Abstract
The failure of Kupffer cells (KCs) to remove endotoxin is an important factor in the pathogenesis of non-alcoholic fatty liver disease (NAFLD). In this study, the effects of exercise training on KC function were studied in terms of in vivo endotoxin clearance and inflammatory responses. Mice were allocated into rest and exercise groups. KC bead phagocytic capacity and plasma steroid hormone levels were determined following exercise training. Endotoxin and inflammatory cytokine levels in plasma were determined over time following endotoxin injection. KC bead phagocytic capacity was potentiated and clearance of exogenously-injected endotoxin was increased in the exercise group. Inflammatory cytokine (TNF-α and IL-6) levels were lower in the exercise group. We found that only DHEA was increased in the plasma of the exercise group. In an in vitro experiment, the addition of DHEA to RAW264.7 cells increased bead phagocytic capacity and attenuated endotoxin-induced inflammatory responses. These results suggest that exercise training modulates in vivo endotoxin clearance and inflammatory responses in association with increased DHEA production. These exercise-induced changes in KC capacity may contribute to a slowing of disease progression in NAFLD patients.
Similar content being viewed by others
Introduction
The problem of obesity continues to worsen as a result of several factors including the westernization of dietary habits and chronic insufficient exercise. According to a recent Japanese nationwide survey, the prevalence of abnormal hepatic function in adults is rapidly increasing1. The increased incidence of non-alcoholic fatty liver disease (NAFLD) contributes significantly to this trend. In some cases, NAFLD progresses to non-alcoholic steatohepatitis (NASH), which is progressive and eventually leads to hepatic cirrhosis or liver cancer.
The “multiple parallel hits” hypothesis has been applied to the pathogenesis of NAFLD. In this context, it is suggested that several factors, including insulin resistance, adipokines, oxidative stress, and enteric bacteria, all damage the liver2. Endotoxin, an enteric bacterially-derived molecule, is thought to play an important role in NAFLD pathogenesis3. In patients with NASH, intestinal permeability is enhanced in fragile intestinal epithelium such that endotoxin passes more easily into the portal vein, resulting in endotoxemia4. Excessive endotoxin is recognized by Toll-like receptors (TLRs) on Kupffer cells (KCs), thereby triggering the inflammatory response. This may lead to accumulation of fat in the liver, development of fibrosis, and eventually NASH. Thus, the capacity of KCs to remove endotoxin may be important in attenuation of the progression of NAFLD.
KCs are liver-resident macrophages, accounting for approximately 80% of the macrophages in the whole body5. KCs participate in the initial step of the innate immune response: phagocytosis of harmful exogenous substances such as endotoxin6,7. Phagocytic capacity is known to be regulated by hormones and cytokines8. In NAFLD, reduced phagocytic capacity of KCs has been reported both in humans and in animal models9,10,11. Phagocytic capacity is reduced in parallel with progression of hepatic lesions in NAFLD9. We developed a mouse model of NASH, the p62:Nrf2 double knockout mouse12 that exhibited reduction in KC phagocytic capacity. In our model, endotoxaemia and the activated KC inflammatory response, both associated with the KCs dysfunction, led to chronic inflammation in the liver. This suggests that abnormalities in KC phagocytic capacity may cause a reduction in in vivo endotoxin clearance, leading to progression of inflammatory liver disease. These conditions are assumed to be involved in the aggravation of NAFLD hepatic lesions and the progression from simple steatosis to NASH.
Prevention and treatment of NAFLD present important medical challenges in clinical practice. At present, there is no consensus regarding prevention and treatment of NAFLD apart from diet and exercise therapy. Furthermore, there is insufficient evidence in support of exercise therapy as an effective modality, compared with diet therapy.
A meta-analysis suggested that exercise therapy may be useful for improvement of hepatic lipid accumulation in NAFLD13. Our group performed a clinical study of exercise therapy suggesting that increased physical activity at moderate to high intensity decreased hepatic lipid accumulation and ameliorated inflammatory/oxidative stress14. In this randomized comparison study, hepatic lipid accumulation and hepatic stiffness was reduced in the high-intensity aerobic exercise group compared with the resistance exercise group. The high-intensity aerobic exercise group also demonstrated improved foreign-body phagocytosis by KCs15. Recovery from suppression of KC activity may contribute to these exercise-induced improvements in NAFLD-related changes.
Acute exercise in animal models affects levels of steroid hormones16,17 and increases KC bead phagocytic capacity16. These results suggest that exercise may modulate KC function such as in vivo clearance and the inflammatory response to endotoxin. However, the specific effects of exercise on KCs and the details of the molecular mechanisms in NAFLD have yet to be elucidated.
In this study, we investigated the effects of exercise training on KC function, particularly on foreign-body phagocytic capacity, in vivo endotoxin clearance, and the inflammatory response to endotoxin. We also performed an in vitro study of the effects of steroid hormones on bead phagocytic capacity and the inflammatory response to endotoxin in RAW264.7 cells.
Methods
Animal care
Seven-week-old male C57/BL/6 J mice were obtained from Charles River Japan (Kanagawa, Japan). The mice were housed with a 12-h light/dark cycle, at room temperature 23.5 ± 2.5 °C, and humidity at 52.5 ± 12.5%. The mice had ad libitum access to food and water. After preliminary breeding for 1 week, the mice were randomly divided into two groups: 3-month rest group (3moR), and 3-month exercise group (3moTr). For the exercise group, treadmill exercise was undertaken (MK-680, Muromachi Kikai). Exercise groups were habituated to treadmill running for 3 days. First day intensity for adaptation was 5 m/min for 10 min and 10 m/min for 10 min. Second and final day intensity was 10 m/min for 10 min and 15 m/min for 10 min. Going forward, exercise intensity was increased to 10 m/min for 5 min, 12 m/min for 5 min, 14 m/min for 5 min, 16 m/min for 5 min, and 18 m/min for 30 min, for a total of 50 min once per day, 5 times per week. To generate macrophage-deficient mice following the 3-month period, we injected Clophosome®-A (FormuMax Scientific) at 8 µL/g body weight immediately following the exercise load. We identified this group as the 3-month rest group with Clophosome-A (Lipo3moR) and the 3-month exercise group with Clophosome-A (Lipo3moTr).
Animal experiments were carried out humanely in accordance with the Regulations for Animal Experiments of University of Tsukuba, and the Fundamental Guidelines for Proper Conduct of Animal Experiments and Related Activities in Academic Research Institutions under the jurisdiction of the Ministry of Education, Culture, Sports, Science, and Technology of Japan, and with approval from the Institutional Animal Care and Use Committees of University of Tsukuba.
Sample collections
Following the exercise protocol, the mice rested for 1 day and were anaesthetized with an intraperitoneal injection of pentobarbital (50 mg/kg body weight). We measured body weight and wet weight of the following: liver, epididymal fat, muscles (soleus, gastrocnemius, plantaris, and tibialis anterior). Samples were then rapidly frozen. Blood samples were collected from the inferior vena cava and centrifuged at 4000 rpm at 4 °C for 15 min. Tissue samples and supernatant were stored at −80 °C. For estimation of whole body skeletal muscle mass, visceral fat mass, and subcutaneous fat mass, anesthetized mice were placed on a bed made of polystyrene form and scanned by a micro-CT scanner (Latheta, LCT-200, Hitachi Aloka Medical).
Separation of liver non-parenchymal cells and analysis of Kupffer cell foreign-body phagocytosis
For the KC phagocytosis assay, we isolated non-parenchymal cells from livers one day following exercise. The mice were anesthetized and perfused with liver perfusion medium (Gibco) for 4 min, followed by DMEM with collagenase Type 4 (Worthington Biochemical), trypsin inhibitor (Wako Chemical), and HEPES (Dojindo) at 37 °C for 10 min. Liver samples were collected and cells were isolated in hepatocyte wash medium (Gibco). To remove parenchymal cells, the samples were centrifuged three times at 30 g for 2 min. The supernatants were centrifuged at 400 g for 8 min, and precipitates including KCs were obtained. The samples were analysed by flow cytometry.
KC foreign-body phagocytosis analysed by flow cytometry
Prior to 5 min of liver perfusion, latex beads (Invitrogen, FluoSpheres®, 1.0 µm diameter, carboxylate-modified) at 0.57 µl/g body weight were injected in the tail vein. Following liver perfusion, the cells were isolated. KC surface marker F4/80 was stained. Percentage of phagocytic cells and fluorescent intensity of latex beads in F4/80-positive cells were evaluated by flow cytometry.
The expression levels of KC surface proteins involved in phagocytosis (CD68, macrophage receptor with collagenous structure; MARCO, macrophage class A scavenger receptors; SR-A) were analysed by flow cytometry. Samples were incubated with APC-conjugated anti-F4/80 (17-4801-82, eBioscience), PerCP/Cy5.5- conjugated anti-CD68 (137010, BioLegend), MARCO (MCA1849, Bio-Rad) and SR-A (AF1797, R&D Systems), followed by incubation with the secondary antibody Alexa Fluor 488 (Invitrogen). All flow cytometry data were collected on a Gallios flow cytometer (Beckman Coulter). Data were analysed using Kaluza flow cytometry data analysis software (v. 1.2, Beckman Coulter).
Immunohistochemistry
Fresh liver tissues were washed with PBS, fixed in 4% paraformaldehyde for 24 h, dehydrated with 70% ethyl alcohol, and embedded in paraffin. Liver tissues were then sectioned at 3 µm. Sections were de-paraffinized using xylene and ethanol. For antigen retrieval, slices were immersed in HistoVT One (Nacalai Tesque) at 37 °C for 20 min. Endogenous peroxidase activity was blocked using 3% H2O2 with methanol and DAKO wash buffer. Blocking One Histo (Nacalai Tesque) was added to samples for 20 min. F4/80 antibodies (HM1066, Hycult Biotechnology) with PBS were added and incubated overnight. The following day, biotinidase rat antibodies were applied. Staining was performed using the Vectastain Universal Elite ABC kit (Vector Laboratories Burlingame). All slides were counterstained with Mayer’s haematoxylin and mounted using permanent mounting media. The slides were analysed by fluorescence microscopy (BZ-X710; Keyence Japan).
Measurements of in vivo endotoxin clearance
After resting for one day following exercise, all groups were injected in the tail vein with endotoxin at 0.01 µg/g body weight (E. coli O111:B4, Sigma-Aldrich). Blood samples were collected with heparin from the same vein at baseline (pre), and at 1.5, 3.0, 6.0, and 12.0 h following injection. Each sample was immediately centrifuged at 4000 rpm for 15 min. The supernatants were stored at −80 °C until assay. Endotoxin levels in plasma samples were assessed using the LAL pyrochrome reagent in Glucasheld buffer (Associates of Cape Cod). To remove the amber colour, we used the PyroColor Diazo Reagents kit (Associates of Cape Cod). Optical density was measured using an iMark Absorbance Microplate Reader at 540 nm (Bio Rad Laboratories).
Measurements of cytokine and steroid hormone concentrations in peripheral blood
Prasma cytokine levels (TNF-α, IL-6, and IL-10) were measured using a multiplex bead analysis system (BioRad Laboratories). Serum testosterone (ADI-900-065, ENZO Life Sciences), estradiol (ES180S-100, Cal Biotech), corticosterone (501320, Cayman Chemical Company), DHEA (DI-900-093, ENZO Life Sciences), leptin (M1305, Morinaga Institute of Biological Science), and adiponectin (MRP300, R&D Systems) were measured according to the manufacturer’s instructions.
In vitro experiments
Mouse RAW264.7 macrophage-derived cells were cultured in DMEM high glucose medium supplemented with 10% fetal bovine serum (FBS), penicillin (50 U/ml), and streptomycin (50 mg/ml) at 5% CO2, 95% humidity, 37 °C.
To evaluate foreign-body phagocytic activity, 2.5 × 105 RAW264.7 cells were plated in 6-well plates and incubated for 24 hours. The cells were then incubated with DHEA (TCI) at various concentrations (1.0, 5.0, 10.0 ng/ml with DMSO) for 12 hours. Latex beads at 0.66 µl/ml DMEM were added for 12 hours. Following incubation, cells were fixed in 4% paraformaldehyde. For flow cytometric analysis, cells were washed with PBS on the dish and collected using a cell scraper. These samples were then washed twice by centrifugation at 4000 rpm for 3 min. Immediately thereafter, bead fluorescence in the cells was analysed by flow cytometry.
To evaluate inflammatory response to endotoxin, following 24-hour culture, the cells were incubated with DHEA (10.0 ng/ml with DMSO) for 12 hours prior to adding endotoxin (100 ng/ml) for 1 hour. After washing with PBS, the cells were lysed in SDS buffer, protease inhibitor cocktail, and phosphatase inhibitor cocktail (Nacalai Tesque). Lysates were stored at −80 °C until assay.
Protein concentration in cell lysates was measured using a BCA protein assay kit (Thermo Scientific Pierce). Dilution with lysis buffer was employed to normalize protein concentrations. Equal amounts of protein (10 µg per well) and corresponding loading buffer were mixed and analysed by gel electrophoresis. The proteins were transferred to nitrocellulose membranes and blocked with Blocking One-P (Nacalai Tesque) for 1 hour. β-Actin (SC-1616, Santa Cruz), IκB-α (SC-371, Santa Cruz), NFκB-p65 (C22B4, Cell Signaling Technology), and phospho-NFκB-p65 (93H1, Cell Signaling Technology) were diluted with Signal Enhancer HIKARI for Western Blotting and ELISA (Nacalai Tesque). The membranes were incubated at 4 °C overnight, followed by incubation with HRP-conjugated secondary antibodies for 2 hours at room temperature. Target proteins were visualized by Chemi-Lumi One Super (Nacalai Tesque) and then exposed using a ChemiDoc XRS+ system chemiluminescence imager (Bio-Rad). Image Lab software (Bio-Rad) was used for image acquisition and densitometry analysis.
Statistical analysis
Statistical analysis was performed using SPSS Statistics for Macintosh, version 21.0 (IBM). Descriptive parameters are expressed as mean ± standard error (SE). For inter-group comparisons, non-parametric (Mann-Whitney U or Kruskal-Wallis test) tests were applied. Statistical significance was defined as P < 0.05 for all analyses.
Results
Changes in body weight and composition
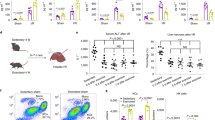
Figure 1a–d displays weights of body, liver, epididymal fat, and hind-limb skeletal muscle (soleus, gastrocnemius, plantaris, and tibialis anterior). At the 3-month time point, there was no significant difference in any parameter between the rest group (3moR) and the exercise group (3moTr). In the analysis by CT, there was no difference in the weight of total-body skeletal muscle between the 3moR and the 3moTr groups (Fig. 1e). Conversely, both the visceral fat mass and the subcutaneous fat mass were lower in the 3moTr group, compared with the 3moR group (Fig. 1e).
Changes in body weight and body composition. (a) Body weight. (b) Liver weight. (c) Epididymal fat weight. (d) Weight of individual skeletal muscles (soleus, gastrocnemius, plantaris, and tibialis anterior). (e) Weight of total-body skeletal muscle, visceral fat, and subcutaneous fat (analysed by CT for small animals). For all groups, n = 8. Values are expressed as mean ± standard error. *P < 0.05, significantly different from the 3moR group.
Changes in number and foreign-body phagocytic capacity of Kupffer cells
Immunohistochemical staining of the livers revealed that there was no difference in the number of the KC surface marker F4/80-positive cells between the 3moR and the 3moTr groups. In the livers of the Lipo3moR mice, the number of F4/80-positive cells was decreased (Fig. 2a). Flow cytometric analysis of the hepatic non-parenchymal cell fraction revealed no difference in terms of percentage of F4/80-positive cells between the 3moR and the 3moTr groups. This percentage was lower in the Lipo3moR group (Fig. 2b).
Changes in foreign-body phagocytic capacity and surface proteins of Kupffer cells (KCs). (a) Immunohistochemistry of F4/80 in liver. The arrow indicates the F4/80-positive cells. Scale bar, 50 µm. (b) Percentage of F4/80-positive cells in liver non-parenchymal cell fraction (flow cytometric analysis). (c) Latex beads phagocytic capacity of KCs. (d) Expression levels of surface proteins of KCs. For all groups, n = 8. Values are expressed as mean ± standard error. *P < 0.05, significantly different from the 3moR group.
Since KC number did not change following 3-month exercise training, foreign-body phagocytic capacity of KCs was analysed by flow cytometry (Fig. 2c). Uptake and fluorescence intensity of latex beads engulfed in F4/80-positive cells were determined (Fig. 2c). In the histogram, the fluorescence intensity of the right-side peak, representing the latex bead-engulfing cells, was increased in the 3moTr group. The number of KCs that had engulfed latex beads as a percentage of all KCs was significantly increased in the 3moTr group compared with the 3moR group. The mean fluorescence intensity (MFI) of the beads engulfed in KCs showed a significant difference in the 3moTr group as compared with that of the 3moR group. The number of CD68-positive KCs was significantly increased in the 3moTr group compared with the 3moR group (Fig. 2d). The percentage of MARCO-positive cells and the percentage of SR-A-positive cells were higher in the 3moTr group, compared with the 3moR group (Fig. 2d). Similarly, the MFI of these proteins were higher in the 3moTr group.
Changes in in vivo endotoxin clearance and cytokine levels
Exercise training caused an increase in foreign-body phagocytic capacity of KCs (Fig. 2b). Endotoxin levels in portal vein blood did not change following 3-month exercise training (Fig. 3a). Therefore, to investigate the capacity of KCs to remove endotoxin, we assessed the time courses of endotoxin and cytokine levels in blood following the administration of endotoxin 24 hours following exercise training (Fig. 3b and c). In Fig. 3b, a peak appeared at 1.5 hours following endotoxin administration in the 3moR group, followed by a gradual decrease in endotoxin levels. In the 3moTr group, a peak in the endotoxin levels appeared at 1.5 hours, but the peak value was significantly lower. The peak values of endotoxin levels in the Lipo3moR and Lipo3moTr groups were higher than those of the 3moR and 3moTr groups. The area under the curve (AUC) value of the endotoxin levels was significantly lower in the 3moTr group compared with that of the 3moR group. The AUC values were higher in the Lipo3moR and Lipo3moTr groups. These results suggest that 3-month exercise training increased endotoxin clearance in vivo.
Changes in in vivo endotoxin clearance and cytokine levels. (a) Endotoxin levels in portal vein blood. Levels were determined immediately following the end of the final exercise load. (b) Time course of endotoxin levels in peripheral blood. (c) Time course of cytokine levels in peripheral blood. (b,c) After administration of endotoxin (0.01 µg/g body weight) into the tail vein, blood was sampled prior to administration (Pre), and at time points of 1.5 h, 3.0 h, 6.0 h, and 12 h following administration. For all groups, n = 8. Values are expressed as mean ± standard error. *P < 0.05, significantly different from the 3moR group.
Since 3-month exercise training increased in vivo endotoxin clearance, changes in cytokine levels are shown in Fig. 3c. In the 3moR group, TNF-α and IL-6 levels peaked at 1.5 hours following endotoxin administration. This was followed by a gradual decrease. Similarly, in the 3moTr group, peaks appeared at the 1.5-hour time point, but the peak values of the TNF-α and IL-6 levels were significantly lower than those of the 3moR group. Cytokine levels in the Lipo3moR and Lipo3moTr groups were lower than those of the 3moR and 3moTr groups. These results suggest that 3-month exercise training reduced the inflammatory response to endotoxin. Plasma IL-10 levels peaked at 1.5 hours following endotoxin administration; however, exercise training had no effect on these levels. Following the macrophage depletion groups (Lipo3moR and Lipo3moTr), the peak values of the IL-10 levels were lower than those in the 3moR and 3moTr groups.
Changes in blood steroid hormone levels and adipokine levels
Steroid hormones and adipokines have been reported to increase KC phagocytic capacity18,19,20,21,22. Therefore, we investigated exercise-induced changes in serum levels of steroid hormones and adipokines (Fig. 4). In all groups, the levels of testosterone, estradiol, and corticosterone showed no significant changes (Fig. 4a–c). DHEA levels were significantly higher in the 3moTr group compared with the 3moR group (Fig. 4d).
The levels of leptin, known as proinflammatory adipokine, were significantly lower in the 3moTr group compared with the 3moR group (Fig. 4e). Also, the levels of adiponectin, known as anti-inflammatory, were lower in the 3moTr group (Fig. 4f).
DHEA-induced changes in foreign-body phagocytic capacity and the inflammatory response of macrophages to endotoxin
Three-month exercise training modified the KC phenotypes in association with increased DHEA levels in the blood (Fig. 4d). Following this observation, we investigated the effects of DHEA administration on the phenotypic changes of macrophage cells (RAW264.7) to endotoxin. The dose of DHEA administration was determined in reference to the differences in DHEA concentrations between the 3moR and the 3moTr groups (Fig. 4d).
The addition of DHEA to RAW264.7 significantly increased the MFI of the cells that had engulfed beads at a DHEA concentration of 10 ng/mL compared with control. DHEA increased bead fluorescence intensity in a concentration-dependent manner. An increase in the number of beads could also be confirmed by flow cytometry (Fig. 5a). Endotoxin administration (100 ng/mL) accelerated the phosphorylation of NFκB-p65 and degradation of IκB-α. Following the addition of DHEA (10 ng/mL), there was no difference in degradation of IκB-α, but phosphorylation of NFκB-p65 was significantly attenuated, compared with the group without the addition of DHEA (Fig. 5b and Fig. S1).
DHEA-induced changes in foreign-body phagocytic capacity and inflammatory response of macrophages to endotoxin. (a) Latex beads in RAW264.7 cells and their mean fluorescence intensity (MFI). Latex beads are shown in green. Scale bar, 50 µm. MFI of latex beads was determined by flow cytometry. (b) Endotoxin-induced changes in inflammatory response signal molecules. Analysis was performed 1 hour following the addition of endotoxin (100 µg/mL). For comparison of phagocytic capacity, n = 6 for all groups, and for comparison of inflammatory response, n = 3 for all groups. Values are expressed as mean ± standard error. *P < 0.05, significantly different from the DMSO group.
Discussion
The principal findings of this study are as follows: exercise training for 3 months caused no change in portal vein endotoxin levels or KC number; exercise training caused an increase in foreign-body phagocytic capacity and an increase in the in vivo clearance of endotoxin injected exogenously; exercise training triggered an attenuation in endotoxin-induced inflammatory responses and thereby in inflammatory cytokine levels. The observed effects of exercise training disappeared in KC-depleted mice, suggesting that the observed effects were caused by exercise-induced changes in KC function.
Exercise training caused an increase in the number of beads engulfed by KCs and a potentiation of in vivo endotoxin clearance (Figs 2c and 3b), without altering endotoxin levels in portal vein blood (Fig. 3a). In a report on the relationship between KC phagocytic capacity and exercise, Yano et al. reported that in F344 rats, acute exercise caused endotoxin level increases in portal vein blood, followed by intestinal mucosal damages, and a consequent increase in KC phagocytic capacity16. In isolated KC experiments, endotoxin increased phagocytic capacity23. In our study, exercise training for 3 months caused an increase in KC phagocytic capacity and a potentiation of in vivo endotoxin clearance (Figs 2c and 3b), without alteration of endotoxin levels in portal vein blood (Fig. 3a). The molecular mechanisms mediating these effects are not currently understood. In another report, when [3H]-endotoxin was injected, approximately 80% was detected in the liver24. Therefore, phagocytic capacity of KC is suspected to be important. Taken together, these results suggest that the effects of exercise training on endotoxin clearance and inflammatory response may be attributable to modification of KC function. To the best of our knowledge, our study provides the first evidence of the benefits of exercise training on KC function.
Exercise training for 3 months increased initial bead uptake by KCs (at 5 min following administration) (Fig. 2c). An increase in CD68 and scavenger receptors on the surface of KCs may contribute to increased phagocytic capacity (Fig. 2d). The CD68-positive cells among KCs constitute the cell population with strong bead phagocytic capacity23. Scavenger receptors (MARCO, SR-A) are involved in phagocytic capacity and endotoxin clearance25,26. Exercise training increased expression of these surface molecules on KCs, resulting in an increase in KC phagocytic capacity. We suggest that this may cause lower peak endotoxin levels in peripheral blood following endotoxin administration. One study reports that acute exercise greater than 30 min contributes to an increase in carbon clearance27. This effect may support our results regarding the exercise-induced increase in foreign-body phagocytic capacity of KCs.
We investigated the effects of exercise training on the in vivo inflammatory response to endotoxin. Following endotoxin administration, peripheral blood levels of inflammatory cytokines such as TNF-α and IL-6, and the level of the anti-inflammatory cytokine IL-10 achieved their peak values at 1.5 h (Fig. 3c). Exercise training decreased the inflammatory response to endotoxin via attenuation of the increase in peak values of TNF-α and IL-6 levels at 1.5 h (Fig. 3c). Increased KC phagocytic capacity due to 3-month exercise training resulted in rapid clearance of endotoxin from the body, leading to an attenuation of the inflammatory response. However, no differences between the exercise and rest groups were observed with respect to IL-10 levels (Fig. 3c). Ortega et al. reported that in human monocytes following aquatic exercise training, the amount of IL-10 secreted following endotoxin administration was higher in the exercise group than in the rest group28. More detailed investigations of this phenomenon are required in the future.
We investigated the mechanisms of exercise-induced alteration in KC function in the absence of increases in portal vein blood endotoxin levels. We measured peripheral blood levels of steroid hormones, which have been reported to affect foreign-body phagocytic capacity18,19,20. Following 3-month exercise training, DHEA levels alone were increased. This coincides with the findings of another mouse study, in which endotoxin was injected following DHEA administration. In that study, the survival rate of mice was increased and secretion of TNF-α was inhibited simulatneously29. These results suggest that exercise training may increase blood DHEA levels to reduce the inflammatory response of KCs to endotoxin stimulation.
We investigated DHEA-induced changes in KC function in in vitro experiments. The addition of DHEA to RAW264.7 cells, at a concentration close to the peripheral blood levels after 3-month exercise training (Fig. 4d), caused a dose-dependent increase in latex bead phagocytic capacity (Fig. 5a), and inhibition of endotoxin-induced phosphorylation of NFκB-p65 (Fig. 5b). These in vitro results suggest that the increase in blood DHEA levels by 3-month exercise training may induce an increase in foreign-body phagocytic capacity and a decrease in the inflammatory response of KCs to endotoxin. In a previous study, it was reported that the addition of EPI, a DHEA analogue, to human monocytes increased phagocytosis of malaria-infected erythrocytes (ring stage)30. Another study showed that the addition of DHEA to RAW264.7 inhibited endotoxin-induced TNF-α secretion31. These reports may support the results observed in our study.
It has been reported that adipokines can increase Kupffer cell phagocytic capacity21,22; thus, leptin, a proinflammatory adipokine, and adiponectin, which is anti-inflammatory, increase macrophage phagocytic capacity. In this study, blood leptin and adiponectin levels were both lower in the 3moTr group than in the 3moR group (Fig. 2b). These results were consistent with those of earlier studies32,33. Thus, it cannot be inferred that increased adipokine levels affect the increase in Kupffer cell phagocytic capacity induced by the 3-month exercise training.
Patients with NAFLD suffer various symptoms, including elevated blood endotoxin levels4, decreased KC phagocytic capacity9, and enhanced inflammatory responses34. Hepatic pathology such as fat accumulation and fibrogenesis in NAFLD correlate negatively with blood DHEA levels35. In our recent report15, we demonstrated that exercise training attenuates NAFLD lesions simultaneously with increasing KC phagocytic capacity and decreasing the immune inflammatory response. This study points to one potential molecular mechanism by which exercise training may be useful for the management of NAFLD.
Conclusion
Exercise training for 3 months in mice increased KC foreign-body phagocytic capacity, thereby increasing in vivo endotoxin clearance, and attenuating the increase in inflammatory responses to endotoxin. It is likely that exercise-induced increases in DHEA production may be associated with these observations.
References
Imamura, Y. et al. Increasing prevalence of diabetes mellitus in association with fatty liver in a Japanese population. J Gastroenterol 49, 1406–1413 (2014).
Tilg, H. & Moschen, A. R. Evolution of inflammation in nonalcoholic fatty liver disease: the multiple parallel hits hypothesis. Hepatology 52, 1836–1846 (2010).
Schnabl, B. & Brenner, D. A. Interactions between the intestinal microbiome and liver diseases. Gastroenterology 146, 1513–1524 (2014).
Wigg, A. J. et al. The role of small intestinal bacterial overgrowth, intestinal permeability, endotoxaemia, and tumour necrosis factor alpha in the pathogenesis of non-alcoholic steatohepatitis. Gut 48, 206–211 (2001).
Bouwens, L., Baekeland, M., De Zanger, R. & Wisse, E. Quantitation, tissue distribution and proliferation kinetics of Kupffer cells in normal rat liver. Hepatology 6, 718–722 (1986).
Mathison, J. C. & Ulevitch, R. J. The clearance, tissue distribution, and cellular localization of intravenously injected lipopolysaccharide in rabbits. J Immunol 123, 2133–2143 (1979).
Smedsrod, B. et al. Cell biology of liver endothelial and Kupffer cells. Gut 35, 1509–1516 (1994).
Imajo, K. et al. Hyperresponsivity to low-dose endotoxin during progression to nonalcoholic steatohepatitis is regulated by leptin-mediated signaling. Cell metab 16, 44–54 (2012).
Iijima, H. et al. Decrease in accumulation of ultrasound contrast microbubbles in non-alcoholic steatohepatitis. Hepatol Res 37, 722–730 (2007).
Cheong, H. et al. Phagocytic function of Kupffer cells in mouse nonalcoholic fatty liver disease models: Evaluation with superparamagnetic iron oxide. J Magn Reson Imaging 41, 1218–1227 (2015).
Tsujimoto, T. et al. Decreased phagocytic activity of Kupffer cells in a rat nonalcoholic steatohepatitis model. World J Gastroenterol 14, 6036 (2008).
Akiyama, K. et al. Deletion of both p62 and Nrf2 spontaneously leads to development of steatohepatitis in mice. Hepatology 60(suppl), 761A (2014).
Keating, S. E., Hackett, D. A., George, J. & Johnson, N. A. Exercise and non-alcoholic fatty liver disease: a systematic review and meta-analysis. J Hepatol 57, 157–166 (2012).
Oh, S. et al. Moderate to vigorous physical activity volume is an important factor for managing nonalcoholic fatty liver disease: a retrospective study. Hepatology 61, 1205–1215 (2015).
Oh, S. et al. High-Intensity Aerobic Exercise Improves Both Hepatic Fat Content and Stiffness in Sedentary Obese Men with Nonalcoholic Fatty Liver Disease. Sci Rep 7, 43029 (2017).
Yano, H., Kinoshita, S. & Kira, S. Effects of acute moderate exercise on the phagocytosis of Kupffer cells in rats. Acta physiologica Scandinavica 182, 151–160 (2004).
Howlett, T. A. Hormonal responses to exercise and training: a short review. Clin endocrinol 26, 723–742 (1987).
Chao, T. C., Phuangsab, A., Van Alten, P. J. & Walter, R. J. Steroid sex hormones and macrophage function: regulation of chemiluminescence and phagocytosis. Am J Reprod Immunol 35, 106–113 (1996).
Liu, Y. et al. Glucocorticoids promote nonphlogistic phagocytosis of apoptotic leukocytes. J Immunol 162, 3639–3646 (1999).
Bongiovanni, B. et al. Effect of cortisol and/or DHEA on THP1-derived macrophages infected with Mycobacterium tuberculosis. Tuberculosis 95, 562–569 (2015).
Mancuso, P. et al. Leptin-deficient mice exhibit impaired host defense in Gram-negative pneumonia. J Immunol 168, 4018–4024 (2002).
Yokota, T. et al. Adiponectin, a new member of the family of soluble defense collagens, negatively regulates the growth of myelomonocytic progenitors and the functions of macrophages. Blood 96, 1723–1732 (2000).
Kinoshita, M. et al. Characterization of two F4/80-positive Kupffer cell subsets by their function and phenotype in mice. J Hepatol 53, 903–910 (2010).
Nakatani, Y. et al. Endotoxin clearance and its relation to hepatic and renal disturbances in rats with liver cirrhosis. Liver 21, 64–70 (2001).
Areschoug, T. & Gordon, S. Scavenger receptors: role in innate immunity and microbial pathogenesis. Cell Microbiol 11, 1160–1169 (2009).
Hampton, R. Y., Golenbock, D. T., Penman, M., Krieger, M. & Raetz, C. R. Recognition and plasma clearance of endotoxin by scavenger receptors. Nature 352, 342–344 (1991).
Sugiura, H. et al. Effects of different durations of exercise on macrophage functions in mice. J Appl Physiol 90, 789–794 (2001).
Ortega, E., Bote, M. E., Giraldo, E. & Garcia, J. J. Aquatic exercise improves the monocyte pro- and anti-inflammatory cytokine production balance in fibromyalgia patients. Scand J Med Sci Sports 22, 104–112 (2012).
Danenberg, H. D., Alpert, G., Lustig, S. & Ben-Nathan, D. Dehydroepiandrosterone protects mice from endotoxin toxicity and reduces tumor necrosis factor production. Antimicrob Agents Chemother 36, 2275–2279 (1992).
Ayi, K. et al. 16alpha-bromoepiandrosterone, an antimalarial analogue of the hormone dehydroepiandrosterone, enhances phagocytosis of ring stage parasitized erythrocytes: a novel mechanism for antimalarial activity. Antimicrob Agents Chemother 46, 3180–3184 (2002).
Ben-Nathan, D., Padgett, D. A. & Loria, R. M. Androstenediol and dehydroepiandrosterone protect mice against lethal bacterial infections and lipopolysaccharide toxicity. J Med Microbiol 48, 425–431 (1999).
Gollisch, K. S. et al. Effects of exercise training on subcutaneous and visceral adipose tissue in normal- and high-fat diet-fed rats. Am J Physiol Endocrinol Metab 297, E495–504 (2009).
He, C. et al. Exercise-induced BCL2-regulated autophagy is required for muscle glucose homeostasis. Nature 481, 511–515 (2012).
Sharifnia, T. et al. Hepatic TLR4 signaling in obese NAFLD. Am J Physiol Gastrointest Liver Physiol 309, G270–278 (2015).
Charlton, M. et al. Low circulating levels of dehydroepiandrosterone in histologically advanced nonalcoholic fatty liver disease. Hepatology 47, 484–492 (2008).
Acknowledgements
This work was supported by in part by Grants-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology, Japan (No. 24650436, 24659104, 16H03255, and 17H02174).
Author information
Authors and Affiliations
Contributions
Substantial contribution to study concept and design: S.K., S.O., E.W., K.K., S.T., T.Y., and J.S.; data acquisition and analysis: S.K., K.A., and S.O.; data interpretation: S.K., K.A., E.W., K.I., and J.S.; article draft: S.K., E.W., K.I., and J.S.; article revision: S.O., K.K., S.T., and T.Y.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Komine, S., Akiyama, K., Warabi, E. et al. Exercise training enhances in vivo clearance of endotoxin and attenuates inflammatory responses by potentiating Kupffer cell phagocytosis. Sci Rep 7, 11977 (2017). https://doi.org/10.1038/s41598-017-12358-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-12358-8
This article is cited by
-
Physical fitness status modulates the inflammatory proteins in peripheral blood and circulating monocytes: role of PPAR-gamma
Scientific Reports (2020)
-
Influence of aerobic fitness on gastrointestinal barrier integrity and microbial translocation following a fixed-intensity military exertional heat stress test
European Journal of Applied Physiology (2020)
-
Protective effect of prebiotic and exercise intervention on knee health in a rat model of diet-induced obesity
Scientific Reports (2019)
-
Characterization of a murine nonalcoholic steatohepatitis model induced by high fat high calorie diet plus fructose and glucose in drinking water
Laboratory Investigation (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.