Abstract
Chronic administration of glucocorticoids has been shown to render individuals highly susceptible to mycobacterial infection and lead to reactivation of latent bacilli. However, the effect of glucocorticoids on innate anti-mycobacterial defense, especially in macrophages remains largely unknown. Here, we found that glucocorticoids inhibited the innate immune response, antimicrobial nitric oxide production and autophagy in mycobacteria-challenged macrophages. Meanwhile, maturation and acidification of mycobacterial phagosomes were attenuated in RAW264.7 cells after glucocorticoids treatment. Consequently, we observed a glucocorticoid-induced increase in the survival of intracellular mycobacteria in both primary macrophages and cell lines. Glucocorticoids treatment decreased the activation of TBK1 kinase, which promotes the maturation of autophagosomes. Inhibition of TBK1 also decreased the production of nitric oxide. Furthermore, several autophagy-related genes were down-regulated, while activation of the Akt/mTOR signaling pathway was increased after glucocorticoids treatment, which may account for autophagy inhibition during mycobacterial infection. Restoration of autophagy with the agonist rapamycin abolished glucocorticoid-mediated enhancement of mycobacterial survival, suggesting that glucocorticoids blocked anti-mycobacterial defense via autophagy inhibition. Collectively, this study demonstrates that glucocorticoids impair innate antimicrobial autophagy and promote mycobacterial survival in macrophages, which is a novel mechanism for glucocorticoid-mediated immunosuppression. Our findings may provide important clues for tuberculosis prevention.
Similar content being viewed by others
Introduction
Tuberculosis (TB) remains a major global health challenge and is the leading cause of mortality among infectious diseases worldwide, with approximately 1.5 million deaths annually1. Mycobacterium tuberculosis (MTB), the causative agent of TB, infects approximately one-third of the global population. Overall, a relatively small proportion (5–15%) of the estimated 2–3 billion infected individuals will develop active TB disease during their lifetime, while the remaining undergo asymptomatic latent infection2. This fact highlights the importance of host immunity in controlling MTB infection.
Several extrinsic and intrinsic factors may impair the immune system and render individuals susceptible to MTB infection or result in reactivation of latent MTB. For example, human immunodeficiency virus (HIV) infection impairs host CD4+ cell response, which leads to secondary infection with MTB and exacerbates the latter disease3. An inheritable deficiency in ubiquitin-like intracellular protein interferon stimulated gene (ISG)-15 reduces the production of interferon (IFN)-γ by lymphocytes and significantly enhances susceptibility to mycobacterial disease in humans4. Additionally, several iatrogenic factors such as the widely-used immunosuppressive agent glucocorticoids, may also disrupt host anti-mycobacterial defense. Therefore, it is crucial to identify risk factors for TB and elucidate the underlying mechanisms for effective prevention of TB reactivation in the future.
Glucocorticoids are steroid hormones that control a variety of fundamental metabolic and homeostatic functions. Synthetic glucocorticoids, such as dexamethasone and hydrocortisone, are generally prescribed in clinics to treat autoimmune and inflammatory diseases, such as rheumatoid arthritis, ulcerative colitis and systemic lupus erythematosus. However, clinical observations have shown that patients treated with glucocorticoids have a substantially increased risk of developing TB5,6,7. In a TB animal model, glucocorticoids treatment after containment resulted in reactivation of the disease8. Several previous reports have demonstrated that glucocorticoids inhibited the proliferation of antigen-specific T cells9. An increased rate of apoptosis and a decrease in IFN-γ secretion were observed in cultured T cells after glucocorticoid methylprednisolone treatment10. In addition, during helper T cell (Th) polarization, glucocorticoids may cause a shift in the Th1/Th2 balance toward a Th2 dominant response, which is detrimental to TB control11, 12. Nevertheless, whether glucocorticoids modulate another arm of the immune system, innate immune defense against mycobacterial infection, remains largely unknown.
Macrophages are major innate immune cells; they are invaded by MTB, which resides in these cells. The invading bacilli are sensed by pattern recognition receptors (PRRs), which initiate the host innate immune response in macrophages13. Pro-inflammatory cytokines and chemokines are secreted at the infection site to recruit different types of leukocytes and orchestrate immune responses and host anti-mycobacterial defense. Several mechanisms are deployed by macrophages to combat invading MTB, such as nitric oxide (NO) and antimicrobial peptides14. In addition, numerous studies in the last decade have demonstrated that the autophagy pathway is activated via PRR signaling or other immunological stimuli, such as T cell-derived IFN-γ, to exert antimicrobial effects15, 16.
Autophagy is an evolutionarily conserved biological process, which is triggered under starvation circumstances by sequential activation of a range of autophagy-related genes (ATGs), such as ATG5, ATG6, ATG7 and ATG1217. Intracellular aggregated proteins and damaged mitochondria are degraded via the autophagy pathway to maintain cytoplasmic homeostasis. Importantly, recent reports have established the critical role of autophagy in antimicrobial defense against intracellular pathogens, such as MTB15, 18. While MTB escapes the host defense by inhibiting phagosome maturation, autophagy promotes the fusion of the MTB phagosome with autophagosomes and facilitates subsequent clearance of the bacilli in autophagolysosomes19, 20. Additionally, antigen presentation capability is enhanced by autophagy in macrophages to elicit protective adaptive immune response to mycobacteria. Deficiency in key ATGs, such as ATG5 in myeloid cells, renders mice highly susceptible to MTB infection with a substantially increased bacterial burden in the lungs21.
The autophagic process is modulated by multiple signaling pathways. Mammalian target of rapamycin (mTOR), a highly conserved serine/threonine kinase, serves as a master negative regulator of autophagy induction22. mTOR negatively regulates autophagy by inhibiting the function of the unc-51-like kinase 1 (ULK1)/ULK2 complex, which plays an important role in autophagy initiation22. mTOR is inhibited by the immunosuppressant rapamycin, which is therefore generally used as an autophagy agonist. mTOR activation is regulated downstream of the class I PI3K- and v-akt murine thymoma viral oncogene homolog (Akt)/protein kinase B (PKB) pathway, and activation of the PI3K-Akt pathway activates mTOR, resulting in suppression of autophagy22. In addition, TANK-binding kinase 1 (TBK1) coordinates assembly and function of the autophagic machinery by phosphorylating the autophagic adaptor p62 (sequestosome1), thus promoting the maturation of autophagosomes and the elimination of intracellular mycobacteria23.
Here, we investigated the role of glucocorticoids in innate host defense against mycobacterial infection in macrophages. Critical anti-mycobacterial machinery—NO and autophagy—were inhibited in macrophages after glucocorticoid treatment. Simultaneously, we observed impaired maturation of mycobacterial phagosomes in glucocorticoid-treated macrophages and an increase in the survival of intracellular mycobacteria. Furthermore, we found that the activation of TBK1 and key ATGs expression were down-regulated, while the activation of the Akt/mTOR signaling pathway was enhanced in glucocorticoid-treated macrophages, thus hindering autophagic flux. Our findings provide new insight into the mechanism of the glucocorticoid-mediated immunosuppression and TB susceptibility, which has important implications for the prevention of TB reactivation.
Results
Glucocorticoids inhibit the innate immune response, nitric oxide production and autophagy in macrophages after mycobacterial infection
We sought to demonstrate the effect of glucocorticoids on innate immunity during mycobacterial infection. First, we treated mycobacteria-challenged macrophages with the synthetic glucocorticoid dexamethasone and analyzed inflammatory cytokines with real-time PCR. M. bovis BCG-induced levels of IL-1β, IL-6 and TNFα were substantially decreased in dexamethasone-treated macrophage-like RAW264.7 cells (Fig. S1a, all p < 0.001). Similarly, hydrocortisone, a short-term glucocorticoid strongly reduced all inflammatory cytokines tested (Fig. S1b, all p < 0.001). Moreover, M. tuberculosis H37Rv-induced levels of IL-1β, IL-6 and TNFα were also decreased dramatically in dexamethasone-treated RAW264.7 cells (Fig. S1c), indicating glucocorticoid-mediated inhibition of innate immunity after mycobacterial infection.
The induction of inducible NO synthase (iNOS) and release of NO were shown to be a powerful innate anti-mycobacterial defense mechanism in mice24. To determine whether glucocorticoids modulate the iNOS/NO pathway after mycobacterial infection in macrophages, we pretreated RAW264.7 cells with glucocorticoids and then infected the cells with M. bovis BCG. The expression of iNOS and the production of NO were detected. Our results showed that macrophages treated with either dexamethasone or hydrocortisone had significantly decreased iNOS expression (Fig. 1a) and NO production (Fig. 1b) after M. bovis BCG infection. Similarly, iNOS expression was also decreased after dexamethasone treatment in macrophages during M. tuberculosis H37Rv infection (Fig. 1c).
Glucocorticoids suppress iNOS/NO and autophagy in mycobacteria-challenged macrophages. (a,b) RAW264.7 cells were pretreated with dexamethasone (DEX) (1 μM), hydrocortisone (HCS) (1 μM) or vehicle control ethanol (mock) for 6 hr and were then challenged with M. bovis BCG (MOI 5) for the indicated time. iNOS mRNA level was assessed with real-time PCR (a). NO in the supernatant was detected with the Griess assay (b). (c) RAW264.7 cells were pretreated with DEX (1 μM) or vehicle control ethanol (mock) for 6 hr and then challenged with M. tuberculosis H37Rv (MOI 5) for the indicated time. iNOS mRNA level was assessed with real-time PCR. (d,e) RAW264.7 cells were pretreated with DEX (1 μM) (d), HCS (1 μM) (e) or vehicle control ethanol (mock) for 6 hr and then challenged with M. bovis BCG (MOI 5) for 24 hr. The LC3 level was detected with Western blot analysis. Full-length blots are presented in Supplementary Figs 4 and 5, respectively. (f) MDMs were pretreated with DEX (1 μM), HCS (1 μM) or vehicle control ethanol (mock) for 6 hr and then challenged with M. bovis BCG (MOI 5) for 24 hr. The LC3 level was detected with Western blot analysis. Full-length blots are presented in Supplementary Fig. 6. (g) RAW264.7 cells were treated as described in (d), and cells were treated with Bafilomycin A1 (Baf. A1, 100 nM) 2 hr before cellular protein extraction for Western blot analysis. The LC3 level was detected with Western blot analysis. Full-length blots are presented in Supplementary Fig. 7. Relative band intensity of LC3 II was calculated after normalization by load control GAPDH and is shown below each lane. For Western blot analysis, GAPDH was used as the loading control, and data are representative of three independent experiments with similar results. For real-time PCR, the level of each mRNA was normalized to that of β-actin mRNA and is expressed relative to expression in unstimulated cells. Data are shown as the mean ± SEM of three independent experiments. *p < 0.05; **p < 0.01; ***p < 0.001. NS, not significant.
Recently autophagy has been recognized as an important component of innate immunity and has been shown as a potent antimicrobial mechanism18. We next explore whether glucocorticoids modulate antimicrobial autophagy after mycobacterial infection in macrophages. Induction of autophagy is characterized by lipidation of LC3 I to form LC3 II which binds to the membrane of autophagosomes. Western blot analysis revealed that mycobacterial infection up-regulated level of LC3 II in macrophages; however, dexamethasone treatment attenuated the increase of LC3 II, suggesting inhibition of autophagy (Fig. 1d). Hydrocortisone also displayed inhibitory effects on autophagy in mycobacteria-challenged macrophages (Fig. 1e). Furthermore, the effects of glucocorticoids on autophagy were also tested in human monocyte-derived macrophages (MDMs). Our results showed that MDMs pretreated with either dexamethasone or hydrocortisone showed significantly decreased the amount of LC3 II with or without M. bovis BCG infection (Fig. 1f). To assess the dynamic autophagic flux, we treated RAW264.7 cells with a selective vacuolar H+ ATPases inhibitor, Bafilomycin A1, to block cargo degradation in autolysosomes. In the presence of Bafilomycin A1, dexamethasone also suppressed the accumulation of LC3 II after mycobacterial infection (Fig. 1g), suggesting that glucocorticoids inhibited autophagy induction rather than promoting autophagosome-lysosome fusion.
Moreover, we examined the effect of glucocorticoids on autophagy by monitoring LC3 distribution in macrophages. RAW264.7 cells stably expressing GFP-LC3 were infected with M. bovis BCG following dexamethasone treatment. Fluorescence microscopy showed that BCG infection triggered obvious GFP-LC3 puncta in macrophages. However, dexamethasone significantly reduced the amount of GFP-LC3 puncta (Fig. 2a,b). Monodansylcadaverine (MDC) was used to label autophagosomes. The number of MDC positive autophagosomes was dramatically decreased in dexamethasone-treated macrophages after mycobacterial infection (Fig. 2c,d). Taken together, these data indicated that glucocorticoids hindered mycobacteria-induced autophagy in macrophages.
Glucocorticoids decrease autophagosome formation in mycobacteria-challenged macrophages. (a,b) RAW264.7 cells stably expressing GFP-LC3 were pretreated with dexamethasone (DEX) (1 μM) or vehicle control ethanol (mock) for 6 hr and then challenged with M. bovis BCG (MOI 5) for 24 hr. Nuclei were stained with DAPI (blue), and GFP-LC3 puncta were monitored with fluorescence microscopy (a). The average number of GFP-LC3 puncta (>1 μm) per cell was counted in at least 200 cells (b). (c,d) RAW264.7 cells were pretreated with DEX (1 μM) or vehicle control ethanol (mock) for 6 hr and then challenged with M. bovis BCG (MOI 5) for 24 hr. Autophagosomes were detected with MDC staining (c). The percentage of MDC vacuole-positive cells was calculated in at least 200 cells (d). Arrows indicate the GFP-LC3 puncta or MDC-positive vacuoles. Scale bar, 5 μm. *p < 0.05; **p < 0.01. NS, not significant.
Impaired maturation of mycobacterial phagosomes in macrophages after glucocorticoid treatment
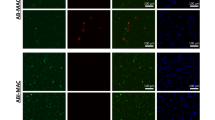
Autophagy has been shown to deliver mycobacterial phagosomes to lysosomes, which overcomes phagosome maturation arrest and facilitates its acidification and subsequent clearance of intracellular bacilli18. Therefore, we next determined whether glucocorticoids modulate the maturation of mycobacterial phagosomes in macrophages. RAW264.7 cells were stained with MDC to display acidic vacuoles in the cytoplasm. Fluorescence microscopy revealed colocalization of MDC-positive vacuoles with Texas-Red-labeled BCG phagosomes in macrophages; however, dexamethasone treatment blocked their colocalization (Fig. 3a), with an approximately one half decrease in MDC-positive BCG phagosomes (Fig. 3b). Moreover, we monitored lysosomes with the specific marker CD63 and assessed the maturation of mycobacterial phagosomes. Dexamethasone-treated RAW264.7 cells showed reduced colocalization of lysosomes and BCG phagosomes (Fig. 3c,d), suggesting inhibition of mycobacterial phagosome maturation. Together, these data indicated that glucocorticoids impaired maturation of mycobacterial phagosomes in macrophages.
Glucocorticoids inhibit the maturation of BCG phagosomes in macrophages. (a,b) RAW264.7 cells were pretreated with dexamethasone (DEX) (1 μM) or vehicle control ethanol for 24 hr and then challenged with Texas-Red-labeled M. bovis BCG (MOI 10) for 1 hr. Autophagosomes were detected with MDC staining (a). The percentage of BCG phagosome colocalizing with MDC-positive vacuoles was calculated in at least 100 phagosomes (b). (c,d) RAW264.7 cells were treated as described in (a,b), and lysosomes were labeled with CD63 (green) (c). The percentage of BCG phagosome colocalizing with CD63-positive vacuoles was calculated in at least 100 phagosomes. (d). Scale bar, 5 μm. **p < 0.01.
Glucocorticoids suppress the clearance of intracellular mycobacteria in macrophages
The glucocorticoid-mediated suppression of antimicrobial autophagy and mycobacterial phagosome maturation prompted us to further determine their role in clearance of intracellular mycobacteria. RAW264.7 cells were pretreated with dexamethasone followed by M. bovis BCG infection, and intracellular viable bacteria were detected with colony-forming unit (CFU) assays. We found that dexamethasone increased the survival of mycobacteria in macrophages at 6, 24, 48, 72 hr post-infection (hpi) (Fig. 4a,b). Intracellular viable bacilli in dexamethasone-treated RAW264.7 cells at 72 hpi were approximately 2-fold greater than those in mock-treated cells (Fig. 4a). Moreover, the percentage of viable mycobacteria, which was calculated compared with the initial internalized bacilli in macrophages, also showed increased mycobacterial survival in dexamethasone-treated cells (Fig. 4b). Cell viability was measured by propidium iodide (PI) staining after pretreatment with dexamethasone and infection with M. bovis BCG for the indicated times (Fig. S2). Our results showed no major decrease in cells viability of either vehicle or dexamethasone treatment through 72 hpi (Fig. S2). To confirm the effects of glucocorticoids on mycobacterial survival, we used another glucocorticoid, hydrocortisone, to treated RAW264.7 cells. Similarly, we observed a substantial increase in viable bacilli after hydrocortisone treatment (Fig. 4c,d). We then determined the role of glucocorticoids in mycobacterial survival using primary bone-marrow-derived macrophages (BMDMs), in which both glucocorticoid agents used promoted the survival of mycobacteria (Fig. 4e,f). MDMs pretreated with either dexamethasone or hydrocortisone showed an increase in the survival of intracellular mycobacteria (Fig. 4g,h). Collectively, these results implied that glucocorticoids antagonized the innate antimicrobial defense against mycobacteria in macrophages.
Increased mycobacterial survival in macrophages after glucocorticoids treatment. (a–d) RAW264.7 cells were pretreated with dexamethasone (DEX) (1 μM), hydrocortisone (HCS) (1 μM) or vehicle control ethanol for 24 hr and then challenged with M. bovis BCG (MOI 10) for 1 hr. The intracellular viable bacilli were determined by CFU assays at the indicated time post-infection (a,c). Survival rate was calculated compared with that of mock-treated cells (b,d). (e–h) BMDMs (e,f) and MDMs (g,h) were treated like RAW264.7 cells as described in (a–d). The intracellular viable bacilli were determined by CFU assays at 72 hpi (e,g). Survival rate was calculated compared with that of the mock-treated cells (f,h). Data are shown as the mean ± SEM of three independent experiments. *p < 0.05; **p < 0.01; ***p < 0.001. NS, not significant.
To further assess whether glucocorticoids affect macrophage-mediated phagocytosis of M. bovis BCG, we pretreated RAW264.7 cells with glucocorticoid agents, followed by fluorescent Texas-Red-labeled M. bovis BCG infection, and phagocytosis was analyzed by flow cytometry. Our results showed that neither dexamethasone nor hydrocortisone had major effects on M. bovis BCG phagocytosis by macrophages (Fig. S3a,b). Moreover, the uptake of M. bovis BCG in macrophages was detected by CFU assays after glucocorticoid treatment. Similarly, RAW264.7 cells pretreated with glucocorticoids showed no difference in the phagocytosis of M. bovis BCG compared with that of mock-treated cells (Fig. S3c,d). The above results indicated that glucocorticoids inhibited intracellular killing of mycobacteria in macrophages without affecting mycobacterial phagocytosis.
Glucocorticoids suppress TBK1 activation in mycobacteria-challenged macrophages
In the autophagy-mediated anti-mycobacterial response, TBK1 is reported to be essential for the maturation of autophagosomes23. Therefore, we next explored whether glucocorticoids modulate TBK1 activation after mycobacterial infection in macrophages. Both dexamethasone and hydrocortisone decreased phosphorylated TBK1 in RAW264.7 cells after M. bovis BCG infection (Fig. 5a). To further determine whether inhibition of TBK1 affected the iNOS/NO pathway, we knocked down TBK1 by RNA interference. Western blot analysis showed that siRNA #2 and siRNA #3 had a stronger silencing efficiency than that of siRNA #1 (Fig. 5b,c). TBK1-silenced cells had attenuated iNOS expression and NO production (Fig. 5d). Moreover, the TBK1 specific inhibitor BX795 was used to inhibit its activity. Cells treated with BX795 showed significantly decreased iNOS expression and NO production after mycobacterial infection (Fig. 5e).
Glucocorticoids inhibit TBK1 activation, and TBK1 silencing decreases iNOS expression and NO production in macrophages during mycobacterial infection. (a) RAW264.7 cells were pretreated with dexamethasone (DEX) (1 μM), hydrocortisone (HCS) (1 μM) or vehicle control ethanol (mock) for 24 hr and then challenged with M. bovis BCG (MOI 5) for the indicated times. Then the phosphorylation level of TBK1 was tested with Western blot analysis. Full-length blots are presented in Supplementary Fig. 8. (b) RAW264.7 cells were transfected with control siRNA (NC) or three TBK1 siRNAs (siTBK1 #1, #2, #3) with different sequences for 24 hr, and the protein level of TBK1 was tested with Western blot. Full-length blots are presented in Supplementary Fig. 9. (c,d) RAW264.7 cells were transfected with NC or siTBK1 #2 or #3 for 24 hr, and then infected with M. bovis BCG for the indicated times. TBK1 (c) and iNOS (d) mRNA level were tested with real-time PCR. NO in the supernatant was detected with the Griess assay (d). (e) RAW264.7 cells were pretreated with a TBK1 inhibitor (BX795) at the indicated concentration for 1 hr, and then infected with M. bovis BCG for the indicated times. iNOS mRNA levels were tested with real-time PCR. NO in the supernatant was detected with the Griess assay. For Western blot analysis, β-Tubulin or GAPDH was used as a loading control, and data are representative of three independent experiments with similar results. For real-time PCR, the level of each mRNA was normalized to that of β-actin mRNA and is expressed relative to expression in unstimulated cells. Data are shown as the mean ± SEM of three independent experiments. *p < 0.05; ***p < 0.001.
Glucocorticoids repress ATG expression and enhance Akt/mTOR pathway activation in mycobacteria-challenged macrophages
Autophagy is a cascade reaction executed by ATGs25. Decreasing or genetically depleting the expression of the key ATGs, such as ATG5, ATG6, ATG7 and ATG12, substantially inhibits the autophagic process26, 27. To explore the underlying mechanism for glucocorticoid-mediated suppression of autophagy, we first screened the expression of key ATGs. Notably, dexamethasone down-regulated the mRNA levels of ATGs (ATG5, ATG6, ATG7 and ATG12) in RAW264.7 cells at 24 hpi, while no major alteration was observed for any of these gene in uninfected cells (Fig. 6a). Similarly, hydrocortisone displayed similar effects on the expression of these ATGs at the mRNA level (Fig. 6b). These findings were further verified with Western blot analysis, which showed decreased protein levels of key ATGs after dexamethasone or hydrocortisone treatment (Fig. 6c). Notably, conjugation of ATG5-ATG12 was also decreased after glucocorticoid treatment (Fig. 6c). We next explored the effect of glucocorticoids on the Akt/mTOR pathway, which is recognized as a major regulatory pathway of autophagy. Our results showed that dexamethasone or hydrocortisone treatment increased the phosphorylation level of Akt after M. bovis BCG infection (Fig. 6d). Meanwhile, the phosphorylation levels of two mTOR substrates, p70 S6 Kinase (p70S6K) and 4E-BP1, were also upregulated in glucocorticoid-treated macrophages (Fig. 6d). These data indicated that glucocorticoids modulated autophagy by multiple mechanisms, including suppression of ATG expression and enhancement Akt/mTOR pathway activation, in macrophages during mycobacterial infection.
Glucocorticoids inhibit autophagy by suppressing the expression of ATGs and enhancing the activation of the Akt/mTOR pathway. (a–c) RAW264.7 cells were pretreated with dexamethasone (DEX) (1 μM), hydrocortisone (HCS) (1 μM) or vehicle control ethanol (mock) for 6 hr and then challenged with M. bovis BCG (MOI 5) for 24 hr. mRNA and protein levels of ATGs were determined by real-time PCR (a,b) and Western blot (c), respectively. Full-length blots are presented in Supplementary Fig. 10. (d) RAW264.7 cells were pretreated with DEX (1 μM), HCS (1 μM) or vehicle control ethanol (mock) for 24 hr and then challenged with M. bovis BCG (MOI 5) for the indicated times. Phosphorylation and total protein levels of the indicated genes were determined by Western blot analysis. Full-length blots are presented in Supplementary Fig. 11. For Western blotting, GAPDH was used as the loading control. Data are representative of three independent experiments with similar results. For real-time PCR, the level of each mRNA was normalized to that of β-actin mRNA and is expressed relative to expression in unstimulated cells. Data are shown as the mean ± SEM of three independent experiments. *p < 0.05; **p < 0.01; ***p < 0.001. NS, not significant.
Glucocorticoids inhibit the clearance of intracellular mycobacteria in macrophages by inhibiting autophagy
To assess whether glucocorticoids promote mycobacterial survival through autophagy inhibition, we activated autophagy with the agonist rapamycin and determined whether it could restore anti-mycobacterial activity in dexamethasone-treated macrophages. While dexamethasone decreased autophagy in BCG-infected macrophages, rapamycin could effectively induce autophagy in dexamethasone-treated cells (Fig. 7a). Next, we detected clearance of mycobacteria in glucocorticoid-treated macrophages after restoration of autophagy with rapamycin treatment. Consistent with the data above, dexamethasone facilitated mycobacterial survival in RAW264.7 cells. However, after autophagy restoration, viable mycobacteria in dexamethasone-treated macrophages were decreased to levels similar to those in cells without glucocorticoid treatment (Fig. 7b,c). These results suggested that the glucocorticoid-mediated decrease in mycobactericidal activity was due to autophagy inhibition.
Glucocorticoids promote BCG survival in macrophages by inhibiting autophagy. (a) RAW264.7 cells were pretreated with dexamethasone (DEX) (1 μM) or vehicle control ethanol (mock) for 6 hr and then challenged with M. bovis BCG (MOI 5) or treated with the vehicle control DMSO or rapamycin (4 μM). LC3 level was detected with Western blot analysis. And GAPDH was used as the loading control. Full-length blots are presented in Supplementary Fig. 12. Data are representative of three independent experiments with similar results. (b,c) RAW264.7 cells were treated as described in (a), and viable bacilli were determined by CFU assays at 6 hpi (b). Survival rate was calculated compared with that of mock-treated cells (c). Data are shown as the mean ± SEM of three independent experiments. *p < 0.05.
Discussion
Glucocorticoids, potent immunosuppressive agents extensively used in almost all clinical specialties could increase susceptibility to mycobacterial infection after long-term administration5,6,7. Previous reports have focused on glucocorticoid-induced inhibition of adaptive immunity, especially T-cell responses28,29,30,31. Here, we investigated the effect of glucocorticoids on innate host defense against mycobacterial infection in macrophages. Glucocorticoids impaired antimicrobial NO production, as well as autophagy and maturation of mycobacterial phagosomes in macrophages, thus facilitating the survival of mycobacteria. Activation of TBK1 and expression of several key ATGs were down-regulated by glucocorticoid treatment, while activation of Akt/mTOR pathway was enhanced after glucocorticoid treatment, which account for the inhibition of autophagy. These findings provide novel mechanistic insight into the immunosuppressive activity of glucocorticoids during mycobacterial infection.
Although glucocorticoids are believed to be promising agents to treat exaggerated systemic inflammatory response, such as sepsis, in clinical reports, a systematic review with meta-analysis revealed poor evidence to support the use of steroids in sepsis patients and questioned the alleged benefits32. Actually, several experimental studies have identified glucocorticoid intake as an independent risk factor for infections. For example, in a pneumococcal pneumonia model, the inhaled corticosteroid fluticasone reduced alveolar macrophages killing of pneumococci33. At the earliest stages of herpes simplex virus-1 infection, glucocorticoids suppressed adaptive antiviral immunity by impairing dendritic cell functions34. Here, we provide experimental evidence showing that glucocorticoids impair innate defense and promote mycobacterial survival in both mouse and human macrophages, which is consistent with a recent study showing that the antimicrobial activity of human macrophages was decreased after dexamethasone treatment35. According to these findings, it is highly recommended to re-evaluate the benefits and risks before prescribing glucocorticoids to individuals at high-risk of TB. Additionally, essential measures should be taken to prevent reactivation of TB in patients undergoing long-term glucocorticoid therapy.
In previous studies, glucocorticoids have been shown to inhibit innate immune signaling, such as TLR-induced inflammatory responses. Dexamethasone treatment markedly suppressed LPS-mediated induction of inflammatory genes by selective inhibition of p38 MAP kinase36. Interferon regulatory factor 3 (IRF3), another signaling branch leading to IFN induction downstream of TLR-3 and TLR-4, was also inhibited by glucocorticoid by targeting TBK1 kinase activation37. In our study, we also observed a decrease in the expression of inflammatory cytokines in glucocorticoid treated macrophages after either M. bovis BCG or M. tuberculosis H37Rv infection. In addition to inflammatory cytokines, NO and autophagy are both important effectors of innate immune responses to mycobacteria24, 25. A previous study demonstrated that dexamethasone substantially reduced LPS-induced iNOS expression in murine neonatal microglial cells38. In the present study, we found that glucocorticoids inhibited iNOS expression and NO production in mycobacteria-infected macrophages, which is consistent with a previous study demonstrating that hydrocortisone treatment decreased iNOS expression and NO production in a mycobacteria-infected mouse model39. Moreover, our results showed that glucocorticoid treatment suppressed autophagy in mycobacteria-challenged macrophages and impaired mycobactericidal activity, which provides new information on the role of glucocorticoid-mediated immunosuppression in innate immunity.
Glucocorticoid-mediated regulation of autophagy has been investigated in other non-infectious models, especially hematological malignancies and musculoskeletal disorders. Glucocorticoids are fundamental drugs commonly used for the treatment of lymphoid leukemia. Autophagy was initiated in lymphoid leukemia cells after dexamethasone treatment and is indispensable for its cytotoxicity40. Aberrant expression of ATGs was associated with glucocorticoid resistance in B-cell type acute lymphoblastic leukemia41. In osteocytes, dexamethasone triggered autophagy to impair dendritic processes and lead to bone loss42, 43. Dexamethasone-induced autophagy regulated the muscle atrophy program44. To the best of our knowledge, this work is the first one to investigate glucocorticoid-mediated regulation of autophagy in an infectious setting. Interestingly, our results showed that glucocorticoids inhibited autophagy in mycobacteria-challenged macrophages, in contrast to leukemia cells. Autophagy is initiated and regulated by various extrinsic and intrinsic stimuli/factors, which differ dramatically between distinct cells. This may explain the discrepancy of glucocorticoid-mediated autophagy regulation between mycobacteria-infected macrophages and leukemia cells.
Autophagy is tightly controlled at different stages by distinct factors. The metabolism master regulator mTOR is active under nutrient-rich circumstances and represses autophagy45. Although mycobacteria induce autophagy and increase the mTOR kinase activity simultaneously after infection46, our study indicated that the present of glucocorticoids further enhanced activation of the Akt/mTOR pathway, which may result in the depression of mycobacteria-mediated autophagy. Rapamycin targets mTOR and inhibits its kinase activity to derepress initiation of autophagy. In this study, we found that glucocorticoids regulated autophagy in macrophages after mycobacterial infection but not rapamycin stimulation. Restoration of autophagy with rapamycin treatment attenuated the promotion of mycobacterial survival mediated by glucocorticoids. These findings indicate that glucocorticoids regulate mycobacteria-induced autophagy, at least partly through enhancement of mTOR signaling.
Glucocorticoids have been reported to inhibit TBK1 phosphorylation and TBK1 kinase activity37, which phosphorylates the autophagic adaptor p62 and promotes autophagosome maturation, without affecting the autophagic initiation23. In our study, we found that glucocorticoids decreased the activation of TBK1, which may account for the suppression of autophagosome maturation. Autophagy is mediated by a cascade reaction of the ATGs25, and decreased expression of key ATGs, such as ATG5, ATG6, ATG7 and ATG12, would substantially inhibit the autophagic process26, 27. In the present study, we found that the levels of several key ATGs, including ATG5, ATG6, ATG7 and ATG12, were increased after mycobacterial infection, suggesting that autophagy induced by mycobacteria may be dependent on elevating the expression of key ATGs. However, ATG5, ATG6, ATG7 and ATG12 were suppressed by glucocorticoid treatment, indicating that glucocorticoids inhibit autophagy by decreasing the expression of key ATGs during mycobacterial infection. Thus, glucocorticoids inhibit mycobacteria-induced autophagy in macrophages by multiple mechanisms, leading to the survival of intracellular mycobacteria.
Glucocorticoids function by binding to glucocorticoids receptors (GRs), which induce various inhibitory molecules or repress transcriptional activity of transcription factors to negatively regulate the TLR pathway47. Activation of GR was reported to inactivate the transcriptional activity of CCAAT/enhancer binding proteinβ (C/EBPβ) and nuclear factor-erythroid derived 2-like 2 (Nrf2) by recruiting silencing mediator for retinoid and thyroid hormone receptors (SMRT) for histone deacetylation48. C/EBPβ and Nrf2 have been shown to modulate the expression of multiple ATGs49,50,51. Thus, glucocorticoids may suppress ATG expression by inhibiting the transcriptional activity of C/EBPβ and Nrf2 during mycobacterial infection, which requires further investigation.
In summary, our results demonstrate a novel mechanism by which glucocorticoids suppress host defense against mycobacterial infection in macrophages. Glucocorticoids repress the activation of TBK1 and attenuate iNOS expression and NO production in macrophages infected with mycobacteria. Moreover, glucocorticoids repress the expression of key ATG, but enhance the activation of the Akt-mTOR pathway during mycobacterial infection, thus decreasing autophagic flux. These changes result in enhancement of intracellular mycobacterial survival. With these findings, we gain new insight into the immunosuppressive activity of glucocorticoids, which may provide useful information about prevention of TB activation.
Materials and Methods
Ethics statement
All animal experiments in this study were carried out in accordance with the recommendations in the Guide for the Care and Use of Laboratory Animals of the National Institutes of Health. For all experiments of human primary macrophages, the study was approved by the Ethics Committee of Southern Medical University and conducted in accordance with the Declaration of Helsinki. Written informed consent was obtained from all participants before the commencement of the study. All experimental protocols were reviewed and approved by the Medical Ethics Board and the Biosafety Management Committee of Southern Medical University.
Reagents
The following reagents were used in this study: Dexamethasone (Sigma-Aldrich, D4902), Hydrocortisone (Sangon Biotech, A610506), Monodansylcadaverine (MDC, Sigma-Aldrich, D4008), Rapamycin (Sigma-Aldrich, V900930), DMSO (Sigma-Aldrich, D2650), Bafilomycin A1 (Santa Cruz, sc-201550), Texas-red (Invitrogen, T-6134), TBK1 inhibitor BX795 (Selleckchem, S1274), Trizol reagent (Invitrogen, 15596-018), Middlebrook 7H9 Broth (BD Difco Laboratories, 271310), Middlebrook 7H10 Agar (BD Difco Laboratories, 262710). The following antibodies were used in this study: LC3 (Novus Biologicals, NB100-2220), GAPDH (ZSGB-BIO, TA-08), CD63 (Santa cruz, sc-15363), ATG5 (Cell Signaling, 12994), ATG6 (Cell Signaling, 3738), ATG7 (Cell Signaling, 8558), ATG12 (Cell Signaling, 4180), β-Tubulin (Cell Signaling, 2128), TBK1/NAK (Cell Signaling, 3013), Phospho-TBK1/NAK (Ser172) (Cell Signaling, 5483), Akt (Cell Signaling, 4691), Phospho-Akt (Ser473) (Cell Signaling, 4060), p70 S6 Kinase (Cell Signaling, 9202), Phospho-p70 S6 Kinase (Thr389) (Cell Signaling, 9206), 4E-BP1 (Cell Signaling, 9644), Phospho-4E-BP1 (Thr37/46) (Cell Signaling, 2855).
Cell culture
RAW264.7 cells (ATCC; TIB-71) were cultured in DMEM supplemented with 10% fetal bovine serum (FBS) and 100 U/ml penicillin, 100 μg/ml streptomycin. For bone-marrow derived macrophages (BMDMs) preparation, firstly, eight-week-old female C57BL/6 mice were purchased from Southern Medical University Animal Supply Center. Secondly, single-cell suspensions of bone marrow cells from the femurs and tibiae were cultured in DMEM containing 10% FBS, 2 mM L-glutamine, 1 mM sodium pyruvate, 100 U/ml penicillin, 100 μg/ml streptomycin, supplemented with 100 ng/ml GM-CSF. Fresh medium was provided on days 3 and 5 of culture. At days 7 of culture, the isolated macrophages were used for further in vitro studies.
Human monocyte-derived macrophages (MDMs) isolation and culture
Human peripheral blood samples from healthy donors were obtained from Guangzhou Blood Center. Peripheral blood mononuclear cells (PBMCs) were isolated by Ficoll (TBDsciences, Tianjin) density gradient centrifugation. Human monocytes were purified from PBMCs by anti-CD14 microbeads (BD Bioscience) according to the manufacturer’s directions. Monocytes were cultured in RPMI-1640 supplemented with 10% FBS and 100 ng/ml GM-CSF for a week to generate MDMs.
Bacterial culture and infection
M. bovis BCG strain 19015 was purchased from the American Type Culture Collection (ATCC), and mycobacteria were grown in Middlebrook 7H9 broth medium or on 7H10 agar plates supplemented with OADC and cultured in a standard tissue culture incubator as described previously19, 20, 52. Mycobacteria were homogenized to generate a single cell suspension, and macrophages were infected with mycobacteria at the indicated multiplicity of infection (MOI).
Transient Transfection
RAW264.7 cells (at approximately 50% confluence) were transiently transfected with 100 nM TBK1 siRNA vs Negative control (NC) siRNA, using Lipofectamine 2000 (Invitrogen) according to the manufacturer’s instructions. All the above siRNAs were purchased from Ribobio.
Colony-forming unit (CFU) assays
RAW264.7 cells were infected with M. bovis BCG at an MOI of 10. After 1 hr incubation at 37 °C, the infected cells were washed extensively with PBS to remove extracellular mycobacteria, and the infected cells were incubated for indicated time, and then lysed in 1 ml of distilled water. Quantitative culturing was performed using 10-fold serial dilutions. Aliquots of each dilution were inoculated in triplicate on Middlebrook 7H10 agar plates supplemented with OADC. Plates were incubated for 3 weeks before colonies were counted.
Propidium iodide (PI) staining
RAW264.7 cells were infected with M. bovis BCG at an MOI of 10. After 1 hr incubation at 37 °C, the infected cells were washed extensively with PBS to remove extracellular mycobacteria, and the infected cells were incubated for indicated time. Cells were collected and stained with PI (Sangon Biotech, E607306) according to the manufacturer’s instructions, and measured by flow cytometry.
Western blot analysis
Western blot analysis was performed as described previously53, 54. Briefly, the whole-cell extract was resolved by SDS-polyacrylamide gel electrophoresis and transferred to polyvinylidene fluoride membranes. The membranes were blocked in 5% bovine serum albumin and then incubated with diluted primary antibodies at 4 °C overnight. Western blot analysis was developed using horseradish peroxidase-conjugated secondary antibody, followed by detection with enhanced chemiluminescence.
Confocal microscopy
Confocal microscopy was performed as described previously19. For immunofluorescence experiments, cells were grown on glass coverslips and treated as indicated, followed by fixation, permeabilization and blocking. Samples were incubated with primary antibody at 4 °C overnight, and then with secondary antibody for 1 hr at room temperature before mounting. In fluorescence experiments, RAW264.7 GFP-LC3 cells were treated as indicated, followed by fixation, permeabilization. Nuclei were labeled with 4,6-diamidino-2-phenylindole (DAPI) staining. MDC staining was performed by adding MDC (50 μM) to cells and incubating at 37 °C for 30 min before fixation. Coverslips were mounted with ProLong Gold antifade reagent (Invitrogen) and visualized using Olympus confocal microscope (FV10-ASW).
RNA isolation and real time-PCR
Total RNA was isolated with Trizol reagent as described before19, 55, 56 and cDNA was synthesized with TransScript One-Step gDNA Removal and cDNA Synthesis SuperMix (TransGen Biotech, AT311-03). TransStart Top Green qPCR SuperMix and an Eppendorf Mastercycler ep realplex4 Real-Time PCR system (Eppendorf) were used for quantitative RT-PCR analysis. β-actin was used as housekeeping gene for data normalization. The primer sequences used for PCR were: β-actin, 5′-GATTACTGCTCTGGCTCCTAGC-3′ (forward) and 5′-GACTCATCGTACTCCTGCTTGC-3′ (reverse); ATG5, 5′-TGCTGAAGGCTGTAGGAGAC-3′ (forward) and 5′-CGAGGCCACCAGTTTAAGGA-3′ (reverse); ATG6, 5′-CAGGAGGAAGAGGCTAACTCAG-3′ (forward) and 5′-GTGACCTTGAGTCTCCGGCT-3′ (reverse); ATG7, 5′-GCAC GAACTGACCCAGAAGA-3′ (forward) and 5′-GTTGGTGTTGTGCAGGGTTC-3′ (reverse); ATG12, 5′-TGCTGAAGGCTGTAGGAGAC-3′ (forward) and 5′-CGAGGCCACCAGTTTAAGGA-3′ (reverse); iNOS, 5′-TCCTCACTGGGACAGCACAGA ATG-3′ (forward) and 5′-GTGTCATGCAAAATCTCTCCACTGCC-3′ (reverse); TBK1, 5′-TGTTCTAGAGGAGCCGTCCA-3′ (forward) and 5′-GGTGCACTATGCCGTTCTCT-3′ (reverse).
Griess assay
RAW264.7 cells were pretreated with dexamethasone, hydrocortisone, BX795, or transfection with Negative control/TBK1 siRNA, and then the supernatant of each sample was collected at 0, 6 and 24 hr after M. bovis BCG challenge. NO levels were determined by measuring its stable end product, nitrite, using a Griess reagent (Sigma, St. Louis, Missouri). One hundred microliter of supernatant was added to an equal volume of Griess reagent in duplicate on a 96-well plate and incubated at room temperature for 15 min. Absorbance (540 nm) was measured and nitrite concentrations were estimated using a standard nitrite curve. Results were expressed as the mean micromoles of nitrite per sample ± SEM.
Statistical analysis
Statistical analysis was performed using GraphPad Prism 5.0 (GraphPad Software, San Diego, CA). Real-time PCR and CFU data are shown as the mean ± SEM. Data between two groups were compared by using Student’s t-test. Differences were considered statistically significant with a p value less than 0.05.
References
World Health Organization. Global tuberculosis control 2015. World Health Organization (2015).
Getahun, H., Matteelli, A., Chaisson, R. E. & Raviglione, M. Latent Mycobacterium tuberculosis infection. New England Journal of Medicine 372, 2127–2135, doi:10.1056/NEJMra1405427 (2015).
Havlir, D. V. & Barnes, P. F. Tuberculosis in patients with human immunodeficiency virus infection. New England Journal of Medicine 340, 367–373, doi:10.1056/NEJM199902043400507 (1999).
Bogunovic, D. et al. Mycobacterial disease and impaired IFN-gamma immunity in humans with inherited ISG15 deficiency. Science. 337, 1684–1688, doi:10.1126/science.1224026 (2012).
Lai, C. C., Lee, M. T., Lee, S. H., Chang, S. S. & Lee, C. C. Risk of incident active tuberculosis and use of corticosteroids. International Journal of Tuberculosis and Lung Disease 19, 936–942, doi:10.5588/ijtld.15.0031 (2015).
Jick, S. S., Lieberman, E. S., Rahman, M. U. & Choi, H. K. Glucocorticoid use, other associated factors, and the risk of tuberculosis. Arthritis and Rheumatism 55, 19–26, doi:10.1002/art.21705 (2006).
Kim, H. A. et al. Mycobacterium tuberculosis infection in a corticosteroid-treated rheumatic disease patient population. Clinical and Experimental Rheumatology 16, 9–13 (1998).
Manabe, Y. C. et al. The aerosol rabbit model of TB latency, reactivation and immune reconstitution inflammatory syndrome. Tuberculosis (Edinb) 88, 187–196, doi:10.1016/j.tube.2007.10.006 (2008).
Braun, C. M. et al. Corticosteroid modulation of human, antigen-specific Th1 and Th2 responses. Journal of Allergy and Clinical Immunology 100, 400–407, doi:10.1016/S0091-6749(97)70255-0 (1997).
Tramsen, L. et al. Immunosuppressive compounds exhibit particular effects on functional properties of human anti-Aspergillus Th1 cells. Infection and Immunity 82, 2649–2656, doi:10.1128/IAI.01700-14 (2014).
Agarwal, S. K. & Marshall, G. D. Jr. Dexamethasone promotes type 2 cytokine production primarily through inhibition of type 1 cytokines. Journal of Interferon and Cytokine Research 21, 147–155, doi:10.1089/107999001750133159 (2001).
Ramirez, F., Fowell, D. J., Puklavec, M., Simmonds, S. & Mason, D. Glucocorticoids promote a TH2 cytokine response by CD4+ T cells in vitro. Journal of Immunology 156, 2406–2412 (1996).
Bhatt, K. & Salgame, P. Host innate immune response to Mycobacterium tuberculosis. Journal of Clinical Immunology 27, 347–362, doi:10.1007/s10875-007-9084-0 (2007).
Liu, P. T. & Modlin, R. L. Human macrophage host defense against Mycobacterium tuberculosis. Current Opinion in Immunology 20, 371–376, doi:10.1016/j.coi.2008.05.014 (2008).
Gutierrez, M. G. et al. Autophagy is a defense mechanism inhibiting BCG and Mycobacterium tuberculosis survival in infected macrophages. Cell 119, 753–766, doi:10.1016/j.cell.2004.11.038 (2004).
Xu, Y. et al. Toll-like receptor 4 is a sensor for autophagy associated with innate immunity. Immunity 27, 135–144, doi:10.1016/j.immuni.2007.05.022 (2007).
Levine, B. & Kroemer, G. Autophagy in the pathogenesis of disease. Cell 132, 27–42, doi:10.1016/j.cell.2007.12.018 (2008).
Deretic, V. et al. Autophagy in immunity against mycobacterium tuberculosis: a model system to dissect immunological roles of autophagy. Current Topics in Microbiology and Immunology 335, 169–188, doi:10.1007/978-3-642-00302-8_8 (2009).
Wang, J. et al. MicroRNA-155 promotes autophagy to eliminate intracellular mycobacteria by targeting Rheb. PLoS Pathog. 9, e1003697, doi:10.1371/journal.ppat.1003697 (2013).
Wang, J. et al. MRP8/14 induces autophagy to eliminate intracellular Mycobacterium bovis BCG. Journal of Infection 70, 415–426, doi:10.1016/j.jinf.2014.09.013 (2015).
Watson, R. O., Manzanillo, P. S. & Cox, J. S. Extracellular M. tuberculosis DNA targets bacteria for autophagy by activating the host DNA-sensing pathway. Cell. 150, 803–815, doi:10.1016/j.cell.2012.06.040 (2012).
Into, T., Inomata, M., Takayama, E. & Takigawa, T. Autophagy in regulation of Toll-like receptor signaling. Cell Signal 24, 1150–1162, doi:10.1016/j.cellsig.2012.01.020 (2012).
Pilli, M. et al. TBK-1 promotes autophagy-mediated antimicrobial defense by controlling autophagosome maturation. Immunity 37, 223–234, doi:10.1016/j.immuni.2012.04.015 (2012).
Thoma-Uszynski, S. et al. Induction of direct antimicrobial activity through mammalian toll-like receptors. Science 291, 1544–1547, doi:10.1126/science.291.5508.1544 (2001).
Levine, B., Mizushima, N. & Virgin, H. W. Autophagy in immunity and inflammation. Nature 469, 323–335, doi:10.1038/nature09782 (2011).
Kimmey, J. M. et al. Unique role for ATG5 in neutrophil-mediated immunopathology during M. tuberculosis infection. Nature 528, 565–569, doi:10.1038/nature16451 (2015).
Tang, B. et al. Shiga toxins induce autophagic cell death in intestinal epithelial cells via the endoplasmic reticulum stress pathway. Autophagy 11, 344–354, doi:10.1080/15548627.2015.1023682 (2015).
Ramirez, F., Fowell, D. J., Puklavec, M., Simmonds, S. & Mason, D. Glucocorticoids promote a TH2 cytokine response by CD4+ T cells in vitro. J Immunol 156, 2406–2412 (1996).
Howard, A. D. & Zwilling, B. S. Reactivation of tuberculosis is associated with a shift from type 1 to type 2 cytokines. Clin Exp Immunol 115, 428–434, doi:10.1046/j.1365-2249.1999.00791.x (1999).
Miyaura, H. & Iwata, M. Direct and indirect inhibition of Th1 development by progesterone and glucocorticoids. J Immunol 168, 1087–1094, doi:10.4049/jimmunol.168.3.1087 (2002).
Mahuad, C. et al. Cortisol and dehydroepiandrosterone affect the response of peripheral blood mononuclear cells to mycobacterial antigens during tuberculosis. Scand J Immunol 60, 639–646, doi:10.1111/j.0300-9475.2004.01514.x (2004).
Volbeda, M. et al. Glucocorticosteroids for sepsis: systematic review with meta-analysis and trial sequential analysis. Intensive Care Medicine 41, 1220–1234, doi:10.1007/s00134-015-3899-6 (2015).
Stolberg, V. R. et al. Glucocorticoid-Augmented Efferocytosis Inhibits Pulmonary Pneumococcal Clearance in Mice by Reducing Alveolar Macrophage Bactericidal Function. Journal of Immunology 195, 174–184, doi:10.4049/jimmunol.1402217 (2015).
Elftman, M. D. et al. Stress-induced glucocorticoids at the earliest stages of herpes simplex virus-1 infection suppress subsequent antiviral immunity, implicating impaired dendritic cell function. Journal of Immunology 184, 1867–1875, doi:10.4049/jimmunol.0902469 (2010).
Steiger, J. et al. Imatinib Triggers Phagolysosome Acidification and Antimicrobial Activity against Mycobacterium bovis Bacille Calmette-Guerin in Glucocorticoid-Treated Human Macrophages. Journal of Immunology 197, 222–232, doi:10.4049/jimmunol.1502407 (2016).
Bhattacharyya, S., Brown, D. E., Brewer, J. A., Vogt, S. K. & Muglia, L. J. Macrophage glucocorticoid receptors regulate Toll-like receptor 4-mediated inflammatory responses by selective inhibition of p38 MAP kinase. Blood 109, 4313–4319, doi:10.1182/blood-2006-10-048215 (2007).
McCoy, C. E., Carpenter, S., Palsson-McDermott, E. M., Gearing, L. J. & O’Neill, L. A. Glucocorticoids inhibit IRF3 phosphorylation in response to Toll-like receptor-3 and -4 by targeting TBK1 activation. Journal of Biological Chemistry 283, 14277–14285, doi:10.1074/jbc.M709731200 (2008).
Gao, W., Li, J., Cirillo, J., Borgens, R. & Cho, Y. Action at a distance: functional drug delivery using electromagnetic-field-responsive polypyrrole nanowires. Langmuir 30, 7778–7788, doi:10.1021/la500033b (2014).
MacMicking, J. D. et al. Identification of nitric oxide synthase as a protective locus against tuberculosis. Proc Natl Acad Sci USA 94, 5243–5248, doi:10.1073/pnas.94.10.5243 (1997).
Laane, E. et al. Cell death induced by dexamethasone in lymphoid leukemia is mediated through initiation of autophagy. Cell Death and Differentiation 16, 1018–1029, doi:10.1038/cdd.2009.46 (2009).
Sarang, Z., Gyurina, K., Scholtz, B., Kiss, C. & Szegedi, I. Altered expression of autophagy-related genes might contribute to glucocorticoid resistance in precursor B-cell type acute lymphoblastic leukemia. European Journal of Haematology 97, 453–460, doi:10.1111/ejh.12753 (2016).
Gao, J. et al. Glucocorticoid impairs cell-cell communication by autophagy-mediated degradation of connexin 43 in osteocytes. Oncotarget 7, 26966–26978, doi:10.18632/oncotarget.9034 (2016).
Yao, W., Dai, W., Jiang, J. X. & Lane, N. E. Glucocorticoids and osteocyte autophagy. Bone 54, 279–284, doi:10.1016/j.bone.2013.01.034 (2013).
Troncoso, R. et al. Dexamethasone-induced autophagy mediates muscle atrophy through mitochondrial clearance. Cell Cycle 13, 2281–2295, doi:10.4161/cc.29272 (2014).
Noda, T. & Ohsumi, Y. Tor, a phosphatidylinositol kinase homologue, controls autophagy in yeast. Journal of Biological Chemistry 273, 3963–3966, doi:10.1074/jbc.273.7.3963 (1998).
Zullo, A. J. & Lee, S. Mycobacterial induction of autophagy varies by species and occurs independently of mammalian target of rapamycin inhibition. Journal of Biological Chemistry 287, 12668–12678, doi:10.1074/jbc.M111.320135 (2012).
Xavier, A. M., Anunciato, A. K., Rosenstock, T. R. & Glezer, I. Gene Expression Control by Glucocorticoid Receptors during Innate Immune Responses. Front Endocrinol (Lausanne) 7, 31, doi:10.3389/fendo.2016.00031 (2016).
Ki, S. H., Cho, I. J., Choi, D. W. & Kim, S. G. Glucocorticoid receptor (GR)-associated SMRT binding to C/EBPbeta TAD and Nrf2 Neh4/5: role of SMRT recruited to GR in GSTA2 gene repression. Mol Cell Biol. 25, 4150–4165, doi:10.1128/MCB.25.10.4150-4165.2005 (2005).
Yuk, J. M. et al. Vitamin D3 induces autophagy in human monocytes/macrophages via cathelicidin. Cell Host Microbe. 6, 231–243, doi:10.1016/j.chom.2009.08.004 (2009).
Yang, C. S. et al. The AMPK-PPARGC1A pathway is required for antimicrobial host defense through activation of autophagy. Autophagy. 10, 785–802, doi:10.4161/auto.28072 (2014).
Pajares, M. et al. Transcription factor NFE2L2/NRF2 is a regulator of macroautophagy genes. Autophagy. 12, 1902–1916, doi:10.1080/15548627.2016.1208889 (2016).
Li, M. et al. microRNA-146a promotes mycobacterial survival in macrophages through suppressing nitric oxide production. Scientific Reports 6, 23351, doi:10.1038/srep23351 (2016).
Yang, K. et al. Functional RIG-I-like receptors control the survival of mesenchymal stem cells. Cell Death & Disease 4, e967, doi:10.1038/cddis.2013.504 (2013).
Yang, K. et al. miR-155 suppresses bacterial clearance in Pseudomonas aeruginosa-induced keratitis by targeting Rheb. Journal of Infectious Diseases 210, 89–98, doi:10.1093/infdis/jiu002 (2014).
Yang, K. et al. Mesenchymal stem cells detect and defend against gammaherpesvirus infection via the cGAS-STING pathway. Scientific Reports 5, 7820, doi:10.1038/srep07820 (2015).
Wang, J. et al. MicroRNA-155 induction by Mycobacterium bovis BCG enhances ROS production through targeting SHIP1. Molecular Immunology 62, 29–36, doi:10.1016/j.molimm.2014.05.012 (2014).
Acknowledgements
This work was supported by National Natural Science Foundation of China (81571951, 81371764, 81601743); Guangdong Natural Science Foundation (2016A030311001, 2014A030313322, 2014A030310176); Guangdong Province Universities and Colleges Pearl River Scholar Funded Scheme (2012) and Medical Science Research Fund of Guangdong Province (A2016217).
Author information
Authors and Affiliations
Contributions
L.M. and J.W. conceived and designed the study; J.W., R.W., H.W. and X.Y. performed the experiments; L.M., J.W. and Q.W. analyzed the data; J.Y. and W.X. contributed reagents/materials/analysis tools; L.M. and J.W. drafted the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wang, J., Wang, R., Wang, H. et al. Glucocorticoids Suppress Antimicrobial Autophagy and Nitric Oxide Production and Facilitate Mycobacterial Survival in Macrophages. Sci Rep 7, 982 (2017). https://doi.org/10.1038/s41598-017-01174-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-01174-9
This article is cited by
-
Hypercalcemia as a rare manifestation of immune reconstitution inflammatory syndrome (IRIS) in a person living with Human Immunodeficiency Virus (HIV) with disseminated nontuberculous mycobacteriosis
Infection (2024)
-
Metformin combined with rapamycin ameliorates podocyte injury in idiopathic membranous nephropathy through the AMPK/mTOR signaling pathway
Journal of Cell Communication and Signaling (2023)
-
Factors associated with active tuberculosis in Colombian patients with systemic lupus erythematosus: a case-control study
Clinical Rheumatology (2021)
-
Glucocorticoid-mediated ER-mitochondria contacts reduce AMPA receptor and mitochondria trafficking into cell terminus via microtubule destabilization
Cell Death & Disease (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.