Abstract
Humoral immune responses to microbial polysaccharide surface antigens can prevent bacterial infection but are typically strain specific and fail to mediate broad protection against different serotypes. Here we describe a panel of affinity-matured monoclonal human antibodies from peripheral blood immunoglobulin M–positive (IgM+) and IgA+ memory B cells and clonally related intestinal plasmablasts, directed against the lipopolysaccharide (LPS) O-antigen of Klebsiella pneumoniae, an opportunistic pathogen and major cause of antibiotic-resistant nosocomial infections. The antibodies showed distinct patterns of in vivo cross-specificity and protection against different clinically relevant K. pneumoniae serotypes. However, cross-specificity was not limited to K. pneumoniae, as K. pneumoniae–specific antibodies recognized diverse intestinal microbes and neutralized not only K. pneumoniae LPS but also non–K. pneumoniae LPS. Our data suggest that the recognition of minimal glycan epitopes abundantly expressed on microbial surfaces might serve as an efficient humoral immunological mechanism to control invading pathogens and the large diversity of the human microbiota with a limited set of cross-specific antibodies.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Julianelle, L. A. Immunological relationships of encapsulated and capsule-free strains of encapsulated pneumoniae (Friedlander’s Bacillus). J. Exp. Med. 44, 683–696 (1926).
Lancefield, R. C. A serological differentiation of human and other groups of hemolytic Streptococci. J. Exp. Med. 57, 571–595 (1933).
Shattock, P. M. F. The use of serology in the classification of micro-organisms. J. Gen. Microbiol. 12, 367–374 (1955).
Tillett, W. S., Avery, O. T. & Goebel, W. F. Chemo-immunological studies in conjugated carbohydrate-proteins: III. Active and passive anaphylaxis with synthetic sugar-proteins. J. Exp. Med. 50, 551–567 (1929).
Vinogradov, E. et al. Structures of lipopolysaccharides from Klebsiella pneumoniae. Eluicidation of the structure of the linkage region between core and polysaccharide O chain and identification of the residues at the non-reducing termini of the O chains. J. Biol. Chem. 277, 25070–25081 (2002).
Trautmann, M. et al. O-antigen seroepidemiology of Klebsiella clinical isolates and implications for immunoprophylaxis of Klebsiella infections. Clin. Diagn. Lab. Immunol. 4, 550–555 (1997).
Hansen, D. S. et al. Klebsiella pneumoniae lipopolysaccharide O typing: revision of prototype strains and O-group distribution among clinical isolates from different sources and countries. J. Clin. Microbiol. 37, 56–62 (1999).
Follador, R. et al. The diversity of Klebsiella pneumoniae surface polysaccharides. Microb. Genomics 2, e000073 (2016).
Podschun, R. & Ullmann, U. Klebsiella spp. as nosocomial pathogens: epidemiology, taxonomy, typing methods, and pathogenicity factors. Clin. Microbiol. Rev. 11, 589–603 (1998).
Kubinak, J. L. & Round, J. L. Do antibodies select a healthy microbiota? Nat. Rev. Immunol. 16, 767–774 (2016).
Mond, J. J., Lees, A. & Snapper, C. M. T. T cell-independent antigens type 2. Annu. Rev. Immunol. 13, 655–692 (1995).
Magri, G. et al. Human secretory IgM emerges from plasma cells clonally related to gut memory B cells and targets highly diverse commensals. Immunity 47, 118–134 (2017).
Bunker, J. J. et al. Natural polyreactive IgA antibodies coat the intestinal microbiota. Science 358, eaan6619 (2017).
Toellner, K.-M. et al. Low-level hypermutation in T cell-independent germinal centers compared with high mutation rates associated with T cell-dependent germinal centers. J. Exp. Med. 195, 383–389 (2002).
Whitfield, C., Richards, J. C., Perry, M. B., Clarke, B. R. & MacLean, L. L. Expression of two structurally distinct D-galactan O antigens in the lipopolysaccharide of Klebsiella pneumoniae serotype O1. J. Bacteriol. 173, 1420–1431 (1991).
Szijártó, V. et al. Both clades of the epidemic KPC-producing Klebsiella pneumoniae clone ST258 share a modified galactan O-antigen type. Int. J. Med. Microbiol. 306, 89–98 (2016).
Stojkovic, K. et al. Identification of d-galactan-III as part of the lipopolysaccharide of Klebsiella pneumoniae Serotype O1. Front. Microbiol. 8, 684 (2017).
Guachalla, L. M. et al. Discovery of monoclonal antibodies cross-reactive to novel subserotypes of K. pneumoniae O3. Sci. Rep. 7, 6635 (2017).
Park, B. S. et al. The structural basis of lipopolysaccharide recognition by the TLR4–MD-2 complex. Nature 458, 1191–1195 (2009).
Jansson, P.-E. et al. Structural studies of the O-antigen polysaccharides of Klebsiella O5 and Escherichia coli O8. Carbohydr. Res. 145, 59–66 (1985).
Lipke, P. N. & Ovalle, R. Cell wall architecture in yeast: new structure and new challenges. J. Bacteriol. 180, 3735–3740 (1998).
Doores, K. J. The HIV glycan shield as a target for broadly neutralizing antibodies. FEBS J. 282, 4679–4691 (2015).
Trama, A. M. et al. HIV-1 envelope gp41 antibodies can originate from terminal ileum B cells that share cross-reactivity with commensal bacteria. Cell Host Microbe 16, 215–226 (2014).
Bayhan, G. I., Senel, S., Tanir, G. & Ozkan, S. Bacteremia caused by Pseudomonas luteola in pediatric patients. Jpn. J. Infect. Dis. 68, 50–54 (2015).
Zhou, Z.-H. et al. The broad antibacterial activity of the natural antibody repertoire is due to polyreactive antibodies. Cell Host Microbe 1, 51–61 (2007).
Polonskaya, Z. et al. T cells control the generation of nanomolar-affinity anti-glycan antibodies. J. Clin. Invest. 127, 1491–1504 (2017).
Fagarasan, S., Kinoshita, K., Muramatsu, M., Ikuta, K. & Honjo, T. In situ class switching and differentiation to IgA-producing cells in the gut lamina propria. Nature 413, 639–643 (2001).
Lindner, C. et al. Diversification of memory B cells drives the continuous adaptation of secretory antibodies to gut microbiota. Nat. Immunol. 16, 880–888 (2015).
Bergqvist, P. et al. Re-utilization of germinal centers in multiple Peyer’s patches results in highly synchronized, oligoclonal, and affinity-matured gut IgA responses. Mucosal Immunol. 6, 122–135 (2013).
Di Niro, R. et al. Salmonella infection drives promiscuous B cell activation followed by extrafollicular affinity maturation. Immunity 43, 120–131 (2015).
Baumgarth, N., Tung, J. W. & Herzenberg, L. A. Inherent specificities in natural antibodies: a key to immune defense against pathogen invasion. Springer Semin. Immunopathol. 26, 347–362 (2005).
Landsverk, O. J. B. et al. Antibody-secreting plasma cells persist for decades in human intestine. J. Exp. Med. 214, 309–317 (2017).
Macpherson, A. J., Köller, Y. & McCoy, K. D. The bilateral responsiveness between intestinal microbes and IgA. Trends Immunol. 36, 460–470 (2015).
Coughlin, R. T. et al. Characterization of pneumococcal specific antibodies in healthy unvaccinated adults. Vaccine 16, 1761–1767 (1998).
Peterson, D. A., McNulty, N. P., Guruge, J. L. & Gordon, J. I. IgA response to symbiotic bacteria as a mediator of gut homeostasis. Cell Host Microbe 2, 328–339 (2007).
Tiller, T. et al. Autoreactivity in human IgG+ memory B cells. Immunity 26, 205–213 (2007).
Benckert, J. et al. The majority of intestinal IgA+ and IgG+ plasmablasts in the human gut are antigen-specific. J. Clin. Invest. 121, 1946–1955 (2011).
Tiller, T. et al. Efficient generation of monoclonal antibodies from single human B cells by single cell RT-PCR and expression vector cloning. J. Immunol. Methods 329, 112–124 (2008).
Murugan, R., Imkeller, K., Busse, C. E. & Wardemann, H. Direct high-throughput amplification and sequencing of immunoglobulin genes from single human B cells. Eur. J. Immunol. 45, 2698–2700 (2015).
Lorin, V. & Mouquet, H. Efficient generation of human IgA monoclonal antibodies. J. Immunol. Methods 422, 102–110 (2015).
Wardemann, H. et al. Predominant autoantibody production by early human B cell precursors. Science 301, 1374–1377 (2003).
Szijártó, V. et al. Bactericidal monoclonal antibodies specific to the lipopolysaccharide O antigen from multidrug-resistant Escherichia coli clone ST131-O25b:H4 elicit protection in mice. Antimicrob. Agents Chemother. 59, 3109–3116 (2015).
Cerca, N. et al. Protection against Escherichia coli infection by antibody to the Staphylococcus aureus poly-N-acetylglucosamine surface polysaccharide. Proc. Natl Acad. Sci. USA 104, 7528–7533 (2007).
Szijártó, V. et al. Endotoxin neutralization by an O-antigen specific monoclonal antibody: A potential novel therapeutic approach against Klebsiella pneumoniae ST258. Virulence 8, 1203–1215 (2017).
Masella, A. P., Bartram, A. K., Truszkowski, J. M., Brown, D. G. & Neufeld, J. D. PANDAseq: paired-end assembler for illumina sequences. BMC Bioinformatics 13, 31 (2012).
Caporaso, J. G. et al. QIIME allows analysis of high-throughput community sequencing data. Nat. Methods 7, 335–336 (2010).
R Development Core Team. R: A Language and Environment for Statistical Computing (R Foundation for Statistical Computing, Vienna, 2008).
Imkeller, K., Arndt, P. F., Wardemann, H. & Busse, C. E. sciReptor: analysis of single-cell level immunoglobulin repertoires. BMC Bioinformatics 17, 67 (2016).
Warnes, G. R. et al. Various R programming tools for plotting data. R package version 2, 1 (2009).
Wickham, H. ggplot2: Elegant Graphics for Data Analysis. (Springer-Verlag, New York, 2009).
Gu, Z., Gu, L., Eils, R., Schlesner, M. & Brors, B. circlize Implements and enhances circular visualization in R. Bioinformatics 30, 2811–2812 (2014).
Acknowledgements
We thank S. Kaluzewski (National Institute of Public Health–National Institute of Hygiene) for an unencapsulated mutant of a prototype O3:K55 strain 5505; S. Melegh (University of Pécs) for clinical isolates Kp2 (O3:K60) and Kp14 (O3:K35); A. Valverde (University Hospital Ramón y Cajal) for clinical isolate Kp81 (O3b:K non-typeable); A. Heidtmann, L. Kummer, B. Jocher and J. Braun for help with sample acquisition; C. Varga for performing animal experiments; C. Busse for help with experimental design; M. Nussenzweig (The Rockefeller University) for recombinant gp140 from strain YU2; and P. Sehr, R. Murugan, P. Thiele, C. Winter, D. Foster, A. Götze and the DKFZ High-Throughput Sequencing Unit of the Genomics and Proteomics Core Facility and the DKFZ and MPIIB Flow Cytometry Core Facilities for technical support. Supported by the European Funding Program Eurostars (E! 7563 – KLEBSICURE), powered by EUREKA and the European Community; the German Federal Ministry of Education and Research (H.W.); and the International Max Planck Research School for Infectious Diseases and Immunology (T.R.).
Author information
Authors and Affiliations
Contributions
T.R., V.S., J.L. and H.W. designed experiments and analyzed data; T.R., V.S., L.M.G., K.S., K. Hartl, L.S. and S. Kocher performed experiments; F.L., M.A.-S., J.S.-B., M.v.F., G.G. and P.H. identified patients and provided samples. S. Klein and K. Heeg provided experimental support; V.S., E.N., G.N. and H.W. conceived of the study; T.R. and H.W. wrote the manuscript; V.S., J.L., E.N. and G.N. edited the manuscript; and all authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
E.N., G.N., L.M.G., K. Hartl, L.S., V.S., T.R. and H.W. have filed patent applications on human antibodies to K. pneumoniae O-antigen; and E.N., G.N., L.M.G., K. Hartl, L.S. and V.S. are employees of Arsanis Biosciences and hold shares in Arsanis, the parent company of Arsanis Biosciences.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 Identification of O3-reactive B cells using biotinylated O3 O-antigen.
a, Schematic linear structure of biotinylated O3 K. pneumoniae O-antigen; repeating unit (outlined), MeP = Methylphosphate; Man = Mannose; KdO = 3-Deoxy-D-manno-oct-2-ulosonic acid; GlcNAc = N-acetylglucosamine; Hep = L-glycero-D-manno-heptose; PEG = Polyethylene glycol. b, Percentage of O3-reactive 7-AAD−, CD19+, CD27+ peripheral blood B cells in eight donors compared to the background staining using non-biotinylated O3 (right). p-value was calculated using two-tailed Student’s t-test. Data are representative of at least two independent experiments.
Supplementary Figure 2 Immunoglobulin gene characteristics of O3-reactive PB and LP B cells.
a, IGH gene isotype distribution for O3-reactive PB memory B cells isolated by flow cytometric single cell sorting. b,c, IGHV gene family usage for O3-reactive PB memory B cells of the indicated isotypes from the same donors as shown in panel a (b) and LP plasmablasts isolated by flow cytometric single cell sorting from the indicated donors (c). d, Percentage of mutated and unmutated IGHV genes from O3-reactive PB memory B cells of the same donors as in panel a. e, Distribution of cell clusters of clonally related (gray boxes) compared to unique non-related (white) O3-reactive B cells in PB memory B cells or LP plasmablasts from the indicated donors. f, Clonal relationship of O3-reactive B cells of the indicated isotypes in PB memory B cells and LP plasmablasts of donors HD02, HD05, and HD10. Colors depict individual B cell clusters. n indicates numbers of analyzed sequences.
Supplementary Figure 3 O3-reactive PB memory B cell and LP plasmablast antibodies bind specifically to O3 O-antigen.
a, Immunoblot with whole O3 LPS for representative mAbs cloned from O3-reactive memory B cells from PB (036, 286) and from LP plasmablasts (601). b, O3 and streptavidin reactivity of individual recombinant mAbs from O3-reactive PB memory B cells (n = 41) and LP plasmablasts (n = 41) based on ELISA area under curve (AUC) measurements. c, Insulin ELISA reactivity of O3-reactive PB memory B cell antibodies (n = 41) under blocking conditions with 2% BSA. d, Polyreactivity ELISA with E. coli LPS, dsDNA and insulin under non-blocking conditions without BSA. Representative mAbs compared to the positive and negative control mAbs are shown. Dashed lines in indicate negative thresholds (b-d). Data are representative data of at least two independent experiments (a-d).
Supplementary Figure 4 Germline reversion of mutated O3-reactive antibodies.
Gene sequence alignment of IGH and IGK or IGL variable regions of the indicated mutated mAbs and their inferred germline counterpart compared to the respective germline V and J gene segments. CDRs are highlighted.
Supplementary Figure 5 O5-specific mAb 703.
a, mAb 703 shows specificity for O5 in immunoblot with whole LPS. b, Reactivity of mAb 703 with intestinal murine microbes as measured by flow cytometry. Sorting gate and percentage of antibody-bound bacteria is indicated. Boxes show the K. pneumoniae O-serotype, S. cerevisiae, and gp140 reactivity profile (strong-black; non-reactive-white). Data are representative of two independent experiments.
Supplementary Figure 6 Immunoglobulin gene features and antibody characteristics of O1-reactive PB B cells.
a, Schematic linear structure of biotinylated O1; repeating units (outlined); Gal = Galactose; KdO = 3-Deoxy-D-manno-oct-2-ulosonic acid; GlcNAc = N-acetylglucosamine; Hep = L-glycero-D-manno-heptose; PEG = Polyethylene glycol. b, Flow cytometric analysis of the frequency of 7-AAD−, CD19+ PB B cells reactive to biotinylated O1 (right) compared to the negative control using non-biotinylated O1 (left) for a representative healthy donor detected by Streptavidin Alexa647 conjugate. Gates and percentages indicate the frequency of O1-reactive cells. c, Percentage of O1-reactive 7-AAD−, CD19+ PB B cells (left) in eight donors compared to the background staining using non-biotinylated O1 (right). p-value was calculated using two-tailed Student’s t-test. d, IGH gene isotype usage for O1-reactive PB memory B cells from the same donors as in panel c. Means (red lines) and SD (black lines) are indicated. e, IGHV gene family usage for O1-reactive PB memory B cells of the indicated isotypes from the same donors as shown in panel d. n represents the number of analyzed IGH sequences per isotype. f, Percent of clonally-related O1-reactive B cells per sample in PB memory B cells of the same donors as in panel d. Means (red lines) and SD (black lines) are indicated. g, Number of somatic hypermutations in IGHV genes of the indicated isotypes from O1-reactive peripheral blood B cells. Data are pooled from the same eight donors as in panel d. Means (red lines) and SD (black lines) are indicated. n represents the number of analyzed IGH sequences per isotype. h, Percentage of mutated and unmutated IGHV genes from O1-reactive PB memory B cells. i, O1-reactivity of mAbs cloned from O1-reactive PB memory B cells as measured by ELISA. Green lines indicate the negative isotype control mAb and red lines the threshold for positivity. n indicates the number of tested mAbs. j, Immunoblot reactivity with O1, O2, and O3 LPS for a representative O1-reactive (anti-galactan II) mAb; + and - indicate serotypes expressing the galactan III or the galactan I variant, respectively. k, O1 and streptavidin reactivity of individual mAbs from O1-reactive PB memory B cells based on ELISA area under curve (AUC) measurements. l, IGHV gene somatic hypermutation counts for ELISA O1-specific mAbs (i, k) of the indicated isotypes (IGHM, n = 3; IGHA, n = 3). Red lines indicate means. m, Anti-O1 ELISA reactivity of the indicated mAb (top) and its predicted germline form (bottom). Green lines indicate reactivity of the negative isotype control mAb. Red lines indicate negative thresholds. n, Reactivity of the O1-reactive mAb 196 with murine intestinal microbes as measured by flow cytometry (Fig. 6a). Sorting gate and percentage of antibody-bound bacteria is indicated. Boxes show the K. pneumoniae O-serotype, S. cerevisiae, and gp140 reactivity profile (non-reactive-white). Red diagonal lines indicate non-tested. Data are representative of at least two independent experiments (b, c, i – k, m, n).
Supplementary Figure 7 Cross-specificity of individual K. pneumoniae O-antigen reactive antibodies with microbes from human intestine.
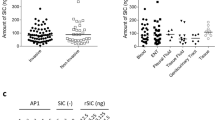
a,b, Reactivity of the indicated mAbs with intestinal microbes of 31/41 tested human stool samples (a) and from a single individual as measured by flow cytometry compared to the PBS negative control (b). Sorting gate and percentage of antibody-bound bacteria are indicated. The K. pneumoniae O-serotype, S. cerevisiae, and gp140 reactivity profiles of each antibody are shown. Data are representative of two independent experiments (b).
Supplementary information
Supplementary Figures and Supplementary Text
Supplementary Figures 1–8 and Supplementary Tables 1-3
Rights and permissions
About this article
Cite this article
Rollenske, T., Szijarto, V., Lukasiewicz, J. et al. Cross-specificity of protective human antibodies against Klebsiella pneumoniae LPS O-antigen. Nat Immunol 19, 617–624 (2018). https://doi.org/10.1038/s41590-018-0106-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41590-018-0106-2
This article is cited by
-
Carbapenem-resistant Klebsiella pneumoniae capsular types, antibiotic resistance and virulence factors in China: a longitudinal, multi-centre study
Nature Microbiology (2024)
-
Tango of B cells with T cells in the making of secretory antibodies to gut bacteria
Nature Reviews Gastroenterology & Hepatology (2023)
-
Colistin resistance mutations in phoQ can sensitize Klebsiella pneumoniae to IgM-mediated complement killing
Scientific Reports (2023)
-
Long-distance relationships - regulation of systemic host defense against infections by the gut microbiota
Mucosal Immunology (2022)
-
Anti-bacterial monoclonal antibodies: next generation therapy against superbugs
Applied Microbiology and Biotechnology (2022)