Abstract
Early recruitment of neutrophils from the blood to sites of tissue infection is a hallmark of innate immune responses. However, little is known about the mechanisms by which apoptotic neutrophils are cleared in infected tissues during resolution and the immunological consequences of in situ efferocytosis. Using intravital multiphoton microscopy, we show previously unrecognized motility patterns of interactions between neutrophils and tissue-resident phagocytes within the influenza-infected mouse airway. Newly infiltrated inflammatory monocytes become a chief pool of phagocytes and play a key role in the clearance of highly motile apoptotic neutrophils during the resolution phase. Apoptotic neutrophils further release epidermal growth factor and promote the differentiation of monocytes into tissue-resident antigen-presenting cells for activation of antiviral T cell effector functions. Collectively, these results suggest that the presence of in situ neutrophil resolution at the infected tissue is critical for optimal CD8+ T cell–mediated immune protection.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding authors upon reasonable request. Source data are provided with this paper.
References
Girard, M. P., Cherian, T., Pervikov, Y. & Kieny, M. P. A review of vaccine research and development: human acute respiratory infections. Vaccine 23, 5708–5724 (2005).
Garner, H. & de Visser, K. E. Neutrophils take a round-trip. Science 358, 42–43 (2017).
Hasenberg, A. et al. Catchup: a mouse model for imaging-based tracking and modulation of neutrophil granulocytes. Nat. Meth. 12, 445–452 (2015).
Hind, L. E. & Huttenlocher, A. Neutrophil reverse migration and a chemokinetic resolution. Dev. Cell 47, 404–405 (2018).
Wang, J. et al. Visualizing the function and fate of neutrophils in sterile injury and repair. Science 358, 111–116 (2017).
Holmgren, L., Bergsmedh, A. & Spetz, A. L. Horizontal transfer of DNA by the uptake of apoptotic bodies. Vox Sang. 83, 305–306 (2002).
Holmgren, L. et al. Horizontal transfer of DNA by the uptake of apoptotic bodies. Blood 93, 3956–3963 (1999).
Bergsmedh, A. et al. Horizontal transfer of oncogenes by uptake of apoptotic bodies. Proc. Natl Acad. Sci. USA 98, 6407–6411 (2001).
Yan, B., Wang, H., Li, F. & Li, C. Y. Regulation of mammalian horizontal gene transfer by apoptotic DNA fragmentation. Br. J. Cancer 95, 1696–1700 (2006).
Hyun, Y. M. et al. Uropod elongation is a common final step in leukocyte extravasation through inflamed vessels. J. Exp. Med. 209, 1349–1362 (2012).
Poo, Y. S. et al. CCR2 deficiency promotes exacerbated chronic erosive neutrophil-dominated chikungunya virus arthritis. J. Virol. 88, 6862–6872 (2014).
Kuziel, W. A. et al. Severe reduction in leukocyte adhesion and monocyte extravasation in mice deficient in CC chemokine receptor 2. Proc. Natl Acad. Sci. USA 94, 12053–12058 (1997).
Oshima, T. et al. Analysis of corneal inflammation induced by cauterisation in CCR2 and MCP-1 knockout mice. Br. J. Ophthalmol. 90, 218–222 (2006).
Hart, S. P., Dransfield, I. & Rossi, A. G. Phagocytosis of apoptotic cells. Methods 44, 280–285 (2008).
Dzhagalov, I. L., Chen, K. G., Herzmark, P. & Robey, E. A. Elimination of self-reactive T cells in the thymus: a timeline for negative selection. PLoS Biol. 11, e1001566 (2013).
Ichikawa, A. et al. CXCL10-CXCR3 enhances the development of neutrophil-mediated fulminant lung injury of viral and nonviral origin. Am. J. Respir. Crit. Care Med. 187, 65–77 (2013).
Reichel, C. A. et al. Chemokine receptors Ccr1, Ccr2, and Ccr5 mediate neutrophil migration to postischemic tissue. J. Leuk. Biol. 79, 114–122 (2006).
De Filippo, K. et al. Mast cell and macrophage chemokines CXCL1/CXCL2 control the early stage of neutrophil recruitment during tissue inflammation. Blood 121, 4930–4937 (2013).
Hartl, D. et al. Infiltrated neutrophils acquire novel chemokine receptor expression and chemokine responsiveness in chronic inflammatory lung diseases. J. Immunol. 181, 8053–8067 (2008).
Beauvillain, C. et al. CCR7 is involved in the migration of neutrophils to lymph nodes. Blood 117, 1196–1204 (2011).
Jia, G. Q. et al. Distinct expression and function of the novel mouse chemokine monocyte chemotactic protein-5 in lung allergic inflammation. J. Exp. Med. 184, 1939–1951 (1996).
Kaur, M. & Singh, D. Neutrophil chemotaxis caused by chronic obstructive pulmonary disease alveolar macrophages: the role of CXCL8 and the receptors CXCR1/CXCR2. J. Pharmacol. Exp. Ther. 347, 173–180 (2013).
Soehnlein, O. & Lindbom, L. Phagocyte partnership during the onset and resolution of inflammation. Nat. Rev. 10, 427–439 (2010).
Wynn, T. A. & Vannella, K. M. Macrophages in tissue repair, regeneration, and fibrosis. Immunity 44, 450–462 (2016).
Dominguez, P. M. & Ardavin, C. Differentiation and function of mouse monocyte-derived dendritic cells in steady state and inflammation. Immunol. Rev. 234, 90–104 (2010).
Jakubzick, C. V., Randolph, G. J. & Henson, P. M. Monocyte differentiation and antigen-presenting functions. Nat. Rev. 17, 349–362 (2017).
Broz, M. L. et al. Dissecting the tumor myeloid compartment reveals rare activating antigen-presenting cells critical for T cell immunity. Cancer Cell 26, 938 (2014).
Chang, T. T., Jabs, C., Sobel, R. A., Kuchroo, V. K. & Sharpe, A. H. Studies in B7-deficient mice reveal a critical role for B7 costimulation in both induction and effector phases of experimental autoimmune encephalomyelitis. J. Exp. Med. 190, 733–740 (1999).
Krummel, M. F., Heath, W. R. & Allison, J. Differential coupling of second signals for cytotoxicity and proliferation in CD8+ T cell effectors: amplification of the lytic potential by B7. J. Immunol. 163, 2999–3006 (1999).
Lindsay, R. S. et al. Antigen recognition in the islets changes with progression of autoimmune islet infiltration. J. Immunol. 194, 522–530 (2015).
Thornton, E. E. et al. Spatiotemporally separated antigen uptake by alveolar dendritic cells and airway presentation to T cells in the lung. J. Exp. Med. 209, 1183–1199 (2012).
Ley, K. The second touch hypothesis: T cell activation, homing and polarization. F1000 Res. 3, 37 (2014).
Serbina, N. V., Jia, T., Hohl, T. M. & Pamer, E. G. Monocyte-mediated defense against microbial pathogens. Annu. Rev. Immunol. 26, 421–452 (2008).
Serbina, N. V., Salazar-Mather, T. P., Biron, C. A., Kuziel, W. A. & Pamer, E. G. TNF/iNOS-producing dendritic cells mediate innate immune defense against bacterial infection. Immunity 19, 59–70 (2003).
Varol, C. et al. Monocytes give rise to mucosal, but not splenic, conventional dendritic cells. J. Exp. Med. 204, 171–180 (2007).
Ginhoux, F. et al. Langerhans cells arise from monocytes in vivo. Nat. Immunol. 7, 265–273 (2006).
Jakubzick, C. et al. Minimal differentiation of classical monocytes as they survey steady-state tissues and transport antigen to lymph nodes. Immunity 39, 599–610 (2013).
Larson, S. R. et al. Ly6C+ monocyte efferocytosis and cross-presentation of cell-associated antigens. Cell Death Differ. 23, 997–1003 (2016).
Schnorrer, P. et al. The dominant role of CD8+ dendritic cells in cross-presentation is not dictated by antigen capture. Proc. Natl Acad. Sci. USA 103, 10729–10734 (2006).
Iyoda, T. et al. The CD8+ dendritic cell subset selectively endocytoses dying cells in culture and in vivo. J. Exp. Med. 195, 1289–1302 (2002).
Desch, A. N. et al. CD103+ pulmonary dendritic cells preferentially acquire and present apoptotic cell-associated antigen. J. Exp. Med. 208, 1789–1797 (2011).
Sichien, D., Lambrecht, B. N., Guilliams, M. & Scott, C. L. Development of conventional dendritic cells: from common bone marrow progenitors to multiple subsets in peripheral tissues. Mucosal. Immunol. 10, 831–844 (2017).
Schlitzer, A. et al. IRF4 transcription factor-dependent CD11b+ dendritic cells in human and mouse control mucosal IL-17 cytokine responses. Immunity 38, 970–983 (2013).
Saederup, N. et al. Selective chemokine receptor usage by central nervous system myeloid cells in CCR2-red fluorescent protein knock-in mice. PLoS ONE 5, e13693 (2010).
Mempel, T. R., Henrickson, S. E. & von Andrian, U. H. T-cell priming by dendritic cells in lymph nodes occurs in three distinct phases. Nature 427, 154–159 (2004).
Herz, J., Johnson, K. R. & McGavern, D. B. Therapeutic antiviral T cells noncytopathically clear persistently infected microglia after conversion into antigen-presenting cells. J. Exp. Med. 212, 1153–1169 (2015).
DiPiazza, A. et al. Pandemic 2009 H1N1 Influenza Venus reporter virus reveals broad diversity of MHC class II-positive antigen-bearing cells following infection in vivo. Sci. Rep. 7, 10857 (2017).
Shortman, K. & Naik, S. H. Steady-state and inflammatory dendritic-cell development. Nat. Rev. 7, 19–30 (2007).
Xu, Y., Loison, F. & Luo, H. R. Neutrophil spontaneous death is mediated by down-regulation of autocrine signaling through GPCR, PI3Kγ, ROS, and actin. Proc. Natl Acad. Sci. USA 107, 2950–2955 (2010).
Lim, K. et al. Neutrophil trails guide influenza-specific CD8+ T cells in the airways. Science 349, aaa4352 (2015).
Hohl, T. M. et al. Inflammatory monocytes facilitate adaptive CD4 T cell responses during respiratory fungal infection. Cell Host Microbe 6, 470–481 (2009).
Zhao, G. et al. Activation of epidermal growth factor receptor in macrophages mediates feedback inhibition of M2 polarization and gastrointestinal tumor cell growth. J. Bio. Chem. 291, 20462–20472 (2016).
Darzynkiewicz, Z., Pozarowski, P., Lee, B. W. & Johnson, G. L. Fluorochrome-labeled inhibitors of caspases: convenient in vitro and in vivo markers of apoptotic cells for cytometric analysis. Methods Mol. Biol. 682, 103–114 (2011).
Acknowledgements
We thank T. Hohl and A. Rivera for CCR2-DTR mouse and F. Yan for EGFR-cKO (Egfrflox/LysMCre) mouse. We especially thank M. Gunzer for CatchupIVM-Red mouse, Y. Gao for the technical assistance with IV-MPM and J. Ashton for help with transcriptomic analyses and depositing RNA-sequencing data. This project was financially supported through grants from the National Institute of Health (nos. AI143182, AI147362 and AI149775 to M.K., no. AI102851 to M.K., D.J.F. and D.J.T., no. AI138415 to H.P. and no. AI070826 to D.J.F.)
Author information
Authors and Affiliations
Contributions
K.L. conducted all in vivo imaging and the mouse influenza infection experiments and analyzed data. T.H.K., A.T., A.M.A., H.P., E.C.R., D.J.F. and D.J.T. performed experiments and analyzed data. M.K. and K.L. conceived, designed and directed this study. M.K. and K.L. wrote the manuscript with suggestions from all the authors. All authors reviewed and discussed the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Jamie D. K. Wilson and Ioana Visan were the primary editors on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Leukocyte recruitment in the influenza-infected trachea.
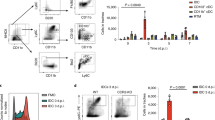
a, Schematic representation of the host immune responses in the airway during influenza infection. The various waves correspond to schemes (neutrophils, monocytes, CD8+ T cells, and macrophages) that summarize the data presented in Fig. 1a,b. b, Flow cytometry analysis of the neutrophil numbers in the dLN (mediastinal lymph node) of naïve or influenza-infected mice. c, Apoptotic neutrophils from WT or LysMCre mice (upper chamber) and bone marrow (BM)-derived macrophages from ROSAtdTomato mice (bottom chamber) were co-cultured for 7 days in the cell impermeable transwell system (0.4 μm pore size). Bar, 50 μm. d, Flow cytometry analysis of the BM and dLN of the mice in the experiments described in Fig. 1j. Note the lack of tdTomato+ cells in the BM and dLN. e, Live BM cells isolated from LysMCre or WT mice (20 – 50 x 106) were injected into the peritoneum of recipient ROSAtdTomato mice. Flow cytometry analysis of the peritoneal lavage revealed tdTomato+/F4/80+ macrophages in the mice that received LysMCre cells. Representative plots of the flow cytometry data from five independent experiments are shown. f, Blood cells (day 4 post HKx31 infection) from Ly6GCre/ROSAtdTomato/Csf1r-EGFP mice were analyzed by flow cytometry.
Extended Data Fig. 2 Monocytes promote neutrophil efferocytosis.
a, In vitro fluorescence images of apoptotic neutrophil-engulfed monocytes. Monocytes (green; GFP+Ly6C+Ly6G−) were sorted from influenza-infected Csf1r-EGFP mouse lungs and co-incubated with apoptotic neutrophils (red) isolated from Ly6GCre/ROSAtdTomato mice. Three hours later, Ly6G−Csfr1GFP cells were sorted again and imaged by fluorescence microscopy. Arrows indicate neutrophil-engulfed monocytes. Scale bar, 25 μm. b, Numbers of monocytes (left) and total neutrophils (middle) and percentages of Annexin V+ neutrophils (right) in the influenza-infected trachea of WT or CCR2 KO mice (n ≥ 3 per group).
Extended Data Fig. 3 Migration of early apoptotic neutrophil.
a, In vitro migration of Annexin V− vs. Annexin V+ neutrophils on the ICAM-1 coated surface. The mean velocity, displacement, and meandering index of the neutrophils are shown. n = 3 per group. Statistical differences were assessed by a nonparametric Mann-Whitney test. b, Chemokine microarray performed with total lysates of monocytes harvested on day 5 post infection from the influenza-infected mouse lung. Chemokine expression levels are expressed as arbitrary units measured by densitometry. c, Neutrophil migration via ICAM-1 with the indicated chemokines. A single assay analyzed at least 10 cells (n = 3 assays per group). *p <0.05 compared with the control. Data were analyzed with the Kruskal-Wallis test followed by Dunn’s posttest.
Extended Data Fig. 4 Monocytes promote T cell activation.
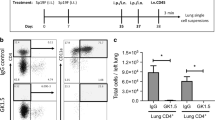
a, Flow cytometry analysis of neutrophils and monocytes from influenza-infected mouse trachea with or without neutrophil depletion. Cells were stained with Ly6C antibody and CD11b antibody (mean ± SEM, n = 4 mice per group). b, Numbers of monocytes (CD11b+Ly6C+Ly6G−) in the influenza-infected mouse trachea with or without neutrophil depletion. Data are presented as the mean ± SEM, n = 4 mice per group. Statistical differences were assessed by nonparametric Mann-Whitney test. c, RFP+ monocytes sorted from the trachea and lungs of HKx31-OVA virus-infected CCR2RFP/+ mice with or without neutrophil depletion were incubated with CD8+ T cells isolated from influenza-infected OT-I mouse dLNs. The monocyte-T cell conjugates were measured by microscopy. Conjugation (%); # monocytes bound to CD8+ T cells/# total monocytes. n ≥ 3 per group. Statistical differences were assessed by nonparametric Mann-Whitney test. d, Numbers of OT-I CD8+ T cells from the dLN and trachea of HKx31-OVA virus-infected WT or CCR2 KO mice. Data are presented as the mean ± SEM, n = 3 mice per group. Statistical differences were assessed by nonparametric Mann-Whitney test. e, Numbers of monocytes (CD11b+Ly6C+Ly6G−) in the influenza-infected trachea of CCR2-DTR and WT mice on day 6 post infection. Diphtheria toxin was injected into both mouse strains on days -1, +1, +3, and +5 post infection. f, Flow cytometry analysis of the production of IFN-γ, TNF, and Granzyme B (Gzm B) in CD8+ T cells on day 7 post infection from WT vs. CCR2-DTR influenza-infected mice treated with diphtheria toxin. Statistical differences were assessed by nonparametric Mann-Whitney test.
Extended Data Fig. 5 Neutrophil EGF regulates DC-differentiation of monocytes.
a, Immunofluorescence image of a permeabilized neutrophil stained with Abs against Ly6G (green) and EGF (red). Scale bar, 5 μm. b, Flow cytometry analysis of EGF in permeabilized mouse neutrophils (day 4 post-infection). c, Secretion of EGF from neutrophils undergoing spontaneous apoptosis. d, Flow cytometry analysis of phagocytic activity (tdTomato) of monocytes (Csf1r-GFP) isolated from the influenza infected lung after co-incubation with tdTomato+ apoptotic neutrophils for 12 h in the presence of PBS or erlotinib (0.1 μg/ml). e, Monocytes (Csf1r-GFP) were isolated from the influenza infected lung. After co-incubation with tdTomato+ apoptotic neutrophils for 12 h in the presence of PBS or erlotinib (0.1 μg/ml), neutrophil-engulfed (tdTomato+) and non-engulfed (tdTomato−) monocytes were sorted, pulsed with OVA peptide, and incubated with CD8+ T cells isolated from influenza-infected OT-I mouse dLNs. Monocyte-T cell conjugation was measured by microscopy. Data are presented as the mean ± SEM, n ≥ 3 mice per group. Statistical differences were assessed by nonparametric Mann-Whitney test.
Supplementary information
Supplementary Information
Primers used in RT–qPCR.
Supplementary Video 1
Neutrophil migration in the influenza-infected mouse trachea. 3D reconstruction of an IV-MPM image showing migration of neutrophils in the mouse trachea (Ly6GCre/ROSAtdTomato) (day 5 after influenza infection) without overt neutrophil reverse migration. Red, neutrophil; white, blood vessel (Ab CD31). Scale bar, 50 μm. See Fig. 1c,d.
Supplementary Video 2
Live image of a color switch in ROSAtdTomato macrophages cocultured with apoptotic LysMCre neutrophils. In cocultures of apoptotic LysMCre neutrophils and ROSAtdTomato macrophages, converted tdTomato+ (red) cells appeared within 24 h and lived for up to 7 d. Scale bar, 20 μm. See Fig. 1f–h.
Supplementary Video 3
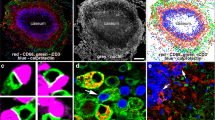
In vivo color switch in ROSAtdTomato phagocytes after engulfing apoptotic LysMCre neutrophils. A representative 3D image showing the in vivo color switch in ROSAtdTomato phagocytes. Neutrophils from LysMCre or WT mice were injected into the ears of ROSAtdTomato B6-Albino recipient mice. Five days later, the presence of tdTomato+ phagocytes (red) in the ears was examined by whole mount tissue staining with CD68 antibody (green) and DAPI (blue). See Fig. 1i.
Supplementary Video 4
IV-MPM of naive Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). In the steady state, 3D reconstruction of an IV-MPM image showed a main tissue-resident macrophage population (green) in the naive trachea. Scale bar, 50 μm. See Fig. 2f.
Supplementary Video 5
IV-MPM of influenza-infected Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). First part, examination of a 3D reconstruction of an IV-MPM image of the tracheal tissue on day 4 postinfection showed the presence of many GFP+ cells (monocyte/macrophage, white arrow) with engulfed tdTomato fluorescence (neutrophil). Scale bar, 20 μm. Second part, in vitro examples of tdTomato+GFP+ monocytes after incubation of tdTomato+ neutrophils and GFP+ monocytes. Scale bar, 20 μm.
Supplementary Video 6
IV-MPM of influenza-infected Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). 3D presentation showing the presence of a GFP+ cell (monocyte/macrophage) actively processing intracellular tdTomato fluorescence after engulfing neutrophils.
Supplementary Video 7
IV-MPM of influenza-infected (day 3) Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). Examination of tracheal tissue on day 3 postinfection showed the presence of both sessile and highly motile GFP+ cells (monocyte/macrophage) and actively migrating neutrophils (orange). Scale bar, 50 μm.
Supplementary Video 8
IV-MPM of influenza-infected (day 5) Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). On day 5 postinfection, most GFP+ cells became less motile, showing a morphology similar to that of tissue-resident macrophages, while most neutrophils (orange) remained highly motile. White, blood vessel (Ab CD31). Scale bar, 50 μm.
Supplementary Video 9
IV-MPM of influenza-infected (day 6) Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). On day 6 postinfection, most GFP+ cells were less motile, showing a morphology similar to that of tissue-resident macrophages, while most neutrophils (orange) remained highly motile. Note that the highly motile neutrophils were not newly extravasating cells from the blood vessels due to tissue injury. Scale bar, 50 μm.
Supplementary Video 10
IV-MPM of influenza-infected Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). 3D reconstruction and two-dimensional projection of IV-MPM images showing migration of neutrophils in the mouse trachea. Neutrophils (orange) in the influenza-infected trachea (day 6) were highly motile during the resolution phase, actively forming multiple serial encounters with the nonmigratory surrounding monocytes/macrophages (green). See Fig. 3c,d.
Supplementary Video 11
IV-MPM of influenza-infected Ly6GCreROSAtdTomatoCsf1r-EGFP mice (trachea). 3D reconstructions of IV-MPM images showing dynamic interactions between neutrophils and phagocytes (day 5 after influenza infection). First part, a highly motile neutrophil (orange, red arrow) during the resolution phase stopped at the target phagocyte (green, yellow arrow) to be engulfed. Second part, both neutrophil (orange, red arrow) and phagocyte (green, yellow arrow) actively migrated before the engulfment. See Fig. 3f.
Supplementary Video 12
T cell–monocyte-derived APC interaction in the influenza-infected trachea. IV-MPM of OT-I GFP+ CD8+ T cells in the influenza-infected trachea of CCR2-RFP mice on day 7 postinfection. OVA-specific CD8+ T cells (green) and CCR2+ monocytes (red) are shown. Scale bar, 50 μm. See Fig. 4e–h. First part, OT-I GFP+ CD8+ T cells and CCR2-RFP monocyte interaction in the HKx31-OVA virus-infected trachea. Second part, OT-I GFP+ CD8+ T cells and CCR2-RFP monocyte interaction in the HKx31-OVA virus-infected trachea. Virus-specific CD8+ T cell interactions with CCR2+ cells were assessed after i.v. injection of MHC I blocking (upper) or isotype control antibodies (lower). Third part, OT-I GFP+ CD8+ T cells and CCR2-RFP monocyte interaction in the HKx31-OVA virus-infected trachea after neutrophil depletion.
Source data
Source Data Fig. 6
Uncropped western blots
Source Data Extended Data Fig. 5
Uncropped western blot
Rights and permissions
About this article
Cite this article
Lim, K., Kim, Th., Trzeciak, A. et al. In situ neutrophil efferocytosis shapes T cell immunity to influenza infection. Nat Immunol 21, 1046–1057 (2020). https://doi.org/10.1038/s41590-020-0746-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41590-020-0746-x
This article is cited by
-
Fluorescence-amplified nanocrystals in the second near-infrared window for in vivo real-time dynamic multiplexed imaging
Nature Nanotechnology (2023)
-
Efferocytosis: a double-edged sword in microbial immunity
Archives of Microbiology (2023)
-
ST3GAL1 and βII-spectrin pathways control CAR T cell migration to target tumors
Nature Immunology (2023)
-
Axl receptor induces efferocytosis, dampens M1 macrophage responses and promotes heart pathology in Trypanosoma cruzi infection
Communications Biology (2022)
-
Drugging the efferocytosis process: concepts and opportunities
Nature Reviews Drug Discovery (2022)