Abstract
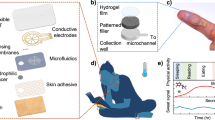
Wearable sweat sensors have the potential to provide continuous measurements of useful biomarkers. However, current sensors cannot accurately detect low analyte concentrations, lack multimodal sensing or are difficult to fabricate at large scale. We report an entirely laser-engraved sensor for simultaneous sweat sampling, chemical sensing and vital-sign monitoring. We demonstrate continuous detection of temperature, respiration rate and low concentrations of uric acid and tyrosine, analytes associated with diseases such as gout and metabolic disorders. We test the performance of the device in both physically trained and untrained subjects under exercise and after a protein-rich diet. We also evaluate its utility for gout monitoring in patients and healthy controls through a purine-rich meal challenge. Levels of uric acid in sweat were higher in patients with gout than in healthy individuals, and a similar trend was observed in serum.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The data that support the plots within this paper and other findings of this study are available from the corresponding author upon request.
Code availability
The custom code used to program microcontroller is available from the corresponding author upon request.
References
Wang, T. J. et al. Metabolite profiles and the risk of developing diabetes. Nat. Med. 17, 448–453 (2011).
Suhre, K. et al. Human metabolic individuality in biomedical and pharmaceutical research. Nature 477, 54–60 (2011).
Illig, T. et al. A genome-wide perspective of genetic variation in human metabolism. Nat. Genet. 42, 137–141 (2010).
Wu, G. Amino acids: metabolism, functions, and nutrition. Amino Acids 37, 1–17 (2009).
Kim, D. H. et al. Epidermal electronics. Science 333, 838–843 (2011).
Someya, T., Bao, Z. & Malliaras, G. G. The rise of plastic bioelectronics. Nature 540, 379–385 (2016).
Kim, J., Campbell, A. S., de Avila, B. E. & Wang, J. Wearable biosensors for healthcare monitoring. Nat. Biotechnol. 37, 389–406 (2019).
Heikenfeld, J. et al. Wearable sensors: modalities, challenges, and prospects. Lab Chip 18, 217–248 (2018).
Park, S. et al. Self-powered ultra-flexible electronics via nano-grating-patterned organic photovoltaics. Nature 561, 516–521 (2018).
Son, D. et al. An integrated self-healable electronic skin system fabricated via dynamic reconstruction of a nanostructured conducting network. Nat. Nanotechnol. 13, 1057–1065 (2018).
Wang, C. et al. Monitoring of the central blood pressure waveform via a conformal ultrasonic device. Nat. Biomed. Eng. 2, 687–695 (2018).
Hua, Q. et al. Skin-inspired highly stretchable and conformable matrix networks for multifunctional sensing. Nat. Commun. 9, 244 (2018).
Wang, C. et al. User-interactive electronic skin for instantaneous pressure visualization. Nat. Mater. 12, 899–904 (2013).
Yang, Y. & Gao, W. Wearable and flexible electronics for continuous molecular monitoring. Chem. Soc. Rev. 48, 1465–1491 (2019).
Gao, W. et al. Fully integrated wearable sensor arrays for multiplexed in situ perspiration analysis. Nature 529, 509–514 (2016).
Lee, H. et al. A graphene-based electrochemical device with thermoresponsive microneedles for diabetes monitoring and therapy. Nat. Nanotechnol. 11, 566–572 (2016).
Koh, A. et al. A soft, wearable microfluidic device for the capture, storage, and colorimetric sensing of sweat. Sci. Transl. Med. 8, 366ra165 (2016).
Bariya, M., Nyein, H. Y. Y. & Javey, A. Wearable sweat sensors. Nat. Electron. 1, 160–171 (2018).
Choi, J., Ghaffari, R., Baker, L. B. & Rogers, J. A. Skin-interfaced systems for sweat collection and analytics. Sci. Adv. 4, eaar3921 (2018).
Emaminejad, S. et al. Autonomous sweat extraction and analysis applied to cystic fibrosis and glucose monitoring using a fully integrated wearable platform. Proc. Natl Acad. Sci. USA 114, 4625–4630 (2017).
Bandodkar, A. J. et al. Battery-free, skin-interfaced microfluidic/electronic systems for simultaneous electrochemical, colorimetric, and volumetric analysis of sweat. Sci. Adv. 5, eaav3294 (2019).
Nakata, S. et al. A wearable pH sensor with high sensitivity based on a flexible charge-coupled device. Nat. Electron. 1, 596–603 (2018).
Heikenfeld, J. et al. Accessing analytes in biofluids for peripheral biochemical monitoring. Nat. Biotechnol. 37, 407–419 (2019).
Lee, H. et al. Wearable/disposable sweat-based glucose monitoring device with multistage transdermal drug delivery module. Sci. Adv. 3, e1601314 (2017).
Jia, W. et al. Electrochemical tattoo biosensors for real-time noninvasive lactate monitoring in human perspiration. Anal. Chem. 85, 6553–6560 (2013).
Feig, D. I., Kang, D. H. & Johnson, R. J. Uric acid and cardiovascular risk. N. Engl. J. Med. 359, 1811–1821 (2008).
Gagliardi, A. C., Miname, M. H. & Santos, R. D. Uric acid: A marker of increased cardiovascular risk. Atherosclerosis 202, 11–17 (2009).
Bhole, V., Choi, J. W., Kim, S. W., de Vera, M. & Choi, H. Serum uric acid levels and the risk of type 2 diabetes: a prospective study. Am. J. Med. 123, 957–961 (2010).
Kodama, S. et al. Association between serum uric acid and development of type 2 diabetes. Diabetes Care 32, 1737–1742 (2009).
Kohagura, K. et al. An association between uric acid levels and renal arteriolopathy in chronic kidney disease: a biopsy-based study. Hypertens. Res. 36, 43–49 (2013).
Terkeltaub, R. Update on gout: new therapeutic strategies and options. Nat. Rev. Rheumatol. 6, 30–38 (2010).
Major, T. J., Dalbeth, N., Stahl, E. A. & Merriman, T. R. An update on the genetics of hyperuricaemia and gout. Nat. Rev. Rheumatol. 14, 341–353 (2018).
Terkeltaub, R. A. Clinical practice. Gout. N. Engl. J. Med. 349, 1647–1655 (2003).
Smith, E. et al. The global burden of gout: estimates from the Global Burden of Disease 2010 study. Ann. Rheum. Dis. 73, 1470–1476 (2014).
Fernstrom, J. D. & Fernstrom, M. H. Tyrosine, phenylalanine, and catecholamine synthesis and function in the brain. J. Nutr. 137, 1539S–1547S (2007).
Russo, P. A., Mitchell, G. A. & Tanguay, R. M. Tyrosinemia: a review. Pediatr. Dev. Pathol. 4, 212–221 (2001).
Levine, R. J. & Conn, H. O. Tyrosine metabolism in patients with liver disease. J. Clin. Invest. 46, 2012–2020 (1967).
D’Andrea, G. et al. Study of tyrosine metabolism in eating disorders. Possible correlation with migraine. Neurol. Sci. 29, S88–S92 (2008).
Capuron, L. et al. Chronic low-grade inflammation in elderly persons is associated with altered tryptophan and tyrosine metabolism: role in neuropsychiatric symptoms. Biol. Psychiatry 70, 175–182 (2011).
Itoh, S. & Nakayama, T. Amino acids in human sweat. Jpn. J. Physiol. 2, 248–253 (1952).
Liappis, N., Kelderbacher, S. D., Kesseler, K. & Bantzer, P. Quantitative study of free amino acids in human eccrine sweat excreted from the forearms of healthy trained and untrained men during exercise. Eur. J. Appl. Physiol. Occup. Physiol. 42, 227–234 (1979).
Reeder, J. T. et al. Waterproof, electronics-enabled, epidermal microfluidic devices for sweat collection, biomarker analysis, and thermography in aquatic settings. Sci. Adv. 5, eaau6356 (2019).
Nyein, H. Y. Y. et al. A wearable microfluidic sensing patch for dynamic sweat secretion analysis. ACS Sens. 3, 944–952 (2018).
Imani, S. et al. A wearable chemical–electrophysiological hybrid biosensing system for real-time health and fitness monitoring. Nat. Commun. 7, 11650 (2016).
Ye, R., James, D. K. & Tour, J. M. Laser-induced graphene. Acc. Chem. Res. 51, 1609–1620 (2018).
Lin, J. et al. Laser-induced porous graphene films from commercial polymers. Nat. Commun. 5, 5714 (2014).
Li, G., Mo, X., Law, W.-C. & Chan, K. C. Wearable fluid capture devices for electrochemical sensing of sweat. ACS Appl. Mater. Interfaces 11, 238–243 (2018).
Harvey, C. J., LeBouf, R. F. & Stefaniak, A. B. Formulation and stability of a novel artificial human sweat under conditions of storage and use. Toxicol. In Vitro 24, 1790–1796 (2010).
Shao, Q., Liu, G., Teweldebrhan, D. & Balandin, A. A. High-temperature quenching of electrical resistance in graphene interconnects. Appl. Phys. Lett. 92, 202108 (2008).
Snakenborg, D., Klank, H. & Kutter, J. P. Microstructure fabrication with a CO2 laser system. J. Micromech. Microeng. 14, 182–189 (2004).
Acknowledgements
This work was supported by a California Institute of Technology Startup grant, the Rothenberg Innovation Initiative (RI2) program, the Carver Mead New Adventures Fund and an American Heart Association grant 19TPA34850157 (all to W.G.). Y.S., X.B. and M.W. acknowledge the China Scholarship Council (CSC) for financial support. J.T. was supported by the National Science Scholarship (NSS) from the Agency of Science Technology and Research (A*STAR) Singapore. We gratefully acknowledge critical support and infrastructure provided for this work by the Kavli Nanoscience Institute and Jim Hall Design and Prototyping Lab at Caltech, and we gratefully thank M. Hunt and B. Dominguez for their help. This project benefited from the use of instrumentation made available by the Caltech Environmental Analysis Center and we gratefully acknowledge guidance from N. Dalleska. We also thank Z. Wang for valuable inputs in patch pattern design.
Author information
Authors and Affiliations
Contributions
W.G. and Y.Y. initiated the concept. W.G., Y.Y., Y.S., X.B., T.K.H. and Z.L. designed the experiments; Y.Y., Y.S., X.B. and J.M. led the experiments and collected the overall data; O.S.P., L.Z. and Y.Y. performed the flow simulation and modeling; J.M. performed the circuit design and test; M.W., J.T. and A.K. contributed to sensor characterization and validation; W.G., Y.Y., Y.S., X.B., J.M., O.S.P., L.Z. and H.Z. contributed the data analysis and co-wrote the paper. All authors provided the feedback on the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Figs. 1–41, Supplementary Tables 1–4 and Supplementary Note 1.
Rights and permissions
About this article
Cite this article
Yang, Y., Song, Y., Bo, X. et al. A laser-engraved wearable sensor for sensitive detection of uric acid and tyrosine in sweat. Nat Biotechnol 38, 217–224 (2020). https://doi.org/10.1038/s41587-019-0321-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41587-019-0321-x
This article is cited by
-
Interindividual- and blood-correlated sweat phenylalanine multimodal analytical biochips for tracking exercise metabolism
Nature Communications (2024)
-
Digitally-defined ultrathin transparent wireless sensor network for room-scale imperceptible ambient intelligence
npj Flexible Electronics (2024)
-
Interstitial fluid-based wearable biosensors for minimally invasive healthcare and biomedical applications
Communications Materials (2024)
-
A wearable aptamer nanobiosensor for non-invasive female hormone monitoring
Nature Nanotechnology (2024)
-
Well-defined in-textile photolithography towards permeable textile electronics
Nature Communications (2024)