Abstract
Thoracic ossification of the ligamentum flavum (TOLF) complicated with dural ossification (DO) is a severe clinical disease. The diagnosis of DO preoperatively remains challenging. The current study retrospectively analyzed imaging features of 102 segments with TOLF from 39 patients and proposed a grading system for evaluating DO risk. Logistic regression results showed that unilateral spinal canal occupational rate (UCOR), tram track signs, and C-signs were all risk factors for DO (odds ratios of 5.393, 19.734 and 72.594, respectively). In validation analyses for the TOLF-DO grading system, sensitivity was 76.0% (19/25), specificity was 91.0% (70/77), and Youden’s index was 0.66. Thus, implementation of the TOLF-DO grading system has the potential to improve the diagnosis of DO.
Similar content being viewed by others
Introduction
Thoracic ossification of the ligamentum flavum (TOLF) complicated with dural ossification (DO) is an uncommon but severe clinical entity1,2,3,4. The pathogenesis of DO remains unclear at present. The diagnosis of DO usually depends on the finding of an “ossified mass” unseparated from the dural sac during operation. Surgical treatment for TOLF-DO is more difficult and risky than simple TOLF5,6,7,8,9. If the presence of DO can be confirmed preoperatively, the safety of the surgical procedure can be ensured to a greater extent. However, it is still difficult to confirm the diagnosis of DO preoperatively based on patient history, clinical observation, and imaging presentation.
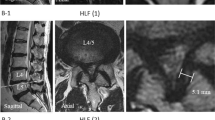
Imaging research regarding TOLF-DO is relatively rare. Muthukumar et al.10 and Sun et al.11 reported that the presence of a “tram track sign” (i.e., a hyperdense bony excrescence with a hypodense center) or “comma sign” (i.e., evidence of ossification of one-half of the circumference of the dura mater) on transverse computed tomography (CT) or magnetic resonance imaging (MRI) scans was significant for the diagnosis of DO. In retrospective case data, both tram track signs and comma signs could be seen in the imaging of TOLF-DO patients. In clinical practice, the ossified mass of the TOLF-DO segment is frequently hypertrophied, while the less hypertrophic adjacent segments are usually not complicated with DO. This pattern suggests that the degree of hypertrophy in the ossified mass may be associated with the occurrence of DO.
In the present study, we retrospectively analyzed imaging features of the segments definitely affected by TOLF-DO and compared them to those of TOLF patients without DO. Based on the statistical results, we propose a grading system for evaluating DO risk and offer this system as a practical tool for the diagnosis of TOLF-DO.
Results
Demographic and clinical characteristics
The study sample included a total of 102 segments with TOLF from 39 patients. Twenty-five of these segments were diagnosed with TOLF-DO, and the other 77 segments were diagnosed as TOLF without DO (TOLF-NDO). The morphological features of the involved segments were observed on bone-window CT transverse images. DO segment locations are listed in Table 1.
The percentage of patients with TOLF-DO in our series of patients was 41.0% (16/39), and the percentage of segments affected by TOLF-DO was 24.5% (25/102). T9–T12 were the segments most commonly affected by DO, accounting for 64% of DO cases (16/25).
TOLF-DO Grading system
We divided unilateral spinal canal occupational rate (UCOR) measurements for 102 TOLF segments into four ranges (0–50%, 50–59%, 60–69%, and 70–100%). The incidence of DO increased gradually with increases in UCOR values. For UCOR values ≥ 60%, the incidence rate of TOLF-DO was higher than that of TOLF-NDO. Tram track sign and C-sign rates in DO segments were also higher than in NDO segments (Fig. 1).
Logistic regression results indicated that UCOR, tram track sign and C-sign were all risk factors for DO (Table 2). Based on odds ratios calculated from this model, we designed a TOLF-DO grading system (Table 3). The system comprised 4 total points, and the existence of DO was highly suspected when the score was greater than 2 points.
Clinical validation of the TOLF-DO grading system
Figure 2 displays the distribution of TOLF-DO risk scores across the 102 segments. Table 2 displays the results of the logistic regression analysis. Tram track sign, C-sign and UCOR ≥ 60% were all risk factors for DO. Table 4 lists diagnostic outcomes for the TOLF-DO grading system and intraoperative diagnosis.
Discussion
TOLF-DO is not uncommon in TOLF. Clinical data in the current study suggested that the incidence of TOLF-DO was 41.0%, compared to estimates of 14% to 61% in previous literature2,3,4, 12, 13. DO often occurs at lower thoracic segments, and the affected region was located at T9–12 for 16 of the 25 segments in our series. Other studies have also reported DO most frequently at T9–12. This region is also the preferred site for TOLF14,15,16.
We retrospectively reviewed CT bone window imaging data for 102 TOLF segments. “Comma signs” had more diagnostic value than “tram track signs” for TOLF-DO. The tram track sign was observed in 17 segments, but the “C-sign” was observed in only one TOLF-NDO segment. The relationship between tram track signs and DO thus requires further clarification. Some researchers have found that a layered presentation (i.e., double-layer sign) in the ossified mass of the posterior longitudinal ligament (OPLL) or a C-shaped (C-sign) high-density ossified zone on the side of the dura is valuable for the diagnosis of DO17,18,19. The low-density zone in the double-layer sign has been explained as an immature ossified ligament20, 21 in the ossified mass. The double-layer sign also indicates that OPLL originates from the dura-side ligament, which increases the possibility that it is accompanied by DO16, 18, 22. Although tram track sign is not a unique imaging feature of TOLF-DO, the existence of DO should be highly suspected in cases where the C-sign is observed. Accordingly, the proposed grading system highlights the diagnostic value of C-sign in DO.
The incidence of DO is apparently correlated with the progress of TOLF23. DO was not observed when the UCOR value was lower than 40%; in contrast, the risk of DO increased significantly when UCOR was at least 60%. To date, no studies have reported a correlation between the occurrence of DO and the thickness of the ossified mass. More TOLF patients are needed to validate the diagnostic significance of TOLF-DO. There is no uniform method to measure COR values in TOLF. The simple and practical measurement of UCOR values for TOLF that we recommend in this study was based on the origin and progression of OLF.
The TOLF-DO grading system had a high specificity (91%) for the diagnosis of DO. For scores less than 2 points, the existence of DO was not suspected. In contrast, the sensitivity was 76%, indicating a 24% rate of missed DO diagnoses. According to the distribution of UCOR values, 10 segments in the 12 cases with UCOR ≥ 70% were diagnosed with DO. We did not evaluate the grading system for UCOR values ≥ 70% because the number of cases meeting this criterion was relatively small. However, according to our clinical experience, the presence of DO should be highly suspected when UCOR values exceed 70%.
The grading system setting and clinical validation were both based on a relatively small number of cases. The feasibility and significance of applying this system to the diagnosis of DO require further investigation with larger sample sizes and in multicenter clinical studies.
Methods
Ethics statement
The treatment protocol and informed consent were approved by the Shanghai Changzheng Hospital Institutional Review Board, and all subjects gave informed consent. All methods were performed in accordance with the Declaration of Helsinki.
CT Imaging examination
Tram track sign and C-sign
The TTS is a hyperdense bony excrescence with a hypodense center (Fig. 3a)10. The edges of the bilateral dura-side ossified mass are curved, forming a “C” sign (Fig. 3b). The C-sign includes all the manifestations of the comma sign10.
Measurement of unilateral spinal canal occupational rate (UCOR) for the ossified mass
OR severity was measured on CT transverse images. The ossified mass of the OLF originates from the bilateral laminae and facet joints, and it then spreads to the midline and posterior vertebral wall. The maximum thickness of the unilateral ossified mass (d) and the distance from the lamina to the midpoint of the posterior vertebral wall (D) were measured. The ratio of d/D was calculated, and the larger value was set as the UCOR (Fig. 4).
Establishment and clinical validation of the TOLF-DO Grading system
Logistic regression was used to evaluate risk factors for TOLF-DO. According to odds ratios for multiple risk factors, we established a TOLF-DO grading system for evaluating risk for DO.
The 102 TOLF segments were evaluated using the TOLF-DO grading system. Intraoperative diagnosis was used as the gold standard. The sensitivity and specificity of the grading system for diagnosis of TOLF-DO were calculated.
Statistical Analysis
Multivariate analyses of risk factors for TOLF-DO were carried out with logistic regression to determine odds ratios (OR) and their 95% confidence intervals (95% CI). A two-tailed P value less than 0.05 was regarded as statistically significant. All statistical analyses were performed using SPSS (version 18.0, SPSS Inc., Chicago, IL).
References
Nishiura, I., Isozumi, T. & Nishihara, K. et al. Surgical approach to ossification of the thoracic yellow ligament. Surg Neurol. 51, 368–372 (1999).
Wang, T., Yin, C., Wang, D. et al. Surgical Technique for Decompression of Severe Thoracic Myelopathy Due to Tuberous Ossification of Ligamentum Flavum. Clin Spine Surg. doi:10.1097/BSD.0000000000000213 (2016).
Yang, Z., Xue, Y. & Zhang, C. et al. Surgical treatment of ossification of the LF associated with dural ossification in the thoracic spine. J Clin Neurosci. 20, 212–6 (2013).
Sun, J., Zhang, C. & Ning, G. et al. Surgical strategies for ossified LF associated with dural ossification in thoracic spinal stenosis. J Clin Neurosci. 21, 2102–6 (2014).
Ando, K., Imagama, S. & Ito, Z. et al. Predictive factors for a poor surgical outcome with thoracic ossification of the LF by multivariate analysis: a multicenter study. Spine (Phila Pa 1976) 38, E748–54 (2013).
Wang, W., Kong, L. & Zhao, H. et al. Thoracic ossification of ligamentum flavum caused by skeletal fluorosis. Eur Spine J. 16, 1119–28 (2007).
Trivedi, P., Behari, S. & Paul, L. et al. Thoracic Myelopathy Secondary to Ossified Ligamentum Flavum. Acta Neurochir. 143, 775–82 (2001).
Kuh, S. U., Kim, Y. S. & Cho, Y. E. et al. Contributing factors affecting the prognosis surgical outcome for thoracic OLF. Eur Spine J. 15, 485–91 (2006).
Chen, X. Q., Yang, H. L. & Wang, G. L. et al. Surgery for thoracic myelopathy caused by ossification of the ligamentum flavum. J Clin Neurosci. 16, 1316–20 (2009).
Muthukumar, N. Dural ossification in ossification of the ligamentum flavum: a preliminary report. Spine. 34, 2654–61 (2009).
Sun, X. Z., Chen, Z. Q. & Qi, Q. et al. Diagnosis and treatment of ossification of the LF associated with dural ossification: clinical article. J Neurosurg Spine. 15, 386–92 (2011).
Li, F., Chen, Q. & Xu, K. Surgical treatment of 40 patients with thoracic ossification of the ligamentum flavum. J Neurosurg Spine. 4, 191–7 (2006).
Wong, W., Kong, L. & Zhao, H. et al. Thoracic ossification of the ligamentumflavum caused by skeletal fluorosis. Eur Spine J 16, 1119–28 (2007).
Miyakoshi, N., Shimada, Y. & Suzuki, T. et al. Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine. J Neurosurg. 99(suppl 3), 251–6 (2003).
Seichi, A., Nakajima, S. & Takeshita, K. et al. Image-guided resection for thoracicossification of the ligamentum flavum. J Neurosurg. 99(suppl 1), 60–3 (2003).
Shiokawa, K., Hanakita, J. & Suwa, H. et al. Clinical analysis and prognosticstudy of ossified ligamentum flavum of the thoracic spine. J Neurosurg. 94(suppl 2), 221–6 (2001).
Hida, K., Lwasaki, Y. & Koyanagi, L. et al. Bone window computed tomography for detection of dural defect associated with cervical ossified posterior longitudinal ligament. Neurol Med Chir 37, 173–5 (1997).
Epstein, N. E. Identification of ossification of the posterior longitudinal ligament extending through the dura on preoperative computed tomographic examinations of the cervical spine. Spine. 26, 182–6 (2001).
Epstein, N. E. Wound-peritoneal shunts: part of the complex management of anterior dural lacerations in patients with ossification of the posterior longitudinal ligament. Surgical Neurology. 72, 630–4 (2009).
Epstein, N. Anterior approaches to cervical spondylosis and ossification of the posterior longitudinal ligament: review of operative technique and assessment of 65 multilevel circumferential procedures. Surg Neurol. 55, 313–24 (2001).
Epstein, N. Diagnosis and surgical management of cervical ossification of the posterior longitudinal ligament. The Spine J 2, 436–49 (2002).
Mizuno, J. & Nakagawa, H. Ossified posterior longitudinal ligament: management strategies and outcomes. The Spine J 6, 282–8 (2006).
Li, B., Qiu, G. & Zhao, Y. A potential method for identifying dural ossification by measuring the degree of spinal stenosis inthoracic ossification of ligamentum flavum. Med Hypotheses. 96, 9–10 (2016).
Acknowledgements
This work was supported by grants from the National Nature Foundation of China (81171753).
Author information
Authors and Affiliations
Contributions
S.Y.Z. and B.Y. are joint first authors. X.S.C. and S.Y.Z. designed the study. B.Y. and X.B.L. collected the clinical data. S.Y.Z., B.Y., X.B.L., L.S.J. and W.Z. analyzed the data. B.Y. and W.Z. did the statistical analysis. S.Y.Z and B.Y. edited the manuscript. S.Y.Z., B.Y., X.S.C and X.B.L. revised the manuscript. X.S.C. and L.S.J. supervised the study. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhou, Sy., Yuan, B., Chen, Xs. et al. Imaging grading system for the diagnosis of dural ossification based on 102 segments of TOLF CT bone-window data. Sci Rep 7, 2983 (2017). https://doi.org/10.1038/s41598-017-03178-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-03178-x
This article is cited by
-
Prevalence, diagnosis, and impact on clinical outcomes of dural ossification in the thoracic ossification of the ligamentum flavum: a systematic review
European Spine Journal (2023)
-
The role of cerebrospinal fluid cross-section area ratio in the prediction of dural ossification and clinical outcomes in patients with thoracic ossification of ligamentum flavum
BMC Musculoskeletal Disorders (2021)
-
Identification of the molecular mechanism and diagnostic biomarkers in the thoracic ossification of the ligamentum flavum using metabolomics and transcriptomics
BMC Molecular and Cell Biology (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.