Abstract
The aim of this meta-analysis of randomized placebo-controlled clinical trials was to assess the effect of ezetimibe on plasma lipoprotein(a) concentrations. Only randomized placebo-controlled trials investigating the impact of ezetimibe treatment on cholesterol lowering that include lipoprotein(a) measurement were searched in PubMed-Medline, SCOPUS, Web of Science and Google Scholar databases (from inception to February 26th, 2018). A random-effects model and generic inverse variance method were used for quantitative data synthesis. Sensitivity analysis was conducted using the leave-one-out method. A weighted random-effects meta-regression was performed to evaluate the impact of potential confounders on lipoprotein concentrations. This meta-analysis of data from 10 randomized placebo-controlled clinical trials (15 treatment arms) involving a total of 5188 (3020 ezetimibe and 2168 control) subjects showed that ezetimibe therapy had no effect on altering plasma Lp(a) concentrations (WMD: −2.59%, 95% CI: −8.26, 3.08, p = 0.370; I2 = 88.71%, p(Q) < 0.001). In the subgroup analysis, no significant alteration in plasma Lp(a) levels was observed either in trials assessing the impact of monotherapy with ezetimibe versus placebo (WMD: −4.64%, 95% CI: −11.53, 2.25, p = 0.187; I2 = 65.38%, p(Q) = 0.005) or in trials evaluating the impact of adding ezetimibe to a statin versus statin therapy alone (WMD: −1.04%, 95% CI: −6.34, 4.26, p = 0.700; I2 = 58.51%, p(Q) = 0.025). The results of this meta-analysis suggest that ezetimibe treatment either alone or in combination with a statin does not affect plasma lipoprotein(a) levels.
Similar content being viewed by others
Introduction
Ezetimibe inhibits absorption of cholesterol at the brush border of the small intestine via the sterol transporter, Niemann-Pick C1-Like1 (NPC1L1)1. This leads to a decreased delivery of cholesterol to the liver, reduction of hepatic cholesterol stores and an increased clearance of cholesterol from the blood and studies have shown a reduction in LDL-cholesterol (LDL-C) by 17% when used alone2 and a reduction of 14–25% in combination with statins3. The IMPROVE-IT (Improved Reduction of Outcomes: Vytorin Efficacy International Trial) in 18144 subjects with recent acute coronary syndrome showed that ezetimibe 10 mg added to simvastatin 40 mg daily reduced LDL-C by 16% with a 6% reduction in the risk of the primary cardiovascular outcome4.
Lipoprotein(a) (Lp(a)) is a low-density lipoprotein (LDL)-like particle with proatherogenic, prothrombotic and proinflammatory properties that make it a significant contributor to atherothrombotic events5,6,7,8,9,10. Lp(a) has been suggested to be an independent risk factor for cardiovascular disease with an increased odds ratio of 1.611; however, a large meta-analysis of 36 prospective studies showed the risk ratio was 1.1312. Lp(a) is associated with acute coronary syndrome13 and increased levels are found commonly in patients with premature coronary heart disease14. Therefore, therapeutic approaches capable of reducing elevated plasma Lp(a) concentrations may be important.
Kinetic studies have concluded that Lp(a) levels are mainly regulated by differences in biosynthesis, and biosynthetic changes have been associated to the Lp(a) lowering activity of anacetrapib15. Recent reports have also indicated the role of plasminogen receptor KT in Lp(a) cell internalization, which is followed by recycling of the apo(a) component16. Additional to these mechanisms, there is evidence showing that Lp(a) serves as an acute-phase reactant and its biosynthesis is augmented by inflammation17,18,19. Ezetimibe is known to possess anti-inflammatory activity and may therefore affect Lp(a) production20,21,22,23. The involvement of the LDL receptor (LDLR) in the catabolism and clearance of plasma Lp(a) has also been discussed24,25. On the other hand, ezetimibe has been reported to potentiate the stimulating activity of statins on LDLR gene expression26. Given these lines of evidence, it might be plausible that the benefits of ezetimibe in improving outcomes, such as that observed in the IMPROVE-IT study, may in part be due to a decrease in Lp(a) levels and this meta-analysis of all randomized controlled trials was undertaken to determine if ezetimibe therapy does decrease Lp(a) levels.
Methods
Search Strategy
This study was designed according to the guidelines of the 2009 preferred reporting items for systematic reviews and meta-analysis (PRISMA) statement27. PubMed-Medline, SCOPUS, Web of Science and Google Scholar databases were searched using the following search terms within titles and abstracts (also in combination with MESH terms): (ezetimibe) AND (lipoprotein(a) OR “lipoprotein (a)” OR Lp(a) OR “Lp (a)”). Sensitivity of the search strategy was increased by using the wild-card term “*”. The search was limited to articles published in English language. The literature was searched from inception to February 26, 2018.
Study Selection
Original studies were included if they met the following inclusion criteria: (i) being a randomized placebo-controlled trial with either parallel or cross-over design, (ii) investigating the impact of ezetimbe vs. placebo (or ezetimibe plus a statin vs. statin alone) on plasma/serum concentrations of Lp(a), and, (iii) presentation of sufficient information on Lp(a) concentrations at baseline and at the end of follow-up in each group or providing the net change values. Exclusion criteria were: (i) non-randomized controlled trials, (ii) lack of a control group for ezetimibe treatment, (iii) observational studies with case-control, cross-sectional or cohort design, and (iv) lack of sufficient information on baseline or follow-up Lp(a) concentrations.
Data extraction
Eligible studies were reviewed and the following data were abstracted: (1) first author’s name; (2) year of publication; (3) country were the study was performed; (4) study design; (5) number of participants in the ezetimibe and control groups; (6) comedications including statins; (7) dose of ezetimibe; (8) treatment duration; (9) age, gender and body mass index (BMI) of study participants; (9) method of Lp(a) assay; and (10) data regarding baseline and follow-up plasma concentrations of Lp(a).
Quality assessment
Included studies were systematically evaluated for the risk of bias according to the Cochrane criteria28, and as previously described, that included the assessment of each study for: adequacy of sequence generation, allocation concealment, blinding, addressing of dropouts (incomplete outcome data) and selective outcome reporting. According to the recommendations of the Cochrane Handbook, a judgment of “yes” indicated low risk of bias, while “no” indicated high risk of bias. Labeling an item as “unclear” indicated an unclear or unknown risk of bias.
Quantitative Data Synthesis
Comprehensive Meta-Analysis (CMA) V2 software (Biostat, NJ)29 was used to undertake the meta-analysis. Effect size was calculated as: (measure at the end of follow-up in the treatment group – measure at baseline in the treatment group) – (measure at the end of follow-up in the control group – measure at baseline in the control group). A random-effects model (using DerSimonian-Laird method) and the generic inverse variance weighting method were used to compensate for the heterogeneity of studies in terms of study design, treatment duration, and the characteristics of populations being studied30. All values were collated as percentage changes. Standard deviations (SDs) of the mean difference were calculated using the following formula: SD = square root [(SDpre-treatment)2 + (SDpost-treatment)2 − (2 R × SDpre-treatment × SDpost-treatment)], assuming a correlation coefficient (R) = 0.531,32,33. Heterogeneity index was assessed using I2 index and Cochrane Q test. If the outcome measures were reported in median and range (or 95% confidence interval), mean and standard SD values were estimated using the method described by Wan et al.34. Where standard error of the mean (SEM) was only reported, SD was estimated using the following formula: SD = SEM × sqrt (n), where n is the number of subjects. Effect sizes were expressed as weighted mean difference (WMD) and 95% confidence interval (CI). If the outcome measures were reported in median and range (or 95% CI), mean and SD values were estimated using the method described by Wan et al.34. In order to evaluate the influence of each study on the overall effect size, a sensitivity analysis was conducted using the leave-one-out method (i.e., removing one study each time and repeating the analysis)35,36,37,38.
Meta-regression
As potential confounder of treatment response, baseline plasma Lp(a) levels were entered into a random-effects meta-regression model to explore their association with the estimated effect size on plasma Lp(a) concentrations37.
Publication bias
Evaluation of funnel plot, Begg’s rank correlation and Egger’s weighted regression tests were employed to assess the presence of publication bias in the meta-analysis38. When there was an evidence of funnel plot asymmetry, potentially missing studies were imputed using the “trim and fill” method39.
Results
Characteristics of included studies
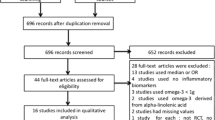
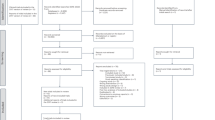
A total of 408 clinical trials were identified of which 390 did not meet the inclusion criteria and were excluded. Eighteen full-text articles were carefully reviewed for eligibility from which 8 studies were excluded due to the lack of control group (n = 3), no ezetimibe arm (n = 2), lp(a) concentrations were not measured (n = 2), and not presenting numerical values (n = 1). After this assessment, 10 clinical trials were selected and included in this systematic review and meta-analysis. Flow chart that detailing the studies identified, screened, those that were eligible and those that were included into the meta-analysis is shown in Fig. 1.
Data were pooled from 10 clinical trials comprising a total of 5188 subjects, including 3020 and 2168 participants in the ezetimibe therapy and control arms (individuals of the cross-over trials were considered in treatment and control groups), respectively. Selected studies were published between 2002 and 2012. The range of intervention periods was from 5 weeks40 to 12 weeks3,41,42,43,44,45,46,47. Study designs of included trials were parallel3,41,42,43,44,45,46,47,48 and cross-over group40. Evaluated studies enrolled subjects with primary hypercholesterolemia3,41,42,43,44,45,46,47,48 and severe hypercholesterolemia40. Characteristics of the included clinical trials are shown in Table 1.
Lp(a) assay methods
The majority of the studies included in the meta-analysis quantified Lp(a) levels by competitive enzyme-linked immunosorbent assay3,41,42,43,44,45,46,48, while other trials determined Lp(a) levels by a nephelometric assay (Dade Behring)40,47.
Risk of bias in the included studies
Several studies showed low risk of bias regarding random sequence generation, only one trial had high risk of bias for this parameter48. Most of the included studies had a lack of information about the allocation concealment, and a high risk of bias was found in one trial48. Several studies presented insufficient information on the blinding process of the participants, study personnel and the outcome assessors, and two trials showed high risk of bias47,48. Almost all of the assessed studies showed that there was a low risk of bias for incomplete outcome data, only one trial exhibited limited information41. Finally, all selected studies presented low risk of bias regarding selective outcome reporting. Cochrane guidelines applied to the assessment of quality of bias in the studies that were included in the meta-analysis are shown in Table 2.
Effect of Ezetimibe on plasma Lp(a) concentrations
Overall, 10 studies comprising 15 treatment arms were included in the meta-analysis. Meta-analysis did not suggest a significant change in plasma Lp(a) concentrations following treatment with ezetimibe (WMD: −2.59%, 95% CI: −8.26, 3.08, p = 0.370; I2 = 88.71%, p(Q) < 0.001) (Fig. 2). The effect size was robust in sensitivity analysis (Fig. 2) and the effect size remained significant or marginally significant after omission of each single study from the meta-analysis.
In the subgroup analysis, no significant alteration in plasma Lp(a) levels was observed either in trials assessing the impact of monotherapy with ezetimibe versus placebo (WMD: −4.64%, 95% CI: −11.53, 2.25, p = 0.187; I2 = 65.38%, p(Q) = 0.005) or in trials evaluating the impact of adding ezetimibe to a statin versus statin therapy alone (WMD: −1.04%, 95% CI: −6.34, 4.26, p = 0.700; I2 = 58.51%, p(Q) = 0.025) (Fig. 3).
Weighted mean difference and 95% confidence intervals for the impact of ezetimibe on plasma Lp(a) concentrations in subgroups of trials administering ezetimibe as monotherapy or in combination with statins displayed as a Forest plot. The results of leave-one-out sensitivity analysis is shown in the lower panel.
Meta-regression
To assess the impact of baseline Lp(a) concentrations on the effect of ezetimibe on plasma Lp(a) levels, a random-effects meta-regression was undertaken. The result did not suggest a significant association under a random-effects meta-regression model (slope: 0.135; 95% CI: −0.504, 0.774; p = 0.679) (Fig. 4).
Publication bias
Visual inspection of Begg’s funnel plots showed an asymmetry in the meta-analyses of ezetimibe’s effects on plasma Lp(a) concentrations. This asymmetry was corrected by imputing four potentially missing studies using “trim and fill” method, yielding a corrected effect size of −5.56 (95% CI: −10.50, −0.61) (Fig. 5). Consistently, Egger’s regression test (t = 3.38, df = 13, p = 0.005) did suggest the presence of publication bias. However, there was no sign of publication bias according to the Begg’s rank correlation test (tau = −0.27, z = 1.39, p = 0.166).
Discussion
In this meta-analysis of randomized placebo-controlled clinical trials, ezetimibe therapy was not related to a significant reduction of plasma Lp(a) levels. This result was robust in the sensitivity analysis and was confirmed both when ezetimibe was used as monotherapy and in combination with a statin. In a previous meta-analysis, ezetimibe monotherapy was found to cause a significant but small and not clinically relevant reduction (7%) in plasma Lp(a) levels49. The present meta-analysis provides a more robust confirmation on the lack of any Lp(a)-lowering effect of ezetimibe compared with referenced meta-analysis because of including a larger number of randomized controlled trials (n = 10 vs. 7). Moreover, in addition to the impact of monotherapy, this meta-analysis also evaluated the impact of the combination of ezetimibe and statins (vs. statin monotherapy) on plasma Lp(a) levels that has not been the subject of any prior meta-analysis.
Lp(a) is associated with acute coronary syndrome13 and increased levels are found commonly in patients with premature coronary heart disease14. Other studies including Lp(a) in a predictive model for cardiovascular prevention have suggested that the inclusion of Lp(a) in the models does increase their predictive value50,51,52,53. However, whilst Lp(a) elevation is associated with cardiovascular disease it is still unclear if there is a benefit in therapeutically targeting its reduction specifically. Although no specific therapy for lowering Lp(a) is as yet approved, the body of evidence supports the reducing effects by lipoprotein apheresis54, proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors55, estrogen mimics and selective estrogen receptor modulators56,57,58, nicotinic acid59 and some nutraceuticals60,61,62,63. Moreover, selective apo(a) antisense therapy has shown promising lowering effects in patients with elevated Lp(a) in phase II trials64. With this background, an additional pharmacological tool for Lp(a)-lowering would be desirable.
Ezetimibe has a modest LDL-C-lowering efficacy that has been associated with a significant improvement of cardiovascular prognosis in the IMPROVE-IT trial4. Given the reduction in plasma LDL-C levels with ezetimibe and the similarity in the lipid composition between Lp(a) and LDL particles2,3, it might be hypothesized that ezetimibe would have also an impact on plasma Lp(a) levels. However, this meta-analysis collecting the inconsistent results of 10 randomized placebo-controlled trials was convincing that this is not the case, despite few studies reported a beneficial effect of ezetimibe on plasma Lp(a) levels3,42,45,47. Clear reasons explaining the divergent results of the included trials did not emerge from the analytical comparison of each of them; however, we cannot rule out the hypothesis that untested or unreported data might have contributed to such an inconsistency. Thus, for instance, whether baseline BMI might have affected the Lp(a)-lowering efficacy of ezetimibe cannot be excluded; accordingly, in 33,42,45,47 out of 4 trials3,42,45,47 reporting a significant impact of ezetimibe on Lp(a), average BMI was almost 29, whereas it was 26 in the only 2 trials40,48 reporting the baseline BMI value of the study participants and which also showed a neutral effect of ezetimibe on Lp(a). Hence, further trials with complete reporting of the baseline characteristics of the study subjects are warranted.
This meta-analysis has a number of limitations. Firstly, effects of ezetimibe therapy on Lp(a) were not the primary aim of the clinical trials and the studies were not powered for this. Secondly, there were only 10 trials available to be analysed giving a modest though robust number of subjects to undertake the analysis. Thirdly, the longest duration of the trials exploring the Lp(a)-lowering effect of ezetimibe was 12 weeks, which might be too short to allow a greater impact on plasma Lp(a) levels. Finally, given the skewed distribution of Lp(a) values in the population, further clarification would benefit from pooled analyses of individual patient data.
Conclusion
The results of this meta-analysis suggest that ezetimibe treatment does not reduce plasma lipoprotein(a) levels and therefore Lp(a) reduction does not contribute to its therapeutic effect in cardiovascular prevention.
Change history
14 February 2020
An amendment to this paper has been published and can be accessed via a link at the top of the paper.
References
Sudhop, T. et al. Inhibition of intestinal cholesterol absorption by ezetimibe in humans. Circulation 106, 1943–1948 (2002).
Knopp, R. H. et al. Effects of ezetimibe, a new cholesterol absorption inhibitor, on plasma lipids in patients with primary hypercholesterolemia. European heart journal 24, 729–741 (2003).
Davidson, M. H. et al. Ezetimibe coadministered with simvastatin in patients with primary hypercholesterolemia. Journal of the American College of Cardiology 40, 2125–2134 (2002).
Cannon, C. P. et al. Ezetimibe Added to Statin Therapy after Acute Coronary Syndromes. The New England journal of medicine 372, 2387–2397, https://doi.org/10.1056/NEJMoa1410489 (2015).
Ellis, K. L., Boffa, M. B., Sahebkar, A., Koschinsky, M. L. & Watts, G. F. The renaissance of lipoprotein(a): Brave new world for preventive cardiology? Progress in Lipid Research 68, 57–82, https://doi.org/10.1016/j.plipres.2017.09.001 (2017).
Ferretti, G. et al. Lipoprotein(a): A missing culprit in the management of athero-thrombosis? Journal of Cellular Physiology, https://doi.org/10.1002/jcp.26050 (2017).
Pirro, M. et al. Lipoprotein(a) and inflammation: A dangerous duet leading to endothelial loss of integrity. Pharmacological Research 119, 178–187, https://doi.org/10.1016/j.phrs.2017.02.001 (2017).
Kronenberg, F. & Utermann, G. Lipoprotein(a): resurrected by genetics. J Intern Med 273, 6–30, https://doi.org/10.1111/j.1365-2796.2012.02592.x (2013).
Schmidt, K., Noureen, A., Kronenberg, F. & Utermann, G. Structure, function, and genetics of lipoprotein (a). J Lipid Res 57, 1339–1359, https://doi.org/10.1194/jlr.R067314 (2016).
Seed, M. et al. Relation of serum lipoprotein(a) concentration and apolipoprotein(a) phenotype to coronary heart disease in patients with familial hypercholesterolemia. The New England journal of medicine 322, 1494–1499, https://doi.org/10.1056/NEJM199005243222104 (1990).
Bennet, A. et al. Lipoprotein(a) levels and risk of future coronary heart disease: large-scale prospective data. Archives of internal medicine 168, 598–608, https://doi.org/10.1001/archinte.168.6.598 (2008).
Erqou, S. et al. Lipoprotein(a) concentration and the risk of coronary heart disease, stroke, and nonvascular mortality. Jama 302, 412–423, https://doi.org/10.1001/jama.2009.1063 (2009).
Dangas, G. et al. Correlation of serum lipoprotein(a) with the angiographic and clinical presentation of coronary artery disease. The American journal of cardiology 83, 583–585, a587 (1999).
Genest, J. J. Jr. et al. Familial lipoprotein disorders in patients with premature coronary artery disease. Circulation 85, 2025–2033 (1992).
Thomas, T. et al. CETP (Cholesteryl Ester Transfer Protein) Inhibition With Anacetrapib Decreases Production of Lipoprotein(a) in Mildly Hypercholesterolemic Subjects. Arteriosclerosis, thrombosis, and vascular biology 37, 1770–1775, https://doi.org/10.1161/ATVBAHA.117.309549 (2017).
Sharma, M., Redpath, G. M., Williams, M. J. & McCormick, S. P. Recycling of Apolipoprotein(a) After PlgRKT-Mediated Endocytosis of Lipoprotein(a). Circulation research 120, 1091–1102, https://doi.org/10.1161/CIRCRESAHA.116.310272 (2017).
Noma, A. et al. Lp(a): an acute-phase reactant? Chem Phys Lipids 67-68, 411–417 (1994).
Wade, D. P. et al. 5′ control regions of the apolipoprotein(a) gene and members of the related plasminogen gene family. Proc Natl Acad Sci USA 90, 1369–1373 (1993).
Wang, J., Hu, B., Kong, L., Cai, H. & Zhang, C. Native, oxidized lipoprotein(a) and lipoprotein(a) immune complex in patients with active and inactive rheumatoid arthritis: plasma concentrations and relationship to inflammation. Clin Chim Acta 390, 67–71, https://doi.org/10.1016/j.cca.2007.12.015 (2008).
Tobaru, T., Seki, A., Asano, R., Sumiyoshi, T. & Hagiwara, N. Lipid-lowering and anti-inflammatory effect of ezetimibe in hyperlipidemic patients with coronary artery disease. Heart Vessels 28, 39–45, https://doi.org/10.1007/s00380-012-0243-8 (2013).
Tie, C. et al. Ezetimibe Attenuates Atherosclerosis Associated with Lipid Reduction and Inflammation Inhibition. PLoS One 10, e0142430, https://doi.org/10.1371/journal.pone.0142430 (2015).
Qin, L. et al. Anti-inflammatory activity of ezetimibe by regulating NF-kappaB/MAPK pathway in THP-1 macrophages. Pharmacology 93, 69–75, https://doi.org/10.1159/000357953 (2014).
Dolezelova, E. et al. Effect of ezetimibe on plasma adipokines: a systematic review and meta-analysis. Br J Clin Pharmacol 83, 1380–1396, https://doi.org/10.1111/bcp.13250 (2017).
Lambert, G. et al. The complexity of lipoprotein (a) lowering by PCSK9 monoclonal antibodies. Clinical science 131, 261–268, https://doi.org/10.1042/CS20160403 (2017).
Watts, G. F. et al. Controlled study of the effect of proprotein convertase subtilisin-kexin type 9 inhibition with evolocumab on lipoprotein(a) particle kinetics. European heart journal, https://doi.org/10.1093/eurheartj/ehy122 (2018).
Gouni-Berthold, I. et al. Effects of ezetimibe and/or simvastatin on LDL receptor protein expression and on LDL receptor and HMG-CoA reductase gene expression: a randomized trial in healthy men. Atherosclerosis 198, 198–207, https://doi.org/10.1016/j.atherosclerosis.2007.09.034 (2008).
Moher, D., L., A., Tetzlaff, J., Altman, D. G. & PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339, b2535, https://doi.org/10.1136/bmj.b2535 (2009).
Higgins JPT, G. S. Handbook for Systematic Reviews of Interventions, Version 5.0.2 edn., (2009).
Borenstein M. H. L., Higgins JPT. Comprehensive Meta-analysis. (2005).
Sutton, A. J., A. K. Jones, D. R., Sheldon, T. A.,. Song F. Methods for meta-analysis in medical research. (2000).
Sahebkar, A. et al. Statin therapy reduces plasma endothelin-1 concentrations: A meta-analysis of 15 randomized controlled trials. Atherosclerosis 241, 433–442, https://doi.org/10.1016/j.atherosclerosis.2015.05.022 (2015).
Sahebkar, A. et al. Association between statin use and plasma D-dimer levels. A systematic review and meta-analysis of randomised controlled trials. Thromb Haemost 114, 546–557, https://doi.org/10.1160/TH14-11-0937 (2015).
Sahebkar, A. et al. Lack of efficacy of resveratrol on C-reactive protein and selected cardiovascular risk factors–Results from a systematic review and meta-analysis of randomized controlled trials. Int J Cardiol 189, 47–55, https://doi.org/10.1016/j.ijcard.2015.04.008 (2015).
Wan, X. W. W., Liu, J. & Tong, T. Estimating Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol. 14, 135, https://doi.org/10.1186/1471-2288-14-135. (2014).
Sahebkar, A. A systematic review and meta-analysis of randomized controlled trials investigating the effects of curcumin on blood lipid levels. Clinical Nutrition 33, 406–414, https://doi.org/10.1016/j.clnu.2013.09.012 (2014).
Sahebkar, A., Cicero, A. F. G., Simental-Mendía, L. E., Aggarwal, B. B. & Gupta, S. C. Curcumin downregulates human tumor necrosis factor-α levels: A systematic review and meta-analysis ofrandomized controlled trials. Pharmacological Research 107, 234–242, https://doi.org/10.1016/j.phrs.2016.03.026 (2016).
Serban, C. et al. A systematic review and meta-analysis of the effect of statins on plasma asymmetric dimethylarginine concentrations. Scientific Reports 5, https://doi.org/10.1038/srep09902 (2015).
Sahebkar, A. Does PPARgamma2 gene Pro12Ala polymorphism affect nonalcoholic fatty liver disease risk? Evidence from a meta-analysis. DNA Cell Biol 32, 188–198, https://doi.org/10.1089/dna.2012.1947 (2013).
Duval, S. T. R. Trim and fill: A simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56, 455–463 (2000).
Geiss, H. C., Otto, C., Hund-Wissner, E. & Parhofer, K. G. Effects of ezetimibe on plasma lipoproteins in severely hypercholesterolemic patients treated with regular LDL-apheresis and statins. Atherosclerosis 180, 107–112 (2005).
Ballantyne, C. M. et al. Ezetimibe Study Group. Effect of ezetimibe coadministered with atorvastatin in 628 patients with primary hypercholesterolemia: a prospective, randomized, double-blind trial. Circulation 107, 2409–2415 (2003).
Dujovne, C. A. et al. Study Group. Efficacy and safety of a potent new selective cholesterol absorption inhibitor, ezetimibe, in patients with primary hypercholesterolemia. Am J Cardiol. 90, 1092–1097 (2002).
Goldberg, A. C., S., A., Liu, J., Capece, R. & Mitchel, Y. B. Ezetimibe Study Group. Efficacy and safety of ezetimibe coadministered with simvastatin in patients with primary hypercholesterolemia: a randomized, double-blind, placebo-controlled trial. Mayo Clin Proc. 79, 620–629 (2004).
Kerzner, B. et al. Ezetimibe Study Group. Efficacy and safety of ezetimibe coadministered with lovastatin in primary hypercholesterolemia. Am J Cardiol. 91, 418–424 (2003).
Knopp, R. H. et al. Ezetimibe Study Group. Effects of ezetimibe, a new cholesterol absorption inhibitor, on plasma lipids in patients with primary hypercholesterolemia. Eur Heart J. 24, 729–741 (2003).
Melani, L. et al. Ezetimibe Study Group. Efficacy and safety of ezetimibe coadministered with pravastatin in patients with primary hypercholesterolemia: a prospective, randomized, double-blind trial. Eur Heart J. 24, 717–728 (2003).
Moutzouri, E. et al. Effect of simvastatin or its combination with ezetimibe on Toll-like receptor expression and lipopolysaccharide - induced cytokine production in monocytes of hypercholesterolemic patients. Atherosclerosis. 225, 381–387, https://doi.org/10.1016/j.atherosclerosis.2012.08.037 (2012).
Saougos, V. G. et al. AD. Differential effect of hypolipidemic drugs on lipoprotein-associated phospholipase A2. Arterioscler Thromb Vasc Biol. 27, 2236–2243, https://doi.org/10.1161/ATVBAHA.107.147280 (2007).
Awad, K. et al. Effect of Ezetimibe Monotherapy on Plasma Lipoprotein(a) Concentrations in Patients with Primary Hypercholesterolemia: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Drugs 78, 453–462, https://doi.org/10.1007/s40265-018-0870-1 (2018).
Willeit, P. et al. Discrimination and net reclassification of cardiovascular risk with lipoprotein(a): prospective 15-year outcomes in the Bruneck Study. Journal of the American College of Cardiology 64, 851–860, https://doi.org/10.1016/j.jacc.2014.03.061 (2014).
Kamstrup, P. R., Tybjaerg-Hansen, A. & Nordestgaard, B. G. Extreme lipoprotein(a) levels and improved cardiovascular risk prediction. Journal of the American College of Cardiology 61, 1146–1156, https://doi.org/10.1016/j.jacc.2012.12.023 (2013).
Kostner, K. M., Kostner, G. M. & Wierzbicki, A. S. Is Lp(a) ready for prime time use in the clinic? A pros-and-cons debate. Atherosclerosis 274, 16–22, https://doi.org/10.1016/j.atherosclerosis.2018.04.032 (2018).
Kostner, K. M., Marz, W. & Kostner, G. M. When should we measure lipoprotein (a)? Eur Heart J 34, 3268–3276, https://doi.org/10.1093/eurheartj/eht053 (2013).
Ezhov, M. V. et al. Specific Lipoprotein(a) apheresis attenuates progression of carotid intima-media thickness in coronary heart disease patients with high lipoprotein(a) levels. Atheroscler Suppl 18, 163–169, https://doi.org/10.1016/j.atherosclerosissup.2015.02.025 (2015).
Karatasakis, A. et al. Effect of PCSK9 Inhibitors on Clinical Outcomes in Patients With Hypercholesterolemia: A Meta-Analysis of 35 Randomized Controlled Trials. J Am Heart Assoc 6, https://doi.org/10.1161/JAHA.117.006910 (2017).
Ferretti, G. et al. Raloxifene Lowers Plasma Lipoprotein(a) Concentrations: a Systematic Review and Meta-analysis of Randomized Placebo-Controlled Trials. Cardiovascular Drugs and Therapy 31, 197–208, https://doi.org/10.1007/s10557-017-6721-6 (2017).
Kotani, K. et al. Tibolone decreases Lipoprotein(a) levels in postmenopausal women: A systematic review and meta-analysis of 12 studies with 1009 patients. Atherosclerosis 242, 87–96, https://doi.org/10.1016/j.atherosclerosis.2015.06.056 (2015).
Sahebkar, A. et al. The Effects of Tamoxifen on Plasma Lipoprotein(a) Concentrations: Systematic Review and Meta-Analysis. Drugs 77, 1187–1197, https://doi.org/10.1007/s40265-017-0767-4 (2017).
Sahebkar, A., Reiner, Ž., Simental-Mendïa, L. E., Ferretti, G. & Cicero, A. F. G. Effect of extended-release niacin on plasma lipoprotein(a) levels: A systematic review and meta-analysis of randomized placebo-controlled trials. Metabolism: Clinical and Experimental 65, 1664–1678, https://doi.org/10.1016/j.metabol.2016.08.007 (2016).
Panahi, Y., Khalili, N., Hosseini, M. S., Abbasinazari, M. & Sahebkar, A. Lipid-modifying effects of adjunctive therapy with curcuminoids-piperine combination in patients with metabolic syndrome: Results of a randomized controlled trial. Complementary Therapies in Medicine 22, 851–857, https://doi.org/10.1016/j.ctim.2014.07.006 (2014).
Panahi, Y. et al. Curcuminoids modify lipid profile in type 2 diabetes mellitus: A randomized controlled trial. Complementary Therapies in Medicine 33, 1–5, https://doi.org/10.1016/j.ctim.2017.05.006 (2017).
Sahebkar, A., Simental-Mendía, L. E., Stefanutti, C. & Pirro, M. Supplementation with coenzyme Q10 reduces plasma lipoprotein(a) concentrations but not other lipid indices: A systematic review and meta-analysis. Pharmacological Research 105, 198–209, https://doi.org/10.1016/j.phrs.2016.01.030 (2016).
Serban, M. C. et al. Impact of L-carnitine on plasma lipoprotein(a) concentrations: A systematic review and meta-analysis of randomized controlled trials. Scientific Reports 6, https://doi.org/10.1038/srep19188 (2016).
Viney, N. J. et al. Antisense oligonucleotides targeting apolipoprotein(a) in people with raised lipoprotein(a): two randomised, double-blind, placebo-controlled, dose-ranging trials. Lancet 388, 2239–2253, https://doi.org/10.1016/S0140-6736(16)31009-1 (2016).
Acknowledgements
All data is available from the authors upon application. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
A.S. and L.S. were involved in the study design, acquisition of data, analysis and interpretation of data, and paper drafting. K.A., M.P., M.B., G.W., C.S. and S.L.A. were involved in the study design, supervision read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sahebkar, A., Simental-Mendía, L.E., Pirro, M. et al. Impact of ezetimibe on plasma lipoprotein(a) concentrations as monotherapy or in combination with statins: a systematic review and meta-analysis of randomized controlled trials. Sci Rep 8, 17887 (2018). https://doi.org/10.1038/s41598-018-36204-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-36204-7
This article is cited by
-
Bibliometric analysis of residual cardiovascular risk: trends and frontiers
Journal of Health, Population and Nutrition (2023)
-
The correlation between lipoprotein(a) elevations and the risk of recurrent cardiovascular events in CAD patients with different LDL-C levels
BMC Cardiovascular Disorders (2022)
-
The Role of Non-statin Lipid-Lowering Medications in Youth with Hypercholesterolemia
Current Atherosclerosis Reports (2022)
-
Lp(a): a New Pathway to Target?
Current Atherosclerosis Reports (2022)
-
Simultaneous Determination of Bempedoic Acid and Ezetimibe in Rat Plasma Using HPLC–PDA and Its Applications to a Pharmacokinetic Study
Chemistry Africa (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.