Abstract
D-type cyclins are central regulators of the cell division cycle and are among the most frequently deregulated therapeutic targets in human cancer1, but the mechanisms that regulate their turnover are still being debated2,3. Here, by combining biochemical and genetics studies in somatic cells, we identify CRL4AMBRA1 (also known as CRL4DCAF3) as the ubiquitin ligase that targets all three D-type cyclins for degradation. During development, loss of Ambra1 induces the accumulation of D-type cyclins and retinoblastoma (RB) hyperphosphorylation and hyperproliferation, and results in defects of the nervous system that are reduced by treating pregnant mice with the FDA-approved CDK4 and CDK6 (CDK4/6) inhibitor abemaciclib. Moreover, AMBRA1 acts as a tumour suppressor in mouse models and low AMBRA1 mRNA levels are predictive of poor survival in cancer patients. Cancer hotspot mutations in D-type cyclins abrogate their binding to AMBRA1 and induce their stabilization. Finally, a whole-genome, CRISPR–Cas9 screen identified AMBRA1 as a regulator of the response to CDK4/6 inhibition. Loss of AMBRA1 reduces sensitivity to CDK4/6 inhibitors by promoting the formation of complexes of D-type cyclins with CDK2. Collectively, our results reveal the molecular mechanism that controls the stability of D-type cyclins during cell-cycle progression, in development and in human cancer, and implicate AMBRA1 as a critical regulator of the RB pathway.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
All accession codes, unique identifiers, and web links for publicly available datasets are available within the article and in the Reporting Summary. Those who carried out the original analysis and collection of the data generated by the DECIPHER community bear no responsibility for the further analysis or interpretation of the data. Mass spectrometry data for cyclin D1 immunopurifications are provided in Supplementary Table 1. The full scanned images obtained by electrophoretic separation are provided in Supplementary Fig. 1. All original data are available from the corresponding authors upon request. Source data are provided with this paper.
Code availability
Custom scripts for image analysis are provided at GitHub (https://github.com/FenyoLab/CRL4AMBRA1_img_analysis). Custom scripts for cancer-related analyses are provided at GitHub (https://github.com/Lesdormis/AMBRA1_analysis).
Change history
31 August 2021
This article was updated to amend the Peer Review File.
References
Malumbres, M. & Barbacid, M. Cell cycle, CDKs and cancer: a changing paradigm. Nat. Rev. Cancer 9, 153–166 (2009).
Kanie, T. et al. Genetic reevaluation of the role of F-box proteins in cyclin D1 degradation. Mol. Cell. Biol. 32, 590–605 (2012).
Qie, S. & Diehl, J. A. Cyclin D degradation by E3 ligases in cancer progression and treatment. Semin. Cancer Biol. 67, 159–170 (2020).
Reichermeier, K. M. et al. PIKES analysis reveals response to degraders and key regulatory mechanisms of the CRL4 network. Mol. Cell 77, 1092–1106.e9 (2020).
Natsume, T., Kiyomitsu, T., Saga, Y. & Kanemaki, M. T. Rapid protein depletion in human cells by auxin-inducible degron tagging with short homology donors. Cell Rep. 15, 210–218 (2016).
Barbash, O., Egan, E., Pontano, L. L., Kosak, J. & Diehl, J. A. Lysine 269 is essential for cyclin D1 ubiquitylation by the SCFFbx4/αB-crystallin ligase and subsequent proteasome-dependent degradation. Oncogene 28, 4317–4325 (2009).
Fimia, G. M. et al. Ambra1 regulates autophagy and development of the nervous system. Nature 447, 1121–1125 (2007).
Davoli, T. et al. Cumulative haploinsufficiency and triplosensitivity drive aneuploidy patterns and shape the cancer genome. Cell 155, 948–962 (2013).
Behan, F. M. et al. Prioritization of cancer therapeutic targets using CRISPR–Cas9 screens. Nature 568, 511–516 (2019).
Rahrmann, E. P. et al. Sleeping Beauty screen identifies RREB1 and other genetic drivers in human B-cell lymphoma. Mol. Cancer Res. 17, 567–582 (2019).
Reddy, A. et al. Genetic and functional drivers of diffuse large B cell lymphoma. Cell 171, 481–494 (2017).
Chytil, A. et al. Construction of a cyclin D1–Cdk2 fusion protein to model the biological functions of cyclin D1–Cdk2 complexes. J. Biol. Chem. 279, 47688–47698 (2004).
Asghar, U., Witkiewicz, A. K., Turner, N. C. & Knudsen, E. S. The history and future of targeting cyclin-dependent kinases in cancer therapy. Nat. Rev. Drug Discov. 14, 130–146 (2015).
Li, W. et al. MAGeCK enables robust identification of essential genes from genome-scale CRISPR/Cas9 knockout screens. Genome Biol. 15, 554 (2014).
Sanjana, N. E., Shalem, O. & Zhang, F. Improved vectors and genome-wide libraries for CRISPR screening. Nat. Methods 11, 783–784 (2014).
Reynders, M. et al. PHOTACs enable optical control of protein degradation. Sci. Adv. 6, eaay5064 (2020).
Lee, J. & Zhou, P. DCAFs, the missing link of the CUL4–DDB1 ubiquitin ligase. Mol. Cell 26, 775–780 (2007).
Bern, M., Kil, Y. J. & Becker, C. Byonic: advanced peptide and protein identification software. Curr. Protoc. Bioinformatics Chapter 13, Unit13.20 (2012).
Donato, V. et al. The TDH–GCN5L1–Fbxo15–KBP axis limits mitochondrial biogenesis in mouse embryonic stem cells. Nat. Cell Biol. 19, 341–351 (2017).
Jeong, Y. T. et al. The ULK1–FBXW5–SEC23B nexus controls autophagy. eLife 7, e42253 (2018).
Kuchay, S. et al. PTEN counteracts FBXL2 to promote IP3R3- and Ca2+-mediated apoptosis limiting tumour growth. Nature 546, 554–558 (2017).
Ran, F. A. et al. Genome engineering using the CRISPR–Cas9 system. Nat. Protoc. 8, 2281–2308 (2013).
Dragicevic, P. in Modern Statistical Methods for HCI (eds Robertson, J. & Kaptein, M.) 291–330 (Springer, 2016).
Róna, G. et al. Dynamics of re-constitution of the human nuclear proteome after cell division is regulated by NLS-adjacent phosphorylation. Cell Cycle 13, 3551–3564 (2014).
Cecchetelli, A., Kwan, R., Krauter, S. & Chiriboga, L. Minimum concentration of cells required for the preparation of compact plasma-thrombin cell blocks. J. Histotechnol. 35, 68–70 (2012).
Glinsmann-Gibson, B. et al. Recommendations for tissue microarray construction and quality assurance. Appl. Immunohistochem. Mol. Morphol. (2020).
Miki, Y. et al. AMBRA1, a novel α-synuclein-binding protein, is implicated in the pathogenesis of multiple system atrophy. Brain Pathol. 28, 28–42 (2018).
Lewitowicz, P. et al. Tumor digital masking allows precise patient triaging: a study based on Ki-67 scoring in gastrointestinal stromal tumors. Scanning 2018, 7807416 (2018).
Lorenzo-Martín, L. F. et al. VAV2 signaling promotes regenerative proliferation in both cutaneous and head and neck squamous cell carcinoma. Nat. Commun. 11, 4788 (2020).
Tuominen, V. J., Ruotoistenmäki, S., Viitanen, A., Jumppanen, M. & Isola, J. ImmunoRatio: a publicly available web application for quantitative image analysis of estrogen receptor (ER), progesterone receptor (PR), and Ki-67. Breast Cancer Res. 12, R56 (2010).
Shaknovich, R. et al. DNA methylation signatures define molecular subtypes of diffuse large B-cell lymphoma. Blood 116, e81–e89 (2010).
Lenz, G. et al. Molecular subtypes of diffuse large B-cell lymphoma arise by distinct genetic pathways. Proc. Natl Acad. Sci. USA 105, 13520–13525 (2008).
D’Angelo, F. et al. The molecular landscape of glioma in patients with Neurofibromatosis 1. Nat. Med. 25, 176–187 (2019).
Compagno, M. et al. Mutations of multiple genes cause deregulation of NF-κB in diffuse large B-cell lymphoma. Nature 459, 717–721 (2009).
Brune, V. et al. Origin and pathogenesis of nodular lymphocyte-predominant Hodgkin lymphoma as revealed by global gene expression analysis. J. Exp. Med. 205, 2251–2268 (2008).
Cerami, E. et al. The cBio cancer genomics portal: an open platform for exploring multidimensional cancer genomics data. Cancer Discov. 2, 401–404 (2012).
Gao, J. et al. Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci. Signal. 6, pl1 (2013).
Tate, J. G. et al. COSMIC: the Catalogue Of Somatic Mutations In Cancer. Nucleic Acids Res. 47 (D1), D941–D947 (2019).
Schmitz, R. et al. Burkitt lymphoma pathogenesis and therapeutic targets from structural and functional genomics. Nature 490, 116–120 (2012).
Clijsters, L. et al. Cyclin F controls cell-cycle transcriptional outputs by directing the degradation of the three activator E2Fs Mol. Cell 74, 1264–1277 (2019).
Yada, M. et al. Phosphorylation-dependent degradation of c-Myc is mediated by the F-box protein Fbw7. EMBO J. 23, 2116–2125 (2004).
Maxwell, P. H. et al. The tumour suppressor protein VHL targets hypoxia-inducible factors for oxygen-dependent proteolysis. Nature 399, 271–275 (1999).
Kubbutat, M. H., Jones, S. N. & Vousden, K. H. Regulation of p53 stability by Mdm2. Nature 387, 299–303 (1997).
Li, Y., Ge, D. & Lu, C. The SMART app: an interactive web application for comprehensive DNA methylation analysis and visualization. Epigenetics Chromatin 12, 71 (2019).
Lin, D. I. et al. Phosphorylation-dependent ubiquitination of cyclin D1 by the SCFFBX4-αB crystallin complex. Mol. Cell 24, 355–366 (2006).
Okabe, H. et al. A critical role for FBXW8 and MAPK in cyclin D1 degradation and cancer cell proliferation. PLoS ONE 1, e128 (2006).
Santra, M. K., Wajapeyee, N. & Green, M. R. F-box protein FBXO31 mediates cyclin D1 degradation to induce G1 arrest after DNA damage. Nature 459, 722–725 (2009).
Wei, S. et al. A novel mechanism by which thiazolidinediones facilitate the proteasomal degradation of cyclin D1 in cancer cells. J. Biol. Chem. 283, 26759–26770 (2008).
Yu, Z. K., Gervais, J. L. & Zhang, H. Human CUL-1 associates with the SKP1/SKP2 complex and regulates p21(CIP1/WAF1) and cyclin D proteins. Proc. Natl Acad. Sci. USA 95, 11324–11329 (1998).
Chen, B. B., Glasser, J. R., Coon, T. A. & Mallampalli, R. K. FBXL2 is a ubiquitin E3 ligase subunit that triggers mitotic arrest. Cell Cycle 10, 3487–3494 (2011).
Chen, B. B. et al. F-box protein FBXL2 targets cyclin D2 for ubiquitination and degradation to inhibit leukemic cell proliferation. Blood 119, 3132–3141 (2012).
Pawar, S. A. et al. C/EBPdelta targets cyclin D1 for proteasome-mediated degradation via induction of CDC27/APC3 expression. Proc. Natl Acad. Sci. USA 107, 9210–9215 (2010).
Crooks, G. E., Hon, G., Chandonia, J. M. & Brenner, S. E. WebLogo: a sequence logo generator. Genome Res. 14, 1188–1190 (2004).
Yang, H. W. et al. Stress-mediated exit to quiescence restricted by increasing persistence in CDK4/6 activation. eLife 9, e44571 (2020).
Cappuccio, G., Ugga, L., Parrini, E., D’Amico, A. & Brunetti-Pierri, N. Severe presentation and complex brain malformations in an individual carrying a CCND2 variant. Mol. Genet. Genomic Med. 7, e708 (2019).
Maini, I. et al. A novel CCND2 mutation in a previously reported case of megalencephaly and perisylvian polymicrogyria with postaxial polydactyly and hydrocephalus. Neuropediatrics 49, 222–224 (2018).
McDermott, J. H. et al. Hypoglycaemia represents a clinically significant manifestation of PIK3CA- and CCND2-associated segmental overgrowth. Clin. Genet. 93, 687–692 (2018).
Mirzaa, G. et al. De novo CCND2 mutations leading to stabilization of cyclin D2 cause megalencephaly-polymicrogyria-polydactyly-hydrocephalus syndrome. Nat. Genet. 46, 510–515 (2014).
Firth, H. V. et al. DECIPHER: Database of Chromosomal Imbalance and Phenotype in Humans Using Ensembl Resources. Am. J. Hum. Genet. 84, 524–533 (2009).
Sameshima, T., Morisada, N., Egawa, T., Kugo, M. & Iijima, K. MPPH syndrome with aortic coarctation and macrosomia due to CCND2 mutations. Pediatr. Int. 62, 115–117 (2020).
Acknowledgements
We thank G. V. Pires, L. Moro, V. Donato, A. Zeke, A. Peschiaroli, M. Swartling, K. Avrampou, J. Wang, E. Hernandez and A. Tsirigos for their contribution to this work, and R. Abraham, S. Dann, K. Nakayama and W. Wei for critically reading the paper. This study makes use of data generated by the DECIPHER community. A full list of centres that contributed to the generation of the data is available from https://decipher.sanger.ac.uk/about/stats and via email from decipher@sanger.ac.uk. Funding for the DECIPHER project was provided by Wellcome. We thank E. Rosser and M. Lees from the Great Ormond Street Hospital for Children NHS Foundation Trust in London, UK, for providing the information on two patients with mutations in CCND2, deposited at DECIPHER (https://decipher.sanger.ac.uk). The Proteomics Laboratory, the Genome Technology Center (GTC), the Experimental Pathology Research Laboratory, the Cytometry and Cell Sorting Laboratory, and the Metabolomics Laboratory at NYU Langone Health are partially supported by the Cancer Center Support Grant P30CA016087 at the Laura and Isaac Perlmutter Cancer Center. The NYULH Center for Biospecimen Research and Development, Histology and Immunohistochemistry Laboratory (RRID:SCR_018304) is supported in part by the Laura and Isaac Perlmutter Cancer Center Support Grant, NIH/NCI P30CA016087, and the National Institutes of Health S10 Grants, NIH/ORIP S10OD01058 and S10OD018338. The authors thank C. I. Silvescu for data acquisition and processing of the mass spectrometry images. D.S. thanks F. Simoneschi, P. Simoneschi, D. Guidi and E. Guidi for continuous support. M.P. thanks T. M. Thor and T. B. Balduur for continuous support. This work was funded by grants from the National Institutes of Health (R01-CA76584 and R35-GM136250) to M.P. and (R01-CA207513-01) to L.B. The F.C. laboratory is supported by grants from the Danish Cancer Society (KBVU R72-A4408, R146-A9364, R231-A14034 to F.C. and R146-A9471 to V.C.), the Novo Nordisk Foundation (NNF13OC0007559, NNF16OC0022544), the Lundbeck Foundation (R233-2016-3360 to F.C. and R209-2015-3505 to V.C.), the LEO Foundation (LF17024 to F.C.), Associazione Italiana per la Ricerca sul Cancro (AIRC project IG 2019 no. 23543 to F.C.), the Italian Ministry of Research (MIUR, project PRIN 2017 Radius), and the Italian Ministry of Health (Ricerca Corrente to F.N.). V.C. is supported by Fondazione Umberto Veronesi. E.M. is an adjunct professor at UniCamillus—Saint Camillus International University of Health Sciences in Rome, Italy. F.B. is supported by a Young Investigator Grant from the Alex’s Lemonade Stand Foundation. M.P. is an investigator with the Howard Hughes Medical Institute.
Author information
Authors and Affiliations
Contributions
D.S. conceived, planned and performed most experiments, and co-wrote the manuscript. G.R., Y.-T.J., A.O., A.A.W. and S.N. helped with biochemical experiments. N.Z. and L.B. performed the DLBCL xenografts. S.J. helped with bioinformatics analyses. F.B. helped with the collection of mouse plasma, embryos and amniotic fluid. S.K. and D.F. performed the automated analysis of live-cell images. Y.S. and D.R.J. performed the LC-MS/MS detection of abemaciclib. G.M., V.C., E.M., F.N. and F.C. performed the experiments with Ambra1+/+ and Ambra1gt/gt mice related to neural development. A.A.A. analysed and scored immunohistochemistry stainings. M.P. conceived, directed and coordinated the study, oversaw the results and co-wrote the manuscript. All authors discussed the results and commented on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
M.P. is a consultant for and has financial interests in Coho Therapeutics, CullGen, Kymera Therapeutics and SEED Therapeutics. M.P. is a cofounder of Coho Therapeutics, and is a member of the scientific advisory board of CullGen, Kymera Therapeutics and SEED Therapeutics, and is a consultant for Santi Therapeutics. The other authors declare no competing interests.
Additional information
Peer review information Nature thanks Piotr Sicinski and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer reviewer reports are available.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 CRL1 does not contribute to the degradation of D-type cyclins.
a, hTERT RPE-1, U-2 OS and HCT-116 cells were treated with MG132 or MLN4924 for 4 h before collection. Cell extracts were immunoblotted for the indicated proteins. b, HCT-116 cells were treated for 3 h with vehicle (DMSO) or MLN4924 followed by cycloheximide for the indicated times before collection. Cell extracts were immunoblotted for the indicated proteins. c, HCT-116 cells were transfected with a non-targeting (N/T) siRNA or an siRNA against DDB1 for three rounds before lysis and immunoblotting for the indicated proteins. d, HCT-116 cells were transfected with a non-targeting siRNA or an siRNA against CUL1 for three rounds followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. e, U-2 OS cells were transfected with a non-targeting siRNA or an siRNA against CUL1 for three rounds followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. f, PC-3 cells were transfected with a non-targeting (N/T) siRNA or an siRNA against CUL1 for three rounds followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. g, hTERT RPE-1 cells were transfected with a non-targeting siRNA or an siRNA against CUL1 for three rounds followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. h, U-2 OS cells were infected with a doxycycline-inducible lentivirus expressing a dominant-negative mutant of CUL1 (DN-CUL1). Cells were treated with doxycycline for the indicated times. Where indicated, cells were exposed to UV (5 mJ cm−2) irradiation for 2 h before collection. Cell extracts were immunoblotted as indicated. i, Representatives images of U-2 OS cells infected with a retrovirus expressing mAzG-CCND1 and treated with MLN4924 for the indicated times. Cells were monitored via live-cell imaging. Scale bar, 20 μm. j, Quantification of relative mAzG-CCND1 nuclear intensity fold change in arbitrary units (A.U.) from single cells tracked over time as in i. Data are mean ± s.d., n = 34 cells. k, Schematic representation of approach 1, aimed at measuring the accumulation of cyclin D1 upon silencing of all human DCAFs and the previously-reported regulators of D-type cyclins45,46,47,48,49,50,51,52 in HCT-116 and U-2 OS cells. l, Schematic representation of approach 2, aimed at identifying the binding partners of FFSS-tagged wild-type cyclin D1 and FFSS-tagged cyclin D1(T286A) compared with empty vector. HCT-116 cells were treated with DMSO, MG132 or MLN4924 for 4 h before lysis and immunoprecipitation with an anti-Flag resin, followed by elution with a 3×Flag peptide. Eluted samples were then analysed by LC-MS/MS for the identification of binding partners. m, Schematic representation of approach 3, aimed at identifying global regulators of cyclin D1 in HCT-116 cells using the whole-genome, CRISPR–Cas9 human GECKOv2 pooled library. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 2 Validation of candidate regulators of D-type cyclins.
a, HCT-116 cells were transfected with a non-targeting siRNA or siRNAs against the indicated targets for two rounds before collection. Cell extracts were immunoblotted as indicated (upper panel). RNA extracts were also collected to measure the relative mRNA levels for each indicated target by quantitative PCR with reverse transcription (RT–qPCR). Each blue column represents the mRNA levels of the target indicated by the respective siRNA and normalized to its corresponding mRNA levels in cells transfected with a non-targeting siRNA (bottom). Data are mean mRNA levels ± s.d., n = 3 independent experiments. b, HCT-116 cells were transfected with a non-targeting siRNA or siRNAs against the indicated targets for two rounds followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. c, HCT-116 cells were transfected with a non-targeting siRNA or an siRNA against DCAF7 followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. d, U-2 OS cells were transfected with a non-targeting siRNA or an siRNA against DCAF8 followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. e, U-2 OS cells were transfected with a non-targeting siRNA or an siRNA against WDR61 followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated (left). RNA extracts were also collected to measure the relative mRNA levels of WDR61 by RT–qPCR (right). Data are mean mRNA levels ± s.d., n = 3 independent experiments. f, hTERT RPE-1 cells were transfected with a non-targeting siRNA or an siRNA against AMBRA1 followed by treatment with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. g, HeLa, HEK 293T, HCT-116, hTERT RPE-1 and U-2 OS cells were transfected with a non-targeting siRNA or an siRNA against AMBRA1 before collection. Cell extracts were immunoblotted for the indicated proteins (l.e., long exposure; m.e., medium exposure; s.e., short exposure). h, Schematic representation of the AMBRA1 genomic locus and gRNA target location. Exon 2 refers to the human AMBRA1 gene in XM_005253009 (GRCh38.p13, NCBI gene: 55626). Representative AMBRA1 wild-type genomic DNA template and knockout mutant sequences identified by TOPO-TA cloning of PCR products from HCT-116, U-2 OS and hTERT-RPE1 cells are depicted. i, Three AMBRA1−/− and one AMBRA1+/+ hTERT RPE-1 clones were treated with cycloheximide for the indicated times, after which cell extracts were immunoblotted for the indicated proteins. j, Two AMBRA1−/− and one AMBRA1+/+ T98G clones were treated with either cycloheximide for the indicated times, MG132 or MLN4924 (both for 4 h) before collection. Cell extracts were then immunoblotted for the indicated proteins. k, HCT-116 cells were infected with a retrovirus expressing mAzG-CCND1 and transfected with a non-targeting siRNA or an siRNA against AMBRA1 for two rounds. Cells were then treated with cycloheximide for the indicated times, after which cell extracts were immunoblotted for the indicated proteins (endo, endogenous; exo, exogenous). l, AMBRA1−/− U-2 OS cells were transiently transfected with a vector expressing a C-terminal 3×Flag-tagged AMBRA1 or an empty vector for 96 h. Where indicated, cells were treated with MLN4924 for 4 h before lysis. Cell extracts were immunoblotted as indicated. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 3 Depletion of AMBRA1 using the auxin-inducible degron system.
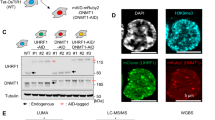
a, Schematic representation of the CRISPR–Cas9-based strategy to insert an N-terminal, 2×Flag-tagged minimal AID (mAID) in the endogenous locus of AMBRA1 (5′-end of exon 2) in HCT-116 cells. Cells were infected with a doxycycline-inducible lentivirus expressing Oryza sativa TIR1 (osTIR1). b, Three knock-in clones were obtained as in a and compared to wild-type clones for proper endogenous tagging of AMBRA1 by immunoblotting. Note the higher molecular weight of 2×Flag-mAID-tagged AMBRA1. c, Three knock-in clones were treated with doxycycline with or without increasing doses of auxin for 12 h. Cell extracts were immunoblotted as indicated. The asterisk indicates a non-specific band. d, One clone of 2×Flag-mAID-AMBRA1 HCT-116 cells (clone #F1) was treated with either DMSO or doxycycline for 12 h, and/or auxin, MG132 and MLN4924 (alone or in combination) for 4 h as indicated. Cell extracts were immunoblotted as indicated. e, Longer exposure from the cyclin D1 and phospho-cyclin D1 (T286) immunoblots described in d. f, Whole-cell extracts from 2×Flag-mAID-AMBRA1 HCT-116 cells pre-treated with either DMSO or doxycycline for 12 h, and exposed to combinations of auxin, MG132 and/or MLN4924 as indicated for 4 h, related to Fig. 2d. Cell extracts were immunoblotted as indicated. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 4 Mutations in the TP motif of D-type cyclins protect them from AMBRA1-mediated degradation.
a, Protein sequence alignment of the extreme C termini of D-type cyclins from different source organisms. Amino acids highlighted in red correspond to the highly conserved TP motif. Asterisks indicate positions that are fully conserved. Colons indicate conservation between groups of strongly similar properties. The dot indicates conservation between groups of weakly similar properties. The alignment was performed in UniProt (https://www.uniprot.org/) using the Clustal Omega algorithm. UniProt identifiers are shown on the left. Source organisms: HUMAN, H. sapiens; BOVIN, Bos taurus; CANLF, Canis familiaris; MOUSE, Mus musculus; RAT, Rattus norvegicus; DANRE, Danio rerio; BRAFL, Branchiostoma floridae; STRPU, Strongylocentrotus purpuratus; CRAGI, Crassostrea gigas; LOTGI, Lottia gigantean; OCTBM, Octopus bimaculoides; STRMM, Strigamia maritima; BOMMO, Bombyx mori; ATTCE, Atta cephalotes; APIME, Apis mellifera; CULQU, Culex quinquefasciatus; HYDVU, Hydra vulgaris; NEMVE, Nematostella vectensis; TRIAD Trichoplax adhaerens. b, Multiple sequence logo of the alignment performed in a generated using WebLogo 3 (http://weblogo.threeplusone.com)53. c, HCT-116 cells were infected with lentiviruses expressing either FFSS-tagged empty vector (EV) or FFSS-tagged wild-type or mutant cyclin D1. Cells were treated with MLN4924 before lysis and affinity purification (AP) with an anti-STREP resin. Proteins were immunoblotted as indicated. d, HEK 293T cells were transiently transfected with plasmids expressing either SF-tagged empty vector or SF-tagged D-type cyclins wild-type or mutants. Cells were treated with MLN4924 before lysis and immunoprecipitation with an anti-Flag resin. Proteins were immunoblotted as indicated. e, HCT-116 cells were infected with retroviruses expressing FFSS-tagged wild-type or mutant cyclin D1. Cells were treated with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. f, HCT-116 cells were infected with retroviruses expressing FFSS-tagged wild-type or mutant cyclin D2. Cells were treated with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. g, HCT-116 cells were infected with retroviruses expressing FFSS-tagged wild-type or mutant cyclin D3. Cells were treated with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. h, HCT-116 cells were transfected with vectors expressing SF-tagged CDC25A, SF-tagged p27, SF-tagged cyclin D1, SF-tagged cyclin D1(T286A) or empty vector. Cells were treated with MLN4924 for 4 h before collection. Lysates were used for an immunoprecipitation with an anti-Flag resin. Proteins were immunoblotted as indicated. i, HCT-116 cells were transfected with vectors expressing HA-tagged FBXO4, SF-tagged TRF1, SF-tagged cyclin D1, SF-tagged cyclin D1(T286A) or empty vector. Cells were treated with MLN4924 for 4 h before collection. Lysates were used for an affinity purification with an anti-Strep resin. Proteins were immunoblotted as indicated. The asterisk indicates a non-specific band. j, HCT-116 cells were transfected with vectors expressing HA-tagged FBXW8, SF-tagged IRS1, SF-tagged cyclin D1, SF-tagged cyclin D1(T286A) or empty vector. Cells were treated with MLN4924 for 4 h before collection. Lysates were used for an immunoprecipitation with an anti-Flag resin. Proteins were immunoblotted as indicated. k, Parental and 2×Flag–mAID–AMBRA1 HCT-116 cells were lysed and their extracts were used for an immunoprecipitation with an anti-Flag resin. Proteins were immunoblotted as indicated. l, One clone of 2×Flag–mAID–AMBRA1 HCT-116 cells (clone F1) was infected with retroviruses expressing GFP-CCND1 or GFP-CCND1(T286A). Cells were treated with doxycycline for 12 h, before exposure to auxin for 4 h before collection as indicated. Control cells were treated with DMSO. Cell extracts were immunoblotted as indicated. m, Parental and AMBRA1−/− HCT-116 and U-2 OS cells were lysed and their extracts were blotted as indicated. The accumulation of cyclin D1 and phosphorylated cyclin D1 (T286) is reported as their corresponding intensity ratios between AMBRA1−/− and parental cells. Data are mean ± s.e.m. (n = 3 biological replicates per group). n, Three different AMBRA1−/− HCT-116 clones (clones D2, F11 and G7), 2×Flag-mAID-AMBRA1 HCT-116 cells (clone F1) and HCT-116 cells transfected with a non-targeting siRNA or an siRNA against AMBRA1 were lysed and their extracts were immunoblotted as indicated (either by employing fluorescently labelled secondary antibodies or by enhanced chemiluminescence). Untransfected CCND1−/− HCT-116 cells or CCND1−/− HCT-116 cells transfected with vectors expressing untagged cyclin D1(WT) or untagged cyclin D1(T286A) were used as control. Where indicated (black triangles), samples were serially diluted before electrophoresis and immunoblotting for easier visual comparison of cyclin D1 and phosphorylated cyclin D1 (T286) levels between groups. The analysis of normalized phosphorylated cyclin D1 (T286) over total cyclin D1 fluorescent intensity levels are provided as bar graphs. The ratios were calculated from lane 2 and lane 4 from each biological group in the fluorescent immunoblot. o, HCT-116 cells were infected with lentiviruses expressing FFSS-tagged cyclin D1 or FFSS-tagged cyclin D1(T286A). Cells were treated with DMSO (N/T) or MLN4924 for 4 h before lysis and immunoprecipitation with an anti-Flag resin, followed by elution with a 3×Flag peptide. Eluted samples were then analysed by LC-MS/MS for the identification of post-translational modifications. The table reports all identified sites in wild-type cyclin D1 and cyclin D1(T286A) that were modified with a di-Gly/114.0429 signature. p, Synthetic, unphosphorylated (amino acids PKAAEEEEEEEEEVDLACTPTDVRDVDI) and phosphorylated (T286) (amino acids PKAAEEEEEEEEEVDLAC-pT-PTDVRDVDI) peptides (2.5 μg each) corresponding to the extreme C terminus of cyclin D1 were spotted on a nitrocellulose membrane before immunoblotting with an anti-phosphorylated cyclin D1 (T286) antibody. q, Synthetic, phosphorylated (T286) peptide corresponding to the sequence of cyclin D1 indicated in p was incubated with in vitro transcribed and translated AMBRA1 from rabbit reticulocytes extracts for the indicated times in the presence of wild-type ubiquitin (Ub) or a mutant of ubiquitin [Ub(K0)] in which all lysine residues have been mutated to arginine. Reactions were stopped with Laemmli buffer. Proteins were immunoblotted as indicated. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 5 Loss of AMBRA1 regulates D-type cyclins during normal cell cycle, upon nutrient deprivation and after genotoxic stress.
a, Three AMBRA1−/− and two AMBRA1+/+ clones were pulsed with EdU for 45 min before fixation with 4% paraformaldehyde, and immunofluorescent staining for the indicated proteins. Detection of EdU was accomplished using the Click-iT Plus EdU Alexa Fluor 647 Imaging Kit (Thermo Fisher Scientific). DAPI was used to detect DNA. Scale bars, 20 μm. b, AMBRA1+/+ and AMBRA1−/− T98G cells were serum-deprived for 72 h. Cells were then released with the re-addition of 10% FBS and collected at the indicated times. Cell extracts were immunoblotted as indicated. c, Representative images of AMBRA1+/+ and AMBRA1 −/− U-2 OS cells stably infected with retroviruses expressing mAzG-CCND1 and mPlum-PCNA and monitored via live-cell imaging. Note that mPlum-PCNA forms nuclear foci during S phase. Scale bar, 20 μm. d, Quantification of mAzG-CCND1 changes in mean nuclear intensity in single cells tracked over time related to c. Plots represent percentage change from t = 0 (PCNA foci formation). Lines show mean and the shaded regions represent the 95% confidence interval. AMBRA1 WT, n = 12 cells; AMBRA1 KO, n = 34 cells. e, U-2 OS cells were infected with a retrovirus expressing mAzG-cyclin D1, and transfected with a non-targeting siRNA or an siRNA against AMBRA1 for two rounds. Cells were then exposed to UV (5 mJ cm−2) irradiation for the indicated times before collection. Cell extracts were immunoblotted as indicated. f, HCT-116 cells were infected with a retrovirus expressing mAzG-cyclin D1, and transfected with a non-targeting siRNA or an siRNA against AMBRA1 for two rounds. Cells were then exposed to UV (5 mJ cm−2) irradiation for the indicated times before collection. Cell extracts were immunoblotted as indicated. g, AMBRA1+/+ and AMBRA1−/− HCT-116 and U-2 OS cells were maintained in normal medium or nutrient-deprived in EBSS for 4 h before collection. Cell extracts were immunoblotted as indicated. h, HCT-116 cells were transfected with a non-targeting siRNA or combinations of siRNAs against AMBRA1, E2F1, E2F2 and E2F3 as indicated for three rounds before lysis and immunoblotting for the indicated proteins. i, T98G cells were transfected with an sgRNA control or an sgRNA targeting AMBRA1. AMBRA1−/− clones positive for gene editing were pooled together. Parental and AMBRA1−/− pooled T98G cells were then infected with a CDK4/6 activity reporter54 and seeded in glass-bottom plates. Three days after seeding, cells were stained with Hoechst 33342 before imaging. Scale bars, 50 μm. j, AMBRA1+/+ and AMBRA1−/− U-2 OS cells were fixed in 4% paraformaldehyde and immunostained as indicated. DAPI was used to detect DNA. Scale bars, 20 μm. k, HCT-116, U-2 OS and hTERT RPE-1 cells were treated with leptomycin B (LMB) for 4 h before exposure to cycloheximide for the indicated times. Cell extracts were immunoblotted as indicated. l, U-2 OS cells were infected with retroviruses expressing either mAZG-tagged wild-type cyclin D1 or cyclin D1 fused to a nuclear localization signal (NLS). Cells were then treated with cycloheximide for the indicated times before collection. Cell extracts were immunoblotted as indicated. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 6 Report of MPPH-derived mutations in CCND2 and evidence of the ability of abemaciclib to cross the murine placental barrier.
a, Graphical representation of MPPH-associated CCND2 mutations affecting T280 and P281 in cyclin D255,56,57,58,59,60. b, Genotype and clinical phenotypes of patient 295112 (https://decipher.sanger.ac.uk)59. c, Genotype and clinical phenotypes of patient 305416 (https://decipher.sanger.ac.uk)59. d, Representative immunofluorescent sections (20× magnification) of the mesencephalic ventricular zone of E13.5 Ambra1+/+ and Ambra1gt/gt embryos stained for cyclin D1, cyclin D2 or p-RB (S807/811). Scale bars, 100 μm. e, Experimental timeline of the daily, oral administration of abemaciclib to pregnant Ambra1gt/+ mice (from E8.5 to E13.5) (1), and collection of amniotic fluid via a 28G insulin syringe from the amniotic sacs of E13.5 embryos for subsequent LC-MS/MS analysis (2). f, Mass spectrometry imaging of abemaciclib in mouse embryos. Left, optical registration image of the slide with each section before MALDI imaging. Right, extracted ion mobility image for abemaciclib (green) as detected based on authentic standards [M+H]+ at 507.2791 m/z (±15 ppm) with a mobility (1/K0) of 1.177 (±1%), maternal dose of 100 mg kg−1. Scale bar, 2 mm. This experiment was performed once. g, h, MS intensity of abemaciclib in tissue samples (g), interpolated abemaciclib concentration in maternal plasma (h, left) and interpolated abemaciclib concentration in amniotic fluid (h, right). Maternal brain, embryonic tissue, amniotic fluid and maternal plasma samples were obtained from mice administrated with daily dosages of abemaciclib mesylate at 8 mg kg−1 or 16 mg kg−1 from E8.5 to E13.5, and at 100 mg kg−1 from E12.5 to E13.5. The abemaciclib MS intensity shown for tissue samples was corrected based on a 3× signal-to-noise cut-off with a floor of 10,000 using the blank controls. The abemaciclib concentration shown in both the amniotic fluid and plasma sample was interpolated based on the standard curve prepared in blank amniotic fluid and blank plasma, respectively. N.D., not detected. This experiment was performed once. i, j, E13.5 Ambra1+/+ and Ambra1gt/gt embryos were collected from pregnant mice treated with vehicle (PBS) or 8 mg kg−1 abemaciclib. Immunofluorescence from sections was quantified to show area of p-RB (S807/811) (i) and cyclin D2 (j) staining in the mesencephalic ventricular zone (MVZ). Data are mean ± s.d. p-Rb (S807/811), n = 3; cyclin D2, n = 3. Adjusted P values were calculated using a two-way ANOVA with Tukey’s multiple comparisons test. k, Protein extracts derived from E9.5, E10.5 and E13.5 Ambra1+/+ and Ambra1gt/gt embryo heads (four independent embryos per group) were immunoblotted for the indicated proteins. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 7 AMBRA1 and D-type cyclins in human cancer.
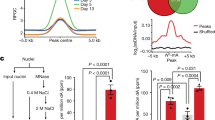
a, Lolliplots showing amino acid positions and numbers of mutations in AMBRA1, FBXO11, CCNF and KEAP1 in pan-cancer samples generated from cBioPortal (https://www.cbioportal.org/) and using the curated set of non-redundant studies36,37 (last accessed: December 2019). b, Scatter plot of cyclin D1 protein levels (RPPA) and mRNA expression levels of AMBRA1 (FPKM-UQ) in different TCGA cohorts. LGG, n = 435; OV, n = 257; PRAD, n = 344; TGCT, n = 124. Pearson correlation analysis was performed to calculate P and R values. The shaded area represents the 95% confidence interval of the regression line. c, Representative immunohistochemistry image fields of AMBRA1−/− and AMBRA1+/+ HCT-116 plasma-thrombin cell blocks stained with either a rabbit polyclonal anti-human AMBRA1 antibody (Proteintech Group 13762-1, lot nos. 00005112 and 00017852, RRID: AB_10642007), a mouse anti-human AMBRA1 clone G-6 antibody (Santa Cruz Biotechnology sc-398204, lot no. G1217, RRID: AB_2861324), or a rabbit anti-human cyclin D1 clone SP4 antibody (Ventana Medical Systems 790-4508, lot no. B08078, RRID: AB_2335988). Scale bar, 50 μm. This experiment was performed once. d, A TMA containing normal and tumour ovarian human specimens was immunostained with antibodies to AMBRA1 and cyclin D1. Violin plots show automated quantification of cyclin D1 intensity levels and pathological scoring of nuclear AMBRA1 intensity levels (0, no expression; 1, faint expression; 2, mild or moderate expression) (n = 44 biologically independent samples). Adjusted P values were calculated using a one-way ANOVA with Dunnett’s multiple comparisons test. e, The graph shows automated quantification of cyclin D1 and AMBRA1 intensity levels from the TMA described in d. n = 44 biologically independent samples. Pearson correlation analysis was performed to calculate P and R2 values. The shaded area represents the 95% confidence interval of the regression line. f, Kaplan–Meier plots showing survival probability of human cancer patients partitioned in low AMBRA1 mRNA levels (n = 2,110 for quantiles 0.2/0.8, and n = 5,273 for quantiles 0.5/0.5) and high AMBRA1 mRNA levels (n = 2,110 for quantiles 0.2/0.8, and n = 5,273 for quantiles 0.5/0.5; TCGA (https://cancer.gov/tcga)). P values were calculated using the log-rank test. Meta P values: 0.0389 (for quantiles 0.2/0.8), 0.0475 (for quantiles 0.5/0.5). g, Priority targets from pan-cancer and cancer-type analyses, as previously described9. CCND1, CCND2, CDK4 and CDK6 are highlighted in red. Select oncogenes are in black.
Extended Data Fig. 8 C-terminal cancer mutations affecting cyclin D1, cyclin D2 and cyclin D3.
a–c, Lolliplots showing the amino acid positions and their mutation numbers in the degron motif of CCND1 (a), CCND2 (b) and CCND3 (c) in pan-cancer, gathered and combined from cBioPortal (curated set of non-redundant studies)36,37, COSMIC (https://cancer.sanger.ac.uk/cosmic)38, and Schmitz et al.39 (indicated by the dagger). Black arrows in c indicate mutations identified in haematopoietic and lymphoid malignancies. del, deletion; fs, frameshift; *, stop codon. Last accessed October 2019.
Extended Data Fig. 9 AMBRA1 CRISPR gene score distribution in DLBCL.
a–c, Average pan- (a), subtype-specific (b) and cell-type specific (c) DLBCL CRISPR gene score distribution, as reported11. ABC, activated B cell-like; GCB, germinal centre B cell-like. Putative oncogenes are depicted in blue; putative tumour suppressors are depicted in red.
Extended Data Fig. 10 AMBRA1 is a tumour suppressor in DLBCL.
a, Differential expression of AMBRA1 in DLBCL compared with normal B-lymphocytes from Compagno et al.34. P = 9.91 × 10−6. b, Differential expression of AMBRA1 in DLBCL compared with normal B-lymphocytes from Brune et al.35. P = 0.003. a, b, Dots indicate maxima and minima; whiskers indicate 90th and 10th percentiles; box edges indicate 75th and 25th percentiles; and centre lines indicate median; P values were calculated using a Student’s t-test, as described (https://www.oncomine.org). c, TCGA-derived, CpG-aggregated methylation values (β-values) of AMBRA1 and other established hypermethylated genes in cancer (depicted in red) compared with hypomethylated genes (depicted in green) in DLBCL. Solid lines denote the mean of β-values for each group. d, Kaplan–Meier plot showing survival probability of patients with DLBCL partitioned in low AMBRA1 mRNA levels (n = 50) and high AMBRA1 mRNA levels (n = 49), combining GEO number GSE2350131 and GEO number GSE1084632, using probe 52731_at (https://www.oncomine.org) (0.10/0.90 quantiles). P values by log-rank test. e, OncoPrint map of the genetic alterations in AMBRA1 and selected RB-pathway genes; TCGA DLBC cohort. f, Heat map showing hierarchical clustering of transcriptional signatures of tumours bearing alterations in either AMBRA1 or CCND3, derived from TCGA DLBC cohort. del, deletion; mut, mutation; amp, amplification; other, tumours bearing unaltered AMBRA1 and CCND3. AMBRA1 (RefSeq XM_005253009) mutations: R439K and D1287G. CCND3 (RefSeq NM_001760) mutation: T283A. g, Gene enrichment analysis of the top 300 most differentially expressed genes in patients harbouring alterations in AMBRA1 and CCND3 from TCGA (DLBC cohort) was performed using Enrichr (https://amp.pharm.mssm.edu/Enrichr/) with BioPlant (2019), Reactome (2016) and NCI-Nature (2016) databases. Asterisks indicate pathways regulated by D-type cyclins. h, BJAB cells were infected with lentiviruses expressing either one of three independent sgRNAs targeting AMBRA1 or one sgRNA targeting luciferase as control (CTRL). Upon FACS sorting, cell populations were treated with cycloheximide for the indicated times, MG132 or MLN4924 (for 4 h) before collection. Cell extracts were immunoblotted for the indicated proteins. i, BJAB cells expressing either control sgRNA targeting luciferase or sgRNA targeting AMBRA1 were xenotransplanted in NSG mice via subcutaneous flank injections. Tumour volume was calculated by caliper measurement. Data are mean tumour volume ± s.d. (n = 3 per group); nonlinear (exponential growth) fitted curves. P values by unpaired, multiple-comparison t-test using the Holm–Sidak method. Day 0: NS; day 13: P = 0.1885]; day 14 P = 0.0045; day 15: P = 0.0083; day 16: P = 0.0048; day 17: P = 0.0223. *P < 0.05. j, The weight of tumours described in i was measured on excised tumours at the experimental end point. Data are mean tumour weight ± s.e.m. (n = 3 per group). P values by unpaired t-test. k, U-2932 cells were infected with lentiviruses expressing either one of three independent sgRNAs targeting AMBRA1 or one sgRNA targeting luciferase as control (CTRL). Upon FACS sorting, cell populations were collected, and cell extracts were immunoblotted as indicated. l, U-2932 expressing either control sgRNA targeting luciferase or sgRNA targeting AMBRA1 were xenotransplanted in NSG mice via subcutaneous flank injections. Tumour volume was calculated by caliper measurement. Data are mean tumour volume ± s.e.m. (n = 5 per group at day 0). P values by unpaired, multiple-comparison t-test using the Holm–Sidak method, until day 40 (the latest time point where at least 3 mice per group were available). Day 23: P = 0.0008; day 25: P = 0.0191; day 26: P = 0.0133; day 27: P = 0.0041; day 30: P = 0.0079; day 31: P = 0.0292; day 32: P = 0.0148; day 33: P = 0.0002; day 34: P = 0.0001; day 37: P = 0.0165; day 38: P = 0.0306; day 39: P = 0.0240; day 40: P = 0.0401. *P < 0.05. These data are from the same dataset shown in Fig. 4c. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 11 Loss of AMBRA1 promotes the formation of CDK2–D-type cyclins complexes.
a, Schematic representation of the experiment used to identify global regulators of the response to CDK4/6 inhibitors in U-2 OS cells using a whole-genome, CRISPR–Cas9 human GECKOv2 pooled library. b, Scatter plot of the candidate hits generated from a. This experiment was performed once, with four technical replicates. P values were calculated using the MAGeCK algorithm14. c, Parental and AMBRA1−/− HCT-116, T98G or U-2 OS cells were treated with various concentrations of abemaciclib. Survival curves were generated using the AlamarBlue assay. Data are mean survival percentage ± s.d. (n = 3 biological replicates per group). The signal from each condition was normalized to an untreated control to adjust for any relative growth difference. d, AMBRA1+/+ and AMBRA1−/− T98G cells were treated with abemaciclib (75 nM) or DMSO for 24 h before collection and immunoblotting for the indicated proteins. e, HCT-116 cells were transfected with a non-targeting siRNA or an siRNA against AMBRA1 for three rounds before treatment with abemaciclib (75 nM) or DMSO for 24 h. Cells were collected and their extracts were immunoblotted for the indicated proteins. f, Parental and AMBRA1−/− HCT-116 cells were collected, and their extracts were used for an immunoprecipitation with an anti-CDK4 antibody or control IgG isotype. Proteins were immunoblotted as indicated. g, HEK 293T were transfected with plasmids expressing either FFSS-tagged cyclin D1, cyclin D2 and cyclin D3 or empty vector before lysis and immunoprecipitation with an anti-Flag resin. Proteins were immunoblotted as indicated. h, AMBRA1−/− HCT-116 cells were collected, and their extracts were used for an immunoprecipitation with an anti-cyclin D1 antibody or control IgG isotype. Proteins were immunoblotted as indicated. i, AMBRA1−/− HCT-116 cells were collected, and their extracts were used for an immunoprecipitation with an anti-cyclin D3 antibody or control IgG isotype. Proteins were immunoblotted as indicated. j, HCT-116 cells were infected with retroviruses expressing either FH-tagged cyclin D1(WT) or cyclin D1(T286A), and their extracts were used for immunoprecipitation with anti-CDK2 antibody or control IgG isotype. Proteins were immunoblotted as indicated. Unless otherwise noted, experiments were performed at least three independent times.
Extended Data Fig. 12 Loss of AMBRA1 desensitizes cells to CDK4/6 inhibitors.
a, HEK 293T cells were (co)transfected for 48 h with FFSS-tagged cyclin D2 or FFSS-tagged cyclin D3, HA-tagged CDK2, or FH-tagged empty vector, in the combinations indicated. After a double-immunoprecipitation, cyclin D–CDK2 complexes were incubated with GST–RB(773-CT) for 30 min with or without 100 nM, 250 nM or 500nM palbociclib, or 500 nM flavopiridol, before stopping the reaction with Laemmli buffer. Proteins were immunoblotted as indicated. b, HEK 293T cells were (co)transfected for 48 h with FFSS-tagged cyclin D1, HA-tagged CDK2, HA-tagged CDK4 or FH-tagged empty vector in the combinations indicated. After a double immunoprecipitation, the purified cyclin D1–CDK4 and cyclin D1–CDK2 complexes were incubated with GST–RB(773-CT) for 30 min with or without 100 nM palbociclib or 100 nM flavopiridol, before stopping the reaction with Laemmli buffer. Proteins were immunoblotted as indicated. c, HEK 293T cells were (co)transfected for 48 h with FFSS-tagged cyclin D3, HA-tagged CDK2, HA-tagged CDK4, or FH-tagged empty vector in the combinations indicated. After a double immunoprecipitation (anti-Flag immunoprecipitation, elution with 3×Flag peptide, then anti-HA immunoprecipitation), cyclin D3–CDK4 and cyclin D3–CDK2 complexes bound to the beads were incubated with GST–RB(773-CT) for 30 min with or without 100 nM, 250 nM or 500nM palbociclib, or 500 nM flavopiridol, before stopping the reaction with Laemmli buffer. Proteins were immunoblotted as indicated. d, Parental and AMBRA1−/− HCT-116 cells were transfected with a non-targeting siRNA or an siRNA against CDK2 for three rounds before treatment with various concentrations of palbociclib (left) or abemaciclib (right). Survival curves were generated using the AlamarBlue assay. Data are mean survival percentage ± s.d. (n = 3 biological replicates per group). The signal from each condition was normalized to an untreated control to adjust for any relative growth difference. e, Before treatment, cell extracts from d were immunoblotted as indicated. f, Working model: by modulating the levels of D-type cyclins, CRL4AMBRA1 controls the execution of cell-cycle progression, thus ensuring proper embryonic development and tumour suppression (top). Impairment of CRL4AMBRA1-mediated degradation of D-type cyclins (for example, alterations or downregulation of AMBRA1 or mutations in the TP motif of D-type cyclins) deregulates cell-cycle progression, and results in embryonic lethality, increased tumorigenic potential, and reduced sensitivity to CDK4/6 inhibitors (bottom). Unless otherwise noted, experiments were performed at least three independent times.
Supplementary information
Supplementary Figure 1
This file contains the full scanned images obtained by electrophoretic separation.
Supplementary Figures
This file contains the representative FACS gating strategy (Supplementary Figure 2), additional information on the identification and detection of abemaciclib by LC-MS/MS (Supplementary Figures 3-5) and the representative image of a stripped membrane for immunoblotting (Supplementary Figure 6).
Supplementary Table 1
The interactors of wild-type cyclin D1 (WT) or mutant cyclin D1(T286A) identified by LC-MS/MS and related to Fig. 1d. For each protein reported, the UniProt accession number is indicated in the first column. # Peptides = total number of PSMs, discounting duplicates. # PSM = total number of PSMs, including duplicate PSMs.
Supplementary Table 2
All cases of MPPH-derived mutations in CCND2 described in the literature55–60 or deposited in Decipher (https://decipher.sanger.ac.uk).
Supplementary Table 3
The mutations in the degron motif of CCND1, CCND2 and CCND3 gathered and combined from cBioPortal (curated set of non-redundant studies, https://www.cbioportal.org/)36,37, COSMIC (https://cancer.sanger.ac.uk/cosmic)38 and, and Schmitz et al. 39. “del” = deletion, “fs” = frameshift, “BL” = Burkitt’s lymphoma, “HIV+” = Human immunodeficiency virus positive, “ABC” = Activated B cell-like, “GCB” = Germinal center B cell-like, “DLBL” = Diffuse large B-cell lymphoma, “NOS” = Not otherwise specified, “AML” = Acute myeloid leukemia, “FL” = Follicular lymphoma. Note, some sample IDs refer to patient-derived cell lines.
Supplementary Table 4
Sequences of primers, siRNA oligos, and gRNAs used in this study. Where applicable, sources and catalog numbers are indicated.
Source data
Rights and permissions
About this article
Cite this article
Simoneschi, D., Rona, G., Zhou, N. et al. CRL4AMBRA1 is a master regulator of D-type cyclins. Nature 592, 789–793 (2021). https://doi.org/10.1038/s41586-021-03445-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-021-03445-y
This article is cited by
-
DCAF13 inhibits the p53 signaling pathway by promoting p53 ubiquitination modification in lung adenocarcinoma
Journal of Experimental & Clinical Cancer Research (2024)
-
AMBRA1 promotes intestinal inflammation by antagonizing PP4R1/PP4c mediated IKK dephosphorylation in an autophagy-independent manner
Cell Death & Differentiation (2024)
-
Reciprocal antagonism of PIN1-APC/CCDH1 governs mitotic protein stability and cell cycle entry
Nature Communications (2024)
-
Zebrafish ambra1b knockout reveals a novel role for Ambra1 in primordial germ cells survival, sex differentiation and reproduction
Biological Research (2023)
-
Leveraging the replication stress response to optimize cancer therapy
Nature Reviews Cancer (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.