Abstract
It is unknown whether YOD (young onset diabetes) and LOD (late onset diabetes) require similar insulin doses for intensive insulin therapy with a metformin add-on to achieve glycemic control. We analyzed data from our two previously performed randomized, controlled open-label trials. Patients were randomized to receive either continuous subcutaneous insulin infusion (CSII) therapy or CSII combined with metformin therapy for 4 weeks. The studies concentrated on the differences in the insulin doses used for the two groups. We included 36 YOD (age < 40 yrs) and 152 LOD (age > 40 yrs) patients. YOD patients who received metformin combined with CSII therapy required significantly lower insulin doses to maintain euglycemic control compared to patients with LOD. A multivariate analysis, controlled for gender and the fasting blood concentration, was performed to determine the significance of the differences between groups, particularly with respect to the total and basal insulin doses. There was a trend toward improvement in β-cell function and insulin resistance in terms of ΔHOMA-B and ΔHOMA-IR in patients with YOD compared to those with LOD. Newly diagnosed T2D patients with YOD required significantly lower insulin doses, particularly basal insulin doses, to maintain glycemic control compared to the LOD patients.
Similar content being viewed by others
Introduction
Patients with young-onset type 2 diabetes (YOD), defined as those less than 40 years old1,2 at diagnosis, have more difficulty with glycemic and lipid control compared to older onset type 2 diabetes (T2D) patients: YOD patients have higher HbA1c values and LDL cholesterol2. Patients with YOD may thus have a higher risk of complications compared to those with T2D of later onset3 and T1D4. This has been shown to be particularly relevant for ischemic heart disease, neuropathy5, retinopathy2, and cardiovascular-renal events with YOD6. These findings call attention to the necessity of more attention on elucidating and defining the unique characteristics of YOD and more aggressive metabolic control3,7. Although some have attributed the lack of consistent treatment in younger patients8,9 as an important reason for fewer patients with YOD achieving an HbA1c target than patients with late-onset diabetes2, this has not been established at this point.
More than half of the patients with newly diagnosed T2D responded well to Continuous Subcutaneous Insulin Infusion (CSII) therapy in terms of improvements in β-cell function and glycemic control for 1 year after cessation of therapy10. Patients with initial poor glycemic control on multiple daily insulin injections (MDIs) who changed to CSII therapy for 6 months achieved a further reduction in HbA1c levels compared to those who were treated with MDI therapy only11, with their HbA1c levels remaining stable for a further 6 months12. Surprisingly, patients with higher baseline HbA1c levels12,13,14, particularly at levels above 9%15, had better improvement in their HbA1c12. Studies further demonstrated that the mechanisms by which CSII favors glycemic control may partly be the improvement in beta-cell function and insulin resistance16,17,18,19.
Metformin, an insulin-sparing diabetes agent20, has been established as the first-line therapy for T2D. Metformin exhibits glucose-lowering efficacy by enhancing insulin sensitivity in the peripheral tissues, such as the liver and muscle21,22,23,24. Studies confirmed that even subjects with T1D achieved significant improvement in glycemic control and lower insulin requirements when they received a metformin add-on to their CSII therapy20. Metformin combined with CSII therapy was reported to have the ability to shorten the time required to achieve euglycemic control, lower the daily insulin dose, and promote an improvement in β cell function25.
However, the response of patients with young-onset type 2 diabetes (YOD) to CSII therapy with or without metformin remains largely unknown. Our clinical trials [ClinicalTrials.gov, CliCTR-TRC-10001218 Registration date 13th Feb. 2011, and ClinicalTrials.gov, number NCT03226210 Registration date: 19th Jul. 2017] were designed to assess the glycemic variability in T2D patients who were treated with intensive insulin with or without metformin add-on. Our results (ClinicalTrials.gov, number CliCTR-TRC-10001218) showed that CSII therapy only provided a significant improvement in glycemic variation in newly diagnosed or in longstanding T2D patients26. In the present paper, we have analyzed the results according to age, and we report that patients with YOD were more sensitive to a metformin combination with CSII therapy in terms of requiring significantly lower insulin doses to maintain euglycemic control compared to those with a later age of onset.
Results
A total of 188 newly diagnosed type 2 diabetic patients (95 patients received CSII in combination with metformin and 93 patients were treated with CSII therapy only) were recruited for the two studies. The enrolled subjects were divided into two groups according to whether the onset age was earlier or later than 40 years. A total of 36 (24%) patients were defined as YOD (28 M/8 F) and 152 (90 M/62 F) were defined as late onset diabetes (LOD). Patients in the YOD and LOD groups had similar C-peptide, insulin, and blood glucose levels at 0, 30, and 120 min after oral glucose loading (P > 0.05). Patients with YOD had a higher body weight (P < 0.01). There were no significant differences in β-cell function (HOMA-B and insulinogenic index, P > 0.05, respectively) and insulin resistance (HOMA-IR, Matsuda index, P > 0.05, respectively) at baseline between the two groups (Table 1).
In this current study, subjects with YOD achieved euglycemic control in 4.8 ± 2.4 days, which was similar to patients with LOD (5.1 ± 2.3, P > 0.05). We analyzed the insulin doses required by patients to maintain glycemic control after achievement of euglycemia control. Our data showed that the total, basal and bolus insulin doses were similar in the two groups (0.45 ± 0.27 vs. 0.51 ± 0.24, 0.25 ± 0.17 vs. 0.27 ± 0.13, and 0.22 ± 0.14 vs. 0.24 ± 0.16 U/Kg/day, P > 0.05, respectively). Moreover, the CGM data showed that the patients in the two groups had similar mean glucose levels per hour (Fig. 1A) and similar glycemic variations in terms of 24-hrs MBG, SD, CV%, MAGE, the time spent on and the incremental AUC of glucose concentration >10 mmol/L (P > 0.05, respectively) (Table 2).
We also did not observe any differences in total, basal and bolus insulin doses (0.61 ± 0.30 vs. 0.59 ± 0.28, 0.33 ± 0.20 vs. 0.30 ± 0.15, and 0.28 ± 0.16 vs. 0.29 ± 0.20 U/Kg/day, P > 0.05, respectively), mean glucose levels per hour (Fig. 1B) and glycemic variations (Table 2) in YOD and LOD patients who received CSII therapy only.
Anti-diabetic drugs such as metformin combined with insulin can significantly reduce the glucose level in diabetics. As expected, our data showed that patients who received the metformin add-on therapy required significantly lower insulin doses in terms of total, basal and bolus insulin doses (0.32 ± 0.15 vs. 0.61 ± 0.30, 0.18 ± 0.09 vs. 0.33 ± 0.20, and 0.15 ± 0.06 vs. 0.28 ± 0.16 U/Kg/day, P < 0.01, respectively) to maintain similar glycemic control compared to those who received insulin therapy alone.
Notably, patients with YOD treated with metformin combination therapy required significantly lower total insulin doses (0.32 ± 0.15 vs. 0.43 ± 0.15 U/Kg/day, P < 0.05) compared to those with LOD to maintain glycemic control in terms of mean glucose levels per hour (Fig. 1C) and 24-hrs MBG, MAGE, the time spend on and the incremental AUC of glucose concentrations above 10 mmol/L (P > 0.05, respectively) (Table 2). Most importantly, YOD patients who were administered metformin combined with CSII showed significant improvements in glycemic variations in terms of SD and CV compared to those of LOD patients (Table 2). The total daily insulin doses were given in two modes: a bolus dose before each meal and a basal dose throughout 24 h. No differences were observed in the bolus doses administered to the two groups (0.15 ± 0.06 vs. 0.19 ± 0.07 U/Kg/day, P > 0.05). However, patients with LOD required significantly lower basal insulin doses to maintain euglycemic control compared to the patients with LOD (0.18 ± 0.09 vs. 0.24 ± 0.09 U/Kg/day, P < 0.05, respectively). In the logistic analysis, only gender and fasting blood glucose concentrations were significantly correlated with insulin doses. A multivariate analysis, controlled for gender and fasting blood concentration, was performed to determine the significance of the differences between groups, particularly with respect to the total and basal insulin doses. Our data showed that patients with YOD required significantly lower total and basal insulin doses compared to those with LOD. To identify the characteristics associated with the decreased insulin doses required by patients with YOD, we compared the baseline data of the two groups. A total of 95 patients (19 with YOD and 76 with LOD) received the metformin add-on therapy. The YOD and LOD patients had similar C-peptide, insulin, and blood glucose levels at 0 and 120 min after oral glucose loading (P > 0.05, respectively), but were dissimilar for age and body weight (P < 0.01, respectively) (Table 1).
We further compared β-cell function and insulin resistance between the groups. Our data showed that there were no significant differences in terms of HOMA-B, insulinogenic index, HOMA-IR, and Matsuda index at baseline (Table 1). After therapy, the YOD and LOD patients still had similar C-peptide, insulin, and blood glucose levels at 0 and 120 min after oral glucose loading, and similar HOMA-B, insulinogenic index, HOMA-IR, and Matsuda index values (P > 0.05, respectively).
We next analyzed changes of β-cell function and insulin resistance before and after therapy. The data indicated a tendency toward improvement in β-cell function and insulin resistance in terms of ΔHOMA-B [23.3 (0.6, 50.4) vs. 14.3 (6.6, 26.7)] and ΔHOMA-IR [−2.9 (−4.1, −0.3) vs. −1.7 (−2.6, −0.3)] in patients with YOD treated with the metformin combination therapy compared to those with LOD, but this tendency was not statistically significant. The improvement in β-cell function and decreased insulin resistance, although not statistically significant, might be attributed to the possibility that patients with YOD might be sensitive to metformin when insulin doses are lowered to maintain glycemic control.
Discussion
The data of this current study indicated that newly diagnosed T2D patients with YOD had a significant increase in metformin sensitivity, which manifested itself when lowering insulin doses to maintain glycemic control compared to those with a later age of onset of diabetes. We also observed some improvements in β-cell function and ameliorated insulin resistance in terms of ΔHOMA-B and ΔHOMA-IR in patients with YOD compared to those with LOD. The observed improvement in β-cell function and insulin resistance might be the reason that patients with YOD might be sensitive to metformin when it is added to maintain glycemic control.
We consecutively recruited 188 subjects from February 2010 to June 2016. A total of 36 patients were diagnosed before 40 years of age, corresponding to a YOD incidence of (24%), which was consistent with findings from a previous study, with an enrolment of 41029 patients and one in five adult T2D patients with YOD2. Previous studies have also focused on the glycemic and lipid metabolism in T2D patients with onset earlier than 257 and ≤45 years of age27. Those results showed that patients with YOD onset had the prominent problem of poor glycemic and lipid control and a higher prevalence of diabetic complications5,6,7,27. Various characteristics of T2D patients with YOD were reported to be associated with poor glycemic control, including younger age2,28, longer disease duration28, and genetic, socioeconomic, or psychological-behavioral factors2. Additional observations also indicated the importance of poor self-management resulting from chronic stress and negative life events29. Smoking and alcohol intake may also contribute to the poor glycemic and lipid control in patients with YOD2. Compared to T2D patients diagnosed at a later age, fewer YOD patients achieved HbA1c levels of <7%2. It is significant to note that T2D patients with an HbA1c level above 6.5% had a higher death rate than those with an HbA1c concentration below 5.7%30. This gives validity to the notion that optimal treatment aimed at improving glycemic control in this high-risk group of diabetic patients is of paramount importance.
Drug-naïve patients with T2D responded well to Continuous Subcutaneous Insulin Infusion (CSII) therapy in terms of improvement in β-cell function and glycemic control. Treatment has shown that half of those patients could maintain euglycemic control for 1 year without any additional glucose-lowering agents10. Patients with poor glycemic control and HbA1c concentrations above 8% after pre-randomization with multiple daily insulin injections (MDIs) can achieve a significant reduction in HbA1c levels11, and their HbA1c levels can remain stable for 12 months with CSII therapy12. A stratified analysis comparing the baseline characteristics revealed that patients with an HbA1c level above 9% were proven to have favorable outcomes associated with the decrease in HbA1c15. In this study, patients in the two groups had HbA1c levels above 10% and similar diabetes duration, β-cell function, and insulin resistance; however, they differed in age and body mass index (BMI). Some patients with different ages, diabetes durations, complications, BMI, insulin resistance31, and different β-cell function or C-peptide levels32 benefit from reductions in their HbA1c levels. Thus, they should respond similarly to the CSII combination with metformin therapy.
Our data showed that T2D patients with YOD required significantly lower insulin doses, particularly basal insulin doses, to maintain glycemic control compared to those with a later onset after 40 years of age in the metformin and CSII therapy group. However, we did not identify any differences in insulin doses in patients with only CSII therapy in the two groups. Those results indicated that T2D patients with YOD were likely to benefit the most from metformin, in view of its demonstrated benefits as a glucose-lowering agent to enhance insulin sensitivity21,22,23,24. Metformin has already been recommended as the first-line glucose-lowering agent in the management of T2D in most guidelines. In combination with insulin in the treatment of T2D, the use of metformin leads to an increase in insulin sensitivity and the reduction of daily insulin doses21,22,23. However, we did not see statistically significant differences in insulin resistance, such as HOMA-IR, Matsuda Index, and Insulinogenic Index at baseline and after therapy between young and older patients who received metformin in addition to CSII therapy. There was some variation in the changes in improvements in β-cell function and insulin resistance in terms of ΔHOMA-B and ΔHOMA-IR from baseline to endpoint in patients with YOD compared to those with LOD. A limitation should be noted: in this study, we did not adequately explain the significantly lower insulin doses that the younger patients with T2D required to maintenance euglycemic control compared to those of the older patients. In our study population, there were significantly more male than female YOD patients. Although sex hormones can affect glucose metabolism and insulin sensitivity, in the LOD patients, there was no difference between male and female patients. Our study did not have sufficient power to distinguish between the YOD male and female patients adequately. Future investigation of the reasons behind treatment by age is necessary to address this important difference.
Patients with high glycemic variations may not have favorable outcomes with CSII therapy31 in terms of improvements in glycemic control, and they may require a CSII in combination with another glucose-lowering agent therapy33. In this study, we did not observe the efficacy of metformin combined with CSII therapy, which resulted in changes of HbA1c concentrations. HbA1c is an important glycemic control index in large-scale clinical trials34,35,36, and the association between the reduction in HbA1c levels and the reduction in the risks of diabetic complications has been well established37. We previously observed that patients with higher HbA1c levels may have a larger MAGE compared to those with a lower HbA1c level38. However, patients with similar HbA1c values do not exhibit the same glycemic variations39,40,41. Our CGM data showed that patients who received metformin add-on insulin therapy had significantly improved glycemic variations in terms of MAGE, SD, CV%, and time spent on and the incremental AUC of glucose concentrations ≥10 mmol/L, which might be significant in avoiding long-term diabetic complications. The drastic blood glucose concentrations may lead to an over-production of peroxynitrite and nitrotyrosine42,43,44, which may be an indicator of diabetic vascular complications45.
In conclusion, our data revealed that newly diagnosed T2D patients with YOD required significantly lower insulin doses, particularly basal insulin doses, to maintain glycemic control compared to LOD patients. Our data indicated that patients with YOD responded well to metformin combined with CSII treatment in terms of lowering the insulin doses necessary to improve β-cell function and alleviate insulin sensitivity.
Materials and Methods
The two studies were both randomized, controlled open-label trials. Study protocols and patient consent forms were approved by the Institutional Ethical Committee of Nanjing First Hospital and the institutional Ethical Committees of the other centers. All patients gave written informed consent to participate. The methods were performed in accordance with the Declaration of Helsinki guidelines, including any relevant details.
This study (CliCTR-TRC-10001218) was a multiple-center, randomized, parallel-group trial, which including a 4–6 day run-in period of diet alone and a 2–3-week randomized phase as previously described26. In the initial testing, T2D patients aged 18–80 years who had an HbA1c value ranging from 9.0% to 12.0% were enrolled from eight centers in China between February 2010 and December 2014. All patients who were admitted as inpatients received intensive insulin therapy without any oral glucose-lowering agent. The other study (NCT03226210) was as a single-center, randomized, controlled open-label study conducted between April 2012 and June 2016. Newly diagnosed T2D cases aged between >18 and <80 years and with HbA1c values >9.0% at diagnosis were recruited. Patients were excluded from the analysis if they had serum creatinine levels ≥1.5 mg/dL (males), ≥1.4 mg/dL (females) or abnormal creatinine clearance, known as hypersensitivity to metformin or insulin. Patients with infection or acute metabolic diabetic complications such as ketoacidosis or hyperosmolar state (coma) and patients who used systemic glucocorticoids in the last 3 months were excluded. If the patients were unable to tolerate the minimum metformin dose (1000 mg/day), they were also excluded from this study. The trial included a screening period to collect baseline parameter values, a 2 ± week treatment period, and a 4-day CGM period. After screening, the enrolled subjects then received metformin add-on CSII therapy. Metformin (Bristol-Myers Squibb, USA) was administered at a dose of 500 mg thrice-daily. The total daily insulin (Aspart, Novo Nordisk, Bagsværd, Denmark) doses were 0.4 IU/kg, which was given employing a two-injection mode: 1/2 of the total daily dose was equally given as boluses before each meal, and the remaining insulin was given as a basal dose.
The two trials were conducted using the same protocol. After completing the baseline assessment and the 3-day CGM46, all patients were subjected to oral glucose tolerance tests (OGTTs). Serum glucose, insulin, and C-peptide concentrations at 0 and 120 min after glucose loading and HbA1c values were measured at the Department of Endocrinology, Nanjing First Hospital, Nanjing Medical University, China. All patients were subjected to retrospective CGM for 3 days (Sof-sensor, CGMS-Gold, Medtronic Incorporated, Northridge, USA) in the hospital by a specialist nurse at baseline and at endpoint26. Insulin doses were subsequently administered by the treating physician according to the blood glucose values obtained by self-monitoring. When euglycemic control was achieved, defined as 80% of fasting blood glucose and 2 h postprandial after each meal was less than 6.1 and 8.0 mmol/L, respectively10, the total daily, basal, and bolus insulin doses were recorded. The glycemic variation parameters, such as the 24 h mean amplitude of glycemic excursions (MAGE), the 24 h mean blood glucose (MBG), the standard deviation (SD) of the MBG, the percentage time duration (%) and the incremental area under curve (AUC) of glucose levels >10.0 mmol/L and <3.9 mmol/L, were calculated and recorded. β-cell function was assessed by the homoeostasis model assessment B (HOMA-B), insulin sensitivity was indicated by HOMA-IR10,47 and the Matsuda index was calculated as previously described48,49.
In this paper, we divided all newly diagnosed T2D cases receiving intensive insulin therapy, with or without metformin, into two groups based on those aged younger than 40 or above 40 years old. The primary endpoint was the between-group differences in insulin doses. The secondary endpoints were the MBG, SD, CV, MAGE, 24-h MBG, and the time spent on and the incremental AUC of hyperglycemia (defined as sensor glucose values >10 mmol/L).
Statistical analysis
The analyses were performed using the SPSS 16.0 (SPSS, Science, Chicago, USA) statistical package. All variables were tested for normal distribution of the data. Data are presented as the means ± SD or as the median (IQR). A binary logistic regression and Pearson analysis (Spearman’s analysis in non-parametric variables) were performed to identify the parameters likely correlated with the change of values in terms of the insulin doses. The efficacy of CSII was analyzed by the paired t-test or Wilcoxon test, whereas differences between the groups were examined using the student’s unpaired t-test or the Mann-Whitney U test. A two-way ANOVA for repeated measurements was used in the comparison of groups. Bonferroni’s correction was followed. All comparisons were 2-sided at the 5% significance level. A P value <0.05 was considered statistically significant.
References
Song, S. H. & Gray, T. A. Early intensive cardiovascular risk management in young people with type 2 diabetes. Diabetes research and clinical practice 92, e70–72, https://doi.org/10.1016/j.diabres.2011.02.027 (2011).
Yeung, R. O. et al. Metabolic profiles and treatment gaps in young-onset type 2 diabetes in Asia (the JADE programme): a cross-sectional study of a prospective cohort. Lancet Diabetes Endocrinol 2, 935–943, https://doi.org/10.1016/S2213-8587(14)70137-8 (2014).
Al-Saeed, A. H. et al. An Inverse Relationship Between Age of Type 2 Diabetes Onset and Complication Risk and Mortality: The Impact of Youth-Onset Type 2 Diabetes. Diabetes care 39, 823–829, https://doi.org/10.2337/dc15-0991 (2016).
Amutha, A. et al. Incidence of complications in young-onset diabetes: Comparing type 2 with type 1 (the young diab study). Diabetes research and clinical practice 123, 1–8, https://doi.org/10.1016/j.diabres.2016.11.006 (2017).
Song, S. H. Complication characteristics between young-onset type 2 versus type 1 diabetes in a UK population. BMJ Open Diabetes Res Care 3, e000044, https://doi.org/10.1136/bmjdrc-2014-000044 (2015).
Luk, A. O. et al. Prospective study on the incidences of cardiovascular-renal complications in Chinese patients with young-onset type 1 and type 2 diabetes. Diabetes care 37, 149–157, https://doi.org/10.2337/dc13-1336 (2014).
Unnikrishnan, R. et al. Younger-onset versus older-onset type 2 diabetes: Clinical profile and complications. Journal of diabetes and its complications 31, 971–975, https://doi.org/10.1016/j.jdiacomp.2017.03.007 (2017).
Wong, M. C. et al. Adherence to oral hypoglycemic agents in 26,782 Chinese patients: a cohort study. J Clin Pharmacol 51, 1474–1482, https://doi.org/10.1177/0091270010382911 (2011).
Gregg, E. W. et al. Characteristics of insured patients with persistent gaps in diabetes care services: the Translating Research into Action for Diabetes (TRIAD) study. Med Care 48, 31–37, https://doi.org/10.1097/MLR.0b013e3181bd4783 (2010).
Weng, J. et al. Effect of intensive insulin therapy on beta-cell function and glycaemic control in patients with newly diagnosed type 2 diabetes: a multicentre randomised parallel-group trial. Lancet 371, 1753–1760, https://doi.org/10.1016/S0140-6736(08)60762-X (2008).
Reznik, Y. et al. Insulin pump treatment compared with multiple daily injections for treatment of type 2 diabetes (OpT2mise): a randomised open-label controlled trial. Lancet 384, 1265–1272, https://doi.org/10.1016/S0140-6736(14)61037-0 (2014).
Aronson, R. et al. Sustained efficacy of insulin pump therapy compared with multiple daily injections in type 2 diabetes: 12-month data from the OpT2mise randomized trial. Diabetes, obesity & metabolism 18, 500–507, https://doi.org/10.1111/dom.12642 (2016).
Cantrell, R. A. et al. A review of treatment response in type 2 diabetes: assessing the role of patient heterogeneity. Diabetes, obesity & metabolism 12, 845–857, https://doi.org/10.1111/j.1463-1326.2010.01248.x (2010).
Bloomgarden, Z. T., Dodis, R., Viscoli, C. M., Holmboe, E. S. & Inzucchi, S. E. Lower baseline glycemia reduces apparent oral agent glucose-lowering efficacy: a meta-regression analysis. Diabetes care 29, 2137–2139, https://doi.org/10.2337/dc06-1120 (2006).
Schutz-Fuhrmann, I. et al. Factors affecting the benefit of insulin dose intensification in people with Type 2 diabetes: an analysis from the OpT2mise randomized trial. Diabetic medicine: a journal of the British Diabetic Association 34, 291–292, https://doi.org/10.1111/dme.13279 (2017).
Retnakaran, R. & Drucker, D. J. Intensive insulin therapy in newly diagnosed type 2 diabetes. Lancet 371, 1725–1726, https://doi.org/10.1016/S0140-6736(08)60736-9 (2008).
Ilkova, H., Glaser, B., Tunckale, A., Bagriacik, N. & Cerasi, E. Induction of long-term glycemic control in newly diagnosed type 2 diabetic patients by transient intensive insulin treatment. Diabetes care 20, 1353–1356 (1997).
Li, Y. et al. Induction of long-term glycemic control in newly diagnosed type 2 diabetic patients is associated with improvement of beta-cell function. Diabetes care 27, 2597–2602 (2004).
Ryan, E. A., Imes, S. & Wallace, C. Short-term intensive insulin therapy in newly diagnosed type 2 diabetes. Diabetes care 27, 1028–1032 (2004).
Meyer, L. et al. The benefits of metformin therapy during continuous subcutaneous insulin infusion treatment of type 1 diabetic patients. Diabetes care 25, 2153–2158 (2002).
Giugliano, D. et al. Metformin for obese, insulin-treated diabetic patients: improvement in glycaemic control and reduction of metabolic risk factors. Eur J Clin Pharmacol 44, 107–112 (1993).
Robinson, A. C., Burke, J., Robinson, S., Johnston, D. G. & Elkeles, R. S. The effects of metformin on glycemic control and serum lipids in insulin-treated NIDDM patients with suboptimal metabolic control. Diabetes care 21, 701–705 (1998).
Yu, J. G., Kruszynska, Y. T., Mulford, M. I. & Olefsky, J. M. A comparison of troglitazone and metformin on insulin requirements in euglycemic intensively insulin-treated type 2 diabetic patients. Diabetes 48, 2414–2421 (1999).
Inzucchi, S. E. et al. Efficacy and metabolic effects of metformin and troglitazone in type II diabetes mellitus. The New England journal of medicine 338, 867–872, https://doi.org/10.1056/NEJM199803263381303 (1998).
Huang, Z. et al. Short-term continuous subcutaneous insulin infusion combined with insulin sensitizers rosiglitazone, metformin, or antioxidant alpha-lipoic acid in patients with newly diagnosed type 2 diabetes mellitus. Diabetes technology & therapeutics 15, 859–869, https://doi.org/10.1089/dia.2013.0013 (2013).
Li, F. F. et al. Blood Glucose Fluctuations in Type 2 Diabetes Patients Treated with Multiple Daily Injections. Journal of diabetes research 2016, 1028945, https://doi.org/10.1155/2016/1028945 (2016).
Deconinck, B., Mathieu, C. & Benhalima, K. Characteristics and cardiovascular complications of a large cohort of adults diagnosed with type 2 diabetes <45 years. Diabetology & metabolic syndrome 9, 28, https://doi.org/10.1186/s13098-017-0227-z (2017).
Chan, J. C. et al. Multifaceted determinants for achieving glycemic control: the International Diabetes Management Practice Study (IDMPS). Diabetes care 32, 227–233, https://doi.org/10.2337/dc08-0435 (2009).
Hessler, D. M., Fisher, L., Mullan, J. T., Glasgow, R. E. & Masharani, U. Patient age: a neglected factor when considering disease management in adults with type 2 diabetes. Patient Educ Couns 85, 154–159, https://doi.org/10.1016/j.pec.2010.10.030 (2011).
Saydah, S., Bullard, K. M., Imperatore, G., Geiss, L. & Gregg, E. W. Cardiometabolic risk factors among US adolescents and young adults and risk of early mortality. Pediatrics 131, e679–686, https://doi.org/10.1542/peds.2012-2583 (2013).
Metzger, M. et al. Factors associated with improved glycemic control following continuous subcutaneous insulin infusion therapy in patients with type 2 diabetes uncontrolled with bolus-basal insulin regimens: an analysis from the OpT2mise randomized trial. Diabetes, obesity & metabolism, https://doi.org/10.1111/dom.12960 (2017).
Reznik, Y. & Huang, S. Reductions in A1C with pump therapy in type 2 diabetes are independent of C-peptide and anti-glutamic acid decarboxylase antibody concentrations. Diabetes technology & therapeutics 16, 816–818, https://doi.org/10.1089/dia.2014.0261 (2014).
Tricco, A. C. et al. Safety and effectiveness of dipeptidyl peptidase-4 inhibitors versus intermediate-acting insulin or placebo for patients with type 2 diabetes failing two oral antihyperglycaemic agents: a systematic review and network meta-analysis. BMJ Open 4, e005752, https://doi.org/10.1136/bmjopen-2014-005752 (2014).
Retinopathy and nephropathy in patients with type 1 diabetes four years after a trial of intensive therapy. The Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications Research Group. The New England journal of medicine 342, 381–389, https://doi.org/10.1056/NEJM200002103420603 (2000).
Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). UK Prospective Diabetes Study (UKPDS) Group. Lancet 352, 837–853 (1998).
The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. The Diabetes Control and Complications Trial Research Group. The New England journal of medicine 329, 977–986, https://doi.org/10.1056/NEJM199309303291401 (1993).
Stratton, I. M. et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ 321, 405–412 (2000).
Li, F. F. et al. Features of glycemic variations in drug naive type 2 diabetic patients with different HbA1c values. Scientific reports 7, 1583, https://doi.org/10.1038/s41598-017-01719-y (2017).
Del Prato, S. In search of normoglycaemia in diabetes: controlling postprandial glucose. Int J Obes Relat Metab Disord 26(Suppl 3), S9–17, https://doi.org/10.1038/sj.ijo.0802172 (2002).
Nathan, D. M. et al. Translating the A1C assay into estimated average glucose values. Diabetes care 31, 1473–1478, https://doi.org/10.2337/dc08-0545 (2008).
Zhou, J. et al. Relationship between HbA1c and continuous glucose monitoring in Chinese population: a multicenter study. PloS one 8, e83827, https://doi.org/10.1371/journal.pone.0083827 (2013).
Ceriello, A. et al. Oscillating glucose is more deleterious to endothelial function and oxidative stress than mean glucose in normal and type 2 diabetic patients. Diabetes 57, 1349–1354, https://doi.org/10.2337/db08-0063 (2008).
Monnier, L. et al. Activation of oxidative stress by acute glucose fluctuations compared with sustained chronic hyperglycemia in patients with type 2 diabetes. Jama 295, 1681–1687, https://doi.org/10.1001/jama.295.14.1681 (2006).
Hu, Y., Liu, W., Huang, R. & Zhang, X. Postchallenge plasma glucose excursions, carotid intima-media thickness, and risk factors for atherosclerosis in Chinese population with type 2 diabetes. Atherosclerosis 210, 302–306, https://doi.org/10.1016/j.atherosclerosis.2009.11.015 (2010).
Nalysnyk, L., Hernandez-Medina, M. & Krishnarajah, G. Glycaemic variability and complications in patients with diabetes mellitus: evidence from a systematic review of the literature. Diabetes, obesity & metabolism 12, 288–298, https://doi.org/10.1111/j.1463-1326.2009.01160.x (2010).
Zhou, J. et al. Reference values for continuous glucose monitoring in Chinese subjects. Diabetes care 32, 1188–1193, https://doi.org/10.2337/dc09-0076 (2009).
Matthews, D. R. et al. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28, 412–419 (1985).
Matsuda, M. & DeFronzo, R. A. Insulin sensitivity indices obtained from oral glucose tolerance testing: comparison with the euglycemic insulin clamp. Diabetes care 22, 1462–1470 (1999).
Sasaki, R. et al. Association of Waist Circumference and Body Fat Weight with Insulin Resistance in Male Subjects with Normal Body Mass Index and Normal Glucose Tolerance. Intern Med 55, 1425–1432, https://doi.org/10.2169/internalmedicine.55.4100 (2016).
Acknowledgements
This research was funded by the Science and Technology Support Program of Jiangsu Province (CN) (No. BL2014010), the National Natural Science Foundation of China (No. 81500606), the Jiangsu provincial scientific project (SBK2015042970) and the Project funded by the China Postdoctoral Science Foundation (2015M581829).
Author information
Authors and Affiliations
Contributions
J.H.M. and L.Y. contributed to the conception and design of the study. F.F.L., B.L.L., G.P.Y., D.F.Z., M.Y.C., and X.F.Z. contributed to conducting the study and data collection. B.L.L., X.F. S., M.Y.C., and J.D.W. contributed to the data analysis. F.F.L. contributed to writing the manuscript and the final approval of the manuscript. We appreciated Prof. Frank Elliott who contributed to the final proof-reading of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Li, Ff., Liu, Bl., Yin, Gp. et al. Young onset type 2 diabetic patients might be more sensitive to metformin compared to late onset type 2 diabetic patients. Sci Rep 7, 16382 (2017). https://doi.org/10.1038/s41598-017-16658-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-16658-x
This article is cited by
-
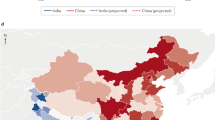
Pathophysiology, phenotypes and management of type 2 diabetes mellitus in Indian and Chinese populations
Nature Reviews Endocrinology (2022)
-
A View Beyond HbA1c: Role of Continuous Glucose Monitoring
Diabetes Therapy (2019)
-
Metformin add-on continuous subcutaneous insulin infusion on precise insulin doses in patients with type 2 diabetes
Scientific Reports (2018)
-
Male Patients with Longstanding Type 2 Diabetes Have a Higher Incidence of Hypoglycemia Compared with Female Patients
Diabetes Therapy (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.