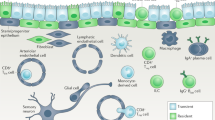
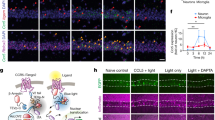
Abstract
Our body has a remarkable ability to remember its past encounters with allergens, pathogens, wounds and irritants, and to react more quickly to the next experience. This accentuated sensitivity also helps us to cope with new threats. Despite maintaining a state of readiness and broadened resistance to subsequent pathogens, memories can also be maladaptive, leading to chronic inflammatory disorders and cancers. With the ever-increasing emergence of new pathogens, allergens and pollutants in our world, the urgency to unravel the molecular underpinnings of these phenomena has risen to new heights. Here we reflect on how the field of inflammatory memory has evolved, since 2007, when researchers realized that non-specific memory is contained in the nucleus and propagated at the epigenetic level. We review the flurry of recent discoveries revealing that memory is not just a privilege of the immune system but also extends to epithelia of the skin, lung, intestine and pancreas, and to neurons. Although still unfolding, epigenetic memories of inflammation have now been linked to possible brain disorders such as Alzheimer disease, and to an elevated risk of cancer. In this Review, we consider the consequences—good and bad—of these epigenetic memories and their implications for human health and disease.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Durrant, W. E. & Dong, X. Systemic acquired resistance. Annu. Rev. Phytopathol. 42, 185–209 (2004).
Pasco, S. T. & Anguita, J. Lessons from Bacillus Calmette–Guerin: harnessing trained immunity for vaccine development. Cells 9, 2109 (2020).
Beeson, P. B. & Technical Assistance of Elizabeth Roberts. Tolerance to bacterial pyrogens: I. Factors influencing its development. J. Exp. Med. 86, 29–38 (1947).
West, M. A. & Heagy, W. Endotoxin tolerance: a review. Crit. Care Med. 30, S64–S73 (2002).
Ekamper, P., van Poppel, F., Stein, A. D. & Lumey, L. H. Independent and additive association of prenatal famine exposure and intermediary life conditions with adult mortality between age 18–63 years. Soc. Sci. Med. 119, 232–239 (2014).
Farber, D. L., Netea, M. G., Radbruch, A., Rajewsky, K. & Zinkernagel, R. M. Immunological memory: lessons from the past and a look to the future. Nat. Rev. Immunol. 16, 124–128 (2016).
Muecksch, F. et al. Increased potency and breadth of SARS-CoV-2 neutralizing antibodies after a third mRNA vaccine dose. Preprint at bioRxiv https://doi.org/10.1101/2022.02.14.480394 (2022).
Laidlaw, B. J. & Ellebedy, A. H. The germinal centre B cell response to SARS-CoV-2. Nat. Rev. Immunol. 22, 7–18 (2022).
Pulendran, B. & Davis, M. M. The science and medicine of human immunology. Science 369, eaay4014 (2020).
Cho, A. et al. Anti-SARS-CoV-2 receptor-binding domain antibody evolution after mRNA vaccination. Nature 600, 517–522 (2021).
Naik, S. et al. Inflammatory memory sensitizes skin epithelial stem cells to tissue damage. Nature 550, 475–480 (2017). This study is the first to report that inflammatory memory is not a property unique to immune cells and is also found in skin epithelial stem cells.
Foster, S. L., Hargreaves, D. C. & Medzhitov, R. Gene-specific control of inflammation by TLR-induced chromatin modifications. Nature 447, 972–978 (2007). This landmark study traces the roots of inflammatory memory and tolerence in marcophages to epigenetic changes in chromatin.
Sun, J. C., Beilke, J. N. & Lanier, L. L. Adaptive immune features of natural killer cells. Nature 457, 557–561 (2009).
Netea, M. G., Quintin, J. & van der Meer, J. W. Trained immunity: a memory for innate host defense. Cell Host Microbe 9, 355–361 (2011).
Ordovas-Montanes, J. et al. Allergic inflammatory memory in human respiratory epithelial progenitor cells. Nature 560, 649–654 (2018).
Christ, A. et al. Western diet triggers NLRP3-dependent innate immune reprogramming. Cell 172, 162–175.e14 (2018).
Kaufmann, E. et al. BCG educates hematopoietic stem cells to generate protective innate immunity against tuberculosis. Cell 172, 176–190.e19 (2018).
Lim, A. I. et al. Prenatal maternal infection promotes tissue-specific immunity and inflammation in offspring. Science 373, eabf3002 (2021). This study identifies intergenerational memory in intestinal offspring epithelial stem cells following in utero esposure to inflammatory mediators.
Wendeln, A. C. et al. Innate immune memory in the brain shapes neurological disease hallmarks. Nature 556, 332–338 (2018). This study identifies a role for innate immune memory in brain-resident microglia in exacerbating Alzheimer disease.
Divangahi, M. et al. Trained immunity, tolerance, priming and differentiation: distinct immunological processes. Nat. Immunol. 22, 2–6 (2021).
Saeed, S. et al. Epigenetic programming of monocyte-to-macrophage differentiation and trained innate immunity. Science 345, 1251086 (2014).
Chen, F. et al. Neutrophils prime a long-lived effector macrophage phenotype that mediates accelerated helminth expulsion. Nat. Immunol. 15, 938–946 (2014).
Freyne, B. et al. Neonatal BCG vaccination reduces interferon-gamma responsiveness to heterologous pathogens in infants from a randomized controlled trial. J. Infect. Dis. 221, 1999–2009 (2020).
Yao, Y. et al. Induction of autonomous memory alveolar macrophages requires T cell help and is critical to trained immunity. Cell 175, 1634–1650.e17 (2018).
Serafini, N. et al. Trained ILC3 responses promote intestinal defense. Science 375, 859–863 (2022).
Mitroulis, I. et al. Modulation of myelopoiesis progenitors is an integral component of trained immunity. Cell 172, 147–161.e12 (2018).
Cirovic, B. et al. BCG vaccination in humans elicits trained immunity via the hematopoietic progenitor compartment. Cell Host Microbe 28, 322–334.e5 (2020).
Moore, R. S., Kaletsky, R. & Murphy, C. T. Piwi/PRG-1 argonaute and TGF-beta mediate transgenerational learned pathogenic avoidance. Cell 177, 1827–1841.e12 (2019).
Klosin, A., Casas, E., Hidalgo-Carcedo, C., Vavouri, T. & Lehner, B. Transgenerational transmission of environmental information in C. elegans. Science 356, 316–319 (2017).
Katzmarski, N. et al. Transmission of trained immunity and heterologous resistance to infections across generations. Nat. Immunol. 22, 1382–1390 (2021).
Kaufmann, E. et al. Lack of evidence for intergenerational inheritance of immune resistance to infections. Nat. Immunol. 23, 203–207 (2022).
Xing, Y. & Naik, S. Under pressure: stem cell–niche interactions coordinate tissue adaptation to inflammation. Curr. Opin. Cell Biol. 67, 64–70 (2020).
Biton, M. et al. T helper cell cytokines modulate intestinal stem cell renewal and differentiation. Cell 175, 1307–1320.e22 (2018).
Gonzales, K. A. U. et al. Stem cells expand potency and alter tissue fitness by accumulating diverse epigenetic memories. Science 374, eabh2444 (2021).
Del Poggetto, E. et al. Epithelial memory of inflammation limits tissue damage while promoting pancreatic tumorigenesis. Science 373, eabj0486 (2021).
Niec, R. E., Rudensky, A. Y. & Fuchs, E. Inflammatory adaptation in barrier tissues. Cell 184, 3361–3375 (2021).
Rodgers, J. T. et al. mTORC1 controls the adaptive transition of quiescent stem cells from G0 to GAlert. Nature 510, 393–396 (2014).
Lau, C. M. et al. Epigenetic control of innate and adaptive immune memory. Nat. Immunol. 19, 963–972 (2018).
Fanucchi, S. et al. Immune genes are primed for robust transcription by proximal long noncoding RNAs located in nuclear compartments. Nat. Genet. 51, 138–150 (2019).
Henikoff, S. & Shilatifard, A. Histone modification: cause or cog? Trends Genet. 27, 389–396 (2011).
Zaret, K. S. Pioneer transcription factors initiating gene network changes. Annu. Rev. Genet. 54, 367–385 (2020).
de Laval, B. et al. C/EBPβ-dependent epigenetic memory induces trained immunity in hematopoietic stem cells. Cell Stem Cell 26, 657–674.e8 (2020).
Larsen, S. B. et al. Establishment, maintenance, and recall of inflammatory memory. Cell Stem Cell 28, 1758–1774.e8 (2021). This study defines the transcription factor-depedent mechanisms underlying persistent chromatin modifications that mediate memory in epithelial stem cells.
Lowes, M. A., Bowcock, A. M. & Krueger, J. G. Pathogenesis and therapy of psoriasis. Nature 445, 866–873 (2007).
Suarez-Farinas, M., Fuentes-Duculan, J., Lowes, M. A. & Krueger, J. G. Resolved psoriasis lesions retain expression of a subset of disease-related genes. J. Invest. Dermatol. 131, 391–400 (2011).
Wang, Y. et al. Long-term culture captures injury-repair cycles of colonic stem cells. Cell 179, 1144–1159.e15 (2019).
Rees, W. D. et al. An in vitro chronic damage model impairs inflammatory and regenerative responses in human colonoid monolayers. Cell Rep. 38, 110283 (2022).
Bryant, D. M. et al. Identification of regenerative roadblocks via repeat deployment of limb regeneration in axolotls. NPJ Regen. Med. 2, 30 (2017).
Maekawa, T. et al. ATF7 mediates TNF-alpha-induced telomere shortening. Nucleic Acids Res. 46, 4487–4504 (2018).
Zhang, W., Qu, J., Liu, G. H. & Belmonte, J. C. I. The ageing epigenome and its rejuvenation. Nat. Rev. Mol. Cell Biol. 21, 137–150 (2020).
Jin-Gyu Cheong, A. R. et al. Epigenetic memory of COVID-19 in innate immune cells and their progenitors. Preprint at bioRxiv https://doi.org/10.1101/2022.02.09.479588 (2022).
Li, X. et al. Maladaptive innate immune training of myelopoiesis links inflammatory comorbidities. Cell 185, 1709–1727.e18 (2022).
Dvorak, H. F. Tumors: wounds that do not heal. Similarities between tumor stroma generation and wound healing. N. Engl. J. Med. 315, 1650–1659 (1986).
Schafer, M. & Werner, S. Cancer as an overhealing wound: an old hypothesis revisited. Nat. Rev. Mol. Cell Bio. 9, 628–638 (2008).
Martins-Green, M., Boudreau, N. & Bissell, M. J. Inflammation is responsible for the development of wound-induced tumors in chickens infected with Rous sarcoma virus. Cancer Res. 54, 4334–4341 (1994).
Sundaram, G. M., Quah, S. & Sampath, P. Cancer: the dark side of wound healing. FEBS J. 285, 4516–4534 (2018).
Guasch, G. et al. Loss of TGFβ signaling destabilizes homeostasis and promotes squamous cell carcinomas in stratified epithelia. Cancer Cell 12, 313–327 (2007).
Alonso-Curbelo, D. et al. A gene–environment-induced epigenetic program initiates tumorigenesis. Nature 590, 642–648 (2021).
Koelwyn, G. J. et al. Myocardial infarction accelerates breast cancer via innate immune reprogramming. Nat. Med. 26, 1452–1458 (2020).
Falvo, D. J. et al. A lineage-specific epigenetic memory of inflammation potentiates Kras-driven pancreatic tumorigenesis. Preprint at bioRxiv https://doi.org/10.1101/2021.11.01.466807 (2021).
Geller, A. E. et al. The induction of peripheral trained immunity in the pancreas incites anti-tumor activity to control pancreatic cancer progression. Nat. Commun. 13, 759 (2022).
Pascual, G. et al. Dietary palmitic acid promotes a prometastatic memory via Schwann cells. Nature 599, 485–490 (2021).
Rozenblatt-Rosen, O., Stubbington, M. J. T., Regev, A. & Teichmann, S. A. The Human Cell Atlas: from vision to reality. Nature 550, 451–453 (2017).
Kim, S. et al. Maternal gut bacteria promote neurodevelopmental abnormalities in mouse offspring. Nature 549, 528–532 (2017).
Choi, G. B. et al. The maternal interleukin-17a pathway in mice promotes autism-like phenotypes in offspring. Science 351, 933–939 (2016).
Vuong, H. E. et al. The maternal microbiome modulates fetal neurodevelopment in mice. Nature 586, 281–286 (2020).
Thion, M. S. et al. Microbiome influences prenatal and adult microglia in a sex-specific manner. Cell 172, 500–516.e16 (2018).
Koren, T. et al. Insular cortex neurons encode and retrieve specific immune responses. Cell 184, 5902–5915.e17 (2021).
Chen, W. T. et al. Spatial transcriptomics and in situ sequencing to study Alzheimer's disease. Cell 182, 976–991.e19 (2020).
Acknowledgements
We thank our many friends and colleagues who have made this field such an exciting and important one; A. Gola, M. Parigi, S. Larsen, C. Cowley, R. Niec, S. Sajjath, D. Rosenblum, P. Konieczny and L. Gueinin-Mace for their helpful comments on our manuscript. Illustrations were generated using Biorender. E.F. is an HHMI Investigator funded by grants from the US National Institutes of Health (R01-AR27883, R01-AR31737 and R01-AR050452). S.N. is a NYSCF Robertson Stem Cell Investigator and is funded by grants from the US National Institutes of Health (1DP2AR079173-01 and R01-AI168462), the Pew Foundation (00034119) and the Packard Foundation.
Author information
Authors and Affiliations
Contributions
S.N and E.F. conceptualized and compiled the manuscript and illustrations.
Corresponding authors
Ethics declarations
Competing interests
S.N. is on the scientific advisory board of Seed Inc., is a consultant for BiomX and receives research funding from Takeda Pharmaceuticals. E.F. has recently served on the scientific advisory boards of L’Oreal and Arsenal Biosciences, and owns stock options for Arsenal Biosciences.
Peer review
Peer review information
Nature thanks Cedric Balnpain, Xing Dai and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Naik, S., Fuchs, E. Inflammatory memory and tissue adaptation in sickness and in health. Nature 607, 249–255 (2022). https://doi.org/10.1038/s41586-022-04919-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-022-04919-3
This article is cited by
-
Bridging tissue repair and epithelial carcinogenesis: epigenetic memory and field cancerization
Cell Death & Differentiation (2024)
-
The enduring neutrophil–stroma dance of multiple myeloma
Nature Immunology (2024)
-
Cellular and molecular mechanisms of skin wound healing
Nature Reviews Molecular Cell Biology (2024)
-
Beyond genetics: driving cancer with the tumour microenvironment behind the wheel
Nature Reviews Cancer (2024)
-
Oncogenic enhancers prime quiescent metastatic cells to escape NK immune surveillance by eliciting transcriptional memory
Nature Communications (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.