Abstract
Sodium butyrate is well-known for its immune-modulatory properties. Studies until now only focused on the in vitro effects of butyrate or assessed local effects in the gut upon butyrate administration. In this trial, we studied the systemic anti-inflammatory effects induced by sodium butyrate supplementation in humans. Nine healthy (Lean) and ten obese (metabolic syndrome group, MetSyn) males were given 4 grams sodium butyrate daily for 4 weeks. PBMCs were isolated before and after supplementation for direct stimulation experiments and induction of trained immunity by oxidized low-density lipoprotein (oxLDL), β-glucan, or Bacillus Calmette-Guérin vaccine (BCG). Butyrate supplementation moderately affected some of the cytokine responses in the MetSyn group. In the direct stimulation setup, effects of butyrate supplementation were limited. Interestingly, butyrate supplementation decreased oxLDL-induced trained immunity in the MetSyn group for LPS-induced IL-6 responses and Pam3CSK4-induced TNF-α responses. Induction of trained immunity by β-glucan was decreased by butyrate in the MetSyn group for Pam3CSK4-induced IL-10 production. In this study, while having only limited effects on the direct stimulation of cytokine production, butyrate supplementation significantly affected trained immunity in monocytes of obese individuals with metabolic complications. Therefore, oral butyrate supplementation may be beneficial in reducing the overall inflammatory status of circulating monocytes in patients with metabolic syndrome.
Similar content being viewed by others
Introduction
The sophisticated symbiosis between humans and colonizing microbes in the gut has been studied intensively during the last decades. Extensive research in the last years has shown that the microbial community living in our gut plays a significant role in maintaining our health. Its main functions include harvesting energy from dietary components, maintaining the intestinal mucosal barrier, and regulating immune responses1,2. One important microbial process that has been linked to all of these functions is represented by the production of short-chain fatty acids (SCFAs), a biological process taking place in the large intestine3.
For the digestion of the complex carbohydrates mainly found in fruit, vegetables and whole grains, we rely on fermentative metabolism by a group of anaerobic gram-positive bacteria in the colon. This process yields energy and SCFAs; mainly acetate, propionate and butyrate. Despite the fact that these metabolites consist of only a few carbon atoms, they have been shown to play a substantial role in health and disease. Butyrate in particular not only constitutes the main source of energy for colonocytes4,5, it has also been the focus of research due to its potent immune-regulating effects. Many studies report inhibition of pro-inflammatory cytokines, NF-κB activation, and nitric oxide production by butyrate in vitro, although the exact effects appear to depend on cell type, stimulus and concentration of butyrate6,7,8,9,10.
Two main mechanisms have been suggested to mediate the effects of butyrate. Firstly, butyrate was reported to be a broad histone deacetylase (HDAC) inhibitor, inhibiting most isoforms of class I and II11,12,13,14. This leads to hyperacetylation of both histone and non-histone proteins such as transcription factors, altering gene expression patterns. Secondly, butyrate binds G protein-coupled receptors 41 and 43, which were later renamed to fatty acid receptors FFA3 and FFA2, respectively. FFA2 is found predominantly on peripheral blood mononuclear cells (PBMCs), monocytes, and neutrophils15,16, but its exact role in regulating the immune system is still a topic of debate. Both protective and detrimental effects of FFA2 are reported in murine models of inflammatory diseases17,18. In addition, it is unknown whether FFA2 is able to directly affect cytokine production or which pathways are involved in this.
The concentrations of butyrate required for HDAC inhibition and FFA2/FFA3 activation both exceed physiological levels in the peripheral blood, but are well within range of butyrate concentrations in the gut12,15,19. We therefore envisage that monocytes can encounter high concentrations of butyrate in the gut and change their inflammatory potential to mediate systemic effects. Previous studies in mice have shown that oral butyrate inhibits cytokine production in peritoneal macrophages20, protects from atherosclerotic lesions in the aorta21, prevents diet-induced obesity, and increases insulin sensitivity and mitochondrial function22. These results suggest that butyrate supplementation may be beneficial for the treatment of metabolic diseases in which exaggerated inflammation plays an important role such as diabetes, atherosclerosis and gout.
Although oral butyrate supplementation in humans has been shown to ameliorate clinical symptoms of inflammatory bowel disease23,24, data on its effects on the inflammatory potential of circulating monocytes are lacking. In the present pilot study, healthy and obese subjects received 4 grams of butyrate daily for 4 weeks. We assessed the effects of butyrate supplementation on the capacity of circulating monocytes to produce innate immune cytokines directly in response to a range of endogenous and pathogenic stimuli. Furthermore, we investigated whether oral butyrate influences the capacity of monocytes to be trained by oxLDL or microbial components to respond more vigorously to a secondary unrelated stimulus, a process described previously as trained innate immunity25,26,27.
Results
Baseline characteristics
Ten lean males and ten obese males were included in the analysis. At baseline, the obese (MetSyn) group was characterized by a higher age, BMI, diastolic blood pressure, fasting plasma glucose, plasma low-density lipoprotein cholesterol, plasma triglycerides, and neutrophils counts, as well as lower plasma high-density lipoprotein cholesterol (Table 1). General data and metabolic syndrome parameters in Table 1 have also been published as baseline characteristics in a previous publication on the same population (Table 1 in28). There is a slight difference with the numbers in the previously published table due to the exclusion of one donor in the other paper28.
Short-chain fatty acid concentrations in plasma and feces
The effects of 4 weeks oral sodium butyrate supplementation were assessed by measuring SCFA levels in the plasma and feces and were compared between volunteers in the Lean and MetSyn group. At baseline, the MetSyn group showed a different composition of plasma SCFA, with a lower percentage of acetate and higher percentages of propionate and butyrate (Table 2) compared to the Lean group. There were no baseline differences in fecal SCFA concentrations between the two groups (Table 3). In contrast, butyrate supplementation affected the fecal SCFA concentrations to a greater extent than plasma levels. Only the plasma propionate concentration was decreased in the MetSyn group after treatment compared to baseline. In feces, total SCFA, acetate, and propionate concentrations were significantly lower after 4-week butyrate supplementation in both the Lean and the MetSyn group. Fecal butyrate concentrations were only significantly decreased after butyrate supplementation in the MetSyn group.
Effects of sodium butyrate treatment on total blood cell counts
To study the possible effects of sodium butyrate supplementation on white blood cell counts, blood differential tests were performed before and after butyrate supplementation. As mentioned above, only neutrophil counts differed significantly at baseline between the lean and obese groups (Table 1). No differences were found in percentages or absolute counts of neutrophils, lymphocytes, or monocytes in whole blood between the time points before and after supplementation (Supplemental Fig. 1).
Cytokine production of circulating peripheral blood mononuclear cells
To assess the effects of oral sodium butyrate supplementation on the cytokine-producing capacity of PBMCs, we stimulated the cells with a range of heat-killed human pathogens. An overall glance on the heatmap (Fig. 1A) representing the mean fold increase or decrease in cytokine production after butyrate supplementation, shows that the differences are mostly small. The following panels in Fig. 1 show the absolute cytokine production of stimuli-cytokine combinations that have a statistically significant effect or show larger effects in the heatmap. Baseline comparison between the groups showed that PBMCs from MetSyn volunteers were only less capable of mounting an IL-6 response to stimulation with Bacteroides fragilis compared to volunteers in the Lean group (Fig. 1B). After 4 weeks of oral butyrate supplementation, PBMCs from MetSyn subjects produced less IL-1β in response to Candida albicans (Fig. 1F) compared to baseline. As shown by the IL-10 production in response to Escheria coli (Fig. 1A,J), there is sometimes large donor variation, causing the heatmap to show somewhat biased differences.
Effects of 4-week butyrate supplementation on PBMC cytokine responses to pathogens. Freshly isolated PBMCs from healthy lean volunteers (Lean) and metabolic syndrome patients (MetSyn) were cultured for 24 hours in the presence of pathogens before and after 4-week supplementation with 4 grams oral butyrate daily. (A) A heatmap shows the mean fold decrease or increase in cytokine production after supplementation in both groups. (B–J) Stimuli-cytokine combinations showing a substantial decrease or increase in panel A are highlighted in separate graphs to show the absolute cytokine values at baseline (BL) and 4 weeks (4 w). Lean n = 9, MetSyn n = 10.
Because gouty arthritis is highly associated with metabolic syndrome, PBMCs were also stimulated with a combination of monosodium urate crystals (MSU) and Toll-like receptor ligands to induce a potent cytokine response. No differences in cytokine production were observed between the Lean and MetSyn groups at baseline (Fig. 2). The heatmap even shows mainly increases in IL-1β and IL-6, and decreases in the anti-inflammatory cytokine IL-1Ra (Fig. 2A). Surprisingly, the IL-1β production in response to a combination of MSU crystals and palmitic acid (C16.0) was significantly increased in the MetSyn group after oral butyrate supplementation (Fig. 2B).
Effects of 4-week butyrate supplementation on PBMC cytokine responses to monosodium urate crystals. Freshly isolated PBMCs from healthy lean volunteers (Lean) and metabolic syndrome patients (MetSyn) were cultured for 24 hours in the presence of monosodium urate crystals in combination with inflammatory stimuli before and after 4-week supplementation with 4 grams oral butyrate daily. (A) A heatmap shows the mean fold decrease or increase in cytokine production after supplementation in both groups. (B–G) Stimuli-cytokine combinations showing a substantial decrease or increase in panel A are highlighted in separate graphs to show the absolute cytokine values at baseline (BL) and 4 weeks (4 w). Lean n = 10, MetSyn n = 7.
Training capacity of innate immune cells
One additional feature of monocytes is their capacity to be trained to produce more cytokines upon secondary stimulation with an unrelated stimulus29. This process is mediated through epigenetic reprogramming and metabolic rewiring of the macrophages and can, among others, be achieved by oxidized low-density lipoprotein (oxLDL), β-glucan, or Bacillus Calmette-Guérin vaccine (BCG)25,26,27,30.
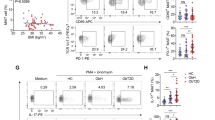
To study the effect of butyrate supplementation on this process, we measured the training capacity of adherent monocytes before and after the 4-week supplementation according to the schedule in Fig. 3. The heatmap (Fig. 4A) shows a few decreases after butyrate production in the MetSyn group. The three strongest specific comparisons (Fig. 4B,E and G) yield statistical significance. After 4 weeks of butyrate supplementation, training induced by β-glucan upon restimulation with Pam3CSK4 was decreased for IL-10 production in the MetSyn group (Fig. 4B). Additionally, monocytes isolated from volunteers in the MetSyn group displayed a decreased training capacity by oxLDL after butyrate supplementation. Upon restimulation with Pam3CSK4, the fold increase in TNF-α production was decreased compared to baseline (Fig. 4E), and upon restimulation with LPS there was a significantly reduced up-regulation of IL-6 (Fig. 4G). There were no differences in baseline training capacity between the Lean and the MetSyn group. In Fig. 5, we show the absolute cytokine responses of the training experiments in which butyrate supplementation had a statistically significant effect. When looking at absolute cytokine levels instead of fold change with training, we observe no significant effects in the IL-10 production after β-glucan training and Pam3CSK4 restimulation (Fig. 5A). However, the TNF-α production upon training with oxLDL and restimulation with Pam3CSK4 is significantly lower compared to the absolute cytokine levels before butyrate supplementation (Fig. 5B). The same is observed with IL-6 production after training with oxLDL and restimulation with LPS (Fig. 5C).
In vitro innate immune training setup. In freshly isolated adherent monocytes from healthy lean volunteers (Lean) and metabolic syndrome patients (MetSyn) training was induced by 24 hour culture with β-glucan, Bacillus Calmette-Guérin vaccine (BCG) or oxidized low-density lipoprotein (oxLDL). The training stimulus was washed out with warm phosphate-buffered saline and cells were rested for 5 days in medium with 10% pooled human serum. On day 6, cells were restimulated with 10 µg/mL Pam3CSK4 or 10 ng/mL E. coli lipopolysaccharide (LPS) for 24 hours, after which supernatant was collected for cytokine ELISAs.
Effects of 4-week butyrate supplementation on monocyte training capacity. In freshly isolated adherent monocytes from healthy lean volunteers (Lean) and metabolic syndrome patients (MetSyn) training was induced as depicted in Fig. 3. This experiment was performed before and after 4-week supplementation with 4 grams oral butyrate daily. (A) A heatmap shows the mean fold decrease or increase in cytokine production with training after supplementation in both groups. (B–G) Stimuli-cytokine combinations showing a substantial decrease or increase in panel A are highlighted in separate graphs to show the fold change with training at baseline (BL) and 4 weeks (4 w). Lean n = 7, MetSyn n = 7.
Effects of 4-week butyrate supplementation on absolute cytokine production in trained monocytes. This figure depicts the absolute cytokine responses in trained monocytes of those experimental setups in Fig. 4 that were significantly affected by butyrate supplementation. (A) shows the IL-10 responses in both groups at baseline (BL) and 4 weeks (4 w) after Pam3CSK4 stimulation with and without β-glucan training. (B) shows the absolute TNF-α responses in both groups after Pam3CSK4 stimulation with and without oxLDL training. (C) shows the IL-6 responses in both groups after LPS stimulation with and without oxLDL training. Time points within one group of volunteers were compared with a Mann-Whitney U-test. Lean n = 7, MetSyn n = 7.
Discussion
In the present study we assessed the effects of 4 weeks oral sodium butyrate supplementation on the inflammatory potential of PBMCs in healthy lean and obese male human volunteers. To our knowledge this is the first clinical trial studying the influence of butyrate supplementation on systemic inflammatory responses in humans.
We show here that in comparison to the potent anti-inflammatory effects of butyrate observed predominantly in in vitro studies, the effects of oral butyrate supplementation on ex vivo cytokine production by PBMCs in this study were limited. Direct stimulation of PBMCs resulted in decreased IL-1β production upon stimulation with Candida albicans conidia, but increased C16.0 + MSU-induced IL-1β after butyrate supplementation in the MetSyn group. This is in contrast to the direct and potent anti-inflammatory effect of butyrate on C16.0 + MSU-induced in vitro cytokine production12. However, in the latter setup relatively high concentrations of butyrate were required to suppress histone deacetylases and the subsequent production of pro-inflammatory cytokines.
More consistent effects were found when assessing the impact of butyrate supplementation on the induction of trained innate immunity. Here, butyrate supplementation decreased oxLDL-induced trained immunity in the MetSyn group for LPS-induced IL-6 responses and Pam3CSK4-induced TNF-α responses. This effect was also seen when looking at absolute cytokine levels instead of training-induced fold increases. In addition, training with β-glucan was decreased for Pam3CSK4-induced IL-10 production. Interestingly, all effects observed after oral butyrate supplementation are limited to the MetSyn group. In the context of metabolic syndrome, especially oxLDL-induced trained innate immunity has been implicated to play a role in the development of atherosclerosis31. Short-term exposure of monocytes to oxLDL was shown to induce long-lasting epigenetic modifications that subsequently lead to a more pro-inflammatory macrophage phenotype27. Therefore, oral butyrate supplementation may be beneficial in preventing oxLDL-induced training of macrophages in patients with metabolic syndrome, possibly slowing down the process of vascular wall inflammation and the development of atherosclerosis.
Within the scope of the current study, we can only speculate on the mechanism of the effects of oral butyrate supplementation on systemic inflammatory responses. Our results suggest that the effects of oral butyrate supplementation are limited when looking at direct cytokine responses, but it may be able to inhibit the induction of trained innate immunity. From previous in vitro work we have seen that high concentrations of butyrate can induce inhibition of class I histone deacetylases, leading to inhibited cytokine production in PBMCs12. Possibly, butyrate concentrations after supplementation are not high enough, or its effects on histone deacetylases do not last long enough to inhibit cytokine responses upon direct stimulation of PBMCs.
The long-lasting effects of trained innate immunity are mediated through epigenetic reprogramming at the level of histone methylation25. Additionally, trained macrophages are characterized by a metabolic shift from mitochondrial oxidative phosphorylation to aerobic glycolysis that is mediated through mammalian target of rapamycin (mTOR) activation26. In contrast, butyrate has been shown to induce mitochondrial respiration and fatty acid oxidation in various in vitro and murine studies4,22,32. Based on this, it can be hypothesized that oral butyrate supplementation leads to high local concentrations of butyrate in the gut, where it can affect cellular metabolism of circulating monocytes, making them less susceptible to training. Furthermore, our observation that only the training capacity of PBMCs from obese males is affected by butyrate supplementation suggests there might be a role for microbiome or diet in this group, or that PBMCs from these subjects are more susceptible to the changes induced by butyrate.
The current study has several limitations. Firstly, this was a pilot study with small numbers in each group, providing only limited power to detect differences in cytokine production as these already show high variability among donors. Secondly, we were unable to detect any increases in butyrate concentration in the feces or plasma after 4 weeks of supplementation. Most likely, this is because butyrate is very quickly utilized as an energy source by colonocytes. With only an estimated 5% of SCFAs being excreted through feces33 and almost all of them present in circulation being metabolized by the liver34, neither plasma nor fecal SCFA concentration are a good measure of the transiently increased SCFA concentrations in the gut. In a recent paper, Canfora et al. shows that the increase in plasma butyrate concentration after colonic administration of sodium butyrate is very quick and already undetectable at 2 hours after colonic infusion35. The 4 weeks of butyrate supplementation did not lead to a stable increase in plasma SCFA levels, due to which we were unable to correlate changes in cytokine production directly to plasma SCFAs. After 4 weeks of butyrate supplementation we even detected decreases in plasma propionate, and fecal total SCFAs, acetate, propionate and butyrate. Within the scope of this study, we unfortunately have no method of exploring why this is occurring. Possibly, the addition of oral butyrate induced flux changes for acetate and propionate as well.
In conclusion, twice daily intake of 2 grams of sodium butyrate for 4 weeks most likely only transiently increased butyrate concentration in the gut. We found that this leads to a decreased training capacity of monocytes by oxLDL and β-glucan in the group of obese males. Oral butyrate supplementation may therefore be beneficial to reduce the overall inflammatory phenotype of circulating monocytes in metabolic syndrome patients and possibly even slow down the development of vascular wall inflammation and atherosclerosis. However, this will need to be studied in larger groups while closely looking at influences of the microbiome and diet on SCFA fluxes, and extensively examining vascular wall inflammation and atherosclerotic plaque formation.
METHODS Study setup
The ex vivo experiments performed in this study are part of the larger OBUGAT study (Effect of Oral BUtyrate on human Glucose and brown fAT metabolism), which has been performed in the Academic Medical Center in Amsterdam, the Netherlands (personal correspondence with prof. Nieuwdorp). In this study, participants received oral butyrate supplementation of 4 grams daily for 4 weeks. Before and after treatment, venous EDTA blood was drawn for ex vivo experiments, and short-chain fatty acid concentrations were determined in plasma and feces. This study was approved by the medical research ethics committee of the Academic Medical Center in Amsterdam (METC number 2013_229) and conducted according to the principles in the Declaration of Helsinki. All volunteers gave informed consent. The study was registered in the WHO International Clinical Trial Registry Platform on 9 January 2014 under the reference number NTR4392.
Subjects
In total 10 healthy lean males and 10 obese males were included in the study. To be eligible for inclusion in the study, subjects in the Lean group must be over 18 years of age and have a body mass index (BMI) of 19–25 kg/m2. Exclusion criteria were smoking, medication use, and an estimated glomerular filtration rate of <60. For inclusion in the obese (MetSyn) group, subjects must be over 18 years of age, have a body mass index (BMI) of >25 kg/m2, and possess 3 of the 5 criteria for metabolic syndrome. These have been described by the American Heart Association and National Heart, Lung, and Blood Institute as fasting plasma glucose ≥5.6 mmol/L, blood pressure ≥130/85 mmHg, triglycerides ≥1.69 mmol/L, high-density lipoprotein cholesterol <1.03 mmol/L, or a waist circumference ≥102 cm36. Exclusion criteria for this group are smoking and medication use.
SCFA measurement in plasma and feces
Acetate, propionate and butyrate concentrations were determined in overnight fasted plasma samples and feces by liquid chromatography tandem mass spectrometry (LC-MS/MS) as described previously37. Feces were collected during 24 hours before study visits at baseline before butyrate supplementation and at 4 weeks after supplementation regime. Subjects kept the samples in the fridge at 3–4 °C before the visit and transported it on ice packs.
PBMC isolation and direct stimulation
Peripheral blood mononuclear cells (PBMCs) were isolated using density gradient centrifugation with Ficoll-Paque and resuspended in Dutch modified RPMI culture medium (Invitrogen) supplemented with 50 µg/mL gentamycin (Centrafarm), 2 mM GlutaMAX and 1 mM pyruvate (Life Technologies). For the first stimulation experiments, the cells were cultured for 24 hours in the presence of 1 × 106 CFU/mL heat-killed Escherichia coli (ATCC 35218, in house), 1 × 106 CFU/mL Staphylococcus aureus (ATCC 29213, in house), 1 × 106 CFU/mL Bacteroides fragilis (ATCC 25285, in house), 1 µg/mL Mycobacterium tuberculosis (H37Rv, in house), 1 × 106 CFU/mL Borrelia burgdorferi (ATCC 35210), or 1 × 106 Candida albicans conidia (UC820, in house). Secondly, in another experiment cells were cultured for 24 hours with 1 µg/mL Pam3CKS4 (EMC Microcollections), 1 ng/mL E. coli lipopolysaccharide (LPS, Sigma), or 50 µM palmitate (C16.0, Sigma, conjugated to human albumin as described in12) alone or in combination with monosodium urate (MSU) crystals (made in house with uric acid, Sigma, and sodium hydroxide, Merck, as described in12).
Trained immunity experiments in adherent monocytes
For the training experiment, PBMCs were plated in a flat-bottom 96-well plate and left to adhere at 37 °C 5% CO2 for 1 hour, after which the cells were gently washed three times with warm phosphate-buffered saline (PBS). Subsequently, the cells were cultured for 24 hours with 1 µg/mL β-glucan (kindly provided by professor David Willliams, TN, USA), 10 µg/mL Bacillus Calmette-Guérin vaccine (BCG, Statens Serum Institute) or 10 µg/mL oxidized LDL (prepared in house as described before38). The cells were washed once with PBS at 37 °C and left to rest for 5 days, replenishing culture medium with 10% human pooled serum at day 3. At day 6, the cells were restimulated for 24 hours with 10 µg/mL Pam3CSK4 or 10 ng/mL E. coli LPS (see Fig. 3).
Cytokine measurements and blood cell counts
After culturing the cells, supernatants were collected from the experiments. Interleukin-1β (IL-1β), interleukin-1 receptor antagonist (IL-1Ra), and tumor necrosis factor-α (TNF-α) concentrations in the supernatant were determined with commercially available ELISA kits from R&D Systems, and the ELISA kits for IL-6 and IL-10 were purchased from Sanquin. Blood differential test was performed with whole EDTA blood by the clinical diagnostic laboratory of the Radboudumc in Nijmegen, the Netherlands.
Statistical analyses
The Lean and MetSyn groups of the study were compared using the Mann-Whitney U test and time points within one group were compared with the Wilcoxon signed rank test, both performed with Graphpad Prism software version 6.0. Due to the small group numbers in this pilot study no correction for multiple testing was applied. The number of subjects per group may differ for the different ex vivo experiments due to exclusion of donors giving a cytokine response to RPMI controls. Exact numbers per experiment are stated in the figure legends.
References
D’Argenio, V. & Salvatore, F. The role of the gut microbiome in the healthy adult status. Clin Chim Acta 451, 97–102, https://doi.org/10.1016/j.cca.2015.01.003 (2015).
Heintz-Buschart, A. & Wilmes, P. Human Gut Microbiome: Function Matters. Trends Microbiol, https://doi.org/10.1016/j.tim.2017.11.002 (2017).
Rios-Covian, D. et al. Intestinal Short Chain Fatty Acids and their Link with Diet and Human Health. Front Microbiol 7, 185, https://doi.org/10.3389/fmicb.2016.00185 (2016).
Donohoe, D. R. et al. The microbiome and butyrate regulate energy metabolism and autophagy in the mammalian colon. Cell metabolism 13, 517–526, https://doi.org/10.1016/j.cmet.2011.02.018 (2011).
Roediger, W. E. Role of anaerobic bacteria in the metabolic welfare of the colonic mucosa in man. Gut 21, 793–798 (1980).
Lachmandas, E. et al. Diabetes Mellitus and Increased Tuberculosis Susceptibility: The Role of Short-Chain Fatty Acids. Journal of diabetes research 2016, 6014631, https://doi.org/10.1155/2016/6014631 (2016).
Liu, T. et al. Short-chain fatty acids suppress lipopolysaccharide-induced production of nitric oxide and proinflammatory cytokines through inhibition of NF-kappaB pathway in RAW264.7 cells. Inflammation 35, 1676–1684, https://doi.org/10.1007/s10753-012-9484-z (2012).
Park, J. S., Lee, E. J., Lee, J. C., Kim, W. K. & Kim, H. S. Anti-inflammatory effects of short chain fatty acids in IFN-gamma-stimulated RAW 264.7 murine macrophage cells: involvement of NF-kappaB and ERK signaling pathways. International immunopharmacology 7, 70–77, https://doi.org/10.1016/j.intimp.2006.08.015 (2007).
Saemann, M. D. et al. Anti-inflammatory effects of sodium butyrate on human monocytes: potent inhibition of IL-12 and up-regulation of IL-10 production. FASEB journal: official publication of the Federation of American Societies for Experimental Biology 14, 2380–2382, https://doi.org/10.1096/fj.00-0359fje (2000).
Segain, J. P. et al. Butyrate inhibits inflammatory responses through NFkappaB inhibition: implications for Crohn’s disease. Gut 47, 397–403 (2000).
Chang, P. V., Hao, L., Offermanns, S. & Medzhitov, R. The microbial metabolite butyrate regulates intestinal macrophage function via histone deacetylase inhibition. Proceedings of the National Academy of Sciences of the United States of America 111, 2247–2252, https://doi.org/10.1073/pnas.1322269111 (2014).
Cleophas, M. C. et al. Suppression of monosodium urate crystal-induced cytokine production by butyrate is mediated by the inhibition of class I histone deacetylases. Annals of the rheumatic diseases 75, 593–600, https://doi.org/10.1136/annrheumdis-2014-206258 (2016).
Vinolo, M. A. et al. Suppressive effect of short-chain fatty acids on production of proinflammatory mediators by neutrophils. The Journal of nutritional biochemistry 22, 849–855, https://doi.org/10.1016/j.jnutbio.2010.07.009 (2011).
Shakespear, M. R., Halili, M. A., Irvine, K. M., Fairlie, D. P. & Sweet, M. J. Histone deacetylases as regulators of inflammation and immunity. Trends in immunology 32, 335–343, https://doi.org/10.1016/j.it.2011.04.001 (2011).
Brown, A. J. et al. The Orphan G protein-coupled receptors GPR41 and GPR43 are activated by propionate and other short chain carboxylic acids. The Journal of biological chemistry 278, 11312–11319, https://doi.org/10.1074/jbc.M211609200 (2003).
Le Poul, E. et al. Functional characterization of human receptors for short chain fatty acids and their role in polymorphonuclear cell activation. The Journal of biological chemistry 278, 25481–25489, https://doi.org/10.1074/jbc.M301403200 (2003).
Maslowski, K. M. et al. Regulation of inflammatory responses by gut microbiota and chemoattractant receptor GPR43. Nature 461, 1282–1286, https://doi.org/10.1038/nature08530 (2009).
Sina, C. et al. G protein-coupled receptor 43 is essential for neutrophil recruitment during intestinal inflammation. Journal of immunology 183, 7514–7522, https://doi.org/10.4049/jimmunol.0900063 (2009).
Cummings, J. H., Pomare, E. W., Branch, W. J., Naylor, C. P. & Macfarlane, G. T. Short chain fatty acids in human large intestine, portal, hepatic and venous blood. Gut 28, 1221–1227 (1987).
Vinolo, M. A. et al. Tributyrin attenuates obesity-associated inflammation and insulin resistance in high-fat-fed mice. American journal of physiology. Endocrinology and metabolism 303, E272–282, https://doi.org/10.1152/ajpendo.00053.2012 (2012).
Aguilar, E. C. et al. Butyrate impairs atherogenesis by reducing plaque inflammation and vulnerability and decreasing NFkappaB activation. Nutrition, metabolism, and cardiovascular diseases: NMCD 24, 606–613, https://doi.org/10.1016/j.numecd.2014.01.002 (2014).
Gao, Z. et al. Butyrate improves insulin sensitivity and increases energy expenditure in mice. Diabetes 58, 1509–1517, https://doi.org/10.2337/db08-1637 (2009).
Di Sabatino, A. et al. Oral butyrate for mildly to moderately active Crohn’s disease. Alimentary pharmacology & therapeutics 22, 789–794, https://doi.org/10.1111/j.1365-2036.2005.02639.x (2005).
Vernia, P. et al. Combined oral sodium butyrate and mesalazine treatment compared to oral mesalazine alone in ulcerative colitis: randomized, double-blind, placebo-controlled pilot study. Digestive diseases and sciences 45, 976–981 (2000).
Saeed, S. et al. Epigenetic programming of monocyte-to-macrophage differentiation and trained innate immunity. Science 345, 1251086, https://doi.org/10.1126/science.1251086 (2014).
Cheng, S. C. et al. mTOR- and HIF-1alpha-mediated aerobic glycolysis as metabolic basis for trained immunity. Science 345, 1250684, https://doi.org/10.1126/science.1250684 (2014).
Bekkering, S. et al. Oxidized low-density lipoprotein induces long-term proinflammatory cytokine production and foam cell formation via epigenetic reprogramming of monocytes. Arterioscler Thromb Vasc Biol 34, 1731–1738, https://doi.org/10.1161/ATVBAHA.114.303887 (2014).
Bouter, K. et al. Differential metabolic effects of oral butyrate treatment in lean versus metabolic syndrome subjects. Clin Transl Gastroenterol 9, 155, https://doi.org/10.1038/s41424-018-0025-4 (2018).
Quintin, J. et al. Candida albicans infection affords protection against reinfection via functional reprogramming of monocytes. Cell Host Microbe 12, 223–232, https://doi.org/10.1016/j.chom.2012.06.006 (2012).
Arts, R. J. et al. Immunometabolic Pathways in BCG-Induced Trained Immunity. Cell Rep 17, 2562–2571, https://doi.org/10.1016/j.celrep.2016.11.011 (2016).
Bekkering, S., Joosten, L. A., van der Meer, J. W., Netea, M. G. & Riksen, N. P. The epigenetic memory of monocytes and macrophages as a novel drug target in atherosclerosis. Clinical therapeutics 37, 914–923, https://doi.org/10.1016/j.clinthera.2015.01.008 (2015).
den Besten, G. et al. Short-Chain Fatty Acids Protect Against High-Fat Diet-Induced Obesity via a PPARgamma-Dependent Switch From Lipogenesis to Fat Oxidation. Diabetes 64, 2398–2408, https://doi.org/10.2337/db14-1213 (2015).
McNeil, N. I., Cummings, J. H. & James, W. P. Short chain fatty acid absorption by the human large intestine. Gut 19, 819–822 (1978).
Bloemen, J. G. et al. Short chain fatty acids exchange across the gut and liver in humans measured at surgery. Clin Nutr 28, 657–661, https://doi.org/10.1016/j.clnu.2009.05.011 (2009).
Canfora, E. E. et al. Colonic infusions of short-chain fatty acid mixtures promote energy metabolism in overweight/obese men: a randomized crossover trial. Sci Rep 7, 2360, https://doi.org/10.1038/s41598-017-02546-x (2017).
Grundy, S. M. et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 112, 2735–2752, https://doi.org/10.1161/CIRCULATIONAHA.105.169404 (2005).
Karlsson, F. H. et al. Gut metagenome in European women with normal, impaired and diabetic glucose control. Nature 498, 99–103, https://doi.org/10.1038/nature12198 (2013).
van Tits, L. J., Demacker, P. N., de Graaf, J., Hak-Lemmers, H. L. & Stalenhoef, A. F. Alpha-tocopherol supplementation decreases production of superoxide and cytokines by leukocytes ex vivo in both normolipidemic and hypertriglyceridemic individuals. The American journal of clinical nutrition 71, 458–464 (2000).
Acknowledgements
This study was supported by an IN-CONTROL CVON grant (CVON2012- 03) of the Netherlands Heart Foundation. MCPC is supported by a grant of the Dutch Arthritis Foundation (nr. 12-2-303). M.G.N. was supported by an E.R.C. Consolidator Grant (#310372) and a Spinoza Grant of the Netherlands Organization for Scientific Research. L.A.B.J. was supported by was supported by a Competitiveness Operational Programme grant of the Romanian Ministry of European Funds (HINT, P_37_762).
Author information
Authors and Affiliations
Contributions
E.S.S. designed the OBUGAT study and included all the subjects. M.C.P.C., J.M.R., S.B., J.Q., M.G.N. and L.A.B.J. set up the in vitro part of the study. M.C.P.C., J.M.R., S.B., J.Q. and K.S. performed all the in vitro stimulation experiments and cytokine measurements. M.C.P.C. wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cleophas, M.C.P., Ratter, J.M., Bekkering, S. et al. Effects of oral butyrate supplementation on inflammatory potential of circulating peripheral blood mononuclear cells in healthy and obese males. Sci Rep 9, 775 (2019). https://doi.org/10.1038/s41598-018-37246-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-37246-7
This article is cited by
-
Maternal microbiota and gestational diabetes: impact on infant health
Journal of Translational Medicine (2023)
-
The potential of tailoring the gut microbiome to prevent and treat cardiometabolic disease
Nature Reviews Cardiology (2023)
-
Non-digestible oligosaccharides-based prebiotics to ameliorate obesity: Overview of experimental evidence and future perspectives
Food Science and Biotechnology (2023)
-
Drug-Resistant Epilepsy and Gut-Brain Axis: an Overview of a New Strategy for Treatment
Molecular Neurobiology (2023)
-
Immunmodulation durch Ernährung bei kritisch kranken Patienten
Die Anaesthesiologie (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.