Abstract
Coronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), is a new human disease with few effective treatments1. Convalescent plasma, donated by persons who have recovered from COVID-19, is the acellular component of blood that contains antibodies, including those that specifically recognize SARS-CoV-2. These antibodies, when transfused into patients infected with SARS-CoV-2, are thought to exert an antiviral effect, suppressing virus replication before patients have mounted their own humoral immune responses2,3. Virus-specific antibodies from recovered persons are often the first available therapy for an emerging infectious disease, a stopgap treatment while new antivirals and vaccines are being developed1,2. This retrospective, propensity score–matched case–control study assessed the effectiveness of convalescent plasma therapy in 39 patients with severe or life-threatening COVID-19 at The Mount Sinai Hospital in New York City. Oxygen requirements on day 14 after transfusion worsened in 17.9% of plasma recipients versus 28.2% of propensity score–matched controls who were hospitalized with COVID-19 (adjusted odds ratio (OR), 0.86; 95% confidence interval (CI), 0.75–0.98; chi-square test P value = 0.025). Survival also improved in plasma recipients (adjusted hazard ratio (HR), 0.34; 95% CI, 0.13–0.89; chi-square test P = 0.027). Convalescent plasma is potentially effective against COVID-19, but adequately powered, randomized controlled trials are needed.
Similar content being viewed by others
Main
SARS-CoV-2 is a positive-sense, single-stranded RNA virus belonging to the family Coronaviridae. Humans infected with SARS-CoV-2 may develop COVID-19, which manifests across a wide spectrum of clinical severity ranging from a mild upper respiratory tract illness to a diffuse viral pneumonia causing acute respiratory failure, with sequelae including acute lung injury, multiorgan dysfunction syndrome and death4,5,6. Although protection from COVID-19 infection or disease has yet to be directly correlated with levels of circulating antibodies against SARS-CoV-2 (ref. 7), providing virus-neutralizing antibodies in the form of convalescent plasma may expedite disease resolution before the maturation of a patient’s own humoral response1,8,9. Historical evidence supports the potential of convalescent plasma transfusions to treat a variety of infectious diseases, including influenza, Argentine hemorrhagic fever and SARS10,11,12; however, their effectiveness in treating other infectious diseases, such as Ebola13, remains inconclusive.
To date, published clinical data regarding convalescent plasma transfusions as treatment for COVID-19 include single-arm, observational studies from China, the United States, Italy5,7,14,15,16 and, most recently, two randomized open-label trials that were terminated before full enrollment17,18. In respiratory infections specifically, the strongest evidence suggests that the benefit of passive antibody transfer is most demonstrable in patients who were treated within days of symptom onset11,19,20,21. Therefore, we hypothesized that treatment of patients with convalescent plasma early in the disease course would reduce morbidity and mortality associated with COVID-19. Here, preliminary outcomes are presented for 39 patients with severe to life-threatening COVID-19 who received convalescent plasma transfusions at a single center, The Mount Sinai Hospital (MSH), in New York City.
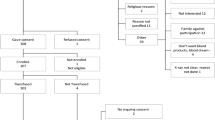
Adult patients admitted to MSH between 24 March 2020 and 8 April 2020 were screened for eligibility to receive a COVID-19 convalescent plasma transfusion under the criteria established for the U.S. Food and Drug Administration (FDA) single-patient emergency investigational new drug (eIND) process (Supplementary Text 1). Forty-five applications requesting individual patient eIND authorization to administer COVID-19 convalescent plasma were submitted to and approved by the FDA. Four patients improved and two patients withdrew consent before receipt of plasma, leaving 39 evaluable patients who received COVID-19 convalescent plasma under compassionate-use guidelines. The average age of convalescent plasma recipients was 55 (standard deviation (s.d.) ± 13) years (Table 1). Approximately two-thirds of the cohort were male and one-third were female, similar to the proportions of men and women with severe disease in previous studies4. Convalescent plasma recipients were, on average, obese (mean body mass index (BMI), 31.7 ± 6.0 kg m−2) but generally had few other baseline comorbidities. The median duration of symptoms before initial presentation was 7 d (range, 0–14 d). The median time between admission and transfusion was 4 d (range, 0–7 d). On the day of transfusion, the majority of the convalescent plasma recipients (34 patients; 87%) required supplemental oxygen via a noninvasive delivery device. Four convalescent plasma recipients (10%) were mechanically ventilated at the time of transfusion.
Convalescent plasma recipients were retrospectively propensity-score matched to control patients who were admitted during the same period, between 24 March 2020 and 8 April 2020. Analyses were performed at 1:4 and 1:2 ratios (convalescent plasma recipients to controls), with and without replacement. In sampling without replacement, each untreated control can be matched to only one treated case, while sampling with replacement allows each untreated control to be matched by similarity in propensity score to more than one treated case. Each method has distinct advantages22; thus, we used both methods for sensitivity analyses. After matching was established, control patients were retrospectively chart reviewed by a medical data team who were blinded to information about the matched convalescent plasma recipient. Predictors not readily available in the system database, such as duration of symptoms before hospital admission and exposures to specific pharmacotherapies (azithromycin, hydroxychloroquine, broad-spectrum antibiotics, therapeutic-dose anticoagulation, corticosteroids, remdesivir, mesenchymal stem cells and interleukin (IL)-1 and IL-6 inhibitors), were manually collected after matching. Subsequently, duration of symptoms before hospital admission was not significantly different between the controls and convalescent plasma recipients for both the 1:2 (Wilcoxon rank-sum test, P = 0.307) and 1:4 (Wilcoxon rank-sum test, P = 0.968) analyses. There were also no significant differences between convalescent plasma recipients and control patients in exposures to the aforementioned pharmacotherapies, except for therapeutic anticoagulation (P = 0.004 for the 1:4 ratio and P = 0.018 for the 1:2 ratio, chi-square test; Supplementary Table 1). Overall, the distribution of the logit propensity score–matched controls was within range of the convalescent plasma recipients, as opposed to the logit propensity score of all patients with COVID-19 system wide who were admitted during the same period (Extended Data Fig. 1).
The day of convalescent plasma transfusion was defined as ‘day 0’ for convalescent plasma recipients. For each control patient, ‘day 0’ was defined as the same hospital day (number of days into their admission) that corresponded to the hospital day on which their matched convalescent plasma recipient received the transfusion (Supplementary Table 2). Although matching was not enforced by admission date, the 156 controls in the 1:4 matched analysis were admitted to the hospital within a median of 4 d (interquartile range (IQR), 2–6 d) of the convalescent plasma recipients to whom they were matched. Control patients were admitted slightly earlier (median, 1 d before; IQR, 5 d before to 4 d after) than the convalescent plasma recipients.
Convalescent plasma recipients and control patients in the 1:4 analysis were 100% matched on their supplemental oxygen requirement on day 0; 69.2% of patients in both groups received high-flow oxygen and 10.3% received invasive mechanical ventilation (Supplementary Table 3). By day 14, clinical conditions had worsened in 17.9% of the convalescent plasma recipients and in 28.2% of the control patients. The covariates-adjusted OR for worsening oxygenation on day 14 was 0.86 (95% CI, 0.75–0.98; chi-square test, P = 0.025). The effect of plasma on oxygenation status appeared to be confounded by the use of therapeutic anticoagulants (unadjusted versus adjusted anticoagulation versus fully adjusted OR: 0.90 versus 0.84 versus 0.86) but not by other drug classes or by duration of symptoms before admission (OR, 0.90–0.91). The plasma group also showed a reduction in the proportion of patients with worsened oxygenation status earlier in hospitalization, but the group differences did not reach statistical significance on day 1 (OR, 0.98; 95% CI, 0.92–1.04; chi-square test, P = 0.443) or day 7 (OR, 0.95; 95% CI 0.84–1.08; chi-square test, P = 0.435).
As of the end of the study (1 May 2020), 12.8% of convalescent plasma recipients and 24.4% of the 1:4 matched control patients had died (21.6% in the 1:2 matched dataset), and 71.8% and 66.7% (68.9%) had been discharged alive, respectively. The median follow-up time was 11 d (range, 1–28 d) for the plasma group and 9 d (range, 0–31 d) for the control group. Overall, survival probability was greater in convalescent plasma recipients than controls (Fig. 1). Without covariate adjustment, the survival benefit of convalescent plasma was significant in the 1:4 matched dataset (HR, 0.39; 95% CI 0.15–0.99; chi-square test P = 0.048; Fig. 2), with potential benefit in the 1:2 matched dataset (HR, 0.47; 95% CI 0.17–1.28; chi-square test P = 0.14). No evidence of confounding was found for any covariates in the survival analysis. Following covariate adjustment (adjusting for duration of symptoms before admission and for exposure to therapeutic anticoagulation and broad-spectrum antibiotics), the 1:4 matched model continued to show significant survival benefit of convalescent plasma (HR, 0.34; 95% CI, 0.13–0.89; chi-square test, P = 0.027). When aggressively adjusting for additional covariates, including mechanical ventilation, corticosteroids, azithromycin, interventional antivirals and IL-6 inhibitors, convalescent plasma remained significantly associated with improved survival (HR, 0.31; 95% CI, 0.12–0.82; chi-square test, P = 0.018). Subgroup analyses showed significant survival benefits of convalescent plasma within the subgroups of patients who were not intubated, had a shorter duration of symptoms and received therapeutic anticoagulation, in comparison to the matched untreated control groups (Fig. 2). However, the effects of convalescent plasma within these subgroups were not significantly different from its effects within the complementary subgroups (chi-square tests for homogeneity for intubated versus non-intubated, P = 0.207; symptoms >7 d versus ≤7 d before admission, P = 0.415; and treated versus not treated with therapeutic anticoagulation, P = 0.306). Because the effects of convalescent plasma were not significantly different within these subgroup pairs, its effect on survival in patients who were not intubated, had a shorter duration of symptoms and received therapeutic anticoagulation also should not be interpreted as significantly better than its effect on survival in those who were intubated, had a longer symptom duration and did not receive anticoagulation therapy. Therefore, these results suggest but do not confirm a benefit of convalescent plasma in non-intubated patients, those with less than a week of symptoms and those also receiving therapeutic anticoagulation. These subgroup findings remain inconclusive, potentially due to a lack of statistical power.
As of 1 May 2020, 5 (12.8%) of 39 convalescent plasma recipients and 38 (24.4%) of 156 1:4 matched control patients had died. The median follow-up time was 11 d (range 1–28 d) for the plasma group and 9 d (0–31 d) for the control group. Overall, improved survival was observed for the plasma versus the control group.
In a covariates-adjusted Cox model, convalescent plasma transfusion was significantly associated with improved survival (HR, 0.34; 95% CI, 0.13–0.89; chi-square test, P = 0.027). Subgroup analyses showed significant survival benefits of convalescent plasma in patients who were not intubated, had a shorter duration of symptoms and received therapeutic anticoagulation. However, these subgroups were not significantly different from their complementary subgroups (chi-square test for homogeneity P = 0.207, P = 0.415 and P = 0.306, respectively). All statistical tests are two-sided.
Before donation, potential convalescent plasma donors were prescreened for SARS-CoV-2-specific serum antibodies with the MSH-ELISA anti-IgG COVID-19 assay, a research assay23,24 that was transitioned to clinical use in the Mount Sinai Laboratory25. Only donors with an MSH-ELISA serum IgG titer of ≥1:320 (n = 25) were referred for plasmapheresis.
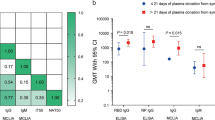
Donors presented for plasma donation at a median of 4 d (IQR, 1–5 d) after their screening antibody test was performed. Stored samples of donor serum and plasma were available for 24 of 25 donors, who provided a total of 76 units of plasma to 38 recipients (Fig. 3). We assessed the total anti-spike IgG titers in transfused plasma units in a lab-based ELISA. We also performed a microneutralization assay to quantify the capacity of donor serum antibodies to inhibit the replication of authentic SARS-CoV-2; 50% neutralization titers are expressed as the reciprocal serum dilution at which in vitro virus infectivity was halved, relative to a serum-free control infection. We observed a correlation between the total anti-spike IgG titer of the donor serum samples, as measured by the clinical MSH-ELISA assay, and both the total anti-spike IgG titers of the plasma units (Spearman correlation coefficient (ρ), 0.83; P < 0.001; Fig. 3a) and the 50% neutralizing titers of the donor serum samples (Spearman ρ, 0.65; P < 0.001; Fig. 3b). Donor serum samples with an MSH-ELISA titer of 1:320 had a geometric mean 50% neutralizing titer (GM-NT) of 1:46 (95% CI, 1:18–1:120); for sera with an MSH-ELISA titer of 1:960, GM-NT was 1:174 (95% CI, 1:71–1:427); and sera measured at an MSH-ELISA titer of ≥1:2,880 had a GM-NT of 1:338 (95% CI, 1:91–1:1,252). However, we observed no correlation between donor neutralization titers and convalescent plasma-recipient outcomes at the end of the study period (Spearman ρ, 0.083; P = 0.62; Fig. 3c). Analysis of variance demonstrated a nonsignificant trend toward higher neutralizing titers in the sera of donors who provided convalescent plasma to the group of recipients that remained hospitalized at the end of the study (Kruskal–Wallis test, P = 0.07; Dunn’s multiple-comparisons test, adjusted P = 0.17 for hospitalized versus discharged and adjusted P = 0.10 for hospitalized versus expired). The majority of convalescent plasma recipients were discharged by 1 May 2020 (n = 28), with few (n = 11) who died or remained hospitalized at the end of the study for comparison. This small sample size limits our ability to draw robust conclusions about the level of neutralizing antibodies necessary to improve convalescent plasma-recipient outcomes. During this time frame, all available MSH-ELISA testing capacity was prioritized for the screening of potential convalescent plasma donors; thus, we were not able to measure anti-SARS-CoV-2 antibody titers before or after transfusion in convalescent plasma recipients.
a, Total anti-SARS-CoV-2 spike protein IgG titers in serum, obtained from plasma donors by clinical MSH-ELISA assay, positively correlate with the total anti-spike IgG titers in plasma units, measured by a lab-based ELISA (Spearman ρ, 0.83; P < 0.001). b, Total anti-spike IgG titers from donors also correlate with the reciprocal serum dilution required to neutralize virus infectivity by 50%, as measured by microneutralization assay (Spearman ρ, 0.65; P < 0.001). c, No correlation was observed between donor neutralization titers and convalescent plasma-recipient outcomes at the end of the study period (Spearman ρ, 0.083; P = 0.62). Plasma ELISAs (a) were performed once (n = 1 replicate per plasma sample), and microneutralization assays (b and c) were performed in duplicate (n = 2 replicates per serum sample). Data from n = 24 donors (a and b) and n = 38 recipients (c) were used to calculate Spearman correlation coefficients and P values. One serum sample showed no measurable neutralization activity in vitro; this point is shown below the dotted line indicating the limit of detection (LOD) (b and c). Donor serum neutralization titer was unavailable for one convalescent plasma recipient who expired; donor titers for the remaining four deceased recipients are shown (c). All statistical tests are two-sided.
Among the 39 convalescent plasma recipients, no serious adverse events were judged to be directly caused by convalescent plasma transfusion. One patient died within 7 d of transfusion, on day 3 after transfusion, of cardiac arrest in the setting of progressive hypoxemia due to COVID-19. The other four deaths during the study period, all due to COVID-19 complicated by multiorgan failure and shock, occurred on days 8, 9, 13 and 14 after transfusion. No suspected occurrences of transfusion-associated adverse events, such as transfusion-associated circulatory overload or transfusion-related acute lung injury were reported.
This initial assessment offers evidence in support of convalescent plasma transfusion as an effective intervention in COVID-19. Preliminary data suggest a mortality benefit, but greater numbers and a randomized trial design are needed to draw definitive conclusions about the efficacy of convalescent plasma for the treatment of COVID-19.
Although controls were retrospectively identified by propensity score matching, the conclusions drawn from these data are not as robust as those from a prospective, randomized, placebo-controlled trial. An important potential confounder in our analysis is the higher proportion of convalescent plasma recipients who were anticoagulated compared to their matched controls. We cannot exclude the possibility that convalescent plasma recipients benefited from generally more assertive clinical management by their primary physican teams. However, the requirement for informed consent should mitigate provider bias to some extent, given that patients who were offered convalescent plasma could and did decline to give consent. Our analyses also did not show that convalescent plasma recipients received any other therapies, including several investigational agents, at a higher rate than controls. Ultimately, our retrospective data cannot address the underlying reason for this discrepancy, and our analysis must be viewed with this caveat in mind.
As in our retrospective study, a prospective, open-label, randomized trial conducted by Li et al.18 also found a trend toward the benefit of convalescent plasma only in the subgroup of less severely ill patients, in which convalescent plasma recipients were significantly more likely to improve clinically than controls (HR, 2.15; 95% CI, 1.07–4.32; P = 0.03). However, no significant difference was observed in the subgroup with life-threatening disease (HR, 0.88; 95% CI, 0.30–2.63; P = 0.83), and the interaction by disease severity failed to reach statistical significance (P value for interaction = 0.17); thus, Li et al. concluded that the findings for the severe and life-threatening subgroups should not be interpreted as significantly different18. Similarly, in our cohort, we found that convalescent plasma recipients who were not mechanically ventilated at the time of transfusion were significantly less likely to die than their matched controls (HR, 0.23; 95% CI, 0.05–0.98; chi-square test, P = 0.46), whereas we were unable to observe an effect of convalescent plasma in recipients who were mechanically ventilated at the time of transfusion (HR 0.79; 95% CI, 0.22–2.79; chi-square test, P = 0.716). While these results are consistent with past literature demonstrating that passive antibody-transfer therapies are most efficacious early in disease11,19,20,21, the effect of convalescent plasma was not significantly different in the non-intubated and intubated recipient groups (chi-square test for homogeneity, P = 0.207), and thus, like Li et al.18, we conclude that the effect of convalescent plasma in these two subgroups should not be interpreted as significantly different. Importantly, the number of mechanically ventilated convalescent plasma recipients in our study is small, and larger randomized trials are still needed to address uncertainties about the effect of convalescent plasma and to define more clearly the patient populations in whom convalescent plasma may have benefit.
This study has many unique strengths. Data from three different time frames (baseline, before transfusion and the day of transfusion) informed the matching of controls to cases to maximize their similarity. New York City has a large and very diverse population, and its metropolitan area was among the earliest and hardest hit by the COVID-19 pandemic in the United States. Over this study’s 16-d enrollment period (24 March 2020 to 8 April 2020), the Mount Sinai Health System (MSHS) admitted 4,152 patients with confirmed COVID-19. This large pool from which to draw control patients permitted an aggressive matching algorithm based on treatment propensity and enabled 1-to-4 matching of cases to controls.
In addition, the efficacy of passive antibody transfer relies heavily on the quality of the donor convalescent plasma. We show that the serum neutralizing antibody titers, measured against a clinical isolate of wild-type SARS-CoV-2, correlate well with the serum antibody titers measured by the MSH-ELISA assay used to prioritize the convalescent donors that we referred for plasmapheresis, both in the donor group presented here (Fig. 3b) and in a larger cohort of individuals screened for serum antibodies within our health system25. Others have reported similar findings26,27,28. We did not observe a correlation between donor serum neutralizing titers and convalescent plasma-recipient outcomes (Fig. 3c), with the caveats that, (1) all of our donors were prescreened to have relatively high anti-SARS-CoV-2 antibody titers before donation and, (2) the sample size is small.
No significant transfusion-related morbidity or mortality was observed in this convalescent plasma-recipient cohort, nor in a much larger national, multicenter cohort29,30; however, potential harms are associated with plasma transfusion. Allergic reactions to plasma are typically mild and self-limited, but anaphylaxis, while rare, can occur. Plasma contains procoagulants, whose additive effects are unknown in COVID-19. Given that COVID-19 is independently associated with hypercoagulability, additional caution should be exercised in patients with acute thrombotic events31. Keeping these risks in mind, additional studies are needed to confirm these findings and draw more definitive conclusions about the efficacy of convalescent plasma transfusion for the treatment of COVID-19 in different populations.
Methods
Ethics and regulatory oversight
Both convalescent plasma treatment and retrospective analysis of data from our electronic medical record database were performed with the oversight of the Icahn School of Medicine at Mount Sinai (ISMMS) Institutional Review Board (IRB nos. 20-03574 and 20-03489). Convalescent plasma recipients were treated under compassionate use, via single-patient eIND applications to the FDA. As required by federal law, the ISMMS IRB was notified of every eIND application, FDA authorization was sought and received for each treated patient before transfusion, and all patients, or their legally authorized representatives, gave informed consent. As a retrospective analysis of compassionate-use treatment data, the study was neither prospectively designed nor registered on clinicaltrials.gov, nor was a data safety monitoring board prospectively convened to oversee this study.
Eligibility and selection of convalescent plasma recipients
Between 24 March 2020 and 8 April 2020, 4,152 patients were hospitalized for COVID-19 in the MSHS. During this period, adult patients admitted to MSH were screened for eligibility to receive a COVID-19 convalescent plasma transfusion under the criteria established for the FDA single-patient eIND process, published 24 March 2020 (Supplementary Text 1). FDA eIND criteria included: age ≥18 years, severe or immediately life-threatening COVID-19 and patient or proxy ability to provide informed consent. Severe disease included at least one of the following: dyspnea; respiratory frequency ≥30 per min; blood oxygen saturation ≤93%; partial pressure of arterial oxygen to fraction of inspired oxygen ratio <300; and/or progression of lung infiltrates by >50% within 24–48 h. Life-threatening disease included at least one of the following: respiratory failure, septic shock and multiple-organ dysfunction or failure. There were no published exclusion criteria. As required by federal law (Code of Federal Regulations; 21CFR312.305 and 21CFR312.310), all patients treated under eIND criteria met the expanded access use requirements as documented on FDA form 3926, which was submitted for each individual patient and reviewed and approved by the FDA before transfusion. Initially, convalescent plasma inventory was limited relative to the number of eligible convalescent plasma recipients under eIND criteria; thus, patients were further prioritized by the following considerations, which were flexible according to plasma supply: (1) ABO blood type; (2) duration of symptoms; (3) length of stay, inclusive of admission at a transferring hospital; and (4) baseline functional status and comorbidities.
Forty-five applications requesting individual patient eIND authorization to administer COVID-19 convalescent plasma were submitted to and approved by the FDA between 28 March and 8 April 2020. Sample size was not determined prospectively. The first eIND application was submitted upon receipt of the first convalescent plasma units from the New York Blood Center, and the last was submitted immediately before the MSHS joined the national Expanded Access Protocol (www.uscovidplasma.org/). Six patients consented to receive convalescent plasma and were granted FDA authorization under eIND criteria, but were not treated; four improved without convalescent plasma and two withdrew consent before transfusion. These six eINDs were withdrawn. Between the end of the study period (1 May 2020) and now (24 July 2020), two additional convalescent plasma recipients died of complications of multiorgan failure due to COVID-19, on days 42 and 88 after transfusion, for an overall death rate of 17.9%. The FDA was notified of all seven deaths and these eINDs were withdrawn. Thirty convalescent plasma patients were discharged from the hospital, for an overall discharge rate of 76.9%; these eINDs were withdrawn. One convalescent plasma recipient remains hospitalized as of 24 July 2020, and this eIND remains open.
Convalescent plasma transfusion
Convalescent plasma donors were screened for SARS-CoV-2 antibody titers with the MSH-ELISA anti-IgG COVID-19 assay, a two-step, spike-protein-directed ELISA23,24 adapted for emergency clinical use and performed by the Mount Sinai Laboratory25. Donors with total anti-spike IgG titers of ≥1:320 on the MSH-ELISA were referred for blood collection at the New York Blood Center, which performed the plasmapheresis and then returned convalescent plasma units and segments (apheresis tubing containing residual plasma) to MSH. Segments were frozen at −20 °C for research use. Convalescent plasma recipients were transfused with two units of ABO type-compatible convalescent plasma. The majority of recipients received both units from a single donor. Each unit, approximately 250 ml in volume, was infused over 1–2 h. Convalescent plasma recipients were monitored every 15 min for signs of transfusion-related reactions and then followed for outcomes after the transfusion.
Propensity score matching of controls to convalescent plasma recipients
A propensity score–matched analysis was conducted within Epic electronic health records from the MSHS from 24 March 2020 to 8 April 2020. Analyses of patient data were performed using SAS 9.4. A logistic regression was fit to predict the potential for plasma therapy based on three sources of information: (1) baseline data, including age, gender, smoking status, obesity, diabetes, chronic obstructive pulmonary disease or sleep apnea and D-dimer and C-reactive protein at admission; (2) data from the day of transfusion (day 0), including supplemental oxygen requirement, length of hospital stay, minimal oxygen saturation, heart rate, respiratory rate and systolic and diastolic blood pressure; and (3) chronological data up to the day of transfusion, including the use of hydroxychloroquine or azithromycin, intubation status and, if intubated, the duration of intubation. Day 0 for convalescent plasma recipients was defined as the day on which they received plasma transfusion. For control patients, day 0 was defined as the day of hospitalization corresponding to the length of stay of their matched convalescent plasma recipient before transfusion. Two sets of matched data were generated based on 1:4 and 1:2 ratios for cases versus controls using the nearest neighbor matching algorithm, with and without replacement, respectively (SAS package: PROC PSMatch). Among the predictors, exact matching was enforced on oxygen requirement on the day of transfusion, length of hospital stay from the day of admission to the day of transfusion, the administration of hydroxychloroquine and azithromycin, and intubation status and duration (Supplementary Table 3). Other medications were administered too infrequently to enforce exact matching.
The distribution of the logit propensity score–matched controls was within range of the convalescent plasma recipients, as opposed to the logit propensity score of the data from patients with confirmed COVID system wide (Extended Data Fig. 1). Balance was well achieved between the plasma and control groups, as all predictors had a standardized mean difference of less than 0.2 (Extended Data Fig. 2). Descriptive results for matched datasets are shown in Supplementary Table 3.
Assessment of respiratory status
Patients were evaluated for their supplemental oxygen requirements and survival at three time points: days 1, 7 and 14 after transfusion. Four categories of supplemental oxygen use status were collected for both cases and controls (Supplementary Tables 2 and 3). These included, in order of increasing severity: room air, without supplemental oxygen; low-flow oxygen delivery by standard nasal cannula; high-flow oxygen delivery, including non-rebreather mask, high-flow nasal cannula or BiPAP noninvasive ventilation; and mechanical ventilation. A patient’s oxygenation status at the three time points was considered to have worsened if they changed from a lower- to a higher-severity category compared to day 0, or if they had died before the time point. A generalized estimating equations approach with a logit link for binary data was used to model the effect of plasma on the odds of oxygenation improvement on days 1, 7 and 14 following transfusion, controlling for oxygen status on day 0. An independent working correlation structure was assumed for the patients within each cluster; however, P values were calculated based on the empirical standard errors. Since some patients with COVID-19 were being discharged with continued home oxygen supplementation during the study period, but this information was not easily obtainable from the database, the oxygen status of all discharged patients was assumed to be no worse than low-flow oxygen by standard nasal cannula. Adjusted covariates included duration of symptoms, use of pharmacotherapies (such as broad-spectrum antibiotics, therapeutic anticoagulation, azithromycin, corticosteroids, hydroxychloroquine and investigational antivirals) and laboratory values, specifically IL-6 levels.
Assessment of outcomes
Kaplan–Meier survival curves were used to depict the overall survival following transfusion. A Cox model was fit to estimate the HR for in-hospital mortality for the plasma group, with matched clusters treated as random effects and onset of intubation as a time-varying covariate. In addition, interactions between convalescent plasma administration and intubation duration were tested to see if the plasma effects were the same in subgroups.
Both survival models were adjusted for duration of symptoms before admission and other therapies administered during admission, as these data were only ascertained by manual chart review after the matching was completed. The initial list of therapies consisted of those used for COVID-19 during the study period, which included azithromycin, broad-spectrum antibiotics, hydroxychloroquine, therapeutic anticoagulants, corticosteroids and investigational therapies, including directly acting antivirals, mesenchymal stem cells and IL-1 and IL-6 inhibitors. Only those that had a chi-square test P value < 0.5, however, were included in the final model for adjustment. A liberal P value was used here to be inclusive of any potential confounders. As a sensitivity analysis, the 1:2 matching data without replacement data were also analyzed, where the balance between the matched pairs was enhanced but the study power was reduced.
Antibody assays and analyses
The MSH anti-IgG COVID-19 enzyme-linked immunosorbent assay
The MSH-ELISA anti-IgG COVID-19 assay23,24,25 is an orthogonal immune assay specific for anti-SARS-CoV-2 spike protein IgG in clinical serum or plasma specimens. It measures the relative concentration of IgG and reports the result as the reciprocal of the highest dilution of serum or plasma giving a positive signal. The assay received FDA emergency use authorization for clinical use on 15 April 2020 (https://www.fda.gov/media/137032/download/) and was also independently authorized as a laboratory developed test for clinical application by the New York State Department of Health at the Mount Sinai Laboratory, Center for Clinical Laboratories, a division of the Department of Pathology, Molecular and Cell-Based Medicine, New York (Clinical Laboratory Improvement Amendments no. 33D1051889).
Enzyme-linked immunosorbent assay
Plasma unit samples were retrieved from frozen apheresis segments, and antibody titers were determined by ELISA, performed in 96-well microtiter plates (Thermo Fisher) coated with 50 μl of recombinant full-length spike protein at a concentration of 2 μg ml−1 overnight at 4 °C. The next day, the plates were washed three times with PBS (Gibco) containing 0.1% Tween-20 (T-PBS; Fisher Scientific). The plates were blocked with 200 μl of blocking solution (T-PBS with 3% wt/vol milk powder (American Bio)) and incubated for at least 1 h at room temperature. Plasma samples were serially diluted in 1% milk prepared in T-PBS and added to the plates after the blocking solution was removed, and then the plates were incubated for 2 h at room temperature. The plates were washed three times with T-PBS using an automatic plate washer (BioTek) and 50 μl of anti-human IgG (Fab-specific) horseradish peroxidase antibody (produced in goat; Sigma, A0293), diluted 1:3,000 in T-PBS containing 1% milk powder, was added to all wells. After 1 h, the plates were washed three times with T-PBS, 100 μl of SigmaFast o-phenylenediamine dihydrochloride (Sigma) was added to all wells, and the reaction stopped after 10 min by adding 50 μl per well of 3 M hydrochloric acid (Thermo Fisher). The plates were read at a wavelength of 490 nm using a plate reader (BioTek), and the endpoint titer was calculated, defined as the last dilution before the signal dropped below an OD490 of 0.15.
Microneutralization assay
Donor serum samples were heat inactivated at 56 °C for 1 h before use. Vero.E6 cells from the American Type Culture Collection (ATCC no. CRL‐1586) were seeded at a density of 20,000 cells per well in a 96-well cell culture plate (Corning, 3595) 1 d before the assay was performed. Cells were maintained in culture in complete DMEM (Gibco), and the medium used for the neutralization assay was 1× MEM (Gibco) supplemented with 2% FBS (Corning). Starting with 1:10, serial dilutions of each sample in duplicate were prepared in a 96-well plate. Six wells in each plate were used as no-virus negative controls, and six wells were used as serum-free, virus-only positive controls. Next, 80 μl of each respective dilution was mixed with 600 median tissue culture doses (TCID50) of SARS‐CoV‐2 isolate USA‐WA1/2020 (BEI Resources, NR‐52281) in 80 μl. The virus–serum mixture was incubated for 1 h. The medium was removed from cells, and 120 μl of virus–serum mixture was added. After 1 h of incubation at 37 °C, the virus–serum mixture was removed, and 100 μl of MEM and 100 μl of each serum dilution was added to the cells. The cells were incubated at 37 °C for 2 d. The medium from the cells was removed, and 150 μl of 10% formaldehyde (Polysciences) was added for 24 h to fix cells and inactivate the virus. The next day, cells were permeabilized and stained using a mouse monoclonal anti-SARS-CoV-2 nucleocapsid antibody (clone 1C7, generated in-house by T. Moran, Center for Therapeutic Antibody Discovery at ISMMS). For each dilution, the inhibition of virus growth, relative to the controls, was calculated. A nonlinear regression was performed in Prism version 7.0 (GraphPad Software) to calculate the 50% inhibitory dilution (ID50), the serum dilution at which virus growth was halved relative to the serum-free, virus-only controls. The 50% neutralizing titer was defined as the reciprocal of the ID50.
Data analysis
Donor serum antibody titers (total IgG against recombinant SARS-CoV-2 full-length spike protein, measured by the clinical MSH-ELISA) were available for all 25 donors who provided the convalescent plasma to this recipient cohort. Stored samples of donor serum, drawn on the same day as the antibody screening test, and unit plasma, retrieved from plasma segments, were available from 24 of 25 donors. The donor for whom these samples were not available had a screening antibody titer of 1:960 and donated both units of plasma to recipient number 15, who expired during the study period. The serum from one donor, who had a screening antibody titer of 1:320, showed no detectable neutralization of SARS-CoV-2 in the microneutralization assay; the 50% neutralization titer of this sample was set at 1 for the purposes of calculating geometric means and correlation coefficients. These data are provided as source data. For recipients who received plasma units from two different donors, the GM-NT of the serum samples from the two donors is presented in Fig. 3c. Spearman’s rank correlation coefficients (ρ) and GM-NTs were calculated in Prism version 8.0 (GraphPad).
Statistical analyses
We did not perform a priori sample size calculations. The convalescent plasma-recipient cohort (n = 39) was a sample of convenience that included all adult patients treated with convalescent plasma under FDA eIND at MSH. The untreated control sample size was determined by matching at 1:2 and 1:4 ratios (cases to controls) by propensity score analysis. Group differences were evaluated by chi-square and Wilcoxon rank-sum tests for categorical and ordinal data, respectively. ORs and HRs are presented with 95% CIs and chi-square P values. Spearman’s rank correlation was used to test for monotonous relationships between plasma donors’ antibody titers and plasma recipients’ clinical outcomes, and analysis of variance was assessed by the Kruskal–Wallis test, followed by Dunn’s multiple-comparison test. All tests were two-sided, and statistical significance was defined as a P value < 0.05, unless otherwise indicated. Descriptive data are reported as number (percent), mean ± s.d., geometric mean (95% CI) or median (range or IQR), as appropriate.
Reporting Summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
Data will be shared in accordance with ISMMS policy on access to and use and disclosure of Mount Sinai data. This process can be initiated upon request to the corresponding author. Source data are provided with this paper.
Code availability
No custom code is associated with this manuscript. The SAS code for these analyses can be downloaded from https://www.researchgate.net/project/Convalescent-plasma-treatment-of-severe-COVID-19-A-propensity-score-matched-control-study/.
References
Casadevall, A. & Pirofski, L. A. The convalescent sera option for containing COVID-19. J. Clin. Invest. 130, 1545–1548 (2020).
Rojas, M. et al. Convalescent plasma in COVID-19: possible mechanisms of action. Autoimmun. Rev. 19, 102554 (2020).
Sharun, K. et al. Antibody-based immunotherapeutics and use of convalescent plasma to counter COVID-19: advances and prospects. Expert Opin. Biol. Ther. 20, 1033–1046 (2020).
Richardson, S. et al. Presenting characteristics, comorbidities and outcomes among 5,700 patients hospitalized with COVID-19 in the New York City area. JAMA 323, 2052–2059 (2020).
Duan, K. et al. Effectiveness of convalescent plasma therapy in severe COVID-19 patients. Proc. Natl Acad. Sci. USA 117, 9490–9496 (2020).
Zhou, F. et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 395, 1054–1062 (2020).
Zhao, J. et al. Antibody responses to SARS-CoV-2 in patients of novel coronavirus disease 2019. Clin. Infect. Dis. https://doi.org/10.1093/cid/ciaa344 (2020).
Chen, L., Xiong, J., Bao, L. & Shi, Y. Convalescent plasma as a potential therapy for COVID-19. Lancet Infect. Dis. 20, 398–400 (2020).
Roback, J. D. & Guarner, J. Convalescent plasma to treat COVID-19: possibilities and challenges. JAMA 323, 1561–1562 (2020).
Luke, T. C., Kilbane, E. M., Jackson, J. L. & Hoffman, S. L. Meta-analysis: convalescent blood products for Spanish influenza pneumonia: a future H5N1 treatment? Ann. Intern. Med. 145, 599–609 (2006).
Mair-Jenkins, J. et al. The effectiveness of convalescent plasma and hyperimmune immunoglobulin for the treatment of severe acute respiratory infections of viral etiology: a systematic review and exploratory meta-analysis. J. Infect. Dis. 211, 80–90 (2015).
Enria, D. A., Briggiler, A. M., Fernandez, N. J., Levis, S. C. & Maiztegui, J. I. Importance of dose of neutralising antibodies in treatment of Argentine haemorrhagic fever with immune plasma. Lancet 2, 255–256 (1984).
Lee, J. S. et al. Anti-Ebola therapy for patients with Ebola virus disease: a systematic review. BMC Infect. Dis. 19, 376 (2019).
Ye, M. et al. Treatment with convalescent plasma for COVID-19 patients in Wuhan, China. J. Med. Virol. https://doi.org/10.1002/jmv.25882 (2020).
Salazar, E. et al. Treatment of COVID-19 patients with convalescent plasma. Am. J. Pathol. 190, 1680–1690 (2020).
Perotti, C. et al. Mortality reduction in 46 severe COVID-19 patients treated with hyperimmune plasma. A proof of concept single arm multicenter interventional trial. Haematologica https://www.haematologica.org/content/early/2020/07/20/haematol.2020.261784.long (2020).
Gharbharan, A. et al. Convalescent plasma for COVID-19. A randomized clinical trial. Preprint at https://www.medrxiv.org/content/10.1101/2020.07.01.20139857v1 (2020).
Li, L. et al. Effect of convalescent plasma therapy on time to clinical improvement in patients with severe and life-threatening COVID-19: a randomized clinical trial. JAMA 324, 460–470 (2020).
Finland, M. The serum treatment of lobar pneumonia. N. Engl. J. Med. 202, 1244–1247 (1930).
Cecil, R. L. Remarks on HE SERUM TREATMENT OF PNEUMONIA. Br. Med. J. 2, 657–662 (1932).
Hung, I. F. N. et al. Hyperimmune IV immunoglobulin treatment: a multicenter double-blind randomized controlled trial for patients with severe 2009 influenza A (H1N1) infection. Chest 144, 464–473 (2013).
Austin, P. C. A comparison of 12 algorithms for matching on the propensity score. Stat. Med. 33, 1057–1069 (2014).
Amanat, F. et al. A serological assay to detect SARS-CoV-2 seroconversion in humans. Nat. Med. 26, 1033–1036 (2020).
Stadlbauer, D. et al. SARS-CoV-2 seroconversion in humans: a detailed protocol for a serological assay, antigen production and test setup. Curr. Protoc. Microbiol. 57, e100 (2020).
Wajnberg, A. et al. SARS-CoV-2 infection induces robust, neutralizing antibody responses that are stable for at least three months. Preprint at http://medrxiv.org/content/early/2020/07/17/2020.07.14.20151126.abstract (2020).
Choe, P. G. et al. Antibody responses to SARS-CoV-2 at 8 weeks postinfection in asymptomatic patients. Emerg. Infect. Dis. 26 (2020).
Klein, S. et al. Sex, age and hospitalization drive antibody responses in a COVID-19 convalescent plasma donor population. J. Clin. Invest. https://doi.org/10.1172/JCI142004 (2020).
Okba, N. M. A. et al. Severe Acute Respiratory Syndrome Coronavirus 2-specific antibody responses in coronavirus disease patients. Emerg. Infect. Dis. 26, 1478–1488 (2020).
Joyner, M. J. et al. Safety update: COVID-19 convalescent plasma in 20,000 hospitalized patients. Mayo Clin. Proc. https://www.mayoclinicproceedings.org/article/S0025-6196(20)30651-0/fulltext (2020).
Joyner, M. J. et al. Early safety indicators of COVID-19 convalescent plasma in 5,000 patients. J. Clin. Invest. 130, 4791–4797 (2020).
Llitjos, J. F. et al. High incidence of venous thromboembolic events in anticoagulated severe COVID-19 patients. J. Thromb. Haemost. 18, 1743–1746 (2020).
Acknowledgements
This study was supported by internal funding from MSH and ISMMS. We thank all of the patients who participated in this study and their families. We also acknowledge the generosity of the thousands of anonymous tristate area residents who recovered from COVID-19 and then volunteered to donate convalescent plasma for the benefit of others. We thank the New York Blood Center, L.-A. Pirofski, T. Schneider, C. Seah, S. Srinivas, D. Tremblay, M. Geiger, C. Lebovits and J. Lustgarten. We acknowledge the assistance of ISMMS medical students: S. Ahsanuddin, A. Paasewe, R. Upadhyay, G. Mellgard, T. Martinson, B. Patil, C. Luo, S. Agrawal, A. Siddiqui, J. Schwarz, L. Piendel, J. Emerson, H. Kaplan, E. Klein, M. Garcia, J. Johnson, L. Maillie and E. Baldwin. We also appreciate the clinical expertise of the Mount Sinai Convalescent Plasma Squad: N. Shuman, D. Delbeau, D. Catamero, G. Sanchez, S. Aird, M. Mann, T. Broome, S. Kleiner-Arje, L. Wolf, A. Lee, L. Gaynes and K. Goodman. We dedicate this work to the New Yorkers who have lost their lives to COVID-19 with a special dedication to the health care workers who will always be remembered for their selflessness during this pandemic.
Author information
Authors and Affiliations
Contributions
J.A.A., A.C., N.M.B., S.T.H.L., H.-M.L., B.K.C. and D.L.R. conceived and designed the study. S.T.H.L., H.-M.L., P.T., M.A.L., E.B., A.D., C.S. and A.Z. analyzed the data. S.T.H.L., N.M.B., J.A.A., J.P.G., F.R., D.R.A., I.B., D.R.M., A.F.B., C.C.-C., J.S.J., S.A.A., A.W., J.B., D.R., A.B.-M. and F.K. participated in the donor plasma collection program and the transfusion of convalescent plasma recipients. Mount Sinai laboratory technicians performed the clinical MSH-ELISA assay, developed by F.A., D.S. and F.K. and transitioned to clinical use by D.R.M., A.F.-B. and C.C.-C. on donor serum samples. F.T.N., F.A. and D.S. performed the lab-based ELISA and microneutralization assays on donor serum and plasma samples, and N.M.B. analyzed the antibody titer data. S.T.H.L., H.-M.L. and N.M.B. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
F. Krammer has filed patent applications for the assay used to select plasma donors, and Mount Sinai has licensed its use to several companies. All other authors have nothing to disclose.
Additional information
Peer review information Alison Farrell is the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Propensity scoring of matched controls and all COVID-positive patients versus convalescent plasma recipients.
The logits of propensity scores were more similarly distributed for convalescent plasma recipients (n=39) and their propensity score-matched controls (n=156) than for all COVID-19 patients admitted to the Mount Sinai Health System between 24 March 2020 and 8 April 2020 (n=4,152). The means are represented by open circles (for convalescent plasma recipients) or plus signs (for matched controls and all COVID patients). The box represents the interquartile range, the center line is the median value, and the whiskers delineate the range between minimum and maximum values.
Extended Data Fig. 2 Standardized mean differences of matched controls and all COVID-positive patients.
Balance was well achieved between the groups of convalescent plasma recipients (n=39) and matched controls (n=156). For each predictor listed on the y-axis, the observed standardized mean difference is represented by green circles for matched controls and by blue X symbols for all COVID-19 patients in the Mount Sinai Health System (n=4,152). Between plasma recipients and matched controls, all treatment predictors had a standardized mean difference of less than 0.2, represented by the blue shading.
Supplementary information
Supplementary Information
Supplementary Tables 1 and 3 and Supplementary Text 1.
Supplementary Table 2
Oxygen supplementation requirements on days 1, 7 and 14 and end-of-study outcomes for convalescent plasma recipients and matched controls.
Source data
Source Data Fig. 1
Excel table and statistical source data.
Source Data Fig. 2
Excel table and statistical source data.
Source Data Fig. 3
Excel table and statistical source data.
Rights and permissions
About this article
Cite this article
Liu, S.T.H., Lin, HM., Baine, I. et al. Convalescent plasma treatment of severe COVID-19: a propensity score–matched control study. Nat Med 26, 1708–1713 (2020). https://doi.org/10.1038/s41591-020-1088-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-020-1088-9
This article is cited by
-
Marine natural products and human immunity: novel biomedical resources for anti-infection of SARS-CoV-2 and related cardiovascular disease
Natural Products and Bioprospecting (2024)
-
Effect of hydrogen/oxygen therapy for ordinary COVID-19 patients: a propensity-score matched case-control study
BMC Infectious Diseases (2023)
-
Plasma-Derived Medicinal Products in Nigeria
SN Comprehensive Clinical Medicine (2023)
-
The clinical outcomes of high neutralizing antibodies titer convalescent plasma therapy in early developed severe COVID-19 patients; a case–control study
Annals of Clinical Microbiology and Antimicrobials (2022)
-
Use of convalescent plasma in pregnant women with early stage COVID-19 infection in a tertiary care hospital in Dubai, February to March 2021: a case series study
BMC Pregnancy and Childbirth (2022)