Abstract
One of most challenging issues in tumor immunology is a better understanding of the dynamics in the accumulation of myeloid-derived suppressor cells (MDSCs) in the tumor microenvironment (TIME), as this would lead to the development of new cancer therapeutics. Here, we show that translationally controlled tumor protein (TCTP) released by dying tumor cells is an immunomodulator crucial to full-blown MDSC accumulation in the TIME. We provide evidence that extracellular TCTP mediates recruitment of the polymorphonuclear MDSC (PMN-MDSC) population in the TIME via activation of Toll-like receptor-2. As further proof of principle, we show that inhibition of TCTP suppresses PMN-MDSC accumulation and tumor growth. In human cancers, we find an elevation of TCTP and an inverse correlation of TCTP gene dosage with antitumor immune signatures and clinical prognosis. This study reveals the hitherto poorly understood mechanism of the MDSC dynamics in the TIME, offering a new rationale for cancer immunotherapy.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Data availability
The microarray data are publicly available (Gene Expression Omnibus accession code GSE150465). A TCGA dataset of 640 patients with CRC is available at cBioPortal (https://www.cbioportal.org/study/summary?id=coadread_tcga). Source data are provided with this paper.
References
Binnewies, M. et al. Understanding the tumor immune microenvironment (TIME) for effective therapy. Nat. Med. 24, 541–550 (2018).
Sharma, P. & Allison, J. P. Immune checkpoint targeting in cancer therapy: toward combination strategies with curative potential. Cell 161, 205–214 (2015).
Trujillo, J. A., Sweis, R. F., Bao, R. & Luke, J. J. T cell-inflamed versus non-T cell-inflamed tumors: a conceptual framework for cancer immunotherapy drug development and combination therapy selection. Cancer Immunol. Res. 6, 990–1000 (2018).
Munn, D. H. & Bronte, V. Immune suppressive mechanisms in the tumor microenvironment. Curr. Opin. Immunol. 39, 1–6 (2016).
Ninomiya, S. et al. Tumor indoleamine 2,3-dioxygenase (IDO) inhibits CD19-CAR T cells and is downregulated by lymphodepleting drugs. Blood 125, 3905–3916 (2015).
Weiss, J. M. et al. Macrophage-dependent nitric oxide expression regulates tumor cell detachment and metastasis after IL-2/anti-CD40 immunotherapy. J. Exp. Med. 207, 2455–2467 (2010).
Jinushi, M. et al. Tumor-associated macrophages regulate tumorigenicity and anticancer drug responses of cancer stem/initiating cells. Proc. Natl Acad. Sci. USA 108, 12425–12430 (2011).
Yu, J. et al. Myeloid-derived suppressor cells suppress antitumor immune responses through IDO expression and correlate with lymph node metastasis in patients with breast cancer. J. Immunol. 190, 3783–3797 (2013).
Mao, Y. et al. Inhibition of tumor-derived prostaglandin-e2 blocks the induction of myeloid-derived suppressor cells and recovers natural killer cell activity. Clin. Cancer Res. 20, 4096–4106 (2014).
Kumar, V., Patel, S., Tcyganov, E. & Gabrilovich, D. I. The nature of myeloid-derived suppressor cells in the tumor microenvironment. Trends Immunol. 37, 208–220 (2016).
Molon, B. et al. Chemokine nitration prevents intratumoral infiltration of antigen-specific T cells. J. Exp. Med. 208, 1949–1962 (2011).
Veglia, F., Perego, M. & Gabrilovich, D. Myeloid-derived suppressor cells coming of age. Nat. Immunol. 19, 108–119 (2018).
Jiang, H. et al. Elevated chronic inflammatory factors and myeloid-derived suppressor cells indicate poor prognosis in advanced melanoma patients. Int. J. Cancer 136, 2352–2360 (2015).
Diaz-Montero, C. M. et al. Increased circulating myeloid-derived suppressor cells correlate with clinical cancer stage, metastatic tumor burden, and doxorubicin-cyclophosphamide chemotherapy. Cancer Immunol. Immunother. 58, 49–59 (2009).
Limagne, E. et al. Accumulation of MDSC and TH17 cells in patients with metastatic colorectal cancer predicts the efficacy of a FOLFOX-bevacizumab drug treatment regimen. Cancer Res. 76, 5241–5252 (2016).
Ackerman, D. & Simon, M. C. Hypoxia, lipids, and cancer: surviving the harsh tumor microenvironment. Trends Cell Biol. 24, 472–478 (2014).
Galluzzi, L., Buque, A., Kepp, O., Zitvogel, L. & Kroemer, G. Immunogenic cell death in cancer and infectious disease. Nat. Rev. Immunol. 17, 97–111 (2017).
Galluzzi, L. et al. Consensus guidelines for the definition, detection and interpretation of immunogenic cell death. J. Immunother. Cancer https://doi.org/10.1136/jitc-2019-000337 (2020).
Gorgulho, C. M., Romagnoli, G. G., Bharthi, R. & Lotze, M. T. Johnny on the spot-chronic inflammation is driven by HMGB1. Front. Immunol. 10, 1561 (2019).
Hiraoka, N. et al. Tumour necrosis is a postoperative prognostic marker for pancreatic cancer patients with a high interobserver reproducibility in histological evaluation. Br. J. Cancer 103, 1057–1065 (2010).
Hangai, S. et al. PGE2 induced in and released by dying cells functions as an inhibitory DAMP. Proc. Natl Acad. Sci. USA 113, 3844–3849 (2016).
Katoh, H. et al. CXCR2-expressing myeloid-derived suppressor cells are essential to promote colitis-associated tumorigenesis. Cancer Cell 24, 631–644 (2013).
Amson, R. et al. Reciprocal repression between P53 and TCTP. Nat. Med. 18, 91–99 (2011).
Cans, C. et al. Translationally controlled tumor protein acts as a guanine nucleotide dissociation inhibitor on the translation elongation factor eEF1A. Proc. Natl Acad. Sci. USA 100, 13892–13897 (2003).
Du, J., Yang, P., Kong, F. & Liu, H. Aberrant expression of translationally controlled tumor protein (TCTP) can lead to radioactive susceptibility and chemosensitivity in lung cancer cells. Oncotarget 8, 101922–101935 (2017).
Amson, R., Pece, S., Marine, J. C., Di Fiore, P. P. & Telerman, A. TPT1/ TCTP-regulated pathways in phenotypic reprogramming. Trends Cell Biol. 23, 37–46 (2013).
Revesz, L. Effect of tumour cells killed by X-rays upon the growth of admixed viable cells. Nature 178, 1391–1392 (1956).
Oshima, M. et al. Loss of Apc heterozygosity and abnormal tissue building in nascent intestinal polyps in mice carrying a truncated Apc gene. Proc. Natl Acad. Sci. USA 92, 4482–4486 (1995).
Tiberio, L. et al. Chemokine and chemotactic signals in dendritic cell migration. Cell. Mol. Immunol. 15, 346–352 (2018).
Highfill, S. L. et al. Disruption of CXCR2-mediated MDSC tumor trafficking enhances anti-PD1 efficacy. Sci. Transl. Med. 6, 237ra267 (2014).
Kawai, T. & Akira, S. The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors. Nat. Immunol. 11, 373–384 (2010).
Gong, T., Liu, L., Jiang, W. & Zhou, R. DAMP-sensing receptors in sterile inflammation and inflammatory diseases. Nat. Rev. Immunol. 20, 95–112 (2020).
Scheeren, F. A. et al. A cell-intrinsic role for TLR2-MYD88 in intestinal and breast epithelia and oncogenesis. Nat. Cell Biol. 16, 1238–1248 (2014).
Fujita, T. et al. Human fortilin is a molecular target of dihydroartemisinin. FEBS Lett. 582, 1055–1060 (2008).
Zhang, F. et al. Dihydroartemisinin inhibits TCTP-dependent metastasis in gallbladder cancer. J. Exp. Clin. Cancer Res. 36, 68 (2017).
Weber, R. et al. Myeloid-derived suppressor cells hinder the anti-cancer activity of immune checkpoint inhibitors. Front. Immunol. 9, 1310 (2018).
Bronte, V. et al. Recommendations for myeloid-derived suppressor cell nomenclature and characterization standards. Nat. Commun. 7, 12150 (2016).
Rooney, M. S., Shukla, S. A., Wu, C. J., Getz, G. & Hacohen, N. Molecular and genetic properties of tumors associated with local immune cytolytic activity. Cell 160, 48–61 (2015).
Kolaczkowska, E. & Kubes, P. Neutrophil recruitment and function in health and inflammation. Nat. Rev. Immunol. 13, 159–175 (2013).
Sinha, P., Clements, V. K., Bunt, S. K., Albelda, S. M. & Ostrand-Rosenberg, S. Cross-talk between myeloid-derived suppressor cells and macrophages subverts tumor immunity toward a type 2 response. J. Immunol. 179, 977–983 (2007).
Zhang, J. et al. CD13hi neutrophil-like myeloid-derived suppressor cells exert immune suppression through arginase 1 expression in pancreatic ductal adenocarcinoma. Oncoimmunology 6, e1258504 (2017).
Kimura, Y. et al. The innate immune receptor dectin-2 mediates the phagocytosis of cancer cells by Kupffer cells for the suppression of liver metastasis. Proc. Natl Acad. Sci. USA 113, 14097–14102 (2016).
Kim, M. et al. Dimerization of translationally controlled tumor protein is essential for its cytokine-like activity. PLoS ONE 4, e6464 (2009).
Walsh, B. J., Gooley, A. A., Williams, K. L. & Breit, S. N. Identification of macrophage activation associated proteins by two-dimensional gel electrophoresis and microsequencing. J. Leukoc. Biol. 57, 507–512 (1995).
Epperly, R., Gottschalk, S. & Velasquez, M. P. A bump in the road: how the hostile AML microenvironment affects CAR T cell therapy. Front. Oncol. 10, 262 (2020).
Wu, T. D. et al. Peripheral T cell expansion predicts tumour infiltration and clinical response. Nature 579, 274–278 (2020).
Price, J. G. et al. CDKN1A regulates Langerhans cell survival and promotes Treg cell generation upon exposure to ionizing irradiation. Nat. Immunol. 16, 1060–1068 (2015).
Seifert, L. et al. The necrosome promotes pancreatic oncogenesis via CXCL1 and Mincle-induced immune suppression. Nature 532, 245–249 (2016).
Biswas, S. K. & Lopez-Collazo, E. Endotoxin tolerance: new mechanisms, molecules and clinical significance. Trends Immunol. 30, 475–487 (2009).
Butcher, S. K., O'Carroll, C. E., Wells, C. A. & Carmody, R. J. Toll-like receptors drive specific patterns of tolerance and training on restimulation of macrophages. Front. Immunol. 9, 933 (2018).
Chiba, S. et al. Recognition of tumor cells by Dectin-1 orchestrates innate immune cells for anti-tumor responses. Elife 3, e04177 (2014).
Takaoka, A. et al. Integral role of IRF-5 in the gene induction programme activated by Toll-like receptors. Nature 434, 243–249 (2005).
Cerami, E. et al. The cBio cancer genomics portal: an open platform for exploring multidimensional cancer genomics data. Cancer Discov. 2, 401–404 (2012).
Gao, J. et al. Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci. Signal. 6, pl1 (2013).
Crowe, A. R. & Yue, W. Semi-quantitative determination of protein expression using immunohistochemistry staining and analysis: an integrated protocol. Bioprotocol https://doi.org/10.21769/BioProtoc.3465 (2019).
Takaoka, A. et al. DAI (DLM-1/ZBP1) is a cytosolic DNA sensor and an activator of innate immune response. Nature 448, 501–505 (2007).
Acknowledgements
We thank H.-F. Yang-Yen and S. Robine for providing Tctpflox mice and Villin-Cre-ERT2 mice, respectively. We also thank T. Nitta, T. Tanoue and K. Honda for providing materials. We thank M. Sugahara for technical assistance. This work was supported in part by a Grant-In-Aid for Young Scientists 18030848 (S. Hangai); Scientific Research (S) 15638461 (T.T.); Scientific Research (A) 20298458 (T.T.); and a Research Fellowship for Young Scientists 19J00887 (S. Hibino) from the Ministry of Education, Culture, Sports, Science of Japan (MEXT); Grant AMED-PRIME JP20gm6110008 (H.Y.) from the Japan Agency for Medical Research and Development; the Uehara Memorial Foundation (S. Hangai); the Takeda Science Foundation (S. Hangai); and the Naito Foundation (H.Y.). The Department of Inflammology is supported by the BONAC Corporation.
Author information
Authors and Affiliations
Contributions
S. Hangai, H.Y. and T.T. designed the research; S. Hangai., Y.K., C.-Y. C., T. Kawamura and H.Y. performed experiments; S. Hangai, Y.K., C.-Y. C., S. Hibino, T. Kawamura, K.M., K.K. and H.Y. analyzed data; T. Kodama, T. Kawamura, D.Y., Y.N., R.T., M.O. and H.O. contributed new reagents or analytic tools; S. Hangai, H.Y. and T.T. gave directions for the project and wrote the paper.
Corresponding authors
Ethics declarations
Competing interests
A patent is pending regarding this study; the patent applicant is the University of Tokyo. Inventors are T.T., H.Y. and S. Hangai. The anti-TCTP monoclonal antibody is covered in the patent application (Japanese patent application no. 2020-147222). The remaining authors declare no competing interests.
Additional information
Peer review information Nature Immunology thanks Michael Lotze and Yuting Ma for their contribution to the peer review of this work. Zoltan Fehervari was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Tumor cell death and release of immunomodulatory molecules.
a, Representative images of hematoxylin & eosin (H&E) and TUNEL staining of the SL4 tumor cells undergoing cell death in C57BL/6 mice (top row). Higher magnification images from the black boxes in the top row are displayed in the lower row. Arrowheads indicate necrotic lesions. Scale bars = 100 μm. The experiments were performed twice with similar results. b, PECs (2 × 105 cells) were incubated with the conditioned supernatant of dead SL4 cells (2 × 106 cells) for 2 hours then subjected to a microarray analysis (n = 2). A volcano plot shows differentially expressed genes indicated in red or green. Sup.: conditioned supernatant. c, PECs (2 × 105 cells) were stimulated with conditioned supernatant of dead SL4 cells (2 × 106 cells) for 2 hours then Cxcl1 (far left), Cxcl2 (near left), Tnf (near right) and Il1b (far right) mRNA were quantified by RT-qPCR (n = 3). Sup.: conditioned supernatant. n represents biologically independent samples (b, c). Data are shown as means ± standard error of the mean (s.e.m.).
Extended Data Fig. 2 Identification of the dead-cell-derived immunomodulator(s).
a, A schematic of strategy to purify immunogenic molecule(s) from the conditioned supernatant. b, Conditioned SL4 supernatant was subjected to anion (Hitrap Q) and cation (Hitrap S) exchange column chromatography. The flow-through of the Hitrap S column was collected and subjected to Hitrap Q column. The binding fraction was collected and then subjected to size-exclusion chromatography. Each fraction was added to PECs (Cxcl1, Cxcl2 and Il1b; 2 × 105 cells) or RAW264.7 cells (Tnf; 2 × 105 cells) and incubated for 2 hours. Cxcl1 (upper), Cxcl2 (upper middle), Tnf (lower middle) and Il1b (lower) mRNA were quantified by RT-qPCR. c, Fractions 25, 26 and 27, which showed cytokine-inducing activity, were subjected to SDS-PAGE and silver staining. The band (indicated by an arrow), the intensity of which correlates with the cytokine mRNA induction level, was excised and then subjected to LC-MS analysis. This analysis revealed that TCTP is the most abundant protein.
Extended Data Fig. 3 Dependence of TCTP for tumor cell growth.
a, SL4 cells were subjected to apoptosis (serum-free and adriamycin) or necrosis (freeze-and-thaw). Conditioned media were collected and TCTP protein levels were determined by immunoblotting (n = 3). b, Sera from B16F10 (left) or Meth-A (right) tumor bearing mice were collected 0 (NTB; n = 3) and 21 (TB; n = 6) days after subcutaneous tumor injection and TCTP levels were quantified by immunoblotting. NTB: non-tumor bearing. TB: tumor bearing. c, TCTP protein expression in SL4, B16F10 and Meth-A cells without (WT) or with CRISPR/Cas9-mediated Tctp gene inactivation (KO). Whole cell lysates of the indicated cell lines were prepared and subjected to immunoblot analysis for the TCTP and β-actin proteins. The experiments were performed twice with similar results. d, Cell number measurements of WT and TCTP KO SL4 cells grown in vitro at the indicated time points (n = 3). e, TCTP WT and KO SL4 cells (2 × 105 cells) were cultured under normal (20% O2, 10% FBS), low serum (20% O2, 1% FBS) or hypoxic (1% O2, 10% FBS) condition. After 72 h, cell numbers were counted (n = 3). f, WT, TCTP KO and WT-TCTP (TCTP KO cells expressing WT TCTP cDNA) SL4 cells (2 × 105 cells) were transplanted subcutaneously into C57BL/6 mice (n = 5) and tumor volumes were measured at the indicated time points. g, h, Cell number measurements of WT and TCTP KO B16F10 (g) or Meth-A cells (h) grown in vitro at the indicated time points (n = 3). n represents biologically independent samples (a, d, e, g, h) or animals (b, f). Unpaired two-sided Student’s t-test (b, e), repeated measures one-way ANOVA with Tukey’s multiple comparisons test (f). Data are shown as means ± s.e.m.
Extended Data Fig. 4 Functional effect of extracellular TCTP in the induction of chemokine mRNAs.
a, Confocal microscopy analysis of SL4 mutant cells. TCTP KO (left), WT-TCTP (TCTP KO cells expressing WT TCTP cDNA; middle), and IL-2ss-TCTP SL4 cells (TCTP cells expressing cDNA for IL-2ss-TCTP; right) were stained for TCTP and nuclei (DAPI). Scale bars = 20 μm. b, PECs (2 × 105 cells) were stimulated with conditioned media from Mock or IL-2ss-TCTP SL4 cells for 2 hours then Cxcl1 (left) and Cxcl2 (right) mRNAs measured by RT-qPCR (n = 3). c, WT and TCTP KO SL4 cells (2 × 105 cells) were transplanted subcutaneously into C57BL/6 mice (n = 5). Tumors were then excised at day 21 and whole tumor lysates were prepared. G-CSF (left) and GM-CSF (right) levels were determined by cytometric bead array (CBA). n represents biologically independent samples (b) or animals (c).Unpaired two-sided Student’s t-test (b, c). Data are shown as means ± s.e.m.
Extended Data Fig. 5 TCTP modulates MDSC number and in vivo tumor growth.
a, WT or TCTP KO B16F10 cells (1 × 105 cells) were transplanted subcutaneously into C57BL/6 mice. After 17 days, single cell suspension was prepared from the tumors and subject to flow cytometry analysis (n = 4). Shown are percentages of PMN-MDSC or M-MDSC within CD45+ cells. b, WT (n = 3) and TCTP KO (n = 4) Meth-A cells (5 × 105 cells) were transplanted into C57BL/6 mice and flow cytometry analysis was performed as in (a). Shown are percentages of PMN-MDSC or M-MDSC within CD45+ cells. c, TCTP KO SL4 cells were transplanted subcutaneously into C57BL/6 mice. At day 1, 4, 7, 10 and 13, PBS control or PMN-MDSCs isolated from spleen and bone marrow from SL4 tumor bearing mice were inoculated intraperitoneally. Tumor volume was then measured at the indicated time points. PBS; n = 5, PMN-MDSC; n = 4. d, Mock (KO) SL4 cells and IL-2ss-TCTP cells (2 × 105 cells) were each transplanted subcutaneously into C57BL/6 mice. Anti-Ly6G or control IgG was administered intraperitoneally every 2 days starting at day 1 (n = 5). (Left) Tumor volume was then measured at the indicated time points. (Right) Shown are percentages of PMN-MDSC within CD45+ cells. e, WT and TCTP KO SL4 cells (2 × 105 cells) were transplanted subcutaneously into C57BL/6 mice (n = 3). After 18 days, single cell suspension was prepared from the tumors and subject to flow cytometry analysis. Mean fluorescence intensity (MFI) of the indicated markers for NK cell activation was determined. n represents biologically independent samples animals (a-e). Unpaired two-sided Student’s t-test (a-c, e), repeated measures one-way ANOVA with Tukey’s multiple comparisons test (d). Data are shown as means ± s.e.m.
Extended Data Fig. 6 Effect of TCTP on the expression of immune checkpoint molecules and angiogenesis.
a, b, Mock and IL-2ss-TCTP SL4 cells (2 × 105 cells) were transplanted subcutaneously into C57BL/6 mice (n = 4). After 21 days, single cell suspension was prepared from the tumors and subject to flow cytometry analysis. Mean fluorescence intensity (MFI) of PD-L1 (a) and PD-1 (b) was determined. c, (Left) Representative CD31 stains of TCTP WT and KO SL4 tumor subcutaneously injected into C57BL/6 mice. The experiments were performed twice with similar results. Scale bar = 100 μm. (Right) Quantification of CD31 positive area (n = 5). n represents biologically independent animals (a-c). Unpaired two-sided Student’s t-test (c). Data are shown as means ± s.e.m.
Extended Data Fig. 7 Extracellular TCTP mediates a crosstalk between PMN-MDSCs and M-MDSCs in tumor immune microenvironment.
a, PECs (2 × 105 cells) or SL4 cells (1 × 105 cells) were stimulated with indicated concentration of a recombinant TCTP for 2 hours and then Cxcl1 mRNA quantified by RT-qPCR (n = 3). b, Cxcl1 mRNA levels in WT and TCTP KO SL4 cells were determined by RT-qPCR n = 3. c, SL4 (2 × 105 cells) cells were transplanted subcutaneously into C57BL/6 mice (n = 3) and after 21 days, single cell suspensions were prepared from the tumors. The indicated immune cell populations were sorted and the levels of Cxcr2 mRNA of each population were determined by RT-qPCR. The experiments were performed twice with similar results. n represents biologically independent samples (a, b) or animals (c). Unpaired two-sided Student’s t-test (b). repeated measures one-way ANOVA with Dunnett’s multiple comparisons test (c). Data are shown as means ± s.e.m.
Extended Data Fig. 8 Extracellular TCTP mediates chemokine induction and in vivo tumor growth via TLR2.
a, WT or TLR2 deficient peritoneal exudate cells (PECs) (2 × 105 cells) were stimulated with the indicated concentrations of recombinant IL-1α for 2 hours and Cxcl1 mRNA levels were quantified by RT-qPCR (n = 3). b, Immunoprecipitaion assay for binding of TCTP to TLR2. HEK293T cells transiently expressing TLR2-YFP together with Flag–TCTP were analyzed by immunoprecipitation with anti-GFP antibody, followed by immunoblotting with anti-Flag antibody (upper). TLR2 and TCTP were detected in whole cell lysates (bottom). The experiments were performed twice with similar results. c, A luciferase reporter construct containing multimerized NFκB binding motifs and the expression vector for the indicated proteins was transfected into HEK293T cells. After 24 h of transfection, HEK293T cells (2 × 104 cells) were seeded onto 96-well plate and stimulated with recombinant TCTP (15 nM or 50 nM) or an agonist for each TLR (Pam3CSK4 300 ng/ml, poly I:C 100 μg/ml, poly U 10 μg/ml, CpG-M 1μM). After 6 h of simulation, cell lysates were extracted and subjected to luciferase assay (n = 3). d, e, SL4 (d) or IL-2ss-TCTP cells (e) (2 × 105 cells) were transplanted subcutaneously into WT (SL4; n = 7, IL-2ss-TCTP; n = 6) or TLR2 KO mice (SL4; n = 5, IL-2ss-TCTP; n = 6). Tumor volumes were measured at the indicated time points. f, IL-2ss-TCTP SL4 cells (2 × 105 cells) were transplanted subcutaneously into C57BL/6 mice and tumor volumes were measured at the indicated time points. O-vanillin (50 mg/kg) was orally administered every two days starting from day 1 following tumor challenge (n = 6). n represents biologically independent samples (a, c) or animals (d-f). Unpaired two-sided Student’s t-test (c-f). Data are shown as means ± s.e.m.
Extended Data Fig. 9 Effect of anti-TCTP monoclonal antibody on Cxcl1 mRNA induction and the TCTP status in human colon cancer.
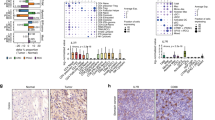
a, Whole cell lysates of WT or TCTP KO SL4 cells were prepared and subjected to immunoblot analysis by 55F3, a monoclonal antibody raised against human TCTP. The experiments were performed twice with similar results. b, PECs (2 × 105 cells) were stimulated with conditioned supernatant of SL4 cells with 55F3 or control IgG and after 2 hours of stimulation, Cxcl1 mRNA levels were determined by RT-qPCR. n = 3. Sup.: conditioned supernatant. c, TCTP WT or KO cells (1 × 105 cells) were transplanted subcutaneously into C57BL/6 mice. DHA (50 mg/kg) or DMSO was injected intraperitoneally every day from day 1 following tumor challenge (n = 6). d, (Left) The expression levels of TCTP in stromal area of normal colonic mucosa and colorectal cancer tissue were compared. (Right) The comparison was also performed between normal colonic crypt and tumor lesions. e, Co-expression plots of CD8A, GZMB, PRF1 or CD69 by TCTP mRNA in a TCGA colorectal cancer dataset (n = 382). Spearman correlation coefficients are shown. f, Correlation of cytolytic activity (defined as the geometric mean of GZMA and PRF1 mRNA expression) and TCTP mRNA in a TCGA colon cancer dataset (n = 382). Spearman correlation coefficients are shown. g, A graphical summary. TCTP is released by dead tumor cells and induces CXCL1/2 chemokines most notably in M-MDSCs. These chemokines in turn recruit PMN-MDSCs into the TIME, thereby suppressing anti-tumor immune responses to promote tumor growth. n represents biologically independent samples (b), animals (c) or human samples (d-f). Repeated measures one-way ANOVA with Dunnett’s multiple comparisons test (b) or Tukey’s multiple comparisons test (c), unpaired two-sided Student’s t-test (d). Data are shown as means ±s.e.m.
Supplementary information
Supplementary Information
The gating strategy for flow cytometry analysis.
Supplementary Tables
Supplementary Tables 1–3.
Source data
Source Data Fig. 1
Statistical source data.
Source Data Fig. 1
Unprocessed immunoblots.
Source Data Fig. 2
Statistical source data.
Source Data Fig. 3
Statistical source data.
Source Data Fig. 4
Statistical source data.
Source Data Fig. 5
Statistical source data.
Source Data Fig. 6
Statistical source data.
Source Data Fig. 7
Statistical source data.
Source Data Extended Data Fig. 1
Statistical source data.
Source Data Extended Data Fig. 2
Statistical source data.
Source Data Extended Data Fig. 2
Unprocessed gel.
Source Data Extended Data Fig. 3
Statistical source data.
Source Data Extended Data Fig. 3
Unprocessed immunoblots.
Source Data Extended Data Fig. 4
Statistical source data.
Source Data Extended Data Fig. 5
Statistical source data.
Source Data Extended Data Fig. 6
Statistical source data.
Source Data Extended Data Fig. 7
Statistical source data.
Source Data Extended Data Fig. 8
Statistical source data.
Source Data Extended Data Fig. 8
Unprocessed immunoblots.
Source Data Extended Data Fig. 9
Statistical source data.
Source Data Extended Data Fig. 9
Unprocessed immunoblots.
Rights and permissions
About this article
Cite this article
Hangai, S., Kawamura, T., Kimura, Y. et al. Orchestration of myeloid-derived suppressor cells in the tumor microenvironment by ubiquitous cellular protein TCTP released by tumor cells. Nat Immunol 22, 947–957 (2021). https://doi.org/10.1038/s41590-021-00967-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41590-021-00967-5
This article is cited by
-
FFAR2 expressing myeloid-derived suppressor cells drive cancer immunoevasion
Journal of Hematology & Oncology (2024)
-
Pharmaceutical targeting of OTUB2 sensitizes tumors to cytotoxic T cells via degradation of PD-L1
Nature Communications (2024)
-
Specific lineage transition of tumor-associated macrophages elicits immune evasion of ascitic tumor cells in gastric cancer with peritoneal metastasis
Gastric Cancer (2024)
-
The combination of PD-L1 expression and the neutrophil-to-lymphocyte ratio as a prognostic factor of postoperative recurrence in non-small-cell lung cancer: a retrospective cohort study
BMC Cancer (2023)
-
Drug-loaded microbubble delivery system to enhance PD-L1 blockade immunotherapy with remodeling immune microenvironment
Biomaterials Research (2023)