Abstract
Pancreatic β-cell insulin production is orchestrated by a complex circuitry involving intracellular elements including cyclic AMP (cAMP). Tackling aberrations in glucose-stimulated insulin release such as in diabetes with pharmacological agents, which boost the secretory capacity of β-cells, is linked to adverse side effects. We hypothesized that a photoactivatable adenylyl cyclase (PAC) can be employed to modulate cAMP in β-cells with light thereby enhancing insulin secretion. To that end, the PAC gene from Beggiatoa (bPAC) was delivered to β-cells. A cAMP increase was noted within 5 minutes of photostimulation and a significant drop at 12 minutes post-illumination. The concomitant augmented insulin secretion was comparable to that from β-cells treated with secretagogues. Greater insulin release was also observed over repeated cycles of photoinduction without adverse effects on viability and proliferation. Furthermore, the expression and activation of bPAC increased cAMP and insulin secretion in murine islets and in β-cell pseudoislets, which displayed a more pronounced light-triggered hormone secretion compared to that of β-cell monolayers. Calcium channel blocking curtailed the enhanced insulin response due to bPAC activity. This optogenetic system with modulation of cAMP and insulin release can be employed for the study of β-cell function and for enabling new therapeutic modalities for diabetes.
Similar content being viewed by others
Introduction
Precise control of complex cellular functions with external stimuli is essential for engineering effective cell therapeutics. Pharmacological manipulations typically exhibit poor cellular specificity and temporal control that is not harmonized with the timescale of relevant physiological processes. One such function is the glucose-stimulated insulin secretion (GSIS) by pancreatic β-cells that is central to blood glucose homeostasis. Aberrant insulin production is a hallmark of diabetes resulting from autoimmune destruction of β-cells (type 1 diabetes; T1D) or hormone resistance by tissues absorbing glucose (type 2 diabetes; T2D). GSIS in β-cells starts with the metabolism of glucose and the ATP/ADP-dependent closure of ATP-sensitive K+ (KATP) channels resulting in membrane depolarization and opening of the voltage-gated Ca2+ channels1. The influx of Ca2+ and increase of its concentration ([Ca2+]i) elicit exocytosis of insulin secretory granules. Of particular relevance to T2D treatment, hormone release can be boosted with secretagogues acting on intermediates of the insulin secretion circuitry in β-cells. Nonetheless, the lack of specificity in such treatments diminishes their effectiveness. For instance, sulfonylureas trigger the closure K+ ATP channels in β-cells and the ensuing membrane depolarization causes insulin secretion regardless of plasma glucose concentrations increasing the risk for hypoglycemic episodes2. K+ ATP channels are also found in other cell types (e.g. cardiomyocytes, non-vascular smooth muscle cells) making such treatments prone to additional side effects3.
To that end, optogenetic approaches have been employed for drug-free control with light of processes including neuronal cell activity4, contractility of cardiomyocytes5 and skeletal muscle cells6, and depolarization of retinal ganglion cells7. These strategies entail the creation of synthetic cellular circuits with light-activated molecules for the manipulation of signaling moieties thereby providing a handle on relevant functions. Optogenetic regulation of glucose homeostasis has been reported with the expression of bacterial channelrhodopsins (ChRs), which respond to light by inducing fluxes of specific ions. Human embryonic kidney 293 (HEK293) cells engineered to display melanopsin, expressed glucagon-like peptide-1 (GLP-1) from an endogenous factor of activated T cells (NFAT)-responsive promoter upon stimulation with blue light8. A return to normoglycemia was noted in diabetic mice after subcutaneous implantation of the engineered HEK293 cells. Along the same vein, others demonstrated the optogenetic control of Ca2+ influx in β-cells with the expression of ChRs9, 10. These results illustrate the feasibility of implementing optogenetic approaches to regulate blood glucose homeostasis. Nevertheless, the light- or agent-induced (e.g. by ionomycin11) increases in [Ca2+]i can lead to insulin secretion by β-cells in the absence of glucose pointing to the inherent risk imposed by ChR-based systems for hypoglycemic excursions.
Cyclic AMP (cAMP) is a major regulator12, 13 of GSIS through its effects on protein kinase A (PKA), the exchange protein activated by cAMP (Epac), and the recruitment of insulin vesicles and their secretion14. Intracellular cAMP ([cAMP]i) is synthesized from ATP by adenylyl cyclases (ACs) while phosphodiesterases (PDEs) are tasked with its rapid degradation. Consequently, AC activation (e.g. by forskolin) or PDE inhibition (e.g. by 3-isobutyl-1-methylxanthine; IBMX) augments GSIS. Incretins such as the GLP-1 and glucose-dependent insulinotropic polypeptide (GIP) released by intestinal cells elevate cAMP in islet β-cells to reduce postprandial blood glucose. While cAMP is an intracellular amplifier of GSIS, it does not induce the release of insulin in the absence of glucose in contrast to [Ca2+]i. As such, cAMP is an attractive target for boosting insulin production particularly in diabetes therapies15,16,17.
To that end, manipulation of cAMP using light has been demonstrated in Drosophila cells, Xenopus oocytes and HEK293 cells18 heterologously expressing photoactivatable ACs (PACs) from lower organisms19, 20. In this study, we hypothesized that β-cell insulin secretion can be controlled by modulating [cAMP]i with illumination. For this purpose, a PAC from the bacterium Beggiatoa (bPAC)20, 21 was expressed in vitro in murine islets and in β-cell lines, which closely mirror the functional attributes of native β-cells. We show that irradiation of bPAC expressed in β-cells elevates [cAMP]i enhancing insulin release, even over repeated cycles of stimulation with blue light. This augmented insulin secretion, which was evident both in monolayers and pseudoislets (PIs) of bPAC-expressing β-cells, was abolished in the presence of a Ca2+ channel blocker, indicating its dependence on Ca2+ influx in the same fashion as a typical GSIS response in islet cells.
Results
Expression of bPAC and [cAMP]i modulation in MIN6 β-cells
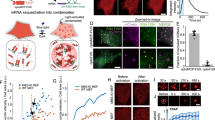
We set out to investigate if [cAMP]i and insulin release can be modulated via light in β-cells upon expression of the bPAC from Beggiatoa. An adenoviral vector, AdbPAC, was constructed for delivering the human codon-optimized bPAC to MIN6 β-cells. The myc tag (fused to the C-terminus of bPAC) and fluorescent protein mCherry were included in the cassette to facilitate the detection of bPAC (Fig. 1A,B). Based on immunostaining and fluorescence, the expression of mCherry was seemingly lower (Fig. 1A), which is typical for cistrons downstream of an IRES element22, 23. Indeed, the fraction of cells expressing bPAC was determined at different multiplicities of infection (MOI) either by immunostaining for the myc tag and microscopy or by flow cytometry for mCherry (Suppl. Fig. S1). Transduction levels increased to almost 55% for MOI of 100 with greater than 70% cell viability. When [cAMP]i was measured, we noted an increase that was commensurate with the bPAC expression based on the MOI (Fig. 1C). Cells infected at MOI of 100 displayed the highest [cAMP]i level with a 10-min photoinduction (8.59 ± 2.36 vs. 2.03 ± 0.53 (dark) ng cAMP/mg total protein, p = 0.035, n = 3).
Expression of bPAC confers light-induced modulation of [cAMP]i in MIN6 β-cells. (A) Fluorescence micrographs of AdbPAC-transduced cells (MOI = 100) stained for bPAC (antibody against the myc tag) and nuclear DNA (DAPI). Expressed mCherry (epifluorescence) is also shown. Bar: 100 µm. (B) Western blot showing the expression of bPAC (myc tag antibody) and β-actin. [cAMP]i levels are shown for various (C) MOI and (D) durations of pulsed (red bars) or continuous illumination (blue bars). Cells in (C) were illuminated for 10 min continuously. *p < 0.05 vs. dark, #p < 0.05 vs. cells infected at MOI of 10–50. Cells in (D) were infected at MOI = 100. *p < 0.05 vs. illumination for 5–20 min. In (C,D): NT: Non-transduced cells. (E) [cAMP]i levels after 10 min of illumination. Times after termination of the illumination are shown. *p < 0.05 vs. samples at 12–20 min. In (C–E): Dark: AdbPAC-infected cells (MOI = 100) without illumination. Results are shown as mean ± SD from at least three independent experiments, with each measurement carried out in triplicates. Some blots were edited for better (clear cut) representation. The entire blots are included in Supplementary Materials.
We also probed the relationship between the duration of illumination and increase in [cAMP]i (‘on’ kinetics). For this purpose, cultures transduced with AdbPAC were stimulated with continuous or pulsed light (5 s on/10 s off) for various durations between 1–20 min in 2.5 mM glucose (Fig. 1D). Compared to bPAC-expressing cells kept in dark, cells exposed to blue light for 5 min or longer exhibited a 6- to 8-fold increase in [cAMP]i. There was also no difference between the two modes of photostimulation in this setup. Conversely, the (‘off’) kinetics were determined of [cAMP]i reduction post-illumination (Fig. 1E). After a 10-min illumination, [cAMP]i levels returned to a stable baseline within 12 min albeit higher than for cells kept in dark (4.75 ± 0.78 vs. 1.99 ± 0.14 ng cAMP/mg total protein, p = 0.023, n = 3). Incubation of bPAC-expressing MIN6 β-cells with an AC inhibitor led to a reduction in the [cAMP]i (Suppl. Fig. S2) further illustrating that the observed increase in the secondary messenger is due to the action of bPAC upon photoactivation. Taken together, our data show that heterologous expression of bPAC in β-cells allows the on-demand alteration of [cAMP]i with light following physiologically relevant kinetics similar to [cAMP]i changes in islet β-cells exposed to changing concentrations of glucose24.
Insulin secretion in β-cells expressing bPAC
The light-mediated modulation of [cAMP]i in bPAC-expressing β-cells prompted us to investigate if insulin release could be regulated in an analogous manner. AdbPAC-transduced MIN6 β-cells at 2.5 mM of glucose secreted 131.65 ± 15.14 ng insulin/mg total protein/h (Fig. 2A) while the rate for non-transduced MIN6 β-cells was 34.97 ± 6.99 ng insulin/mg total protein/h (p = 2.74 × 10−3, n = 4). Similarly, bPAC-expressing cells at 25 mM glucose released 296.6 ± 63.25 vs. 87.57 ± 31.8 ng insulin/mg total protein/h (p = 6.91 × 10−3, n = 4) for control cells. Thus, blue light triggered an analogous increase (~3.5-fold) in bPAC-positive cells at low and high concentrations of glucose. In contrast, this increase was not observed in bPAC-expressing cells that were kept in dark. Of note, cells infected with AdGFP (control) did not differ in their hormone secretion from uninfected cells, suggesting that the adenoviral transduction did not affect the secretory function of β-cells. Additionally, the expression of bPAC and photostimulation augmented the rate of insulin release in another β-cell line (βTC cells; Suppl. Fig. S3), supporting the notion that the enhanced insulin secretion that we observed upon photoexposure of bPAC was not applicable only to MIN6 β-cells. The ratio of hormone secretion rates at 25 mM to 2.5 mM glucose was similar (~2.2–2.5) between cells expressing bPAC and those that did not suggesting that light-stimulated bPAC causes a surge in the rate of insulin release but at a constant ratio.
Insulin secretion by β-cells expressing bPAC. (A) MIN6 β-cells expressing bPAC displayed higher rates of insulin release (ng insulin/mg total protein/h) upon exposure to light compared to cells kept in dark and non-transduced cells or cells infected with AdGFP. MOI = 100; illumination for 30 min; *p < 0.05 vs. all other samples at 25 mM glucose; #p < 0.05 vs. all other samples at 2.5 mM glucose. (B) [cAMP]i and insulin secretion for MIN6 β-cells in the absence of glucose (MOI = 100); *p < 0.05 vs. all other samples. (C) Insulin secretion was determined in MIN6 β-cell monolayers (without bPAC expression) treated with various secretagogues at 2.5 or 25 mM glucose (see Materials and Methods). Results are shown as mean ± SD from at least three independent experiments.
These data show that elevation of [cAMP]i amplifies the secretion of insulin in the presence of glucose, even at 2.5 mM glucose, in bPAC-expressing MIN6 β-cells after activation with light. This behavior parallels the response of AdbPAC-transduced primary islets (see results in the next section) after photostimulation and is in support of a previous report indicating the resemblance in the regulation of insulin secretion between particular insulinoma lines and normal β-cells25.
Most transformed β-cell lines however exhibit hypersensitivity to glucose compared to primary β-cells26. This prompted us to measure the [cAMP]i and insulin secretion rate in the absence of glucose. Indeed, while AdbPAC-transduced MIN6 β-cells exhibited a significantly higher [cAMP]i after illumination (3.82 ± 0.3 vs. 2.17 ± 0.47 ng /mg total protein for cells without transduction; p = 3.3 × 10−3, n = 3), their insulin secretion was not different than that of the control cultures (Fig. 2B).
We also compared the enhanced hormone release due to treatment with blue light of bPAC-expressing cells with that resulting from incubation with various secretagogues (Fig. 2C). The responses were statistically similar even when cells were cultured with forskolin (AC activator) and IBMX (phosphodiesterase inhibitor), indicating that bPAC expression and activation by light mimics the amplifying effects of secretagogues on the insulin release by β-cells. Of note, the [cAMP]i levels of AdbPAC-transduced cells exposed to light were higher than for β-cells treated with forskolin or IBMX (Suppl. Fig. S4), suggesting that there may be an upper threshold in [cAMP]i above which there is no further significant increase in insulin secretion.
Transduced cells were also subjected to repeated cycles of light stimulation to assess the secretory capacity of β-cells over successive activations of bPAC and the potential effects on viability (Fig. 3A). Cells were stimulated with light every 12 h for 2 days. The rate of insulin release for bPAC-expressing cells exposed to light at 2.5 mM glucose remained constant and higher than for control cultures. After 36 h, insulin release was similar to that of the control cells most likely because of the ‘dilution effect’ caused by cell proliferation on the expressed transgene that was delivered with an adenoviral vector. Indeed, proliferation did not differ among non-transduced cells and bPAC-expressing cells stimulated with light or kept in the dark (Fig. 3B). Even the fractions of viable and apoptotic cells in these populations were similar after four repeated stimulations with blue light (Fig. 3C,D) suggesting that there were no adverse effects of cAMP modulation on the cell viability and proliferation.
Repeated stimulation of β-cells expressing bPAC. (A) Cells were illuminated with blue light every 12 hours for 2 days. Cells expressing bPAC (bPAC) displayed higher rates of insulin release (ng insulin/mg total protein/h) upon exposure to light vs. non-transduced MIN6 β-cells (control). MOI = 100; *p < 0.05 vs. control cells. (B) Proliferation, (C) cell viability and (D) apoptosis (TUNEL) of MIN6 β-cells expressing bPAC and stimulated with light (blue curve), kept in dark (red curve) or non-transduced cells (green). The time points correspond to those shown in (A) plus a final time point (48 h) at 12 hours after the last stimulation for insulin secretion. Results are shown as mean ± SD from at least three independent experiments.
Light-triggered enhancement of insulin release in murine islets and MIN6 β-cell pseudoislets expressing bPAC
In addition to β-cells lines, which represent relatively homogeneous β-cell populations, we determined the effect of bPAC activation in murine islets. Islets expressing bPAC and exposed to blue light for 30 min exhibited higher [cAMP]i both at 2.8 mM (1.82 ± 0.36 ng cAMP/mg total protein) and 20.2 mM (21.66 ± 5 ng cAMP/mg total protein) of glucose compared to islets not carrying the bPAC gene (0.28 ± 0.08 (2.8 mM) and 2.13 ± 0.62 (20.2 mM) ng cAMP/mg total protein; Fig. 4A). This translated to augmented insulin secretion for islets transduced with the AdbPAC (Fig. 4B). The insulin secretion rate of primary islets at 20.2 mM glucose was almost 5-fold higher than the corresponding rate at 2.8 mM glucose. This was not different (~4.5-fold) for islets transduced with AdGFP but was higher than for AdbPAC-expressing islets, which displayed greater insulin secretion rates both at 20.2 mM and 2.8 mM of glucose, i.e. 19.14 and 10.83 ng insulin/islet/h (p = 6.7 × 10−3, n = 3), respectively. The higher hormone release by AdbPAC-transduced islets vs. control islets at 2.8 mM was aligned with the higher [cAMP]i (Fig. 4A) similar to our observations with MIN6 β-cells described above. These findings also underline the amplifying role of cAMP on insulin secretion in the presence of glucose.
Expression of bPAC by murine islets and MIN6 β-cell PIs. (A) [cAMP]i content and (B) insulin secretion rate of murine islets without transduction (control) or transduced with AdbPAC or AdGFP. All islets were incubated with the stated concentration of glucose while exposed to blue light. *p < 0.01 AdbPAC-transduced vs. control islets in corresponding conditions. **p < 0.01, AdbPAC-transduced islets at 20.2 mM vs. 2.8 mM glucose. (C) Micrographs of PIs of MIN6 β-cells transduced with AdbPAC. Brightfield and epifluorescence (mCherry) images are shown. Bar: 100 µm. (D) The rate of insulin release by PIs of MIN6 β-cells expressing bPAC was higher upon illumination (30 min) with blue light (bPAC + light; MOI = 100) compared to PIs of regular MIN6 cells (control). *p < 0.05. For forskolin treatment: **, ***p < 0.05 vs. control and bPAC + light at 2.5 mM or 25 mM glucose, respectively. Treatment with IBMX, tolbutamide or KIC resulted in significantly higher release rates than those of the control samples (control; p < 0.05) for the corresponding glucose concentration but similar to those of PIs expressing bPAC and exposed to light.
Dispersed islet cells including primary and insulinoma β-cells re-organize into aggregates or ‘pseudoislets’ (PIs) exhibiting ultrastructural characteristics of native islets and higher GSIS27, 28 than monolayer cultures. We have shown that insulinoma PIs, which can be formed either in static or stirred-suspension cultures, respond to glucose and secretagogues with enhanced insulin secretion29. Thus, we questioned if this response could be further enhanced with photostimulation of PIs comprising β-cells expressing bPAC. To address this, MIN6 β-cells transduced with AdbPAC were cultured to form PIs (Fig. 4C). These PIs showed greater rates of insulin release upon illumination than PIs of control MIN6 β-cells both at 2.5 mM (439.32 ± 66.43 vs. 267.47 ± 41.05 ng insulin/mg total protein/h, p = 0.018, n = 3) and 25 mM of glucose (1048.82 ± 75.3 vs. 612.37 ± 31 ng insulin/mg total protein/h, p = 7.5 × 10−4, n = 3) (Fig. 4D). Of note, the ratio of rates at 25 mM over 2.5 mM of glucose was similar for PIs with (~2.4) or without (~2.3) the expression of bPAC analogous to our observations in monolayer cultures. The enhanced secretion of insulin at either glucose level by PIs of bPAC β-cells exposed to light was not different than that by PIs treated with IBMX, tolbutamide or KIC (Fig. 4D) but were lower compared to that of PIs incubated with forskolin (2.5 mM: 796.64 ± 148.92, p = 0.019; 25 mM: 1652.52 ± 264.88 ng insulin/mg total protein/h, p = 0.019, n = 3). Hence, insulin secretion can be modulated optogenetically in primary islets and β-cell PIs. We found in the latter that the enhancement achieved through blue light illumination is equivalent to that gained by treating PIs with known chemical secretagogues.
Optogenetic regulation of insulin release is Ca2+-dependent
The increase in β-cell [cAMP]i due to extracellular glucose elicits events leading to plasma membrane depolarization and opening of the L-type voltage-dependent Ca2+ channels that mediate ion influx, subsequent fusion of secretory vesicles and the secretion of the hormone. In fact, agents (e.g. KCl) that elevate [Ca2+]i in β-cells can trigger insulin secretion even in the absence of glucose. We thus wondered if the Ca+2 dependence is maintained during insulin secretion in our system given that photoactivation of bPAC induces an increase in [cAMP]i. Released insulin was measured in monolayer or PI cultures of bPAC-expressing cells upon incubation with nifedipine, a blocker of L-type Ca+2 channels (Fig. 5A). In monolayers, the inclusion of the Ca2+-channel blocker reduced the secretion rate by 47% and 40% at 2.5 and 25 mM glucose, respectively. Nifedipine treatment led to a similar decrease in PIs at 2.5 mM (45%) but the decline was less pronounced at 25 mM (27%). We also obtained evidence of the light-triggered changes in [Ca2+]i by analyzing ion influx after incubation with CaSiR-1. A greater increase in [Ca2+]i was noted in cells irradiated with blue light than in those cells kept in dark (Fig. 5B,C). Therefore, the insulin secretion is Ca2+-dependent in bPAC expressing-β-cells similar to native β-cells. Moreover, the blue light activation of bPAC results in [Ca2+]i increase aligned with the augmented insulin release by these cells.
Optogenetic enhancement of insulin release in bPAC-expressing MIN6 β-cells is Ca+2-dependent. (A) Insulin secretion rates for AdbPAC-transduced MIN6 β-cells in monolayers (left graph) or PIs (right graph). Light: Cells were illuminated for 30 min. *, **p < 0.05 vs. corresponding samples exposed to blue light in the absence of nifedipine at 2.5 mM or 25 mM glucose, respectively. (B) Effect of blue light irradiation on the [Ca2+]i of bPAC-expressing MIN6 β-cells exposed to 2.5 mM (left) or 25 mM glucose (right). The fluorescence intensities of irradiated (20 s; filled markers) and unirradiated cells (hollow markers) were measured for up to 200 s post-irradiation. The results are shown from representative experiments, as the ratio (percentage) of the change in fluorescence intensity from baseline (ΔF = F − Fo) to the baseline intensity (Fo). (C) As for (B) but presenting the area under the curve (AUC) from three independent experiments. ***p < 0.001.
Discussion
Exogenous regulation of [cAMP]i, which is an amplifier rather than an inducer of insulin secretion, is a promising avenue for enhancing β-cell function particularly for clinical applications. [cAMP]i levels are dictated mainly by cAMP synthesis and degradation by ACs and PDEs, respectively. In vivo AC activation with incretins to elevate [cAMP]i is hampered by their rapid clearance by dipeptidylpeptidase-4 (DPP4) and PDE inhibition is challenging because islet cells express multiple PDE types30, 31. Here, we describe the optogenetic regulation of [cAMP]i and thus of insulin secretion in β-cells. To our knowledge, control of insulin release via optogenetic modulation of [cAMP]i using a photoactivatable AC has not been demonstrated to date. In recent reports, ectopic expression of ChRs in MIN6 β-cells and islets led to changes in hormone secretion through light-triggered variations in Ca2+ influx9, 10. Interestingly, illumination induced the release of insulin by these cells in a manner that was independent of glucose metabolism. An almost 40% increase in insulin was noted after ChR stimulation in glucose-free medium9, and secretion was enhanced at low but not at high glucose concentrations9, 10. Moreover, ChRs require a ‘co-factor’ (retinal) for light-triggered activity, and the sequence of processes involving ChR-mediated [Ca2+]i increase, activation of gene transcription (e.g. GLP-18) and translation may result in a slower overall response. Furthermore, high-fat diet and fatty acids enhance [Ca2+]i 32, 33 making plausible the hypothesis that an exaggerated Ca2+ response could contribute to the initial hyperinsulinemia seen in T2D. This could confound the prospective regulation of Ca2+ signaling as a way to potentiate insulin production. Hence, targeting cAMP directly may be advantageous because its increase either by treatment with agents such as forskolin and IBMX or through bPAC activation with light amplifies GSIS. We observed that illumination of bPAC-expressing β-cells (MIN6, βTC) and primary islets resulted in increased secreted insulin even at low glucose concentrations but not in glucose-free medium. The observed response is aligned with the role of cAMP as an amplifier of insulin release in the presence of glucose. Indeed, no change in basal insulin release by MIN6 cells was noted in buffer devoid of glucose despite a raise in [cAMP]i due to bPAC activation. Therefore, this mode of amplification of the secretory function does not abolish control of glucose on insulin release in β-cells.
The augmented insulin production due to [cAMP]i elevation also points to a reduced number of β-cells or islets required – for instance, in a transplantation setting – to generate sufficient hormone amounts for glucose homeostasis. In fact, the secretion rate of bPAC-expressing β-cell monolayers or PIs was enhanced evenly and proportionally at 2.5 mM and 25 mM maintaining approximately the same constant ratio (2.2–2.5) as regular MIN6 cell monolayers or PIs. Such even increase in insulin secretion was not observed in primary islets. This insulin secretion ratio was lower after photoactivation of bPAC (~1.8) in primary islets compared to non-transduced islets (~5). This can be attributed to the pronounced enhancement of insulin release at 2.8 mM glucose with bPAC activation. Other factors however, may also need to be factored in such as a potential upper limit in the release of insulin at high glucose despite the significantly elevated [cAMP]i and the presence of other endocrine cells, which are also exposed to AdbPAC upon transduction of the islets.
When exposed to blue light for 30 minutes every 12 hours, AdbPAC-transduced MIN6 β-cells exhibited consistently higher insulin secretion over 36 hours but a slight decline was noted subsequently. Lower viability and enhanced apoptosis were ruled out as reasons for this decline. The reduction in insulin secretion, which was still on par with that from non-transduced MIN6 β-cells, was most likely due to a ‘dilution effect’ associated with the continuous cell proliferation and transient transgene expression. This issue can be addressed with the generation of β-cell lines stably expressing genes encoding for photoactivatable ACs.
The system also exhibited favorable kinetics with the [cAMP]i increasing within 5 minutes of photoactivation. This timeframe is comparable with that of [cAMP]i increase in murine β-cells within intact pancreatic islets following elevation of glucose concentration from 3 to 20 mM24. The [cAMP]i returned to a stable level within 8 minutes after illumination was terminated but was marginally higher than the baseline, i.e. for cells kept in dark. This did not affect the proliferation and viability of the cells over multiple cycles of stimulation. In fact, elevated [cAMP]i (e.g., after incretin stimulation) promotes β-cell proliferation through PKA-dependent mechanisms and suppresses apoptosis34, 35 partly due to the increased expression of the anti-apoptotic proteins Bcl-2 and Bcl-xL36, 37. Further studies are warranted about the potential long-term effects of optogenetic modulation of [cAMP]i on the β-cells.
To that end, β-cells engineered to express bPAC can be used as a tool for studying the role of [cAMP]i and its interaction with other signaling pathways in normal islets and those from diabetes patients. For instance, a bidirectional relation between [cAMP]i and [Ca2+]i fluctuations has been hypothesized although the exact mechanism remains unclear38. Also, maladaptation of cAMP signaling has been reported in several animal models of diabetes including decreased glucose-induced production of [cAMP]i 39 and lower expression of PDEs40. In vitro, prolonged culture of β-cells in high concentrations of glucose results in alterations in [cAMP]i activity41. Extensive β-cell juxtaposition seen in PIs increases cAMP responsiveness42 resulting in augmented GSIS compared to monolayer β-cell cultures as we and others have observed. These observations raise important questions, many of which can be potentially addressed using an optogenetic platform such as the one described here.
In addition to their value as a research tool, bPAC-expressing β-cells can be utilized, for example, as PIs, in a retrievable encapsulation device. This could be integrated into an autonomous bioartificial pancreas device with a low-power light source and existing glucose sensors (e.g. a wireless sensor fitted in a contact lens43) to control illumination. The blue light’s relatively poor tissue penetration is not expected to hinder the efficient stimulation of cells in this setup. Yet, the sensitivity of PACs can be shifted toward the infrared spectrum through protein engineering44. Additionally, available human β-cell lines45, 46 which are clinically more relevant than their rodent counterparts, can be modified for optogenetic regulation of cAMP. Beyond β-cell lines, human pluripotent stem cell (hPSC)-derived insulin-secreting cells may also be engineered to express PACs aiming at correcting defective GSIS, which is a major challenge in the generation of functional β-cells from hPSCs. Overall, optogenetic approaches such as the one presented here are expected to enable technologies which will enhance our understanding of β-cell physiology and contribute to biomedical solutions for pancreas pathologies.
Materials and Methods
Cell culture
Mouse MIN647 and βTC48 β-cells were maintained in DMEM containing 10% fetal bovine serum (FBS) (all from ThermoFisher Scientific, Waltham, MA) at 37 °C and 5% CO2. Cells were split 1:4 at 70–90% confluence. PIs were formed by seeding 2–5 × 104 cells/ml onto Petri dishes or 105 cells/ml in 125-ml ProCulture spinner flasks29 (Corning, NY). In spinner flask PI cultures, half-volume medium changes were performed every 2–3 days. AD293 cells (Cell Biolabs Inc., San Diego, CA) used for recombinant adenovirus production were cultured in the same medium as above but supplemented with 1% MEM non-essential amino acids (ThermoFisher). Cell viability was determined by Trypan Blue staining (ThermoFisher) using a hemocytometer or a TC20 counter (Bio-Rad Laboratories, Hercules, CA).
Murine islet isolation and culture
An abdominal incision was performed to 8-week old male C57BL/6 mice under anesthesia to access the pancreas, which was inflated and harvested. Digestion was carried out with collagenase (CIzyme RI from Vitacyte, Indianapolis, IN). Gradient centrifugation and gravity sedimentation of islets were carried out in lymphocyte separation medium (Corning) and Hank’s balanced salt solution (ThermoFisher). Islets were handpicked under a microscope, counted and cultured in RPMI 1640 (MP Biomedicals, Santa Ana, CA) supplied with 10% FBS (ThermoFisher) in Petri dishes at 37 °C and 5% CO2. Intact islets underwent two rounds of adenoviral transduction (MOI as stated, ~1,500 cells/islet) 48 h apart.
bPAC gene and adenovirus construction
A human-codon optimized bPAC gene was synthesized (GeneArt, ThermoFisher) from the available bPAC sequence (accession number: GU461306.2)21. A cMyc-derived epitope (myc tag: EQKLISEEDL) was added to the C-terminus of bPAC followed by an internal ribosomal entry site (IRES) sequence, the mCherry gene and the SV40 polyA tail. The bPAC-cMyc-IRES-mCherry cassette was inserted into the pShuttle-CMV vector for generation of an adenovirus (AdbPAC) in 293AD cells with the AdEasy system (Agilent Technologies, Santa Clara, CA)49. The AdGFP adenovirus carrying the GFP gene under the CMV promoter was obtained from the Baylor College of Medicine Vector Development Core (Houston, TX). Purification and titer determination of the adenoviral particles were carried out using the ViraBind and QuickTiter kits (Cell Biolabs), respectively. For AdbPAC propagation, 293AD cells were transduced at 70% confluence.
Arduino-driven LED arrays for blue light stimulation
Arrays were constructed with 6 or 12 LEDs (470 nm; Mouser Electronics, Mansfield, TX) for stimulation of cells cultured in 6- or 12-well plates. For control of its operation, each array was connected to an Arduino board (Adafruit, New York, NY) that was programmed accordingly. In this configuration, the light power on the culture surface was 0.18 mW/mm2 measured with a S120C sensor connected to PM100D light meter (Thorlabs Inc., Newton, NJ). For pulsed stimulation the light cycle was 5 sec on/10 sec off.
[cAMP]i and secreted insulin assays
[cAMP]i and secreted insulin were determined typically 48 h after transduction. For experiments with murine islets, between 8–20 islets (per well of 24-well plate) were used for each condition. Medium was replaced with Krebs-Ringer bicarbonate buffer (KRB (mM): 129 NaCl; 4.8 KCl; 1.2 KH2PO4; 1.2 MgSO4; 2.5 CaCl2; 5 NaHCO3; 10 HEPES, pH = 7.2) with 0.1% BSA and 2.5 mM glucose. After 3 h, the buffer was replaced with fresh KRB with no glucose, 2.5 mM (cells/PIs) or 2.8 mM (murine islets) (basal level) and 25 mM (cells/PIs) or 20.2 mM (murine islets) glucose (supraphysiological level) as stated and cells/islets were further incubated with or without illumination. At the same time, the AC inhibitor MDL12330A50 (100 μM; Sigma-Aldrich, St. Louis, MO), L-type Ca2+ blocker nifedipine (10 µM; Abcam, Cambridge, MA) or secretagogues (all from Sigma-Aldrich) were also added as stated: 10 µM forskolin, 10 µM 3-isobutyl-1-methylxanthine (IBMX), 500 nM phorbol 12-myristate 13-acetate (PMA), 100 µM tolbutamide and 15 mM ketoisocaproate (KIC). Cells were lysed at different times in 0.1 M HCl for determination of [cAMP]i via enzyme-linked immunosorbent assay (ELISA; Cayman Chemical Co., Ann Arbor, MI) following the manufacturer’s instructions. Supernatant was collected and analyzed for secreted insulin by ELISA (EMD Millipore, Billerica, MA) as described29. Insulin and [cAMP]i measurements were normalized with the total protein content of the corresponding cell lysates determined via the Bradford method (ThermoFisher). Of note, insulin secretion for primary islets was normalized with respect to the number of islets utilized.
Experiments involving multiple cycles of stimulation with light, were initiated 48 h post-transduction. For this purpose, the following procedure was repeated every 12 h: The culture medium in all wells of 12-well plates was replaced with KRB containing 2.5 mM glucose and cells were incubated for 2 h. Then, KRB was removed and fresh KRB with 2.5 mM glucose was added for 30 min along with or without blue light illumination. Subsequently, supernatants and cells were collected from at least 3 wells for determination of secreted insulin and total protein (as described above). The buffer in the remaining wells was replaced with fresh culture medium and the procedure was repeated 12 h later for up to 2 days.
In these experiments, cell numbers and the fractions of live (Trypan Blue; see above) and apoptotic cells (TUNEL assay; see below) were determined from samples collected before the exchange of medium with KRB.
TUNEL assay
DNA fragmentation-related apoptosis was assessed by terminal deoxynucleotidyl transferase dUTP nick-end labeling (TUNEL) using the FlowTACS apoptosis detection kit (Trevigen) according to the manufacturer’s instructions as we reported29. Briefly, cells in aliquots were fixed with 3.7% formaldehyde for 10 min and stained with 10 μg/ml propidium iodide in PBS for 5 min. Then, the samples were permeabilized with cytonin for 30 min, labeled with terminal deoxynucleotidyl transferase (TdT) for 40 min at 37 °C and incubated with a streptavidin–FITC antibody in the dark for 10 min. After two washes with PBS, the samples were analyzed via flow cytometry. Appropriate gating was applied to screen out cellular debris and cell clumps. Positive (cells treated with nuclease) and negative (cells without TdT primary antibody incubation) controls were used to set up bins for apoptotic, and non-apoptotic ranges.
Immunocytochemistry
Cells were fixed with 4% paraformaldehyde (Sigma) in PBS for 20 min, permeabilized/blocked in PBS with 0.1% Triton X-100 (Mallinckrodt Baker, Phillipsburg, NJ) and 1% bovine serum albumin (BSA; Sigma) for 30 min and incubated overnight at 4 °C with a rabbit antibody against the myc epitope (cat. no. 2272, Cell Signaling Technology, Danvers, MA). After three washes with PBS, cells were incubated with a donkey anti-rabbit secondary antibody conjugated to Alexa 488 (Jackson Immunoresearch Laboratories Inc., West Grove, PA) for 1 h at room temperature. Nuclear DNA was stained with DAPI (Vectashield, Vector Laboratories, Burlingame, CA). Images were acquired with a Leica TCS SPE confocal microscope (Leica Microsystems Inc., Buffalo Grove, IL) and quantitative analysis was performed with the Leica LAS X software. Images from at least 10 separate fields per experiment were used for analysis.
Western blot analysis
Cells were lysed in radioimmunoprecipitation (RIPA) buffer supplemented with a protease inhibitor cocktail (EMD Biosciences, CA) for 30 min and total protein was determined (Bradford; ThermoFisher). Cell lysates were boiled for 5 min at 95 °C, loaded to a sodium dodecyl sulfate-polyacrylamide gel (30 μg of total protein/lane) and after gel electrophoresis and protein transfer to polyvinylidene difluoride (PVDF) membranes (Thermo Fisher Scientific), the membranes were blocked with 5% milk in Tris-buffered saline with 0.05% Tween-20 (TBS/T) for 1 h at room temperature. After 3 washes with TBS/T, the membranes were incubated with primary antibodies against myc-tag (Cell Signaling Technology) and β-actin (cat. no. A1978, Sigma) in a shaker at 4 °C overnight. Following 3 more TBS/T washes, secondary horseradish peroxidase (HRP)-conjugated antibodies (Jackson ImmunoResearch Laboratories Inc.) were added for 1 h at room temperature. Membranes were washed 3 times and proteins were detected in a C-DiGit blot scanner after adding WesternSure ECL substrate (Li-Cor Biotechnology, Lincoln, NE).
Intracellular Ca2+ measurement
Cells were washed once with Hank’s Balanced Salt Solution (HBSS) and loaded with the calcium indicator CaSiR-1 acetoxymethyl ester (Goryo Chemical Inc., Sapporo, Japan) (5 μM final concentration) at 37 °C for 20 min in the dark51 according the manufacturer’s instructions. The loading solution was then replaced with KRB containing 2.5 mM or 25 mM glucose. Cells were placed on a Leica TCS SPE confocal microscope (Leica Microsystems Inc., Buffalo Grove, IL) and irradiated with a 488-nm laser light for 20 s immediately followed by the recording of fluorescence intensity in the range of 650–750 nm (emitted light) after excitation with a far-red (635 nm) laser light. Cells in each field were selected based on mCherry fluorescence (excitation with a 532-nm laser) and analyzed using the Leica LAS X software. Between 20–30 cells were analyzed per sample. A region of interest was defined for each cell and the average fluorescent intensity was calculated. These intensities were averaged over all mCherry-positive cells. Average intracellular Ca2+ levels were quantified as the change in average fluorescence intensity at different time points above the initial fluorescence (ΔF = F − Fo) divided by the initial intensity (Fo). The area under the curve (AUC) was calculated from temporal data of ΔF/Fo via a script in MATLAB (Mathworks, Natick, MA).
Statistical analysis
Results are expressed as mean ± standard deviation (SD) from at least 3 independent experiments with each experimental point analyzed in triplicates. Analysis of variance and the posthoc Tukey test were performed using Prism 7 (GraphPad Software, Inc., La Jolla, CA). Values of p < 0.05 were considered as significant.
References
Henquin, J. C. Triggering and amplifying pathways of regulation of insulin secretion by glucose. Diabetes 49, 1751–1760 (2000).
Doyle, M. E. & Egan, J. M. Pharmacological agents that directly modulate insulin secretion. Pharmacol Rev 55, 105–131, doi:10.1124/pr.55.1.7 (2003).
Stephan, D., Winkler, M., Kuhner, P., Russ, U. & Quast, U. Selectivity of repaglinide and glibenclamide for the pancreatic over the cardiovascular K(ATP) channels. Diabetologia 49, 2039–2048, doi:10.1007/s00125-006-0307-3 (2006).
Deisseroth, K. et al. Next-generation optical technologies for illuminating genetically targeted brain circuits. J Neurosci 26, 10380–10386, doi:10.1523/JNEUROSCI.3863-06.2006 (2006).
Bingen, B. O. et al. Light-induced termination of spiral wave arrhythmias by optogenetic engineering of atrial cardiomyocytes. Cardiovasc Res 104, 194–205, doi:10.1093/cvr/cvu179 (2014).
Sakar, M. S. et al. Formation and optogenetic control of engineered 3D skeletal muscle bioactuators. Lab Chip 12, 4976–4985, doi:10.1039/c2lc40338b (2012).
Busskamp, V. & Roska, B. Optogenetic approaches to restoring visual function in retinitis pigmentosa. Curr Opin Neurobiol 21, 942–946, doi:10.1016/j.conb.2011.06.001 (2011).
Ye, H., Daoud-El Baba, M., Peng, R. W. & Fussenegger, M. A synthetic optogenetic transcription device enhances blood-glucose homeostasis in mice. Science 332, 1565–1568, doi:10.1126/science.1203535 (2011).
Kushibiki, T., Okawa, S., Hirasawa, T. & Ishihara, M. Optogenetic control of insulin secretion by pancreatic beta-cells in vitro and in vivo. Gene Ther 22, 553–559, doi:10.1038/gt.2015.23 (2015).
Reinbothe, T. M., Safi, F., Axelsson, A. S., Mollet, I. G. & Rosengren, A. H. Optogenetic control of insulin secretion in intact pancreatic islets with beta-cell-specific expression of Channelrhodopsin-2. Islets 6, e28095, doi:10.4161/isl.28095 (2014).
Bernal-Mizrachi, E. et al. Defective insulin secretion and increased susceptibility to experimental diabetes are induced by reduced Akt activity in pancreatic islet beta cells. J Clin Invest 114, 928–936, doi:10.1172/JCI20016 (2004).
Samols, E., Marri, G. & Marks, V. Promotion of Insulin Secretion by Glucagon. Lancet 2, 415–416 (1965).
Malaisse, W. J., Malaisse-Lagae, F. & Mayhew, D. A possible role for the adenylcyclase system in insulin secretion. J Clin Invest 46, 1724–1734, doi:10.1172/JCI105663 (1967).
Seino, S. & Shibasaki, T. PKA-dependent and PKA-independent pathways for cAMP-regulated exocytosis. Physiol Rev 85, 1303–1342, doi:10.1152/physrev.00001.2005 (2005).
Furman, B., Pyne, N., Flatt, P. & O’Harte, F. Targeting beta-cell cyclic 3′5′ adenosine monophosphate for the development of novel drugs for treating type 2 diabetes mellitus. A review. The Journal of pharmacy and pharmacology 56, 1477–1492, doi:10.1211/0022357044805 (2004).
Ahren, B. Islet G protein-coupled receptors as potential targets for treatment of type 2 diabetes. Nature reviews. Drug discovery 8, 369–385, doi:10.1038/nrd2782 (2009).
Lovshin, J. A. & Drucker, D. J. Incretin-based therapies for type 2 diabetes mellitus. Nat Rev Endocrinol 5, 262–269, doi:10.1038/nrendo.2009.48 (2009).
Schroder-Lang, S. et al. Fast manipulation of cellular cAMP level by light in vivo. Nature methods 4, 39–42, doi:10.1038/nmeth975 (2007).
Iseki, M. et al. A blue-light-activated adenylyl cyclase mediates photoavoidance in Euglena gracilis. Nature 415, 1047–1051, doi:10.1038/4151047a4151047a (2002).
Ryu, M. H., Moskvin, O. V., Siltberg-Liberles, J. & Gomelsky, M. Natural and engineered photoactivated nucleotidyl cyclases for optogenetic applications. The Journal of biological chemistry 285, 41501–41508, doi:10.1074/jbc.M110.177600 (2010).
Stierl, M. et al. Light modulation of cellular cAMP by a small bacterial photoactivated adenylyl cyclase, bPAC, of the soil bacterium Beggiatoa. The Journal of biological chemistry 286, 1181–1188, doi:10.1074/jbc.M110.185496 (2011).
Hennecke, M. et al. Composition and arrangement of genes define the strength of IRES-driven translation in bicistronic mRNAs. Nucleic Acids Res 29, 3327–3334 (2001).
Thompson, S. R. So you want to know if your message has an IRES? Wiley Interdiscip Rev RNA 3, 697–705, doi:10.1002/wrna.1129 (2012).
Tengholm, A. Cyclic AMP dynamics in the pancreatic beta-cell. Ups J Med Sci 117, 355–369, doi:10.3109/03009734.2012.724732 (2012).
D’Ambra, R., Surana, M., Efrat, S., Starr, R. G. & Fleischer, N. Regulation of insulin secretion from beta-cell lines derived from transgenic mice insulinomas resembles that of normal beta-cells. Endocrinology 126, 2815–2822, doi:10.1210/endo-126-6-2815 (1990).
Efrat, S. Regulation of insulin secretion: insights from engineered beta-cell lines. Ann N Y Acad Sci 1014, 88–96 (2004).
Hopcroft, D. W., Mason, D. R. & Scott, R. S. Structure-function relationships in pancreatic islets: support for intraislet modulation of insulin secretion. Endocrinology 117, 2073–2080 (1985).
Hauge-Evans, A. C., Squires, P. E., Persaud, S. J. & Jones, P. M. Pancreatic beta-cell-to-beta-cell interactions are required for integrated responses to nutrient stimuli: enhanced Ca2+ and insulin secretory responses of MIN6 pseudoislets. Diabetes 48, 1402–1408 (1999).
Lock, L. T., Laychock, S. G. & Tzanakakis, E. S. Pseudoislets in stirred-suspension culture exhibit enhanced cell survival, propagation and insulin secretion. J Biotechnol 151, 278–286, doi:10.1016/j.jbiotec.2010.12.015 (2011).
Waddleton, D. et al. Phosphodiesterase 3 and 4 comprise the major cAMP metabolizing enzymes responsible for insulin secretion in INS-1 (832/13) cells and rat islets. Biochem Pharmacol 76, 884–893, doi:10.1016/j.bcp.2008.07.025 (2008).
Heimann, E. et al. Expression and regulation of cyclic nucleotide phosphodiesterases in human and rat pancreatic islets. PloS one 5, e14191, doi:10.1371/journal.pone.0014191 (2010).
Remizov, O. et al. Palmitate-induced Ca2+ -signaling in pancreatic beta-cells. Mol Cell Endocrinol 212, 1–9 (2003).
Gonzalez, A. et al. Insulin hypersecretion in islets from diet-induced hyperinsulinemic obese female mice is associated with several functional adaptations in individual beta-cells. Endocrinology 154, 3515–3524, doi:10.1210/en.2013-1424 (2013).
Hui, H., Nourparvar, A., Zhao, X. & Perfetti, R. Glucagon-like peptide-1 inhibits apoptosis of insulin-secreting cells via a cyclic 5′-adenosine monophosphate-dependent protein kinase A- and a phosphatidylinositol 3-kinase-dependent pathway. Endocrinology 144, 1444–1455, doi:10.1210/en.2002-220897 (2003).
Granata, R. et al. Acylated and unacylated ghrelin promote proliferation and inhibit apoptosis of pancreatic beta-cells and human islets: involvement of 3′,5′-cyclic adenosine monophosphate/protein kinase A, extracellular signal-regulated kinase 1/2, and phosphatidyl inositol 3-Kinase/Akt signaling. Endocrinology 148, 512–529, doi:10.1210/en.2006-0266 (2007).
Kim, S. J., Nian, C., Widenmaier, S. & McIntosh, C. H. Glucose-dependent insulinotropic polypeptide-mediated up-regulation of beta-cell antiapoptotic Bcl-2 gene expression is coordinated by cyclic AMP (cAMP) response element binding protein (CREB) and cAMP-responsive CREB coactivator 2. Mol Cell Biol 28, 1644–1656, doi:10.1128/MCB.00325-07 (2008).
Furman, B., Ong, W. K. & Pyne, N. J. Cyclic AMP signaling in pancreatic islets. Advances in experimental medicine and biology 654, 281–304, doi:10.1007/978-90-481-3271-3_13 (2010).
Borodinsky, L. N. & Spitzer, N. C. Second messenger pas de deux: the coordinated dance between calcium and cAMP. Sci STKE 2006, pe22, doi:10.1126/stke.3362006pe22 (2006).
Dachicourt, N., Serradas, P., Giroix, M. H., Gangnerau, M. N. & Portha, B. Decreased glucose-induced cAMP and insulin release in islets of diabetic rats: reversal by IBMX, glucagon, GIP. The American journal of physiology 271, E725–732 (1996).
Dolz, M. et al. cAMP-secretion coupling is impaired in diabetic GK/Par rat β-cells: a defect counteracted by GLP-1. American Journal of Physiology - Endocrinology And Metabolism 301, E797–E806, doi:10.1152/ajpendo.00652.2010 (2011).
Roger, B. et al. Adenylyl cyclase 8 is central to glucagon-like peptide 1 signalling and effects of chronically elevated glucose in rat and human pancreatic beta cells. Diabetologia 54, 390–402, doi:10.1007/s00125-010-1955-x (2011).
Iwasaki, M. et al. Establishment of new clonal pancreatic beta-cell lines (MIN6-K) useful for study of incretin/cyclic adenosine monophosphate signaling. J Diabetes Investig 1, 137–142, doi:10.1111/j.2040-1124.2010.00026.x (2010).
Honore, F., Otis, B. & Nelson, A. Reader communication with contact lens sensors and display device. US 09128305 (2015).
Ryu, M. H. et al. Engineering adenylate cyclases regulated by near-infrared window light. Proc Natl Acad Sci U S A 111, 10167–10172, doi:10.1073/pnas.1324301111 (2014).
Ravassard, P. et al. A genetically engineered human pancreatic beta cell line exhibiting glucose-inducible insulin secretion. J Clin Invest 121, 3589–3597, doi:10.1172/JCI58447 (2011).
Scharfmann, R. et al. Development of a conditionally immortalized human pancreatic beta cell line. J Clin Invest 124, 2087–2098, doi:10.1172/JCI72674 (2014).
Miyazaki, J. I. et al. Establishment of a Pancreatic Beta-Cell Line That Retains Glucose-Inducible Insulin-Secretion - Special Reference to Expression of Glucose Transporter Isoforms. Endocrinology 127, 126–132 (1990).
Efrat, S. et al. Beta-cell lines derived from transgenic mice expressing a hybrid insulin gene-oncogene. Proc Natl Acad Sci U S A 85, 9037–9041 (1988).
Jing, D., Kehoe, D. E. & Tzanakakis, E. S. Expression of Reg family proteins in embryonic stem cells and its modulation by Wnt/beta-catenin signaling. Stem Cells Dev 19, 1307–1319, doi:10.1089/scd.2009.0398 (2010).
Borner, S. et al. FRET measurements of intracellular cAMP concentrations and cAMP analog permeability in intact cells. Nat Protoc 6, 427–438, doi:10.1038/nprot.2010.198 (2011).
Egawa, T. et al. Development of a far-red to near-infrared fluorescence probe for calcium ion and its application to multicolor neuronal imaging. J Am Chem Soc 133, 14157–14159, doi:10.1021/ja205809h (2011).
Acknowledgements
Funding support has been provided by the National Science Foundation (NSF; CBET-1547785, CBET-1603524) to EST. We thank the laboratory of Dr. Gordon Weir (Joslin Diabetes Center, Boston, MA) for technical assistance with the isolation of murine islets. We express our appreciation to members of the Tzanakakis laboratory for discussions and comments during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
F.Z. conducted experimental procedures. E.S.T. directed the study and designed the experiments. F.Z. and E.S.T. wrote the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, F., Tzanakakis, E.S. Optogenetic regulation of insulin secretion in pancreatic β-cells. Sci Rep 7, 9357 (2017). https://doi.org/10.1038/s41598-017-09937-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-09937-0
This article is cited by
-
PACmn for improved optogenetic control of intracellular cAMP
BMC Biology (2021)
-
The C-terminal region affects the activity of photoactivated adenylyl cyclase from Oscillatoria acuminata
Scientific Reports (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.