Abstract
Propylene glycol and glycerol are electronic cigarettes vehicles allowing liquid vaporization and nicotine transport. The respective effects of these different constituents on the cardiovascular system are unknown. We assessed the differential effects of vehicles (propylene glycol and glycerol) and nicotine on microcirculatory function, arterial stiffness, hemodynamic parameters and oxidative stress. Twenty-five tobacco smokers were exposed to vaping with and without nicotine, and sham vaping, in a randomized, single blind, 3-period crossover design study. Neither sham-vaping nor vaping in the absence of nicotine resulted in modifications of cardiovascular parameters or oxidative stress. In contrast, vaping with nicotine: 1) impaired acetylcholine mediated vasodilation (mean ± standard error mean) (area under curve, perfusion unit (PU), 3385 ± 27PU to 2271 ± 27PU, p < 0.0001); 2) increased indices of arterial stiffness, namely augmentation index corrected for heart rhythm (−3.5 ± 1.5% to 1.9 ± 2.3%; p = 0.013) and pulse wave velocity (4.9 ± 0.1 m.s−1 to 5.3 ± 0.1 m.s−1; p < 0.0001); 3) increased systolic and diastolic blood pressures as well as heart rate (all p < 0.0001) and finally; 4) raised plasma myeloperoxidase (median [interquartile range]) (13.6 ng.ml−1 [10–17.7] to 18.9 ng.ml−1 [12.2–54.4], p = 0.005). Our findings demonstrated that high temperature e-cigarette vehicle vaporization does not alter micro- and macro-vascular function, and oxidative stress, and that these effects are solely attributable to nicotine.
Similar content being viewed by others
Introduction
Electronic cigarettes (e-cigarettes) are battery-powered devices that aerosolize a liquid (i.e. “e-liquid”) composed of propylene glycol (PG) and/or glycerol (GLY), flavorings and most commonly, nicotine. Suspension of fine particles in a gas forms the aerosol, that is inhaled (i.e. “vaped”)1,2. Literature suggests that e-cigarettes vaping may be safer than tobacco smoking3,4. In addition to be a smoking cessation aid5; e-cigarettes are also used for recreational purposes6. About 5% of adults in the western world are current e-cigarettes users7.
Since its first sales in the 2000s, the growing e-cigarettes market has quickly evolved and is poised to grow over $47 billion by 20258. E-cigarettes are becoming increasingly powerful and deliver now high energy level to low coil resistance (sub-ohm vaping). Sub-ohm vaping increases the temperature of the coil in contact with e-liquid impregnated wick9. The sub-ohm modality enhances vapor and heat production9,10,11,12, and is accompanied by a decrease of nicotine concentration in the e-liquid, which is in turn vaped in larger amount to maintain a sufficient nicotine plasma level13,14.
Several studies have demonstrated endothelial dysfunction, oxidative stress imbalance and arterial stiffness increase after vaping e-cigarette with nicotine15,16,17. The pharmacological actions of nicotine make it impossible to distinguish the respective effects of the carriers themselves (PG and GLY) and nicotine on the endothelial dysfunction, oxidative stress and arterial stiffness increase they observed15. Nicotine is an alkaloid which rise blood pressure and heart rate, and induces vasoconstriction through mechanisms such as catecholamine releases and endothelial dysfunction18. PG and GLY can undergo combustion when vaporized at high wattage and thereby produce carbonyls, which are known cardiovascular toxicants15,19,20. Although the carbonyls produced in realistic vaping conditions are likely far less than during tobacco combustion21, a potential toxic effect on the cardiovascular system cannot be excluded15.
Using a placebo-controlled, randomized, single blind crossover design study, we tested the hypothesis that the PG and GLY carriers do not affect the cardiovascular system in contrast to the nicotine contained in the e-liquid which exerts toxic effects on micro- and macrovascular function when occasional tobacco smokers vape at high temperature.
Methods
Additional information on the study design and the details of the methods is provided in the data supplement. The datasets generated during and/or analyzed during the current study are available from the corresponding author.
Participants
Twenty-five healthy occasional tobacco smokers (18 males; mean age 23 ± 0.4 years; weight 72 ± 2 kg; height 178 ± 2 cm; body mass index 23 ± 0.4 kg.m−2; median cumulative pack-year 0.2 [interquartile range 0.1–0.8]) were enrolled at our academic center (Erasme University Hospital, Brussels, Belgium) between January 2017 and November 2017. Participants were enrolled on the basis of their excellent vaping tolerance. An informed consent was obtained from all the study participants after having received complete information about the study design, which was approved by the local Ethics Committee (Hôpital Erasme - CCB: B406201629930) and conformed to the Declaration of Helsinki. The study is registered at ClinicalTrials.gov (January 30, 2017), identifier NCT03036644.
Study design, randomization and masking
This randomized study was placebo-controlled, single-blind with a three-period crossover design. The periods consisted of: 1) vaping without nicotine; 2) vaping with nicotine; and 3) sham-vaping. Allocation to the sequence order was performed according to a computer-generated randomization list (Flow diagram of the participants course during the study - CONSORT–in appendix). The investigators were unaware of the experimental session since allocation and exposure to the sessions was supervised by an unblinded member who did not participate in any other aspect of the study. Volunteers were unmasked since they could notice that the vaping device was turned on or off.
Vaping protocol
The carrier used in the two e-liquids was a mix of 50% PG and 50% GLY pharmaceutical grade (Fagron©, Waregem, Belgium). One e-liquid was nicotine free (0 mg.ml−1), whereas nicotine (Nicobrand©, Coleraine, UK) was added to the other one at a concentration of 3 mg.ml−1. A last-generation high-power vaping device with popular and commercially available parts in U.S (Smoke©, Shenzen, China) was used. E-cigarettes were set-up at 60 Watts (0.4Ω dual coils). Vaping sessions (with and without nicotine) consisted of 25 puffs (4-s puffs at 30-s intervals) in order to create sub-ohm vaping conditions (personal data, please see data supplement)9. During the sham-vaping session, strict supervision of the participants ensured that they followed exactly the same respiratory maneuvers, but with the e-cigarette turned off.
Study assessments
Indices of skin microcirculatory blood flow (Laser Doppler imager (Moor©))
By using a laser Doppler imager (MOORLDI2-IR, Moor Instruments©, Axminster, UK)22, we measured acetylcholine (Ach) and sodium nitroprusside (SNP) hyperemia at the level of the right forearm (middle part) 60 minutes after vaping and sham-vaping. Ach and SNP were administered percutaneously using iontophoresis22,23. On the contralateral forearm, we tested the skin hyperemic response to local heating after pretreatment with L-N-arginine-methyl-ester (L-NAME) or saline (placebo) iontophoresis, to evaluate nitric oxide (NO)-mediated vasodilation22,23. Skin blood flow was measured automatically (LDI version 5.3D software, Moor Instruments©) and was expressed in perfusion units, PU (arbitrary units of blood flow).
Hemodynamic parameters
Finger systolic and diastolic blood pressure (SBP and DBP) waveforms were obtained throughout the sessions with a beat-to-beat hemodynamic monitoring system (Finometer Pro, FMS©, Amsterdam, the Netherlands) on the right middle finger24.
Arterial stiffness assessment
Aortic wave reflection assessment: Central aortic hemodynamics, and augmentation index corrected for heart rate (AIx75), were estimated using pulse wave and wave separation analysis (SphygmoCor Px system©; Atcor Medical, Sydney, Australia) as previously described25. Measurements were made ten minutes before and five-minute after exposure.
Pulse wave velocity measurements: The carotid-femoral pulse wave velocity (PWV) was determined, immediately before and ten-minute after exposure, from sequential waveform measurements at carotid and femoral sites, by means of applanation tonometry and SphygmoCor software26.
Oxidative stress and nicotine assessment
Blood was drawn in the left antecubital vein 15 minutes before and 30 minutes after vaping (with and without nicotine) or sham-vaping. Total myeloperoxidase, protein-bound 3-chlorotyrosine and homocitrulline were measured in the plasma as previously described27,28. Nicotine was assessed in the serum before and 30 minutes after the nicotine vaping exposure by means of a mass spectrometer (Agilent QQQ 6490, Agilent©, Santa Clara, USA) with a jet stream electrospray ion source and an Agilent 1260 series LC system was used for quantification of plasma nicotine.
Data analysis
This is presented in the Data Supplement.
Outcome measures
The primary outcome was the impact of vaping on skin microcirculatory blood flow function (Ach mediated vasodilation). Secondary outcomes included continuous hemodynamic parameters, arterial stiffness and oxidative stress analyses after exposure.
Statistical analysis
Continuous data were tested for normality using the Kolmogorov-Smirnov test. If the data were normally distributed, the data were expressed in mean ± (standard error of the mean) or if not median [interquartile range, P25–P75]. To our knowledge, the effects of vaping on skin microcirculatory blood flow has not yet been assessed. Therefore, sample calculation was not possible, but a posteriori computation leaded to more than 90% power for the primary end-point (Ach mediated vasodilation). We finally computed statistics on 21 subjects (7 by group, due to missing values in some groups) in a 3 × 3 cross-over trial testing three periods: vaping without nicotine, vaping with nicotine and sham-vaping in a random order. The statistical analysis consisted in 3 × 3 ANOVA for cross-over design. Carry-over effect and time effect were not significant. Therefore, the three periods were pooled leading to 21 measures for vaping without nicotine, vaping with nicotine and sham-vaping. The three periods were compared using an ANOVA for repeated measures or a Friedman test depending if the data were Gaussian or not. If the F-value was significant, pairwise comparisons were made using either a paired Student t-test or Wilcoxon signed rank test accordingly. The Bonferroni’s correction was applied. Effect of the three experimental sessions on hemodynamic variables were assessed by a two-factors (session, time) ANOVA with repeated measures on time and interaction session × time including baseline measurements. Pairwise comparisons were performed as previously described. Correlation analyses used the Spearman non-parametric correlation coefficient. All these analyses were performed using SPSS software version 22 (Chicago, USA). A p-value < 0.05 was considered significant.
Data availability statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
As mentioned in the methods
An informed consent was obtained from all the study participants after having received complete information about the study design, which was approved by the local Ethics Committee (Hôpital Erasme - CCB: B406201629930) and conformed to the Declaration of Helsinki. The study is registered at ClinicalTrials.gov (January 30, 2017), identifier NCT03036644.
Results
There were no differences in any baseline variables in the study population between the three sessions (Table 1). The mean e-liquid volume consumed after sham-vaping, vaping without nicotine and vaping with nicotine was 0.08 ± 0.02 ml, 2.1 ± 0.2 ml (p vs. sham-vaping < 0.0001) and 1.7 ± 0.2 ml (p vs. sham-vaping < 0.0001; and p vs. vaping without nicotine = 0.09), respectively.
Primary outcome
Effect of vaping on acetylcholine and sodium nitroprusside hyperemia (endothelial-dependent and -independent vasodilation)
Sixty minutes after vaping with nicotine, Ach mediated vasodilation was decreased in comparison to sham-vaping (area under the curve (AUC), 3385 ± 27 PU to 2271 ± 27 PU; p < 0.0001) and vaping without nicotine (AUC, 3207 ± 35 PU to 2271 ± 27 PU; p < 0.0001) (Fig. 1a). Vasodilatory responses to SNP were not affected by nicotine vaping (ANOVA session effect; p > 0.8) (Fig. 1b). Compared to vaping without nicotine or sham vaping, the Ach/SNP ratio decreased in case of nicotinic vaping from 1.3 ± 0.06 to 0.9 ± 0.05 (p < 0.001 vs vaping without nicotine and p < 0.0001 vs sham-vaping). In comparison to sham-vaping, nicotine free vaping exposure did not affect skin vasodilator responses to Ach (p > 0.2; Fig. 1a) nor SNP (ANOVA session effect; p > 0.8; Fig. 1b).
Endothelial microcirculatory function. Effect of (a) acetylcholine and (b) sodium nitroprusside iontophoresis after sham-vaping (open circle), nicotine free vaping (open square) and nicotine vaping (closed triangle). Effect of skin pretreatment by saline (continuous line) and L-N-arginine-methyl-ester (dotted line) iontophoresis on skin hyperemic response to local heating (c) after sham vaping, nicotine free vaping and nicotine vaping. Nicotine vaping decreased acetylcholine mediated vasodilation in comparison to sham-vaping (p < 0.0001) and vaping without nicotine (p < 0.0001). Sodium nitroprusside induced vasodilation was not affected by any of the three experimental sessions (ANOVA session effect; p > 0.8). Vasodilation induced by heat in presence of saline or L-N-arginine-methyl-ester were not affected by vaping with and without nicotine and sham-vaping (ANOVA session effect; p > 0.1). BSL indicates baseline; Scan 1 → 10 denotes the time from the first scan to the last scan (150 s per scan).
Effect of vaping on skin thermal hyperemia in presence of L-N-arginine-methyl-ester (endothelial NO bioavailibility)
None of the three experimental sessions affected the skin vasodilatory response to heating in the control condition (pretreatment with normal saline) (ANOVA session effect; p > 0.9; Fig. 1c) nor the response to heating after pretreatment with L-NAME (ANOVA session effect; p > 0.1) (Fig. 1c) or the delta heating-AUC between control and L-NAME pretreated skin (ANOVA session effect; p > 0.1).
Secondary outcomes
Hemodynamic variables
In comparison to baseline, nicotinic vaping induced a sustained rise in SBP and DBP as well as in heart rate (Fig. 2) with the peaks reached during the exposure: 1) SBP from: 109 ± 1 mm Hg to 121 ± 2 mm Hg (p < 0.0001; Fig. 2a); 2) DBP from: 68 ± 1 mm Hg to 78 ± 2 mm Hg (p < 0.0001; Fig. 2b); and 3) heart rate from: 59 ± 1 bpm to 77 ± 3 bpm (p < 0.0001; Fig. 2c). This rise in SBP persisted approximately 60 min after vaping, and lasted for 120 min for DBP and heart rate. Compared to baseline, nicotine free vaping increased SBP and DBP during the limited period of exposure but not thereafter: 1) SBP from: 111 ± 2 mm Hg to 118 ± 5 mm Hg (p < 0.001; Fig. 2a); and 2) DBP from: 68 ± 1 mm Hg to 73 ± 2 mm Hg (p < 0.01; Fig. 2b).
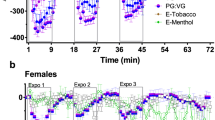
Hemodynamic parameters. Changes in (a) systolic blood pressure (SBP), (b) diastolic blood pressure (DBP) and (C) heart rate (HR) over time in the sham-vaping (open circle), nicotine free vaping (open square) and nicotine vaping (closed triangle) sessions. Nicotine vaping, compared to baseline (BSL), was associated with an increase in systolic and diastolic blood pressure as well as heart rate for 60 minutes, 120 minutes and 120 minutes post-exposure, respectively. In comparison to BSL, vaping without nicotine increased diastolic blood pressure and heart rate during the limited period of exposure. p-value for the time*session interaction effects for systolic and diastolic blood pressure as well as for heart rate were <0.001, <0.0001 and <0.0001, respectively. p-value for comparisons vs. BSL: *p < 0.05, **p < 0.01, ***p < 0.001. Data are the mean ± SEM.
Aortic wave reflection and pulse wave velocity
In comparison to baseline, vaping with nicotine increased the AIx75 (−3.5 ± 1.5% to 1.9 ± 2.3%; p = 0.013) and PWV (4.9 ± 0.1 m. s−1 to 5.3 ± 0.1 m. s−1; p < 0.0001). In contrast, vaping without nicotine and sham-vaping affected neither AIx75 (p > 0.6 vs baseline and p > 0.3 vs baseline, respectively) nor PWV (p > 0.8 vs baseline and p > 0.4 vs baseline, respectively) (Table 2).
Oxidative stress biomarkers and nicotine concentration assessments
Plasma myeloperoxidase and its oxidized proteins products: Compared to baseline, plasma myeloperoxidase increased after nicotine vaping exposure (13.6 ng. ml−1 [10–17.7] to 18.9 ng. ml−1 [12.2–54.4], p = 0.001), but did not do so after vaping without nicotine or sham-vaping (p > 0.3 and p > 0.4, respectively). In the nicotine vaping session, the Ach/SNP ratio was inversely correlated to the rise in myeloperoxidase in the plasma (r = −0.53, p = 0.017). Vaping with nicotine and sham-vaping did not affect concentrations of serum protein-bound 3-chlorotyrosine/tyrosine ratio or homocitrulline/lysine ratio (All p > 0.2). Compared to baseline, vaping without nicotine decreased protein-bound 3-chlorotyrosine/tyrosine ratio (x10−6) (59.8 [49–67.5] to 57.1 [45.7–62.6]; p = 0.004) (Table 2).
Serum nicotine concentration: In the nicotinic vaping session, baseline median nicotine level was 0 ng. ml−1 [0–0] and rose to 8.9 ng.ml−1 [6.9–16.3] 30 minutes after vaping (p < 0.0001 vs. baseline). Serum nicotine concentration did not correlate with any of the parameters we assessed, except with the total amount of nicotinic e-liquid vaped (r = 0.68, p = 0.001).
Discussion
The main new findings of our study can be summarized as follow: in young and healthy tobacco smokers, acute exposure to high temperature vaporization of a pharmaceutical grade nicotine free PG/GLY mix (50:50): (1) did not alter microcirculatory function as well as arterial stiffness and oxidative stress; (2) whereas vaping the same mix plus nicotine decreased microcirculatory endothelial-dependent function, increased arterial stiffness, provoked a sustain raise in blood pressure and heart rate and increased plasma myeloperoxidase.
E-cigarettes are mainly used to quit smoking by former tobacco smokers who often suffer from cardiovascular disease5,15. The efficiency of nicotine replacement therapies is primarily determined by relief of smoking abstinence symptoms. Last generation high output wattage e-cigarettes, which vaporize large amount of e-liquid per puff, have been shown efficient to relieve these symptoms as they deliver quickly a high nicotine level29,30. Former smokers who completely shift to e-cigarettes purchase the last generation e-cigarettes we used in this study12,13, which make our results especially relevant for cardiovascular disease prevention. We are not aware of other studies which assess the acute cardiovascular effects of these new devices vaporizing e-liquid at high temperature. The cardiovascular parameters we measured have been shown very sensitive and reproducible to detect subtle changes in vascular regulation after acute exposure to various stimuli, and are commonly used to identify increased cardiovascular risk population22,23,25,26. The intense vaping conditions used in our study were intended to maximize our ability to detect any harmful effect of e-cigarette on microcirculation, arterial stiffness, hemodynamic parameters and oxidative stress. Overheated PG/GLY produces free radicals and volatile carbonyls (i.e. acrolein) by thermal degradation, which are potent vasoconstrictors and oxidative stressors15,19,20,21. When they are weaned from tobacco smoking, regular high wattage e-cigarettes users decrease nicotine concentration in the e-liquid, which in turn is vaped in larger amounts and thereby enhance volatile carbonyls emission31. The e-cigarette we used has been shown to emit these volatile carbonyls9, but using this device without nicotine under intense use conditions altered none of the above-mentioned parameters in our study.
Participants’ serum nicotine concentrations at 30 minutes after nicotine vaping were similar to those attained after tobacco cigarette smoking or last generation e-cigarettes vaping in other studies14,32. The symptomatic effects of nicotine are highly variable33 since all subjects achieved normal values of serum nicotine concentration after vaping, but four participants experimented nevertheless nicotinic symptoms (e.g. stomach ache, headache and weakness) and nine complained of some degree of throat irritation34. The sympathetic nervous system is activated when nicotine binds its cholinergic receptors, and this activates the cardiovascular system. The sympathomimetic effects of nicotine are mediated by the following mechanisms: activation of peripheral chemoreceptors, direct effects on the brain stem, intrapulmonary chemoreceptors stimulation, catecholamine release from the adrenals and direct release of catecholamines from vascular nerve endings. Among the numerous nicotine-released neurotransmitters, epinephrine, norepinephrine, dopamine, Ach, serotonin or also vasopressin could contribute to effects of nicotine on blood vessels15. We found that nicotine impaired Ach mediated vasodilation without disturbing the hyperemic test in response to heating after L-NAME or saline (placebo) pretreatment. Ach dilates vessels mainly by activation of NO synthase and prostaglandin (PG) production35. The heat-induced hyperemia in the presence of L-NAME assesses chiefly the contribution of the NO-mediated vasodilation in this response22,23. Thus, our results suggest that nicotine alters vasodilatation rather through a PG -dependent than a NO-dependent pathway. This is in agreement with studies where nicotine decreased PG synthesis in the vascular endothelium via an increase in oxidative stress36,37,38. Although not formally observed in our study, nicotine can also impair NO bioavailability39. Differences in the route and rate of nicotine administration, as well as the evidence that the effects of nicotine are highly variable in function of its pharmacokinetics, could perhaps explain these differences18,33. In addition, the variability in nicotine pharmacodynamics, and the limited number of subjects investigated in this study, could explain the lack of correlations between serum nicotine concentration and cardiovascular or oxidative stress parameters we assessed18,33.
We found that the oxidative effector enzyme myeloperoxidase increased in plasma early after nicotine vaping, but not in case of nicotine-free vaping. Myeloperoxidase is mainly stored in the azurophil granules of the polymorphonuclear neutrophils and monocytes40. Neutrophils are activated in the sputum of e-cigarettes users, but whether this can be attributed specifically to the effects of nicotine per se is unknown41. Whereas myeloperoxidase has a protective role in inflammatory processes, persistent generation of myeloperoxidase-derived oxidants may become deleterious and can also contribute to the development of cardiovascular diseases. Plasma myeloperoxidase levels are positively correlated with an increased cardiovascular risk42. The magnitude of microvascular endothelial dysfunction after nicotine vaping was related to the rise of plasma myeloperoxidase in our participants. In vitro nicotine exposure has been shown to activate leucocytes and promote release of myeloperoxidase acutely, and this impaired Ach mediated vasodilation42, as we also observed. Myeloperoxidase-induced endothelial dysfunction could be in part mediated by NO-independent mechanisms, an observation supported by the fact that NO-mediated vasodilation remained unaffected in our study. The other effects we observed on micro- and macro-circulatory functions, such as endothelial dysfunction and the rises in blood pressure, heart rate and arterial stiffness, are in good agreement with previous studies on the acute cardiovascular effects of nicotine15,18. Nicotine exerts pharmacologic effects that could contribute to acute cardiovascular events and accelerated atherogenesis experienced by cigarette smokers. Studies of nicotine medications indicate that the risks of nicotine without tobacco combustion are low compared to cigarette smoking, but are still of concern in people with cardiovascular disease15,18,43. Although PG/GLY vaporization under intense use conditions did not disturb cardiovascular function, this should however not motivate vapers to do so, since our results address only the effects of a single acute exposition on the cardiovascular system, while other important target organs such as the upper and lower airways were not assessed in this study.
We enrolled only occasional smokers with low cumulative cigarettes pack-year in this study, instead of never-smokers, because we believed that the latter would not be able to vape e-cigarettes as required in this protocol. Thus, our results may not necessarily apply to other groups such as heavy smokers and non-smokers. In addition, older subjects, with a higher cardiovascular risk or lung disease were not studied, and our results cannot be extrapolated to such conditions. Another limitation of this study is the small number of subjects investigated as well as the absence of their blinding during the exposure; but the latter is an intrinsic limitation of this kind of study. The participants were carefully selected and only those able to vape at high wattage were recruited, the majority of them reported to inhale the vapor directly to the lungs; which is not practiced by all the vapers. Twenty-five puffs lasting 4 seconds with more than 1.5 ml vaporized were investigated, this is quite different of regular vapers habits, who instead vape a total of 120–235 puffs a day during several sessions and consume a mean of 4 ml e-liquid per day44. Thus although our study resulted in a larger inhalation of e-liquid over a shorter period of time, there is no reason to believe that cardiovascular safety of PG/GLY inhalation in large amount we assessed would be more detrimental when used in lesser quantity. Last, regular vapers may not disclose the same response that the occasional smokers we investigated and this will require also further studies.
In conclusion, our study reveals the new finding that high temperature e-cigarette vehicles vaporization and inhalation in occasional smokers does not alter micro and macrovascular endothelial function, as well as oxidative stress. These effects are merely attributable to the nicotine present in the e-liquid.
References
Dinakar, C. & O’Connor, G. T. The health effects of electronic cigarettes. N Engl J Med. 375, 1372–1381, https://doi.org/10.1056/NEJMra1502466 (2016).
Chun, L. F., Moazed, F., Calfee, C. S., Matthay, M. A. & Gotts, J. E. Pulmonary toxicity of e-cigarettes. Am J Physiol Lung Cell Mol Physiol. 313, L193–L206, https://doi.org/10.1152/ajplung.00071.2017 (2017).
McNeill, A. et al. E-cigarettes: an evidence update. Public Health England, August 2015. https://www.gov.uk/government/publications/e-cigarettes-an-evidence-update (accessed November 30, 2017).
Piepoli, M. F. et al. European guidelines on cardiovascular disease prevention in clinical practice: The Sixth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of 10 societies and by invited experts) Developed with the special contribution of the European Association for Cardiovascular Prevention & Rehabilitation (EACPR). Eur Heart J. 37, 2315–81, https://doi.org/10.1093/eurheartj/ehw106 (2016).
Pasquereau, A., Guignard, R., Andler, R. & Nguyen-Thanh, V. Electronic cigarettes, quit attempts and smoking cessation: a 6-month follow-up. Addiction. 112, 1620–1628, https://doi.org/10.1111/add.13869 (2017).
Pepper, J. K. et al. Risk Factors for Youth E-Cigarette “Vape Trick” Behavior. J Adolesc Health. https://doi.org/10.1016/j.jadohealth.2017.05.010 (2017).
Kasza, K. A. et al. Tobacco-Product use by adults and youths in the united states in 2013 and 2014. N Engl J Med. 376, 342–353, https://doi.org/10.1056/NEJMx170001 (2017).
Global e-cigarette & vaporizer, device and aftermarket, analysis and forecast, 2016–2025. https://www.researchandmarkets.com/reports/3845485/global-e-cigarette-and-vaporizer-device-and (accessed November 30, 2017).
Talih, S. et al. “Juice Monsters”: Sub-ohm vaping and toxic volatile aldehyde emissions. Chem Res Toxicol. 30, 1791–1793, https://doi.org/10.1021/acs.chemrestox.7b00212 (2017).
Barrington-Trimis, J. L. et al. Type of e-cigarette device used among adolescents and young adults: Findings from a pooled analysis of 8 studies of 2,166 vapers. Nicotine Tob Res, https://doi.org/10.1093/ntr/ntx069 (2017).
Etter, J. F. Throat hit in users of the electronic cigarette: An exploratory study. Psychol Addict Behav. 30, 93–100, https://doi.org/10.1037/adb0000137 (2016).
Yingst, J. M. et al. Factors associated with electronic cigarette users’ device preferences and transition from first generation to advanced generation devices. Nicotine Tob Res. 17, 1242–6, https://doi.org/10.1093/ntr/ntv052 (2015).
Dawkins, L. E., Kimber, C. F., Doig, M., Feyerabend, C. & Corcoran, O. Self-titration by experienced e-cigarette users: blood nicotine delivery and subjective effects. Psychopharmacology (Berl). 233, 2933–41, https://doi.org/10.1007/s00213-016-4338-2 (2016).
Marsot, A. & Simon, N. Nicotine and cotinine levels with electronic cigarette: A Review. Int J Toxicol. 35, 179–85, https://doi.org/10.1177/1091581815618935 (2016).
Benowitz, N. L. & Fraiman, J. B. Cardiovascular effects of electronic cigarettes. Nat Rev Cardiol. 14, 447–456, https://doi.org/10.1038/nrcardio.2017.36 (2017).
Carnevale, R. et al. Acute Impact of Tobacco vs Electronic Cigarette Smoking on Oxidative Stress and Vascular Function. Chest. 150, 606–12, https://doi.org/10.1016/j.chest.2016.04.012 (2016).
Vlachopoulos, C. et al. Electronic Cigarette Smoking Increases Aortic Stiffness and Blood Pressure in Young Smokers. J Am Coll Cardiol. 67, 2802–2803, https://doi.org/10.1016/j.jacc.2016.03.569 (2016).
Benowitz, N. L. & Burbank, A. D. Cardiovascular toxicity of nicotine: Implications for electronic cigarette use. Trends Cardiovasc Med 26, 515–23, https://doi.org/10.1016/j.tcm.2016.03.00 (2016).
Jensen, R. P., Strongin, R. M. & Peyton, D. H. Solvent Chemistry in the Electronic Cigarette Reaction Vessel. Sci Rep. 7, 42549, https://doi.org/10.1038/srep42549 (2017).
Geiss, O., Bianchi, I. & Barrero-Moreno, J. Correlation of volatile carbonyl yields emitted by e-cigarettes with the temperature of the heating coil and the perceived sensorial quality of the generated vapours. Int J Hyg Environ Health. 219, 268–77, https://doi.org/10.1016/j.ijheh.2016.01.004 (2016).
Farsalinos, K. E., Voudris, V. & Poulas, K. E-cigarettes generate high levels of aldehydes only in ‘dry puff’ conditions. Addiction. 110, 1352–6, https://doi.org/10.1111/add.12942 (2015).
Dreyfuss, C. et al. L-NAME iontophoresis: a tool to assess NO-mediated vasoreactivity during thermal hyperemic vasodilation in humans. J Cardiovasc Pharmacol. 61, 361–8, https://doi.org/10.1097/FJC.0b013e3182858f81 (2013).
Wauters, A. et al. Acute exposure to diesel exhaust impairs nitric oxide-mediated endothelial vasomotor function by increasing endothelial oxidative stress. Hypertension. 62, 352–8, https://doi.org/10.1161/HYPERTENSIONAHA.111.00991 (2013).
Guelen, I. et al. Finometer, finger pressure measurements with the possibility to reconstruct brachial pressure. Blood Press Monit 8, 27–30 (2003).
Adamopoulos, D. et al. Acute effects of nicotine on arterial stiffness and wave reflection in healthy young non-smokers. Clin Exp Pharmacol Physiol. 36, 784–9, https://doi.org/10.1111/j.1440-1681.2009.05141.x (2009).
Doupis, J., Papanas, N., Cohen, A., McFarlan, L. & Horton, E. Pulse wave analysis by applanation tonometry for the measurement of arterial stiffness. Open Cardiovasc Med J. 10, 188–95, https://doi.org/10.2174/1874192401610010188 (2016).
Franck, T. et al. A new easy method for specific measurement of active myeloperoxidase in human biological fluids and tissue extracts. Talanta. 80, 723–9, https://doi.org/10.1016/j.talanta.2009.07.052 (2009).
Delporte, C. et al. Simultaneous measurement of protein-bound 3-chlorotyrosine and homocitrulline by LC-MS/MS after hydrolysis assisted by microwave: application to the study of myeloperoxidase activity during hemodialysis. Talanta. 99, 603–9, https://doi.org/10.1016/j.talanta.2012.06.044 (2012).
Farsalinos, K., Poulas, K. & Voudris, V. Changes in puffing topography and nicotine consumption depending on the power setting of electronic cigarettes. Nicotine Tob Res. https://doi.org/10.1093/ntr/ntx219 (2017).
Spindle, T. R. et al. The influence of a mouthpiece-based topography measurement device on electronic cigarette user’s plasma nicotine concentration, heart rate, and subjective effects under directed and ad libitum use conditions. Nicotine Tob Res. 19, 469–476, https://doi.org/10.1093/ntr/ntw174 (2017).
Kosmider, L., Kimber, C. F., Kurek, J., Corcoran, O. & Dawkins, L. E. Compensatory puffing with lower nicotine concentration e-liquids increases carbonyl exposure in e-cigarette aerosols. Nicotine Tob Res. https://doi.org/10.1093/ntr/ntx162 (2017).
Wagener, T. L. et al. Have combustible cigarettes met their match? The nicotine delivery profiles and harmful constituent exposures of second-generation and third-generation electronic cigarette users. Tob Control. 26, e23–e28, https://doi.org/10.1136/tobaccocontrol-2016-053041 (2017).
Benowitz, N. L., Jacob, P. 3rd, Jones, R. T. & Rosenberg, J. Interindividual variability in the metabolism and cardiovascular effects of nicotine in man. J Pharmacol Exp Ther. 221, 368–72 (1982).
Dawkins, L. & Corcoran, O. Acute electronic cigarette use: nicotine delivery and subjective effects in regular users. Psychopharmacology (Berl). 231, 401–7, https://doi.org/10.1007/s00213-013-3249-8 (2014).
Kellogg, D. L. Jr, Zhao, J. L., Coey, U. & Green, J. V. Acetylcholine-induced vasodilation is mediated by nitric oxide and prostaglandins in human skin. J Appl Physiol (1985) 98, 629–32 (2005).
Bull, H. A., Pittilo, R. M., Woolf, N. & Machin, S. J. The effect of nicotine on human endothelial cell release of prostaglandins and ultrastructure. Br J Exp Pathol. 69, 413–21 (1988).
Zou, M. H. & Bachschmid, M. Hypoxia-reoxygenation triggers coronary vasospasm in isolated bovine coronary arteries via tyrosine nitration of prostacyclin synthase. J Exp Med. 190, 135–9 (1999).
Klein, L. W. Cigarette smoking, atherosclerosis and the coronary hemodynamic response: a unifying hypothesis. J Am Coll Cardiol. 4, 972–4 (1984).
Tonnessen, B. H., Severson, S. R., Hurt, R. D. & Miller, V. M. Modulation of nitric-oxide synthase by nicotine. J Pharmacol Exp Ther. 295, 601–6 (2000).
Csató, V. et al. Myeloperoxidase evokes substantial vasomotor responses in isolated skeletal muscle arterioles of the rat. Acta Physiol (Oxf). 214, 109–23, https://doi.org/10.1111/apha.12488 (2015).
Reidel, B. et al. E-Cigarette Use Causes a Unique Innate Immune Response in the Lung Involving Increased Neutrophilic Activation and Altered Mucin Secretion. Am J Respir Crit Care Med. https://doi.org/10.1164/rccm.201708-1590OC (2017).
Rudolph, T. K. et al. Myeloperoxidase deficiency preserves vasomotor function in humans. Eur Heart J. 33, 1625–34, https://doi.org/10.1093/eurheartj/ehr193 (2012).
Wolk, R. et al. Hemodynamic and autonomic effects of smokeless tobacco in healthy young men. J Am Coll Cardiol. 45, 910–4 (2005).
Etter, J. F. Characteristics of users and usage of different types of electronic cigarettes: findings from an online survey. Addiction 111, 724–33, https://doi.org/10.1111/add.13240 (2016).
Acknowledgements
This study was supported by the “Fonds Erasme pour la Recherche Médicale”, Belgium (M.C.); the “Fondation pour la Chirurgie Cardiaque”, Belgium (M.C.); the “Fondation Emile Saucez-René Van Poucke”, Belgium (M.C.); the “Prix Docteur & Mrs Rene Tagnon”, Belgium (M.C.); the “Fondation IRIS”, Belgium (M.C.); the “Prix de l’Association André Vésale”, Belgium (M.C.); a research grant of Astra Zeneca, Belgium (P.v.d.B.); the “Fonds Fruit de Deux Vies’, Belgium (P.v.d.B.); the “Fond David and Alice Van Buuren”, Belgium (P.v.d.B.).
Author information
Authors and Affiliations
Contributions
M.C. and P.V.D.B. conceived the idea and the design of the study. M.C. has full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. M.C. and C.M. performed the statistical analysis. M.C. enrolled the participants and took outcome measurements. B.D.B., W.Z., A.C. assured the steps of randomization (sequence generation, allocation concealment, and intervention administration). G.D. performed serum nicotine analysis. M.C., F.R., K.Z.B., P.V.A., C.D. performed oxidative stress biomarkers analysis. M.C. drafted the manuscript. C.M., F.R., K.Z.B., P.V.A., C.D., N.D., P.V.D.B. revisited critically the manuscript for important intellectual content. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chaumont, M., de Becker, B., Zaher, W. et al. Differential Effects of E-Cigarette on Microvascular Endothelial Function, Arterial Stiffness and Oxidative Stress: A Randomized Crossover Trial. Sci Rep 8, 10378 (2018). https://doi.org/10.1038/s41598-018-28723-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-28723-0
This article is cited by
-
Effects of Electronic Cigarette Vaping on Cardiac and Vascular Function, and Post-myocardial Infarction Remodeling in Rats
Cardiovascular Toxicology (2024)
-
Evidence of premature vascular dysfunction in young adults who regularly use e-cigarettes and the impact of usage length
Angiogenesis (2024)
-
Varied effects of tobacco smoke and e-cigarette vapor suggest that nicotine does not affect endothelium-dependent relaxation and nitric oxide signaling
Scientific Reports (2023)
-
E-cigarette effects on vascular function in animals and humans
Pflügers Archiv - European Journal of Physiology (2023)
-
Elektrische Zigaretten – Stand der Forschung aus gefäßmedizinischer Sicht
Gefässchirurgie (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.