. & Jensen-Taubman, S. TIMP-2 modulates cancer cell transcriptional profile and enhances E-cadherin/beta-catenin complex expression in A549 lung cancer cells. Oncotarget. 4, 166–76 (2013).
Popper, H. H. Progression and metastasis of lung cancer. Cancer Metastasis Rev. 35, 75–91 (2016).
Gabor, S. et al. Invasion of blood vessels as significant prognostic factor in radically resected T1-3N0M0 non-small-cell lung cancer. Eur J Cardiothorac Surg. 25, 439–42 (2004).
Sawabata, N. Prognosis of lung cancer patients in Japan according to data from the Japanese Joint Committee of Lung Cancer Registry. Respir Investig. 52, 317–21 (2014).
Stetler-Stevenson, W. G. Tissue inhibitors of metalloproteinases in cell signaling: metalloproteinase-independent biological activities. Sci Signal. 1, 6 (2008).
Oh, J. et al. Tissue inhibitors of metalloproteinase 2 inhibits endothelial cell migration through increased expression of RECK. Cancer Res. 64, 9062–9 (2004).
Seo, D. W. et al. TIMP-2 mediated inhibition of angiogenesis. Cell. 114, 171–80 (2003).
Martin-Belmonte, F. & Perez-Moreno, M. Epithelial cell polarity, stem cells and cancer. Nat Rev Cancer. 12, 23–38 (2011).
Zhu, L. et al. Prognostic value of tissue inhibitor of metalloproteinase-2 expression in patients with non-small cell lung cancer: a systematic review and meta-analysis. PLoS One 10, e0124230 (2015).
Kim, S. H. et al. Antagonism of VEGF-A – induced increase in vascular permeability by an integrin α3β1-Shp-1-cAMP/PKA pathway. Blood. 120, 4892–902 (2012).
Guedez, L. et al. TIMP-2 targets tumor associated-myeloid suppressor cells with effects in cancer immune dysfunction and angiogenesis. J Immunother. 35, 502–12 (2012).
Ren, J. et al. sFRP1 inhibits epithelial-mesenchymal transition in A549 human lung adenocarcinoma cell line. Cancer Biother Radiopharm. 28, 565–71 (2013).
Kaur, P. et al. Epigenetic silencing of sFRP1 activates the canonical Wnt pathway and contributes to increased cell growth and proliferation in hepatocellular carcinoma. Tumor Biol. 33, 325–36 (2012).
Tian, J. et al. MicroRNA-130b promotes lung cancer progression via PPARγ/VEGF-A/BCL-2-mediated suppression of apoptosis. J Exp Clin Cancer Res. 35, 105 (2016).
Zhong, Z. D. et al. NF-Y and Sp1 cooperate for the transcriptional activation and cAMP response of human tissue inhibitor of metalloproteinases-2. J Biol Chem. 24, 18602–10 (2000).
De Clerck, Y. A. et al. Characterization of the promoter of the gene encoding human tissue inhibitor of metalloproteinases-2 (TIMP-2). Gene. 2, 185–91 (1994).
Acknowledgements
This study was partially supported by Platform Project for Supporting Drug Discovery and Life Science Research (Basis for Supporting Innovative Drug Discovery and Life Science Research (BINDS)) from AMED under Grant Number JP18am0101084.
Author information
Authors and Affiliations
Contributions
Conception and design: T.H., K.T. Development of methodology: T.H., K.K., H.E., Y.U., K.K., K.T. Acquisition of data: T.H., K.J., T.N., M.S., K.M., M.A., A.T., T.U., H.E., Y.N., K.K., Y.U., H.H., M.Y., Y.S., K.K., T.F., K.T. Analysis and interpretation of data: T.H., K.J., H.E., Y.N., K.K., Y.U., H.H., K.T. Writing, review and/or revision of the manuscript: T.H., K.J., T.N., M.S., K.M., M.A., A.T., T.U., H.E., Y.N., K.K., Y.U., H.H., M.Y., Y.S., K.K., T.F., K.T.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hirono, T., Jingushi, K., Nagata, T. et al. MicroRNA-130b functions as an oncomiRNA in non-small cell lung cancer by targeting tissue inhibitor of metalloproteinase-2. Sci Rep 9, 6956 (2019). https://doi.org/10.1038/s41598-019-43355-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-43355-8
This article is cited by
-
Construction of miRNA–mRNA networks for the identification of lung cancer biomarkers in liquid biopsies
Clinical and Translational Oncology (2022)
-
APE1 controls DICER1 expression in NSCLC through miR-33a and miR-130b
Cellular and Molecular Life Sciences (2022)
-
ALKBH4 promotes tumourigenesis with a poor prognosis in non-small-cell lung cancer
Scientific Reports (2021)
-
LncRNA KCNQ1OT1 promotes cell proliferation, migration and invasion via regulating miR-129-5p/JAG1 axis in non-small cell lung cancer
Cancer Cell International (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.