Abstract
Anti-CD19 chimeric antigen receptor (CAR) T cell therapy has led to unprecedented responses in patients with high-risk hematologic malignancies. However, up to 60% of patients still experience disease relapse and up to 80% of patients experience CAR-mediated toxicities, such as cytokine release syndrome or immune effector cell-associated neurotoxicity syndrome. We investigated the role of the intestinal microbiome on these outcomes in a multicenter study of patients with B cell lymphoma and leukemia. We found in a retrospective cohort (n = 228) that exposure to antibiotics, in particular piperacillin/tazobactam, meropenem and imipenem/cilastatin (P-I-M), in the 4 weeks before therapy was associated with worse survival and increased neurotoxicity. In stool samples from a prospective cohort of CAR T cell recipients (n = 48), the fecal microbiome was altered at baseline compared to healthy controls. Stool sample profiling by 16S ribosomal RNA and metagenomic shotgun sequencing revealed that clinical outcomes were associated with differences in specific bacterial taxa and metabolic pathways. Through both untargeted and hypothesis-driven analysis of 16S sequencing data, we identified species within the class Clostridia that were associated with day 100 complete response. We concluded that changes in the intestinal microbiome are associated with clinical outcomes after anti-CD19 CAR T cell therapy in patients with B cell malignancies.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
We utilized the BMTagger database, which was built with human genome assembly GRCh38, to remove human contamination from the metagenomic shotgun sequencing samples. Data requests will be reviewed by the corresponding authors at MSK and the University of Pennsylvania. Patient-related data not included in the paper were generated as part of clinical trials and may be subject to patient confidentiality. We will review requests for stool sequence data. Any data and materials that can be shared will be released via a material transfer agreement. Raw ASV counts and annotation, as well as shotgun pathway counts and accompanying clinical annotation, are provided in the Supplementary Data files.
Code availability
The code and the corresponding figures can be accessed at GitHub (https://vdblab.github.io/CART_and_microbiome/). Additionally, we have created an open license with a DOI of the code available at https://doi.org/10.5281/zenodo.5701510.
Change history
17 October 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41591-022-02069-7
References
Park, J. H. et al. Long-term follow-up of CD19 CAR therapy in acute lymphoblastic leukemia. N. Engl. J. Med. 378, 449–459 (2018).
Lee, D. W. et al. T cells expressing CD19 chimeric antigen receptors for acute lymphoblastic leukaemia in children and young adults: a phase 1 dose-escalation trial. Lancet 385, 517–528 (2015).
Davila, M. L. et al. Efficacy and toxicity management of 19-28z CAR T cell therapy in B cell acute lymphoblastic leukemia. Sci. Transl. Med. 6, 224ra225 (2014).
Maude, S. L. et al. Tisagenlecleucel in children and young adults with B-cell lymphoblastic leukemia. N. Engl. J. Med. 378, 439–448 (2018).
Neelapu, S. S. et al. Axicabtagene ciloleucel CAR T-cell therapy in refractory large B-cell lymphoma. N. Engl. J. Med. 377, 2531–2544 (2017).
Schuster, S. J. et al. Tisagenlecleucel in adult relapsed or refractory diffuse large B-cell lymphoma. N. Engl. J. Med. 380, 45–56 (2019).
Wang, M. et al. KTE-X19 CAR T-cell therapy in relapsed or refractory mantle-cell lymphoma. N. Engl. J. Med. 382, 1331–1342 (2020).
Chong, E. A., Ruella, M. & Schuster, S. J. Five-year outcomes for refractory B-cell lymphomas with CAR T-cell therapy. N. Engl. J. Med. 384, 673–674 (2021).
Abramson, J. S. et al. Lisocabtagene maraleucel for patients with relapsed or refractory large B-cell lymphomas (TRANSCEND NHL 001): a multicentre seamless design study. Lancet 396, 839–852 (2020).
Sotillo, E. et al. Convergence of acquired mutations and alternative splicing of CD19 enables resistance to CART-19 immunotherapy. Cancer Discov. 5, 1282–1295 (2015).
Orlando, E. J. et al. Genetic mechanisms of target antigen loss in CAR19 therapy of acute lymphoblastic leukemia. Nat. Med. 24, 1504–1506 (2018).
Ruella, M. et al. Induction of resistance to chimeric antigen receptor T cell therapy by transduction of a single leukemic B cell. Nat. Med. 24, 1499–1503 (2018).
Spiegel, J. Y. et al. Outcomes of patients with large B-cell lymphoma progressing after axicabtagene ciloleucel therapy. Blood 137, 1832–1835 (2021).
Santomasso, B., Bachier, C., Westin, J., Rezvani, K. & Shpall, E. J. The other side of CAR T-cell therapy: cytokine release syndrome, neurologic toxicity, and financial burden. Am. Soc. Clin. Oncol. Educ. Book 39, 433–444 (2019).
Gust, J. et al. Endothelial activation and blood–brain barrier disruption in neurotoxicity after adoptive immunotherapy with CD19 CAR-T cells. Cancer Discov. 7, 1404–1419 (2017).
Santomasso, B. D. et al. Clinical and biological correlates of neurotoxicity associated with CAR T-cell therapy in patients with B-cell acute lymphoblastic leukemia. Cancer Discov. 8, 958–971 (2018).
Taraseviciute, A. et al. Chimeric antigen receptor T cell-mediated neurotoxicity in nonhuman primates. Cancer Discov. 8, 750–763 (2018).
Ruella, M. & Locke, F. L. Beat pediatric ALL MRD: CD28 CAR T and transplant. Blood 134, 2333–2335 (2019).
Guedan, S., Ruella, M. & June, C. H. Emerging cellular therapies for cancer. Annu. Rev. Immunol. 37, 145–171 (2019).
Siegler, E. L. & Kenderian, S. S. Neurotoxicity and cytokine release syndrome after chimeric antigen receptor T cell therapy: insights into mechanisms and novel therapies. Front. Immunol. 11, 1973 (2020).
Karschnia, P. et al. Clinical presentation, management, and biomarkers of neurotoxicity after adoptive immunotherapy with CAR T cells. Blood 133, 2212–2221 (2019).
Viaud, S. et al. The intestinal microbiota modulates the anticancer immune effects of cyclophosphamide. Science 342, 971–976 (2013).
Daillère, R. et al. Enterococcus hirae and Barnesiella intestinihominis facilitate cyclophosphamide-induced therapeutic immunomodulatory effects. Immunity 45, 931–943 (2016).
Uribe-Herranz, M. et al. Gut microbiota modulate dendritic cell antigen presentation and radiotherapy-induced antitumor immune response. J. Clin. Invest. 130, 466–479 (2020).
Yang, K. et al. Suppression of local type I interferon by gut microbiota-derived butyrate impairs antitumor effects of ionizing radiation. J. Exp. Med. 218, e20201915 (2021).
Sivan, A. et al. Commensal Bifidobacterium promotes antitumor immunity and facilitates anti-PD-L1 efficacy. Science 350, 1084–1089 (2015).
Gopalakrishnan, V. et al. Gut microbiome modulates response to anti–PD-1 immunotherapy in melanoma patients. Science 359, 97–103 (2018).
Matson, V. et al. The commensal microbiome is associated with anti-PD-1 efficacy in metastatic melanoma patients. Science 359, 104–108 (2018).
Vétizou, M. et al. Anticancer immunotherapy by CTLA-4 blockade relies on the gut microbiota. Science 350, 1079–1084 (2015).
Routy, B. et al. Gut microbiome influences efficacy of PD-1-based immunotherapy against epithelial tumors. Science 359, 91–97 (2018).
Andrews, M. C. et al. Gut microbiota signatures are associated with toxicity to combined CTLA-4 and PD-1 blockade. Nat. Med. 27, 1432–1441 (2021).
Peled, J. U. et al. Microbiota as predictor of mortality in allogeneic hematopoietic-cell transplantation. N. Engl. J. Med. 382, 822–834 (2020).
Uribe-Herranz, M. et al. Gut microbiota modulates adoptive cell therapy via CD8α dendritic cells and IL-12. JCI Insight 3, e94952 (2018).
Baruch, E. N. et al. Fecal microbiota transplant promotes response in immunotherapy-refractory melanoma patients. Science 371, 602–609 (2021).
Davar, D. et al. Fecal microbiota transplant overcomes resistance to anti-PD-1 therapy in melanoma patients. Science 371, 595–602 (2021).
Pflug, N. et al. Efficacy of antineoplastic treatment is associated with the use of antibiotics that modulate intestinal microbiota. Oncoimmunology 5, e1150399 (2016).
Shono, Y. et al. Increased GVHD-related mortality with broad-spectrum antibiotic use after allogeneic hematopoietic stem cell transplantation in human patients and mice. Sci. Transl. Med. 8, 339ra71 (2016).
Morjaria, S. et al. Antibiotic-induced shifts in fecal microbiota density and composition during hematopoietic stem cell transplantation. Infect. Immun. 87, e00206-19 (2019).
Brook, I., Wexler, H. M. & Goldstein, E. J. C. Antianaerobic antimicrobials: spectrum and susceptibility testing. Clin. Microbiol. Rev. 26, 526–546 (2013).
Hirayama, A. V. et al. The response to lymphodepletion impacts PFS in patients with aggressive non-Hodgkin lymphoma treated with CD19 CAR T cells. Blood 133, 1876–1887 (2019).
Vercellino, L. et al. Predictive factors of early progression after CAR T-cell therapy in relapsed/refractory diffuse large B-cell lymphoma. Blood Adv. 4, 5607–5615 (2020).
Nastoupil, L. J. et al. Standard-of-care axicabtagene ciloleucel for relapsed or refractory large B-cell lymphoma: results from the US Lymphoma CAR T Consortium. J. Clin. Oncol. 38, 3119–3128 (2020).
Lee, D. W. et al. ASTCT consensus grading for cytokine release syndrome and neurologic toxicity associated with immune effector cells. Biol. Blood Marrow Transplant. 25, 625–638 (2019).
Braniste, V. et al. The gut microbiota influences blood–brain barrier permeability in mice. Sci. Transl. Med. 6, 263ra158 (2014).
Ochoa-Repáraz, J. et al. Central nervous system demyelinating disease protection by the human commensal Bacteroides fragilis depends on polysaccharide A expression. J. Immunol. 185, 4101–4108 (2010).
Taur, Y. et al. The effects of intestinal tract bacterial diversity on mortality following allogeneic hematopoietic stem cell transplantation. Blood 124, 1174–1182 (2014).
Bray, J. R. & Curtis, J. T. An ordination of the upland forest communities of southern Wisconsin. Ecol. Monogr. 27, 325–349 (1957).
Segata, N. et al. Metagenomic biomarker discovery and explanation. Genome Biol. 12, R60 (2011).
Dubin, K. et al. Intestinal microbiome analyses identify melanoma patients at risk for checkpoint-blockade-induced colitis. Nat. Commun. 7, 10391 (2016).
Schluter, J. et al. The gut microbiota is associated with immune cell dynamics in humans. Nature 588, 303–307 (2020).
Kanehisa, M. & Goto, S. KEGG: Kyoto Encyclopedia of Genes and Genomes. Nucleic Acids Res. 28, 27–30 (2000).
Cellini, B. et al. Pyridoxal 5′-phosphate-dependent enzymes at the crossroads of host–microbe tryptophan metabolism. Int. J. Mol. Sci. 21, 5823 (2020).
Chaput, N. et al. Baseline gut microbiota predicts clinical response and colitis in metastatic melanoma patients treated with ipilimumab. Ann. Oncol. 28, 1368–1379 (2017).
Frankel, A. E. et al. Metagenomic shotgun sequencing and unbiased metabolomic profiling identify specific human gut microbiota and metabolites associated with immune checkpoint therapy efficacy in melanoma patients. Neoplasia 19, 848–855 (2017).
Arpaia, N. et al. Metabolites produced by commensal bacteria promote peripheral regulatory T-cell generation. Nature 504, 451–455 (2013).
Kespohl, M. et al. The microbial metabolite butyrate induces expression of Th1-associated factors in CD4+ T cells. Front. Immunol. 8, 1036 (2017).
Schuster, S. J. et al. Chimeric antigen receptor T cells in refractory B-cell lymphomas. N. Engl. J. Med. 377, 2545–2554 (2017).
Frey, N. V. et al. Optimizing chimeric antigen receptor T-cell therapy for adults with acute lymphoblastic leukemia. J. Clin. Oncol. 38, 415–422 (2020).
Locke, F. L. et al. Long-term safety and activity of axicabtagene ciloleucel in refractory large B-cell lymphoma (ZUMA-1): a single-arm, multicentre, phase 1-2 trial. Lancet Oncol. 20, 31–42 (2019).
Porter, D., Frey, N., Wood, P. A., Weng, Y. & Grupp, S. A. Grading of cytokine release syndrome associated with the CAR T cell therapy tisagenlecleucel. J. Hematol. Oncol. 11, 35 (2018).
Dethlefsen, L., Huse, S., Sogin, M. L. & Relman, D. A. The pervasive effects of an antibiotic on the human gut microbiota, as revealed by deep 16S rRNA sequencing. PLoS Biol. 6, e280 (2008).
Dethlefsen, L. & Relman, D. A. Incomplete recovery and individualized responses of the human distal gut microbiota to repeated antibiotic perturbation. Proc. Natl Acad. Sci. USA 108, 4554–4561 (2011).
Doan, T. et al. Gut microbial diversity in antibiotic-naive children after systemic antibiotic exposure: a randomized controlled trial. Clin. Infect. Dis. 64, 1147–1153 (2017).
Buffie, C. G. et al. Profound alterations of intestinal microbiota following a single dose of clindamycin results in sustained susceptibility to Clostridium difficile-induced colitis. Infect. Immun. 80, 62–73 (2012).
Sinha, R. et al. Assessment of variation in microbial community amplicon sequencing by the Microbiome Quality Control (MBQC) project consortium. Nat. Biotechnol. 35, 1077–1086 (2017).
Stein-Thoeringer, C. K. et al. Lactose drives Enterococcus expansion to promote graft-versus-host disease. Science 366, 1143–1149 (2019).
Jenq, R. R. et al. Intestinal Blautia is associated with reduced death from graft-versus-host disease. Biol. Blood Marrow Transplant. 21, 1373–1383 (2015).
Callahan, B. J. et al. DADA2: high-resolution sample inference from Illumina amplicon data. Nat. Methods 13, 581–583 (2016).
Camacho, C. et al. BLAST+: architecture and applications. BMC Bioinformatics 10, 421 (2009).
McElreath, R. Statistical Rethinking: a Bayesian Course with Examples in R and Stan (CRC Press, 2020).
Kassambara, A. ggpubr: ‘ggplot2’ Based Publication Ready Plots. R package version 0.4.0 https://cran.r-project.org/web/packages/ggpubr/index.html (2020).
Wickham, H. et al. Welcome to the tidyverse. J. Open Source Softw. 4, 1686 (2019).
Acknowledgements
We acknowledge the Integrated Genomics Operation at MSK, which performed all the 16S and metagenomic shotgun sequencing for the fecal microbiome cohort and healthy controls. This research was supported by the following funding sources: Damon Runyon Physician-Scientist Award (M.Sm.); Burroughs Wellcome Fund Postdoctoral Enrichment Program (M.Sm.); American Society of Hematology-Robert Wood Johnson Foundation and Harold Amos Medical Faculty Development Program (M.Sm.); Fauci Fellowships — National Italian American Foundation and Mario Luvini fellowship grant – Fondazione Ticinese per la Ricerca sul Cancro (G.G.); National Cancer Institute (NCI) grant no. K08CA194256 (S.G.); Lymphoma Research Foundation (LRF) Career Development Award (M.R.); Gilead Research Scholar Award (M.R.); Gabrielle’s Angel Foundation (M.R.); Emerson Collective Award (M.R.); Laffey-McHugh Foundation (M.R.); Berman and Maguire Funds for Lymphoma Research at the University of Pennsylvania (M.R.); NCI grant no. 1K99CA212302 (M.R.); grant no. R00CA212302 (M.R.); Center for Precision Medicine Accelerator Award (M.R. and A.F.); grant no. 1R01CA219871-01A1 (A.F.); University of Pennsylvania-Novartis Alliance (S.G. and C.H.J.); grant no. 1P01CA214278 (C.H.J.); grant no. R01CA226983 (C.H.J.); Scholar in Clinical Research award from the Leukemia and Lymphoma Society (A.G.); American-Italian Cancer Foundation Postdoctoral Research Fellowship and Associazione Italiana contro le Leucemie-Linfomi e Mieloma Milano e Provincia Organizzazione Non Lucrativa di Utilità Sociale (M.P.); grant no. P01 CA23766 (M-A.P.); grant no. P30 CA008748 National Institutes of Health/NCI MSK Cancer Center Support Grant (M-A.P., S.M.D., J.U.P., M.Sm. and M.R.M.B.); LRF Postdoctoral Fellowship Grant (E.A.C.); grant no. K08HL143189 (J.U.P); Parker Institute for Cancer Immunotherapy (J.U.P.); grant nos. R01-CA228358, R01-CA228308, R01-HL147584, P01-CA023766, R01-HL125571, R01-HL123340 and P01-AG052359 (M.R.M.B.); Starr Cancer Consortium (M.R.M.B.); Tri-Institutional Stem Cell Initiative (M.R.M.B.); the Lymphoma Foundation (M.R.M.B.); the Susan and Peter Solomon Divisional Genomics Program (M.R.M.B.); Cycle for Survival (M.R.M.B.); and the Parker Institute for Cancer Immunotherapy (M.R.M.B.).
Author information
Authors and Affiliations
Contributions
M.Sm., M.R., M.R.M.B. and A.F. designed, performed and supervised the research. A.D. performed the bioinformatics analysis on 16S and shotgun sequencing. S.M.D. and G.G. performed the analysis of the antibiotic cohort. J.Sl., A.C. and P.G. coordinated the fecal microbiome collection at MSK, while R.P., G.G., K.V.A., M.R., S.B., S.G., A.G. and A.F. coordinated collection at the University of Pennsylvania. G.A., E.F., E.G.P. aided in the processing of the fecal samples at MSK. P.S.H., E.D., E.R.L., Y.T., and J.C. contributed to data analysis. J.R., T.J., M.P., and A.O.A. assisted in the collection of clinical data. J.H.P., M.L.P., E.H., M-A.P., R.J.B., M.Sa., and I.R. were the principal investigators or provided oversight of the CD19 CAR T cell clinical trials at MSK. S.J.S., D.L.P., E.A.C., A.L.C.G., S.N., J.Sv., D.L.P., M.R., A.G., C.W.F., J.G., S.I.G., C.H.J. and N.F. were the principal investigators or provided oversight of the CD19 CAR T cell clinical trials at the University of Pennsylvania. M.Sm., M.R., M.R.M.B., A.F., A.D., G.G., A.L.C.G. and J.Sc. provided significant intellectual contribution to the study design and research. M.Sm., M.R., M.R.M.B., A.F., J.U.P. and G.G. wrote the manuscript. All authors reviewed and approved the manuscript.
Corresponding authors
Ethics declarations
Competing interests
M.Sm. has served as a consultant for Janssen and has a patent application related to the microbiome (PCT/US2019/056137). A.L.C.G. is currently employed by Xbiome. E.G.P. serves on the advisory board of Diversigen and has received speaker honoraria from Bristol Myers Squibb, Celgene, Seres Therapeutics, MedImmune, Novartis and Ferring Pharmaceuticals and is an inventor on patent application nos. WPO2015179437A1 and WO2017091753A1; he holds patents that receive royalties from Seres Therapeutics. M.A.P. reports honoraria from AbbVie, Astellas Pharma, Bristol Myers Squibb, Celgene, Equilium, Incyte, Karyopharm, Kite Pharma/Gilead, Merck, Miltenyi Biotec, MorphoSys, Novartis, Nektar Therapeutics, Omeros, Takeda and VectivBio. M.A.P. serves on the data and safety monitoring boards of Cidara Therapeutics, Medigene, Sellas Life Sciences and Servier, and the scientific advisory board of NexImmune. M.A.P. has ownership interests in NexImmune and Omeros. M.A.P. has received research support for clinical trials from Incyte, Kite Pharma/Gilead, Miltenyi Biotec and Novartis. J.H.P. has received consulting fees from Amgen, Novartis, Autolus, Kite Pharma, Bristol Myers Squibb, Takeda, Servier, Innate Pharma, Kura Oncology, AstraZeneca, Curocell and Intellia Therapeutics and serves on the scientific advisory board of Artiva. E.A.C. serves on the advisory boards for Novartis, Bristol Myers Squibb and Kite Pharma. J.U.P. reports research funding, intellectual property fees and travel reimbursement from Seres Therapeutics and consulting fees from DaVolterra and from MaaT Pharma. J.U.P. has filed intellectual property applications related to the microbiome (reference nos. 62/843,849, 62/977,908 and 15/756,845). M.R.M.B. has received research support and stock options from Seres Therapeutics and stock options from Notch Therapeutics and Pluto Therapeutics; he has received royalties from Wolters Kluwer, has consulted, received honoraria from or participated in advisory boards for Seres Therapeutics, WindMIL Therapeutics, Merck, Magenta Therapeutics, Frazier Healthcare Partners, Nektar Therapeutics, Notch Therapeutics, Forty Seven, Priothera, Ceramedix, LyGenesis, Pluto Therapeutics, Novartis (spouse), Kite Pharma (spouse), BeiGene (spouse); he has intellectual property licensing with Seres Therapeutics and Juno Therapeutics and holds a fiduciary role on the Foundation Board of DKMS (a nonprofit organization). J.Sv. has served as a consultant for Adaptive, AstraZeneca, Atara, Bristol Myers Squibb, Seattle Genetics, Imbrium and Genmab. J.Sv. has received research funding from AstraZeneca, Bristol Myers Squibb, Incyte, Merck, Seattle Genetics, TG Therapeutics and Pharmacyclics. J.Sc. is cofounder of Postbiotics Plus. J.G. reports research funding from Loxo and serves on the advisory boards of Kite Pharma, Genentech, AbbVie and TG Therapeutics. M.Sa. and R.B. hold patents related to CD19 CAR T cells. M.R., S.I.G. and S.J.S. hold patents related to CD19 CAR T cells. M.R. has served as a consultant for NanoString, Bristol Myers Squibb, GlaxoSmithKline, Bayer and AbClon. M.R. receives research funding from AbClon, NanoString and Beckman Coulter. M.R. is the scientific founder of ViTToria Biotherapeutics. C.H.J. has received grant support from Novartis and has patents related to CAR therapy with royalties paid from Novartis to the University of Pennsylvania. He is also a scientific cofounder and holds equity in DeCART Therapeutics and Tmunity Therapeutics. He serves on the board of AC Immune and is a scientific advisor to Cabaletta Bio, Celldex Therapeutics, Carisma Therapeutics, Viracta Therapeutics and WIRB-Copernicus Group. A.G. has research funding from Novartis, Janssen, Tmunity Therapeutics and CRISPR Therapeutics and honoraria from Janssen and GlaxoSmithKline. The other authors declare no competing interests.
Peer review
Peer review information
Nature Medicine thanks Leo Lahti, Christian Jobin and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Saheli Sadanand was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Impact of antibiotic exposure in patients with hematologic malignancies treated with anti-CD19 CAR T cell therapy according to institution.
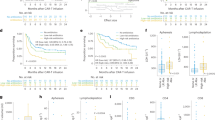
(A) Frequency of antibiotic exposure in the four weeks prior to CD19 CAR T cell infusion in patients with NHL and ALL treated at MSK (upper panel, n = 127) and Penn (bottom panel, n = 101). Purple denotes patients with ALL, while orange denotes patients with NHL. (B and C) Kaplan-Meier curves of overall survival (OS) by log-rank test according to the exposure to P-I-M antibiotics within 4 weeks before CD19 CAR T cell infusion in patients with ALL and NHL treated at MSK (B, n = 127) and Penn (C, n = 101). The dark gray line is estimated Kaplan-Meier survival probability for patients not exposed to P-I-M antibiotics, while the dark yellow line is the estimated probability for patients exposed to P-I-M antibiotics. The shading is the estimated pointwise 95% confidence interval, and the tick marks indicate censored events. Abbreviations: Trimeth./Sulfameth.: trimethoprim/sulfamethoxazole; IV: intravenous; NHL: non-Hodgkin lymphoma; ALL: acute lymphoblastic leukemia; MSK: Memorial Sloan Kettering Cancer Center; Penn: University of Pennsylvania; P-I-M: exposure to either piperacillin/tazobactam, imipenem/cilastatin or meropenem within the 4 weeks before CD19 CAR T cell infusion; Not exposed: patients exposed to non-P-I-M plus patients who did not receive any antibiotics; IV: intravenous; p: p-value.
Extended Data Fig. 2 Impact of any antibiotic exposure in patients with non-Hodgkin lymphoma treated with anti-CD19 CAR T cell therapy.
(A and B) Kaplan-Meier (A) progression-free (PFS) and (B) overall survival (OS) curves by log-rank test in NHL populations according to exposure to any antibiotic within 4 weeks before CD19 CAR T cell infusion (n = 137). The dark gray line is the estimated Kaplan-Meier survival estimates for patients not exposed to any antibiotic treatment, while the dark yellow line is the estimated probability for patients exposed to any antibiotic treatment. The shading indicates the pointwise 95% confidence interval, and the tick marks indicate censored events. (C) Histograms of the frequencies of any grade CRS and ICANS by two-sided Wilcoxon rank-sum test according to the exposure to any antibiotic within the 4 weeks before CD19 CAR T cell infusion in patients with NHL (n = 137). Blue indicates the presence of CRS or ICANS of any grade, while red indicates the absence of CRS or ICANS of any grade. Abbreviations: NHL: non-Hodgkin lymphoma; p: p-value; CRS: cytokine releasing syndrome; ICANS: immune effector cell-associated neurotoxicity.
Extended Data Fig. 3 Survival analysis comparison of different antibiotics exposure on non-Hodgkin lymphoma patients treated with CD19 CAR T cells.
(A and B) Kaplan-Meier curves of (A) progression-free survival (PFS) and (B) overall survival (OS) by log-rank test. Data shows the combined NHL population (n = 137) treated with different antibiotics in the 4 weeks before CD19 CAR T cell infusion. The dark gray line is the estimated Kaplan-Meier survival probability for patients not exposed to P-I-M antibiotics or cefepime (n = 107), the dark yellow line is the estimated probability for patients exposed to P-I-M antibiotics (n = 21), and the dark green line is the estimated probability for patients not exposed to P-I-M antibiotics and exposed to cefepime (n = 9). The shading is the estimated pointwise 95% confidence interval, and the tick marks indicate censored events. P values are shown (log-rank test). Abbreviations: NHL: non-Hodgkin lymphoma; P-I-M: exposure to either piperacillin/tazobactam, imipenem/cilastatin or meropenem within the 4 weeks before CD19 CAR T cell infusion; No P-I-M antibiotic exposure: patients exposed to non-P-I-M plus patients who did not receive any antibiotics within 4 weeks before CD19 CAR T cell infusion; p: p-value.
Extended Data Fig. 4 Survival analysis comparison of piperacillin/tazobactam compared to cefepime exposure in non-Hodgkin lymphoma patients treated with CD19 CAR T cells.
(A and B) Kaplan-Meier curves of (A) progression-free survival (PFS) and (B) overall survival (OS) by log-rank test. Data shows patients from the combined NHL population treated with piperacillin/tazobactam or cefepime in the 4 weeks before CD19 CAR T cell infusion. The dark blue line is the estimated Kaplan-Meier survival probability for patients exposed to piperacillin/tazobactam (n = 18) and the dark green line is the estimated probability for patients exposed to cefepime (n = 12). The shading is the estimated pointwise 95% confidence interval, and the tick marks indicate censored events. P values are shown (log-rank test). P values are shown (log-rank analysis). The p-values are not stratified by Center. Abbreviations: NHL: non-Hodgkin lymphoma; p: p-value.
Extended Data Fig. 5 Survival analysis comparison of P-I-M versus non-P-I-M exposure in non-Hodgkin lymphoma patients receiving at least one antibiotic before treatment with CD19 CAR T cells.
(A and B) Kaplan-Meier curves of (A) progression-free survival (PFS) and (B) overall survival (OS) by log-rank test. Data shows patients from the combined NHL population treated with P-I-M or non-P-I-M antibiotics in the 4 weeks before CD19 CAR T cell infusion. Patients who did not receive any antibiotic in the four weeks prior to CAR T cell infusion are excluded from this analysis. The dark gray line is the estimated Kaplan-Meier survival probability for patients exposed to P-I-M (n = 21) and the dark yellow line is the estimated probability for patients exposed to non-P-I-M (n = 60). The shading is the estimated pointwise 95% confidence interval, and the tick marks indicate censored events. P values are shown (log-rank test). The p-values are not stratified by Center. Abbreviations: NHL: non-Hodgkin lymphoma; p: p-value.
Extended Data Fig. 6 Timing of fecal sample collection relative to the start of conditioning chemotherapy and CD19 CAR T cell infusion.
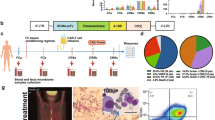
Forty-eight patients were evaluated in the fecal microbiome cohort. Of the forty-eight patients, the fecal samples of fourteen were collected before the start of conditioning chemotherapy, whereas thirty-four fecal samples were collected after the start of conditioning chemotherapy. All the baseline fecal microbiome samples were collected prior to CD19 CAR T cell infusion. The red square denotes the start of conditioning chemotherapy. The black circle denotes the collection of the baseline fecal sample prior to CAR T cell infusion. Day 0 denotes the day of CD19 CAR T cell infusion.
Extended Data Fig. 7 Flow diagram of the fecal microbiome sample collection.
Fifty-one unique patients were collected upon informed consent. Of the fifty-one patients, one patient did not have sufficient fecal material for sequencing and two patients failed during the amplification or quality control step. Following these exclusions, there were forty-eight patients in the fecal microbiome cohort. Of these patients, we successfully amplified and sequenced the 16S ribosomal RNA gene with ≥ 200 reads per sample from forty-five patients. Forty-five patients passed quality control measures for metagenomic shotgun sequencing. There were three non-overlapping patients in the 16S and metagenomic shotgun sequencing cohorts. Hence, there were 48 unique patients in the fecal microbiome cohort.
Extended Data Fig. 8 The association of intestinal microbiota and clinical response in recipients of CD19 CAR T cells, including subset analysis institution.
(A to E) All data reported in this figure are based on 16S rRNA gene sequencing data. (A) Inverse Simpson diversity index of the fecal microbiome in the baseline fecal samples by institution, MSK (n = 26) and Penn (n = 19), compared to healthy volunteers (n = 30) by two-sided Wilcoxon rank-sum test. The middle line is the median, the box limits represent the upper and lower quartiles, the whiskers note 1.5x the interquartile range, and the dots represent the individual data points. (B to C) Beta-diversity was calculated using the Bray-Curtis dissimilarity between a reference point defined by the average of healthy volunteers and each of 30 samples from healthy volunteers. Healthy volunteers were compared to the 45 baseline patient samples (B) and by institution (MSK n = 26; Penn n = 19) (C) by two-sided Wilcoxon rank-sum test. This healthy volunteer cohort has been investigated in a prior study32. The middle line is the median, the box limits represent the upper and lower quartiles, the whiskers note 1.5x the interquartile range, and the dots represent the individual data points. (D to E) Patient samples with higher (one standard deviation above the mean) (red) or lower (one standard deviation below the mean) (blue) Inverse Simpson diversity index. The coefficients for the predicted probability of (C) Day 100 CR and (D) toxicity by Inverse Simpson diversity index. The coefficients correspond to the Bayesian models for Day 100 CR and toxicity, respectively, in Fig. 3e.
Extended Data Fig. 9 Principal Coordinates Analysis (PCoA) visualization of beta-diversity of fecal samples of CAR T cell patients and healthy volunteers.
All data reported in this figure are based on 16S rRNA gene sequencing data. Fecal microbiome composition of the CAR T cell patients (n = 45) and healthy volunteers (n = 30) was displayed in a PCoA. Composition was assessed using beta-diversity calculated with Bray-Curtis dissimilarity. Data visualized at the genus level. Red dots indicate CAR T cells patients and green dots indicate healthy volunteers.
Extended Data Fig. 10 Boxplots of the relative abundance of selected taxa from LEfSe of Day 100 CR.
All data reported in this figure are based on 16S rRNA gene sequencing data from patients (n = 45). The relative abundance of Bacteroides, Bifidobacterium, Blautia, Faecalibacterium, Longicatena, and Ruminococcus are presented. Data is categorized by patients who did not achieve a Day 100 CR (No), and patients who achieved a Day 100 CR (Yes). Dots indicate relative abundance of the baseline fecal sample from a CAR T cell patient. Two-sided Wilcoxon rank-sum test was used to calculate the p-values, and the p-values were adjusted for multiple hypothesis testing. The middle line is the median, the box limits represent the upper and lower quartiles, the whiskers note 1.5x the interquartile range, and the dots represent the individual data points.
Supplementary information
Supplementary Information
Supplementary Tables 1 and 2 and Supplementary Figs. 1–3.
Supplementary Data 1
Sample ID (sid), clinical outcomes (day 100 CR and toxicity, center (MSK (M) or University of Pennsylvania (P)) and inverse Simpson diversity index of baseline fecal samples by 16S rRNA gene sequencing.
Supplementary Data 2
Annotation of the bacterial taxa identified by each ASV.
Supplementary Data 3
ASV counts by 16S rRNA gene sequencing for baseline fecal samples.
Supplementary Data 4
Shotgun pathway counts by metagenomic shotgun sequencing for baseline fecal samples.
Supplementary Data 5
Sample ID (sid), center (MSK (M) or University of Pennsylvania (P)) and clinical outcomes (day 100 CR and toxicity).
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Smith, M., Dai, A., Ghilardi, G. et al. Gut microbiome correlates of response and toxicity following anti-CD19 CAR T cell therapy. Nat Med 28, 713–723 (2022). https://doi.org/10.1038/s41591-022-01702-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-022-01702-9
This article is cited by
-
Gastrointestinal infections and gastrointestinal haemorrhage are underestimated but serious adverse events in chimeric antigen receptor T-cell recipients: A real-world study
Cancer Gene Therapy (2024)
-
Utilization of the microbiome in personalized medicine
Nature Reviews Microbiology (2024)
-
Bacteria and bacteriophage consortia are associated with protective intestinal metabolites in patients receiving stem cell transplantation
Nature Cancer (2024)
-
Altered microbial bile acid metabolism exacerbates T cell-driven inflammation during graft-versus-host disease
Nature Microbiology (2024)
-
A multi-cohort phase 1b trial of rituximab in combination with immunotherapy doublets in relapsed/refractory follicular lymphoma
Annals of Hematology (2024)