Abstract
Bacillus anthracis, Yersinia pestis, and Francisella tularensis are the causative agents of Tier 1 Select Agents anthrax, plague, and tularemia, respectively. Currently, there are no licensed vaccines against plague and tularemia and the licensed anthrax vaccine is suboptimal. Here we report F. tularensis LVS ΔcapB (Live Vaccine Strain with a deletion in capB)- and attenuated multi-deletional Listeria monocytogenes (Lm)-vectored vaccines against all three aforementioned pathogens. We show that LVS ΔcapB- and Lm-vectored vaccines express recombinant B. anthracis, Y. pestis, and F. tularensis immunoprotective antigens in broth and in macrophage-like cells and are non-toxic in mice. Homologous priming-boosting with the LVS ΔcapB-vectored vaccines induces potent antigen-specific humoral and T-cell-mediated immune responses and potent protective immunity against lethal respiratory challenge with all three pathogens. Protection against anthrax was far superior to that obtained with the licensed AVA vaccine and protection against tularemia was comparable to or greater than that obtained with the toxic and unlicensed LVS vaccine. Heterologous priming-boosting with LVS ΔcapB- and Lm-vectored B. anthracis and Y. pestis vaccines also induced potent protective immunity against lethal respiratory challenge with B. anthracis and Y. pestis. The single vaccine platform, especially the LVS ΔcapB-vectored vaccine platform, can be extended readily to other pathogens.
Similar content being viewed by others
Introduction
Bacillus anthracis, Yersinia pestis, and Francisella tularensis, the causative agents of anthrax, plague, and tularemia, respectively, are classified as Tier 1 Select Agents of bioterrorism. When B. anthracis, Y. pestis, and F. tularensis infect humans by the respiratory route, the route of greatest concern in an intentional bioterrorist attack, they cause highly fatal diseases - pulmonary anthrax, pneumonic plague, and pneumonic tularemia, respectively. Pulmonary anthrax has a mortality as high as 100% untreated and 45% with treatment1; pneumonic plague is rapidly lethal (~50–90%) untreated2; and pneumonic tularemia has a mortality of up to 40–60% untreated and can be highly fatal even with appropriate antibiotic treatment3. Because B. anthracis, Y. pestis and F. tularensis are relatively easy to manufacture, environmentally hardy, and cause high mortality, they are considered among the most likely pathogens to be employed by terrorists and are consequently classified as Tier 1 Select Agents; indeed, they were developed as bioweapons during WWII and the Cold War4,5.
Although antibiotics can afford protection against B. anthracis, Y. pestis and F. tularensis in animal models, the critical period for treatment following aerosol challenge is very short (24–72 h)6. Furthermore, antibiotic-resistant strains of these pathogens can be developed by genetic engineering4,7, emerge from long-term antibiotic treatment8, or acquired naturally from transferable plasmids9. Hence, relying on currently available antibiotics to counter an intentional outbreak of anthrax, plague, or tularemia is not a practical public health plan. In view of the potential catastrophic consequences of the intentional airborne spread of these pathogens and the increasing development of antibiotic-resistant strains, vaccines are needed to protect against inhaled B. anthracis, Y. pestis, and F. tularensis and other Tier 1 Select Agents. The currently available licensed human anthrax vaccines are the U.S. anthrax vaccine adsorbed (AVA) and the U.K. anthrax vaccine precipitated (AVP); both are undefined acellular subunit vaccines, containing primarily the B. anthracis Protective Antigen (PA) with a lesser amount of Lethal Factor (LF) and other proteins. AVA requires 5 vaccinations followed by annual boosters and its duration of efficacy is unknown. In addition, AVA causes adverse reactions such as local soreness, redness, itching and swelling at the site of injection. The complexity of the immunization schedule and adverse effects of AVA make it unattractive. There are currently no licensed vaccines against plague or tularemia. The Y. pestis EV76 strain was developed and used in humans in the former Soviet Union; however, it has significant toxicity and is not licensed in the U.S.2. The F. tularensis Live Vaccine Strain (LVS) has been extensively studied in the U.S.; this unlicensed vaccine is relatively toxic and provides incomplete protection against aerosolized F. tularensis10. Practically speaking, a single vector platform vaccine against F. tularensis, B. anthracis, and Y. pestis that is highly efficacious is needed as it would simplify manufacture, regulatory approval, clinical evaluation, and vaccine administration, be more acceptable to people than multiple individual vaccines, and be less costly. Currently, no single vector platform vaccine against Tier 1 Select Agents is available.
In the case of B. anthracis and Y. pestis, subunit vaccines including B. anthracis PA and LF antigens or Y. pestis F1 capsular antigen and low calcium response V (LcrV) antigen in adjuvants or vaccines comprising a live attenuated heterologous vector expressing these antigens have induced strong protection in preclinical studies11,12,13,14. However, in the case of F. tularensis, subunit vaccines or vaccines comprising live attenuated heterologous vectors expressing F. tularensis proteins show relatively poor efficacy against high dose F. tularensis aerosol challenge in comparison with LVS, which itself is suboptimal15,16. Thus, protection against aerosolized highly virulent Type A F. tularensis strains requires a live homologous vector such as LVS or deletional mutants of LVS or Type A F. tularensis strains. Our live homologous LVS ΔcapB vector has significant advantages over the alternative approaches of single-deletional (unsafe) or double-deletional (ineffective) mutants of virulent Type A F. tularensis in terms of safety, efficacy, and regulatory approval. While >10,000-fold less virulent than the toxic LVS strain in mice, LVS ΔcapB is highly protective - ~100% protection against aerosolized F. tularensis SchuS4 after intranasal (i.n.) immunization, and strong protection after intradermal (i.d.) immunization17. rLVS ΔcapB expressing F. tularensis proteins induces strong cellular and humoral immune responses and protection comparable to immunization with LVS after single i.n. and i.d. immunization either as a standalone vaccine or as a prime vaccine to animals heterologously boosted with recombinant Listeria monocytogenes (Lm) expressing IglC (rLm/iglC)18,19. However, whether multiple i.d. doses of the non-toxic rLVS ΔcapB expressing the F. tularensis fusion protein comprising the immunodominant domains of IglA, IglB, and IglC (rLVS ΔcapB/iglABC) would yield even greater protection, e.g. protection greater than that of LVS, has not been investigated. Finally, optimal immunoprotection against Y. pestis requires T-cell responses20,21 and the live vectors proposed here induce such responses.
Attenuated Lm vectors, including Lm ΔactA, Lm ΔactA ΔinlB, and Lm ΔactA ΔinlB ΔuvrAB prfA(G155S) (abbreviated as Lm ΔactA ΔinlB prfA hereafter), have been developed as vaccine vectors for delivery of cancer and infectious diseases antigens and have major advantages over other vectors as described by us and others15,18,22,23,24.
Here we describe a novel single vector vaccine platform against Tier I Select Agents B. anthracis, Y. pestis, and F. tularensis comprising LVS ΔcapB as a vaccine vector to express heterologously immunoprotective domains of B. anthracis LF and PA antigens or Y. pestis F1 and LcrV antigens, or to overexpress homologously F. tularensis immunodominant domains of IglA, IglB, and IglC19, respectively. We compare the immunogenicity and efficacy of homologous priming-boosting with the single LVS ΔcapB vectored vaccine platform with that of heterologous priming-boosting with the LVS ΔcapB - Lm vectored vaccine platform where the vaccines express the same immunoprotective antigens. We show that homologous priming-boosting with individual rLVS ΔcapB vaccines expressing B. anthracis, Y. pestis, and F. tularensis antigens induces potent protection against respiratory challenge with lethal doses of all three pathogens – potency superior to that of the existing licensed AVA vaccine against B. anthracis challenge and the unlicensed and toxic LVS vaccine against F. tularensis challenge.
Results
Construction and characterization of attenuated recombinant B. anthracis and Y. pestis vaccines
We constructed the following B. anthracis and Y. pestis vaccine candidates by using LVS ΔcapB17 and Lm ΔactA ΔinlB prfA25 as vaccine vectors (Table S1): (1) rLVS ΔcapB/Ba expressing the shuttle plasmid-encoded fusion protein of B. anthracis antigens LF amino-terminal PA binding domain [LFn, 255 aa]26,27 and the PA extended carboxy-terminal host cell receptor-binding domain [PAc, 183 aa]12 separated by a flexible linker GGSG (LFnPAc) and driven by the F. tularensis bfr promoter (upstream of FTT_1441)28; (2) rLVS ΔcapB/Yp expressing the fusion protein of Y. pestis F1 and LcrV (F1V), separated by the GGSG linker and driven by the F. novicida omp promoter (upstream of FTN_1451)29,30; (3) rLm ΔactA ΔinlB prfA/ActAN-Ba and rLm ΔactA ΔinlB prfA/LLOss-Ba expressing the secreted forms of the fusion protein of B. anthracis LFnPAc downstream of the Lm actA promoter, ligated in frame with the actA-encoded N-terminal 100 amino acid of ActA (ActAN-BaLFnPAc), or downstream of the Lm hly promoter, ligated in frame with the hly-encoded Listeriolycin O (LLO) signal sequence (LLOss-BaLFnPAc)24; and (4) rLm ΔactA ΔinlB prfA/ActAN-Yp and rLm ΔactA ΔinlB prfA/LLOss-Yp expressing secreted forms of ActAN-YpF1V and LLOss-YpF1V, respectively.
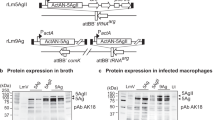
Evaluation of the LVS ΔcapB-vectored vaccines showed that the 51 kDa fusion protein of B. anthracis, LFnPAc, is expressed by rLVS ΔcapB/Ba grown on agar (Fig. 1a, left panel, lane 2), but not by the LVS ΔcapB vector control (lane 1), as detected by monoclonal antibody to B. anthracis PA protein, which also detected the 83-kDa PA protein (lane 3). Similarly, the 55 kDa fusion protein of Y. pestis F1V is expressed by rLVS ΔcapB/Yp grown on agar (Fig. 1a, right panel, lanes 2–5), as detected by goat polyclonal antibody to Y. pestis LcrV, and has a molecular mass similar to the F1-LcrV monomer protein (lane 6). F. tularensis Bfr was detected as a 17-kDa protein31 from the LVS ΔcapB vector as well as from rLVS ΔcapB/Ba (Fig. 1a, left panel, lanes 1 and 2) and rLVS ΔcapB/Yp (Fig. 1a, right panel, lanes 2–5). The expression of the fusion proteins of B. anthracis and Y. pestis was also detected in human macrophage-like THP-1 cells infected with rLVS ΔcapB/Ba as double bands (Fig. 1b, lane 4) and rLVS ΔcapB/Yp as a single band (Fig. 1b, lanes 5 & 6), respectively. Although the rLVS ΔcapB vaccine strains showed somewhat delayed growth kinetics in broth (Fig. S2a), they grew similarly to the parental LVS ΔcapB strain in infected THP-1 cells (data not shown) and in mouse macrophage-like J774A.1 cells (Fig. S3a).
Expression of heterologous fusion proteins of B. anthracis and Y. pestis by rLVS ΔcapB and rLm ΔactA ΔinlB prfA vaccines grown on agar and in infected macrophage-like cells. (a) Expression of B. anthracis (left) and Y. pestis (right) fusion proteins by rLVS ΔcapB grown on agar. Single colonies of chocolate agar grown rLVS ΔcapB/Ba and rLVS ΔcapB/Yp (4 clones) were lysed in SDS sample buffer and lysates analyzed by Western blotting using a mixture of antibody to B. anthracis PA and to F. tularensis Bfr (left panel) or antibody to Y. pestis LcrV protein followed by antibody to Bfr (right panel). Left panel, lane 1, LVS ΔcapB vector; lane 2, rLVS ΔcapB/Ba; lane 3, PA protein control; lane 4, protein mass standards. Right panel, lane 1, protein mass standards; lanes 2–5, rLVS ΔcapB/Yp; lane 6, monomer of F1-LcrV (F1V) protein control. (b) Expression of fusion proteins by rLVS ΔcapB in infected human macrophage-like cells. Monocytic THP-1 cells seeded on 24-well plates and differentiated in the presence of PMA were left uninfected or infected with LVS ΔcapB, rLVS ΔcapB/Ba or rLVS ΔcapB/Yp; cells were lysed at 24 h post infection, and cell lysates analyzed by Western blotting using a mixture of antibody to B. anthracis PA and to Y. pestis LcrV. Lanes 1 & 7, two different protein standards; lane 2, uninfected control; lane 3, LVS ΔcapB; lane 4, rLVS ΔcapB/Ba; lanes 5 and 6, two clones of rLVS ΔcapB/Yp vaccines; lane 8, B. anthracis PA and degraded proteins; lane 9, Y. pestis F1-LcrV monomer protein and degraded proteins. (c) Expression and secretion of heterologous fusion proteins by rLm vaccines in broth. Culture filtrates of Lm vector or rLm vaccines were analyzed by Western blotting using antibody to B. anthracis PA (left panel) or to Y. pestis LcrV (right panel). Left panel, lane 1, protein mass standards; lane 2, Lm vector; lane 3, rLm/ActAN-Ba; lane 4, rLm/LLOss-Ba. Right panel, lane 1, protein mass standards; lane 2, Lm vector; lanes 3 & 4, two clones of rLm/ActAN-Yp; lanes 5 & 6, two clones of rLm/LLOss-Yp. (d) Expression of heterologous fusion proteins by rLm vaccines in infected mouse macrophage-like cells. Monolayers of J774A.1 cells were not infected or infected with a stationary culture of rLm vaccines similarly as described above in the legend to b . Lysates were subjected to Western blotting analysis using antibody to B. anthracis PA (left) or to Y. pestis LcrV (right). Left panel, lane 1, protein standards; lane 2, uninfected control; lane 3, rLm/ActAN-Ba; lane 4, rLm/LLOss-Ba; lane 5, PA protein. Right panel, lane 1, protein standards; lane 2, rLm/ActAN-Yp; lane 3, rLm/LLOss-Yp; lane 4, F1-LcrV protein control. (a–d) On the left border of each panel are listed the masses of protein standards; on the right border are listed the proteins of interest. Each blot was processed by using the Bio-Rad imaging system (ChemiDoc XRS) and Quantity One software, which allows the overlap of a white-light image, for visualization of the protein standards (a, left panel lane 4 and right panel lane 1; b–d, lane 1), and a chemiluminescent image, for visualization of the antibody-labeled protein bands. The full-length blots in panels b–d are shown in the Supplementary Information (Fig. S1).
Lm-vectored vaccines were assessed for expression and secretion of B. anthracis and Y. pestis fusion proteins after growth in broth and in infected mouse macrophage-live J774A.1 cells by evaluating culture filtrates by Western blotting using antibodies specific to B. anthracis PA or to Y. pestis LcrV. As shown in Fig. 1c, the antibody to PA or LcrV detected major protein bands of 59-kDa ActAN-BaLFnPAc (ActAN-Ba) (Fig. 1c, left panel, lane 3), 51-kDa LLOss-BaLFnPAc (LLOss-Ba) (lane 4), 63-kDa ActAN-YpF1V (ActAN-Yp) (Fig. 1c, right panel, lanes 3 & 4), and 56-kDa LLOss-YpF1V (LLOss-Yp) (lanes 5 & 6), expressed and secreted by rLm ΔactA ΔinlB prfA/ActAN-Ba, rLm ΔactA ΔinlB prfA/LLOss-Ba, rLm ΔactA ΔinlB prfA/ActAN-Yp, and rLm ΔactA ΔinlB prfA/LLOss-Yp, respectively, as predicted, but not by the Lm vector controls (Fig. 1c, left and right panels, lane 2). The expression of the fusion proteins of B. anthracis and Y. pestis was also detected from J774A.1 cells infected with rLm ΔactA ΔinlB prfA/ActAN-Ba (Fig. 1d, left panel, lane 3) or rLm ΔactA ΔinlB prfA/LLOss-Ba (lane 4) or with rLm ΔactA ΔinlB prfA/ActAN-Yp (Fig. 1d, right panel, lane 2) or rLm ΔactA ΔinlB prfA/LLOss-Yp (lane 3), respectively. The rLm vaccines strains grew similarly to the parental Lm ΔactA ΔinlB prfA strain in broth (Fig. S2b) and in infected J774A.1 cells (Fig. S3b). Because rLm ΔactA ΔinlB prfA/LLOss-Ba and rLm ΔactA ΔinlB prfA/LLOss-Yp expressed the B. anthracis and Y. pestis fusion proteins more abundantly in both broth and in macrophages than rLm ΔactA ΔinlB prfA/ActAN-Ba and rLm ΔactA ΔinlB prfA/ActAN-Yp vaccines, respectively, we chose to use rLm ΔactA ΔinlB prfA/LLOss-Ba and rLm ΔactA ΔinlB prfA/LLOss-Yp in the following studies where they are hereafter referred to as rLm/Ba and rLm/Yp, respectively.
Initial in vivo studies examined dissemination, clearance, and plasmid stability of the newly constructed B. anthracis and Y. pestis vaccines. Our results showed that rLVS ΔcapB/Ba grew and disseminated similarly to the parental LVS ΔcapB, while rLVS ΔcapB/Yp showed delayed growth and dissemination (Figs S4 and S5). The shuttle plasmid-encoded antigen expression cassettes in rLVS ΔcapB/Ba and rLVS ΔcapB/Yp were stably maintained in mouse liver, spleen, local skin (after i.d. administration), and lung (after i.n. administration) up to 14 days post vaccination (data not shown); The rLm/Ba and rLm/Yp vaccines also showed systemic dissemination, similar to the parental Lm vector, and all were cleared by Day 7 post vaccination (Fig. S6).
Vaccine immunogenicity and protective immunity against pulmonary anthrax
To examine the protective immunity of the LVS ΔcapB- and Lm-vectored B. anthracis vaccines, we sham-immunized the mice, or immunized them twice with AVA (BEI NR-2642, BioThrax) subcutaneously (s.q., its standard route of immunization) in a 100-μL volume after the AVA vaccine was diluted (0.25 ml: 0.75 ml) in sterile PBS32, or immunized homologously with rLVS ΔcapB/Ba mucosally (i.n.) or systemically (i.d.), or heterologously primed with rLVS ΔcapB/Ba (i.n. or i.d.) and subsequently boosted with rLm/Ba [i.n. or i.m.; i.m. is the most immunogenic systemic route for Lm33], as indicated in Fig. 2a. All mice were bled at Week 7, one week prior to challenge; challenged at Week 8 with 205,000 B. anthracis Ames spores (~5 LD50; the pre-determined LD50 for B. anthracis Ames spores was ~40,000 CFU); and monitored for survival for three weeks. Homologous priming-boosting with rLVS ΔcapB/Ba i.n. or i.d. and heterologous priming-boosting with rLVS ΔcapB/Ba – rLm/Ba, i.n./i.n. or i.d./i.m induced elevated PA-, LF- and HI-LVS-specific serum antibodies (Fig. 2b, leftmost panel); the LF- and HI-LVS antibody titers were significantly higher than those of sham- and AVA-immunized mice (Fig. 2b, leftmost and rightmost panels); these live-vectored vaccines tended to induce more LF- and PA-specific IgG2a than IgG1 antibody, representing stimulation of Th1 and Th2 immune responses, respectively (Fig. 2b, middle and rightmost panels). AVA vaccination induced high antibody titers, dominated by IgG1, specific to PA, the major component of AVA vaccine, but not to LF and HI-LVS (Fig. 2b). Systemic homologous priming-boosting with rLVS ΔcapB/Ba (Group D) and heterologous priming-boosting with rLVS ΔcapB/Ba – rLm/Ba i.n./i.n. (Group E) and i.d./i.m (Group F) showed significant protection (P < 0.001–0.01 vs. sham-immunized mice) (Fig. 2c). The licensed AVA vaccine did not induce significant protection compared with sham-immunized mice, and heterologous priming-boosting with rLVS ΔcapB/Ba – rLm/Ba systemically was significantly more protective than the AVA vaccine (P = 0.02) (Fig. 2c). Interestingly, mean survival time three weeks post-challenge correlated with pre-challenge serum antibody to LF but not to PA (Fig. 2d).
Two immunizations by homologous priming-boosting with rLVS ΔcapB/Ba or by heterologous priming-boosting with rLVS ΔcapB/Ba - rLm ΔactA ΔinlB prfA/Ba induce humoral immune responses and protective immunity against respiratory challenge with virulent B. anthracis Ames spores. (a) Experiment schedule. Mice (n = 8/group) were immunized homologously twice, 4 weeks apart, with PBS intranasally (i.n.) (Sham), AVA (0.025 ml) subcutaneously (s.q.), or 106 CFU rLVS ΔcapB/Ba (rLVS/Ba) i.n. or intradermally (i.d.), or heterologously with 106 CFU rLVS ΔcapB/Ba i.n. or i.d. and rLm/Ba i.n. or intramuscularly (i.m.), 4 weeks apart; bled at Week 7; challenged at week 8 with B. anthracis Ames spores (205,000/mouse, ~5 LD50); and monitored for survival for three weeks, as indicated. (b) Serum antibody after vaccination. Sera were assayed for antibody endpoint titer to B. anthracis PA and LF antigens and to F. tularensis heat-inactivated LVS (HI-LVS). Values are mean + SEM of serum antibody endpoint titer for n = 8 mice per group. Differences among individual groups were evaluated by Two-way ANOVA with Tukey’s correction. Values significantly different from the Sham group are marked with asterisks over the comparison groups. *P < 0.05; **P < 0.01; ***P < 0.001; ****P < 0.0001. (c) Survival after vaccination and challenge. The survival curve of each vaccinated group is compared with that of Group A (Sham) or Group B (AVA) by the log-rank test (Mantel-cox); P values for individual vaccine groups significantly different from the Sham or AVA group are marked with asterisks and “§”, respectively, color-coded to the color of the vaccine symbol; **P < 0.01; ***P < 0.001 vs. Sham group; §P < 0.05 vs. AVA group. (d) Correlation between serum antibody and mean survival time. Linear regression was used to obtain values for the slope and intercept and the correlation coefficient (R2) between pre-challenge serum antibody and post-challenge mean survival time at 21 days post-challenge. Two-tailed P values were calculated for the correlation.
Subsequently, we explored the efficacy of three homologous (rLVS ΔcapB/Ba or rLm/Ba) or heterologous (one rLVS ΔcapB/Ba prime + two rLm/Ba boosts) immunizations, both mucosally (i.n.) and systemically (i.d. for rLVS ΔcapB/Ba and i.m. for rLm/Ba), and compared them with that of sham or AVA immunization (s.q.), and with one rLVS ΔcapB/Ba prime + one rLm/Ba boost vaccination, as depicted in Fig. 3a. The immunized animals were bled, subsequently challenged with 371,000 B. anthracis Ames spores (~10 LD50), and monitored for 3 weeks (Fig. 3a). As shown on the left side of Fig. 3b, mice homologously primed-boosted with rLVS ΔcapB/Ba i.n. (Group C) or i.d. (Group D) or with rLm/Ba i.n. (Group E) or i.m. (Groups F) produced significantly greater amounts of B. anthracis PA and/or LF antigen-specific serum IgG antibody, dominated by subtype IgG2a, than sham-immunized mice (Fig. 3b, top left two panels), consistent with the results from Experiment I (Fig. 2a and b) and additional experiments (Fig. S7a–d, Group C). Of note, as in the previous experiment, mice immunized with AVA produced PA-specific antibody, but did not produce LF-specific serum antibody. Upon challenge, mice homologously primed-boosted with rLVS ΔcapB/Ba or rLm/Ba, systemically or mucosally, had greater survival than sham- and AVA-immunized mice; the survival of mice immunized systemically with rLVS ΔcapB/Ba and rLm/Ba and mucosally with rLm/Ba was significantly greater than that of the sham-immunized mice (Fig. 3b, bottom left panel).
Three immunizations by homologous priming-boosting with rLVS ΔcapB/Ba or by heterologous priming-boosting with rLVS ΔcapB/Ba – rLm ΔactA ΔinlB prfA/Ba induce high-level antibody responses and potent protective immunity against virulent B. anthracis respiratory challenge. (a) Experiment schedule. Mice (n = 8/group) were immunized two or three times homologously with 106 CFU rLVS ΔcapB/Ba (rLVS/Ba) or rLm ΔactA ΔinlB prfA/Ba (rLm/Ba) or heterologously first with rLVS/Ba and subsequently with rLm/Ba, as indicated. Controls were sham-immunized with PBS i.d. or with AVA s.q. three times. All mice were bled at week 11; challenged at week 12 with B. anthracis Ames spores (371,000 CFU, ~10 LD50); and monitored for survival for 3 weeks post-challenge. (b) Serum antibody prior to challenge and survival post challenge. Top panels. Sera were assayed for IgG or IgG subtypes IgG1 and IgG2a to B. anthracis PA and LF proteins, as indicated, after homologous (left two panels) and heterologous (right two panels) prime-boost vaccination. Values are mean + SEM of serum antibody endpoint titer for n = 8 per group. Differences in serum endpoint titer among individual groups were analyzed by two-way ANOVA with Tukey’s corrections. *P < 0.05; **P < 0.01; ****P < 0.0001 vs. Sham group. Bottom panels. The survival curve of each vaccinated group, color-coded as indicated in panel b, after homologous (left) and heterologous (right) prime-boost vaccination and challenge is compared with that of the Sham group by the log-rank test (Mantel-cox); P values for vaccine groups that are significantly different from the Sham group are marked with one or more asterisks color-coded to the color of the vaccine symbol. *P < 0.05 and **P < 0.01. (c) Correlation between serum antibody and mean survival time. The correlation coefficient (R2) and one-tailed P values were obtained as described in legend to Fig. 2d.
As shown on the right side of Fig. 3b, mice heterologously primed-boosted with rLVS ΔcapB/Ba - rLm/Ba, mucosally (i.n./i.n.) (Group G & H) or systemically (i.d./i.m.) (Group I & J) also produced significantly greater amounts of B. anthracis PA and LF antigen-specific serum IgG antibody than sham-immunized mice, dominated by subtype IgG2a to PA and LF (Fig. 3b, top right two panels; Fig. S7b–e, Groups E and F), and elevated levels of serum antibodies that neutralized anthrax toxin (assayed in mouse macrophage cell line J774A.1), as did AVA-immunized mice (Fig. S7f, Groups B, E, and F). After challenge, these heterologously primed-boosted mice (Groups G, H, I, J) showed significantly increased survival compared with the sham-immunized mice (P < 0.05 or P < 0.01), whether boosted only once (Groups G and I) or twice (Groups H and J) with rLm/Ba (Fig. 3b, bottom, right panel). In contrast, survival of mice immunized with the AVA vaccine was not significantly different from that of sham-immunized mice (P = 0.3) (Fig. 3b, bottom panels). These results indicate that both systemic and mucosal homologous priming-boosting with rLVS ΔcapB/Ba or rLm/Ba and both systemic and mucosal heterologous priming-boosting with rLVS ΔcapB/Ba - rLm/Ba induce strong protective immunity against lethal respiratory challenge with B. anthracis spores. As in the previous challenge experiment, mean survival time 3 weeks post-challenge correlated with pre-challenge serum antibody to LF but not to PA (Fig. 3c) or to toxin neutralizing antibody (Fig. S8).
To investigate T-cell mediated immune responses induced by rLVS ΔcapB and rLm vaccines, we immunized mice, observed them for signs of discomfort or weight loss, and assayed their lung and spleen cells for cytokine secretion and intracellular cytokine staining in response to in vitro stimulation with B. anthracis and F. tularensis antigens (Figs 4a and S9). After vaccination with rLVS ΔcapB/Ba i.n., rLm/Ba i.n. or i.m., or AVA s.q., mice did not show signs of significant discomfort (e.g. ruffled fur) or weight loss (data not shown). As expected, mice immunized with the rLVS ΔcapB/Ba and rLm/Ba anthrax vaccines developed T-cell mediated immune responses, dominated by Th1 responses (Figs 4 and 5). Lung and spleen cells of mice immunized with rLVS ΔcapB/Ba i.n. twice (Group C) or once (Group D) or heterologously primed-boosted with rLVS ΔcapB/Ba - rLm/Ba i.n./i.n. (Group E) or i.n./i.m. (Group F) secreted much higher levels of IFN-γ and IL-4 in response to LF and HI-LVS than sham- (statistically significant) or AVA-immunized mice (Fig. 4b). In response to LF and HI-LVS, these mice had elevated levels of lung and spleen CD4+ T cells expressing IFN-γ, TNF-α, IL-2, and IL-17A compared with sham- and AVA-immunized mice and greater frequencies of polyfunctional CD4+ T cells expressing IFN-γ, TNF-α, IL-2, and/or IL-17 than sham-immunized mice (Figs. 4c, 5); the heterologously immunized mice had especially high levels of cytokine-expressing CD4+ T cells (Fig. 4c, leftmost and rightmost upper and lower panels), and modestly increased levels of CD8+ T-cells secreting IFN-γ in the lung when boosted i.n. and in the spleen when boosted i.m. (Fig. 4d). In response to PA, CD4+ T-cells from mice heterologously primed-boosted by the i.n. route also had increased cytokine-producing cells in the lung and to a much less extent in the spleen; not unexpectedly, when the booster was instead administered systemically (i.m.), there were increased cytokine positive CD4+ T-cells in the spleen (Fig. 4c, middle upper and lower panels). With a few minor exceptions, the AVA vaccine induced very poor cell-mediated immune responses (Fig. 4b–d). Mice immunized i.d. once with rLVS ΔcapB/Ba or heterologously primed-boosted with rLVS ΔcapB/Ba i.d. – rLm/Ba i.m. also showed enhanced IFN-γ secretion by lung and spleen cells and increased frequencies of lung and spleen CD4+ T cells expressing IFN-γ, TNF-α, IL-2 and/or IL-17A in response to LF and HI-LVS compared with sham-immunized mice and mice immunized with AVA (data not shown). These results indicate that both homologous priming-boosting with rLVS ΔcapB/Ba and heterologous priming-boosting with rLVS ΔcapB/Ba – rLm/Ba vaccines induce F. tularensis and B. anthracis antigen-specific Th1-type cytokine secretion and polyfunctional CD4+ T cells.
Homologous prime-boost vaccination with rLVS ΔcapB/Ba or heterologous prime-boost vaccination with rLVS ΔcapB/Ba - rLm ΔactA ΔinlB prfA/Ba induces antigen-specific cell-mediated immune responses. (a) Experiment schedule. Mice (n = 4/group) were immunized homologously with PBS i.n. (Sham), AVA s.q., or 106 CFU rLVS ΔcapB/Ba (rLVS/Ba) i.n., or heterologously with rLVS/Ba i.n. followed by 106 CFU rLm ΔactA ΔinlB prfA/Ba (rLm/Ba) i.n. or i.m. as indicated. At week 7, all mice were bled, euthanized, and their lung and spleen cells assayed for cytokine secretion and intracellular cytokine staining. (b) Antigen-specific cytokine secretion. Single cell suspensions of lung and spleen cells were stimulated with B. anthracis PA or LF proteins or F. tularensis heat-inactivated LVS (HI-LVS) for 3 days, as indicated, and cell supernatants assayed for interferon gamma (IFN-γ) (left two panels) and IL-4 (right two panels) by ELISA. Shown are the amounts of IFN-γ and IL-4 in the culture supernate in response to PA, LF, and HI-LVS. (c,d) Cytokine-expressing CD4+ (c) and CD8+ (d) T cells. Lung and spleen cells were stimulated with LF, PA, or HI-LVS as indicated at the top of the panels (c) or on the horizontal axis (d) and assayed by intracellular cytokine staining for CD4+ (c) and CD8+ (d) T cells expressing IFN-γ, TNF-α, IL-2, and/or IL-17A. Shown are the frequencies of CD4+ T cells expressing IFN-γ, TNF-α, IL-2, and/or IL-17A (c) and CD8+ T cells expressing IFN-γ (d). Values in b–d are means + SEM. Differences among individual groups were evaluated by Two-way ANOVA with Tukey’s correction. Values significantly different from the Sham group are marked with asterisk(s) over brackets above the comparison groups; *P < 0.05; **P < 0.01; ***P < 0.001; ****P < 0.0001. Results shown are representative of three similar experiments.
Heterologous prime-boost vaccination with rLVS ΔcapB/Ba - rLm ΔactA ΔinlB prfA/Ba induces elevated frequencies of LF- and PA-specific polyfunctional lung and spleen CD4+ T-cells producing IFN-γ, IL-2, TNF-α, and IL-17. As described in Fig. 4a and indicated by the colors and letters at the bottom of the figure, mice (n = 4/group) were sham-immunized or immunized with various vaccines. Lung (left panels) and spleen (right panels) cells were stimulated with LF (a,b), PA (c,d), HI-LVS (e,f), or PMA (g,h) and assayed by intracellular cytokine staining for 15 possible combinations of CD4+ T-cells expressing IFN-γ, TNF-α, IL-2, and/or IL-17A. Values are means + SEM and differences among individual groups were analyzed by Two-way ANOVA with Tukey’s multiple comparisons test (Prism). Values significantly different from the Sham group are marked with asterisks over the comparison groups. In panels e, f and g, the Sham group is indicated by a short bar with an open end and the comparison groups are indicated by a short vertical line across the short bar. *P < 0.05; **P < 0.01; ***P < 0.001; ****P < 0.0001. Results shown are representative of three similar experiments.
Vaccine immunogenicity and protective immunity against pneumonic plague
To evaluate the protective efficacy of rLVS ΔcapB- and rLm-vectored Y. pestis vaccines administered by the mucosal and systemic routes, we sham-immunized mice, or immunized them once with the unlicensed EV76 vaccine s.q. (its standard route of administration), or twice homologously with rLVS ΔcapB/Yp i.n. or i.d. or heterologously primed-boosted with rLVS ΔcapB/Yp (i.n. or i.d.) - rLm/Yp (i.n. or i.m., respectively), as indicated in Fig. 6a. All mice were bled at Week 8; challenged at Week 9 with 1900 CFU Y. pestis CO92 strain (~8 LD50; the pre-determined LD50 for Y. pestis CO92 was ~250 CFU), and monitored for signs of illness, weight change, and survival for three weeks. Mice immunized with rLVS ΔcapB/Yp i.d or with rLm/Yp i.m. did not show signs of significant discomfort (e.g. ruffled fur) or weight loss (data not shown); in one experiment, mice immunized with rLVS ΔcapB/Yp i.n. showed transient mild weight loss (~5%) but rapidly recovered such that their weights matched that of sham-immunized controls by at least Day 6 post–vaccination (data not shown). Homologous priming-boosting with rLVS ΔcapB/Yp i.n. or i.d. (Groups C, D) or heterologous priming-boosting with rLVS ΔcapB/Yp – rLm/Yp i.n. or i.m. (Groups E, F) induced significantly elevated serum antibody titers to LcrV protein and to F1/LcrV fusion protein, balanced between IgG1 and IgG2a, compared with sham-immunization (Fig. 6b) (Fig. S10a,b, upper panel, Groups B, E, & F). The majority of the IgG antibody induced by LVS ΔcapB- and Lm-vectored vaccines was directed to LcrV. In contrast, mice immunized with EV76 produced very little antibody to LcrV (small amounts of IgG1 and IgG2a were evident) but substantial amounts of IgG to F1 and F1-LcrV (Fig. 6b).
Two immunizations by homologous priming-boosting with rLVS ΔcapB/Yp or heterologous priming-boosting with rLVS ΔcapB - rLm ΔactA ΔinlB prfA/Yp induces humoral immune responses and protective immunity against respiratory challenge with virulent Y. pestis. (a) Experiment schedule. Mice (n = 8/group) were immunized homologously twice with PBS (Sham) or 106 CFU LVS ΔcapB/Yp (rLVS/Yp) or once with 106 CFU EV76, or heterologously first with 106 CFU rLVS ΔcapB/Yp and then with 106 CFU rLm ΔactA ΔinlB prfA/Yp (rLm/Yp). All mice were bled at Week 8; challenged at week 9 with virulent Y. pestis (CO92) (1,900 CFU/mouse, ~8 LD50); and monitored for survival for three weeks, as indicated. (b) Serum antibody after vaccination. Sera were assayed for IgG antibody specific to F1, LcrV, or the monomer of F1-LcrV proteins (leftmost panel) and subtypes IgG1 and IgG2a antibodies specific to LcrV or F1-LcrV (middle and rightmost panels, resp.). Data are mean + SEM of serum antibody endpoint titer for n = 8 per group. Differences among individual groups were analyzed by two-way ANOVA with Tukey’s correction. ****P < 0.0001 vs. Sham. (c) Survival after challenge. The survival curve of each vaccinated group is compared with the Sham group (Group A) by the log-rank test (Mantel-cox); P values that are significantly different from the Sham group are marked with one or more asterisks color-coded to the color of the vaccine symbol. There were no changes in percent survival of mice in any group after day 14 post challenge until the end of the experiment. *P < 0.05; **P < 0.01; ***P < 0.001; ****P < 0.0001. (d) Correlation between serum antibody and mean survival time. The correlation coefficient (R2) and one-tailed P values were obtained as described in legend to Fig. 2D.
Systemic homologous priming-boosting with rLVS ΔcapB/Yp i.d. (Group D) or heterologous priming-boosting with rLVS ΔcapB/Yp – rLm/Yp (i.d./i.m.) (Group F) showed significant protection against challenge with Y. pestis CO92 compared with sham-immunized mice (P = 0.02 and P = 0.01, respectively), albeit less than EV76 (Fig. 6c). Mean survival time three weeks post-challenge was correlated with pre-challenge serum IgG antibody to F1 but not to LcrV (Fig. 6d).
Subsequently, we explored the efficacy of three homologous immunizations, both mucosally (i.n. for rLVS ΔcapB/Yp) and systemically (i.d. for rLVS ΔcapB/Yp and i.m. for rLm/Yp) and three heterologous immunizations systemically, as described in Fig. 7a. Controls were sham-immunized with PBS, administered the EV76 vaccine once s.q, or primed-boosted with rLVS ΔcapB/Yp – rLm/Yp once systemically. Mice were bled; subsequently challenged with 1800 CFU virulent Y. pestis CO92 (~7 LD50); and monitored for survival for three weeks. Among the vaccines and administration regimens tested, three homologous priming-boosting immunizations with rLVS ΔcapB/Yp i.d. (Group D) induced significantly greater serum antibody titers to F1 antigen than sham-immunized mice, balanced between subtypes IgG1 and IgG2a (Fig. 7b, left panel), similar to mice vaccinated with EV76. Homologous priming-boosting with rLVS ΔcapB/Yp (i.n. or i.d) (Groups C, D) but not with rLm/Yp (i.m.) (Group E), and heterologous priming-boosting systemically (with one or two boosts) (Groups F, G) induced significantly elevated LcrV-specific IgG antibody compared with sham-immunized mice, balanced between subtypes IgG1 and IgG2a (Fig. 7b, right panel). Mice immunized with EV76 produced abundant IgG antibody to F1 antigen, but relatively little to LcrV (Fig. 7b). Mice homologously prime-boosted with rLVS ΔcapB/Yp i.n. or heterologously prime-boosted with rLVS ΔcapB/Yp – rLm/Yp (i.n./i.n. or i.n./i.m.) also developed T-cell mediated immunity, as evidenced by IFN-γ secretion by lung and spleen cells in response to F1 and/or LcrV (Fig. S10b, lower panels).
Three systemic immunizations by homologous priming-boosting with LVS ΔcapB/Yp induce high level antibody responses and potent protective immunity against respiratory challenge with virulent Y. pestis CO92 strain. (a) Experiment schedule. Mice (n = 8/group) were immunized homologously three times with 106 CFU rLVS ΔcapB/Yp (rLVS/Yp) or with 106 CFU rLm ΔactA ΔinlB prfA/Yp (rLm/Yp) or heterologously with rLVS ΔcapB/Yp and subsequently rLm/Yp. Mice vaccinated with PBS i.d. (Sham, Group A) or 106 CFU Y. pestis vaccine strain EV76 served as controls. All the mice were bled at Week 11; challenged with Y. pestis CO92 (1,800 CFU/mouse, ~7 LD50) at Week 12; and monitored for survival for 3 weeks post-challenge, as indicated. (b) Serum antibody after vaccination. Sera were assayed for antibody endpoint titer of IgG or IgG subtypes IgG1 and IgG2a to Y. pestis F1 (left panel) and LcrV (right panel) proteins. Data are mean + SEM of serum antibody endpoint titer for n = 8 per group. Differences among individual groups were analyzed by two-way ANOVA with Tukey’s correction. ***P < 0.001; ****P < 0.0001 vs. Sham. (c) Survival after vaccination and challenge. The survival curve of each vaccinated group is compared with that of the Sham group by the log-rank test (Mantel-cox); P values for vaccine groups significantly different from the Sham group are marked with one or more asterisks color-coded to the color of the vaccine symbol. *P < 0.05; ***P < 0.001. (d) Correlation between serum antibody and mean survival time. The correlation coefficient (R2) and one-tailed P values were obtained as described in legend to Fig. 2D.
Mice immunized three times i.d. with rLVS ΔcapB/Yp (Group D) survived significantly longer than sham-immunized mice (P = 0.03); mice primed-boosted with rLVS ΔcapB/Yp - rLm/Yp (Group F) also survived longer than sham-immunized mice, although the difference was not statistically significant (Fig. 7c). As in the previous experiment shown in Fig. 6, the amount of serum antibody specific to F1, but not to LcrV, was highly correlated with the mean survival time three weeks post-challenge (P < 0.001, P < 0.0001 and P < 0.0001 for IgG, IgG1 and IgG2a, respectively) (Fig. 7d). These results indicate that systemic homologous priming-boosting with rLVS ΔcapB/Yp induces strong protective immunity against Y. pestis CO92 respiratory challenge and that vaccine efficacy is correlated with F1-specific antibody.
Potent protective immunity against pneumonic tularemia
In previous studies, we have shown that heterologous priming-boosting with LVS ΔcapB or rLVS ΔcapB overexpressing IglC as the prime vaccine and rLm expressing F. tularensis IglC (rLm/iglC) as the booster vaccine induces potent protective immunity in mice against virulent F. tularensis Schu S4 respiratory challenge18. We have also shown that immunization with rLVS ΔcapB/iglABC is highly safe and induces greater protective immunity than the parental LVS ΔcapB vector against F. tularensis Schu S4 respiratory challenge19. However, the efficacy of homologous priming-boosting with this vaccine has not been investigated. To evaluate the efficacy of homologous priming-boosting with rLVS ΔcapB/iglABC, both systemically and mucosally, we immunized BALB/c mice once or twice i.d. or i.n. with this vaccine, as indicated in Fig. 8a. Control mice were sham-immunized with PBS, immunized i.d. with the unlicensed LVS vaccine (which is highly lethal by the i.n. route), or i.d. with the LVS ΔcapB vector. Mice were challenged with 10 CFU F. tularensis Schu S4 (~10 LD50) at Week 10 and monitored for survival for 3 weeks. All immunized mice survived significantly longer than the sham-immunized mice (P = 0.03 for LVS ΔcapB and P = 0.001 or 0.0001 for all other groups vs. sham-immunized mice). Mice immunized i.d. once (Group D) or twice (Group E) or i.n. twice (Group F) with rLVS ΔcapB/iglABC survived significantly longer than mice immunized once with the LVS ΔcapB vector (P = 0.006, P = 0.0001, and P = 0.0005, respectively); mice immunized i.d. or i.n. twice with rLVS ΔcapB/iglABC (Groups E and F) had survival times equivalent to or greater than that of mice immunized with LVS (Group B); differences were not statistically significant (Fig. 8b).
Two immunizations by homologous priming-boosting with rLVS ΔcapB/iglABC induces strong protection against respiratory challenge with the virulent F. tularensis Schu S4 strain. (a) Schedule - Experiment VI. Mice (n = 8/group) were immunized once with PBS (Sham), 104 CFU LVS, 106 CFU LVS ΔcapB vector, or 106 CFU rLVS ΔcapB/iglABC; or twice with 106 CFU rLVS ΔcapB/iglABC; challenged i.n. with F. tularensis Schu S4 (10 CFU, ~10 LD50) at Week 10; and monitored for signs of illness, weight change, and death for 3 weeks, as indicated. (b) Survival after vaccination and challenge – Experiment VI. The survival curve of each vaccinated group is compared with that of the Sham (Group A) or LVS ΔcapB vector (Group C) group by the log-rank test (Mantel-cox); P values for vaccine groups that are significantly different from the Sham or LVS ΔcapB vector control group are marked with asterisk(s) and multiple “§”, respectively, color-coded to the color of the vaccine symbol. *P < 0.05; ***P < 0.001; and ****P < 0.0001 vs. Group A (Sham); §§P < 0.01; §§§P < 0.001 vs. Group C (vector control). (c) Schedule - Experiment VII. Mice (n = 8/group) were immunized once with PBS (Sham), 104 CFU LVS, or 106 CFU rLVS ΔcapB/iglABC three times at Weeks 0, 4, and 8, or twice at Weeks 4 and 8, bled at Week 13, and challenged i.n. with 2 CFU (2 LD50) or 6 CFU (6 LD50) F. tularensis Schu S4 at Week 14, and monitored for 3 weeks, as indicated. (d) Survival after vaccination and challenge and serum antibody pre-challenge – Experiment VII. Upper panels – Survival. The survival curve after challenge with 2 LD50 (left panel) or 6 LD60 (right panel) of each vaccinated group is compared with that of either the sham- or LVS-immunized group by the log-rank test (Mantel-cox); P values that are significantly different from the control group are marked with asterisk(s) color-coded to the color of the vaccine symbol. ***P < 0.001 vs. Group A (Sham); *P < 0.05 vs. Group B (LVS). Lower panel- Serum antibody after vaccination. Sera were assayed for IgG and subtypes IgG1 and IgG2a specific to heat-inactivated LVS. Data are mean + SEM of serum antibody endpoint titer for n = 8 per group. Differences among individual groups were compared by two-way ANOVA with Tukey’s correction. Values that are significantly different between two groups are marked with asterisk(s) over an open horizontal line crossing above the two groups. As indicated by the asterisks above the Sham group, its titers were significantly different from all other groups. *P < 0.05; **P < 0.01; and ****P < 0.0001.
In a subsequent experiment comparing two vs. three doses of rLVS ΔcapB/iglABC, we immunized mice i.d. or i.n. twice or three times with rLVS ΔcapB/iglABC; control mice were immunized i.d. once with PBS (Sham) or LVS. All the mice were bled, challenged i.n. with 2 or 6 CFU (LD50 ≈ 1 CFU) of F. tularensis Schu S4, and monitored for survival for 3 weeks (Fig. 8c). Consistent with the experiment described above, all the immunized mice survived significantly longer than the sham-immunized mice (P < 0.001) (Fig. 8d, upper panels). Notably, 100% of mice immunized with rLVS ΔcapB/iglABC i.n. either twice or three times survived challenge with 2 or 6 LD50, the highest survival rate among the groups; and the survival of rLVS ΔcapB/iglABC immunized mice was significantly greater (P < 0.05) than that of LVS-immunized mice after the 6 LD50 challenge (Fig. 8d upper panels). Interestingly, when the rLVS ΔcapB/iglABC vaccine was administered by the i.d. route, three immunizations were not more efficacious than two immunizations; differences in survival between these mice and LVS-immunized mice were not statistically significant. All the immunized mice had F. tularensis antigen-specific IgG antibody, balanced between IgG1 and IgG2a, at levels significantly greater than sham-immunized mice (P < 0.0001) (Fig. 8d, lower panels). Mice immunized i.d. three times with rLVS ΔcapB/iglABC (group D) had antibody (IgG and IgG1) level significantly greater than LVS-immunized mice (P < 0.05 and P < 0.0001, resp.). Mice immunized with rLVS ΔcapB/iglABC i.n. twice (group E) or three times (group F) had antibody (IgG, IgG1, and IgG2a) levels significantly higher than mice immunized i.d. once with LVS (P < 0.0001) or i.d. twice or three times with rLVS ΔcapB/iglABC (P < 0.05 – P < 0.0001) (Fig. 8d, lower panel). While not examined herein, a previous study demonstrated that rLVS ΔcapB/iglABC also induces strong cell-mediated immune responses, which play a dominant role in host defense against F. tularensis19. These results show that systemic and especially mucosal homologous priming-boosting with rLVS ΔcapB/iglABC induces strong protective immunity against virulent F. tularensis Schu S4 respiratory challenge.
Discussion
In this study, we report single platform vaccines including homologous LVS ΔcapB-vectored vaccines and heterologous LVS ΔcapB and Lm-vectored vaccines against three Tier I pathogens, the causative agents for anthrax, plague and tularemia. We show that LVS ΔcapB- and Lm-vectored vaccines express recombinant B. anthracis, Y. pestis, and F. tularensis immunoprotective proteins on solid agar or in broth, and in macrophage-like cells in vitro; the shuttle plasmids for antigen expression in LVS ΔcapB vectored vaccines are stable after passage in broth, macrophages, and mice. All vaccines are safe in mice after systemic (i.d. or i.m.) or mucosal (i.n.) immunization. Homologous priming-boosting with LVS ΔcapB-vectored B. anthracis, Y. pestis, or F. tularensis vaccines administered mucosally or systemically induces potent antigen-specific humoral and T cell-mediated (including both CD4+ and CD8+) immune responses, known to be important for long-lasting potent immunoprotection against the target pathogens of anthrax34,35,36, plague20,37,38, and tularemia39,40,41,42,43 in animal models, and potent protective immunity against respiratory challenge with lethal doses of these pathogens. Protection against anthrax was far superior to that obtained with the licensed AVA vaccine and protection against tularemia was comparable to or greater than that obtained with the toxic and unlicensed LVS vaccine. Heterologous priming-boosting with LVS ΔcapB- and Lm-vectored B. anthracis and Y. pestis vaccines also induced potent protective immunity against respiratory challenge with virulent B. anthracis spores and Y. pestis.
Studies on the immunity induced by anthrax vaccines, mostly comprising PA and LF antigens or their immunodominant domains, have focused on serum antibody (mostly Th2 biased) and toxin neutralization antibody; the role of T cell mediated immunity has not been widely investigated12,44. Thus, the cumbersome immunization regimen for the licensed AVA vaccine (consisting primarily of PA with some LF protein) entails repeated boosting to induce sufficient toxin neutralizing activity for protection. With respect to a potential role for cell-mediated immunity, Glomski et al. reported that IFN-γ-producing CD4+ lymphocytes, but not humoral immune responses, mediate spore-induced immunity to capsulated B. anthracis36. Also, in this regard, Altman has reported that patients recovered from cutaneous anthrax, who anecdotally exhibit long-term protection from subsequent infection, show high frequencies of CD4+ T cells in response to PA and LF34. In our study, the AVA vaccine, which gave very poor protection against respiratory challenge with B. anthracis, induced strong antibody responses and toxin neutralization activity but essentially no T-cell responses to PA, and neither humoral nor T-cell responses to LF. In contrast, homologous prime-boost vaccination with rLVS ΔcapB/Ba and heterologous prime-boost vaccination with rLVS ΔcapB/Ba – rLm/Ba expressing an LFnPAc fusion protein, which gave strong protection against B. anthracis respiratory challenge, not only induced PA- and LF-specific serum IgG, dominated by Th1-type IgG2a, and toxin neutralizing antibody, but also induced strong T-cell responses, including IFNγ-, TNFα-, and/or IL2-expressing multifunctional CD4+ T cells, suggesting a role for T-cell mediated immunity in addition to humoral immunity in protection against anthrax. In our study, the antibody titer to LF, but not to PA, correlated with protection. The lack of correlation between protection and anti-PA antibody in our study is consistent with results of some studies45,46 but contrasts with the results of others47,48,49.
Currently there is no licensed vaccine against Y. pestis. Vaccines studied preclinically include live attenuated Y. pestis vaccines, such as EV76; subunit vaccines based primarily on F1 and LcrV antigens; and live attenuated heterologous bacterial (Salmonella and Yersinia pseudotuberculosis) or viral (adenovirus, modified vaccinia Ankara, or bacteriophage) vectors expressing F1 and/or LcrV50,51,52,53,54,55. These vaccines have their advantages and disadvantages. Generally speaking, live attenuated Y. pestis vaccines, while effective, induce serious local and systemic reactions55; subunit vaccines are effective but do not induce high levels of cell-mediated immunity, likely important for long-lasting protection56; heterologous bacterial vectors are safe but have not been as effective as subunit vaccines57; and viral vectored vaccines are effective but may be limited by preexisting immunity. Immunology studies have shown that antibodies to F1 and LcrV provide short-term protective immunity against challenge with Y. pestis; however, F1-LcrV-specific T cell responses with a preferential Th1 polarization are also critical for protection against Y. pestis55,57. Our study shows that homologous prime-boost vaccination (two or three doses) with rLVS ΔcapB/Yp or heterologous prime-boost vaccination with rLVS ΔcapB/Yp-rLm/Yp induces significantly elevated serum antibody to F1-LcrV, balanced between IgG1 and IgG2a, elevated IFN-γ secretion by spleen and lung cells, and partial protection against pneumonic challenge with virulent Y. pestis; protection correlates with serum antibody to F1. Protection was not as great as that induced by immunization with the toxic and unlicensed EV76 vaccine, which induced much higher levels of antibody to F1 antigen; the suboptimal protective immunity induced by rLVS ΔcapB/Yp and/or rLm/Yp vaccines may have been due to the relatively poor immunogenicity of their F1-LcrV fusion protein construct. It has been shown that the mutated form of F1, F1mut, folds into a monomer, rather than polymerizing as a linear fiber, enhancing its immunogenicity11,54. Potentially, the efficacy of our vaccines can be substantially enhanced by similarly expressing F1mut as well as by expanding the antigen repertoire by the addition of other immunoprotective antigens.
As with plague, there are no licensed vaccines against tularemia. The most promising vaccine candidates being studied preclinically, like the unlicensed LVS vaccine, are live attenuated Francisella vaccines, including our LVS ΔcapB vectored vaccine, derived ultimately from F. tularensis subsp. holarctica17; vaccines derived from the nonhuman pathogen F. novicida58; and vaccines derived from the highly virulent human pathogen F. tularensis subsp. tularensis Schu S4 strain59,60,61. Single deletional mutants of F. tularensis Schu S4 are effective, comparable to LVS and the rLVS ΔcapB vaccines, but safety considerations dictate the need for at least one additional major attenuating deletion; thus far, such additional deletions have resulted in impotent vaccines62. In contrast, our rLVS ΔcapB/iglABC vaccine is highly potent; has three major attenuating deletions; is >10,000-fold less virulent than LVS in the mouse model; is unmarked, i.e. devoid of antibiotic resistance genes; and has an excellent safety profile17.
Our previous studies have shown that systemic (i.d.) vaccination with a single dose of rLVS ΔcapB/iglABC induces potent CD4+ and CD8+ T cell immune responses, Th1-dominated serum antibody, and partial protection against respiratory challenge with F. tularensis Schu S419. Our study here shows that systemic i.d. vaccination with just two doses rLVS ΔcapB/iglABC induces substantial protection to pneumonic challenge with F. tularensis Schu S4 strain, equivalent to the LVS vaccine; mucosal (i.n.) vaccination with either two or three doses of rLVS ΔcapB/iglABC provides 100% protection.
To our knowledge, our platform is the first to demonstrate efficacy against three Tier 1 Select Agents. Vaccines have previously been described against two pathogens, including a vaccinia-based vaccine against smallpox and anthrax32 and subunit vaccines against anthrax and plague11,63. Among the strategies tested in our proof of principle studies – (a) LVS ΔcapB- vs. Lm-vectored vaccines; (b) homologous vs. heterologous prime-boost vaccination; (c) mucosal vs. systemic (i.d. for rLVS ΔcapB and i.m. for rLm) vaccine administration; (d) one vs. two vs. three immunization doses – we found that three homologous i.d. vaccinations with the LVS ΔcapB-vectored B. anthracis, Y. pestis, and F. tularensis vaccines is a strategy that works well for all three target pathogens. This strategy has the major advantage of being a single vector platform, induces strong antigen-specific T-cell and humoral immune responses, and provides potent efficacy against all three pathogens. In the case of F. tularensis, mucosal i.n. delivery of the rLVS ΔcapB/iglABC vaccine was somewhat superior to i.d. delivery of this vaccine; however, the i.n. route raises safety issues and administering this one vaccine by that route and the anthrax and plague vaccines by the i.d. route would preclude concurrent immunization of all three vaccines together. In the case of B. anthracis, the heterologous prime-boost vaccination strategy was also highly effective; however, this approach would require development of two vaccines based upon different vectors and likely require administration by two different routes, a significant disadvantage in terms of cost and complexity of development, manufacture, and regulatory approval, and ease of clinical administration.
With respect to safety in humans, both the LVS and the Lm ΔactA ΔinlB parental vectors have established safety profiles in humans. LVS, which retains significant virulence in animals and shows residual toxicity in humans, is the only tularemia vaccine demonstrated efficacious in humans. In comparison with its wild-type F. tularensis subsp. holarctica parent, LVS has two major attenuating deletions, FTT0918 (virulence determinate of SCHU S4) and pilA64,65, and as noted above, our LVS ΔcapB vector has a third major attenuating deletion, capB, rendering it >10,000 fold less virulent for mice than LVS by the i.n. route. The Lm ΔactA ΔinlB vector has been shown to be safe in humans23, and the additionally modified Lm ΔactA ΔinlB prfA(G155S) vector retains the attenuation of the parental Lm ΔactA ΔinlB vector in mice25 while providing significantly enhanced antigen-specific T-cell mediated immune responses24,25. Our study shows that the LVS ΔcapB- and Lm ΔactA ΔinlB prfA(G155S)-vectored F. tularensis, B. anthacis, and Y. pestis vaccines are safe and efficacious in BALB/c mice. Further validation of genetic stability and safety of the vaccines will be required prior to human studies.
In summary, our live attenuated single vector vaccine platform elicits robust humoral and T-cell mediated immune responses and protective immunity against three target pathogens – the agents of anthrax, plague, and tularemia – and overcomes the problems of poor immunogenicity and lack of immunological memory often associated with subunit vaccines against these pathogens. As already noted, a single vector platform vaccine has numerous advantages in terms of production cost, regulatory approval, ease of administration, and patient acceptability. This vaccine platform can be extended readily to cover other pathogens including other Tier 1 Select Agents such as Burkholderia pseudomallei and Burkholderia mallei.
Materials and Methods
Cell line, bacteria, and vaccines
Mouse macrophage-like J774A.1 cells (ATCC TIB-67) and human macrophage-like THP-1 cells (ATCC TIB-202) were negative for mycoplasma contamination and cultured as described previously15,24. F. tularensis Live Vaccine Strain (LVS) was obtained from the Centers for Disease Control and Prevention (Atlanta, Ga.). B. anthracis AVA (Anthrax vaccine adsorbed) vaccine was obtained from BEI Resources. Y. pestis attenuated EV76 strain was obtained from Centers for Disease Control and Prevention, Fort Collins, CO. Virulent strains of B. anthracis (Ames spores), Y. pestis (CO92), and F. tularensis (Schu S4) were originally obtained from BEI Resources, stored at −80 °C, and used in animal challenge experiments at Colorado State University (CSU) only. The LVS, LVS ΔcapB vector, recombinant LVS ΔcapB vaccine, Lm vector, and recombinant Lm (rLm) vaccine stocks were prepared, stored and used as described previously by us15,17,18.
Mice
Six to eight week old female BALB/c mice were purchased from Charles River Laboratory (Wilmington, MA) or Taconic (Hudson, NY) and randomly assigned to experimental groups. Animals for immunology studies and for efficacy studies prior to challenge were maintained in a specific-pathogen-free animal facility and used according to protocols approved by the UCLA and CSU Institutional Animal Care and Use Committees. After challenge with virulent B. anthracis, Y. pestis, or F. tularensis, animals were maintained in a BSL3 facility at CSU and used according to protocols approved by the CSU IACUC.
Proteins, antibodies, and vaccine controls
We obtained the following reagents through the NIH NIAID Biodefense and Emerging Infections Research Resources Repository: genomic DNA from B. anthracis, strain Sterne BA695 (Δlef243), NR-9540; genomic DNA from Y. pestis strain CO92, DD-494; monoclonal antibody to PA, AB-BA-PA-MAB1; goat polyclonal antibody to LcrV, NR-31022; goat polyclonal antibody to F1-Antigen, NR-31024; PA protein, NR-3780; Lethal Factor (LF-HMA) protein, NR-4368; LcrV protein, NR-32875; F1 protein, NR-44223; F1-LcrV monomer protein, NR-2562; Anthrax Vaccine Adsorbed (AVA) (BioThrax™), NR-2642; and AVA pooled human plasma, NR-28672. Rabbit polyclonal antibody to F. tularensis Bacterioferritin (Bfr) was produced in our laboratory31.
Construction and verification of rLVS ΔcapB vaccines expressing B. anthracis, Y. pestis, or F. tularensis fusion proteins encoded by genes amplified from B. anthracis, Y. pestis, and F. tularensis genomic DNAs, respectively
Using LVS ΔcapB and pFNL-derived shuttle vectors66, we constructed recombinant LVS ΔcapB (rLVS ΔcapB) vaccine candidates, rLVS ΔcapB/bfr-iglABC (rLVS ΔcapB/iglABC)19, rLVS ΔcapB/Ba, and rLVS ΔcapB/Yp, using a strategy similar to one published previously19. Specifically, we constructed the shuttle plasmid for expressing B. anthracis fusion protein LFnPAc, pFNL/bfr-BaLFnPAc(GGSG), by replacing the gro-gfp expression cassette in pFNLTB6 gro-gfp (KanR)66 with the bfr-BaLFnPAc(GGSG) expression cassette comprising the F. tularensis bacterioferritin promoter (upstream of FTT_1441, bfr, amplified from the genomic DNA of an clinical isolate of SCHU S4 strain), a Shine-Dalgarno sequence, a 6-nucleotide spacer, followed by the coding sequence for B. anthracis LFn26,27 and PAc12 separated by a GGSG linker (LFnPAc). The coding sequence for LFnPAc was amplified by two-step overlap PCRs. First, we amplified the coding sequences for LFn and PAc by using the genomic DNA of B. anthracis (BEI NR-9540) and primer pairs LF_Fw1 (TAACAATAGGAGGTACGTAATGGCGGGCGGTCATGGTGATG) and LFn_Rv (TGTTTGTTGATCGAAATTACCAGAACCACCTAGATTTATTTCTTGTT) for LFn, and primer pairs PAc_Fw (AACAAGAAATAAATCTAGGTGGTTCTGGTAATTTCGATCAACAAACA) and PA_Rv1 (TGAAACGAG CTAGTGGATCCTTATCCTATCTCATAGCCTTTTT) for PAc, respectively. Secondly, we used the PCR products of LFn and PAc and primer pairs LF_Fw1 and PA_Rv1 to amplify the coding sequence for fusion protein LFnPAc, which was subsequently cloned into the pFNL-derived shuttle vector. We verified the inserted sequence by restriction analysis and nucleotide sequencing, electroporated the resultant shuttle plasmid into LVS ΔcapB, and selected clones that were kanamycin-resistant and stably expressed the targeted antigens shown by Western blotting. Similarly, we constructed rLVS ΔcapB/Yp carrying the shuttle plasmid pFNL/omp-YpF1V(GGSG) for expressing the Y. pestis fusion protein of F1 (170 aa) and LcrV (326 aa) separated by the GGSG linker (F1V) driven by the F. novicida outer membrane promoter (upstream of FTN_1451, omp, amplified from F. novicida genomic DNA). The coding sequence for F1 and LcrV were amplified from the genomic DNAs of Y. pestis (BEI DD-494) by using primer pair F1_Fw1 (GACTAAAAGGAGGTACGTAATGAAAAAAATCAGTTCCGTTAT) and F1_Rv (TGTTCGTAGGCTCTAATCATACCAGAACCACCTTGGTTAGATACGGTTAC) for F1 and primer pair LcrV_Fw (GTAACCGTATCTAACCAAGGTGGTTCTGGTATGATTAGAGCCTACGAACA) and LcrV_Rv1 (CGAGCTAGTGGATCCTCATTTACCAGACGTGTCATCTA) for LcrV, respectively.
Construction and verification of attenuated recombinant Listeria monocytogenes vaccines expressing B. anthracis, Y. pestis, and F. tularensis fusion proteins
Using Lm ΔactA ΔinlB ΔuvrAB prfA(G155S) (Lm ΔactA ΔinlB prfA, generously provided by J. Skoble of Aduro Biotech, previously Anza Therapeutics)25,33,67 as a vector, we constructed recombinant Listeria-vectored vaccine candidates expressing immunogenic fusion proteins of B. anthracis, Y. pestis, or F. tularensis, using methodology described previously by us and others15,22,24,68. Briefly, we amplified the encoding sequence for the fusion protein of B. anthracis LFnPAc and Y. pestis F1V from the above described F. tularensis shuttle plasmids by PCR with primer pairs LF_Fw2 (AGGTGGATCCATGGCGGGCGGTCATGGTG) and PA_Rv2 (CGGTGGCGGCCGCTTATCCTATCTCATAGCCTTTTTTA) for LFnPAc and F1_Fw2 (CGAGGGATCCATGAAAAAAATCAGTTCCGTTAT) and LcrV_Rv2 (ATATGCGGCCGCTCATTTACCAGACGTGTCATCTA) for F1V, respectively, ligated them with either the Lm hly promoter and the coding sequence for the listeriolysin O (encoded by hly) signal sequence (LLOss) or the Lm actA promoter and the coding sequence for the ActA N-terminal 100 amino acids (ActAN), and cloned into a phage-based Listeria site-specific integration vector derived from pPL2 (kindly provided by J. Skoble)68. We subsequently integrated the resultant plasmid into the 3′ end of tRNAarg on the bacterial chromosome of the recipient Lm ΔactA ΔinlB prfA strain from the donor SM10 strain carrying the integration plasmid through conjugation to obtain rLm vaccines. We confirmed all the molecular plasmid constructs by nucleotide sequencing and verified the final recombinant L. monocytogenes strains by colony PCR for chromosomal integration and by Western blotting for heterologous protein expression.
Heterologous protein expression by and growth kinetics of LVS ΔcapB- and Listeria-vectored vaccines in broth culture and in infected macrophage-like cells
To assess protein expression by rLVS ΔcapB vaccines grown on agar, we grew each of the vaccine stocks on Chocolate agar, selected single colonies, lysed them in SDS buffer, applied the lysates to SDS-PAGE, and analyzed protein expression by Western blotting. Secreted proteins in the supernate of Brain Heart Infusion (BHI) broth culture of rLm vaccines were precipitated by the TCA-acetone method and analyzed by Western blotting. Monoclonal antibodies specific to B. anthracis PA (BEI, DD-9) and goat polyclonal antisera specific to Y. pestis LcrV (BEI, NR-31022) were used as primary antibody in Western blotting. To assay protein expression of LVS ΔcapB-vectored vaccines in macrophage-like cells, we seeded monocytic THP-1 cells at 3 × 105 cells/well on 24-well plates and differentiated them in the presence of PMA for 3 days. Vaccine vector (LVS ΔcapB) and rLVS ΔcapB vaccines were grown on Chocolate agar supplemented without (vector) or with (vaccines) kanamycin (7.5 μg/ml) for 3 days. The differentiated THP-1 cells were left uninfected or infected with rLVS ΔcapB/Ba or rLVS ΔcapB/Yp opsonized with human serum at a multiplicity of infection (MOI) of 10:1 (bacteria: cell) and incubated at 37 °C for 1 h. The cells were then washed with RPMI three times and incubated with complete RPMI supplemented with gentamycin (0.1 μg/ml) to inhibit extracellular bacterial growth. At 24 h post infection, medium was removed from wells; cells were lysed, and cell lysates analyzed by Western blotting using a mixture of monoclonal antibody to B. anthracis PA antigen and goat polyclonal antibody to Y. pestis LcrV antigen. Protein expression of Lm-vectored vaccines in macrophage-like cells was assayed as described previously15,24. Growth kinetics of LVS ΔcapB- and Lm-vectored vaccines in broth and in infected macrophages were assayed as described in the Supplemental Information (legends to Figs S2 and S3, resp.) and as published by us previously15,19,24.
Immune response analysis
Groups of 4–8 BALB/c mice were immunized as indicated in Figs 2a, 3a, 4a, 6a and 8a,c, Figs S7a and S10a. In experiments studying immunology and efficacy of B. anthracis, Y. pestis and F. tularensis vaccines, mice were bled one week prior to challenge. In experiments studying immunology only, mice were bled at one week post rLm boosting and subsequently euthanized; spleens and lungs removed; single cell suspensions of spleen and lung cells prepared and suspended in T cell medium; and cells enumerated as described previously19. Serum was isolated and stored at −80 °C until use. Serum antibody, in vitro stimulation and production of IFN-γ and IL-4 by murine immune lung and spleen cells, and intracellular cytokine staining of lung and spleen cells for flow cytometry analysis were assayed as published by us previously15,19,24.
Serum antibody
Sera were tested for IgG antibody response by enzyme-linked immunosorbent assay (ELISA) using standard procedures15. Briefly, ninety-six-well microtiter plates were coated with recombinant protein PA (BEI, NR-3780), LF (NR-4268), F1 (NR-44223), LcrV (NR-32875), or F1-LcrV monomer (NR-2563) at 1 µg/ml each, or heat-inactivated LVS (HI-LVS, 2 × 107/ml) diluted in carbonate buffer overnight at 4 °C and afterwards processed at ambient temperature. The plates were washed three times with 0.05%Tween20-PBS, blocked in 3% BSA-PBS for 3 h, incubated with each serum sample serially diluted 2-fold twelve times at a starting dilution of 1:20 or 1:50 in 1% BSA-PBS for 90 min, and washed again. Bound antibody was detected by using alkaline phosphatase-conjugated goat anti-mouse IgG (Sigma, St. Louis, MO), subtypes IgG1 (Sigma), IgG2a (Abcam), IgG2b (sigma), or IgG3 (Sigma) diluted in 1% BSA-PBS and incubating for 90 min. Plates were developed with 100 µl of p-nitrophenylphosphate substrate (BioRad), and the A415 was read using a multiscan microplate reader (iMark, BioRad). The results are presented as the mean antibody endpoint titer and SE of the mean (SEM). Antibody endpoint titer is defined as the mean log dilution that yields an OD greater than the mean OD of Sham sera plus three standard deviations at the same serum dilution.
In vitro stimulation and production of IFN-γ and IL-4 by murine immune splenocytes
A single cell suspension of 1.0 × 105 splenocytes or lung cells per well was seeded in U-bottom 96-well plates and incubated with T-cell medium alone, or T-cell medium supplemented with 2 µg/mL of recombinant PA, LF, F1, LcrV, or F1-LcrV monomer for three days. After a 3-day incubation, the culture supernatant fluid was collected, cell debris removed by centrifugation, and the supernatant fluid stored in assay diluent (BD Biosciences) at −80 °C until use. The production of mouse IFN-γ and IL-4 in the culture supernatant fluid was assayed using a mouse cytokine EIA kit (BD Biosciences)24.
In vitro stimulation and intracellular cytokine staining for flow cytometry analysis
A single cell suspension of 7.5 × 105 lung cells or 1.5 × 106 splenocytes per well was seeded in U-bottom 96-well plates and stimulated with 2 µg/mL of recombinant PA or LF, or 2 × 107/ml of HI-LVS in the presence of anti-CD28 monoclonal antibody (Clone 37.51) for a total of 6 h, and processed for Flow Cytometry analysis as described previously by us19,24. The frequencies of live CD4+ and CD8+ T cells producing any of the 15 possible combinations of four cytokines (IFN-γ, TNF-α, IL-2, and IL-17A) were uniquely distinguished using logic combinations of the gates for each cytokine and FACSDiva (BD) software. Background frequencies of cells producing cytokines without antigen stimulation were subtracted.
Protective efficacy
Efficacy of rLVS ΔcapB- and rLm-vectored B. anthracis, Y. pestis, and F. tularensis vaccines was studied at CSU similarly to what was previously described by us17,18,19. Virulent strains of B. anthracis (Ames), Y. pestis (CO92), and F. tularensis (Schu S4) were originally obtained from BEI Resources, stored at −80 °C, and used to make working stocks for animal challenge experiments at CSU. Briefly, Y. pestis was grown to log phase at 37 °C in BHI broth and F. tularensis was grown on modified Mueller-Hinton agar plates and colonies collected into Mueller-Hinton broth. For both Y. pestis and F. tularensis, glycerol was added to the harvested bacterial suspensions to 15% (v/v) and the suspensions frozen in aliquots at −80 °C. B. anthracis spores were prepared using published procedures69, resuspended in PBS, and frozen in in aliquots at −80 °C. We pre-determined that the 50% lethal dose (LD50) of B. anthracis (Ames) spores, Y. pestis CO92, and F. tularensis Schu S4 administered intranasally (i.n.) in BALB/c mice is approximately 40,000, 250, and 1 CFU, respectively. Mice were sham-immunized or immunized with 2 or 3 doses of rLVS ΔcapB or rLm vaccines (homologous prime-boost vaccination) or primed-boosted with rLVS ΔcapB - rLm vaccines (heterologous prime-boost vaccination), challenged i.n. with virulent B. anthracis (Ames) spores, Y. pestis CO92, or F. tularensis Schu S4, weighed, and monitored for illness and death for 3 weeks, as indicated. Mice that met predetermined humane endpoints for euthanasia were euthanized and counted as a death. Mean survival time was calculated by dividing the sum of the surviving days of all animals by the total number of animals examined, with animals surviving until the end of the experiment given a time of 21 days, when the experiment was terminated.
Statistical analyses
The sample sizes for assaying vaccine clearance and dissemination (4/group/time point), immune responses after vaccination (4/group), and efficacy (8/group) after challenge were estimated based on previous and pilot studies (GraphPad StatMate 2.0). Means and SE of the mean (SEM) of serum antibody endpoint titer, cytokine production, and frequencies of cytokine-producing CD4+ and CD8+ T cells were reported, and means compared across groups by ANOVA with Tukey’s correction for multiple comparisons test using GraphPad Prism, 6.04 (San Diego, CA). A log-rank analysis (Mantel-Cox test) (Prism 6.04) was used to determine the significance of differences in survival curves among mice in vaccinated and control groups. Linear regression was used to obtain values for the slope and intercept and the correlation coefficient (R2) between pre-challenge serum antibody endpoint titer and post-challenge mean survival time (days) at 21 days post-challenge.
Data availability
All data supporting the findings of this study are available within the article and its supplementary information files or from the corresponding author upon request.
Change history
15 August 2018
The HTML and PDF versions of this Article previously published contained a version of Figure 6 in which the text for Figure 6a appeared incorrectly. This has now been corrected in the HTML and PDF versions of the Article.
References
Jernigan, D. B. et al. Investigation of bioterrorism-related anthrax, United States, 2001: epidemiologic findings. Emerg Infect Dis 8, 1019–1028 (2002).
Rosenzweig, J. A. et al. Progress on plague vaccine development. Appl Microbiol Biotechnol 91, 265–286 (2011).
Matyas, B. T., Nieder, H. S. & Telford, S. R. III. Pneumonic tularemia on Martha’s Vineyard: clinical, epidemiologic, and ecological characteristics. Ann N Y Acad Sci 1105, 351–377 (2007).
Alibek K. Biohazard: the chilling true story of the largest covert biological weapons program in the world, told from the inside by the man who ran it. Random House, Inc. (1999).
Inglesby, T. V. et al. Plague as a biological weapon: medical and public health management. Working Group on Civilian Biodefense. JAMA 283, 2281–2290 (2000).
Peterson, J. W. et al. Protection Afforded by Fluoroquinolones in Animal Models of Respiratory Infections with Bacillus anthracis, Yersinia pestis, and Francisella tularensis. Open Microbiol J 4, 34–46 (2010).
Pavlov, V. M., Mokrievich, A. N. & Volkovoy, K. Cryptic plasmid pFNL10 from Francisella novicida-like F6168: the base of plasmid vectors for Francisella tularensis. FEMS Immunol Med Microbiol 13, 253–256 (1996).
Athamna, A. et al. Selection of Bacillus anthracis isolates resistant to antibiotics. J Antimicrob Chemother 54, 424–428 (2004).
Galimand, M. et al. Multidrug resistance in Yersinia pestis mediated by a transferable plasmid. N Engl J Med 337, 677–680 (1997).
Titball, R. W. & Oyston, P. C. A vaccine for tularaemia. Expert opinion on biological therapy 3, 645–653 (2003).
Tao, P. et al. A Bivalent Anthrax-Plague Vaccine That Can Protect against Two Tier-1 BioterrorPathogens, Bacillus anthracis and Yersinia pestis. Frontiers in immunology 8, 687 (2017).
Baillie, L. W. et al. An anthrax subunit vaccine candidate based on protective regions of Bacillus anthracis protective antigen and lethal factor. Vaccine 28, 6740–6748 (2010).
Friedlander, A. M. & Little, S. F. Advances in the development of next-generation anthrax vaccines. Vaccine 27(Suppl 4), D28–32 (2009).
Galen, J. E. et al. A bivalent typhoid live vector vaccine expressing both chromosome- and plasmid-encoded Yersinia pestis antigens fully protects against murine lethal pulmonary plague infection. Infect Immun 83, 161–172 (2015).
Jia, Q., Lee, B. Y., Clemens, D. L., Bowen, R. A. & Horwitz, M. A. Recombinant attenuated Listeria monocytogenes vaccine expressing Francisella tularensis IglC induces protection in mice against aerosolized Type A F. tularensis. Vaccine 27, 1216–1229 (2009).
Huntley, J. F. et al. Native outer membrane proteins protect mice against pulmonary challenge with virulent type A Francisella tularensis. Infect Immun 76, 3664–3671 (2008).
Jia, Q. et al. A Francisella tularensis live vaccine strain (LVS) mutant with a deletion in capB, encoding a putative capsular biosynthesis protein, is significantly more attenuated than LVS yet induces potent protective immunity in mice against F. tularensis challenge. Infect Immun 78, 4341–4355 (2010).
Jia, Q., Bowen, R., Sahakian, J., Dillon, B. J. & Horwitz, M. A. A heterologous prime-boost vaccination strategy comprising the Francisella tularensis live vaccine strain capB mutant and recombinant attenuated Listeria monocytogenes expressing F. tularensis IglC induces potent protective immunity in mice against virulent F. tularensis aerosol challenge. Infect Immun 81, 1550–1561 (2013).
Jia, Q. et al. Francisella tularensis Live Vaccine Strain deficient in capB and overexpressing the fusion protein of IglA, IglB, and IglC from the bfr promoter induces improved protection against F. tularensis respiratory challenge. Vaccine 34, 4969–4978 (2016).
Lin, J. S. et al. TNFalpha and IFNgamma contribute to F1/LcrV-targeted immune defense in mouse models of fully virulent pneumonic plague. Vaccine 29, 357–362 (2010).
Szaba, F. M. et al. TNFalpha and IFNgamma but not perforin are critical for CD8 T cell-mediated protection against pulmonary Yersinia pestis infection. PLoS Pathog 10, e1004142 (2014).
Bruhn, K. W., Craft, N. & Miller, J. F. Listeria as a vaccine vector. Microbes Infect 9, 1226–1235 (2007).
Le, D. T. et al. A live-attenuated Listeria vaccine (ANZ-100) and a live-attenuated Listeria vaccine expressing mesothelin (CRS-207) for advanced cancers: phase I studies of safety and immune induction. Clin Cancer Res 18, 858–868 (2012).
Jia, Q., Dillon, B. J., Maslesa-Galic, S. & Horwitz, M. A. Listeria-vectored vaccine expressing the Mycobacterium tuberculosis 30 kDa major secretory protein via the constitutively active prfA* regulon boosts BCG efficacy against tuberculosis. Infect Immun 85, e00245–00217 (2017).
Lauer, P. et al. Constitutive Activation of the PrfA regulon enhances the potency of vaccines based on live-attenuated and killed but metabolically active Listeria monocytogenes strains. Infect Immun 76, 3742–3753 (2008).
Pannifer, A. D. et al. Crystal structure of the anthrax lethal factor. Nature 414, 229–233 (2001).
Ballard, J. D., Collier, R. J. & Starnbach, M. N. Anthrax toxin-mediated delivery of a cytotoxic T-cell epitope in vivo. Proc Natl Acad Sci USA 93, 12531–12534 (1996).
Zaide, G. et al. Identification and characterization of novel and potent transcription promoters of Francisella tularensis. Appl Environ Microbiol 77, 1608–1618 (2011).
Gallagher, L. A. et al. A comprehensive transposon mutant library of Francisella novicida, a bioweapon surrogate. Proc Natl Acad Sci USA 104, 1009–1014 (2007).
Ludu, J. S. et al. Genetic elements for selection, deletion mutagenesis and complementation in Francisella spp. FEMS Microbiol Lett 278, 86–93 (2008).
Lee, B. Y., Horwitz, M. A. & Clemens, D. L. Identification, recombinant expression, immunolocalization in macrophages, and T-cell responsiveness of the major extracellular proteins of Francisella tularensis. Infect Immun 74, 4002–4013 (2006).
Merkel, T. J. et al. Development of a highly efficacious vaccinia-based dual vaccine against smallpox and anthrax, two important bioterror entities. Proc Natl Acad Sci USA 107, 18091–18096 (2010).
Brockstedt, D. G. et al. Listeria-based cancer vaccines that segregate immunogenicity from toxicity. Proc Natl Acad Sci USA 101, 13832–13837 (2004).
Altmann, D. M. Host immunity to Bacillus anthracis lethal factor and other immunogens: implications for vaccine design. Expert Rev Vaccines 14, 429–434 (2015).
Chitlaru, T., Altboum, Z., Reuveny, S. & Shafferman, A. Progress and novel strategies in vaccine development and treatment of anthrax. Immunol Rev 239, 221–236 (2011).
Glomski, I. J., Corre, J. P., Mock, M. & Goossens, P. L. Cutting Edge: IFN-gamma-producing CD4 T lymphocytes mediate spore-induced immunity to capsulated Bacillus anthracis. J Immunol 178, 2646–2650 (2007).
Quenee, L. E., Ciletti, N. A., Elli, D., Hermanas, T. M. & Schneewind, O. Prevention of pneumonic plague in mice, rats, guinea pigs and non-human primates with clinical grade rV10, rV10-2 or F1-V vaccines. Vaccine 29, 6572–6583 (2011).
Lin, J. S., Kummer, L. W., Szaba, F. M. & Smiley, S. T. IL-17 contributes to cell-mediated defense against pulmonary Yersinia pestis infection. J Immunol 186, 1675–1684 (2011).
Chen, W., KuoLee, R., Shen, H. & Conlan, J. W. Susceptibility of immunodeficient mice to aerosol and systemic infection with virulent strains of Francisella tularensis. Microb Pathog 36, 311–318 (2004).
Conlan, W. J., Shen, H., Kuolee, R., Zhao, X. & Chen, W. Aerosol-, but not intradermal-immunization with the live vaccine strain of Francisella tularensis protects mice against subsequent aerosol challenge with a highly virulent type A strain of the pathogen by an alphabeta T cell- and interferon gamma- dependent mechanism. Vaccine 23, 2477–2485 (2005).
Wu, T. H. et al. Intranasal vaccination induces protective immunity against intranasal infection with virulent Francisella tularensis biovar A. Infect Immun 73, 2644–2654 (2005).
Griffin, A. J., Crane, D. D., Wehrly, T. D. & Bosio, C. M. Successful protection against tularemia in C57BL/6 mice is correlated with expansion of Francisella tularensis-specific effector T cells. Clin Vaccine Immunol 22, 119–128 (2015).
Eneslatt, K. et al. Signatures of T cells as correlates of immunity to Francisella tularensis. PLoS One 7, e32367 (2012).
Boyaka, P. N. et al. Effective mucosal immunity to anthrax: neutralizing antibodies and Th cell responses following nasal immunization with protective antigen. J Immunol 170, 5636–5643 (2003).
Ivins, B. E., Welkos, S. L., Little, S. F., Crumrine, M. H. & Nelson, G. O. Immunization against anthrax with Bacillus anthracis protective antigen combined with adjuvants. Infect Immun 60, 662–668 (1992).
Turnbull, P. C., Broster, M. G., Carman, J. A., Manchee, R. J. & Melling, J. Development of antibodies to protective antigen and lethal factor components of anthrax toxin in humans and guinea pigs and their relevance to protective immunity. Infect Immun 52, 356–363 (1986).
Reuveny, S. et al. Search for correlates of protective immunity conferred by anthrax vaccine. Infect Immun 69, 2888–2893 (2001).
Chen, L. et al. Comprehensive analysis and selection of anthrax vaccine adsorbed immune correlates of protection in rhesus macaques. Clin Vaccine Immunol 21, 1512–1520 (2014).
Fay, M. P. et al. Anthrax vaccine-induced antibodies provide cross-species prediction of survival to aerosol challenge. Sci Transl Med 4, 151ra126 (2012).
Leary, S. E., Griffin, K. F., Garmory, H. S., Williamson, E. D. & Titball, R. W. Expression of an F1/V fusion protein in attenuated Salmonella typhimurium and protection of mice against plague. Microb Pathog 23, 167–179 (1997).
Sun, W., Sanapala, S., Rahav, H. & Curtiss, R. III. Oral administration of a recombinant attenuated Yersinia pseudotuberculosis strain elicits protective immunity against plague. Vaccine 33, 6727–6735 (2015).
Boyer, J. L. et al. Protective immunity against a lethal respiratory Yersinia pestis challenge induced by V antigen or the F1 capsular antigen incorporated into adenovirus capsid. Hum Gene Ther 21, 891–901 (2010).
Brewoo, J. N., Powell, T. D., Stinchcomb, D. T. & Osorio, J. E. Efficacy and safety of a modified vaccinia Ankara (MVA) vectored plague vaccine in mice. Vaccine 28, 5891–5899 (2010).
Tao, P. et al. Mutated and bacteriophage T4 nanoparticle arrayed F1-V immunogens from Yersinia pestis as next generation plague vaccines. PLoS Pathog 9, e1003495 (2013).
Feodorova, V. A. & Motin, V. L. Plague vaccines: current developments and future perspectives. Emerging microbes & infections 1, e36 (2012).
Kummer, L. W. et al. Antibodies and cytokines independently protect against pneumonic plague. Vaccine 26, 6901–6907 (2008).
Williamson, E. D. & Oyston, P. C. Protecting against plague: towards a next-generation vaccine. Clin Exp Immunol 172, 1–8 (2013).
Chu, P. et al. Live attenuated Francisella novicida vaccine protects against Francisella tularensis pulmonary challenge in rats and non-human primates. PLoS Pathog 10, e1004439 (2014).
Reed, D. S. et al. Live attenuated mutants of Francisella tularensis protect rabbits against aerosol challenge with a virulent type A strain. Infect Immun 82, 2098–2105 (2014).
Rockx-Brouwer, D. et al. Low dose vaccination with attenuated Francisella tularensis strain SchuS4 mutants protects against tularemia independent of the route of vaccination. PLoS One 7, e37752 (2012).
Conlan, J. W. Tularemia vaccines: recent developments and remaining hurdles. Future Microbiol 6, 391–405 (2011).
Conlan, J. W. et al. Differential ability of novel attenuated targeted deletion mutants of Francisella tularensis subspecies tularensis strain SCHU S4 to protect mice against aerosol challenge with virulent bacteria: effects of host background and route of immunization. Vaccine 28, 1824–1831 (2010).
DuBois, A. B., Freytag, L. C. & Clements, J. D. Evaluation of combinatorial vaccines against anthrax and plague in a murine model. Vaccine 25, 4747–4754 (2007).
Salomonsson, E. et al. Reintroduction of two deleted virulence loci restores full virulence to the live vaccine strain of Francisella tularensis. Infect Immun 77, 3424–3431 (2009).
Twine, S. et al. A mutant of Francisella tularensis strain SCHU S4 lacking the ability to express a 58-kilodalton protein is attenuated for virulence and is an effective live vaccine. Infect Immun 73, 8345–8352 (2005).
Maier, T. M. et al. Construction and characterization of a highly efficient Francisella shuttle plasmid. Appl Environ Microbiol 70, 7511–7519 (2004).
Yan, L. et al. Selected prfA* mutations in recombinant attenuated Listeria monocytogenes strains augment expression of foreign immunogens and enhance vaccine-elicited humoral and cellular immune responses. Infect Immun 76, 3439–3450 (2008).
Lauer, P., Chow, M. Y., Loessner, M. J., Portnoy, D. A. & Calendar, R. Construction, characterization, and use of two Listeria monocytogenes site-specific phage integration vectors. J Bacteriol 184, 4177–4186 (2002).
Lyons, C. R. et al. Murine model of pulmonary anthrax: kinetics of dissemination, histopathology, and mouse strain susceptibility. Infect Immun 72, 4801–4809 (2004).
Acknowledgements
We thank Nicole Marlenee for technical support with in vivo challenge experiments at CSU and Scott Beardon for providing the EV76 strain of Y. pestis.
Author information
Authors and Affiliations
Contributions
M.A.H. and Q.J. conceived and oversaw the project; R.B. oversaw in vivo challenge experiments; Q.J. designed molecular constructs; Q.J., B.T.C. and A.C.K. completed vaccine molecular construction; Q.J. B.J.D. and S.M.G conducted in vitro and in vivo immunology experiments; Q.J. processed data; Q.J. and M.A.H. wrote the manuscript. All authors reviewed the manuscript in final form.
Corresponding author
Ethics declarations
Competing Interests
This study was supported by National Institutes of Health grant AI101189. Flow cytometry was performed in the UCLA Jonsson Comprehensive Cancer Center (JCCC) and Center for AIDS Research Flow Cytometry Core Facility that is supported by National Institutes of Health awards P30 CA016042 and 5P30 AI028697, and by the JCCC, the UCLA AIDS Institute, and the David Geffen School of Medicine at UCLA. M.A.H. and Q.J. are inventors on patent applications filed by UCLA that include data presented herein.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jia, Q., Bowen, R., Dillon, B.J. et al. Single vector platform vaccine protects against lethal respiratory challenge with Tier 1 select agents of anthrax, plague, and tularemia. Sci Rep 8, 7009 (2018). https://doi.org/10.1038/s41598-018-24581-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-24581-y
This article is cited by
-
Replicating bacterium-vectored vaccine expressing SARS-CoV-2 Membrane and Nucleocapsid proteins protects against severe COVID-19-like disease in hamsters
npj Vaccines (2021)
-
Plague vaccines: new developments in an ongoing search
Applied Microbiology and Biotechnology (2021)
-
Plague vaccine: recent progress and prospects
npj Vaccines (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.