Abstract
This study used insurance claims data to evaluate obstetric outcomes in pregnant women with and without depression because population study for Asian women on the issue is limited. We identified 5,064 women with depression at pregnancy in 2005–2013, and 20,024 pregnant women without depression, frequency matched by age, pregnant year and parity. Obstetric events during pregnancy and deliveries were evaluated. The depression group had more events than comparisons for hyperemesis (39.3 vs. 35.5%), abortion (3.3 vs. 2.6%), malpresentation (12.3 vs. 10.3%), C-section (40.2 vs. 34.6%) and intrauterine fetal demise (0.7 vs. 0.4%); risks of these events were significant for childbearing depressed women, not for the 35+ years subgroup. These incidences were higher in depressed women taking antidepressant than those without the medication, but were significant in childbearing depressed subgroup for hyperemesis and C-section with odds ratios of 1.18 (95% confidence intervals (CI), 1.02–1.36) and 1.29 (95% CI, 1.11–1.49), respectively. Incident preterm and low birth weight births were also higher in the depression group than in comparisons, but weren’t significant. In conclusion, women with depression during pregnancy may develop more adverse events than comparisons and are more likely to have a C-section delivery.
Similar content being viewed by others
Introduction
The prevalence of depression has increased in recent years, up to approximately 20% of pregnant women reported having depressive disorders1,2,3. Depressive disorders during pregnancy have been associated with negative pregnant outcomes, such as preeclampsia, preterm delivery, premature rupture of membranes, and low infant birth weight. These events lead to neonatal and maternal morbidity and higher healthcare costs4,5,6,7,8,9. There are more studies on neonatal outcomes than studies on other obstetric outcomes associated with maternal depression during pregnancy10,11,12,13,14,15.
Studies on whether depression during pregnancy is associated with increased adverse events on the mother and fetus remain inconclusive. Approximately 15% of women are classified as depressed in a cohort study of 228,876 singleton pregnancies in the Tennessee Medicaid population2. The risk of preterm birth and infant convulsions are more common in depressed women who have received medications12. A study in Sweden found that planned Cesarean deliveries are more common in women with depression and/or anxiety during pregnancy5. A study conducted in Taiwan found that women with depression are less likely to have prenatal care but incur higher expenses for other types of healthcare16. Another follow-up study based on a small sample of depressed pregnant women failed to observe significant unfavorable obstetric outcomes17. Women may discontinue antidepressant use prior to conception or during the first trimester of pregnancy to ensure safe fetal development18. The study of the California County Mental Health System reported that the risk of obstetric complications is lower for depressed women treated in the system than those treated in other settings, with adjusted odds ratios (aORs) of 1.32 and 1.72, respectively, compared with general women15. The study of the California County Mental Health System reported that mental illness was associated with elevated risk of obstetric complications; however, the analysis included several types of mental illnesses, and data on depression was not reported separately.
Findings on adverse events for pregnant women with depression are inconsistent. The inconsistency can be related to the limited sample size of studies or the quality of data19,20. A recent systemic study analyzed 23 studies covering 25 663 women with untreated antenatal depression reported that these women were more likely to have low birth weight infant and preterm birth21. Among these 23 studies, a Korean study failed to find an association between pregnant depression and low birth weight22. Information from a population-based study with larger samples for Asian women is limited. A recent study conducted in China reported that prenatal depression combined with anxiety is at a higher risk of having a low birth weight baby23. Because of the scarcity of research for Asian population, it remains both opportunity and challenges. In the present study, we used large insurance claims data to investigate whether pregnant women with depression is associated with adverse obstetric outcomes and neonatal outcomes during pregnancy and delivery. The obstetric outcomes were compared between two groups; one group consisted of women with depression and the other group had no such disorder before and during pregnancy. We further assessed whether the association between depression and obstetric complications differs by maternal age at birth and antidepressant medication.
Results
Baseline characteristics of study cohorts
Table 1 shows that most women in this study were mainly low-income population in the age of 25–34, living in the northern Taiwan and pregnant for the first time. Women in the depression group were more prevalent with comorbidities than were the non-depression group. Approximately one fifth depressed women were prescribed for antidepressant less than 6 months and only 0.3% depression women were on the medications for longer than 6 months.
Incidence of obstetric and delivery events
Incident maternal obstetric complications were more likely to occur in the depression group than in the comparison group (Table 2). Significant differences were observed in the multivariable logistic regression analysis. The depressed women were at a greater risk for hyperemesis (adjusted OR = 1.16, 95% CI = 1.08–1.25), abortion (adjusted OR = 1.33, 95% CI = 1.10–1.61), malpresentation (adjusted OR = 1.20, 95% CI = 1.08–1.33), and intrauterine fetal demise (adjusted OR = 1.69, 95% CI = 1.12–2.56). The occurrence of Cesarean sections was 6% higher in the depression group than in the comparison group (40.2% vs. 34.6%, adjusted OR = 1.25, 95% CI = 1.16–1.34). Therefore, women with depression had a lower rate of normal spontaneous delivery (59.2% vs. 65.1%; adjusted OR = 0.80, 95% CI = 0.74–0.85). Compared to the non-depression group, the depression group had higher rates of preterm delivery (6.4 vs. 5.4%) and low birth weight births (2.6 vs. 2.4%), but differences were not significant.
Table 3 shows the adverse obstetric events were significant mainly for younger depressed groups. The interaction between age and depression was significant only for Cesarean section use (p = 0.03).
Obstetric events associated with antidepressant use
In the depression group, the use of antidepressant medication was associated with slightly increased events of hyperemesis, chorioamnionitis, preterm birth and Cesarean section use, compared non-users, with an adjusted OR of 2.23 (95% CI = 1.19–4.17) for chorioamnionitis (Table 4). Age-specific analysis shows that the medication relationship was significant in 25–34 years old group for only hyperemesis and Cesarean section use (Table 5). Interaction between age and medication was significant only for Cesarean section (p = 0.04).
Discussion
In the present study, we observed that the baseline comorbidities were more prevalent in the depression group than in the non-depressed group, and the vast majority of depressed women were untreated during pregnancy. This study demonstrates increased events of hyperemesis, abortion, malpresentation, Cesarean Section, and intrauterine fetal death in women with depression during pregnancy. Depressed women aged 25 to 34 had the higher risk of hyperemesis, abortion, malpresentation, Cesarean Section in the age stratified analysis. When examining antidepressant medication, we found depressed women with antidepressant medication did not increase much risk at complications. Hyperemesis and Cesarean Section remained the risk in the childbearing age depressed women with antidepressant medication.
Although this study presented some research feature is differing characteristics among the study groups, as well as other studies, the mechanism of depression associated with adverse obstetric outcomes in pregnant women remains unclear. Women with depression display abnormalities in hypothalamic-pituitary-adrenal axis activity and exhibit high baseline cortisol levels and promoted response to the arginine vasopressin and corticotropin-releasing hormone24.
Our data revealed that depressed pregnant women had a higher risk of hyperemesis gravidarum, the risk remained in the childbearing age women with antidepressant medication. However, the risk of hyperemesis gravidarum among childbearing age women was similar in those with antidepressants treatment and those without antidepressants treatment. The reported incidence of hyperemesis gravidarum is relatively rare, varies across ethnic groups, and is dependent on diagnostic criteria25. In our study, it is more common because of the diagnostic criteria also included excessive vomiting during pregnancy. A meta-analysis of 59 studies estimated that near 70% of pregnant women experience nausea and/or vomiting and 1.1% with hyperemesis gravidarum26. Hyperemesis gravidarum is a primary reason for sick leave and hospitalization during pregnancy27,28. Nausea and vomiting of pregnancy (NVP) cause a substantial negative effect on the quality of life for women29,30. Wood et al. indicated that the effects of NVP are amplified with increased severity of NVP symptoms30. Finding in this study echo previous studies investigating the association between depression and hyperemesis25,31,32. Bearing in mind that both depression and hyperemesis gravidarum leads to uncomfortable experience among pregnant women. Considerable support should be considered and provided.
Our study also found an increased odds ratio of abortion among the depressed women. The abortion risk may be explained by the decreased levels of Nerve Growth Factor (NGF). Recent studies found that NGF levels are significantly lower among depressed women33 and lower NGF level is associated with abortion34. NGF is involved in pregnancy maintenance35, with an aberrant distribution in placental tissue relevant to pregnancy failure36. There have been several studies focused on the association between antidepressant and abortion, yet the study findings are controversial. Most of studies indicated that antidepressants associated with increased risk of abortion37,38,39. A recent review found that there was no statistically significant impact of antidepressant exposure on rates of spontaneous abortion14. Similarly, our study observed no significantly increased risk among depressed women without antidepressant. These controversial finding may reflect residual confounding by depression severity and adverse lifestyle38,40,41.
The present study also found that depressed women had a higher odds ratio of malpresentation, particularly in those aged 25 to 34. Malpresentation is an important cause of dystocia leading to a risky delivery, and especially for primiparous women42. Research on malpresentation is scarce, the etiology is still unclear. Known possible risks include a large baby, polyhydramnios, multiple pregnancy, low-lying placenta, preterm labor, and anomalies of the fetus, uterus or pelvis43. When malpresentations occur, primiparous women are at a greater risk for operative delivery than are multiparous women42. However, we cannot find out the cause of malpresentation among depressed women in our study, it remains unanswered for the future study.
Consistent with previous studies, pregnant women with depression in our study were at a higher risk of Cesarean delivery5,6,17,44,45,46,47. The significant risk still remained in the childbearing age depressed women with antidepressant medication in the age stratified analysis. The operation is performed generally for reducing the pain threshold, increasing pain perception, impairing uterine contractility and psychological distress44. While experiencing pain, pregnant women with depression had difficulty to function and cooperate properly during labor. Obstetricians may intentionally or unintentionally prefer other operative deliveries due to symptoms of depression44. In addition, women might feel anxiety and fear of childbirth and request Cesarean delivery5.
In this study, around 80% of depression women are unmedicated during the pregnancy, one fifth depressed women took antidepressants for a short period. This observation is consistent with a large cohort study which shows that most women discontinued antidepressants before the second trimester of pregnancy12. Patients who discontinue medications may experience more serious depression symptoms before conception or recurrent depression during pregnancy48,49. The potential risk to the infant of antidepressant use during pregnancy is controversial14. In our study, the risk of medicated group resembled with un-medicated group. A careful treatment plan is essential for women under antidepressant treatment who plan to conceive or become pregnant.
The present study is strengthened by using a large population data, allowing a high statistical power to capture multiple pregnant outcomes to be compared between depressed women and non-depressed women. We were also capable to stratify data to observe the variation of outcomes by age and antidepressant. This circumstance allowed us not only to investigate the role of depression itself, but also consider the effect of antidepressant medication. In addition, our study focused on pregnancy related outcomes within the pregnancy pathway, rather than delivery or neonatal outcomes. It provided complete information for depressed women and health care professionals to weigh benefits and risks.
This study also has some limitations. Demographic data such as education level, lifestyle history, and marital status, are not available in the data analysis. However, the study sample is unlikely to be affected by these potential confounders because Chinese pregnant women not only avoid unhealthy behaviors but also withdraw the treatment that might harm the fetus. Although our study did not provide the education level of the study sample, levels of income is associated with education. Our data was unable to show a significant difference in income between our study groups and the potential effect is reduced. The second limitation is that information on mental disorders before 1996 was not available, but we were able to ascertain caseness and outcomes based on medical contacts during the follow-up window. However, such measurement errors in both exposure and outcome ascertainments are obscured instead of exaggerated the association of interest. The third limitation is that among depression group only 15 (0.3%) women had the medications for longer than 6 months. We were unable to observe whether women with antidepressant are at a higher risk for complications because of the small sample size. To bridge this gap with adverse outcome, future studies will need to provide enough subjects to evaluate outcomes related to medication.
This population-based retrospective cohort study presented that pregnant women with depression are associated with higher risk of hyperemesis, abortion, malpresentation, and Cesarean Section. These findings have important clinical implications for pregnant women and health care professionals. To make a decision about care during pregnancy, depressed women and clinicians must weigh risks and benefits of treatment options against the consequence associated with untreated illness. The underlying mechanisms on severity of depression, comorbidities, and obstetric outcomes still require further explorations.
Methods
Data source and study population
The Department of Health of Taiwan launched a single-payer National Health Insurance (NHI) program in March 1995. Approximately 99% of the 23 million people in Taiwan registered in this program by 2000. With the authorization from the Bureau of National Health Insurance, the National Health Research Institutes of Taiwan established several data files of reimbursement claims publicly available for research.
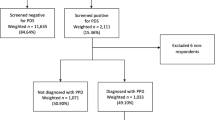
We obtained from the National Health Research Institutes the Longitudinal Health Insurance Database, containing claims data from 1996 to 2013 for one million persons randomly selected from all insured people. Diagnoses were coded with the International Classification of Disease, 9th Revision, Clinical Modification (ICD-9-CM). From the 2005–2013 claims data, we identified pregnant women who had the diagnosis of depression during pregnancy (ICD-9-CM codes of depression: 296.2, 296.20 to 296.25, 296.2, 296.30 to 296.35, 296.82, 300.4, 309.0, 309.1, 309.28, and 311). Only pregnant women with the depression diagnosis for at least 3 times in the outpatient records or for at least once depression diagnosis in the inpatient records were included in the depression cohort. Depressed women with the history of schizophrenia (ICD-9-CM 295), bipolar disorders (ICD-9-CM 296, 296.2, and 296.3) and/or anxiety (ICD-9-CM 300) were excluded. There were 5,064 women eligible for inclusion in the depression group. For each depressed woman, we identified 4 pregnant women without the history of depression, schizophrenia, bipolar disorders and anxiety as the comparison group, frequency matched by age, parity and pregnancy year. Overall, 20,024 women were identified for the non-depressed group. The Research Ethics Committee of China Medical University and Hospital approved this study (CMUH-104-REC2–115). The original identification number of each person in this secondary database has been encrypted and replaced with surrogate identification. The study population was waived from informed consent process because there was no breach of privacy.
Outcome measures
We examined obstetric adverse outcomes occurred during pregnancy and post-delivery in both groups. We evaluated incident events of hyperemesis, gestational diabetes, preeclampsia/eclampsia, abortion, intrauterine growth retardation, antepartum hemorrhage, placenta previa, placental abruption, premature rupture of membranes, chorioamnionitis, postpartum hemorrhage, preterm delivery, low birth weight, malpresentation, normal spontaneous delivery, Cesarean section, vacuum extraction delivery and intrauterine fetal death.
Statistical analyses
We used SAS software version 9.4 (SAS Institute Inc., Carey, USA) to perform data analyses for this study. The Chi-square test was used to examine the differences between the depression group and the comparison group for the baseline sociodemographic characteristics, including age (<25, 25–34 and ≥35 years), geographic region of residence (Northern, Central, Southern, and Eastern), monthly income (<15,840 NTD [one USD is equivalent to 30–34 NTD, which is 30.3 NTD recently], 15,841~25,000 NTD and ≥25,001 NTD), pregnancy history, and comorbidities. Comorbidity was considered if the woman was diagnosed at least twice in the outpatient claims or once in the inpatient claims. Diabetes, hypertension, hyperthyroidism, and anemia were the comorbidities included in this study. We measured the number and incidence rate of each of aforementioned pregnancy events for both the depression and comparison groups. Univariate and multiple logistic regression analyses assessed the odds ratio (OR) of each obstetric event associated with the depression status. Both crude OR and adjusted OR with 95% confidence intervals (CI) were presented. Age, geographic region, parity, and comorbidity were included in the multivariable analysis. Age-specific analyses were further performed to identify high-risk age group if the obstetric event appeared significant. Interactions between age and depression were examined for these events. Further data analysis compared the controls against depression with and without medication. Age-specific analyses were also performed to identify high-risk age group if the obstetric event appeared significant. Interactions between age and anti-depressant medication were examined for these events.
Data availability
The data that support the findings of this study were obtained from National Health Research Institutes (NHRI) of the Ministry of Health and Welfare in Taiwan but restrictions apply to the availability of these data, which were used under license for our study, and so are not publicly available for duplication. Data can be requested only from the Ministry of Health and Welfare.
Change history
08 November 2018
A correction to this article has been published and is linked from the HTML and PDF versions of this paper. The error has not been fixed in the paper.
References
Ververs, T. et al. Prevalence and patterns of antidepressant drug use during pregnancy. Eur J Clin Pharmacol 62, 863–870, https://doi.org/10.1007/s00228-006-0177-0 (2006).
Ververs, T., van Dijk, L., Yousofi, S., Schobben, F. & Visser, G. H. Depression during pregnancy: views on antidepressant use and information sources of general practitioners and pharmacists. BMC Health Serv Res 9, 119, https://doi.org/10.1186/1472-6963-9-119 (2009).
Wisner, K. L., Gelenberg, A. J., Leonard, H., Zarin, D. & Frank, E. Pharmacologic treatment of depression during pregnancy. JAMA 282, 1264–1269 (1999).
Alder, J., Fink, N., Bitzer, J., Hosli, I. & Holzgreve, W. Depression and anxiety during pregnancy: a risk factor for obstetric, fetal and neonatal outcome? A critical review of the literature. J Matern Fetal Neonatal Med 20, 189–209, https://doi.org/10.1080/14767050701209560 (2007).
Andersson, L., Sundstrom-Poromaa, I., Wulff, M., Astrom, M. & Bixo, M. Implications of antenatal depression and anxiety for obstetric outcome. Obstet Gynecol 104, 467–476, https://doi.org/10.1097/01.AOG.0000135277.04565.e9 (2004).
Bonari, L. et al. Perinatal risks of untreated depression during pregnancy. Canadian journal of psychiatry. Revue canadienne de psychiatrie 49, 726–735 (2004).
Koren, G., Matsui, D., Einarson, A., Knoppert, D. & Steiner, M. Is maternal use of selective serotonin reuptake inhibitors in the third trimester of pregnancy harmful to neonates? CMAJ 172, 1457–1459, https://doi.org/10.1503/cmaj.1041100 (2005).
Li, D., Liu, L. & Odouli, R. Presence of depressive symptoms during early pregnancy and the risk of preterm delivery: a prospective cohort study. Hum Reprod 24, 146–153, https://doi.org/10.1093/humrep/den342 (2009).
Wisner, K. L. et al. Major depression and antidepressant treatment: impact on pregnancy and neonatal outcomes. Am J Psychiatry 166, 557–566, https://doi.org/10.1176/appi.ajp.2008.08081170 (2009).
Ban, L., Tata, L. J., West, J., Fiaschi, L. & Gibson, J. E. Live and non-live pregnancy outcomes among women with depression and anxiety: a population-based study. PLoS One 7, e43462, https://doi.org/10.1371/journal.pone.0043462 (2012).
Galbally, M., Snellen, M. & Lewis, A. J. A review of the use of psychotropic medication in pregnancy. Curr Opin Obstet Gynecol 23, 408–414, https://doi.org/10.1097/GCO.0b013e32834b92f3 (2011).
Hayes, R. M. et al. Maternal antidepressant use and adverse outcomes: a cohort study of 228,876 pregnancies. Am J Obstet Gynecol 207(49), e41–49, https://doi.org/10.1016/j.ajog.2012.04.028 (2012).
Martini, J., Knappe, S., Beesdo-Baum, K., Lieb, R. & Wittchen, H. U. Anxiety disorders before birth and self-perceived distress during pregnancy: associations with maternal depression and obstetric, neonatal and early childhood outcomes. Early Hum Dev 86, 305–310, https://doi.org/10.1016/j.earlhumdev.2010.04.004 (2010).
Ross, L. E. et al. Selected pregnancy and delivery outcomes after exposure to antidepressant medication: a systematic review and meta-analysis. JAMA Psychiatry 70, 436–443, https://doi.org/10.1001/jamapsychiatry.2013.684 (2013).
Thornton, D., Guendelman, S. & Hosang, N. Obstetric complications in women with diagnosed mental illness: the relative success of California’s county mental health system. Health Serv Res 45, 246–264, https://doi.org/10.1111/j.1475-6773.2009.01058.x (2010).
Lin, H. C., Lin, Y. J., Hsiao, F. H. & Li, C. Y. Prenatal care visits and associated costs for treatment-seeking women with depressive disorders. Psychiatr Serv 60, 1261–1264, https://doi.org/10.1176/ps.2009.60.9.1261 (2009).
Wang, S. Y. & Chen, C. H. The association between prenatal depression and obstetric outcome in Taiwan: a prospective study. J Womens Health (Larchmt) 19, 2247–2251, https://doi.org/10.1089/jwh.2010.1988 (2010).
Freeman, M. P. Antidepressant medication treatment during pregnancy: prevalence of use, clinical implications, and alternatives. J Clin Psychiatry 72, 977–978, https://doi.org/10.4088/JCP.11f07206 (2011).
Chambers, C., Moses-Kolko, E. & Wisner, K. L. Antidepressant use in pregnancy: new concerns, old dilemmas. Expert Rev Neurother 7, 761–764, https://doi.org/10.1586/14737175.7.7.761 (2007).
Gawley, L., Einarson, A. & Bowen, A. Stigma and attitudes towards antenatal depression and antidepressant use during pregnancy in healthcare students. Adv Health Sci Educ Theory Pract 16, 669–679, https://doi.org/10.1007/s10459-011-9289-0 (2011).
Jarde, A. et al. Neonatal Outcomes in Women With Untreated Antenatal Depression Compared With Women Without Depression: A Systematic Review and Meta-analysis. JAMA Psychiatry 73, 826–837, https://doi.org/10.1001/jamapsychiatry.2016.0934 (2016).
Chang, H. Y. et al. Prenatal maternal depression is associated with low birth weight through shorter gestational age in term infants in Korea. Early Hum Dev 90, 15–20, https://doi.org/10.1016/j.earlhumdev.2013.11.006 (2014).
Yang, S. et al. Symptoms of anxiety and depression during pregnancy and their association with low birth weight in Chinese women: a nested case control study. Arch Womens Ment Health 20, 283–290, https://doi.org/10.1007/s00737-016-0697-2 (2017).
Gelman, P. L., Flores-Ramos, M., Lopez-Martinez, M., Fuentes, C. C. & Grajeda, J. P. Hypothalamic-pituitary-adrenal axis function during perinatal depression. Neuroscience bulletin 31, 338–350, https://doi.org/10.1007/s12264-014-1508-2 (2015).
Mitchell-Jones, N. et al. Psychological morbidity associated with hyperemesis gravidarum: a systematic review and meta-analysis. BJOG 124, 20–30, https://doi.org/10.1111/1471-0528.14180 (2017).
Einarson, T. R., Piwko, C. & Koren, G. Quantifying the global rates of nausea and vomiting of pregnancy: a meta analysis. J Popul Ther Clin Pharmacol 20, e171–183 (2013).
Dorheim, S. K., Bjorvatn, B. & Eberhard-Gran, M. Sick leave during pregnancy: a longitudinal study of rates and risk factors in a Norwegian population. BJOG 120, 521–530, https://doi.org/10.1111/1471-0528.12035 (2013).
Gazmararian, J. A. et al. Hospitalizations during pregnancy among managed care enrollees. Obstet Gynecol 100, 94–100 (2002).
Bustos, M., Venkataramanan, R. & Caritis, S. Nausea and vomiting of pregnancy - What’s new? Auton Neurosci 202, 62–72, https://doi.org/10.1016/j.autneu.2016.05.002 (2017).
Wood, H., McKellar, L. V. & Lightbody, M. Nausea and vomiting in pregnancy: blooming or bloomin’ awful? A review of the literature. Women Birth 26, 100–104, https://doi.org/10.1016/j.wombi.2012.10.001 (2013).
Kjeldgaard, H. K., Eberhard-Gran, M., Benth, J. S., Nordeng, H. & Vikanes, A. V. History of depression and risk of hyperemesis gravidarum: a population-based cohort study. Arch Womens Ment Health, https://doi.org/10.1007/s00737-016-0713-6 (2017).
Hizli, D., Kamalak, Z., Kosus, A., Kosus, N. & Akkurt, G. Hyperemesis gravidarum and depression in pregnancy: is there an association? J Psychosom Obstet Gynaecol 33, 171–175, https://doi.org/10.3109/0167482X.2012.717129 (2012).
Kaihola, H., Olivier, J., Poromaa, I. S. & Akerud, H. The effect of antenatal depression and selective serotonin reuptake inhibitor treatment on nerve growth factor signaling in human placenta. PLoS One 10, e0116459, https://doi.org/10.1371/journal.pone.0116459 (2015).
Dhobale, M. V., Pisal, H. R., Mehendale, S. S. & Joshi, S. R. Differential expression of human placental neurotrophic factors in preterm and term deliveries. Int J Dev Neurosci 31, 719–723, https://doi.org/10.1016/j.ijdevneu.2013.09.006 (2013).
Tometten, M., Blois, S. & Arck, P. C. Nerve growth factor in reproductive biology: link between the immune, endocrine and nervous system? Chemical immunology and allergy 89, 135–148, https://doi.org/10.1159/000087962 (2005).
Frank, P. et al. Balanced levels of nerve growth factor are required for normal pregnancy progression. Reproduction 148, 179–189, https://doi.org/10.1530/REP-14-0112 (2014).
Nakhai-Pour, H. R., Broy, P. & Berard, A. Use of antidepressants during pregnancy and the risk of spontaneous abortion. CMAJ 182, 1031–1037, https://doi.org/10.1503/cmaj.091208 (2010).
Kjaersgaard, M. I. et al. Prenatal antidepressant exposure and risk of spontaneous abortion - a population-based study. PLoS One 8, e72095, https://doi.org/10.1371/journal.pone.0072095 (2013).
Nikfar, S., Rahimi, R., Hendoiee, N. & Abdollahi, M. Increasing the risk of spontaneous abortion and major malformations in newborns following use of serotonin reuptake inhibitors during pregnancy: A systematic review and updated meta-analysis. Daru 20, 75, https://doi.org/10.1186/2008-2231-20-75 (2012).
Johansen, R. L., Mortensen, L. H., Andersen, A. M., Hansen, A. V. & Strandberg-Larsen, K. Maternal use of selective serotonin reuptake inhibitors and risk of miscarriage - assessing potential biases. Paediatr Perinat Epidemiol 29, 72–81, https://doi.org/10.1111/ppe.12160 (2015).
Andersen, J. T., Andersen, N. L., Horwitz, H., Poulsen, H. E. & Jimenez-Solem, E. Exposure to selective serotonin reuptake inhibitors in early pregnancy and the risk of miscarriage. Obstet Gynecol 124, 655–661, https://doi.org/10.1097/AOG.0000000000000447 (2014).
Gardberg, M., Leonova, Y. & Laakkonen, E. Malpresentations–impact on mode of delivery. Acta Obstet Gynecol Scand 90, 540–542, https://doi.org/10.1111/j.1600-0412.2011.01105.x (2011).
Arulkumaran, S. In Dewhurst’s Textbook of Obstetrics and Gynaecology (ed Keith Edmonds) Ch. Malpresentation, malposition, cephalopelvic disproportion and obstetric procedures 311 (Wiley-Blackwell, (2012).
Chung, T. K., Lau, T. K., Yip, A. S., Chiu, H. F. & Lee, D. T. Antepartum depressive symptomatology is associated with adverse obstetric and neonatal outcomes. Psychosom Med 63, 830–834 (2001).
Johnstone, S. J., Boyce, P. M., Hickey, A. R., Morris-Yatees, A. D. & Harris, M. G. Obstetric risk factors for postnatal depression in urban and rural community samples. Aust N Z J Psychiatry 35, 69–74, https://doi.org/10.1046/j.1440-1614.2001.00862.x (2001).
Yedid Sion, M., Harlev, A., Weintraub, A. Y., Sergienko, R. & Sheiner, E. Is antenatal depression associated with adverse obstetric and perinatal outcomes? J Matern Fetal Neonatal Med 29, 863–867, https://doi.org/10.3109/14767058.2015.1023708 (2016).
Navaratne, P., Foo, X. Y. & Kumar, S. Impact of a high Edinburgh Postnatal Depression Scale score on obstetric and perinatal outcomes. Sci Rep 6, 33544, https://doi.org/10.1038/srep33544 (2016).
Cohen, L. S. et al. Relapse of major depression during pregnancy in women who maintain or discontinue antidepressant treatment. Jama 295, 499–507 (2006).
Sit, D. et al. Mother-infant antidepressant concentrations, maternal depression, and perinatal events. The Journal of clinical psychiatry 72, 994–1001 (2011).
Acknowledgements
This study is supported in part by Taiwan Ministry of Health and Welfare Clinical Trial Center (MOHW106-TDU-B-212-113004); Academia Sinica Taiwan Biobank, Stroke Biosignature Project (BM10501010037); NRPB Stroke Clinical Trial Consortium (MOST 105-2325-B-039-003); Tseng-Lien Lin Foundation, Taichung, Taiwan; Taiwan Brain Disease Foundation, Taipei, Taiwan; Katsuzo and Kiyo Aoshima Memorial Funds, Japan; China Medical University Hospital; CMU under the Aim for Top University Plan of the Ministry of Education, Taiwan. The funding agencies had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. No additional external funding received for this study. FC Sung and SI Wu have equal contribution for this study.
Author information
Authors and Affiliations
Contributions
Study concept development: H.C.H., C.Y.Y.C. and H.S.S.; study design: H.C.H., C.Y.Y.C., F.C.S. and P.C.C.; designed and performed the study’s data analysis: H.C.H., C.H.M. and J.P.H.; data interpretation: all authors; draft manuscript and literature study: H.C.H., F.C.S., P.C.C., T.C.L., Y.L.T. and S.I.W.; final approval of the version to be published: F.C.S. and S.I.W.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Huang, HC., Sung, FC., Chen, PC. et al. Obstetric outcomes in pregnant women with and without depression: population-based comparison. Sci Rep 7, 13937 (2017). https://doi.org/10.1038/s41598-017-14266-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-14266-3
Keywords
This article is cited by
-
Psychiatric disorders in term-born children with marginally low birth weight: a population-based study
Child and Adolescent Psychiatry and Mental Health (2024)
-
A longitudinal cohort study of gestational diabetes mellitus and perinatal depression
BMC Pregnancy and Childbirth (2022)
-
The impact of maternal prenatal mental health disorders on stillbirth and infant mortality: a systematic review and meta-analysis
Archives of Women's Mental Health (2021)
-
Prenatal selective serotonin reuptake inhibitors and therapeutic hypothermia for suspected hypoxic ischemic encephalopathy
Journal of Perinatology (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.