Abstract
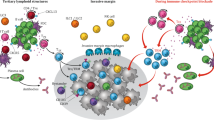
Inhibitors of the PD-1–PD-L1 axis have been approved as therapy for many human cancers. In spite of the evidence for their widespread clinical activity, little is known about the immunological alterations that occur in human cancer tissue after PD-1 blockade. We developed and employed a patient-derived tumor fragment platform to dissect the early immunological response of human tumor tissue to ex vivo PD-1 blockade. We observed that the capacity of immune cells to be reactivated ex vivo was predictive of clinical response, and perturbation analyses identified tumor-resident T cells as a key component of this immunological response. In addition, through combined analysis of baseline properties and immune response capacity, we identified a new subgroup of infiltrated tumors that lacks the capacity to respond to PD-1 blockade. Finally, the baseline presence of tertiary lymphoid structures and their components correlated with the capacity of cancers to undergo intratumoral immune cell reactivation.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
All relevant flow cytometry, immunohistochemistry and cytokine/chemokine data are provided as supplementary data.
Code availability
No custom code was developed. All code used in this study is either specified in the Methods or available from the corresponding author.
References
Xin Yu, J. et al. Trends in clinical development for PD-1/PD-L1 inhibitors. Nat. Rev. Drug Discov. 19, 163–164 (2020).
Yost, K. E. et al. Clonal replacement of tumor-specific T cells following PD-1 blockade. Nat. Med. 25, 1251–1259 (2019).
Wu, T. D. et al. Peripheral T cell expansion predicts tumour infiltration and clinical response. Nature 579, 274–278 (2020).
Zhang, J. et al. Compartmental analysis of T-cell clonal dynamics as a function of pathologic response to neoadjuvant PD-1 blockade in resectable non-small cell lung cancer. Clin. Cancer Res. 26, 1327–1337 (2020).
Strauss, L. et al. Targeted deletion of PD-1 in myeloid cells induces antitumor immunity. Sci. Immunol. 5, eaay1863 (2020).
Mayoux, M. et al. Dendritic cells dictate responses to PD-L1 blockade cancer immunotherapy. Sci. Transl. Med. 12, eaav7431 (2020).
Tumeh, P. C. et al. PD-1 blockade induces responses by inhibiting adaptive immune resistance. Nature 515, 568–571 (2014).
Amaria, R. N. et al. Neoadjuvant immune checkpoint blockade in high-risk resectable melanoma. Nat. Med. 24, 1649–1654 (2018).
Huang, A. C. et al. A single dose of neoadjuvant PD-1 blockade predicts clinical outcomes in resectable melanoma. Nat. Med. 25, 454–461 (2019).
Neal, J. T. et al. Organoid modeling of the tumor immune microenvironment. Cell 175, 1972–1988.e16 (2018).
Jenkins, R. W. et al. Ex vivo profiling of PD-1 blockade using organotypic tumor spheroids. Cancer Discov. 8, 196–215 (2018).
Blank, C. et al. PD-L1/B7H-1 inhibits the effector phase of tumor rejection by T cell receptor (TCR) transgenic CD8+ T cells. Cancer Res. 64, 1140–1145 (2004).
Gros, A. et al. PD-1 identifies the patient-specific CD8+ tumor-reactive repertoire infiltrating human tumors. J. Clin. Invest. 124, 2246–2259 (2014).
Gros, A. et al. Prospective identification of neoantigen-specific lymphocytes in the peripheral blood of melanoma patients. Nat. Med. 22, 433–438 (2016).
Thommen, D. S. et al. A transcriptionally and functionally distinct PD-1+ CD8+ T cell pool with predictive potential in non-small-cell lung cancer treated with PD-1 blockade. Nat. Med. 24, 994–1004 (2018).
Herbst, R. S. et al. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature 515, 563–567 (2014).
Sharma, P. & Allison, J. P. The future of immune checkpoint therapy. Science 348, 56–61 (2015).
Hegde, P. S., Karanikas, V. & Evers, S. The where, the when, and the how of immune monitoring for cancer immunotherapies in the era of checkpoint inhibition. Clin. Cancer Res. 22, 1865–1874 (2016).
Galon, J. & Bruni, D. Approaches to treat immune hot, altered and cold tumours with combination immunotherapies. Nat. Rev. Drug Discov. 18, 197–218 (2019).
Sanmamed, M. F. et al. Changes in serum interleukin-8 (IL-8) levels reflect and predict response to anti-PD-1 treatment in melanoma and non-small-cell lung cancer patients. Ann. Oncol. 28, 1988–1995 (2017).
Schalper, K. A. et al. Elevated serum interleukin-8 is associated with enhanced intratumor neutrophils and reduced clinical benefit of immune-checkpoint inhibitors. Nat. Med. 26, 688–692 (2020).
Yuen, K. C. et al. High systemic and tumor-associated IL-8 correlates with reduced clinical benefit of PD-L1 blockade. Nat. Med. 26, 693–698 (2020).
Wherry, E. J. et al. Molecular signature of CD8+ T cell exhaustion during chronic viral infection. Immunity 27, 670–684 (2007).
Baitsch, L. et al. Extended co-expression of inhibitory receptors by human CD8 T-cells depending on differentiation, antigen-specificity and anatomical localization. PLoS ONE 7, e30852 (2012).
Thommen, D. S. et al. Progression of lung cancer is associated with increased dysfunction of T cells defined by coexpression of multiple inhibitory receptors. Cancer Immunol. Res. 3, 1344–1355 (2015).
Kurtulus, S. et al. Checkpoint blockade immunotherapy induces dynamic changes in PD-1−CD8+ tumor-infiltrating T cells. Immunity 50, 181–194.e6 (2019).
Siddiqui, I. et al. Intratumoral Tcf1+PD-1+CD8+ T cells with stem-like properties promote tumor control in response to vaccination and checkpoint blockade immunotherapy. Immunity 50, 195–211.e10 (2019).
Miller, B. C. et al. Subsets of exhausted CD8+ T cells differentially mediate tumor control and respond to checkpoint blockade. Nat. Immunol. 20, 326–336 (2019).
Sade-Feldman, M. et al. Defining T cell states associated with response to checkpoint immunotherapy in melanoma. Cell 175, 998–1013.e20 (2018).
Krishna, S. et al. Stem-like CD8 T cells mediate response of adoptive cell immunotherapy against human cancer. Science 370, 1328–1334 (2020).
Duhen, T. et al. Co-expression of CD39 and CD103 identifies tumor-reactive CD8 T cells in human solid tumors. Nat. Commun. 9, 2724 (2018).
Byrne, A. et al. Tissue-resident memory T cells in breast cancer control and immunotherapy responses. Nat. Rev. Clin. Oncol. 17, 341–348 (2020).
Edwards, J. et al. CD103+ tumor-resident CD8+ T cells are associated with improved survival in immunotherapy-naïve melanoma patients and expand significantly during anti-PD-1 treatment. Clin. Cancer Res. 24, 3036–3045 (2018).
Menares, E. et al. Tissue-resident memory CD8+ T cells amplify anti-tumor immunity by triggering antigen spreading through dendritic cells. Nat. Commun. 10, 4401 (2019).
Ansel, K. M. et al. A chemokine-driven positive feedback loop organizes lymphoid follicles. Nature 406, 309–314 (2000).
Gettinger, S. N. et al. A dormant TIL phenotype defines non-small cell lung carcinomas sensitive to immune checkpoint blockers. Nat. Commun. 9, 3196 (2018).
Schietinger, A. et al. Tumor-specific T cell dysfunction is a dynamic antigen-driven differentiation program initiated early during tumorigenesis. Immunity 45, 389–401 (2016).
Philip, M. et al. Chromatin states define tumour-specific T cell dysfunction and reprogramming. Nature 545, 452–456 (2017).
Scheper, W. et al. Low and variable tumor reactivity of the intratumoral TCR repertoire in human cancers. Nat. Med. 25, 89–94 (2019).
Rizvi, N. A. et al. Cancer immunology. Mutational landscape determines sensitivity to PD-1 blockade in non-small cell lung cancer. Science 348, 124–128 (2015).
Helmink, B. A. et al. B cells and tertiary lymphoid structures promote immunotherapy response. Nature 577, 549–555 (2020).
Petitprez, F. et al. B cells are associated with survival and immunotherapy response in sarcoma. Nature 577, 556–560 (2020).
Cabrita, R. et al. Tertiary lymphoid structures improve immunotherapy and survival in melanoma. Nature 577, 561–565 (2020).
Decalf, J., Albert, M. L. & Ziai, J. New tools for pathology: a user’s review of a highly multiplexed method for in situ analysis of protein and RNA expression in tissue. J. Pathol. 247, 650–661 (2019).
Rodriques, S. G. et al. Slide-seq: a scalable technology for measuring genome-wide expression at high spatial resolution. Science 363, 1463–1467 (2019).
Vickovic, S. et al. High-definition spatial transcriptomics for in situ tissue profiling. Nat. Methods 16, 987–990 (2019).
Roederer, M., Nozzi, J. L. & Nason, M. C. SPICE: exploration and analysis of post-cytometric complex multivariate datasets. Cytometry A 79, 167–174 (2011).
McInnes, L., Healy, J. & Melville, J. UMAP: uniform manifold approximation and projection for dimension reduction. Preprint at arXiv https://arxiv.org/abs/1802.03426v3 (2020).
Samusik, N., Good, Z., Spitzer, M. H., Davis, K. L. & Nolan, G. P. Automated mapping of phenotype space with single-cell data. Nat. Methods 13, 493–496 (2016).
Dijkgraaf, F. E. et al. Tissue patrol by resident memory CD8+ T cells in human skin. Nat. Immunol. 20, 756–764 (2019).
Acknowledgements
We thank D. Peters and the NKI-AVL Core Facility for Molecular Pathology & Biobanking for supplying and processing the NKI-AVL Biobank material, the NKI-AVL flow cytometry facility for assistance with sorting and flow cytometric analyses, L. Rozeman for assistance with the acquisition of clinical data and all members of the Thommen and Schumacher laboratories for helpful discussions. This work was supported by a PhD fellowship from the Portuguese Foundation for Science and Technology (no. SFRH/BD/52042/2012) through the Graduate Program in Basic and Applied Biology to P.V., by a KWF Young investigator grant (no. 12046) and the Swiss National Science Foundation (no. P300PB_177881) to D.S.T. and by an ERC AdG SENSIT grant (no. 742259) to T.N.S.
Author information
Authors and Affiliations
Contributions
T.N.S. and D.S.T. conceived the study. P.V., L.M.R., A.Z., J.B.A.G.H., T.N.S. and D.S.T. conceived the experimental design. P.V., M.d.B., L.M.R., S.H.H., S.B., M.v.d.B. and P.H. performed the experiments. P.V., M.d.B., L.M.R., T.N.S. and D.S.T. analyzed the data. A.B., C.U.B., K.J.H. and K.M. contributed to the collection of patient samples and data. J.S. and K.M. performed the pathological characterization of patient samples. L.M.R., J.S. and K.M. performed the digital image analysis. P.V., T.N.S. and D.S.T. wrote the manuscript. All authors reviewed and edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
T.N.S. is an advisor to Adaptive Biotechnologies, Allogene Therapeutics, Merus, Neogene Therapeutics and Scenic Biotech. He is a recipient of research support from Merck KGaA, a stockholder in Allogene Therapeutics, Merus, Neogene Therapeutics and Scenic Biotech and is venture partner at Third Rock Ventures, all outside of the current work. D.S.T. received research funding from Bristol Myers Squibb, outside of the current work. The other authors declare no competing interests.
Additional information
Peer review information Nature Medicine thanks Karuna Ganesh and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Javier Carmona was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Development and validation of ex vivo patient-derived tumor fragment (PDTF) cultures.
a, Macroscopic image of a lung tumor processed into PDTFs. PDTFs from distinct tumor regions were mixed to offset the effects of tumor heterogeneity and were immediately cryopreserved. b, Flow plots showing total live cells and T cell (CD45+CD3+), non-T cell (CD45+CD3−) and non-immune cell subsets (CD45−CD3−) of digested PDTFs and culture supernatant after 48 h of culture in absence of the matrix (left), and quantification of these subsets in three tumor samples (right). c, Viability and lymphocyte efflux (measured by manual counting of cells in culture supernatants) of PDTFs cultured for 48 h in either medium, collagen, or complete matrix (top), and quantification of T cells (CD45+CD3+), non-T cells (CD45+CD3−) and non-immune cells (CD45−CD3−) in PDTFs cultured in these conditions. Representative flow plots (middle) and mean and s.e.m. of three PDTF cultures (bottom) are depicted. d, Correlation matrix depicting the Spearman co-efficient (left) and heatmap (right) of cytokine/chemokine measurements performed at 24, 36, and 48 h of PDTF cultures for four different tumors. The log2 fold change (L2FC) relative to the matching 12 h sample is depicted. e, Antibody penetration assays, comparing overlap in fluorescence of two antibodies recognizing different epitopes of the same target. Antibodies were either added to the culture at indicated time points, or were used for subsequent staining after tissue processing into single cell suspensions (anti-CD8, left), or tissue slides (anti-EpCAM, right). Shown is one of 4 independent experiments. f, Correlation matrix depicting the Spearman co-efficient (left) and heatmap (right) of cytokine/chemokine measurements at 48 h in two parallel cultures from each tumor for six different tumors. Normalized values for each parameter are depicted.
Extended Data Fig. 2 Ex vivo treatment of PDTFs with anti-PD-1.
a, Representative flow plot (LU019) and correlation of PD-1 expression analyzed directly ex vivo and after 48 h of culture on either CD8+ (left) or CD4+ (right) T cells (n = 37). b, T cell activation (LU019) and cytokine/chemokine secretion upon either anti-PD-1 or a matching human IgG4 (S228P) isotype control treatment. The bar graph indicates the fold change compared to the untreated culture. c, Comparison of ex vivo anti-PD-1 treatment for 24 h and 48 h, expressed as log2 fold change (L2FC) relative to untreated PDTFs (n = 3). d, Study cohort overview.
Extended Data Fig. 3 Reproducibility of PDTF responses.
a, T cell activation and cytokine/chemokine profiling upon PD-1 blockade in two independently performed PDTF cultures for five responding tumors and one non-responding tumor. Normalized delta values between the treated and the untreated condition are depicted. b, Immunological responses of individual tumor fragments. The fold change and P value for each parameter of each untreated or anti-PD-1 treated fragment was calculated against the mean of all untreated fragments (n = 3 PDTF-R tumors). c, Fold change and P value for each parameter of averaged anti-PD-1 treated versus untreated PDTFs from the same experiment as in (b). Significance in b and c were calculated for each parameter and comparison by unpaired two-sample t test with two-stage linear step-up procedure of Benjamini, Krieger and Yekutieli. d, Violin plots showing the range of response scores (as defined in Extended Data Fig. 4) for 100 randomly selected combinations of 1-7 individual tumor fragments for both the untreated and anti-PD-1 treated condition. Data are derived from the experiment shown in (b). The dashed line indicates the response score when using data from all 8 tumor fragments, as done in standard PDTF cultures, the grey shaded area indicates a positive response score. Note that the data also emphasize heterogeneity in response capacity – but not response type - of individual tumor fragments of a given tumor (b).
Extended Data Fig. 4 Development of the PDTF response score.
a, Potential of indicated markers defined by the area under the receiver operator curve (AUROC) to discriminate between anti-PD-1 responsive and non-responsive tumors. b, ROC curves of the 12 parameters selected for the score. As a comparison, plots for two parameters with no discriminative value (IL8 and IL17F) are depicted. c, Weighting of the twelve parameters used in the score. d, PDTF response scores for 11 tumors for which two or three lesions from distinct localizations were tested (Supplementary Table 3). Tumors with concordant (8/11) and discordant (3/11) responses are indicated. e, PDTF response score and matched clinical response for lesions derived from either lymph node metastases (left, n = 27) or primary tumors (P)/distant metastases (M) (right, n = 18). Significance was determined by Fisher’s exact test.
Extended Data Fig. 5 T cell activation upon ex vivo PD-1 blockade in PDTF-R and PDTF-NR tumors.
a, Expression of T cell activation markers in CD4+ T cells (top) and CD8+ T cells (bottom) from untreated or anti-PD-1 treated PDTF cultures, as assessed by flow cytometry. Data are from the same responding tumor sample as in Fig. 2a (LU012). b, Expression of T cell activation markers in CD3+ T cells and secretion of T cell effector cytokines in PDTFs that were either untreated, treated with PD-1 blockade, or treated with anti-CD3 antibodies, as assessed by flow cytometry and bead-based immunoassay, respectively. Data from a representative infiltrated non-responding tumor sample (LU010) are depicted. c, Quantification of CD137 and OX40 expression on CD3+ T cells in PDTFs that were either untreated, treated with PD-1 blockade, or treated with anti-CD3 antibodies (n = 10 PDTF-NRs). *P < 0.05, **P < 0.01 by Kruskal-Wallis test corrected for multiple comparisons.
Extended Data Fig. 6 Immunological responses upon ex vivo PD-1 blockade.
Comparison of additional parameters assessed in untreated and anti-PD-1 treated PDTFs that are not depicted in Fig. 2c. Values are displayed separately for PDTF-R and PDTF-NR. *P < 0.05, **P < 0.01, ***P < 0.001 by two-tailed Wilcoxon test.
Extended Data Fig. 7 Modulation of the anti-PD-1 response by LCK inhibition or IFNγ receptor blockade.
a-b, Titration of Lck inhibitor (LCKi) (a) and IFNγ receptor 1 blocking antibody (aIFNγR1) (b) in PBMCs stimulated with anti-CD3/anti-CD28 for 48 h. LCKi was added 2 h and aIFNγR1 1 h before PD-1 blockade at the indicated concentrations. The differential inhibition of CD137 expression on CD3+ T cells and CXCL10 secretion reflect interference at the level of T cell activation (LCKi), or downstream, at the level of IFNγ-induced gene expression (aIFNγR1). Viability was comparable for both compounds and at all dosing levels. Shown are 2 independent experiments. Bars and error bars indicate mean + s.e.m. c, Flow plot depicting blockade of the IFNγR1 in the presence of aIFNγR1 during culture, as measured using a fluorescently labeled aIFNγR1 antibody that binds to the same epitope. d, Flow plots depicting activation of CD8+ T cells, as measured by CD137 expression, and CD4+ T cells, as measured by OX40 expression, in PDTFs that were either uncultured or treated with anti-PD-1, anti-PD-1+aIFNγR1 or anti-PD-1+LCKi for 48 h. One representative example of 8 PDTF cultures is depicted. e, T cell activation and cytokine/chemokine profiling of 8 PDTF-R tumors treated with anti-PD-1, anti-PD-1 + αIFNgR1, or anti-PD-1+LCKi for 48 h. Data are expressed as log2 fold change (L2FC) relative to the untreated condition.
Extended Data Fig. 8 Immune composition of PDTF-R and PDTF-NR tumors.
a, Flow plots depicting the gating strategy and tSNE clustering of immune subsets. b, Quantification of indicated immune cell subsets within total immune cells (CD45+) for the four distinct TME subtypes (desert, excluded, infiltrated non-responders, and infiltrated-responders, n = 37). Shown are mean + /- s.d., *P < 0.05, **P < 0.01 by Kruskal-Wallis test. c, Correlation between the percentage of CD8+ T cells quantified by either flow cytometry or IHC in matched samples (n = 35). Significance was determined by linear regression analysis. d, Digital quantification of CD8+ T cells in intratumoral and stromal regions displayed per tumor type (n = 35). Bars and error bars indicate mean + s.d..
Extended Data Fig. 9 Steady-state cytokine and chemokine profiles.
Quantification of additional parameters assessed in untreated PDTFs after 48 h of culture (n = 37) that are not depicted in Fig. 3g. Values are displayed separately for desert, excluded, infiltrated PDTF-NR and infiltrated PDTF-R tumors. Shown are mean + /- s.d., *P < 0.05, **P < 0.01 by Kruskal-Wallis test corrected for multiple comparisons.
Extended Data Fig. 10 T cell differentiation states and tumor reactivity across distinct TME types.
a, SPICE analysis47 visualizing the co-expression of distinct immune checkpoints on CD8+ T cells within the TME subtypes (as indicated by the pie arc). Means of all tumors per TME subtype (Desert, n = 10; Excluded, n = 5; Infiltrated PDTF-NR, n = 6; Infiltrated PDTF-R, n = 13) are depicted. b-d, Quantification of TCF-1, CD39, and CD103 expression on PD-1+CD8+ T cells by flow cytometry (n = 34). Shown are mean + /- s.d., **P < 0.01 by Kruskal-Wallis test corrected for multiple comparisons. e, Violin plots showing the expression of PD-1, CD39, CD103, and TCF-1 in the clusters defined in Fig. 5a. f, Detection of HLA class-I on total live cells in the absence or presence of an HLA I blocking antibody. g, Tumor reactivity (measured as production of either IFNγ, TNFα, or both) within expanded CD4+ T cells in the absence or presence of tumor digest for five PDTF-R and six PDTF-NR tumors.
Supplementary information
Supplementary Information
Supplementary Figs. 1–4 and Supplementary Tables 1–3.
Supplementary Data 1
PDTF culture setup and validation.
Supplementary Data 2
PDTF cultures with ex vivo PD-1 blockade and perturbations.
Supplementary Data 3
Immune composition and tumor microenvironment analyses.
Rights and permissions
About this article
Cite this article
Voabil, P., de Bruijn, M., Roelofsen, L.M. et al. An ex vivo tumor fragment platform to dissect response to PD-1 blockade in cancer. Nat Med 27, 1250–1261 (2021). https://doi.org/10.1038/s41591-021-01398-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-021-01398-3
This article is cited by
-
Fcγ receptors and immunomodulatory antibodies in cancer
Nature Reviews Cancer (2024)
-
BEHAV3D: a 3D live imaging platform for comprehensive analysis of engineered T cell behavior and tumor response
Nature Protocols (2024)
-
Tumor histoculture captures the dynamic interactions between tumor and immune components in response to anti-PD1 in head and neck cancer
Nature Communications (2024)
-
GITR and TIGIT immunotherapy provokes divergent multicellular responses in the tumor microenvironment of gastrointestinal cancers
Genome Medicine (2023)
-
Newly developed 3D in vitro models to study tumor–immune interaction
Journal of Experimental & Clinical Cancer Research (2023)