Abstract
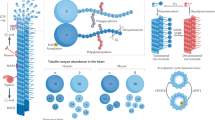
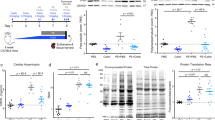
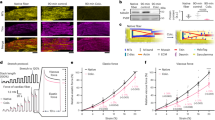
Detyrosinated microtubules provide mechanical resistance that can impede the motion of contracting cardiomyocytes. However, the functional effects of microtubule detyrosination in heart failure or in human hearts have not previously been studied. Here, we utilize mass spectrometry and single-myocyte mechanical assays to characterize changes to the cardiomyocyte cytoskeleton and their functional consequences in human heart failure. Proteomic analysis of left ventricle tissue reveals a consistent upregulation and stabilization of intermediate filaments and microtubules in failing human hearts. As revealed by super-resolution imaging, failing cardiomyocytes are characterized by a dense, heavily detyrosinated microtubule network, which is associated with increased myocyte stiffness and impaired contractility. Pharmacological suppression of detyrosinated microtubules lowers the viscoelasticity of failing myocytes and restores 40–50% of lost contractile function; reduction of microtubule detyrosination using a genetic approach also softens cardiomyocytes and improves contractile kinetics. Together, these data demonstrate that a modified cytoskeletal network impedes contractile function in cardiomyocytes from failing human hearts and that targeting detyrosinated microtubules could represent a new inotropic strategy for improving cardiac function.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Tsutsui, H., Ishihara, K. & Cooper, G. Cytoskeletal role in the contractile dysfunction of hypertrophied myocardium. Science 260, 682–687 (1993).
Collins, J. F. et al. The role of the cytoskeleton in left ventricular pressure overload hypertrophy and failure. J. Mol. Cell. Cardiol. 28, 1435–1443 (1996).
Tagawa, H. et al. Cytoskeletal role in the transition from compensated to decompensated hypertrophy during adult canine left ventricular pressure overloading. Cir. Res. 82, 751–761 (1998).
Ishibashi, Y. et al. Role of microtubules in myocyte contractile dysfunction during cardiac hypertrophy in the rat. Am. J. Physiol. 271, H1978–87 (1996).
Bailey, B. A., Dipla, K., Li, S. & Houser, S. R. Cellular basis of contractile derangements of hypertrophied feline ventricular myocytes. J. Mol. Cell. Cardiol. 29, 1823–1835 (1997).
Kerr, J. P. et al. Detyrosinated microtubules modulate mechanotransduction in heart and skeletal muscle. Nat. Commun. 6, 8526 (2015).
Robison, P. et al. Detyrosinated microtubules buckle and bear load in contracting cardiomyocytes. Science 352, aaf0659 (2016).
Robison, P. & Prosser, B. L. Microtubule mechanics in the working myocyte. J. Physiol. 595, 3931–3937 (2017).
Agnetti, G. et al. Desmin modifications associate with amyloid-like oligomers deposition in heart failure. Cardiovasc. Res. 102, 24–34 (2014).
Burke, M. A. et al. Molecular profiling of dilated cardiomyopathy that progresses to heart failure. JCI Insight 1, e86898 (2016).
Chen, J., Bardes, E. E., Aronow, B. J. & Jegga, A. G. ToppGene Suite for gene list enrichment analysis and candidate gene prioritization. Nucleic Acids Res. 37, W305–11 (2009).
Frolova, E. G. et al. Thrombospondin-4 regulates fibrosis and remodeling of the myocardium in response to pressure overload. FASEB J. 26, 2363–2373 (2012).
Wulfkuhle, J. D. et al. Domain analysis of supervillin, an F-actin bundling plasma membrane protein with functional nuclear localization signals. J. Cell Sci. 112, 2125–2136 (1999).
Takahashi, M. et al. Phenotypic consequences of beta1-tubulin expression and MAP4 decoration of microtubules in adult cardiocytes. Am. J. Physiol. Heart Circ. Physiol. 285, H2072–83 (2003).
Cheng, G. et al. Basis for MAP4 dephosphorylation-related microtubule network densification in pressure overload cardiac hypertrophy. J. Biol. Chem. 285, 38125–38140 (2010).
Prota, A. E. et al. Structural basis of tubulin tyrosination by tubulin tyrosine ligase. J. Cell Biol. 200, 259–270 (2013).
Prins, K. W. et al. Dystrophin is a microtubule-associated protein. J. Cell Biol. 186, 363–369 (2009).
Caporizzo, M. A. et al. Strain-rate dependence of elastic modulus reveals silver nanoparticle induced cytotoxicity. Nanobiomedicine (Rij) 2, 9 (2015).
Gomez, A. M., Kerfant, B. G. & Vassort, G. Microtubule disruption modulates Ca2+ signaling in rat cardiac myocytes. Circ. Res. 86, 30–36 (2000).
Janke, C. & Bulinski, J. C. Post-translational regulation of the microtubule cytoskeleton: Mechanisms and functions. Nat. Rev. Mol. Cell Biol. 12, 773–786 (2011).
Zile, M. R. et al. Cardiocyte cytoskeleton in patients with left ventricular pressure overload hypertrophy. J. Am. Coll. Cardiol. 37, 1080–1084 (2001).
Zhang, C. et al. Microtubule-mediated defects in junctophilin-2 trafficking contribute to myocyte T-tubule remodeling and Ca2+ handling dysfunction in heart failure. Circulation 129, 1742–1750 (2014).
Stones, R., Benoist, D., Peckham, M. & White, E. Microtubule proliferation in right ventricular myocytes of rats with monocrotaline-induced pulmonary hypertension. J. Mol. Cell. Cardiol. 56, 91–96 (2013).
Prins, K. W. et al. Colchicine depolymerizes microtubules, increases junctophilin-2, and improves right ventricular function in experimental pulmonary arterial hypertension. J. Am. Heart Assoc. 6, e006195 (2017).
Lemler, M. S. et al. Myocyte cytoskeletal disorganization and right heart failure in hypoxia-induced neonatal pulmonary hypertension. Am. J. Physiol. Heart Circ. Physiol. 279, H1365–76 (2000).
Prosser, B. L., Ward, C. W. & Lederer, W. J. X-ROS signaling: Rapid mechano-chemo transduction in heart. Science 333, 1440–1445 (2011).
Prins, K. W., Asp, M. L., Zhang, H., Wang, W. & Metzger, J. M. Microtubule-mediated misregulation of junctophilin-2 underlies T-tubule disruptions and calcium mishandling in mdx mice. JACC: Basic Transl. Sci. 1, 122–130 (2016).
Shiels, H. et al. Stable microtubules contribute to cardiac dysfunction in the streptozotocin-induced model of type 1 diabetes in the rat. Mol. Cell. Biochem. 294, 173–180 (2007).
Wang, X., Li, F., Campbell, S. E. & Gerdes, A. M. Chronic pressure overload cardiac hypertrophy and failure in guinea pigs: II. Cytoskeletal remodeling. J. Mol. Cell. Cardiol. 31, 319–331 (1999).
Miragoli, M. et al. Microtubule-dependent mitochondria alignment regulates calcium release in response to nanomechanical stimulus in heart myocytes. Cell Rep. 14, 140–151 (2016).
Rochdi, M., Sabouraud, A., Girre, C., Venet, R. & Scherrmann, J. M. Pharmacokinetics and absolute bioavailability of colchicine after i.v. and oral administration in healthy human volunteers and elderly subjects. Eur. J. Clin. Pharmacol. 46, 351–354 (1994).
Terkeltaub, R. A. Clinical practice: gout. N. Engl. J. Med. 349, 1647–1655 (2003).
Yancy, C. W. et al. 2013 ACCF/AHA guideline for the management of heart failure: A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J. Am. Coll. Cardiol. 62, e147–239 (2013).
Cuffe, M. S. et al. Short-term intravenous milrinone for acute exacerbation of chronic heart failure: A randomized controlled trial. JAMA 287, 1541–1547 (2002).
Lang, R. M. et al. Recommendations for chamber quantification. Eur. J. Echocardiogr. 7, 79–108 (2006).
Dipla, K., Mattiello, J. A., Jeevanandam, V., Houser, S. R. & Margulies, K. B. Myocyte recovery after mechanical circulatory support in humans with end-stage heart failure. Circulation 97, 2316–2322 (1998).
Simithy, J. et al. Characterization of histone acylations links chromatin modifications with metabolism. Nat. Commun. 8, 1141 (2017).
Cox, J. & Mann, M. MaxQuant enables high peptide identification rates, individualized p.p.b.-range mass accuracies and proteome-wide protein quantification. Nat. Biotechnol. 26, 1367–1372 (2008).
Elias, J. E. & Gygi, S. P. Target-decoy search strategy for increased confidence in large-scale protein identifications by mass spectrometry. Nat. Methods 4, 207–214 (2007).
Vizcaíno, J. A. et al. 2016 update of the PRIDE database and related tools. Nucleic Acids Res. 44, 447–456 (2016).
Acknowledgements
We would like thank the Quantitative Proteomics Resource Core of the Perelman School of Medicine and the Penn Center for Musculoskeletal Disorders Histology Core at the University of Pennsylvania. This work was supported by funding from the National Institutes of Health (NIH) R01-HL133080 to B.L.P. and T32 R05346-09 to P.R., the American Heart Association 17POST33440043 to M.A.C., and by the Center for Engineering MechanoBiology through a grant from the National Science Foundation’s Science and Technology Center program: 15-48571. The procurement of human heart tissue was enabled by grants from the NIH (HL089847 and HL105993) to K.B.M.
Author information
Authors and Affiliations
Contributions
B.L.P., C.Y.C., M.A.C., and K.B.M. designed the study. B.L.P., C.Y.C., M.A.C., K.B., A.V., N.A.K., A.I.B., P.R., J.G.H., and A.K.S. carried out the data acquisition and analysis. M.P.M., C.Y.C., A.B., and B.L.P. carried out the proteomic analysis. B.L.P., C.Y.C., M.A.C., P.R., and K.B.M. interpreted the data. B.L.P. and C.Y.C. prepared the manuscript. All authors participated in the critical review and revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–6
Supplementary Tables
Supplementary Tables 1–6
Supplementary Video 1
Skeletonized 3D reconstruction of the microtubule network from Airyscan imaging of a failing human myocyte (DCM) labeled with Tyr-tubulin antibody to demonstrate the density of the microtubule network
Supplementary Video 2
Microtubule buckling in a contracting non-failing myocyte infected with AdV-EMTB for 48 h
Supplementary Video 3
Microtubule buckling in a contracting failing myocyte (DCM) infected with AdV-EMTB for 48 h
Supplementary Data
Spreadsheet of mass spectrometry data
Rights and permissions
About this article
Cite this article
Chen, C.Y., Caporizzo, M.A., Bedi, K. et al. Suppression of detyrosinated microtubules improves cardiomyocyte function in human heart failure. Nat Med 24, 1225–1233 (2018). https://doi.org/10.1038/s41591-018-0046-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-018-0046-2
This article is cited by
-
Distinct cytoskeletal regulators of mechanical memory in cardiac fibroblasts and cardiomyocytes
Basic Research in Cardiology (2024)
-
The origin of myocardial passive stiffness: more than the sum of its parts?
Pflügers Archiv - European Journal of Physiology (2024)
-
Surfaceome mapping of primary human heart cells with CellSurfer uncovers cardiomyocyte surface protein LSMEM2 and proteome dynamics in failing hearts
Nature Cardiovascular Research (2023)
-
Compressive forces stabilize microtubules in living cells
Nature Materials (2023)
-
Titin governs myocardial passive stiffness with major support from microtubules and actin and the extracellular matrix
Nature Cardiovascular Research (2023)