Abstract
The therapeutic potential of donor-derived mesenchymal stromal cells (MSCs) has been investigated in diverse diseases1, including steroid-resistant acute graft versus host disease (SR-aGvHD)2. However, conventional manufacturing approaches are hampered by challenges with scalability and interdonor variability, and clinical trials have shown inconsistent outcomes3,4. Induced pluripotent stem cells (iPSCs) have the potential to overcome these challenges, due to their capacity for multilineage differentiation and indefinite proliferation5,6. Nonetheless, human clinical trials of iPSC-derived cells have not previously been completed. CYP-001 (iPSC-derived MSCs) is produced using an optimized, good manufacturing practice (GMP)-compliant manufacturing process. We conducted a phase 1, open-label clinical trial (no. NCT02923375) in subjects with SR-aGvHD. Sixteen subjects were screened and sequentially assigned to cohort A or cohort B (n = 8 per group). One subject in cohort B withdrew before receiving CYP-001 and was excluded from analysis. All other subjects received intravenous infusions of CYP-001 on days 0 and 7, at a dose level of either 1 × 106 cells per kg body weight, to a maximum of 1 × 108 cells per infusion (cohort A), or 2 × 106 cells per kg body weight, to a maximum dose of 2 × 108 cells per infusion (cohort B). The primary objective was to assess the safety and tolerability of CYP-001, while the secondary objectives were to evaluate efficacy based on the proportion of participants who showed a complete response (CR), overall response (OR) and overall survival (OS) by days 28/100. CYP-001 was safe and well tolerated. No serious adverse events were assessed as related to CYP-001. OR, CR and OS rates by day 100 were 86.7, 53.3 and 86.7%, respectively. The therapeutic application of iPSC-derived MSCs may now be explored in diverse inflammatory and immune-mediated diseases.
Similar content being viewed by others
Main
Mesenchymal stromal cells promote an immunosuppressive and immunoregulatory environment by secretion of cytokines, chemokines, growth factors and extracellular vesicles7,8, as well as by activation of indoleamine 2,3-dioxygenase (IDO) production in recipient phagocytes when undergoing apoptosis9. MSCs lack human leukocyte antigen class II antigen expression, which allows allogeneic administration without donor–recipient matching. There is general consensus that MSCs derived from primary sources (including bone marrow, adipose tissue, umbilical cord blood and placenta) are safe and well tolerated10.
However, there are substantial scalability and consistency challenges associated with primary donor-derived MSC production. There is substantial donor-dependent variability in the propensity of MSCs to be activated by interferon-gamma and tumor necrosis factor-alpha, which leads to upregulation of IDO expression and results in suppression of T-cell proliferation11,12,13. Additionally, MSC gene expression, differentiation, proliferation and colony-forming capacity vary markedly among donors.14,15. Furthermore, repeated recruitment and qualification of donors is costly and logistically challenging. While extensive ex vivo culture expansion of MSCs can be employed to produce large numbers of therapeutic doses per donation, this may lead to replicative senescence and other changes to MSC properties, even at relatively low culture expansion levels15. Indeed, clinical data suggest that minimally expanded, bone marrow–derived MSCs (BM-MSCs) are associated with better outcomes in SR-aGvHD patients compared to moderately expanded passage 3–4 BM-MSCs16.
We have developed a new iPSC- and mesenchymoangioblast (MCA)-based manufacturing platform to address these challenges, by eliminating the need to rely on new donors and minimizing the level of culture expansion once MSCs are formed.
SR-aGvHD is a disease characterized by very poor prognosis and high mortality rates17. Therapeutic use of MSCs for the treatment of SR-aGvHD was introduced by Le Blanc and colleagues in 2004, with positive results18. In a previously published study in a humanized mouse model of aGvHD, the iPSC-derived MSC product CYP-001 reduced bone marrow infiltration and expression of proinflammatory molecules (NOTCH1, TBET and PKCΘ) by CD4 and CD8 T cells, attenuated disease severity and prolonged survival19.
In this study we have optimized the manufacture of CYP-001 and investigated its safety, tolerability and efficacy for the treatment of adults with SR-aGvHD in a multicenter, phase I, open-label, dose-escalation clinical trial (NCT02923375). As the first completed human clinical trial of iPSC-derived cells in any disease, this study is relevant not only to SR-aGvHD but also to many other diseases for which MSCs may have therapeutic utility.
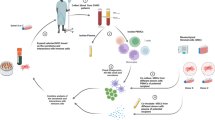
The Cymerus proprietary manufacturing process, which is used to manufacture CYP-001, is represented in Fig. 1. This new production platform generates MSCs from iPSCs via an apelin receptor+ lateral plate mesoderm intermediate cell with fibroblast growth factor-2 (FGF2)-dependent colony-forming potential, known as an MCA20,21. This approach allows for the production of well-defined MSCs that express lateral plate, but not paraxial or intermediate, mesoderm markers.
The manufacturing process consists of three stages: (1) iPSC banking, (2) iPSC expansion and differentiation to MSCs to freeze and intermediate bank and (3) MSC expansion and formulation of final clinical product. Based on the existing banking strategy, approximately 9 × 104 vials, each containing 1 × 106 iPSCs, can be generated from a single iPSC line. At the current processing scale, a single vial of 1 × 106 iPSCs is capable of giving rise to 3.2 × 1010 MSCs on average, while the entire iPSC bank has the capacity to generate 2.9 × 1015 MSCs, or 29 million clinical doses (each containing 1 × 108 MSCs).
The iPSCs used in the manufacture of CYP-001 were derived by reprogramming peripheral blood mononuclear cells from a healthy adult donor using episomal, nonintegrating, oriP/EBNA1−based plasmids.
We used a PCR assay on both predifferentiated iPSCs and the finished MCA-derived MSC product to verify that reprogramming plasmids were not integrated into the reprogrammed cells. Comparative genomic hybridization (CGH) and single-nucleotide polymorphism (SNP) analysis showed there were no differences in iPSC samples taken before and after expansion through ten passages, indicating that iPSCs are genomically stable during in vitro expansion. The results from the iPSC samples were also compared to an Agilent Reference genome, and there were no mutations of known or potential clinical significance.
We developed an optimized, GMP-compliant manufacturing process utilizing xenogen-, serum- and feeder-free conditions. We eliminated the use of murine feeders, in contrast to the original protocol developed by Vodyanik et al.20, instead using chemically defined conditions for iPSC maintenance as previously described by Chen et al.22. We also optimized the mesenchymal colony-forming medium (M-CFM) compared to that used by Vodyanik et al., and implemented a modified version of the protocol described by Uenishi et al.23 to achieve mesoderm induction. The optimized process generated MSCs with superior performance in a previously described immunopotency assay24.
To avoid the risk of teratoma formation or aberrant differentiation in vivo, the CYP-001 manufacturing process was designed to ensure the absence of residual iPSCs in the final product by incorporation of the following steps: (1) after the induction of mesoderm, cells were cultured in a single-cell suspension in semisolid medium, which does not support iPSC survival; (2) cells were passed through a mesh filtration step, which eliminates small clumps of undifferentiated iPSCs; and (3) iPSC-derived MSCs were expanded in adherent cell culture conditions, which do not support survival or expansion of undifferentiated iPSCs.
To confirm these mitigation steps, we conducted an experiment in which undifferentiated iPSCs were seeded in place of MSC progenitor cells in the M-CFM culture step. After culturing for a duration equivalent to that of the differentiation process, cells were collected and cultured under conditions that support the growth and expansion of human pluripotent stem cells. No iPSC colony formation was observed (lower limit of detection, 0.001%), and microscopic observations detected only single dead cells that did not attach or divide in the flowthrough fraction plated. We conclude that residual iPSCs do not survive M-CFM culture, and that any dead iPSCs in this culture are removed before the MSC expansion stage of the process, providing reassurance that the final CYP-001 product is free from residual iPSCs.
The cells in CYP-001 meet the minimal criteria for defining multipotent MSCs as proposed by the International Society for Cell and Gene Therapy19,25. The process is highly efficient, yielding a homogenous population of CD105+, CD73+, CD90+, CD43/45–, CD31– and HLA-DR− MSCs (Supplementary Table 1).
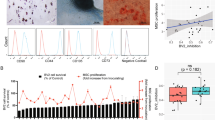
We developed a new assay to quantitate potential residual undifferentiated stem cells by measuring the LIN28 gene, which is associated with the pluripotent stem cell state. Samples were subjected to a procedure that selectively amplifies the growth of undifferentiated iPSCs in a background of MSCs, to increase the sensitivity of quantitative reverse-transcription polymerase chain reaction (qRT–PCR) for residual iPSC detection (lower limit of detection, 0.001%). We also performed an in vitro tumorigenicity assay to detect the potential presence of transformed cells capable of colony formation in soft agar. No contaminating undifferentiated iPSCs or colony formation in soft agar have been detected in any batch of CYP-001 manufactured to date.
Global gene expression (transcriptome) analysis performed on MCA-derived MSCs demonstrated a very high degree of consistency in gene expression and isoforms between lots (Extended Data Figs. 1 and 2).
Extended Data Fig. 3 shows a CONSORT diagram for the phase I clinical trial. The study recruited male and female subjects who had received an allogeneic hematopoietic stem cell transplant and subsequently been diagnosed with grade II–IV aGvHD. Subjects were required to meet all of the following criteria: (1) failure to respond/disease progression after at least 3 days’ intravenous or oral treatment with an appropriate corticosteroid at a dose of at least 1 mg kg–1 d–1; (2) treated with a steroid regimen and duration consistent with normal practice at the relevant clinical site; and (3) considered to be steroid resistant in the opinion of the investigator. These criteria were selected to allow for intersite variability in clinical practice.
The primary objective was to assess the safety and tolerability of CYP-001, while the secondary objective was to evaluate the efficacy of CYP-001 (assessed by best response to treatment by days 28 and 100 and OS at days 28 and 100; Supplementary Table 2). Subjects who completed the 100-day primary evaluation period then entered a 2-year safety and survival follow-up phase.
Between 10 May 2017 and 22 May 2018, a total of 16 subjects were screened, all of whom were enrolled. Before enrollment, ten subjects had been treated with corticosteroid doses of 1 mg kg–1 d–1 while six had received doses of 1.5–2.0 mg kg–1 d–1. Fifteen subjects were treated with CYP-001 in one of two dose cohorts. One subject withdrew before receiving CYP-001 after experiencing a myocardial infarction, and was therefore excluded from analysis. Patients were sequentially assigned to cohort A or cohort B. Subjects enrolled in cohort A (n = 8) received two doses of CYP-001 (1 × 106 cells per kg body weight up to a maximum dose of 1 × 108 cells, administered intravenously on days 0 and 7). Subjects enrolled in cohort B (n = 7) were treated on the same schedule, using 2 × 106 cells per kg body weight for each dose up to a maximum dose of 2 × 108 cells. Participants received CYP-001 from a total of four different batches in this study.
Baseline characteristics of subjects in the two cohorts are shown in Supplementary Table 3, while baseline aGvHD staging and grading data by subject are shown in Supplementary Table 4.
Treatment with CYP-001 was well tolerated, with no notable differences observed between the two cohorts (Table 1). Five adverse events (AEs) were assessed by the investigator as possibly related (defined as AEs with a reasonable time relationship to CYP-001 administration, but which could also be explained by disease or other drugs): abdominal pain, diarrhea, febrile neutropenia, arthralgia and renal impairment (each n = 1). No AEs were assessed by the investigator as probably or definitely related to CYP-001 treatment. A small number of AEs (8/104 events) were classified as severe: febrile neutropenia (n = 3), blister (n = 2), rash erythematosus (n = 1), pruritis (n = 1) and pneumonia (n = 1). One instance of severe febrile neutropenia was assessed by the investigator as possibly related to CYP-001 treatment, and all other severe AEs were assessed as unlikely related or not related. Five serious adverse events (SAEs) were reported (lower respiratory tract infection, pneumonia, febrile neutropenia, parainfluenza virus infection and hypokalemia), but no SAEs were assessed by the investigator as possibly, probably or definitely related to CYP-001. No subjects discontinued treatment due to AEs.
Of the 15 subjects enrolled, 13 survived until day 100. One subject in cohort A died of pneumonia on day 28 (which was deemed unrelated to the study drug) and one subject in cohort B showed no improvement in aGvHD and withdrew to commence palliative care on day 22.
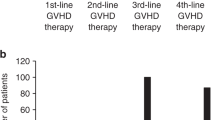
A summary of aGvHD responses, OS and aGvHD grade by days 28 and 100 of the primary evaluation period is provided in Table 2, while change in aGvHD status and best response for individual subjects by day 100 in the primary evaluation period is shown in Fig. 2. By day 100, CR and OS were observed in 53.3 and 86.7% of subjects, respectively, with no dose-dependent differences. The median time to both first response and best response was earlier in the high-dose cohort (3 and 14 d, respectively) than in the low-dose cohort (14 and 60 d, respectively).
Change in aGvHD status and best response in individual subjects by day100. Asterisk (*) shows subject B5 withdrew from the trial on day 22 to commence palliative care; cross (†) shows that subject A3 showed PR at days 14 and 21 but died due to pneumonia on day 28. Eight subjects were enrolled in each cohort, but one subject in cohort B withdrew before infusion of CYP-001.
Concomitant aGvHD medication use is summarized in Supplementary Table 5. All subjects in both cohorts continued treatment with concomitant standard of care aGvHD medications, with universal systemic corticosteroid (glucocorticoid) use. Additional immunosuppressants were used in 10/15 subjects (66.7%). Among the latter, calcineurin inhibitors were prescribed more frequently in the low-dose (75%) than in the high-dose (57.1%) cohort, as were selective immunosuppressants (75 versus 14.3%, respectively). Of note, all 13 subjects who had a day 100 visit were either receiving no systemic steroids by that time (n = 7) or receiving a lower dose than at day 0 (n = 6). Additionally, two subjects who were on intravenous steroids at day 0 were transitioned to oral steroids at day 100.
Discussion
Our study demonstrates that iPSC-derived MSCs can be manufactured using a new cell differentiation and expansion platform that eliminates major issues of supply, scalability and consistency.
Our iPSC-based approach has the potential to overcome the fundamental limitations of conventional, donor-derived MSC production processes, as it facilitates the manufacture of an effectively limitless number of MSCs from a single blood donation. It also avoids the need for excessive culture expansion of differentiated MSCs, by instead harnessing the indefinite replication potential of iPSCs. Performing MSC production under xenogen-, serum- and feeder-free conditions minimizes the potential for contamination with zoonotic agents and further reduces potential sources of variability. The use of MCA colony-forming mesodermal progenitors allows for the production of a consistent MSC product of well-defined origin. Moreover, the colony-forming step during manufacture provides an additional line of safety since undifferentiated iPSCs are not capable of surviving in MCA-specific, semisolid, colony-forming cultures.
Other groups have explored diverse approaches to overcome the scalability and consistency challenges associated with conventional MSC production. For example, the MSC-FFM method achieves dose-to-dose consistency within an MSC bank derived from pooled bone marrow mononuclear cells from multiple donors, with encouraging clinical trial results26. This facilitates the production of a larger quantity of MSCs from a single bank than a single-donor approach, with a similar level of culture expansion. However, each bank would suffice for the treatment of only ~175 patients at the highest dose regimen used in the clinical trial (four infusions at 2 × 106 cells per kg body weight). Evidence of consistency between banks produced using this method requires further exploration.
A single iPSC bank is sufficient to generate ~375,000 batches of CYP-001, equating to approximately 29 million clinical doses at the current processing scale. Our process also has the potential to be scaled up further to produce a considerably higher number of doses per bank as development progresses.
Our clinical trial demonstrates that, within a limited number of subjects with SR-aGVHD, CYP-001 is safe and tolerable. Additionally, although further trials with larger sample sizes will be required to confirm efficacy, the aGvHD response and OS rates observed are encouraging.
Outcomes in our study compare favorably with those in previously published studies involving BM-MSCs and other second-line agents. However, such comparisons should be interpreted with caution, in light of differences between trials including sample sizes, the definition of steroid resistance and the use of concomitant medications.
Across 15 published clinical trials involving the treatment of SR-aGvHD with BM-MSCs2, day 28 OR rates ranged from 45 to 86.5% compared to 62.5% (low dose) and 87.5% (high dose) in our study. Day 28 CR rates after BM-MSC treatment in the same published trials ranged from 6.5 to 65% compared to 12.5% (low dose) and 57.1% (high dose) in our study. Day 100 survival rates ranged from 34.4 to 57.3% in the three BM-MSC studies reviewed that reported 100-day survival, compared to 87.5% (low dose) and 85.7% (high dose) in our study. Similarly, in a recently published phase III study, 260 subjects with SR-aGvHD received standard of care plus either (1) placebo or (2) 8 to 12 infusions of BM-MSCs27. The day 28 OR rate in the BM-MSC group was 58%, with a 100-day OS rate of <50%27. It is also noteworthy that subjects in our study received 2 infusions each, compared to between 3 and 12 infusions each in the BM-MSC studies.
Other second-line agents used in patients with SR-aGvHD include ruxolitinib, etanercept and extracorporeal photopheresis (ECP). In a recently published phase III study, patients treated with ruxolitinib showed day 28 CR and OR rates of 34 and 62%, respectively28, while response rates observed in a phase II study with the same agent were marginally lower29. Day 28 CR and OR rates of 0–20 and 50–53%, respectively, were reported in trials with etanercept30,31, while in a case series of patients treated with ECP the 1-month CR and OR rates were 33 and <50%, respectively32. It is also important to consider the safety concerns associated with other agents, in particular ruxolitinib and etanercept, in comparison to MSCs.
Based on day 28 responses rates, it appears that the higher dose level of CYP-001 led to improved outcomes compared to the lower dose. However, we note that patients who received the higher dose were approximately 20 years younger on average, which may have impacted treatment response, and both groups achieved comparable response rates by day 100.
All subjects were administered corticosteroids, and most (10/15) were administered immunosuppressants during our study. The use of other second-line agents after day 28, as was allowed per protocol, may be a further confounding factor regarding day 100 outcomes. Additionally, although we demonstrated that CYP-001 exhibits a highly consistent gene expression profile between batches, differences in epigenetic and functional features may exist. Nonetheless, these data highlight the importance of pursuing investigations of iPSC-derived MSCs in the treatment of SR-aGvHD and will inform dosing regimens in future studies involving CYP-001.
Although initially tested in aGVHD, iPSC-derived MSCs may be used in the future for a range of other clinical targets. Encouraging data on the potential utility of iPSC-derived MSCs manufactured using this platform have already been generated in preclinical models of critical limb ischemia33, asthma34,35, organ transplant rejection36 and acute respiratory distress syndrome37. Furthermore, we note that primary MSCs have been investigated for a wide range of other therapeutic indications, and we hypothesize that iPSC-derived MSCs could be expected to show similar in vivo effects more generally. The scalability and consistency of this iPSC-derived process could prove to be even more advantageous if the cells are shown to have beneficial effects in one or more conditions with a much higher incidence than aGvHD.
Other studies are investigating diverse iPSC-derived cellular products in conditions including age-related macular degeneration38, heart failure39, Parkinson’s disease40 and solid tumors (no. NCT03841110), but clinical trial results have yet to be reported.
The challenges of scalability, reproducibility and consistency of iPSC-derived products, which have been overcome herein, are pertinent to the application of iPSC technology regardless of the disease target. This study represents the first report of a completed human clinical trial using iPSC-derived cells in any disease.
Methods
Manufacture of CYP-001
CYP-001 was manufactured on behalf of the sponsor (Cynata Therapeutics Limited) by Waisman Biomanufacturing.
The iPSCs used in the manufacture of CYP-001 were derived by Cellular Dynamics International, Inc., by reprogramming peripheral blood mononuclear cells from a healthy adult donor using episomal, nonintegrating, oriP/EBNA1-based plasmids, as previously described41.
Donor starting material (whole blood) was collected from healthy adult donors by BloodCenter of Wisconsin, Inc. Donor screening criteria included the standard criteria for donating blood, in addition to a number of additional exclusion criteria (provision of informed consent; at least 18 years old; weight at least 110 pounds (equivalent to 49.9 kg); hemoglobin ≥12.5 g dl–1; no history of bone marrow transplant, cancer or neurological disease). Any subject who met any exclusion criterion was automatically excluded from donation. The medical history of prospective donors was reviewed by medical staff to determine whether the subject was suitable to donate, and a form was completed by the principal investigator in all cases to confirm eligibility. Additionally, prospective donors were subjected to the standard infectious disease testing for blood donors. Donor testing and medical examination were performed in compliance with the donor eligibility requirements specified in the US Food & Drug Administration (FDA) Human Cells, Tissues, and Cellular and Tissue-Based Products (HCT/P) regulations (no. 21 CFR 1271).
Whole blood samples were collected from each donor using standard 250-ml blood bags. One sample was provided for reprogramming while an additional sample was taken for donor testing. All pathogen testing was performed using test kits approved by the US FDA in a FDA-registered HCT/P testing facility.
Reagents and media used in the manufacture of CYP-001 are described in Supplementary Tables 6–11. The process involved the following steps.
-
(1)
iPSCs were thawed in E8 Complete Medium (E8CM; DMEM/F12 Base Medium + E8 Supplement) + 1 µM H1152 (a rho-associated, coiled-coil-containing protein kinase (ROCK) inhibitor) on Vitronectin-coated (0.5 µg cm–2) six-well plates and incubated at 37 °C, 5% CO2, 20% O2 (normoxia).
-
(2)
iPSCs were expanded over three passages in E8CM (without ROCK inhibitor) on Vitronectin-coated (0.5 µg cm–2) six-well plates and incubated at 37 °C, 5% CO2, 20% O2 (normoxia) before initiation of the differentiation process.
-
(3)
iPSCs were harvested and seeded as single cells/small colonies at 5 × 103 cells cm–2 on Collagen IV-coated (0.5 µg cm–2) six-well plates in E8CM + 10 µM Y27632 and incubated at 37 °C, 5% CO2, 20% O2 (normoxia) for 24 h.
-
(4)
E8CM + 10 µM Y27632 was replaced with differentiation medium (Supplementary Table 9) and the plates were further incubated at 37 °C, 5% CO2, 5% O2 (hypoxia) for 48 h.
-
(5)
Colony-forming cells were harvested from differentiation medium-adherent culture as a single-cell suspension, transferred to M-CFM (Supplementary Table 10) suspension culture in ultra-low-attachment six-well plates and incubated at 37 °C, 5% CO2, 20% O2 (normoxia) for 12 d.
-
(6)
Colonies (passage 0) were harvested and seeded on Fibronectin/Collagen I-coated (0.67 µg cm–2 Fibronectin, 1.2 µg cm–2 Collagen I) plasticware with a modified smoothed finite element method (M-SFEM) and incubated at 37 °C, 5% CO2, 20% O2 (normoxia) for 3 d.
-
(7)
From passage 1 to 5, colonies were harvested and seeded as single cells at 1.3 × 104 cells cm–2 in M-SFEM on Fibronectin/Collagen 1-coated plasticware and incubated at 37 °C, 5% CO2, 20% O2 (normoxia) for 3 d.
-
(8)
The final harvested MCA-derived MSCs were washed with DPBS and harvested into resuspension medium (Plasma-Lyte A Injection pH 7.4 (Baxter) and 10% human serum albumin (HSA, Baxter)), pooled and centrifuged. A cell count was performed and a final dilution made to achieve a target cell concentration of 10 × 106 cells ml–1. These cells were then diluted 1:1 with cold cryopreservation solution (Plasma-Lyte A Injection pH 7.4, 10% HSA, 5% DMSO) to give a final cell concentration of 5 × 106 cells ml–1 in Plasma-Lyte A Injection pH 7.4, 10% HSA and 2.5% DMSO. Units of the finished product were then filled into CryoStore Freezing Bags (Origen; 20 ml fill volume), immediately cryopreserved in a controlled-rate freezer programmed to a freezing profile of −1 °C min–1 and subsequently stored in the vapor phase of liquid nitrogen.
To confirm the inability of residual iPSCs to survive the M-CFM process stage, we conducted an experiment in which undifferentiated iPSCs were seeded in place of MSC progenitor cells in the M-CFM culture step. We investigated whether iPSCs could survive in M-CFM culture. iPSCs were thawed and expanded according to the same procedure used in the manufacture of CYP-001. M-CFM culture was then executed as per the CYP-001 process, with the exception that the differentiation process was omitted and thus undifferentiated iPSCs were seeded in place of MSC progenitor cells. After culturing for a duration equivalent to that of the normal differentiation process, cells were strained through 100-µm strainers and both flowthrough and strained fractions were collected, centrifuged, pooled and resuspended in E8CM plus a ROCK inhibitor and cultured in one well each of a six-well plate coated with Laminin 521 and E-Cadherin. E8CM is a xenogen- and feeder-free medium specially formulated for the growth and expansion of human pluripotent stem cells. The ROCK inhibitor enhances survival and expansion of singularized iPSCs, while Laminin 521 and E-Cadherin form a coating matrix that also enhances survival and expansion of singularized iPSCs. Collectively, this culture system supports iPSC survival and growth, which means that if any residual undifferentiated iPSCs survive M-CFM culture, they would be expected to survive and proliferate when transferred to this culture system.
Quality control
Release tests were performed to ascertain the quality and safety of the manufactured CYP-001 product. A PCR assay with primers specific to the reprogramming vector used to generate the iPSC line was undertaken to verify that reprogramming plasmids were not integrated into the reprogrammed cells. This assay, which has a lower limit of detection of less than one copy of plasmid per assay, was performed on samples of iPSCs (before differentiation) and again on the finished MCA-derived MSC product.
The residual undifferentiated iPSC assay was performed to quantitate residual undifferentiated stem cells by TaqMan Gene Expression Assay (qRT–PCR) targeting LIN28, a gene associated with the pluripotent stem cell state. Test samples were subjected to a procedure that selectively amplifies the growth of undifferentiated iPSCs in a background of MSCs, to increase the sensitivity of qRT–PCR for residual iPSC detection. This step involves culturing the product in E8CM with a ROCK inhibitor on Laminin 521/E-Cadherin-coated cultureware for 6 d.
Cells were prepared for total RNA isolation using RNAprotect Cell Reagent, then centrifuged for 5 min at 4,000 r.p.m. (Sorvall ID 0018 or equivalent) to collect any formed cells and precipitate. Total RNA was isolated using the QIAGEN RNeasy Plus Mini Kit, complementary DNA was prepared using the High Capacity RNA-to-cDNA Kit and TaqMan Gene Expression Assay was performed for LIN28 and GAPDH. The average cycle where the fluorescent signal crosses the threshold for real-time qPCR and qRT–PCR assays (Cq(50)) and percentage relative s.d. were calculated for each LIN28 and GAPDH ± the real-time dataset. The average Cq(50) values were normalized by subtracting the average GAPDH Cq(50) (n = 3) from the average LIN28 Cq(50) (n = 3). Comparisons were performed between samples for normalized average Cq(50) values to determine whether the 0.001% iPSC spiked sample (amplified) could be detected above background and whether GAPDH Cq(50) percentage relative s.d. for all samples was ≤5%.
The in vitro tumorigenicity assay using soft agar colony formation42 was performed as follows. Cells from the test sample plus a positive control (HT-1080 cells) and a negative control (WI-38) were plated at concentrations of both 1 × 105 and 1 × 106 cells per Petri dish and incubated for 14 d. Photographs were taken of each dish after 14 d to confirm colony formation in the positive control, no colony formation in the negative control and to ascertain relative colony growth in the test sample (at both cell concentrations for each).
Comparative genomic hybridization and SNP analysis were performed to determine whether there was a tendency for iPSCs to acquire abnormalities during culture expansion. CGH/SNP testing was performed using the Agilent SurePrint G3 Human CGH + SNP Microarray Kit (4×180k), with a probe length of 60 mer, and analyzed using Agilent CytoGenomics Edition 4.0.2.21 software. iPSC samples at passage 21 (the master cell bank passage level) and passage 31 (beyond the passage level used in MCA-derived MSC manufacture) were tested.
Global gene expression (transcriptome) analysis was performed by messenger RNA sequencing (mRNA-seq) on MCA-derived MSCs produced in three separate lots, to determine consistency in gene expression between lots. Total RNA was extracted from MCA-derived MSC samples, from which mRNA was then isolated and analyzed using the Illumina HiSeq 2500 platform. Normalized transcripts per kilobase million counts for each sample were then calculated and plotted against one another, and the Pearson correlation was computed to determine the degree of consistency of gene expression and isoforms between samples.
Phase I clinical trial of iPSC-derived cells: CYP-001 in acute SR-aGvHD
Details of the study design are provided in the Life Sciences Reporting Summary.
This phase I, multicenter, open-label, dose-escalation study investigated the safety, tolerability and efficacy of two doses of CYP-001. CYP-001 was supplied as 1 × 108 (100 million) MCA-derived MSCs formulated in 20 ml of serum-free cryoprotectant medium, which contained 2.5% DMSO and 10% HSA. The product was stored and shipped at or below −140 °C and thawed to 37 °C at the clinical site immediately before subject administration.
Subjects were recruited from the United Kingdom (five sites) and Australia (two sites) from 10 May 2017 to 28 August 2018. Written informed consent was obtained from all subjects by the principal investigator (or subinvestigator) following full disclosure of the study and before initiation of any study-related assessment or investigation. The study was designed, implemented and reported in accordance with the International Conference on Harmonization/Harmonized Tripartite Guidelines for Good Clinical Practice, with applicable local regulations, and with the ethical principles laid down in the Declaration of Helsinki. The protocol was approved by the North East–York Research Ethics Committee, Jarrow, UK, on behalf of all participating centers in the United Kingdom (reference no. 16/NE/0316) and the Royal Adelaide Hospital Human Research Ethics Committee, Adelaide, Australia, on behalf of both participating centers in Australia (reference no. HREC/16/RAH/412).
Five protocol amendments were made during the duration of the study, none of which had a material impact on clinical outcomes. Protocol amendments 1–3 were made before study commencement (6 July 2016, 7 November 2016, 22 November 2016). Protocol amendment 4 was made on 18 May 2017 (with one subject enrolled into cohort A) to replace the exclusion criterion of sepsis with severe or uncontrolled systemic infection (bacterial, viral or fungal) likely to impact the subject’s ability to participate in the trial. Protocol amendment 5 was made on 13 Nov 2017 (with seven subjects enrolled into cohort A) to redefine SR-aGvHD as failure to respond or progress after oral treatment in addition to intravenous treatment, and to remove the exclusion criterion relating to Eastern Cooperative Oncology Group grade 3 or higher.
Study subjects
The study recruited male and female subjects aged 18–70 years (inclusive) who had undergone an allogeneic hematopoietic stem cell transplant to treat a hematological disorder (including, but not limited to, hematological malignancy) and who had subsequently been diagnosed using consensus grading with grade II–IV SR-aGvHD (based on the 1994 Consensus Conference on Acute GVHD Grading)43.
Prospective participants were required to provide written informed consent before screening. All subjects were required to have failed to respond to at least 3 d of steroid treatment (≥1 mg kg–1 d–1), administered in accordance with standard management at each center. Specifically, (1) the participant must have failed to respond, or progressed, after at least 3 d of intravenous or oral treatment with an appropriate corticosteroid at a dose of at least 1 mg kg–1 d–1; (2) the steroid regimen and duration administered must be consistent with normal practice at the relevant clinical site; and (3) the participant must have steroid-resistant aGvHD in the opinion of the investigator. The life expectancy of subjects must have been at least 1 month at the time of screening in the opinion of the investigator. Female participants of childbearing potential were required to return a negative urine pregnancy test at screening. Participants were also required to agree to comply with measures intended to prevent female participants becoming pregnant and male participants fathering children for 3 months following the last dose of CYP-001.
Prospective participants were ineligible if they were: pregnant or breastfeeding; had received any investigational research agent within 30 d or five half-lives (whichever is longer) before the first dose of CYP-001; had a known or suspected current alcohol or substance abuse problem; had a progressive or relapsing hematological malignancy, a current solid tumor or previous malignant solid tumor likely to recur during the period of the study (except basal or squamous cell carcinomas); had heart failure (New York Heart Association functional class II–IV) and/or pulmonary failure; were hemodynamically unstable and/or at high risk of cardiovascular events; had terminal organ failure (minimal hepatic and/or renal function); had meningitis, pneumonia with hypoxemia, human immunodeficiency virus or another severe or uncontrolled systemic infection likely to impact on the ability of the patient to participate in the trial; and/or had any other medical or psychiatric condition that made the patient unsuitable for participation in the study.
Study design, treatments, visits, assessments and outcome measures
Eligible subjects were recruited to either cohort A (low-dose CYP-001: intravenous infusion of 1 × 106 cells per kg body weight, up to a maximum dose of 1 × 108 cells on days 0 and 7) or cohort B (high-dose CYP-001; intravenous infusion of 2 × 106 cells per kg body weight, up to a maximum dose of 2 × 108 cells on days 0 and 7) according to a sequential, sentinel dosing protocol. During the primary evaluation period (days 0–100), subjects were asked to attend study visits on days 0, 3, 7, 14, 21, 28, 60 and 100.
The first eight subjects were enrolled into cohort A. After the eighth subject had completed their day 28 assessments, safety data were reviewed by an independent data safety monitoring board to determine whether an additional eight subjects could be enrolled into cohort B. Infusions were administered using a Fresenius Kabi Volumat MC Agilia Infusion Pump and Fresenius Kabi VL SP22, at a rate of 1 ml min–1. Subjects were also permitted to receive standard of care medications. Following completion of the primary evaluation period, surviving subjects then entered a 2-year safety and survival follow-up phase.
Outcome measures
The primary outcome was safety. In the primary evaluation period, safety endpoints were based on physical examination, vital signs, pulse oximetry (oxygen saturation), safety laboratory tests (biochemistry, hematology, urinalysis, viral screening), AEs and SAEs. The incidence and severity of AEs up to day 28 and SAEs possibly related to the study drug after day 28 were recorded. In the follow-up period, safety endpoints were limited to SAEs deemed possibly, probably or definitely related to the study drug, and malignancy status.
Efficacy assessments included aGvHD stage/grade (according to the 1994 Consensus Conference on Acute GvHD Grading Criteria29; Supplementary Table 2), malignancy status, response status (CR, partial response (PR), stable disease, disease progression) and survival status. In the primary evaluation period, efficacy endpoints were the proportion of subjects showing CR by day 28 and PR by day 28 (both obtained from the ‘best’ response reported on days 3, 7, 14, 21 or 28), the proportion of subjects showing CR by day 100 and PR by day 100 (both obtained from the best response reported on days 3, 7, 14, 21, 28, 60 or 100) and OS at days 28 and 100. In the follow-up period, efficacy endpoints were OS and aGvHD status at months 6,12,18 and 24, and additional aGvHD treatment required.
Additional assessments included aGvHD treatment received. Blood was also collected for potential future biomarker analysis.
Statistical analyses
No formal sample size was calculated for this early phase I safety study, because a cohort of eight subjects per group is generally accepted as appropriate for testing of initial clinical safety. All safety and efficacy analyses were performed on the safety set consisting of all enrolled subjects who received at least one dose of the investigational product, CYP-001, regardless of whether they received the second dose. The primary analysis was performed at the conclusion of the primary evaluation period. Categorical data were summarized using counts and percentages. Continuous data were summarized using mean, median, s.d., minimum and maximum. All data from subjects who withdrew prematurely from the study were included in any analysis where possible. No imputations were made for analysis purposes, and all available data were used in the data summaries. Safety and efficacy results are presented for the safety set from the primary evaluation period only for those subjects who were included in the study for a minimum of 6 months after CYP-001 treatment.
Reporting Summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
All reasonable requests for raw and analyzed data that are not included in this manuscript or online content will be promptly reviewed by the senior authors to determine whether the request is subject to any intellectual property or confidentiality obligations. Patient-related data may be subject to patient confidentiality restrictions. Any data and materials that can be shared will be released via a material transfer agreement. All raw and analyzed global gene expression data can be found at the NCBI Gene Expression Archive (accession no. GSE150969).
References
Kabat, M., Bobkov, I., Kumar, S. & Grumet, M. Trends in mesenchymal stem cell clinical trials 2004–2018: is efficacy optimal in a narrow dose range? Stem Cells Transl. Med. 9, 17–27 (2020).
Elgaz, S. et al. Clinical use of mesenchymal stromal cells in the treatment of acute graft-versus-host disease. Transfus. Med. Hemother. 46, 27–34 (2019).
Galipeau, J. The mesenchymal stromal cells dilemma—does a negative phase III trial of random donor mesenchymal stromal cells in steroid-resistant graft-versus-host disease represent a death knell or a bump in the road? Cytotherapy 15, 2–8 (2013).
François, M. et al. Human MSC suppression correlates with cytokine induction of indoleamine 2,3-dioxygenase and bystander M2 macrophage differentiation. Mol. Ther. 20, 187–195 (2012).
Takahashi, K. et al. Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell 131, 861–872 (2007).
Yu, J. et al. Induced pluripotent stem cell lines derived from human somatic cells. Science 318, 1917–1920 (2007).
Galipeau, J. & Sensébé, L. Mesenchymal stromal cells: clinical challenges and therapeutic opportunities. Cell Stem Cell 22, 824–833 (2018).
Harrell, C. R. et al. Mesenchymal stem cell–derived exosomes and other extracellular vesicles as new remedies in the therapy of inflammatory diseases. Cells 8, 1605 (2019).
Galleu, A. et al. Apoptosis in mesenchymal stromal cells induces in vivo recipient-mediated immunomodulation. Sci. Transl. Med. 9, 7828 (2017).
Sharma, R. R. et al. Mesenchymal stem or stromal cells: a review of clinical applications and manufacturing practices. Transfusion 54, 1418–1437 (2014).
Wegmeyer, H. et al. Mesenchymal stromal cell characteristics vary depending on their origin. Stem Cells Dev. 22, 2606–2618 (2013).
Martin, I. et al. Challenges for mesenchymal stromal cell therapies. Sci. Transl. Med. 20, eaat2189 (2019).
Ketterl, N. et al. A robust potency assay highlights significant donor variation of human mesenchymal stem/progenitor cell immune modulatory capacity and extended radio-resistance. Stem Cell Res. Ther. 6, 236 (2015).
Siegel, G. et al. Phenotype, donor age and gender affect function of human bone marrow-derived mesenchymal stromal cells. BMC Med. 11, 146 (2013).
Wagner, W. et al. Replicative senescence of mesenchymal stem cells: a continuous and organized process. PLoS ONE 5, e2213 (2008).
von Bahr, L. et al. Long-term complications, immunologic effects, and role of passage for outcome in mesenchymal stromal cell therapy. Biol. Blood Marrow Transplant. 18, 557–564 (2012).
Garnett, C. et al. Treatment and management of graft-versus-host disease: improving response and survival. Ther. Adv. Hematol. 4, 366–378 (2013).
Le Blanc, K. et al. Treatment of severe acute graft-versus-host disease with third party haploidentical mesenchymal stem cells. Lancet 363, 1439–1441 (2004).
Ozay, E. I. et al. Cymerus™ iPSC-MSCs significantly prolong survival in a pre-clinical, humanized mouse model of graft-vs-host disease. Stem Cell Res. 35, 101401 (2019).
Vodyanik, M. A. et al. A mesoderm-derived precursor for mesenchymal stem and endothelial cells. Cell Stem Cell 7, 718–729 (2010).
Slukvin, I. I. & Kumar, A. The mesenchymoangioblast, mesodermal precursor for mesenchymal and endothelial cells. Cell. Mol. Life Sci. 75, 3507–3520 (2018).
Chen, G. et al. Chemically defined conditions for human iPS cell derivation and culture. Nat. Methods 8, 424–429 (2011).
Uenishi, G. et al. Tenascin C promotes hematoendothelial development and T lymphoid commitment from human pluripotent stem cells in chemically defined conditions. Stem Cell Rep. 3, 1073–1084 (2014).
Slukvin, I., Uenishi, G., Hei, D. & Drier, D. Colony forming medium and use thereof. Patent WO2017156580A1 (2017).
Dominici, M. et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8, 315–317 (2006).
Bader, P. et al. Effective treatment of steroid and therapy-refractory acute graft versus-host disease with a novel mesenchymal stromal cell product (MSC-FFM). Bone Marrow Transplant. 53, 852–862 (2018).
Kebriaei, P. et al. A phase 3 randomized study of remestemcel-L versus placebo added to second-line therapy in patients with steroid-refractory acute graft-versus-host disease. Biol. Blood Marrow Transplant. 26, 835–844 (2020).
Zeiser, R. et al. Ruxolitinib for glucocorticoid-refractory acute graft-versus-host disease. N. Engl. J. Med. 382, 1800–1810 (2020).
Jagasia, M. et al. Ruxolitinib for the treatment of steroid-refractory acute GVHD (REACH1): a multicenter, open-label, phase 2 trial. Blood 135, 1739–1749 (2020).
Park, J. H. et al. Etanercept for steroid-refractory acute graft versus host disease following allogeneic hematopoietic stem cell transplantation. Korean J. Intern. Med. 29, 630–636 (2014).
De Jong, C. N. et al. Etanercept for steroid-refractory acute graft-versus-host disease: a single center experience. PLoS ONE 12, e0187184 (2017).
Greinix, H. T. et al. Extracorporeal photochemotherapy in the treatment of severe steroid-refractory acute graft-versus-host disease: a pilot study. Blood 96, 2426–2431 (2000).
Koch, J. M. et al. Mesenchymoangioblast-derived mesenchymal stromal cells inhibit cell damage, tissue damage and improve peripheral blood flow following hindlimb ischemic injury in mice. Cytotherapy 18, 219–228 (2016).
Royce, S. G. et al. Intranasal administration of mesenchymoangioblast-derived mesenchymal stem cells abrogates airway fibrosis and airway hyperresponsiveness associated with chronic allergic airways disease. FASEB J. 31, 4168–4178 (2017).
Royce, S. G. et al. iPSC- and mesenchymoangioblast-derived mesenchymal stem cells provide greater protection against experimental chronic allergic airways disease compared with a clinically used corticosteroid. FASEB J. 33, 6402–6411 (2019).
Khan, M. A. et al. iPSC-derived MSC therapy induces immune tolerance and supports long-term graft survival in mouse orthotopic tracheal transplants. Stem Cell Res. Ther. 10, 290 (2019).
Millar, J. E. et al. Combined mesenchymal stromal cell therapy and ECMO in ARDS: a controlled experimental study in sheep. Am. J. Respir. Crit. Care Med. https://doi.org/10.1164/rccm.201911-2143OC (2020).
Mandai, M., Kurimoto, Y. & Takahashi, M. Autologous induced stem-cell-derived retinal cells for macular degeneration. N. Engl. J. Med. 377, 792–793 (2017).
Ylä-Herttuala, S. iPSC-derived cardiomyocytes taken to rescue infarcted heart muscle in coronary heart disease patients. Mol. Ther. 26, 2077 (2018).
Stoddard-Bennett, T. & Reijo Pera, R. Treatment of Parkinson’s disease through personalized medicine and induced pluripotent stem cells. Cells 8, 26 (2019).
Mack, A. A. et al. Generation of induced pluripotent stem cells from CD34+ cells across blood drawn from multiple donors with non-integrating episomal vectors. PLoS ONE 6, e27956 (2011).
Borowicz, S. et al. The soft agar colony formation assay. J. Vis. Exp. 92, e51998 (2014).
Przepiorka, D. et al. 1994 Consensus Conference on Acute GVHD Grading. Bone Marrow Transplant. 15, 825–828 (1995).
Acknowledgements
We thank the University of Wisconsin Bioinformatics Resource Center for providing mRNA-seq analysis services, and all site investigators, coinvestigators, study coordinators, other study staff and study participants. Medical writer C. Markey, of Markey Medical Consulting Pty Ltd, assisted in the preparation of an earlier version of a draft manuscript describing this work. J.E.J.R. is supported by a National Health and Medical Research Council Investigator Grant (1177305) for ‘driving clinical cell and gene therapy in Australia’, as well as funding from Cure the Future, Therapeutic Innovation Australia and an anonymous foundation.
Author information
Authors and Affiliations
Contributions
I.S., G.I.U., D.D. and D.H. developed and optimized the manufacturing process. I.S., D.D., D.H. and L.S.L. developed and optimized quality control assays and designed the experiment to verify that iPSCs do not survive M-CFM culture. K.K. designed the clinical trial and wrote the protocol. A.J.C.B., A.P., J.E.G., M.H.G., R.R., D.T.Y. and J.E.J.R. were principal investigators in the clinical trial. K.K. and J.E.J.R. prepared the first drafts of the manuscript. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Competing interests
Patent applications (some of which have been granted) covering aspects of the technology described in this manuscript have been filed by Wisconsin Alumni Research Foundation (which invests in the University of Wisconsin-Madison), Cellular Dynamics International (now FUJIFILM Cellular Dynamics) and Cynata Therapeutics. The patents with inventors including D.D., D.H., G.I.U., K.K. and I.S. cover the processes used to generate iPSCs and differentiate iPSCs into MSCs, as well as the residual undifferentiated iPSC assay. Cynata Therapeutics funded the work described in this manuscript. K.K. is an employee and shareholder of Cynata Therapeutics. I.S. is a cofounder, shareholder and scientific advisor of Cynata Therapeutics. L.S.L. and D.D. are employees of Waisman Biomanufacturing, University of Wisconsin-Madison, which provides contract manufacturing services to Cynata Therapeutics. D.H. is a former employee of both Waisman Biomanufacturing and Cellular Dynamics International. G.I.U. and J.E.J.R. have received travel grants from Cynata Therapeutics. A.J.C.B., A.P., J.E.G., M.H.G., R.R. and D.T.Y. declare no relevant competing interests.
Additional information
Peer review information Jerome Staal was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 mRNAseq global gene expression analysis showing gene correlation and Pearson correlation coefficients.
mRNAseq global gene expression (transcriptome) analysis from three batches (CYN-IPSC-MSC-P5B-FP-001; CYN-IPSC-MSC-P5B-FP-002; CYN-IPSC-MSC-P5B-FP-003) showing gene correlation [log[2](TPM+1)] and Pearson correlation coefficients (R).
Extended Data Fig. 2 mRNAseq global gene expression analysis showing isoform correlation and Pearson correlation coefficients.
mRNAseq global gene expression (transcriptome) analysis from three batches (CYN-IPSC-MSC-P5B-FP-001; CYN-IPSC-MSC-P5B-FP-002; CYN-IPSC-MSC-P5B-FP-003) showing isoform correlation [log[2](TPM+1)] and Pearson correlation coefficients (R).
Extended Data Fig. 3 CONSORT diagram.
Clinical trial summary (CONSORT diagram).
Supplementary information
Supplementary Information
Supplementary Tables 1–11.
Rights and permissions
About this article
Cite this article
Bloor, A.J.C., Patel, A., Griffin, J.E. et al. Production, safety and efficacy of iPSC-derived mesenchymal stromal cells in acute steroid-resistant graft versus host disease: a phase I, multicenter, open-label, dose-escalation study. Nat Med 26, 1720–1725 (2020). https://doi.org/10.1038/s41591-020-1050-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-020-1050-x
This article is cited by
-
Mesenchymal stromal cells plus basiliximab improve the response of steroid-refractory acute graft-versus-host disease as a second-line therapy: a multicentre, randomized, controlled trial
BMC Medicine (2024)
-
Challenges of mesenchymal stem cells in the clinical treatment of COVID-19
Cell and Tissue Research (2024)
-
A mutant methionyl-tRNA synthetase-based toolkit to assess induced-mesenchymal stromal cell secretome in mixed-culture disease models
Stem Cell Research & Therapy (2023)
-
Exploring the promising potential of induced pluripotent stem cells in cancer research and therapy
Molecular Cancer (2023)
-
Cell therapies for autism spectrum disorder: a systematic review of clinical applications
Middle East Current Psychiatry (2023)