Abstract
Avian pathogenic Escherichia coli (APEC), collectively known as causative agent of extraintestinal infections, is an important cause of morbidity and mortality in poultry. Currently, quorum sensing (QS), biofilm formation and virulence factors are considered as novel prospective targets for antimicrobial therapy to control APEC invasion. In addition, inflammatory responses are also served as the major pathological features of APEC invasion. This study was aimed to explore the effect of baicalin on APEC and APEC-induced inflammatory responses. After treatment with baicalin, we mainly examined the AI-2 secretion, biofilm formation, expression of virulence genes of APEC, and the levels of inflammatory cytokines, as well as the expression of NF-κB pathway. Our results showed that baicalin significantly inhibited the QS via decreasing the AI-2 secretion, biofilm formation, and the expression of virulence genes of APEC such as LsrB, LsrK, LuxS, pfs, H-NS, fimA, fimB, fyuA, csgA, csgB, and rpoS. Moreover, baicalin significantly attenuated the release of lactate dehydrogenase (LDH), and the adhesion of APEC to chicken type II pneumocytes to reduce cell damage. Furthermore, baicalin also inhibited the expression of pro-inflammatory cytokines and NF-κB activation. Thus, our data revealed that baicalin could interfere with the quorum sensing, biofilm formation and virulence genes expression to relieve the APEC pathogenicity. Additionally, baicalin decreased the inflammatory responses of chicken type II pneumocytes induced by APEC. Taken together, these data provide a novel potential pharmaco-therapeutic approach to chicken colibacillosis.
Similar content being viewed by others
Introduction
Chicken colibacillosis, as one of the principal causes of morbidity and mortality in poultry worldwide, is characterized by multiple organ lesions such as air sacculitispericarditis, peritonitis, salpingitis, synovitis, osteomyelitis or yolk sac infection, and caused by a group of pathogens designated avian pathogenic Escherichia coli (APEC)1,2. Quorum sensing (QS) is a widespread signaling system that controls the responses of bacterial populations to cell density, consisting of signal molecules (autoinducers), signal synthases, and signal receptors3. The signal molecules mainly includes autoinducer 1 (AI-1) and autoinducer 2 (AI-2). Of which, the AI-2 QS system is widely present in most gram-negative and gram-positive bacteria and has been proved to regulate the gene expression and physiological behaviors of bacteria in either intraspecies or interspecies communication4. The pathogenicity of APEC is also regulated by QS systems, and AI-2 regulates the expression of genes involved in various processes, including secretion of virulence factors, biofilm formation, motility, genetic competence, sporulation, and antibiotic production5,6. APEC has plentiful virulence factors, including QS signal molecule synthesis genes (LuxS and pfs), transported and phosphorylated genes(LsrB and LsrK), bacterial survival stress related genes (rpos and H-NS), iron uptaking related genes (IucD and fyuA), type 1 pili (fimA and fimB), and curly pili A (csgA and csgB)7. Han has reported the luxS mutant of APEC showed a reduced bacterial mortility and decreased mRNA levels of the virulence-related genes8. Some findings have suggested that the identified AI-2 inhibitors possess anti-biofilm effects against APEC- O78 likely through the down-regulation of genes associated with adhesion, motility, and capsule synthesis among others5,9. Meanwhile, the biofilm, surface-associated bacterial communities embedded in an extracellular matrix, protects against host immune reactions or antibiotics, and is a major problem in the context of chronic infection10.
In addition, the inflammatory response is considered to be the first defense line against the pathogenic invasion11. The pathogenic stimulation will lead to the production of a large number of pro-inflammatory cytokines, including TNF-α, IL-1β, and so on. These up-regulated cytokines cause edema, cellular metabolic stress, and tissue necrosis12. IL-1β and IL-6 were significantly increased in mice with sepsis induced by E. coli13 and the mice treated with Lepidium sativum polysaccharides significantly inhibited E. coli-induced inflammation by reducing the circulating levels of TNF-α14.
QS, biofilm formation and virulence factors contribute significantly to the immune evasion and the tolerance to a variety of antimicrobial treatments, and an vital role on inflammatory response after APEC invasion.
The flavonoids have been demonstrated as QS inhibitors to suppress the bacterial cell-cell signaling15,16,17,18,19,20, such as naringenin, kaempferol, quercetin, apigenin, baicalein and so on. Baicalin (Fig. 1), one flavonoid compound extracted from the dried roots of Huangqin, has been proved to possess inhibitory effects on virulence phenotypes regulated by QS in Pseudomonas aeruginosa16. However, whether baicalin could interfere QS in APEC remains unknown. On the other hand, some recent studies have reported that baicalin can alleviates IL-1β-induced inflammatory injury in chondrocytes21, protect against lead-induced renal oxidative damage in mice22, and lessen the liver inflammation caused by lipopolysaccharide in chicken23. In addition, baicalin reduced age-related inflammation through blocking pro-inflammatory NF-κB activation24. Based on this, we investigated the effects of baicalin on QS, biofilm formation, virulence genes expression of APEC and inflammatory responses induced by APEC, aiming to find one new treatment to suppress the chicken colibacillosis.
Material and Methods
Reagents and bacterial strains
Baicalin (purity ≥ 98%) was purchased from Chengdu Must Biotechnology Co., Ltd. (Chengdu, China). Luria-Bertani (LB) medium was obtained from Sigma-Aldrich (St.Louis, MO, USA). Fetal bovine serum (FBS) and DMEM were obtained from Gibco (Invitrogen S.r.l., Milan, Italy). TRIZOL reagent and PrimeScriptTM RT Reagent Kit with gDNA Eraser were purchased from TaKaRa (Da Lian, Liaoning, China). All other chemicals were of reagent grade. Chicken mAb phospho-NF-κB p65 antibodies and chicken mAb Phospho-IκBα were purchased from Sangon Biotech Company (Shanghai, China).
Bacterial strains and growth condition
APEC-O78 strain (CVCC1418) was purchased from Chinese Veterinary Culture Collection Center (CVCC, Beijing, China). The bacteria were grown routinely in LB agar plates and then pick a single colony to LB medium for culturing at 37 °C overnight. The OD600 was monitored with a SynergyTM HT Multi-Mode Microplate Reader (BioTek Instruments, Winooski, VT). Vibrio harveyi BB152 (V. harveyi BB152) (sensor1+ sensor2+) strain was provided by Dr. Han of Shanghai Veterinary Research Institute (CAAS, Shanghai, China), Vibrio harveyi BB170 (V. harveyi BB170) (sensor1− sensor2+) strain was donated by Dr. Ke of College of Ocean & Earth Sciences (Xiamen University, Xiamen, China) and cultivated in modified autoinducer bioassay medium at 30 °C25. E. coli DH5α (engineering E. coli, no pathogenicity) was purchased from Takara Bio Inc.
Determination of the minimum inhibitory concentration (MIC) of baicalin
The MIC of baicalin against APEC-O78 was determined according to the standard Clinical and Laboratory Standards Institute (CLSI) broth microdilution method. Baicalin was initially dissolved in pure dimethyl sulfoxide (DMSO), and diluted in LB broth to result in final concentration of 12.5, 25 and 50 μg/mL. The bacteria solution at an initial turbidity of 0.05 (OD600) were added to the 96-well microtitre plate. Each well contains 50 μL of bacteria and 100 μL of baicalin (final concentrations: 1.5625–100 μg/mL) in LB medium. After 24 h incubation at 37 °C, the OD600 was measured.
Growth curve analysis
To verify whether baicalin influences the growth of APEC-O78 and V. harveyi BB170, the bacterial growth curve was examined after cultivating in the presence of baicalin, and the APEC-O78 or V. harveyi BB170 alone as control. The concentrations of baicalin were selected from 12.5–50 μg/mL. In brief, the APEC-O78 was added into 50 mL of LB medium and V. harveyi BB170 was added into 50 mL of AB medium. Then, baicalin and APEC-O78 or V. harveyi BB170 were co-cultured at 37 °C or 30 °C, and the value of OD600 was measured using a plate reader at 1 h intervals for 7 h.
Assay for AI-2 activity of V. harveyi BB170 and APEC-O78
The AI-2 bioassay was performed as described previously26 with some modifications. After baicalin was co-cultured with APEC-O78 in DMEM at 37 °C for 4 h, cell-free culture fluids were collected by centrifugation at 12,000 × g at 4 °C for 10 min, filtered by 0.22 μm filters and stored at −80 °C until subsequent analysis.
V. harveyi BB170, used as an AI-2 reporter strain, was diluted by 1:5000 in fresh AB medium and then 180 μL of the bacterial culture was mixed with 20 μL of the collected supernatants or diluted baicalin (12.5, 25 and 50 μg/mL). Then incubated in a black flat-bottomed 96-well plate (Corning Costar, Fisher Scientific, Canada) at 30 °C for 4 h. The DH5α supernatant was regarded as negative control and the V. harveyi BB152 supernatant detected as positive control. Bioluminescence was measured via BHP9504 microplate luminescence analyzer (Beijing Hamamatsu Photonics Technology Co., Beijing, China) and experiments were done in triplicate.
Detection of biofilm formation
The biofilm formation was measured by a crystal violet straining method. Briefly, 150 μL of diluted baicalin was transferred to a 96-well microtiter plate with 50 μL bacterium solution (OD600 = 0.05) with incubation at 37 °C for 24 h. Then, the wells were washed gently three times with 200 μL of PBS, fixed with methanol for 15 min and stained with 200 μL of 0.1% crystal violet for 5 min at room temperature. The wells were then washed with 200 μL of sterile water three times and dried at 37 °C for 10 min, 150 μL of 33% glacial acetic acid was added to the wells to dissolve the crystal violet. The total biofilm cells were then measured at 570 nm.
Expression of virulence genes and inflammatory genes
The transcriptional levels of APEC-O78 virulence genes and inflammatory genes of chicken type II pneumocytes were tested using qRT-PCR after incubating with baicalin (12.5, 25 and 50 μg/mL) for 4 h. The RNA was extracted by TRIZOL reagent according to the manufacturer’s instruction, and then 1 μg of RNA was reverse transcribed to cDNA by reverted first strand synthesis kit with oligo (dT) primers (Thermo Scientific, Waltham, MA, USA). The PCR reactions were performed using a 7500 real-time PCR system (Applied Biosystems, Foster, CA) with FastStart SYBR Green PCR Master Mix (Roche, Mannheim, Germany). The rrsG and ACTB gene were served as housekeeping genes and the untreated E. coli and cells as a reference sample. Primers for real-time PCR are listed in Table 1.
Culture of chicken type II pneumocytes
The isolation and culture of chicken type II pneumocytes were performed as described previously11. In brief, the lung tissues of 13-day-old chicken embryos (Jilin Academy of Agricultural Sciences, Changchun, China) were digested by 0.25% trypsin and 0.1% IV collagenase (Invitrogen-Gibco, Grand Island, NY, USA) for 10 min and 15 min, respectively, and then the total cells were attachment cultured for twice. Finally, the unattached cells were collected and diluted with 20% fetal bovine serum (FBS) DMEM to cell count for 2 × 106 cells/mL. Cells were incubated into a 6-well plate for 18 h at 37 °C. The attaching cells on culture dish were chicken type II pneumocytes.
Cell viability assay by MTT
The effect of baicalin on cell viability was evaluated using MTT colorimetric assay. Chicken type II pneumocytes were seeded in a 96-well plate (2 × 106 cells/ml, 100 μL) and were treated with different concentrations of baicalin for 18 h. After treatment with MTT solution for 4 h, the supernatants were removed and the formazan produced was dissolved in 150 μL of DMSO per well. The plate was shaken for 10 min. Finally, resulting absorbance was measured at 570 nm using a Bio-Tek microplate reader (Bio-Tek Instruments Inc., Winooski, VT, USA).
Lactate dehydrogenase (LDH) activity detection
After APEC-O78 infected chicken type II pneumocytes cells for 4 h with baicalin in a 24-well plate, the supernatants were collected after centrifugation at 300 × g for 5 min and 12,000 × g for 10 min. The LDH activity was determined according to the manufacturer’s protocol (Jiancheng Technology Co., Nanjing, China). LDH activity was calculated as follows: LDH activity (U/L) = (Aexp–Acon)/(Asta–Abla) × 0.2 × 1000, where Aexp is the absorbance of test samples, Acon is the absorbance of control samples, Asta standard hole, and Abla of blank wells.
Adhesion assay
Confluent monolayers of chicken type II pneumocytes cells (106 cells/well) were cultured with APEC-O78 suspensions and different concentrations of baicalin to obtain a multiplicity of infection (MOI) of 1:100 in a 6-well plate. The plate was incubated for 4 h at 37 °C and 5% CO2. Monolayers were then washed three times with PBS, then 400 μl of 1% Triton X-100 (Sigma, St. Louis, MO, USA) were added to 6-well plate and co-incubated for 5 min to disrupt the cells. Viable bacterial cells were determined by plating dilutions of the lysates onto agar.
Measurement of cytokine production by ELISA
After treatment with APEC-O78 suspensions and baicalin (12.5, 25, 50 and 100 μg/mL) in 12-well plate, the culture supernatant was collected. Inflammatory cytokines TNF-α, IL-1β and IL-4 were detected using chicken ELISA kits (BPRO, Lengton Bioscience Co., Ltd., Shanghai, China) according to the instructions of the manufacturer. Finally, the absorbance of each sample was determined by a microplate reader and was calculated according to the standard curve.
Western blot assay
Western blotting was used to determine the expression of NF-κB pathway. The cell samples were dissociated by RIPA lysis buffer (Beyotime Biotechnology, Jiangsu, China) supplemented with protease inhibitor mixture (Roche Applied Science, Indianapolis, USA) and centrifuged at 12,000 × g for 15 min at 4 °C. Then, the cell lysates were fractionated on 12% SDS-PAGE and transferred to PVDF membranes. These PVDF membranes were blocked with 5% BSA for 4 h and then incubated with special primary antibody (1:500 dilution) at 4 °C overnight. Afterwards, the membranes were incubated with the corresponding HRP labeled secondary antibodies (1:25,000 dilution) at room temperature for 2 h, and then washed three times using TBST buffer. The immunoreactive proteins were detected using an enhanced chemiluminescence western blotting detection kit. The β-actin protein served as an internal control.
Statistical analysis
All results in this study were evaluated using one-way ANOVA in SPSS 13.0 software (SPSS Inc., Chicago, IL, USA). Data are presented as the means ± standard deviations (SDs) of at least three independent experiments. P values of less than 0.05 were considered statistically significant.
Compliance with Ethical Standards
All the animal researches and facilities were carried out in accordance with the experimental practices and standards. All experiments comply with the manual of the care and use of laboratory animals published by the US National Institutes of Health. All experimental protocols were approved by the Institutional Animal Care and Use Committee of Jilin University (IACUC).
Results
The antibacterial effect of baicalin on APEC-O78
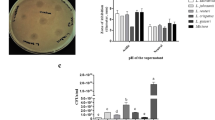
We detected the MIC of baicalin and the growth curve of APEC-O78 to assess the antibacterial effect of baicalin on APEC-O78. As shown in Fig. 2A, baicalin (1.5625–100 μg/mL) had no inhibitory effect on the growth of APEC-O78. Therefore, the MIC of baicalin against APEC-O78 was >100 μg/mL. Furthermore, Fig. 2B,C showed that baicalin (12.5–50 μg/mL) had no effect on the growth curve of APEC-O78 and V. harveyi BB170.
MIC of baicalin against APEC-O78 and growth curve of APEC-O78 and V. harveyi BB170 with baicalin. Baicalin (1.5625–100 μg/mL) incubated with APEC-O78 at 37 °C for 24 h, and then the OD600 was measured. (B) Baicalin (12.5, 25, 50 μg/mL) and APEC-O78 or (C) V. harveyi BB170 co-cultured at 37 °C, and then the value of OD600 of inocula was counted at 1 h intervals for 7 h.
AI-2 Measurement
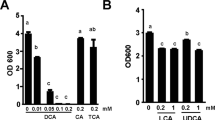
According to the above described measurement condition, the effect of baicalin on AI-2 production of V. harveyi BB170 and APEC was measured. As the Fig. 3A shows, the AI-2 reporter strain V. harveyi BB170, can produce the AI-2 in the process of growth. Baicalin (25 and 50 μg/mL) significantly inhibited the AI-2 production of V. harveyi BB170. Meanwhile, the data revealed that baicalin (12.5, 25 and 50 μg/mL) significantly reduced the AI-2 production compared with APEC in the absence of baicalin (Fig. 3B) and excluded the effect of baicalin on V. harveyi BB170.
Biofilm formation
The inhibition of APEC-O78 biofilm formation by the baicalin was measured using a crystal violet staining method. As a result, all three concentrations of baicalin had good potentials for disrupting APEC-formed biofilm. As shown in Fig. 4, baicalin (12.5, 25 and 50 μg/mL) was able to significantly reduce the biofilm formation.
Expression of virulence genes
The qRT-PCR results (Fig. 5) demonstrates that the related virulence genes (LsrB, LsrK, LuxS, PFS, HNS, fimB, fyuA, csgA, csgB, rpoS) of APEC-O78 were decreased significantly except for the fimA gene after treatment with baicalin (12.5, 25 and 50 μg/mL).
Cytotoxicity of baicalin to chicken type II pneumocytes
Whether baicalin had a toxic effect on chicken type II pneumocytes was analyzed by MTT assay. The results in Fig. 6 showed that baicalin (1.5625–100 μg/mL) had no effect on cell viabilities of chicken type II pneumocytes.
Effect of baicalin on APEC-infected chicken type II pneumocytes
We explored the protective effect of baicalin on APEC-infected chicken type II pneumocytes by examining the count of APEC-O78 adherent on cells and LDH release of APEC-infected cells. The examination of LDH revealed that 12.5–50 μg/mL of baicalin significantly reduced the LDH release of chicken type II pneumocytes infected by APEC-O78 (Fig. 7A). Furthermore, bacterial adhesion assay exhibited that 12.5, 25 and 50 μg/mL of baicalin significantly inhibited the adhesion of APEC-O78 on chicken type II pneumocytes (Fig. 7B).
LDH activity examination and adhesion assay. (A) APEC-infected chicken type II pneumocytes treated with baicalin for 4 h. Then suspension was collected for LDH examination. (B) The supernatants above diluted and viable bacterial cells were determined by plating dilutions of the lysates onto agar. ##p < 0.01 is significantly different from the control group; *p < 0.05 and **p < 0.01 are significantly different from the APEC-O78 group.
Effect of baicalin on APEC-induced inflammatory cytokine production
The levels of inflammatory cytokines TNF-α, IL-1β, and IL-4 were tested by ELISA. As shown in Fig. 8A–C, baicalin significantly inhibited the expression of pro-inflammatory cytokines, TNF-α and IL-1β, and increased the levels of anti-inflammatory cytokines IL-4 induced by APEC-O78. In addition, the gene expression of TNF-α, IL-1β, and IL-4 were consistent with the results of ELISA (Fig. 9A–C).
The Effect of baicalin on APEC-induced inflammatory cytokine production. After the cells exposed to APEC-O78 and baicalin(12.5, 25, 50 μg/mL), extracellular levels of TNF-α (A), IL-1β (B), and IL-4 (C) were measured using ELISA kits. ##p < 0.01 is significantly different from the control group; *p < 0.05 and **p < 0.01 are significantly different from the APEC-O78 group.
The mRNA expression of inflammatory genes after treatment with baicalin. Total RNA was extracted and reverse transcribed to cDNA, the mRNA expression of TNFIP2 (A), IL-1β (B), and IL-4 (C) were detected by qRT-PCR. ##p < 0.01 is significantly different from the control group; *p < 0.05 and **p < 0.01 are significantly different from the APEC-O78 group.
Effect of baicalin on APEC-induced NF-κB signaling pathway
The NF-κB signaling pathway plays an important role in the production of inflammatory cytokines. In order to test the protective mechanism of bacalin on APEC-induced inflammatory response, the expression of NF-κB signaling pathway proteins were tested in the present study. The results showed that the expression of phosphorylated NF-κB p65 and phosphorylated IκB were markedly increased in the APEC-O78 group compared with the control group. However, baicalin significantly inhibited the expression of phosphorylated NF-κB p65 and phosphorylated IκB induced by APEC-O78 (Fig. 10).
Effects of baicalin on NF-κB pathway activation by APEC-O78. Chicken type II pneumocytes were treated with baicalin and infected by APEC for 4 h, and then the protein levels were analyzed by western blotting (A). Finally, the blots were semi-quantified (B,C). ##p < 0.01 is significantly different from the control group; *p < 0.05 and **p < 0.01 are significantly different from the APEC-O78 group.
Discussion
In order to handle with bacterical infections, the effect of baicalin on QS of APEC-O78 and inflammatory response induced by APEC-O78 were tested in the present study. We have demonstrated that baicalin is able to inhibit QS, biofilm formation and the expression of virulence genes. In addition, the results showed that baicalin treatment significantly increased the levels of IL-4, as well as inhibited the levels of TNF-α and IL-1β though suppressing the activation of NF-κB signaling pathway.
QS is adjusted by auto-inducers which are small chemical signals to regulate a wide variety of cellular activities, such as motility, virulence, antibiotic production, biosurfactant formation, and biofilm formation27. AI-2 is produced by the activated methyl cycle by the AI-2 synthase Pfs and LuxS28. LsrB, along with other proteins that form the Lsr transport system, acts as the substrate binding protein of an ATP binding cassette (ABC) transport system responsible for AI-2 internalization. Once inside the cell, AI-2 is phosphorylated by the kinase LsrK29. It has been reported that the AI-2 secretion influences the rpoS and H-NS expression when the bacteria encounter different environment stress30. RpoS and H-NS control the expressions of many genes related to cellular responses to a variety of changes of environmental conditions and genes related to biofilm formation31,32,33. In this study, our results showed that baicalin markedly decreased the rpoS and H-NS gene expression and biofilm formation. Hence, in this study, baicalin may reduce the rpoS and H-NS expression of APEC-O78 by inhibiting the AI-2 production. The high pathogenicity of APEC is involved in many virulence factors including adhesion, iron-binding, proteins, antiserum factors, outer membrane proteins, and hemolysis, such as fimA and fimB (type 1 pili), fyuA (iron uptaking), csgA and csgB (curly pili A), and so on8. In the present study, baicalin reduced the fimB, fyuA, csgA and csgB gene expression. The fimB is related in the type 1 fimbriae which are the major bacterial adherence factor to both biotic and abiotic for E. coli. The fyuA, as a structural gene in the core region of the high pathogenicity island, influence the iron uptake capacity of APEC and the expressions of some virulence factors. Tu34 has proved that irp2 and fyuA knockout APEC strain has weakened transcription of virulence genes and capacity to adhere to DF-1 cells. As our data shows, baicalin can effectively suppress the adhesion of APEC-O78 to chicken type II pneumocytes. Therefore, baicalin attenuated the adhesion capacity of APEC-O78 by inhibiting the virulence genes expression. Curli fimbria is known to be associated with bacterial biofilm formation and the UPEC-4 ▵csgA mutant lost its adherence to HTB-9 but continued to adhere to the HUVEC and Vero cells35. The inhibitory effect of baicalin on APEC-O78 biofilm formation and adhesion capacity may be concerned with curli fimbria gene - csgA and csgB. However, this assumption needs more evidence to verify. In this study, baicalin significantly decreased the biofilm formation, AI-2 secretion and virulence genes expression, consistent with the suppression of the LDH release of chicken type II pneumocytes induced by APEC-O78.
The inflammatory response is important for defense against the pathogenic invasion. TNF-α, and IL-1β are the main pro-inflammatory cytokines36. IL-4 and IL-10, on the other hand, are the main anti-inflammatory cytokines and considered to have ability to inhibit the production of pro-inflammatory cytokines37,38. In the APEC-O78 induced inflammatory injury of chicken type II pneumocytes, the expression of TNF-α and IL-1β were increased, and the production of IL-4 and IL-10 were reduced11. Furthermore, the production of pro-inflammatory cytokines is required for the activation of NF-κB signaling pathway activation39,40,41. In the present study, the results showed that baicalin treatment significantly increased the levels of IL-4, as well as inhibited the levels of TNF-α and IL-1β though suppressing the activation of NF-κB signaling pathway induced by APEC-O78 in chicken type II pneumocytes.
In conclusion, baicalin reduced cell damage of APEC-infected chicken type II pneumocytes through interfering with QS, biofilm formation, and the expression of virulence genes. Meanwhile, baicalin inhibited the release of inflammatory cytokines through alleviating the activation of NF-κB signaling pathway induced by APEC-O78. Our study suggested that baicalin may be a potential therapeutic agent for the treatment of APEC induced colibacillosis.
Data Availability
All data generated or analysed during this study are included in this published article (and its Supplementary Information files).
References
Dziva, F. & Stevens, M. P. Colibacillosis in poultry: unravelling the molecular basis of virulence of avian pathogenic Escherichia coli in their natural hosts. Avian pathology: journal of the W.V.P.A 37, 355–366, https://doi.org/10.1080/03079450802216652 (2008).
Ewers, C., Janssen, T., Kiessling, S., Philipp, H. C. & Wieler, L. H. Molecular epidemiology of avian pathogenic Escherichia coli (APEC) isolated from colisepticemia in poultry. Veterinary microbiology 104, 91–101, https://doi.org/10.1016/j.vetmic.2004.09.008 (2004).
Rajkumari, J. et al. Cinnamic acid attenuates quorum sensing associated virulence factors and biofilm formation in Pseudomonas aeruginosa PAO1. Biotechnology letters, https://doi.org/10.1007/s10529-018-2557-9 (2018).
Yu, L. et al. Autoinducer2 affects trimethoprim-sulfamethoxazole susceptibility in avian pathogenic Escherichia coli dependent on the folate synthesis-associate pathway. MicrobiologyOpen, https://doi.org/10.1002/mbo3.582 (2018).
Helmy, Y. A., Deblais, L., Kassem, I. I., Kathayat, D. & Rajashekara, G. Novel small molecule modulators of quorum sensing in avian pathogenic Escherichia coli (APEC). Virulence 9, 1640–1657, https://doi.org/10.1080/21505594.2018.1528844 (2018).
Wang, S. et al. Escherichia coli Type III Secretion System 2 ATPase EivC Is Involved in the Motility and Virulence of Avian Pathogenic Escherichia coli. Frontiers in microbiology 7, 1387, https://doi.org/10.3389/fmicb.2016.01387 (2016).
Peng, L. Y. et al. Rutin inhibits quorum sensing, biofilm formation and virulence genes in avian pathogenic Escherichia coli. Microbial pathogenesis, https://doi.org/10.1016/j.micpath.2018.04.007 (2018).
Han, X. et al. The luxS gene functions in the pathogenesis of avian pathogenic Escherichia coli. Microbial pathogenesis 55, 21–27, https://doi.org/10.1016/j.micpath.2012.09.008 (2013).
Roberts, I. S. The biochemistry and genetics of capsular polysaccharide production in bacteria. Annual review of microbiology 50, 285–315, https://doi.org/10.1146/annurev.micro.50.1.285 (1996).
DePas, W. H. et al. Biofilm formation protects Escherichia coli against killing by Caenorhabditis elegans and Myxococcus xanthus. Applied and environmental microbiology 80, 7079–7087, https://doi.org/10.1128/AEM.02464-14 (2014).
Zhang, L. Y. et al. Astragaloside IV Inhibits the Inflammatory Injury of Chicken Type II Pneumocytes Induced by Avian Pathogenic Escherichia coli. Inflammation 39, 1660–1669, https://doi.org/10.1007/s10753-016-0400-9 (2016).
Ren, G. et al. Inflammatory cytokine-induced intercellular adhesion molecule-1 and vascular cell adhesion molecule-1 in mesenchymal stem cells are critical for immunosuppression. Journal of immunology 184, 2321–2328, https://doi.org/10.4049/jimmunol.0902023 (2010).
Song, K. H. et al. Effects of low-dose irradiation on mice with Escherichia coli-induced sepsis. Toxicology and applied pharmacology 333, 17–25, https://doi.org/10.1016/j.taap.2017.08.008 (2017).
Ahmad, A. et al. Inhibitory effects of Lepidium sativum polysaccharide extracts on TNF-alpha production in Escherichia coli-stimulated mouse. 3 Biotech 8, 286, https://doi.org/10.1007/s13205-018-1309-9 (2018).
Vikram, A., Jayaprakasha, G. K., Jesudhasan, P. R., Pillai, S. D. & Patil, B. S. Suppression of bacterial cell-cell signalling, biofilm formation and type III secretion system by citrus flavonoids. Journal of applied microbiology 109, 515–527, https://doi.org/10.1111/j.1365-2672.2010.04677.x (2010).
Omwenga, E. O., Hensel, A., Shitandi, A. & Goycoolea, F. M. Chitosan nanoencapsulation of flavonoids enhances their quorum sensing and biofilm formation inhibitory activities against an E. coli Top 10 biosensor. Colloid Surface B 164, 125–133, https://doi.org/10.1016/j.colsurfb.2018.01.019 (2018).
Das, A. et al. Antibiofilm activity of Parkia javanica against Pseudomonas aeruginosa: a study with fruit extract. Rsc Adv 7, 5497–5513, https://doi.org/10.1039/c6ra24603f (2017).
Skogman, M. E., Kanerva, S., Manner, S., Vuorela, P. M. & Fallarero, A. Flavones as Quorum Sensing Inhibitors Identified by a Newly Optimized Screening Platform Using Chromobacterium violaceum as Reporter Bacteria. Molecules 21, Artn 121110.3390/Molecules21091211 (2016).
Manner, S. & Fallarero, A. Screening of Natural Product Derivatives Identifies Two Structurally Related Flavonoids as Potent Quorum Sensing Inhibitors against Gram-Negative Bacteria. International journal of molecular sciences 19, Artn 134610.3390/Ijms19051346 (2018).
Luo, J. et al. Baicalin inhibits biofilm formation, attenuates the quorum sensing-controlled virulence and enhances Pseudomonas aeruginosa clearance in a mouse peritoneal implant infection model. Plos One 12, ARTN e017688310.1371/journal.pone.0176883 (2017).
Yang, X., Zhang, Q., Gao, Z., Yu, C. & Zhang, L. Baicalin alleviates IL-1beta-induced inflammatory injury via down-regulating miR-126 in chondrocytes. Biomedicine & pharmacotherapy = Biomedecine & pharmacotherapie 99, 184–190, https://doi.org/10.1016/j.biopha.2018.01.041 (2018).
Zhang, Z. et al. The Protective Effect of Baicalin Against Lead-Induced Renal Oxidative Damage in Mice. Biological trace element research 175, 129–135, https://doi.org/10.1007/s12011-016-0731-2 (2017).
Cheng, P. et al. Baicalin Alleviates Lipopolysaccharide-Induced Liver Inflammation in Chicken by Suppressing TLR4-Mediated NF-kappaB Pathway. Frontiers in pharmacology 8, 547, https://doi.org/10.3389/fphar.2017.00547 (2017).
Lim, H. A. et al. PPARgamma activation by baicalin suppresses NF-kappaB-mediated inflammation in aged rat kidney. Biogerontology 13, 133–145, https://doi.org/10.1007/s10522-011-9361-4 (2012).
Bassler, B. L., Greenberg, E. P. & Stevens, A. M. Cross-species induction of luminescence in the quorum-sensing bacterium Vibrio harveyi. Journal of bacteriology 179, 4043–4045 (1997).
Han, X. G. & Lu, C. P. Detection of autoinducer-2 and analysis of the profile of luxS and pfs transcription in Streptococcus suis serotype 2. Current microbiology 58, 146–152, https://doi.org/10.1007/s00284-008-9291-9 (2009).
Lee, D. J. et al. Analysis of two quorum sensing-deficient isolates of Pseudomonas aeruginosa. Microbial pathogenesis 119, 162–169, https://doi.org/10.1016/j.micpath.2018.04.014 (2018).
Zhang, Y. et al. LsrB-based and temperature-dependent identification of bacterial AI-2 receptor. AMB Express 7, 188, https://doi.org/10.1186/s13568-017-0486-y (2017).
Pereira, C. S., de Regt, A. K., Brito, P. H., Miller, S. T. & Xavier, K. B. Identification of functional LsrB-like autoinducer-2 receptors. Journal of bacteriology 191, 6975–6987, https://doi.org/10.1128/JB.00976-09 (2009).
Patten, C. L., Kirchhof, M. G., Schertzberg, M. R., Morton, R. A. & Schellhorn, H. E. Microarray analysis of RpoS-mediated gene expression in Escherichia coli K-12. Molecular genetics and genomics: MGG 272, 580–591, https://doi.org/10.1007/s00438-004-1089-2 (2004).
Guan, J. et al. Roles of RpoS in Yersinia pseudotuberculosis stress survival, motility, biofilm formation and type VI secretion system expression. Journal of microbiology 53, 633–642, https://doi.org/10.1007/s12275-015-0099-6 (2015).
Wan, B. et al. Global transcriptional regulation by H-NS and its biological influence on the virulence of Enterohemorrhagic Escherichia coli. Gene 588, 115–123, https://doi.org/10.1016/j.gene.2016.05.007 (2016).
Hong, S. H., Wang, X. & Wood, T. K. Controlling biofilm formation, prophage excision and cell death by rewiring global regulator H-NS of Escherichia coli. Microbial biotechnology 3, 344–356, https://doi.org/10.1111/j.1751-7915.2010.00164.x (2010).
Tu, J. et al. The irp2 and fyuA genes in High Pathogenicity Islands are involved in the pathogenesis of infections caused by avian pathogenic Escherichia coli (APEC). Polish journal of veterinary sciences 19, 21–29, https://doi.org/10.1515/pjvs-2016-0004 (2016).
Cordeiro, M. A., Werle, C. H., Milanez, G. P. & Yano, T. Curli fimbria: an Escherichia coli adhesin associated with human cystitis. Brazilian journal of microbiology: publication of the Brazilian Society for Microbiology 47, 414–416, https://doi.org/10.1016/j.bjm.2016.01.024 (2016).
Satoh, H., Firestein, G. S., Billings, P. B., Harris, J. P. & Keithley, E. M. Proinflammatory cytokine expression in the endolymphatic sac during inner ear inflammation. Journal of the Association for Research in Otolaryngology: JARO 4, 139–147 (2003).
Xing, Z., Ohkawara, Y., Jordana, M., Graham, F. L. & Gauldie, J. Adenoviral vector-mediated interleukin-10 expression in vivo: intramuscular gene transfer inhibits cytokine responses in endotoxemia. Gene therapy 4, 140–149, https://doi.org/10.1038/sj.gt.3300371 (1997).
Hurdayal, R. & Brombacher, F. The role of IL-4 and IL-13 in cutaneous Leishmaniasis. Immunol Lett 161, 179–183, https://doi.org/10.1016/j.imlet.2013.12.022 (2014).
Hu, Y. et al. Protective effects of total alkaloids from Dendrobium crepidatum against LPS-induced acute lung injury in mice and its chemical components. Phytochemistry 149, 12–23, https://doi.org/10.1016/j.phytochem.2018.02.006 (2018).
Li, N. et al. Sodium butyrate alleviates LPS-induced acute lung injury in mice via inhibiting HMGB1 release. International immunopharmacology 56, 242–248, https://doi.org/10.1016/j.intimp.2018.01.017 (2018).
Ding, Y. et al. Mechanism of long non-coding RNA MALAT1 in lipopolysaccharide-induced acute kidney injury is mediated by the miR-146a/NF-kappaB signaling pathway. International journal of molecular medicine 41, 446–454, https://doi.org/10.3892/ijmm.2017.3232 (2018).
Acknowledgements
This work was supported by the National Natural Science Foundation of China (No. 31372470) and the Special Fund for Agro-scientific Research in the Public Interest (201403051).
Author information
Authors and Affiliations
Contributions
Lu-Yuan Peng, Ben-Dong Fu and Hai-Qing Shen wrote the main manuscript and analyzed the data. Meng Yuan and Zong-Mei Wu analyzed the partical data. Ke Song, Chun-Lei Zhang, Qiang An, Fang Xia, Jia-Lin Yu and Peng-Fei Yi prepared Figures 2–10.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Peng, LY., Yuan, M., Wu, ZM. et al. Anti-bacterial activity of baicalin against APEC through inhibition of quorum sensing and inflammatory responses. Sci Rep 9, 4063 (2019). https://doi.org/10.1038/s41598-019-40684-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-40684-6
This article is cited by
-
Biofilm-mediated infections by multidrug-resistant microbes: a comprehensive exploration and forward perspectives
Archives of Microbiology (2024)
-
Development of an amoxicillin-radix scutellaria extract formulation and evaluation of its pharmacokinetics in pigs
BMC Veterinary Research (2023)
-
The effects of baicalin on piglets challenged with Glaesserella parasuis
Veterinary Research (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.