Abstract
The clearance of damaged myelin sheaths is critical to ensure functional recovery from neural injury. Here we show a previously unidentified role for microvessels and their lining endothelial cells in engulfing myelin debris in spinal cord injury (SCI) and experimental autoimmune encephalomyelitis (EAE). We demonstrate that IgG opsonization of myelin debris is required for its effective engulfment by endothelial cells and that the autophagy–lysosome pathway is crucial for degradation of engulfed myelin debris. We further show that endothelial cells exert critical functions beyond myelin clearance to promote progression of demyelination disorders by regulating macrophage infiltration, pathologic angiogenesis and fibrosis in both SCI and EAE. Unexpectedly, myelin debris engulfment induces endothelial-to-mesenchymal transition, a process that confers upon endothelial cells the ability to stimulate the endothelial-derived production of fibrotic components. Overall, our study demonstrates that the processing of myelin debris through the autophagy–lysosome pathway promotes inflammation and angiogenesis and may contribute to fibrotic scar formation.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Data availability
All data supporting the findings of the current study are available from the corresponding authors upon reasonable request.
References
Ahuja, C. S. et al. Traumatic spinal cord injury. Nat. Rev. Dis. Primers 3, 17018 (2017).
Schwab, M. E. & Bartholdi, D. Degeneration and regeneration of axons in the lesioned spinal cord. Physiol. Rev. 76, 319–370 (1996).
Franklin, R. J. & Ffrench-Constant, C. Remyelination in the CNS: from biology to therapy. Nat. Rev. Neurosci. 9, 839–855 (2008).
Chen, M. S. et al. Nogo-A is a myelin-associated neurite outgrowth inhibitor and an antigen for monoclonal antibody IN-1. Nature 403, 434–439 (2000).
Filbin, M. T. Myelin-associated inhibitors of axonal regeneration in the adult mammalian CNS. Nat. Rev. Neurosci. 4, 703–713 (2003).
Kotter, M. R., Li, W. W., Zhao, C. & Franklin, R. J. Myelin impairs CNS remyelination by inhibiting oligodendrocyte precursor cell differentiation. J. Neurosci. 26, 328–332 (2006).
Syed, Y. A. et al. Antibody-mediated neutralization of myelin-associated EphrinB3 accelerates CNS remyelination. Acta Neuropathol. 131, 281–298 (2016).
Jeon, S. B., Yoon, H. J., Park, S. H., Kim, I. H. & Park, E. J. Sulfatide, a major lipid component of myelin sheath, activates inflammatory responses as an endogenous stimulator in brain-resident immune cells. J. Immunol. 181, 8077–8087 (2008).
Sun, X. et al. Myelin activates FAK/Akt/NF-kappaB pathways and provokes CR3-dependent inflammatory response in murine system. PLoS One 5, e9380 (2010).
Wang, X. et al. Macrophages in spinal cord injury: phenotypic and functional change from exposure to myelin debris. Glia 63, 635–651 (2015).
Napoli, I. & Neumann, H. Protective effects of microglia in multiple sclerosis. Exp. Neurol. 225, 24–28 (2010).
Neumann, H., Kotter, M. R. & Franklin, R. J. Debris clearance by microglia: an essential link between degeneration and regeneration. Brain 132, 288–295 (2009).
Guo, L. et al. Rescuing macrophage normal function in spinal cord injury with embryonic stem cell conditioned media. Mol. Brain 9, 48 (2016).
Ponath, G. et al. Myelin phagocytosis by astrocytes after myelin damage promotes lesion pathology. Brain 140, 399–413 (2017).
Ng, M. T., Stammers, A. T. & Kwon, B. K. Vascular disruption and the role of angiogenic proteins after spinal cord injury. Transl. Stroke Res. 2, 474–491 (2011).
Whetstone, W. D., Hsu, J. Y., Eisenberg, M., Werb, Z. & Noble-Haeusslein, L. J. Blood-spinal cord barrier after spinal cord injury: relation to revascularization and wound healing. J. Neurosci. Res. 74, 227–239 (2003).
Rengarajan, M., Hayer, A. & Theriot, J. A. Endothelial cells use a formin-dependent phagocytosis-like process to internalize the bacterium listeria monocytogenes. PLoS Pathog. 12, e1005603 (2016).
Dini, L. et al. Phagocytosis of apoptotic bodies by liver endothelial cells. J. Cell. Sci. 108, 967–973 (1995).
Steffan, A. M., Gendrault, J. L., McCuskey, R. S., McCuskey, P. A. & Kirn, A. Phagocytosis, an unrecognized property of murine endothelial liver cells. Hepatology 6, 830–836 (1986).
Arnaoutova, I. & Kleinman, H. K. In vitro angiogenesis: endothelial cell tube formation on gelled basement membrane extract. Nat. Protoc. 5, 628–635 (2010).
Smith, M. E. Phagocytic properties of microglia in vitro: implications for a role in multiple sclerosis and EAE. Microsc. Res. Tech. 54, 81–94 (2001).
Gaultier, A. et al. Low-density lipoprotein receptor-related protein 1 is an essential receptor for myelin phagocytosis. J. Cell. Sci. 122, 1155–1162 (2009).
Hart, S. P., Smith, J. R. & Dransfield, I. Phagocytosis of opsonized apoptotic cells: roles for ‘old-fashioned’ receptors for antibody and complement. Clin. Exp. Immunol. 135, 181–185 (2004).
Jones, F. S. The effect of heat on antibodies. J. Exp. Med. 46, 291–301 (1927).
Vermeer, A. W. & Norde, W. The thermal stability of immunoglobulin: unfolding and aggregation of a multi-domain protein. Biophys. J. 78, 394–404 (2000).
Tooze, S. A., Abada, A. & Elazar, Z. Endocytosis and autophagy: exploitation or cooperation?. Cold Spring Harb. Perspect. Biol. 6, a018358 (2014).
Deshmane, S. L., Kremlev, S., Amini, S. & Sawaya, B. E. Monocyte chemoattractant protein-1 (MCP-1): an overview. J. Interferon. Cytokine Res. 29, 313–326 (2009).
Soderblom, C. et al. Perivascular fibroblasts form the fibrotic scar after contusive spinal cord injury. J. Neurosci. 33, 13882–13887 (2013).
Zhu, Y., Soderblom, C., Trojanowsky, M., Lee, D. H. & Lee, J. K. Fibronectin matrix assembly after spinal cord injury. J. Neurotrauma 32, 1158–1167 (2015).
Ignotz, R. A. & Massagué, J. Transforming growth factor-beta stimulates the expression of fibronectin and collagen and their incorporation into the extracellular matrix. J. Biol. Chem. 261, 4337–4345 (1986).
Piera-Velazquez, S., Mendoza, F. A. & Jimenez, S. A. Endothelial to mesenchymal transition (endomt) in the pathogenesis of human fibrotic diseases. J. Clin. Med. 5, E45 (2016).
Winkler, E. A., Bell, R. D. & Zlokovic, B. V. Central nervous system pericytes in health and disease. Nat. Neurosci. 14, 1398–1405 (2011).
Lopes Pinheiro, M. A. et al. Internalization and presentation of myelin antigens by the brain endothelium guides antigen-specific T cell migration. eLife 5, e13149 (2016).
Vargas, M. E., Watanabe, J., Singh, S. J., Robinson, W. H. & Barres, B. A. Endogenous antibodies promote rapid myelin clearance and effective axon regeneration after nerve injury. Proc. Natl Acad. Sci. USA 107, 11993–11998 (2010).
Brosius Lutz, A. et al. Schwann cells use TAM receptor-mediated phagocytosis in addition to autophagy to clear myelin in a mouse model of nerve injury. Proc. Natl Acad. Sci. USA 114, E8072–E8080 (2017).
Gomez-Sanchez, J. A. et al. Schwann cell autophagy, myelinophagy, initiates myelin clearance from injured nerves. J. Cell. Biol. 210, 153–168 (2015).
Hellström, M. et al. Lack of pericytes leads to endothelial hyperplasia and abnormal vascular morphogenesis. J. Cell. Biol. 153, 543–553 (2001).
Li, Y. et al. Pericytes impair capillary blood flow and motor function after chronic spinal cord injury. Nat. Med. 23, 733–741 (2017).
Wu, F., Liu, L. & Zhou, H. Endothelial cell activation in central nervous system inflammation. J. Leukoc. Biol. 101, 1119–1132 (2017).
Kawano, H. et al. Role of the lesion scar in the response to damage and repair of the central nervous system. Cell Tissue Res. 349, 169–180 (2012).
Fernandez, E. & Pallini, R. Connective tissue scarring in experimental spinal cord lesions: significance of dural continuity and role of epidural tissues. Acta Neurochir. (Wien) 76, 145–148 (1985).
Hinz, B. et al. The myofibroblast: one function, multiple origins. Am. J. Pathol. 170, 1807–1816 (2007).
Zhu, Y. et al. Hematogenous macrophage depletion reduces the fibrotic scar and increases axonal growth after spinal cord injury. Neurobiol. Dis. 74, 114–125 (2015).
Logan, A. et al. Effects of transforming growth factor beta 1 on scar production in the injured central nervous system of the rat. Eur. J. Neurosci. 6, 355–363 (1994).
Yoshioka, N. et al. Small molecule inhibitor of type I transforming growth factor-β receptor kinase ameliorates the inhibitory milieu in injured brain and promotes regeneration of nigrostriatal dopaminergic axons. J. Neurosci. Res. 89, 381–393 (2011).
Fee, D. B. et al. Traumatic brain injury increases TGF beta RII expression on endothelial cells. Brain Res. 1012, 52–59 (2004).
Young, W. Spinal cord contusion models. Prog. Brain. Res. 137, 231–255 (2002).
Wu, H. et al. Caveolin-1 is critical for lymphocyte trafficking into central nervous system during experimental autoimmune encephalomyelitis. J. Neurosci. 36, 5193–5199 (2016).
Mi, S. et al. LINGO-1 antagonist promotes spinal cord remyelination and axonal integrity in MOG-induced experimental autoimmune encephalomyelitis. Nat. Med. 13, 1228–1233 (2007).
Gitik, M., Liraz-Zaltsman, S., Oldenborg, P. A., Reichert, F. & Rotshenker, S. Myelin down-regulates myelin phagocytosis by microglia and macrophages through interactions between CD47 on myelin and SIRPα (signal regulatory protein-α) on phagocytes. J. Neuroinflammation 8, 24 (2011).
Hackett, A. R. et al. STAT3 and SOCS3 regulate NG2 cell proliferation and differentiation after contusive spinal cord injury. Neurobiol. Dis. 89, 10–22 (2016).
Bolger, A. M., Lohse, M. & Usadel, B. Trimmomatic: a flexible trimmer for Illumina sequence data. Bioinformatics 30, 2114–2120 (2014).
Kim, D. et al. TopHat2: accurate alignment of transcriptomes in the presence of insertions, deletions and gene fusions. Genome. Biol. 14, R36 (2013).
Li, H. et al. The sequence alignment/map format and SAMtools. Bioinformatics 25, 2078–2079 (2009).
Anders, S., Pyl, P. T. & Huber, W. HTSeq--a Python framework to work with high-throughput sequencing data. Bioinformatics 31, 166–169 (2015).
Love, M. I., Huber, W. & Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 15, 550 (2014).
Wu, H., Wang, C. & Wu, Z. A new shrinkage estimator for dispersion improves differential expression detection in RNA-seq data. Biostatistics 14, 232–243 (2013).
Benjamini, Y. & Hochberg, Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J. R. Stat. Soc. B 57, 289–300 (1995).
Wang, X. et al. MIF produced by bone marrow-derived macrophages contributes to teratoma progression after embryonic stem cell transplantation. Cancer Res. 72, 2867–2878 (2012).
Wu, J., Wrathall, J. R. & Schachner, M. Phosphatidylinositol 3-kinase/protein kinase Cdelta activation induces close homolog of adhesion molecule L1 (CHL1) expression in cultured astrocytes. Glia 58, 315–328 (2010).
Acknowledgements
We thank C. Badland for the artwork of Supplemental Fig. 13. We thank W. Lin and J. Wang for assisting with animal experiments. We thank D. Meckes for providing reagents. We thank R. Nowakowski and G. Hammel for editing the manuscript and thank F. Lin for help with some statistics. This work was supported by a visiting student scholarship granted to T.Z. from China Scholarship Council, Hong Kong Health and Medical Research Fund (03142036) and the National Basic Research Program of China (2014CB502200) to W.W., National Institutes of Health (R01GM072611-4) and National Science Foundation (DMS-1662139) to J.F. and National Science Foundation (DMS-0714589, DMS-1661727) to Y.R.
Author information
Authors and Affiliations
Contributions
Y.R. and Y.Z conceived the study. Y.R., Y.Z., and T.Z. designed the experiments and analyzed the data. T.Z. and Y.Z. executed most of the experiments. L.S. performed flow cytometry, guided MBP ELISA and led the sample preparation for RNA sequencing. S.R.B., H.S. and W.W. established the mouse EAE model and provided EAE spinal cord samples. Y.J. and C.L. designed the CRISPR–Cas9 knockout of Atg5. Y.L. performed spinal cord injection and some SCI. A.J.R. analyzed the RNA-sequencing data. X.W. provided the preliminary phenotype on in vivo microvessel angiogenesis after SCI. Z.C. provided some preliminary SCI tissues. Z.H. assisted in tissues collection and cryosectioning. N.Z. assisted in western blot assay and some quantifications. X.S., J.L., J.F. and W.W. analyzed some data. T.L.M. helped design some of the experiments, contributed to discussion and edited the manuscript and figures. J.L., J.F., C.L., W.W. and G.W. contributed to discussion. Y.Z., Y.R. and T.Z. wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
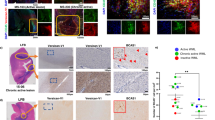
Supplementary Figure 1 Internalization of myelin debris (MBP, green) by microvessels (CD31, red) in injured and uninjured regions of spinal cords from different time points after SCI.
The x-y and x-z views show myelin debris was internalized by microvessels in injured regions of spinal cords from 1-day, 3-day and 5-day SCI mice. The staining was performed in three mice with similar results. Scale bar, 20 μm.
Supplementary Figure 2 MOG-induced EAE disease phases and behavioral assessment.
(a) The graph shows disease progression through the 3 stages described. Arrows indicate the number of animals used for the assessment up until the specified sacrifice date. Following MOG35–55/CFA immunization but before onset, C57BL/6J mice do not display any motor deficits (pre-onset stage), however several days later, at the onset of disease the tail becomes weak or flaccid and the mice start showing hind limb weakness (onset stage). After disease onset, the mice progressively lose hind limb function and may even develop forelimb weakness consequent to hind limb paralysis (disease stage), with a disease peak occurring relatively soon after onset. EAE score is shown as means ± s.e.m. The number of mice collected for EAE score analysis is: n =14 for 7 days post induction; n =8 for 11 days post induction; n = 4 for 15 days post induction. (b) Immunostaining for MBP (red) and nucleus (blue) spinal cord lumbar segment and thoracic segment after 15-day EAE. The arrowheads indicate the demyelinated plaques. Lumbar segment has more severe demyelination than thoracic segment. The staining was performed in two mice with similar results. Scale bar, 500 μm.
Supplementary Figure 3 BMDMϕ engulf myelin debris rapidly.
Detection of engulfed CFSE-myelin debris (green) in BMDMϕ (F4/80, red) exposed to myelin debris for 0, 15 min, 1 hr and 3 hr, respectively. This staining was performed more than five times with similar results. Scale bar, 5 μm.
Supplementary Figure 4 CR3 or Mac2 is involved in BMDMϕ engulfment of myelin debris, but not involved in endothelial cell engulfment of myelin debris.
(a, b) Detection of myelin debris (green) engulfment by BMDMϕ (a) and BMECs (b) that were pre-treated with the indicated neutralizing antibodies for 3 hr, followed by myelin debris treatment for 3 hr and 72 hr, respectively. A combined use of CR3 and Mac2 neutralizing antibodies blocked BMDMϕ uptake of myelin debris, but had no effect on BMEC uptake of myelin debris. This staining was performed three times with similar results. Scale bar, 100 μm.
Supplementary Figure 5 Deficiency of MBP, a proposed ligand for LRP-1 receptor, appears to not affect myelin debris uptake by BMECs.
Detection of engulfed CFSE-myelin debris (CFSE, green or MBP, red) in BMECs (CD31, purple) exposed to myelin debris (isolated from wild-type mice) and MBP-deficient myelin debris (isolated from Shiverer mice) for 72 hr. This staining was performed more than five times with similar results. Scale bar, 20 μm.
Supplementary Figure 6 Serum-dependent engulfment of myelin debris by BMECs.
Detection of engulfed CFSE-myelin debris (green) in BMECs after 48 hr exposure to myelin debris in the presence of 0%, 1% and 5% FBS. This staining was performed more than five times with similar results. Scale bar, 100 μm.
Supplementary Figure 7 Generation and characterization of Atg5-knockout BMEC cell line.
(a) Diagram showing Atg5 gene locus and guide RNA targeting sequence. (b) Verification of genomic editing of Atg5 by CRISPR-Cas9 system using T7E1 assay. T7E1 assay was run in acrylamide gel, which caused inaccurate indication of 100bp DNA ladder. The PCR product band is 440bp. Two digestion bands are 228 and 212bp, which are indistinguishable from each other in the gel. This assay was performed twice with similar results. (c) Functional verification of Atg5-/-BMECs by immunostaining of poly-ubiquitin (green) and p62 (red). The staining was performed twice with similar results. Scale bar, 20 μm. (d) Cell death analysis of Atg5-/- BMECs and drugs-treated wild-type BMECs by propidium iodide (PI) staining. Drug dose and incubation period are corresponding to Fig. 4k. H2O2 treatment was included as positive control. Data are shown as means ± s.e.m. (n = 3 independent experiments). p<0.00001 (****) by unpaired two-sided Student’s t-test.
Supplementary Figure 8 Additional data on in vivo angiogenesis.
(a) Microvessels (CD31, red) in normal spinal cord from uninjured mice and injured spinal cords from mice at 1 week or 6 weeks after SCI. The insets showed the enlarged images. Quantitative data are shown in Fig. 5b. Scale bar, 200 μm; 20 μm in inset images. (b) Representative images and quantification of Ki-67 positive (green) and CD31 (red) microvessels after the indicated injections into normal spinal cords in mice. Scale bar, 100 μm; 50 μm in zoomed images. Data are shown as means ± s.e.m. from 3 mice. Myelin vs PBS, p = 0.6779 (ns); naïve ECs vs PBS, p = 0.0474 (*); myelin-ECs vs PBS, p = 0.0004 (***); myelin-ECs vs naïve ECs, p = 0.0005 (***); myelin-ECs (IgG-inactivated) vs myelin-ECs, p = 0.0005 (***) by unpaired two-sided Student’s t-test.
Supplementary Figure 9 The cellular consequences of necrotic neuronal cells or zymosan engulfment by BMECs and BMDMϕ.
(a) Characteristic morphology of neuronal cells that were differentiated from N2A cells, a mouse neuroblastoma cell line. Neuronal differentiation assay was repeated at least five times. Scale bar, 50 μm. (b) BMECs (red) engulfment of necrotic neuronal cell (green) for 72 hr. BMEC nuclei (Hoechst staining) were shown in pseudo white. Arrowhead indicated the squeezed BMEC nucleus by the engulfed necrotic cell. The staining was performed four times with similar results. Scale bar, 10 μm. (c) Quantification of the percentage of BMDMϕ and BMECs that contained necrotic cells after 6 hr and 72 hr engulfment, respectively. Data are shown as means ± s.e.m. from 3 biologically independent replicates. p = 0.0006 (***) by unpaired two-sided Student’s t-test. (d, e, f) BMECs were treated with or without necrotic cells. (d) Proliferation assessed by counting BMEC nuclei, p = 0.0418 (*). (e) Mcp-1 gene expression detected by q-PCR analysis, p = 0.9510 (ns). (f) α-SMA+/CD31+ cells were counted, p = 0.5369 (ns). Data are shown as means ± s.e.m. from 3 biologically independent cultures by unpaired two-sided Student’s t-test. (g, h) Detection of zymosan engulfment by BMDMϕ and BMECs. Zymosan was labelled by CFSE in green. The staining was performed three times with same results. Scale bar, 10 μm.
Supplementary Figure 10 Analysis of astrocytes’ effects on BMECs using a co-culture system.
(a) Primary mouse astrocytes were isolated and characterized by GFAP staining (green). (b) Diagram showing astrocyte-BMEC co-culture in a transwell. (c) BMEC proliferation after co-cultured with the indicated astrocytes. Myelin-treated BMECs were included as positive control. Data are shown as means ± s.e.m. from 3 biologically independent cultures. Control astrocytes vs medium, p = 0.0712 (ns); LPS-treated astrocytes vs medium, p = 0.1566 (ns); myelin debris-treated ECs vs medium, p = 0.0466 (*) by unpaired two-sided Student’s t-test.
Supplementary Figure 11 Additional data on inflammation.
(a) Quantification of number of GFP+ BMDCs associated with microvessels is shown in Fig. 6a. Data are shown as means ± s.e.m. (n = 3 mice). p = 0.0043(**), p = 0.0003 (***), p<0.00001 (****) by unpaired two-sided Student’s t-test. (b) Quantification of number of Iba1+ cells associated with one microvessel with normal size or increased size in Fig. 6b. Data are shown as means ± s.e.m. (n = 3 mice). p = 0.0114 (*) by paired two-sided Student’s t-test. (c) Representative images showing adhered BMDMϕ (Mac-2, red) on BMECs with the indicated treatments. Quantitative data are shown in Fig. 6c’. Scale bar, 100 μm. (d) Representative images of Iba-1 (green) and GFAP staining (red) after the indicated injections into normal spinal cords in mice. Scale bar, 100 μm; 10 μm in inset images. (e) Quantification of Iba-1 fluorescent intensity shown in d and Fig. 6h. Data are shown as means ± s.e.m. (n = 3 injected mice). Myelin debris vs PBS, p = 0.0527 (ns); naïve ECs vs PBS, p = 0.1942 (ns); myelin-ECs vs PBS, p = 0.0038 (**); myelin-ECs vs naïve ECs, p = 0.0286 (*); myelin-ECs vs myelin debris, p = 0.0067 (**); myelin-ECs (IgG-inactivated) vs myelin-ECs, p = 0.0279 (*) by unpaired two-sided Student’s t-test. (f) Quantification of GFAP fluorescent intensity is shown in d. Data are shown as means ± s.e.m. (n = 3 injected mice). Myelin debris vs PBS, p = 0.1523 (ns); naïve ECs vs PBS, p = 0.3266 (ns); myelin-ECs vs PBS, p = 0.0183 (*); myelin-ECs vs naïve ECs, p = 0.0349 (*); myelin-ECs vs myelin debris, p = 0.044 (*); myelin-ECs (IgG-inactivated) vs myelin-ECs, p = 0.0336 (*) by unpaired two-sided Student’s t-test.
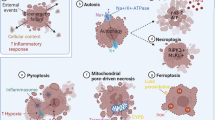
Supplementary Figure 12 Schematic diagram depicting the novel function of microvascular endothelial cells in engulfment and autophagic processing of myelin debris, which in turn boosts secondary injury by promoting inflammation, microvessel dilation, and fibrotic scar formation.
(a) In the injured spinal cord, one of the immediate responses to SCI is the fragmentation of myelin sheaths into myelin debris, which can be quickly cleared by professional phagocytes such as BMDMϕ and microglia. We demonstrated that microvessels and the lining microvascular endothelial cells are able to engulf myelin debris which promote chronic inflammation and pathological healing. The microvessels in injury core are dilated (not depicted), in close vicinity to BMDMϕ, deposit high levels of pro-fibrotic components like collagen and fibronectin. These changes in the injury core, all of which could be stemmed as a result of microvascular engulfment of myelin debris, are closely associated with the progression of SCI. (b) Mechanisms for myelin debris entry, processing and actions in microvascular ECs. IgG opsonization of myelin debris is engulfed by endothelial cells through Fc receptor. Engulfed myelin debris is delivered through autophagosomes to lysosomes for myelin degradation into neutral lipids. Functionally, myelin debris uptake promotes endothelial cells proliferation/angiogenesis, endothelial inflammation and endothelial deposition of pro-fibrotic components, which could contribute to the dilation of microvessels, chronic inflammation and fibrotic scar formation seen in injury core.
Supplementary information
Rights and permissions
About this article
Cite this article
Zhou, T., Zheng, Y., Sun, L. et al. Microvascular endothelial cells engulf myelin debris and promote macrophage recruitment and fibrosis after neural injury. Nat Neurosci 22, 421–435 (2019). https://doi.org/10.1038/s41593-018-0324-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41593-018-0324-9
This article is cited by
-
Proteomics of mouse brain endothelium uncovers dysregulation of vesicular transport pathways during aging
Nature Aging (2024)
-
hBcl2 overexpression in BMSCs enhances resistance to myelin debris-induced apoptosis and facilitates neuroprotection after spinal cord injury in rats
Scientific Reports (2024)
-
Genes in Axonal Regeneration
Molecular Neurobiology (2024)
-
Endothelial cells and macrophages as allies in the healthy and diseased brain
Acta Neuropathologica (2024)
-
Endothelial cell-derived exosomes boost and maintain repair-related phenotypes of Schwann cells via miR199-5p to promote nerve regeneration
Journal of Nanobiotechnology (2023)