Abstract
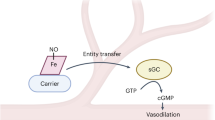
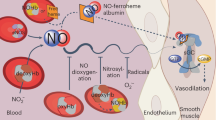
Singlet molecular oxygen (1O2) has well-established roles in photosynthetic plants, bacteria and fungi1,2,3, but not in mammals. Chemically generated 1O2 oxidizes the amino acid tryptophan to precursors of a key metabolite called N-formylkynurenine4, whereas enzymatic oxidation of tryptophan to N-formylkynurenine is catalysed by a family of dioxygenases, including indoleamine 2,3-dioxygenase 15. Under inflammatory conditions, this haem-containing enzyme is expressed in arterial endothelial cells, where it contributes to the regulation of blood pressure6. However, whether indoleamine 2,3-dioxygenase 1 forms 1O2 and whether this contributes to blood pressure control have remained unknown. Here we show that arterial indoleamine 2,3-dioxygenase 1 regulates blood pressure via formation of 1O2. We observed that in the presence of hydrogen peroxide, the enzyme generates 1O2 and that this is associated with the stereoselective oxidation of l-tryptophan to a tricyclic hydroperoxide via a previously unrecognized oxidative activation of the dioxygenase activity. The tryptophan-derived hydroperoxide acts in vivo as a signalling molecule, inducing arterial relaxation and decreasing blood pressure; this activity is dependent on Cys42 of protein kinase G1α. Our findings demonstrate a pathophysiological role for 1O2 in mammals through formation of an amino acid-derived hydroperoxide that regulates vascular tone and blood pressure under inflammatory conditions.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Triantaphylidès, C. & Havaux, M. Singlet oxygen in plants: production, detoxification and signaling. Trends Plant Sci. 14, 219–228 (2009).
Glaeser, J., Nuss, A. M., Berghoff, B. A. & Klug, G. Singlet oxygen stress in microorganisms. Adv. Microb. Physiol. 58, 141–173 (2011).
Beseli, A., Goulart da Silva, M. & Daub, M. E. The role of Cercospora zeae-maydis homologs of Rhodobacter sphaeroides 1O2-resistance genes in resistance to the photoactivated toxin cercosporin. FEMS Microbiol. Lett. 362, 1–7 (2015).
Ronsein, G. E., Oliveira, M. C., Miyamoto, S., Medeiros, M. H. G. & Di Mascio, P. Tryptophan oxidation by singlet molecular oxygen [O2(1∆g)]: mechanistic studies using 18O-labeled hydroperoxides, mass spectrometry, and light emission measurements. Chem. Res. Toxicol. 21, 1271–1283 (2008).
Efimov, I. et al. Structure and reaction mechanism in the heme dioxygenases. Biochemistry 50, 2717–2724 (2011).
Wang, Y. et al. Kynurenine is an endothelium-derived relaxing factor produced during inflammation. Nat. Med. 16, 279–285 (2010).
Ignarro, L. J., Cirino, G., Casini, A. & Napoli, C. Nitric oxide as a signaling molecule in the vascular system: an overview. J. Cardiovasc. Pharmacol. 34, 879–886 (1999).
Gómez-Jiménez, J. et al. l-arginine: nitric oxide pathway in endotoxemia and human septic shock. Crit. Care Med. 23, 253–258 (1995).
López, A. et al. Multiple-center, randomized, placebo-controlled, double-blind study of the nitric oxide synthase inhibitor 546C88: effect on survival in patients with septic shock. Crit. Care Med. 32, 21–30 (2004).
Bakker, J. et al. Administration of the nitric oxide synthase inhibitor NG-methyl-l-arginine hydrochloride (546C88) by intravenous infusion for up to 72 hours can promote the resolution of shock in patients with severe sepsis: results of a randomized, double-blind, placebo-controlled multicenter study (study no. 144–002). Crit. Care Med. 32, 1–12 (2004).
Sakakibara, K. et al. Kynurenine causes vasodilation and hypotension induced by activation of KCNQ-encoded voltage-dependent K+ channels. J. Pharmacol. Sci. 129, 31–37 (2015).
Fazio, F. et al. Vasorelaxing action of the kynurenine metabolite, xanthurenic acid: the missing link in endotoxin-induced hypotension? Front. Pharmacol. 8, 214 (2017).
Sanders, J., Peter, F., Scott, E., Saad, M. H. & Carr, R. H. Process for converting tryptophan into kynurenine. WO Patent 2009/135843 (2009).
Yamamoto, Y., Brodsky, M. H., Baker, J. C. & Ames, B. N. Detection and characterization of lipid hydroperoxides at picomole levels by high-performance liquid chromatography. Anal. Biochem. 160, 7–13 (1987).
Nakagawa, M. et al. Dye-sensitized photooxygenation of tryptophan: 3a-hydroperoxypyrroloindole as a labile precursor of formylkynurenine. Chem. Pharm. Bull. (Tokyo) 29, 1013–1026 (1981).
Mano, C. M. et al. Excited singlet molecular O2 (1∆g) is generated enzymatically from excited carbonyls in the dark. Sci. Rep. 4, 5938 (2014).
Taniguchi, T. et al. Indoleamine 2,3-dioxygenase. Kinetic studies on the binding of superoxide anion and molecular oxygen to the enzyme. J. Biol. Chem. 254, 3288–3294 (1979).
Ohnishi, T., Hirata, F. & Hayaishi, O. Indoleamine 2,3-dioxygenase. Potassium superoxide as substrate. J. Biol. Chem. 252, 4643–4647 (1977).
Shimizu, T., Nomiyama, S., Hirata, F. & Hayaishi, O. Indoleamine 2,3-dioxygenase. J. Biol. Chem. 253, 4700–4706 (1978).
Freewan, M. et al. Human indoleamine 2,3-dioxygenase is a catalyst of physiological heme peroxidase reactions: implications for the inhibition of dioxygenase activity by hydrogen peroxide. J. Biol. Chem. 288, 1548–1567 (2013).
Prendergast, G. C., Malachowski, W. P., DuHadaway, J. B. & Muller, A. J. Discovery of IDO1 inhibitors: from bench to bedside. Cancer Res. 77, 6795–6811 (2017).
Ogilby, P. R. Singlet oxygen: there is indeed something new under the sun. Chem. Soc. Rev. 39, 3181–3209 (2010).
Thomas, S. R. et al. Post-translational regulation of human indoleamine 2,3-dioxygenase activity by nitric oxide. J. Biol. Chem. 282, 23778–23787 (2007).
Iida, S., Ohkubo, Y., Yamamoto, Y. & Fujisawa, A. Parabanic acid is the singlet oxygen specific oxidation product of uric acid. J. Clin. Biochem. Nutr. 61, 169–175 (2017).
Kanofsky, J. R. Singlet oxygen production by biological systems. Chem. Biol. Interact. 70, 1–28 (1989).
Russell, G. A. Deuterium-isotope effects in the autoxidation of aralkyl hydrocarbons. Mechanism of the interaction of peroxy radicals. J. Am. Chem. Soc. 79, 3871–3877 (1957).
Burgoyne, J. R. et al. Cysteine redox sensor in PKGIα enables oxidant-induced activation. Science 317, 1393–1397 (2007).
Prysyazhna, O., Rudyk, O. & Eaton, P. Single atom substitution in mouse protein kinase G eliminates oxidant sensing to cause hypertension. Nat. Med. 18, 286–290 (2012).
Matoba, T. et al. Hydrogen peroxide is an endothelium-derived hyperpolarizing factor in mice. J. Clin. Invest. 106, 1521–1530 (2000).
Nakamura, T. et al. Prevention of PKG1α oxidation augments cardioprotection in the stressed heart. J. Clin. Invest. 125, 2468–2472 (2015).
Rudyk, O. et al. Protein kinase G oxidation is a major cause of injury during sepsis. Proc. Natl Acad. Sci. USA 110, 9909–9913 (2013).
Changsirivathanathamrong, D. et al. Tryptophan metabolism to kynurenine is a potential novel contributor to hypotension in human sepsis. Crit. Care Med. 39, 2678–2683 (2011).
Weishaupt, K. R., Gomer, C. J. & Dougherty, T. J. Identification of singlet oxygen as the cytotoxic agent in photoinactivation of a murine tumor. Cancer Res. 36, 2326–2329 (1976).
Munn, D. H. & Mellor, A. L. IDO in the tumor microenvironment: inflammation, counter-regulation, and tolerance. Trends Immunol. 37, 193–207 (2016).
Cheong, J. E. & Sun, L. Targeting the IDO1/TDO2–KYN–AhR pathway for cancer immunotherapy—challenges and opportunities. Trends Pharmacol. Sci. 39, 307–325 (2018).
Pantouris, G., Serys, M., Yuasa, H. J., Ball, H. J. & Mowat, C. G. Human indoleamine 2,3-dioxygenase-2 has substrate specificity and inhibition characteristics distinct from those of indoleamine 2,3-dioxygenase-1. Amino Acids 46, 2155–2163 (2014).
Anantharaman, A. et al. Studies on interaction of norbixin with DNA: multispectroscopic and in silico analysis. Spectrochim. Acta A Mol. Biomol. Spectrosc. 144, 163–169 (2015).
Tao, M. et al. Process for the synthesis of an indoleamine 2,3-dioxygenase inhibitor. WO/2015/070007 A1. International Application No.: PCT/US2014/064531 (2015).
Littlejohn, T. K. et al. Expression and purification of recombinant human indoleamine 2,3-dioxygenase. Protein Expr. Purif. 19, 22–29 (2000).
Terentis, A. C. et al. The heme environment of recombinant human indoleamine 2,3-dioxygenase. Structural properties and substrate-ligand interactions. J. Biol. Chem. 277, 15788–15794 (2002).
Littlejohn, T. K., Takikawa, O., Truscott, R. J. & Walker, M. J. Asp274 and His346 are essential for heme binding and catalytic function of human indoleamine 2,3-dioxygenase. J. Biol. Chem. 278, 29525–29531 (2003).
Hirata, F. & Hayaishi, O. Studies on indoleamine 2,3-dioxygenase. I. Superoxide anion as substrate. J. Biol. Chem. 250, 5960–5966 (1975).
Maghzal, G. J., Thomas, S. R., Hunt, N. H. & Stocker, R. Cytochrome b 5, not superoxide anion radical, is a major reductant of indoleamine 2,3-dioxygenase in human cells. J. Biol. Chem. 283, 12014–12025 (2008).
Maghzal, G. J. et al. Assessment of myeloperoxidase activity by the conversion of hydroethidine to 2-chloroethidium. J. Biol. Chem. 259, 5580–5595 (2014).
Sattler, W., Mohr, D. & Stocker, R. Rapid isolation of lipoproteins and assessment of their peroxidation by HPLC postcolumn chemiluminescence. Methods Enzymol. 233, 469–489 (1994).
Motterlini, R. et al. CORM-A1: a new pharmacologically active carbon monoxide-releasing molecule. FASEB J. 19, 284–286 (2005).
Martinez, G. R., Ravanat, J.-L., Medeiros, M. H. G., Cadet, J. & Di Mascio, P. Synthesis of a naphthalene endoperoxide as a source of 18O-labeled singlet oxygen for mechanistic studies. J. Am. Chem. Soc. 122, 10212–10213 (2000).
Miyamoto, S. et al. Direct evidence of singlet molecular oxygen generation from peroxynitrate, a decomposition product of peroxynitrite. Dalton Trans. 7, 5720–5729 (2009).
Scotcher, J. et al. Disulfide-activated protein kinase G Iα regulates cardiac diastolic relaxation and fine-tunes the Frank–Starling response. Nat. Commun. 7, 13187 (2016).
Mellor, A. L. et al. Cutting edge: induced indoleamine 2,3 dioxygenase expression in dendritic cell subsets suppresses T cell clonal expansion. J. Immunol. 171, 1652–1655 (2003).
Yang, H., Wang, H. & Jaenisch, R. Generating genetically modified mice using CRISPR/Cas-mediated genome engineering. Nat. Protoc. 9, 1956–1968 (2014).
Zhao, X. et al. Arterial pressure monitoring in mice. Curr. Protoc. Mouse Biol. 1, 105–122 (2011).
Krege, J. H., Hodgin, J. B., Hagaman, J. R. & Smithies, O. A noninvasive computerized tail-cuff system for measuring blood pressure in mice. Hypertension 25, 1111–1115 (1995).
Fenger-Gron, J., Mulvany, M. J. & Christensen, K. L. Mesenteric blood pressure profile of conscious, freely moving rats. J. Physiol. (Lond.) 488, 753–760 (1995).
Mulvany, M. J. & Halpern, W. Contractile properties of small arterial resistance vessels in spontaneously hypertensive and normotensive rats. Circ. Res. 41, 19–26 (1977).
Piantadosi, C. A. & Tatro, L. G. Regional H2O2 concentration in rat brain after hyperoxic convulsions. J. Appl. Physiol. 69, 1761–1766 (1990).
Pfaffl, M. W. A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res. 29, e45 (2001).
Sakash, J. B., Byrne, G. I., Lichtman, A. & Libby, P. Cytokines induce indoleamine 2,3-dioxygenase expression in human atheroma-associated cells: implications for persistent Chlamydophila pneumoniae infection. Infect. Immun. 70, 3959–3961 (2002).
Fu, R. et al. Enzyme reactivation by hydrogen peroxide in heme-based tryptophan dioxygenase. J. Biol. Chem. 286, 26541–26554 (2011).
Headlam, H. A. & Davies, M. J. Beta-scission of side-chain alkoxyl radicals on peptides and proteins results in the loss of side-chains as aldehydes and ketones. Free Radic. Biol. Med. 32, 1171–1184 (2002).
Lewis-Ballester, A. et al. Structural insights into substrate and inhibitor binding sites in human indoleamine 2,3-dioxygenase 1. Nat. Commun. 8, 1693 (2017).
Acknowledgements
We thank D. Cheng, S. Kong, D. Newington and J. Wu for their technical assistance in the project; N. Smith and R. M. Graham for advice on the TAC experiment; and R. M. Graham and C. C. Winterbourn for their critique of the manuscript. This work was funded by grants from the National Health and Medical Research Council of Australia (NHMRC): 1020400 to R.S. and R.J.P., and 1052616 to R.S. P.D.M. thanks FAPESP (Fundação de Amparo à Pesquisa do Estado de São Paulo, N°. 2012/12663-1, CEPID Redoxoma N°. 2013/07937-8), CNPq (Conselho Nacional para o Desenvolvimento Científico e Tecnológico, N°. 301307/2013-0), PRPUSP (Pró-Reitoria de Pesquisa da Universidade de São Paulo, NAP Redoxoma N°. 2011.1.9352.1.8) and John Simon Guggenheim Memorial Foundation (Fellowship) for financial support. R.S. is supported by NHMRC Senior Principal Research Fellowship 1111632. The work also received support from New South Wales Health.
Reviewer information
Nature thanks D. Gutterman, E. Raven and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
G.J.M., C.P.S. and R.S. designed the study. G.J.M., A.M.G., S.S., Y.Y., R.J.P. and R.S. designed and carried out the chemical characterization and urate oxidation experiments. N.N., J.O.O. and J.B.B. designed the synthesis and characterization of epacadostat. A.M.G. and C.S. purified cis-norbixin. G.J.M., P.D.M., A.A. S.S., F.M.P. and R.S. designed and carried out 1O2-detection experiments. C.P.S., G.J.M., A.A., J.T., P.E. and R.S. designed the studies with isolated enzymes. C.P.S., P.C., O.P., J.-P.S., Y.W., L.L.D. and R.S. designed and carried out arterial-relaxation studies. G.J.M. and R.S. designed and carried out the H2O2-detection experiments. G.J.M., A.A., J.T., S.S., O.P. and J.S. carried out and analysed the isolated-enzyme experiments. C.P.S. and K.W. carried out and analysed arterial PKG1α experiments. K.W. designed and carried out the vascular smooth muscle studies. C.P.S. and Y.W. carried out and analysed blood pressure experiments. Y.W., C.P.S., L.L.D. and R.S. designed and carried out the TAC and atherosclerosis studies. All authors interpreted data. C.P.S., G.J.M. and R.S. wrote the original manuscript and R.S. wrote the revised manuscript. All authors reviewed the revised manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Only peak 6 induces arterial relaxation in resistance and conduit arteries from different vascular beds and species.
a, Lack of relaxation of pre-constricted abdominal aortas from wild-type mice without (naive) and with IFN-γ pretreatment, and with intact (+EC) or denuded endothelium (−EC), in response to purified Kyn (n = 9) or NFK (n = 4). b, Representative myography traces of purified Trp-induced relaxation of IFN-γ-pretreated and noradrenaline (NA) pre-constricted abdominal arteries from: wild-type (Ido1+/+) mice without (top) and with the IDO1 inhibitor 1-l-methyltryptophan (1-L-MT) (middle); and Ido1−/− mice (bottom). c, Relaxation of noradrenaline pre-constricted abdominal aortas from Ido1+/+ or Ido1−/− (n = 6) mice in response to vehicle (open bars) or purified Trp (filled bars) ± 1-L-MT, with IDO1 expression induced ex vivo by IFN-γ-pretreatment or in vivo by LPS treatment of mice. d, Concentration-dependent arterial relaxation of noradrenaline pre-constricted, endothelium-denuded mouse abdominal aorta by purified peaks 1–6. e–i, Peak 6 concentration-dependent arterial relaxation in endothelium-denuded mouse (e), rat (f, g, h) and porcine (i) arteries pre-constricted with noradrenaline (e, f) or the thromboxane A2 receptor agonist U46619 (g, h, i). Data show mean ± s.e.m. of n = 18 and 6 (c, vehicle treatment for IFN-γ and LPS, respectively), n = 5 (c, Trp without IFN-γ), n = 10 and 6 (c, Trp addition for IFN-γ and LPS, respectively), n = 5 and 6 (c, Trp addition in presence of 1-MT for IFN-γ and LPS, respectively), n = 6 (c, Trp addition in Ido1−/− for IFN-γ and LPS, respectively) n = 4 (d–h) and n = 5 (i) independent experiments, with type and diameter range of the arteries indicated. Data shown in b are representative of the data shown in c.
Extended Data Fig. 2 Characterization of reaction products formed during 1O2-mediated oxidation of tryptophan.
a, LC–MS chromatogram of reaction products from the oxidation of l-tryptophan by Rose Bengal and O2 and light, showing molecular ions, [M + H]+ for peaks 1–8. b, MS/MS spectra of precursor ions with m/z ratio of 221 (peaks 2 and 4) and 237 (peaks 5 and 6). c, HPLC chromatograms of reaction products from l-tryptophan oxidation by Rose Bengal and O2 and light, showing retention times of peaks 1–6 monitored at 230 nm and their corresponding post-column chemiluminescence (CL) signals. d, HPLC-UV and chemiluminescence chromatograms of peaks 5 and 6 after their chemical reduction with sodium borohydride. Data shown are representative of six (a) and two independent experiments (b–d).
Extended Data Fig. 3 Identification of reaction products formed during 1O2-mediated oxidation of Trp.
a, Comparison of molecular ions and fragmentation pattern of peaks 2 and 4 with those of chemically reduced peaks 5 and 6. b, Comparison of 1H NMR spectra of peaks 2 and 4 (top) with those of chemically reduced peaks 5 and 6 (bottom). c, d, 1H NMR spectra of irradiated peak 2 (c) in CD3OD/D2O and peak 4 (d) in CD3OD (top spectra). The arrow indicates the spectral peak irradiated. The bottom spectra show the respective NOE differential spectra of the irradiated peak with the dashed oval indicating anti-phase NOE interaction. e, f, Structures of peak 2 (trans-WOH) and peak 4 (cis-WOH) showing irradiated proton H8a and indication of the NOE correlation. Data shown are representative of two (a, b) and one separate experiments (c, d).
Extended Data Fig. 4 Conversion of cis-WOOH to NFK.
a, Spectral changes during incubation of cis-WOOH in phosphate buffer at 37 °C measured in 15-min intervals. Arrows indicate increase (↑) and left shift (←) in absorbance, whereas the inset shows spectrum of authentic NFK. b, 1H NMR spectra of cis-WOOH in D2O and 25 °C recorded at 5 min (top) and 360 min (middle). Arrows indicate increases in spectral peaks at 4.1, 7.6, 7.9, 8.1 and 8.3 p.p.m. Bottom shows 1H NMR spectra of authentic NFK. c, Time-dependent loss of cis-WOOH and formation of NFK during incubation of cis-WOOH at 37 °C in the presence of DTPA, as assessed by LC–MS/MS. d, Light emission upon addition of cis-WOOH in D2O phosphate buffer at 72 °C (left), with corresponding chemiluminescence spectra (right). e, Proposed mechanism of formation of cis-WOOH from 1O2-mediated oxidation of Trp. Data shown are representative spectra of one (b, c) and two separate experiments (a, d).
Extended Data Fig. 5 Role of 1O2 in IDO1–H2O2-mediated oxidation of Trp to cis-WOOH and Trp-induced arterial relaxation.
a, LC–MS/MS analysis of cis-WOOH (circles) and trans-WOOH (squares) following exposure of Trp to Rose Bengal and O2 and light for the time indicated. b, Formation of cis- and trans-WOOH during oxidation of Trp by Rose Bengal and O2 and light (RB) and IDO1–H2O2. c, Inhibition of IDO1–H2O2-mediated cis-WOOH formation by different pharmacological IDO1 inhibitors (all tested at 1 mM), with results expressed as the percentage of cis-WOOH formed in presence versus absence of inhibitor (control). d, IDO1-mediated formation of Trp-derived metabolites with bolus addition of H2O2 in Ar or O2-flushed buffer. Metabolite yield is expressed as percentage of that observed in the reaction under air. e, Trp-induced relaxation of mouse abdominal aortas pretreated with mouse recombinant IFN-γ and vehicle (Ctrl), polyethylene glycol (PEG) or PEG-catalase (PEG-Cat). f, Fluorescence changes upon addition of H2O2 to SOSG in the presence of human serum albumin (HSA, red), or IDO1 without (green) and with Trp (black). g, LC–MS/MS chromatograms of the reaction mixture of IDO1 and EAS after incubation without (top) and with H2O2 (bottom). h, Fluorescence changes upon addition of H2O2 to SOSG in the presence of either IDO1 ± inactivated carbon monoxide-releasing molecule-A1 (iCORM-A1, green), IDO1 pretreated with CORM-A1 (red), urate (blue), or DEANO (black). i, NIR emission upon addition to H2O2 of IDO1 pretreated with CO gas. j, Formation of cis- and trans-WOOH during oxidation of Trp by horseradish peroxidase (HRP)–H2O2, myeloperoxidase (MPO)–H2O2 and purified IDO2–H2O2. k, Trp-induced relaxation of pre-constricted abdominal aortas from wild-type, Ido1−/− or Ido1−/−Ido2−/− mice. l, Effect of cis-norbixin (100 μM) on relaxation of IFN-γ-pretreated mouse abdominal aorta induced by Trp or the nitric oxide donor DEANO. In b, c and f, reactions were initiated by the addition of H2O2–Trp and the mixtures incubated for 5–15 min at 25 °C before products were quantified by LC–MS/MS. Data shown are mean ± s.e.m. of three (a–d, j, k, relaxation to DEANO in l) or five (e, relaxation to Trp in l) independent experiments, or representative data (f, h) of three independent experiments. Ep, epacadostat; NLG, NLG919; RB, Rose Bengal. *P = 0.05 compared with absence of inhibitor (c) or air control (d), one-tailed Mann–Whitney test. The specific P values indicated were derived using a one-sided Mann–Whitney (l) and a Kruskal–Wallis test with Dunn’s multiple comparison (e).
Extended Data Fig. 6 Mechanism of 1O2 formation by IDO1–H2O2.
Known mechanisms of 1O2 generation by dark reactions in biochemical systems involve superoxide radical anion, thiyl radicals, hypochlorite plus H2O2, energy transfer from excited triplet carbonyls, or peroxy radicals25. For all reactions, IDO1 (2 or 4 μM) was incubated for 5 min (h for 30 min) at 25 °C in the presence of 100 μM DTPA, 100 μM Trp and the scavengers and substrates indicated, with the reaction being initiated by addition of a 50-fold molar excess of H2O2. cis-WOOH was then quantified by LC–MS/MS. a, b, Lack of effect of Cu/Zn superoxide dismutase (SOD) and NEM on cis-WOOH formation by IDO1–H2O2, which suggests that superoxide and thiyl radicals are unlikely to be involved in 1O2 generation by IDO1–H2O2. Results in a are expressed as the percentage of cis-WOOH formed in the presence versus absence (control) of 100 U SOD, whereas in b the results are expressed as percentage of Trp converted to cis-WOOH. c, Lack of effect of IDO1–H2O2 on conversion of HE to 2-chloroethidium (2-Cl-E+) in PBS, as determined by LC–MS/MS, ruling out the involvement of hypochlorite. d, Scavengers of excited carbonyls (sorbate) modestly, and scavengers of oxygen-centred radicals (DMPO) substantially, attenuate formation of cis-WOOH by IDO1–H2O2. e, Support for the implied involvement of protein peroxy radicals by the formation of IDO1 fragments (double arrow) and dimers (arrow) upon reaction of IDO1 with H2O2 in the absence or presence of Trp or DMPO as assessed by SDS–PAGE under non-reducing conditions and visualization of proteins by silver stain. f, g, Formation of IDO1-associated dityrosine-specific fluorescence and IDO1 hydroperoxides during exposure of IDO1 to H2O2 in 100 mM phosphate buffer in the absence of Trp ± DMPO (f) or ± ascorbate (Asc, g). Reaction mixtures were subjected to size exclusion chromatography with HPLC–UV214 nm (left) and (f) fluorescence or (g) post-column chemiluminescence (CL) detection (right). Ascorbate was used as a reductant for protein hydroperoxides. h, IDO1–H2O2-mediated conversion of EAS (1 mM) to EAS endoperoxide (EAS-O2) in the absence and presence of DMPO. Inhibition of formation of dityrosine fluorescence and conversion of EAS to EAS-O2 by DMSO suggests59 that the reaction of IDO1 with H2O2 yields a porphyrin radical, which delocalizes to aromatic amino acid residues of IDO1, most probably a Tyr residue. The resulting amino acid-derived phenoxy radical may then engage in dityrosine formation, β-scission and/or fragmentation reactions, as well as formation of protein peroxy radicals (Extended Data Fig. 9a), in accordance with known chemistry60. Consistent with this possibility, reaction of IDO1 with H2O2 also generated protein carbonyls (i), the formation of which was inhibited by Trp and DMPO. Following reaction, IDO1 was denatured with 6% SDS in the presence of dinitrophenylhydrazine (DNPH) before protein was transferred onto nitrocellulose membrane, and carbonyls detected using anti-DNPH antibody. Qualitative data shown are representative of 2–3 separate experiments. Quantitative data shown are mean ± s.e.m. of three independent experiments. *P ≤ 0.05 (Mann–Whitney, one-sided) compared with absence of inhibitors (a, d).
Extended Data Fig. 7 Role of PKG1α in arterial relaxation by IDO1–cis-WOOH.
a, b Concentration–response curves to cis-WOOH after pretreatment of denuded mouse abdominal aortas with vehicle (filled squares) or the competitive cGMP PKG inhibitor RP-8-CPT-cGMP (a, open squares), or the competitive ATP binding PKG inhibitor KT 5283 (b, open squares). c, Relaxation of pre-constricted mouse mesenteric resistance arteries from LPS-treated wild-type (black) and PKG1α(C42S) knock-in mice (grey) by the nitric oxide donor DEANO (n = 4 for both genotypes). d, e, IDO activity in kidney homogenate (d) and plasma kynurenine-to-tryptophan ratio (as an index of systemic IDO activity) (e) obtained from wild-type (WT) or PKG1α(C42S) knock-in (KI) mice after treatment with LPS. f, Dimerization of PKG1α in human smooth muscle cells induced by Trp, 1 μM H2O2 or both, in the presence (+) or absence (–) of the IDO1 inhibitor epacadostat (n = 5). Cells were pretreated with (+) or without (–) 100 ng ml−1 rhIFN-γ for 72 h. Data show mean ± s.e.m. of 5 (a, f), 4 (b, c, e) or 3–4 (d) independent experiments. *P ≤ 0.05 using repeated measures two-way ANOVA with Šidák multiple comparison post hoc test (a–c), Kruskal–Wallis with Dunn’s test (f). NS, not significant (Mann–Whitney).
Extended Data Fig. 8 Role of IDO1 in pressure-overload related cardiac pathophysiology and experimental atherosclerosis.
a, Cardiac expression of Ido1 mRNA after sham and TAC for 21 days (n = 3 mice per treatment), with IFN-γ-treated hearts (n = 2 mice) as positive control. Inset, increase in ventricle weight-to-tibia length ratio as evidence for TAC-induced cardiac hypertrophy. b, c, IDO1 staining (brown colour) of (b) atherosclerotic lesions in thoracic aorta and (c) resistance vessel in kidney of Apoe−/− (top, representative of n = 1 and 4 mice for b and c, respectively) and Apoe−/−Ido1−/− mice (bottom, representative of n = 2 and 3 mice for b and c, respectively) after six months of Western diet. Middle panels represent rabbit negative immunoglobulin fraction control staining of (b) atherosclerotic lesions in thoracic aorta (representative of n = 1 mouse) and (c) resistance vessels in kidney (representative of n = 4 animals) of Apoe−/− mice after six months of Western diet. For each animal, sections were taken in duplicate. Magnification 60× (b) and 20× (c). Arrow heads (c) indicate microvessels. d, Plasma concentrations of Trp and Kyn in Apoe−/− and Apoe−/−Ido1−/− mice after six months of Western diet with n indicating the number of animals used. e, Trp-induced relaxation of pre-constricted, atherosclerotic lesion-containing aortic rings isolated from Apoe−/− and Apoe−/−Ido1−/− mice in the presence or absence of IDO1 inhibitor 1-MT after six months of Western diet with individual data points reflecting the number of animals used for each treatment. f, Systolic blood pressure (SBP) of Apoe−/− and Apoe−/−Ido1−/− mice before (−) and after (+) administration of 1-D-MT (n = 6 animals for each group). The specific P values indicated were derived from a two-tailed Mann Whitney (d) and Kruskal–Wallis test with Dunn’s multiple comparisons (e, f).
Extended Data Fig. 9 Proposed mechanism for formation of 1O2 by IDO1 plus H2O2 and chemical synthesis of epacadostat.
a, Proposed mechanism for formation of 1O2 by IDO1 plus H2O2. Reaction of Fe3+-haem IDO1 with H2O2 results in formation of the two-electron oxidized form, compound I, consisting of a Fe4+=O iron centre and a porphyrin cation radical (not shown). The latter is transferred to an amino acid side chain of IDO1, such as Trp (not shown) or—more likely—a Tyr such as Y126 or Y353, which are close to the active-site haem in IDO161. The IDO1 tyrosyl radical may then engage in the formation of fluorescent di-tyrosine crosslinks or H-abstraction reactions leading to protein fragmentation according to established pathways60. Alternatively, a resonance form of the IDO1 tyrosyl radical may add to molecular oxygen, resulting in the formation of a quinone peroxy radical at the para position (for example, shown on R1-Tyr-R2) or the ortho position (for example, shown on R6-Tyr-R7). The resulting intermediate quinone peroxy radical may then participate in inter- or intra-residue peroxy radical combination, the latter subsequent to additional H-abstraction and oxidation reactions and formation of a putative intra-residue di-peroxy radical. For inter-residue peroxy radical combination to occur, it is hypothesized that the haem of IDO1 catalyses the decomposition of the hydroperoxide to an alkoxy radical. In the scheme, this reaction is combined with oxygen addition to the alpha carbon radical. The resulting tetroxides will decay with release of 1O2 according to the Russell mechanism26. The observed stereospecific formation of cis-WOOH by IDO1–H2O2–l-Trp suggests formation of 1O2 close to the active site haem rather than release into the bulk phase, and may therefore be more consistent with the intra-residue peroxy radical combination pathway. For clarity, the R1–R7 labels represent the continuation of the peptide backbone. In the case of the inter-residue peroxy radical combination, it is envisioned that peroxy radicals on two different Tyr residues within the same IDO1 molecule combine. b, Chemical synthesis of epacadostat.
Supplementary information
Rights and permissions
About this article
Cite this article
Stanley, C.P., Maghzal, G.J., Ayer, A. et al. Singlet molecular oxygen regulates vascular tone and blood pressure in inflammation. Nature 566, 548–552 (2019). https://doi.org/10.1038/s41586-019-0947-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-019-0947-3
This article is cited by
-
A photothermal-response oxygen release platform based on a hydrogel for accelerating wound healing
NPG Asia Materials (2023)
-
Hydrogen peroxide signaling via its transformation to a stereospecific alkyl hydroperoxide that escapes reductive inactivation
Nature Communications (2021)
-
Preparation, validation and use of a vasoactive tryptophan-derived hydroperoxide and relevant control compounds
Nature Protocols (2021)
-
Redox control in the pathophysiology of influenza virus infection
BMC Microbiology (2020)
-
Photochemical upconversion of near-infrared light from below the silicon bandgap
Nature Photonics (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.