Abstract
Amnestic mild cognitive impairment (aMCI) conversion to Alzheimer’s disease (AD) is seen in a sizable portion of aMCI patients; correlates predicting such conversion are poorly defined but neuroinflammation and the reactivation of chronic viral infections are suspected to play a role in this phenomenon. We analyzed these aspects in two homogeneous groups of aMCI who did or did not convert to AD over a 24-months period. Results showed that at baseline in those aMCI individuals who did not convert to AD: 1) Aβ1-42 stimulated production of the pro-inflammatory cytokines IL6 and IL1β by CD14+ cells was significantly reduced (p = 0.01), 2) CD14+/IL-33+ cells were increased (p = 0.0004); 3) MFI of TLR8 and TLR9 was significantly increased, and 4) better preserved hippocampus volumes were observed and correlated with IL33+/CD14+ cells. Notably, Aβ1-42 stimulated production of the antiviral cytokine IFN-λ was increased as well in non-AD converters, although with a borderline statistical significance (p = 0.05). Data herein indicating that proinflammatory cytokines are reduced, whereas IFN-λ production and TLR8 and 9 MFI are augmented in those aMCI in whom AD conversion is not observed suggest that the ability to mount stronger antiviral response within an antiiflammatory milieu associates with lack of AD conversion.
Similar content being viewed by others
Introduction
Mild cognitive impairment (MCI) is defined as a subjective and objective decline in cognitive performance that is greater than expected for an individual’s age and education level, but does not meet criteria for the diagnosis of dementia1,2,3. Elderly MCI patients are nevertheless at high-risk for developing dementia and, in particular, Alzheimer’s disease (AD)3,4,5. Recently, the International Working Group (IWG) introduced the terminology of MCI to refer to individuals with cognitive impairment that is not as severe as compared to what is seen in AD patients6. This situation thus represents a borderline condition between normal aging and AD7. Notably, although the diagnostic accuracy has certainly increased, correlates of MCI conversion to AD are still poorly defined.
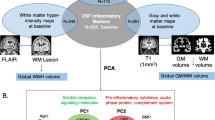
The estimated annual rate of MCI conversion to AD ranges between 10% and 15%8, and MCI individuals in whom memory loss is the predominant symptom (amnestic MCI -aMCI-) are more prone to progress to AD. Predictive studies have described a number of biological and cognitive factors, including cognitive reserve9, performance in cognitive testing10, and the presence and concentration of biomarkers in the cerebrospinal fluid (CSF)11,12,13; that are suggested to correlate with AD conversion. Volumetric magnetic resonance imaging (MRI)14,15,16 and fluorodeoxyglucose and Pittsburgh compound B positron emission tomography (FGD-PET, PIB-PET)17,18 can also be useful in order to recognize those patients in whom AD conversion is more likely to occur. In particular, hippocampal volume as measured with MRI advanced techniques is a well-known biomarker of downstream neural degeneration or injury2. Although not suitable for defining preclinical AD-stage if considered as unique index, this downstream topological biomarker is adequate for the screening of subjects at risk, as recently stressed19.
The validity of these results is nevertheless hampered by the fact that most of published studies utilized a single marker to predict progression to AD9,10,14,15,16 even if this phenomenon is multifactorial. Such multidimensionality,is reflected in the observation that a combination of MRI (hippocampal volumes)14,15,16, genetic (ApoE)20 and humoral (CSF levels of beta amyloid and phosporylated τ protein)11,12,13 indexes is currently suggested to have the greatest predictive value toward AD conversion.
Genetic and environmental factors interact in the pathogenesis of AD, a complex and still scarcely understood process in which viral infections, and in particular Human Herpes Simplex virus type 1 infection (HSV-1) are suggested to play a role21,22,23,24,25. Microbial infections stimulate innate immunity via binding of the pathogen associated molecular patterns (PAMPS) they express to toll like receptors (TLR). Nucleic acids produced upon viral replication, in particular, ligate TLR8 and 926,27 result in the activation of innate immunity and the production of multiple cytokines, amongst which interferon-lambda (IFN-λ) plays a pivotal role in limiting viral replication and the infection of target cells28. Recent results indicating that TLR expression is increased in immune cells of MCI individuals29,30 led to hypothesize that stronger immune responses to viruses could be detected in these individuals.
We analyzed whether immune correlates that predict MCI conversion into AD could be identified analyzing immunological parameters in a cohort of aMCI patients in whom AD conversion was or was not observed over a 24-months period. In addition, we also analyzed one of the MRI biomarker of AD-associated neural injury, the hippocampal volume.
Results herein suggest that stronger antiviral responses in the absence of inflammation is correlated to better preservation of the hippocampus volume and could predict AD conversion.
Results
Clinical characteristics of the individuals enrolled in the study
Demographic and clinical characteristic of the individuals enrolled in the study are summarized in Table 1. As per inclusion criteria, no differences were observed in gender, age, years of education, global cognitive levels (MMSE) and ApoE4 status when AD converters and AD non-converters were compared at baseline.
TLR8 and TLR9 expressing CD14+ cells
CD14+ immune cells of AD converters and AD non-converters were either unstimulated or stimulated with TLR8 and 9 agonists (ODN and ssRNA, respectively), and the percentage of TLR-expressing cells was examined by flow-cytometry. Results showed that, whilst no differences were seen in unstimulated conditions (<1% of CD14+ cells expressed TLR8 or TLR9; data not shown), agonist-stimulated TLR8- and TLR9-expressing CD14+ cells were augmented, albeit not significantly, in AD non-converters (medians: TLR8 = 2.9%, TLR9 = 3.1%) compared to AD converter (medians: TLR8 = 1.6%, TLR9 = 2%; p = 0.06 in both cases) (Fig. 1). Notably, though, TLR8 and TLR9 Mean Fluorescence Intensity (MFI) was significantly increased in AD non-converters compared to AD converters (p = 0.0004, and p = 0.0001, respectively) (Table 2).
TLR8 and TLR9 expressing CD14+ cells: TLR8- (upper panels) and TLR9- (lower panels) expressing CD14+ cells upon stimulation with specific agonists (ODN and ssRNA, respectively). Representative results in MCI individuals who did (AD-converters) or did not (AD non-converters) convert to AD over a 24-months period are presented in the left part of the figure; in the upper right corner the percentage of CD14/TLR8+ and CD14/TLR9+ cells is shown. Summary results were obtained in 21 AD converters and 25 AD non-converters and are shown in the bar graphs. The boxes stretch from the 25 to the 75 percentile; the line across the boxes indicates the median values; the lines stretching from the boxes indicate extreme values. Outside values are displayed as separate points.
Pro-and anti-inflammatory cytokine mRNA expression in Aβ1-42 stimulated PBMC
Quantitative PCR analyses were performed in PBMC that were either cultured in medium alone or were stimulated with Aβ1-42 (Fig. 2A). Results obtained in Aβ1-42– stimulated cells indicated that IL-1β and IL-6 mRNA was greatly reduced in AD non-converters compared to AD converters (IL1β > 200 fold; IL6 > 1000 fold; p = 0.04 and p = 0.05 respectively). In contrast, no significant results (n-Fold change < 2) were obtained for IFN-λ 1,2,3 mRNA expression. Results also showed that IL-33 mRNA was robustly (>100 fold) increased in AD non-converters (Fig. 2A).
Pro-and- anti-inflammatory cytokine mRNA expression and protein in stimulated cells: (A) Aβ1-42-stimulated IL-1β, IL-6 and IL-33 mRNA expression in MCI individuals who did (AD converters, N = 21) or did not (AD non-converters, N = 25) convert to AD over a 24-months period. Gene expression was calculated relative to GAPDH housekeeping gene. The expression of the genes is assessed by single real-time quantitative RT-PCR and shown as median of fold-change expression from the unstimulated samples. Summary results are shown in the bar graphs using TIGR Multi Experiment Viewer (MeV)v4.9. Aβ1-42-stimulated IL-1β and IL-6 production (B); IL-33 expressing CD14+ cells (%) (C), and IFN-λ production (D) in PBMC of MCI individuals who did (AD converters; N = 21) or did not (AD non-converters; N = 25) convert to AD over a 24-months period. The boxes stretch from the 25 to the 75 percentile; the line across the boxes indicates the median values; the lines stretching from the boxes indicate extreme values. Outside values are displayed as separate points. Statistical significance is shown.
Pro-and anti-inflammatory cytokine production by Aβ1-42 -stimulated PBMC
Cytokine production was measured by ELISA in supernatants of PBMC that were either unstimulated or were stimulated with Aβ1-42. Once again, no differences were observed in unstimulated conditions (data not shown). When Aβ1-42- stimulated IL-1β and IL-6 production was measured, nevertheless, results showed that both these pro-inflammatory cytokines were significantly reduced in AD non-converters, compared to AD converters (p = 0.005 and p = 0.014 respectively) (Fig. 2B). These results support the idea that the presence of an inflammatory milieu associates with AD conversion in individuals with a diagnosis of aMCI.
IL-33 could not be measured in supernatants of Aβ1-42-stimulated PBMC, possibly because the mature form of this cytokine is not cleaved and secreted. Results obtained by flow-cytometry, nevertheless showed that CD14+/IL-33+ cells were significantly increased in AD non-converters compared to AD converters (p = 0.0004) (Fig. 3B).
Brain mask of aMCI-typical Hippocampus-region and MRI analysis: an example of automatic hippocampal segmentation using the ADABoost algorithm. Coronal, axial and sagittal brain views in a single subject are shown in the upper part (A); left (LH) and right (RH) hyppocampal volumes as evaluated by MRI in MCI individuals who did (AD converters, N = 13) or did not (AD non-converters, N = 14) convert to AD over a 24-months period. The boxes stretch from the 25 to the 75 percentile; the line across the boxes indicates the median values; the lines stretching from the boxes indicate extreme values. Outside values are displayed as separate points. Statistical significance is shown (B).
Antiviral cytokines: IFN-λ 1–3 production by Aβ1-42- stimulated PBMC
IFN-λ 1–3 production by unstimulated and Aβ1-42- stimulated PBMC was measured in all the individuals enrolled in the study. Results showed that Aβ1-42- stimulated IFN-λ 1–3-production was higher in AD non-converters compared to AD converters (p = 0.05), suggesting that the ability to mount robust antiviral immune responses correlates with lack of progression to AD (Fig. 3C).
MRI results and correlations
High-resolution structural MRI acquisition was available at baseline in 27 aMCI individuals, 13 of whom did (5 males, mean age 75 ± 6.3 years) and 14 of whom did not (6 males, mean age 73 ± 7.1 years) progress to AD. The two “MRI subgroups” (AD converters and AD non-converters) were comparable for age (two sample t-test, p = 0.4785) and gender (chi-square, p = 0.8731) at baseline. MRI volumetric measurements at baseline showed a trend indicating a better preservation of hippocampi volumes in AD non-converters, with a stronger effect when the right hippocampus was analyzed (AD non-converters vs. AD converters, left hippocampus (H-LV), F(1,27) = 13.7, p = 0.001 (and right hippocampus (H-RV), F(1,27) = 17.25, p = 0.004 (Fig. 3B).
Notably, the analyses of correlations indicated a significant positive association between CD14+/IL-33+ cells and the volumes of both left and right (p = 0.049 and p = 0.043 respectively) hippocampus in AD non-converters alone (Fig. 4). No significant differences were found when correlations between MRI results and other immunological parameters were evaluated.
MRI analysis and correlations: Rank correlation between Aβ1-42 stimulated IL-33 producing CD14+ cells and the Left (L) and Right (R) hippocampus volume (HV) in MCI individuals who did (N = 13) or did not (N = 14) convert to AD. Statistical significance and Spearman’s coefficient of rank correlation (rho) are shown.
Discussion
In mild cognitive impairment a slight but noticeable and measurable decline in cognitive abilities can be detected. Individuals with a diagnosis of MCI, and in particular those with a diagnosis of amnestic MCI (aMCI), have an increased risk of developing AD. Clinical, biological and imaging markers predicting MCI conversion to AD are still poorly clarified, possibly because the etiopathogenesis of AD itself is still barely understood. We analyzed immunologic and imaging markers in two groups of aMCI individuals who did or did not convert to AD over a 24 months period. We described herein a combination of these markers that might be useful in predicting which patients will convert to AD.
We focused on imaging analyses of MRI-based measures of hippocampal volumes, one of the core diagnostic criteria for probable AD dementia2; thus we verified whether this parameter could be used as a biomarker to assess the presence of downstream neuronal degeneration or injury. Notably, hippocampal volume was recently suggested to be a possibly adequate index for the screening of subjects at risk of developing AD19,31.
Results showed that, besides being associated with a peculiar cytokine profile, lack of MCI conversion to AD in our aMCI individuals was also correlated with better preserved hippocampal volumes, with a more pronounced effect in the right hippocampus. Importantly, better preserved hippocampal volumes were associated with higher percentages of circulating CD14+/IL-33+ cells in AD non-converters alone, suggesting a role for this cytokine in contrasting progression to AD in individuals with a diagnosis of aMCI. It is worth remarking that our analysis was adjusted for age, considering that increased variability in cognition with age has been argued as an indication of pathological processes32. These results support data indicating that MCI affects the size of the hippocampus, and that this parameter, together with the rate of hippocampus shrinkage, can be useful in predicting whether MCI does progress to AD33.
Viral infections, and in particular reactivation of HSV-1 infection34,35 are suggested to be involved in the pathogenesis of AD34; this hypothesis was recently reinforced by data indicating that accumulation of Aβ in the brain, the hallmark of AD, could play an antimicrobial role36. Immune defenses against viruses are initiated by ligation of TLR3, 8 and 9 by products of viral replication; this results in the production of cytokines with inflammatory and antiviral properties37. We and others have observed that the expression of TLRs that are engaged by viral PAMPs is up-regulated in CD14+ immune cells of MCI individuals30,38 possibly suggesting that stronger antiviral responses could be present in MCI. As a confirmation of this hypothesis, we show herein the presence of a significantly higher density of TLR8 and 9 on CD14+ cells in MCI patients that did not converter to AD, suggesting that a higher expression of viral PAMPs-specific immune sensors is associated with lack of disease progression.
Amongst the cytokines that were differentially modulated in AD converters and AD non-converters, and that are part of TLR-stimulated innate immune responses, IFN-λ stood out. IFN-λ includes at least three slightly different proteins that trigger mechanisms that contribute to the clearance of viral infections39,40 and, in particular, potently target HSV-141,42. We recently described the presence of a positive correlation between HSV-1-specific serum antibody titers and grey matter volumes in the brain area that are classically affected by AD43. It is thus tempting to speculate that stronger IFN-λ-mediated antiviral responses could play a role in avoiding progression to AD by impeding the excessive reactivation of viruses that persistently infect the CNS, possibly including HSV-1.
AD has been associated with neuroinflammation as the production of a number of pro-inflammatory cytokines is increased in cells of AD patients44. We observed that Aβ1-42-stimulated production of IL-1β and IL-6, in particular, discriminate between those aMCI individuals who progress to AD, and those in whom such progression is not observed. IL-1β has long been known to play a role in the pathogenesis of AD41,45. This cytokine promotes amyloid plaque deposition, induces a loss of phagocytic activity by the microglia, stimulates the hyperphosphorylation of τ protein, and affects synaptic plasticity46. As a consequence, IL-1β can impair learning and memory processes. IL-1β also recruits peripheral leukocytes to the brain parenchyma45. Peripheral monocytes are able to directly cross the BBB, both generating novel microglial cells and potentially further extending chronic neuroinflammation47. Since these cells are considered to be better at amyloid plaque removal than resident microglia48, increases in IL-1β production were suggested to be a -possibly futile- attempt by the brain parenchyma to control β-amyloid accumulation. IL-6 concentration is also known to be increased both in animal models of AD and in patients49,50. Aβ directly stimulates the generation of IL-6 by human cortical neurons, playing a role in the production and the processing of amyloid precursor protein (APP). IL-6 also plays an important role in regulating cognitive function. Thus: i) elevated IL-6 correlates with age-related cognitive decline in humans, and ii) excessive IL-6 production alters spatial learning and memory51,52. Our results indicate that higher IL-1β and IL-6 production is detected in aMCI individuals converting into AD, reinforcing the idea that increased quantities of these inflammatory cytokines play a deleterious role in the development of AD.
IL-33 was also analyzed; this cytokine belongs to the IL-1β family and is a dual function protein with both intra and extra-cellular mechanisms of action. IL-33 can interact with the transcription factor NF-KB reducing NF-KB-triggered gene expression to dampen pro-inflammatory signalling53. Nuclear IL-33 can also induce the expression of intercellular and of vascular adhesion molecules for endothelial cell activation though binding to the p65 promoter54. Thus, IL-33 may have a role in regulating pathophysiology and inflammatory responses in the CNS55. IL-33 is reduced in AD brains, and this cytokine is believed to have a neuroprotective role secondary to the reduction of Aβ peptides secretion and the activation of their phagocytosis by the microglia56. The complexity of this cytokine is further underlined by recent results showing that three different polymorphism within the IL-33 gene resulting in a protective haplotype are associated with risk of AD56. Notably, recent results showed that in the APP/PS1 mouse model of AD IL-33 polarizizes microglia/macrophage toward an anti-inflammatory phenotype and reduces the expression of proinflammatory cytokines, including IL-1β and IL-652,57. Indeed our results indicate that increased amounts of IL-33 correlate with lower production of IL-1β and IL-6 in AD non-converters. Taken together, these results suggest that higher amounts of IL-33 in aMCI individuals in whom AD conversion is not observed is a successful strategy to reduce neuroinflammation.
All aMCI patients enrolled in the study were selected after retrospective analysis of a cohort of MCI patients; selection was based on the availability of neurocognitive evaluation at baseline and after 24 months, and of peripheral blood cells (PBMC) samples and brain MRI at baseline. Although the overall validity of our data is somewhat limited by the small number of patients analyzed, these results suggest that neuroinflammation, possibly associated with weaker antiviral responses, plays a fundamental pathogenetic role in AD.
Methods
Patients
This study was approved by and carried out in accordance with the guidelines of the ethic committee of the Don Gnocchi Foundation. All participants or, if unable, their care-givers, gave informed consent to a protocol approved by the local ethics committee according to a protocol approved by the local ethics of the Don Gnocchi Foundation. The study conformed to the ethical principles of the Helsinki Declaration.
A large cohort of MCI individuals is followed by the Unit of Rehabilitative Neurology at the Don C. Gnocchi Foundation in Milano, Italy; a portion of these individuals is affected by amnestic MCI (aMCI). The diagnosis of aMCI fulfills Grundman’s and Petersen’s operational criteria7,58. Within the aMCI cohort two homogeneous groups of subjects (21 AD converters and 25 AD non-converters) were selected for the study. Inclusion criteria were based on: a) availability of a clinical follow up for at least 24 months; b) neurocognitive evaluation (MMSE) at baseline as well as after follow-up; c) availability of PBMC samples at baseline; and d) availability of a 3D single high-resolution structural MRI acquisition at baseline in addition to conventional MRI scans (in this case data were available in 13 AD converters and 14 AD non- converters) at baseline. The clinical diagnosis of AD was performed according to the NINCDS-ADRDA work group criteria2. The study conformed to the ethical principles of the Helsinki Declaration. All patients or, if unable, their care-givers, gave informed consent to a protocol approved by the local ethics committee.
Blood sample collection and cell separation
Whole blood was collected by venipuncture in EDTA-containing Vacutainer tubes (Becton Dickinson & Co, Rutherford, NJ, USA). Peripheral blood mononuclear cells (PBMCs) were separated on lymphocyte separation medium (Ficoll-Hypaque, Organon Teknika Corp, Durham, NC, USA) and washed twice in PBS; viable leukocytes were determined using a TC20 Automated Cell Counter (Biorad Hercules,California, USA), PBMC were frozen and cold-preserved in liquid nitrogen in a cryoprotective media containing 10% dimethyl sulfoxide (DMSO) and fetal bovine serum (FBS). When needed for the experiments PBMC were thawed at 37 °C, washed in PBS and resuspended in RPMI 1640 to ensure optimal PBMC viability (>90%) for the cell culture.
Cell cultures
PBMC (1 × 106/ml) were cultured in RPMI 1640 supplemented with 10% human serum, 2 mM L- glutamine, and 1% penicillin (Invitrogen, Ltd, Paisley, UK) and incubated at 37 °C in a humidified 5% CO2 atmosphere for 24 h. PBMC were stimulated with 10 μg/ml synthetic oligonucleotides containing unmethylated CpG dinucleotides (ODN); 2 μg/ml single-stranded RNA oligonucleotide (ssRNA); or Aβ1-42 (10 μg/ml)(Sigma-Aldrich), St. Louis, MO or medium alone. Supernatants were used for cytokine detection; PBMC pellet were used for flow-cytometry analyses.
ApoE genotyping
Genomic DNA was isolated from whole blood by phenol-chloroform extraction. Customer-design Taqman probes for the 112 and 158 codons were used to determine the genotype of apolipoprotein E gene (APOE)43.
RNA extraction and reverse transcription
RNA was extracted from unstimulated or Aβ1-42 stimulated-PBMC and reverse transcribed into first-strand cDNA59,60. Real Time quantitative Reverse Transcription PCR (RQPCR) was performed using the ABI Prism 7000 instrument (PE Applied Biosystems, Foster City, CA, USA) with gene specific primers and SybrGreen chemistry described elsewhere59,60. The following cytokines were analyzed: IL-1β, IL-6, IL-33 (Qiagen, Hilden Germany) and IFNλ 1, 2, 3 (Sino Biological, LuDong Area, BDA China). Specific PCR products amplification was detected using the RT2 SYBR Green Fluor with a 25 μl final volume of 12.5 μl RT2 qPCR Mastermix (Qiagen), 10.5 μl H2O, 1.0 μl of either diluted template RT2 qPCR Primer Assay. Results were expressed as ΔΔCt and presented as ratios between the target gene and the Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) housekeeping mRNA. Experiments were individually run on each one of the individuals included in the study.
Flow cytometry immunofluorescent staining
PBMC were stained with anti-CD14-PC7 (clone RMO52, isotype mouse IgG2a, Beckman Coulter) and treated with the FIX and PERM Cell kit (eBioscience, San Diego, CA) before being stained with TLR8-PE (clone 610015, isotype mouse IgG1, R&D Systems), TLR9-FITC (clone M9.D6, isotype rat IgG2a, eBioscience), or IL33-APC (clone 390412, isotype rat IgG2b, R&D Systems) specific mAbs.
Flow cytometry
Analyses were performed using a Beckman-Coulter Cytomics FC-500 flow cytometer equipped with a single 15 mW argon ion laser operating at 488 nm and interfaced with CXP Software 2.1 and Beckman-Coulter GALLIOS flow cytometer equipped with a 22 mW Blue Solid State Diode laser operating at 488 nm and with a 25 mW Red Solid State Diode laser operating at 638 nm, and interfaced with Kaluza analysis software. Green florescence from FITC was collected through a 525-nm bandpass filter, orange-red fluorescence from PE was collected through a 575-nm bandpass filter and blue fluorescence from PC7 was collected through a 770-nm bandpass filter excited by 488 nm laser (FC-500); far-red fluorescence from APC was collected through a 660/20-nm bandpass filter excited by 638 nm laser (GALLIOS). Two-hundred-thousand cells were acquired and gated on lymphocyte and monocyte forward and side scatter properties. Data were collected using linear amplifiers for forward and side scatter and logarithmic amplifiers for fluorescences. Samples were first run using isotype control or single fluorochrome-stained preparations for color compensation. Rainbow Calibration Particles (Spherotec, Inc. Lake Forest, IL) were used to standardize flow-cytometry results in samples obtained over time.
Measurement of cytokines: ELISA
IL-1β, IL-6, IL-33 and human Interferon-lambda (IFN-λ)1–3 concentration was measured in supernatants of either unstimulated or Aβ1-42-stimulated PBMC by multiplex sandwich immunoassays according to the manufacturer’s recommendations (Quantikine Immunoassay; R&D Systems). Briefly, 200 μl per well of standard, sample, or control were transferred into the IL-1β, IL-6 or IFN-λ antigens coated polystyrene microwells and the plates were incubated for 2 hours at room temperature. After three washing steps with washing buffer to remove the unbound proteins, 200 μl of Human IL-1β IL-6 or IFN-λ peroxidase conjugate was added to each well and incubated at room temperature for 2 hours. After re-washing step, 200 μl of chromogen/substrate solution were added to each well and incubated at room temperature for 20 min protect from light. Finally, 50 μl of stop solution were added to each well and the reaction stopped. The wells were read on a plate reader (Sunrise, Tecan, Mannedorf, Switzerland) and optical densities (OD) of wells were determined at 450/620 nm. The measured absorbance is proportional to the concentration of cytokines (IL-1β or IL-6) and IFN-λ present in the supernatants expressed in pg/ml and calculated by dividing optical density (OD) measurement generated from the assay by OD cut-off calibrator. All the experiments were performed in duplicate. Sensitivity (S) and Assay Range (AR) were as flows: S: IL-1β = 1 pg/ml, IL-6 = 0,7 pg/ml and IFN-λ = 50ng/ml; AR: IL-1β 3.9–250 pg/ml, IL-6 3.1–300 pg/ml, IFN-λ = 62,5–4000 ng/ml.
MRI analysis
Hippocampal volume data have been extracted for each subject from high-resolution T1 3D images collected using a 1.5T scanner (Siemens, AVANTO) at the time of MCI diagnosis - MPRAGE; TR/TE = 1900/3.37 ms, FoV = 192 mm × 256 mm, in-plane resolution 1 mm × 1 mm, slice thickness = 1 mm, number of axial slices = 176) using AdaBoost (see Fig. 3A), a fully-automated machine-learning segmentation algorithm61,62. ADABoost is a fully-automated machine-learning segmentation algorithm implementing the EADCADNI harmonized hippocampal segmentation protocol for Alzheimer-related pathologies, able to automatically segment subcortical structures as hippocampus. Hippocampal volumetries were compared across the two groups (AD-converters and AD non-converters) at baseline and were also used to compute regression analyses with anti-inflammatory cytokines production.
Statistical analysis
Quantitative data were not normally distributed (Shapiro-Wilk test) and are thus summarized as median and interquartile range (IQR; 25° and 75° percentile). Firstly, comparisons between two groups (AD converters and non converters) were analyzed to evaluate immunological differences; comparisons were made using a 2-tailed Mann-Whitney U test for independent samples. Data analysis was performed using the MedCalc statistical package (MedCalc Software bvba, Mariakerke, Belgium).
Secondly, we performed Kruskal-Wallis ANOVA models, adjusted for MMSE to compare right and left hippocampal volume levels in the two groups of AD converters and AD non-converters. This analysis was performed using the package “sm” of the R software, freely available. Thirdly, separately in each group of AD-converters and AD non-converters, we calculated the correlations (using Spearman’s coefficient) between hippocampal volume levels and other immune parameters. P-values < 0.05 are reported as statistically significant in the text. Power was calculated with the G-power software63. Notwithstanding the small samples, effect sizes were reasonably large and attained power was above 0.90 for all comparisons.
References
Albert, M. S. et al. The diagnosis of mild cognitive impairment due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 7, 270–9 (2011).
McKhann, G. M. et al. The diagnosis of dementia due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 7, 263–9 (2011).
Sperling, R. A. et al. Toward defining the preclinical stages of Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 7, 280–92 (2011).
Luck, T. et al. Prediction of incident dementia: impact of impairment in instrumental activities of daily living and mild cognitive impairment-results from the German study on ageing, cognition, and dementia in primary care patients. Am J Geriatr Psychiatry 20, 943–54 (2012).
Manly, J. J. et al. Frequency and course of mild cognitive impairment in a multiethnic community. Ann Neurol. 63, 494–506 (2008).
Dubois, B. et al. Revising the definition of Alzheimer’s disease: a new lexicon. Lancet Neurol. 9, 1118–27 (2010).
Petersen, R. C. et al. Mild Cognitive Impairment. Arch Neurol. 56, 303–8 (1999).
Petersen, R. C. et al. Mild cognitive impairment as a diagnostic entity. J. Intern. Med. 256, 183–194 (2004).
Valenzuela MJ and Sachdev P. Brain reserve and dementia: A systematic review. Psychol Med. 36, 441–54 (2006).
Albert, M. S., Moss, M. & Blacker, D. Longitudinal change in cognitive performance among individuals with mild cognitive impairment. Neuropsychology 21, 158–169 (2007).
Buchhave, P. et al. Cerebrospinal fluid levels of amyloid 1-42, but not of tau, are fully changed already 5 to 10 years before the onset of Alzheimer dementia. Arch Gen Psychiatry 69, 98–106 (2012).
van Rossum, I. et al. Injury markers predict time to dementia in subjects with MCI and amyloid pathology. Neurology 7–9, 1809–1816 (2012).
Canuet, L. et al. Network disruption and cerebrospinal fluid amyloid-beta and phospho-tau levels in mild cognitive impairment. J Neurosci. 35, 10325–30 (2015).
Devanand, D. P. et al. Hippocampal and entorhinal atrophy in mild cognitive impairment: Prediction of Alzheimer disease. Neurology 68, 828–836 (2006).
López, M. E. et al. Alpha-band hypersynchronization in progressive mild cognitive impairment: a magnetoencephalography study. J Neurosci. 34, 14551–59 (2014).
Clerx, L. et al. Measurements of medial temporal lobe atrophy for prediction of Alzheimer’s disease in subjects with mild cognitive impairment. Neurobiol Aging. 34, 2003–13 (2013).
Grimmer, T. et al. The usefulness of amyloid imaging in predicting the clinical outcome after two years in subjects with mild cognitive impairment. Curr. Alzheimer Res. 10, 82–5 (2013).
Hatashita, S. & Yamasaki, H. Diagnosed mild cognitive impairment due to Alzheimer’s disease with PET biomarkers of beta amyloid and neuronal dysfunction. PLoS One 8, e66877 (2013).
Dubois, B. et al. Preclinical Alzheimer’s disease: Definition, natural history, and diagnostic criteria. Alzheimers Dement 12(3), 292–323 (2016).
Reitz, C. & Mayeux, R. Use of genetic variation as biomarkers for mild cognitive impairment and progression of mild cognitive impairment to dementia. J. Alzheimers Dis. 19, 229–251 (2010).
Ball, M. J. Limbic predilection in Alzheimer’s dementia: is reactivated herpesvirus involved? Can. J. Neurol. Sci. 9, 303–6 (1982).
Itzhaki, R. F. et al. Herpes simplex virus type 1 in brain and risk of Alzheimer’s disease. Lancet 349(9047), 241–244 (1997).
Letteneur, L. et al. Seropositivity to herpes simplex virus antibodies and risk of Alzheimer’s disease: a population-based cohort study. PLoS One 3(11), e3637 (2008).
Itzhaki, R. F. et al. Microbes and Alzheimer’s Disease. J. Alzheimers Dis. 51(4), 979–84 (2016).
Agostini, S. et al. High avidity HSV-1 antibodies correlate with absence of amnestic Mild Cognitive Impairment conversion to Alzheimer’s disease. Brain Behav Immun. 58, 254–260 (2016).
Lester, S. N. & Kui, L. Toll like receptors in antiviral immunity. J. Mol Biol. 426(6), 1246–1264 (2014).
Zhang, Y. et al. HCV RNA Activates APCs via TLR7/TLR8 While Virus Selectively Stimulates Macrophages Without Inducing Antiviral Responses. Scientific Reports 6, 29447 (2016).
Egli, A. et al. The impact of the interferon-lambda family on the innate and adaptive immune response to viral infections. Emerg Microbes Infect. 3(7), e51 (2014).
Saresella, M. et al. Increased activity of Th-17 and Th-9 lymphocytes and a skewing of the post-thymic differentiation pathway are seen in Alzheimer’s disease. Brain Behav. Immun. 5(3), 539–47 (2011).
Gambuzza, M. E. et al. Toll-like receptors in Alzheimer’s disease: a therapeutic perspective. CNS Neurol Disord Drug Targets 13, 1542–58 (2014).
Khan, V. et al. A Multi-Cohort Study of ApoE 4 and Amyloid-_Effects on the Hippocampus in Alzheimer’s Disease. J. Alzheimer’s Dis. 56, 1159–1174 (2017).
Ferreira, D. et al. Cognitive Variability during Middle-Age: Possible Association with Neurodegeneration and Cognitive Reserve. Front Aging Neurosci. 9, 188 (2017).
Carmichael, O. et al. and the Alzheimer’s Disease Neuroimaging Initiative. Localized hippocampus measures are associated with Alzheimer pathology and cognition independent of total hippocampal volume. Neurobiol. Aging. 33(6), 1124 e31–41 (2012).
Lovheim, H. et al. Herpes simplex infection and the risk of Alzheimer’s disease: A nested case-control study. Alzheimer’s Dem. 11, 587–92 (2015).
Harris, S. A. & Harris, E. A. Herpes Simplex Virus Type 1 and other pathogens are key causative factors in sporadic Alzheimer’s disease. J. Alzheimers Dis. 48, 319–53 (2015).
Bourgade, K. et al. Protective Effect of Amyloid-β Peptides Against Herpes Simplex Virus-1 Infection in a Neuronal Cell Culture Model. J. Alzheimers Dis. 50, 1227–41 (2016).
Lester, S. N. & Li, K. Toll-like receptors in antiviral innate immunity. J. Mol Biol 6, 1246–64 (2014).
Saresella M. et al. A complex proinflammatory role for peripheral monocytes in Alzheimer’s disease 3, 403–13 (2014).
Levy, D. E. & Garcia-Sastre, A. The virus battles: IFN induction of the antiviral state and mechanisms of viral evasion. Cytokine Growth Factor Rev 12, 143–56 (2001).
Kotenko, S. V. et al. IFN-lambdas mediate antiviral protection through a distinct class II cytokine receptor complex. Nat. Immunol. 4, 69–77 (2003).
Griffin, W. S. et al. Interleukin-1 mediates Alzheimer and Lewy body pathologies. J. Neuroinflammation. 16(3), 58 (2006).
Licastro, F. et al. Variants in antiviral genes are risk factors for cognitive decline and dementia. J Alzheimers Dis 46, 655–63 (2015).
Mancuso, R. et al. Relationship between herpes simplex virus-1-specific antibody titers and cortical brain damage in Alzheimer’s disease and amnestic mild cognitive impairment. Front Aging Neurosci. 6, 285 (2014).
Heneka, M. T. & O’Banion, M. K. Inflammatory processes in Alzheimer’s disease. J. Neuroimmunol. 184, 69–91 (2007).
Saresella, M. et al. The NLRP3 and NLRP1 inflammasomes are activated in Alzheimer’s disease. Mol. Neurodegener. 3(11(1)), 23 (2016).
Shaftel, S. S. et al. Chronic interleukin-1beta expression in mouse brain leads to leukocyte infiltration and neutrophil-independent blood brain barrier permeability without overt neurodegeneration. J Neurosci 27, 9301–9 (2007).
Prokop, S. et al. Impact of peripheral myeloid cells on amyloid-β pathology in Alzheimer’s disease–like mice. J. Exp Med. 212(11), 1811–1818 (2015).
Rezai-Zadeh, K. et al. How to get from here to there: macrophage recruitment in Alzheimer’s disease. Curr. Alzheimer Res. 8, 156–63 (2011).
Bermejo, P. et al. Differences of peripheral inflammatory markers between mild cognitive impairment and Alzheimer’s disease. Immunol Lett 117, 198–202 (2008).
Arosio, B. et al. Interleukin-10 and interleukin-6 gene polymorphisms as risk factors for Alzheimer’s disease. Neurobiol. Aging 25, 1009–15 (2004).
Weaver, J. D. et al. Interleukin-6 and risk of cognitive decline: MacArthur studies of successful aging. Neurology. 59, 371–8 (2002).
Kiecolt-Glaser, J. K. Chronic stress and age-related increases in the proinflammatory cytokine IL-6. Proc Natl Acad Sci USA 100, 9090–5 (2003).
Ali, S. et al. The dual function cytokine IL-33 interacts with the transcription factor NF-kappaB to dampen NF-kappaB-stimulated gene transcription. J Immunol. 187, 1609–1616 (2011).
Choi, Y. S. et al. Nuclear IL-33 is a transcriptional regulator of NF-kappaB p65 and induces endothelial cell activation. Biochem Biophys Res Commun. 421, 305–311 (2012).
Miller, A. M. Role of IL33 in inflammation and disease. J Inflamm. 8(1), 22 (2011).
Chapuis, J. et al. Transcriptomic and genetic studies identify IL-33 as a candidate gene for Alzheimer’s disease. Mol. Psychiatry 14, 1004–16 (2009).
Fu A.K. et al. IL-33 ameliorates Alzheimer's disease like pathology and cognitive decline. Proc. Nat. Acad Sci USA 113, e2705–13 (2016).
Grundman, M. et al. Mild cognitive impairment can be distinguished from Alzheimer disease and normal aging for clinical trials. Arch. Neurol. 61, 59–66 (2004).
Biasin M. et al. TLR activation pathways in HIV-1-exposed seronegative individuals. J. Immunol. 184, 2710–17 (2010).
Biasin M. et al. Apolipoprotein B mRNA-editing enzyme, catalytic polypeptide-like 3G: a possible role in the resistance to HIV of HIV-exposed seronegative individuals. J. Infect. Dis. 195, 960–64 (2007).
Cover K.S. et al. Reproducibility of hippocampal atrophy rates measured with manual, FreeSurfer, AdaBoost, FSL/FIRST and the MAPS-HBSI methods in Alzheimer's disease. Psychiatry Res. 252, 26–35 (2016).
Boccardi M. et al. EADC-ADNI Working Group on The Harmonized Protocol for Manual Hippocampal Segmentation and for the Alzheimer's Disease Neuroimaging Initiative. Training labels for hippocampal segmentation based on the EADC-ADNI harmonized hippocampal protocol. Alzheimers Dement. 11(2), 175–83 (2015).
Faul, F. et al. G Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behavior Research Methods. 39(2), 175–191. (2007).
Acknowledgements
This work was supported by 2015–2016 Ricerca Corrente (Italian Ministry of Health). The authors thank all the partners in FP7 neuGRID (www.neugrid4you.eu) for the support and provision of compunting resources.
Author information
Authors and Affiliations
Contributions
F.L.R., M.S. conceived and designed the research. F.P. and I.M. performed the experiments. F.B. and M.C. performed MRI analysis. E.C. and R.N. are responsible for the clinical cohorts of patients. E.R. performed statistical analysis. F.LR. and M.C. analyzed the data and prepared the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
La Rosa, F., Saresella, M., Baglio, F. et al. Immune and Imaging Correlates of Mild Cognitive Impairment Conversion to Alzheimer’s Disease. Sci Rep 7, 16760 (2017). https://doi.org/10.1038/s41598-017-16754-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-16754-y
This article is cited by
-
27-hydroxycholesterol causes cognitive deficits by disturbing Th17/Treg balance and the related immune responses in mild cognitive impairment patients and C57BL/6J mice
Journal of Neuroinflammation (2023)
-
Phospholipase D3 degrades mitochondrial DNA to regulate nucleotide signaling and APP metabolism
Nature Communications (2023)
-
IL-33 and its decoy sST2 in patients with Alzheimer’s disease and mild cognitive impairment
Journal of Neuroinflammation (2020)
-
The role of interleukin-33 in patients with mild cognitive impairment and Alzheimer’s disease
Alzheimer's Research & Therapy (2020)
-
The small molecule CA140 inhibits the neuroinflammatory response in wild-type mice and a mouse model of AD
Journal of Neuroinflammation (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.