Abstract
To discover novel genes underlying amyotrophic lateral sclerosis (ALS), we aggregated exomes from 3,864 cases and 7,839 ancestry-matched controls. We observed a significant excess of rare protein-truncating variants among ALS cases, and these variants were concentrated in constrained genes. Through gene level analyses, we replicated known ALS genes including SOD1, NEK1 and FUS. We also observed multiple distinct protein-truncating variants in a highly constrained gene, DNAJC7. The signal in DNAJC7 exceeded genome-wide significance, and immunoblotting assays showed depletion of DNAJC7 protein in fibroblasts in a patient with ALS carrying the p.Arg156Ter variant. DNAJC7 encodes a member of the heat-shock protein family, HSP40, which, along with HSP70 proteins, facilitates protein homeostasis, including folding of newly synthesized polypeptides and clearance of degraded proteins. When these processes are not regulated, misfolding and accumulation of aberrant proteins can occur and lead to protein aggregation, which is a pathological hallmark of neurodegeneration. Our results highlight DNAJC7 as a novel gene for ALS.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
The sequencing data discussed in this publication were obtained through dbGaP and are available under the following accession codes: MIGen Exome Sequencing: Ottawa Heart (phs000806.v1.p1); MIGen Exome Sequencing: Leicester UK Heart Study (phs001000.v1.p1); Swedish Schizophrenia Population-Based Case-control Exome Sequencing (phs000473.v2.p2); Genome-Wide Association Study of Amyotrophic Lateral Sclerosis (phs000101.v5.p1).
Code availability
Code used to conduct the analysis is provided online (Supplementary Software).
Change history
19 December 2019
An amendment to this paper has been published and can be accessed via a link at the top of the paper.
References
Strong, M. J. et al. Amyotrophic lateral sclerosis–frontotemporal spectrum disorder (ALS-FTSD): revised diagnostic criteria. Amyotroph. Lateral Scler. Frontotemporal Degener. 18, 153–174 (2017).
Al-Chalabi, A., van den Berg, L. H. & Veldink, J. Gene discovery in amyotrophic lateral sclerosis: implications for clinical management. Nat. Rev. Neurol. 13, 96–104 (2017).
Al-Chalabi, A. Perspective: don’t keep it in the family. Nature 550, S112 (2017).
Singh, T. et al. Rare loss-of-function variants in SETD1A are associated with schizophrenia and developmental disorders. Nat. Neurosci. 19, 571–577 (2016).
Mohanan, V. et al. C1orf106 is a colitis risk gene that regulates stability of epithelial adherens junctions. Science 359, 1161–1166 (2018).
Manning, A. et al. A low-frequency inactivating AKT2 variant enriched in the Finnish population is associated with fasting insulin levels and type 2 diabetes risk. Diabetes 66, 2019–2032 (2017).
Hamburg, M. A. & Collins, F. S. The path to personalized medicine. N. Engl. J. Med. 363, 301–304 (2010).
Nelson, M. R. et al. The support of human genetic evidence for approved drug indications. Nat. Genet. 47, 856–860 (2015).
Cirulli, E. T. et al. Exome sequencing in amyotrophic lateral sclerosis identifies risk genes and pathways. Science 347, 1436–1441 (2015).
Smith, B. N. et al. Exome-wide rare variant analysis identifies TUBA4A mutations associated with familial ALS. Neuron 84, 324–331 (2014).
Smith, B. N. et al. Mutations in the vesicular trafficking protein annexin A11 are associated with amyotrophic lateral sclerosis. Sci. Transl Med. 9, eaad9157 (2017).
Kenna, K. P. et al. NEK1 variants confer susceptibility to amyotrophic lateral sclerosis. Nat. Genet. 48, 1037–1042 (2016).
Nicolas, A. et al. Genome-wide analyses identify KIF5A as a novel ALS gene. Neuron 97, 1268–1283.e6 (2018).
van Rheenen, W. et al. Genome-wide association analyses identify new risk variants and the genetic architecture of amyotrophic lateral sclerosis. Nat. Genet. 48, 1043–1048 (2016).
Lackie, R. E. et al. The Hsp70/Hsp90 chaperone machinery in neurodegenerative diseases. Front. Neurosci. 11, 254 (2017).
Swinnen, B. & Robberecht, W. The phenotypic variability of amyotrophic lateral sclerosis. Nat. Rev. Neurol. 10, 661–670 (2014).
Farhan, S. M. et al. The Ontario Neurodegenerative Disease Research Initiative (ONDRI). Can. J. Neurol. Sci. 44, 196–202 (2017).
Farhan, S. M. K., Gendron, T. F., Petrucelli, L., Hegele, R. A. & Strong, M. J. OPTN p.Met468Arg and ATXN2 intermediate length polyQ extension in families with C9orf72 mediated amyotrophic lateral sclerosis and frontotemporal dementia. Am. J. Med. Genet. B Neuropsychiatr. Genet. 177, 75–85 (2018).
Aarsland, D., Zaccai, J. & Brayne, C. A systematic review of prevalence studies of dementia in Parkinson’s disease. Mov. Disord. 20, 1255–1263 (2005).
Hely, M. A., Reid, W. G., Adena, M. A., Halliday, G. M. & Morris, J. G. The Sydney multicenter study of Parkinson’s disease: the inevitability of dementia at 20 years. Mov. Disord. 23, 837–844 (2008).
Fagerberg, L. et al. Analysis of the human tissue-specific expression by genome-wide integration of transcriptomics and antibody-based proteomics. Mol. Cell. Proteomics 13, 397–406 (2014).
Consortium, G. T. The Genotype-Tissue Expression (GTEx) project. Nat. Genet. 45, 580–585 (2013).
Jiang, J. et al. Structural basis of J cochaperone binding and regulation of Hsp70. Mol. Cell 28, 422–433 (2007).
Kampinga, H. H. & Craig, E. A. The HSP70 chaperone machinery: J proteins as drivers of functional specificity. Nat. Rev. Mol. Cell Biol. 11, 579–592 (2010).
Mayer, M. P. & Bukau, B. Hsp70 chaperones: cellular functions and molecular mechanism. Cell. Mol. Life Sci. 62, 670–684 (2005).
Clerico, E. M., Tilitsky, J. M., Meng, W. & Gierasch, L. M. How Hsp70 molecular machines interact with their substrates to mediate diverse physiological functions. J. Mol. Biol. 427, 1575–1588 (2015).
Uddin, M. S. et al. Autophagy and Alzheimer’s disease: from molecular mechanisms to therapeutic implications. Front. Aging Neurosci. 10, 04 (2018).
Irwin, D. J., Lee, V. M. & Trojanowski, J. Q. Parkinson’s disease dementia: convergence of alpha-synuclein, tau and amyloid-beta pathologies. Nat. Rev. Neurosci. 14, 626–636 (2013).
Imarisio, S. et al. Huntington’s disease: from pathology and genetics to potential therapies. Biochem. J. 412, 191–209 (2008).
Brundin, P., Melki, R. & Kopito, R. Prion-like transmission of protein aggregates in neurodegenerative diseases. Nat. Rev. Mol. Cell Biol. 11, 301–307 (2010).
Ross, C. A. & Poirier, M. A. Protein aggregation and neurodegenerative disease. Nat. Med. 10 (Suppl.), S10–S17 (2004).
Winklhofer, K. F., Tatzelt, J. & Haass, C. The two faces of protein misfolding: gain- and loss-of-function in neurodegenerative diseases. EMBO J. 27, 336–349 (2008).
Gidalevitz, T., Ben-Zvi, A., Ho, K. H., Brignull, H. R. & Morimoto, R. I. Progressive disruption of cellular protein folding in models of polyglutamine diseases. Science 311, 1471–1474 (2006).
Voisine, C., Pedersen, J. S. & Morimoto, R. I. Chaperone networks: tipping the balance in protein folding diseases. Neurobiol. Dis. 40, 12–20 (2010).
Brehme, M. et al. A chaperome subnetwork safeguards proteostasis in aging and neurodegenerative disease. Cell Rep. 9, 1135–1150 (2014).
Roodveldt, C. et al. Chaperone proteostasis in Parkinson’s disease: stabilization of the Hsp70/alpha-synuclein complex by Hip. EMBO J. 28, 3758–3770 (2009).
Auluck, P. K., Chan, H. Y., Trojanowski, J. Q., Lee, V. M. & Bonini, N. M. Chaperone suppression of alpha-synuclein toxicity in a Drosophila model for Parkinson’s disease. Science 295, 865–868 (2002).
Wacker, J. L. et al. Loss of Hsp70 exacerbates pathogenesis but not levels of fibrillar aggregates in a mouse model of Huntington’s disease. J. Neurosci. 29, 9104–9114 (2009).
Kovacs, G. G. et al. Prominent stress response of Purkinje cells in Creutzfeldt–Jakob disease. Neurobiol. Dis. 8, 881–889 (2001).
Jones, G., Song, Y., Chung, S. & Masison, D. C. Propagation of Saccharomyces cerevisiae [PSI+] prion is impaired by factors that regulate Hsp70 substrate binding. Mol. Cell. Biol 24, 3928–3937 (2004).
Chen, H. J. et al. The heat shock response plays an important role in TDP-43 clearance: evidence for dysfunction in amyotrophic lateral sclerosis. Brain 139, 1417–1432 (2016).
Udan-Johns, M. et al. Prion-like nuclear aggregation of TDP-43 during heat shock is regulated by HSP40/70 chaperones. Hum. Mol. Genet. 23, 157–170 (2014).
Zhang, Y. J. et al. Phosphorylation regulates proteasomal-mediated degradation and solubility of TAR DNA binding protein-43 C-terminal fragments. Mol. Neurodegener. 5, 33 (2010).
Benatar, M. et al. Randomized, double-blind, placebo-controlled trial of arimoclomol in rapidly progressive SOD1 ALS. Neurology 90, e565–e574 (2018).
Hageman, J. et al. A DNAJB chaperone subfamily with HDAC-dependent activities suppresses toxic protein aggregation. Mol. Cell 37, 355–369 (2010).
Outeiro, T. F. et al. Formation of toxic oligomeric alpha-synuclein species in living cells. PLoS One 3, e1867 (2008).
Crippa, V. et al. The small heat shock protein B8 (HspB8) promotes autophagic removal of misfolded proteins involved in amyotrophic lateral sclerosis (ALS). Hum. Mol. Genet. 19, 3440–3456 (2010).
Sharp, P. S. et al. Protective effects of heat shock protein 27 in a model of ALS occur in the early stages of disease progression. Neurobiol. Dis. 30, 42–55 (2008).
Novoselov, S. S. et al. Molecular chaperone mediated late-stage neuroprotection in the SOD1G93A mouse model of amyotrophic lateral sclerosis. PLoS One 8, e73944 (2013).
Ganna, A. et al. Ultra-rare disruptive and damaging mutations influence educational attainment in the general population. Nat. Neurosci. 19, 1563–1565 (2016).
Ganna, A. et al. Quantifying the impact of rare and ultra-rare coding variation across the phenotypic spectrum. Am. J. Hum. Genet. 102, 1204–1211 (2018).
McLaren, W. et al. The Ensembl variant effect predictor. Genome Biol. 17, 122 (2016).
Lek, M. et al. Analysis of protein-coding genetic variation in 60,706 humans. Nature 536, 285–291 (2016).
Wang, X. Firth logistic regression for rare variant association tests. Front. Genet. 5, 187 (2014).
Lam, H. Y. et al. Performance comparison of whole-genome sequencing platforms. Nat. Biotechnol. 30, 78–82 (2011).
O’Rawe, J. et al. Low concordance of multiple variant-calling pipelines: practical implications for exome and genome sequencing. Genome Med. 5, 28 (2013).
Samocha, K. E. et al. A framework for the interpretation of de novo mutation in human disease. Nat. Genet. 46, 944–950 (2014).
Acknowledgements
The authors thank and acknowledge the consent and cooperation of all study participants. Many thanks are given to F. Cerrato for helping assemble the dataset and providing general project management, and to T. Poterba, J. Bloom, D. King and C. Seed for their assistance in Hail. Data used in this research were in part obtained from the UK MND Collections for MND Research, funded by the MND Association and the Wellcome Trust. The authors thank people from MND and their families for their participation in this project. The project is supported through the following funding organizations under the aegis of the JPND (www.jpnd.eu (United Kingdom, Medical Research Council (MR/L501529/1; MR/R024804/1)), the Economic and Social Research Council (ES/L008238/1)) and through the Motor Neurone Disease Association. This study represents independent research part funded by the National Institute for Health Research (NIHR) Biomedical Research Centre at South London and Maudsley NHS Foundation Trust and King’s College London. Samples used in this research were in part obtained from the UK National DNA Bank for MND Research, funded by the MND Association and the Wellcome Trust. We acknowledge sample management undertaken by Biobanking Solutions funded by the Medical Research Council at the Centre for Integrated Genomic Medical Research, University of Manchester. The CReATe consortium (U54NS092091) is part of the Rare Diseases Clinical Research Network (RDCRN), an initiative of the Office of Rare Diseases Research (ORDR), NCATS. This consortium is funded through collaboration between NCATS and the NINDS. Additional support is provided by the ALS Association (17-LGCA-331). S.M.K.F. was supported by the ALS Canada Tim E. Noël Postdoctoral Fellowship. J.R.K. was supported by the Project ALS Tom Kirchhoff Family Postdoctoral Fellowship and acknowledges K. Mamia and L. T. Kane for their work banking fibroblasts.
Author information
Authors and Affiliations
Consortia
Contributions
S.M.K.F., M.J.D. and B.M.N. conceived and designed the experiments. S.M.K.F., S.D.T., H.P., B.N.S., E.R., G.W., J.W., A.S., A.I., A.A.K., D.A.M., S.G., K.E., R.R., J.L.M., R.S., S.Z., M.B., J.P.T., M.N., M.G., P.J.S., K.E.M., A.A.-C., B.T., C.E.S., D.B.G., M.B.H. and B.M.N. collected samples, prepared samples for analysis or were involved in clinical evaluation. M.B. and J.P.T. were the lead contacts for the CReATe Consortium. S.D.T. and C.E.S. were the lead contacts for the FALS Consortium. D.B.G. and M.B.H. were the lead contacts for the ALSGENS Consortium. S.M.K.F. performed all experiments and executed data analyses. D.P.H., L.E.A., A.E.B. and S.D.T. provided analysis suggestions. J.R.K. completed the cell culture, RNA and protein analyses. S.M.K.F. performed the primary writing of the manuscript with input from D.P.H., C.C., M.J.D. and B.M.N. All authors approved the final manuscript. M.J.D. and B.M.N. supervised the research.
Corresponding authors
Ethics declarations
Competing interests
As a possible conflict of interest, M.N.’s participation is supported by a consulting contract between Data Tecnica International and the National Institute on Aging, NIH, Bethesda, MD, USA. M.N. also consults for Lysosomal Therapeutics Inc, the Michael J. Fox Foundation and Vivid Genomics, among others. The other other authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Figure 1 Initial sample quality control analysis.
(A) Sample call rate. (B) Sample mean depth. (C) Sample mean genotype quality. (D) Sample transition to transversion ratio. (E) Sample heterozygous to homozygous ratio. (F) Sample insertion to deletion ratio. (G) Number of SNPs in each sample. (H) Number of singletons in each sample. N=3,864 ALS cases; N=7,839 controls. The box and whisker plots display the mean, minimum, and maximum.
Supplementary Figure 2 Principal component analysis of ALS dataset with 1000 Genomes.
(A) PC1 and PC2 of ALS dataset with 1000 Genomes. Cases, controls, and the European population is shown. N=3,864 ALS cases; N=7,839 controls. Each point represents one individual. (B) PC1 and PC3 of ALS dataset with 1000 Genomes. Cases, controls, and the European population is shown. (C) PC2 and PC3 of ALS dataset with 1000 Genomes. Cases, controls, and the European population is shown. (D) PC1 and PC2 of ALS dataset with 1000 Genomes. Cases, controls, and the European subpopulations are shown. (E) PC1 and PC3 of ALS dataset with 1000 Genomes. Cases, controls, and the European subpopulations are shown. (F) PC2 and PC3 of ALS dataset with 1000 Genomes. Cases, controls, and the European subpopulations are shown.
Supplementary Figure 3 All models together.
Model 1: Sample variation. The graph display the mean and standard deviation. P-values from firth logistic regression test are also displayed. Multiple test correction P-value: 0.0125. N=3,864 ALS cases; N=7,839 controls. Model 2: Sample variation, sample sex, PC1-PC10. Model 3: Sample variation, sample sex, PC1-PC10, and total exome count (summation of synonymous, benign missense, damaging missense, and PTV). Model 4: Sample variation, sample sex, PC1-PC10, and benign variation count (summation of synonymous and benign missense variation).
Supplementary Figure 4 Exome wide enrichment of SNV-based PTVs and indel-based PTVs in ALS cases.
Extension of Fig. 1: Evaluating the effects of SNV-based and indel-based PTVs within singletons (AC=1), doubletons (AC=2), ultra-rare singletons (AC=1, 0 in DiscovEHR), and rare variants (MAF<0.01 in our dataset, DiscovEHR and ExAC). Odds ratios and 95% confidence intervals for each class of variation are depicted by different colors. P-values are also displayed. Model 3 evaluates sample variation with the covariates, sample sex, PC1-10, and total exome count (summation of synonymous variation, benign missense variation, damaging missense variation, and PTV SNV or PTV indel). Model 4 evaluates sample variation with the covariates, sample sex, PC1-10, and benign variation (summation of synonymous and benign missense variation). The graph display the mean and standard deviation. P-values from firth logistic regression test are also displayed. Multiple test correction P-value: 0.0125. N=3,864 ALS cases; N=7,839 controls.
Supplementary Figure 5 Enrichment of variants in constrained genes in ALS cases.
Extension of Fig. 2a, b: (a) Evaluating the effects of constrained genes in synonymous variants, benign missense variants, damaging missense variants, and PTVs within singletons (AC=1), doubletons (AC=2), ultra-rare singletons (AC=1, 0 in DiscovEHR), and rare variants (MAF<0.01 in our dataset, DiscovEHR and ExAC). Odds ratios and 95% confidence intervals for each class of variation are depicted by different colors. P-values are also displayed. Model 3 evaluates sample variation with the covariates, sample sex, PC1-10, and total exome count (summation of synonymous variation, benign missense variation, damaging missense variation, and PTV). Model 4 evaluates sample variation with the covariates, sample sex, PC1-10, and benign variation (summation of synonymous and benign missense variation). (b) Evaluating the residual effects with constrained genes removed. The graph display the mean and standard deviation. P-values from firth logistic regression test are also displayed. Multiple test correction P-value: 0.0125. N=3,864 ALS cases; N=7,839 controls.
Supplementary Figure 6 Burden analysis of known ALS genes.
Extension of Fig. 3a: Evaluating the effects of known ALS genes in synonymous variants, benign missense variants, damaging missense variants, and PTVs within singletons (AC=1), doubletons (AC=2), ultra-rare singletons (AC=1, 0 in DiscovEHR), and rare variants (MAF<0.01 in our dataset, DiscovEHR and ExAC). Odds ratios and 95% confidence intervals for each class of variation are depicted by different colors. P-values are also displayed. Model 3 evaluates sample variation with the covariates, sample sex, PC1-10, and total exome count (summation of synonymous variation, benign missense variation, damaging missense variation, and PTV). Model 4 evaluates sample variation with the covariates, sample sex, PC1-10, and benign variation (summation of synonymous and benign missense variation). The graph display the mean and standard deviation. P-values from firth logistic regression test are also displayed. Multiple test correction P-value: 0.0125. N=3,864 ALS cases; N=7,839 controls.
Supplementary Figure 7 Analysis of other neurodegenerative disease genes.
Extension of Fig. 3b: Evaluating the effects of genes associated with other neurodegenerative disease (motor neuron diseases: primary lateral sclerosis, progressive muscular atrophy, progressive bulbar palsy, and spinal muscular atrophy; diseases with overlapping phenotypes: frontotemporal dementia, Parkinson’s disease, Pick’s disease, and Alzheimer’s disease) in synonymous variants, benign missense variants, damaging missense variants, and PTVs within singletons (AC=1), doubletons (AC=2), ultra-rare singletons (AC=1, 0 in DiscovEHR), and rare variants (MAF<0.01 in our dataset, DiscovEHR and ExAC). Odds ratios and 95% confidence intervals for each class of variation are depicted by different colors. P-values are also displayed. Model 3 evaluates sample variation with the covariates, sample sex, PC1-10, and total exome count (summation of synonymous variation, benign missense variation, damaging missense variation, and PTV). Model 4 evaluates sample variation with the covariates, sample sex, PC1-10, and benign variation (summation of synonymous and benign missense variation). The graph display the mean and standard deviation. P-values from firth logistic regression test are also displayed. Multiple test correction P-value: 0.0125. N=3,864 ALS cases; N=7,839 controls.
Supplementary Figure 8 Analysis of brain specific genes.
Extension of Fig. 3c: Analysis of brain specific genes in synonymous variants, benign missense variants, damaging missense variants, and PTVs within singletons (AC=1), doubletons (AC=2), ultra-rare singletons (AC=1, 0 in DiscovEHR), and rare variants (MAF<0.01 in our dataset, DiscovEHR and ExAC). Odds ratios and 95% confidence intervals for each class of variation are depicted by different colors. P-values are also displayed. Model 3 evaluates sample variation with the covariates, sample sex, PC1-10, and total exome count (summation of synonymous variation, benign missense variation, damaging missense variation, and PTV). Model 4 evaluates sample variation with the covariates, sample sex, PC1-10, and benign variation (summation of synonymous and benign missense variation). The graph display the mean and standard deviation. P-values from firth logistic regression test are also displayed. Multiple test correction P-value: 0.0125. N=3,864 ALS cases; N=7,839 controls.
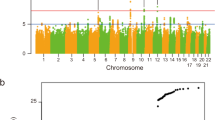
Supplementary Figure 9 Quantile–quantile plots of ultra-rare singletons.
(a) Ultra-rare singletons (AC = 1, 0 in DiscovEHR database) for PTV. PTVs in NEK1 and OPTN, which are known ALS genes, are enriched in ALS cases. NEK1 and OPTN P values are displayed. (b) Ultra-rare singleton (AC = 1, 0 in DiscovEHR database) for damaging missense variants. Damaging missense variants in SOD1 are enriched in ALS cases. SOD1 P value is displayed.
Supplementary Figure 10 DNAJC7 qPCR and immunoblot assays.
(A-B) Relative levels of DNAJC7 mRNA in human fibroblasts using either primers recognizing exons 4 and 6 (A) or exons 13 and 14 (B). Levels for each sample were normalized to GAPDH and displayed relative to the average normalized levels of the healthy controls. Data are displayed as the mean of technical replicates with SD. (C) Uncropped immunoblot of human fibroblast protein lysates probed for the N-terminus of DNAJC7. Similar results were obtained in n=3 independent blots.
Rights and permissions
About this article
Cite this article
Farhan, S.M.K., Howrigan, D.P., Abbott, L.E. et al. Exome sequencing in amyotrophic lateral sclerosis implicates a novel gene, DNAJC7, encoding a heat-shock protein. Nat Neurosci 22, 1966–1974 (2019). https://doi.org/10.1038/s41593-019-0530-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41593-019-0530-0
This article is cited by
-
Genetics screening in an Italian cohort of patients with Amyotrophic Lateral Sclerosis: the importance of early testing and its implication
Journal of Neurology (2024)
-
Rare DNAJC7 Variants May Play a Minor Role in Chinese Patients with ALS
Molecular Neurobiology (2024)
-
Disruption of ER ion homeostasis maintained by an ER anion channel CLCC1 contributes to ALS-like pathologies
Cell Research (2023)
-
Metamorphism in TDP-43 prion-like domain determines chaperone recognition
Nature Communications (2023)
-
Amyotrophic lateral sclerosis: a neurodegenerative disorder poised for successful therapeutic translation
Nature Reviews Drug Discovery (2023)