Abstract
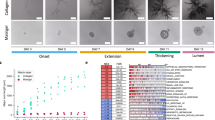
Tubular epithelia are a basic building block of organs and a common site of cancer occurrence1,2,3,4. During tumorigenesis, transformed cells overproliferate and epithelial architecture is disrupted. However, the biophysical parameters that underlie the adoption of abnormal tumour tissue shapes are unknown. Here we show in the pancreas of mice that the morphology of epithelial tumours is determined by the interplay of cytoskeletal changes in transformed cells and the existing tubular geometry. To analyse the morphological changes in tissue architecture during the initiation of cancer, we developed a three-dimensional whole-organ imaging technique that enables tissue analysis at single-cell resolution. Oncogenic transformation of pancreatic ducts led to two types of neoplastic growth: exophytic lesions that expanded outwards from the duct and endophytic lesions that grew inwards to the ductal lumen. Myosin activity was higher apically than basally in wild-type cells, but upon transformation this gradient was lost in both lesion types. Three-dimensional vertex model simulations and a continuum theory of epithelial mechanics, which incorporate the cytoskeletal changes observed in transformed cells, indicated that the diameter of the source epithelium instructs the morphology of growing tumours. Three-dimensional imaging revealed that—consistent with theory predictions—small pancreatic ducts produced exophytic growth, whereas large ducts deformed endophytically. Similar patterns of lesion growth were observed in tubular epithelia of the liver and lung; this finding identifies tension imbalance and tissue curvature as fundamental determinants of epithelial tumorigenesis.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
All relevant data and protocols are included within the paper, Extended Data and Supplementary Information. Source Data for Figs. 1d, f, 2i–k, m, 3d, 4a, b, d and Extended Data Figs. 1d, f, 2b, 5e, 6b–g, i–l, 7d, f, i, j, m, n, 8a–d, f, h, 10e, f are provided with this paper. The original datasets and resulting analyses, as well as methodological details, are available from the corresponding authors upon reasonable request.
References
Bailey, J. M. et al. p53 mutations cooperate with oncogenic Kras to promote adenocarcinoma from pancreatic ductal cells. Oncogene 35, 4282–4288 (2016).
Ferreira, R. M. M. et al. Duct- and acinar-derived pancreatic ductal adenocarcinomas show distinct tumor progression and marker expression. Cell Reports 21, 966–978 (2017).
Ferone, G. et al. SOX2 is the determining oncogenic switch in promoting lung squamous cell carcinoma from different cells of origin. Cancer Cell 30, 519–532 (2016).
Guest, R. V. et al. Cell lineage tracing reveals a biliary origin of intrahepatic cholangiocarcinoma. Cancer Res. 74, 1005–1010 (2014).
Paszek, M. J. et al. Tensional homeostasis and the malignant phenotype. Cancer Cell 8, 241–254 (2005
Zhang, Q. et al. Fbxw7 deletion accelerates Kras G12D-driven pancreatic tumorigenesis via Yap accumulation. Neoplasia 18, 666–673 (2016).
Rhim, A. D. et al. EMT and dissemination precede pancreatic tumor formation. Cell 148, 349–361 (2012).
Hanahan, D. & Coussens, L. M. Accessories to the crime: functions of cells recruited to the tumor microenvironment. Cancer Cell 21, 309–322 (2012).
Öhlund, D. et al. Distinct populations of inflammatory fibroblasts and myofibroblasts in pancreatic cancer. J. Exp. Med. 214, 579–596 (2017).
Heer, N. C. & Martin, A. C. Tension, contraction and tissue morphogenesis. Development 144, 4249–4260 (2017).
Goeckeler, Z. M. & Wysolmerski, R. B. Myosin light chain kinase-regulated endothelial cell contraction: the relationship between isometric tension, actin polymerization, and myosin phosphorylation. J. Cell Biol. 130, 613–627 (1995).
Elliott, H. et al. Myosin II controls cellular branching morphogenesis and migration in three dimensions by minimizing cell-surface curvature. Nat. Cell Biol. 17, 137–147 (2015).
Lomakin, A. J. et al. Competition for actin between two distinct F-actin networks defines a bistable switch for cell polarization. Nat. Cell Biol. 17, 1435–1445 (2015).
Heid, I. et al. Early requirement of Rac1 in a mouse model of pancreatic cancer. Gastroenterology 141, 719–730.e7 (2011).
Baer, R. et al. Pancreatic cell plasticity and cancer initiation induced by oncogenic Kras is completely dependent on wild-type PI 3-kinase p110α. Genes Dev. 28, 2621–2635 (2014).
Pickup, M. W., Mouw, J. K. & Weaver, V. M. The extracellular matrix modulates the hallmarks of cancer. EMBO Rep. 15, 1243–1253 (2014).
Schäfer, C. et al. Differential KrasV12 protein levels control a switch regulating lung cancer cell morphology and motility. Converg. Sci. Phys. Oncol. 2, 035004 (2016).
Magudia, K., Lahoz, A. & Hall, A. K-Ras and B-Raf oncogenes inhibit colon epithelial polarity establishment through up-regulation of c-myc. J. Cell Biol. 198, 185–194 (2012).
Mendoza, M. C., Vilela, M., Juarez, J. E., Blenis, J. & Danuser, G. ERK reinforces actin polymerization to power persistent edge protrusion during motility. Sci. Signal. 8, ra47 (2015).
Nguyen, D. H. D. et al. Myosin light chain kinase functions downstream of Ras/ERK to promote migration of urokinase-type plasminogen activator-stimulated cells in an integrin-selective manner. J. Cell Biol. 146, 149–164 (1999).
Shen, Q., Rigor, R. R., Pivetti, C. D., Wu, M. H. & Yuan, S. Y. Myosin light chain kinase in microvascular endothelial barrier function. Cardiovasc. Res. 87, 272–280 (2010).
Bielmeier, C. et al. Interface contractility between differently fated cells drives cell elimination and cyst formation. Curr. Biol. 26, 563–574 (2016).
Alt, S., Ganguly, P. & Salbreux, G. Vertex models: from cell mechanics to tissue morphogenesis. Phil. Trans. R. Soc. Lond. B 372, 20150520 (2017).
Clark, A. G., Wartlick, O., Salbreux, G. & Paluch, E. K. Stresses at the cell surface during animal cell morphogenesis. Curr. Biol. 24, R484–R494 (2014).
Sancho, R., Gruber, R., Gu, G. & Behrens, A. Loss of Fbw7 reprograms adult pancreatic ductal cells into α, δ, and β cells. Cell Stem Cell 15, 139–153 (2014).
Reichert, M. & Rustgi, A. K. Pancreatic ductal cells in development, regeneration, and neoplasia. J. Clin. Invest. 121, 4572–4578 (2011).
Marchetti, M. C. et al. Hydrodynamics of soft active matter. Rev. Mod. Phys. 85, 1143–1189 (2013).
Prost, J., Jülicher, F. & Joanny, J. F. Active gel physics. Nat. Phys. 11, 111–117 (2015).
Salbreux, G. & Jülicher, F. Mechanics of active surfaces. Phys. Rev. E 96, 032404 (2017).
Means, A. L., Xu, Y., Zhao, A., Ray, K. C. & Gu, G. CK19CreERT knockin mouse line allows for conditional DNA recombination in epithelial cells in multiple endodermal organs. Genesis 46, 318–323 (2008).
Desai, B. M. et al. Preexisting pancreatic acinar cells contribute to acinar cell, but not islet β cell, regeneration. J. Clin. Invest. 117, 971–977 (2007).
Solar, M. et al. Pancreatic exocrine duct cells give rise to insulin-producing β cells during embryogenesis but not after birth. Dev. Cell 17, 849–860 (2009).
Hingorani, S. R. et al. Preinvasive and invasive ductal pancreatic cancer and its early detection in the mouse. Cancer Cell 4, 437–450 (2003).
Pan, F. C. et al. Spatiotemporal patterns of multipotentiality in Ptf1a-expressing cells during pancreas organogenesis and injury-induced facultative restoration. Development 140, 751–764 (2013).
Jackson, E. L. et al. Analysis of lung tumor initiation and progression using conditional expression of oncogenic K-ras. Genes Dev. 15, 3243–3248 (2001).
Hoeck, J. D. et al. Fbw7 controls neural stem cell differentiation and progenitor apoptosis via Notch and c-Jun. Nat. Neurosci. 13, 1365–1372 (2010).
Hara, M. et al. Transgenic mice with green fluorescent protein-labeled pancreatic β-cells. Am. J. Physiol. Endocrinol. Metab. 284, E177–E183 (2003).
Marino, S., Vooijs, M., van Der Gulden, H., Jonkers, J. & Berns, A. Induction of medulloblastomas in p53-null mutant mice by somatic inactivation of Rb in the external granular layer cells of the cerebellum. Genes Dev. 14, 994–1004 (2000).
Snippert, H. J. et al. Intestinal crypt homeostasis results from neutral competition between symmetrically dividing Lgr5 stem cells. Cell 143, 134–144 (2010).
Madisen, L. et al. A robust and high-throughput Cre reporting and characterization system for the whole mouse brain. Nat. Neurosci. 13, 133–140 (2010).
Srinivas, S. et al. Cre reporter strains produced by targeted insertion of EYFP and ECFP into the ROSA26 locus. BMC Dev. Biol. 1, 4 (2001).
Huch, M. et al. Unlimited in vitro expansion of adult bi-potent pancreas progenitors through the Lgr5/R-spondin axis. EMBO J. 32, 2708–2721 (2013).
Boj, S. F. et al. Organoid models of human and mouse ductal pancreatic cancer. Cell 160, 324–338 (2015).
Acknowledgements
We thank C. Cremona, V. Gebala, M. Popovic, N. Tapon and B. Thompson for comments on the manuscript, and the Francis Crick Institute Biological Research, Experimental Histopathology and Light Microscopy facilities for technical support. This work was supported by the Francis Crick Institute, which receives its core funding from Cancer Research UK (FC001039, FC001317), the UK Medical Research Council (FC001039, FC001317) and the Wellcome Trust (FC001039, FC001317). This work was also supported by an ERC grant to A.B. (281661).
Reviewer information
Nature thanks G. Danuser, N. Minc and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
R.M.M.F., C.G. and V.M.-Y.W. contributed equally to this work. H.A.M., S.A., G.S. and A.B. conceived and designed the study. H.A.M. performed the experiments and analyses. C.G. and V.M.-Y.W. helped with organoid experiments. S.A. performed and analysed simulations, and G.S. analysed the continuum theory. R.M.M.F. assisted with study design and interpretation of data. C.G.C. assisted with lesion identification and description. G.S. and A.B. supervised the study. All authors discussed and interpreted the results and participated in writing the manuscript.
Corresponding authors
Ethics declarations
Competing interests
H.A.M. and A.B. are inventors on a UK patent application (1818567.8) relating to a solution for the preparation of samples for 3D imaging.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Preserved organ integrity after FLASH.
a, FLASH staining of an insulin (Ins)–GFP reporter mouse for amylase (Amy), Krt19 and Ins–GFP. Left, 3D reconstruction that demonstrates the complex organization of islets and pancreatic ducts. Scale bar, 100 μm. Right panels show an optical section through the area indicated in the left panel (white dotted rectangle), showing preserved compartmentalization into exocrine and endocrine glands as seen by mutually exclusive staining for Amy, Krt19 and Ins–GFP. Scale bars, 50 μm. Representative of five mice. b, Three-dimensional view of a high-calibre duct (32-μm diameter) stained for Krt19 and DNA, demonstrating preserved epithelial integrity. Scale bar, 50 μm. b′, Left, optical section through the indicated area in b (red dashed rectangle), demonstrating the continuous duct-cell monolayer and preserved duct lumen. Scale bar, 30 μm. Representative of six mice. Right, staining for Krt19 and DNA on a 4-μm tissue section of paraffin-embedded pancreas. Scale bar, 30 μm. c, FLASH staining for tdTomato (tdTOM) and Krt19 on pancreata of Rosa26CAG-tdTomato;Hnf1bcreERT2 mice without (left) and with (right) intraperitoneal injection of 100 μg tamoxifen per gram bodyweight. Scale bars, 500 μm. Representative of three mice. d, Arborization of the ductal tree. Each dot represents one duct and lines indicate ramification. For three Krt19-stained pancreata, z-stacks of at least 30 random high-magnification views were taken. Per view, the largest duct was identified and diameters were measured for four subsequent branching ducts to categorize the mode of arborization. For ducts with more than one furcation, the sequence was continued with the biggest duct ramifying from it. Terminal duct cells were assigned a duct diameter of 0 μm to indicate ending of the ductal tree. e, Cell division direction was measured on two-cell clones from tamoxifen-treated Rosa26LSL-Confetti;Hnf1bcreERT2 mice as the angle determined with respect to the line connecting both nuclei and the directionality of the duct (n = 263 clones, 5 mice). f, Direction of cell division and cell aspect ratio in ducts of varying diameter. Solid lines represent exponential fits. Cell division, n = 263 clones, 5 mice; aspect ratio, n = 120 ducts, 7 mice.
Extended Data Fig. 2 Exophytic and endophytic neoplasia in KrasG12D;Fbw7flox/flox model.
a, KFCk19 mouse model for tumour induction in the ductal epithelium triggered by Fbw7 exon deletion and KrasG12D activation. b, Recombination efficiency of low-dose tamoxifen injection and number of transformed clones per number of recombined cells per duct were quantified one week after tamoxifen injection in KFCk19 mice. EYFP-traced Krt19+ cells were quantified per duct, and total number of duct cells was estimated by dividing the duct length by the average cell length measured for this duct and multiplying this by the average number of circumscribing cells for this duct. Transformed clones were recognized as groups of more than three EYFP-traced cells sharing an interface. One dot represents one duct (112 ducts, 3 mice). c, d, KFH mouse model for alternative targeting of pancreatic ducts. d, Left, 3D rendering of exophytic neoplasia (top) and endophytic neoplasia (bottom) of KFH mice. Staining for Krt19 and tdTomato. Scale bars, 100 μm. Right, H & E staining for KFH exophytic (top) and endophytic (bottom) lesions. Scale bars, 100 μm. Representative of four mice. e, H & E and Alcian blue–periodic acid Schiff (AB/PAS) staining for exophytic and endophytic lesions in KFCk19 mice, demonstrating non-mucinous character typical of duct-derived neoplasia2. Scale bars, 100 μm. Representative of three mice. f, Experimental strategy for visualizing the connection of exophytic neoplasia with the ductal tree. The extrahepatic bile duct was cannulated at the ampulla, and the pancreas ductal tree perfused with 50 μl FITC-labelled dextran (DexFITC). g, Uptake of FITC-labelled dextran by an exophytic KFCk19 lesion, demonstrating lesion connection to the ductal system. Left, 3D view; right, optical section. Scale bars, 50 μm. Representative of four mice.
Extended Data Fig. 3 Morphology progression of acinar-derived neoplasia.
a, Schematic illustrating genetic strategy for acinar cell transformation by KrasG12D activation with concomitant p53flox/flox or Fbw7 flox/flox deletion, using Ela1–CreERT or Ptf1a–ERT2 drivers. b, c, KrasG12D;Fbw7 flox/flox;Ela1creERT (KFEla1) mice. b, Three-dimensional view of acinar-to-ductal metaplasia, as identified by local upregulation of Krt19 expression in acinar cells. tdTomato-traced acini connected to a terminal duct are shown. Arrowhead demarcates Krt19 expression by the middle acinus, forming a small ring of acinar-derived tdTomato-traced Krt19+ cells. Scale bar, 50 μm. Representative of three mice. c, Three-dimensional projection of a globular KFEla1 lesion in contact with a small-calibre duct (dotted line). Scale bar, 20 μm. c′, Optical sections of the lesion shown in c, demonstrating tdTomato tracing (top) and globular morphology (bottom). Scale bars, 20 μm. Representative of three mice. d–g, KrasG12D; p53flox/flox;Ela1creERT mice (KPEla1 mice). d, Three-dimensional view of a globular tdTomato-traced KPEla1 lesion connected to a terminal duct (arrowhead). Scale bar, 50 μm. Representative of four mice. e, Three-dimensional projection of a large KPEla1 lesion, showing the central grape-like morphology of back-to-back globular structures and the maintained connection to several small-calibre ducts (arrowheads) at the lesion edge. Scale bar, 200 μm. e′, Higher magnification of area indicated in e (white dotted rectangle), demonstrating the seamless connection of acinar-derived Krt19+ cells and wild-type ductal epithelium (dotted lines). Scale bar, 30 μm. Representative of four mice. f, Retrograde perfusion of the ductal tree with FITC-labelled dextran, as in Extended Data Fig. 2f, demonstrating direct connection of acinar-derived lesions to the ductal system. Three-dimensional view of a KPEla1 lesion. Scale bar, 50 μm. Representative of three mice. g, H & E staining of a KPEla1 lesion demonstrating globular morphology. Scale bar, 100 μm. Representative of six mice. h, KrasG12D;p53flox/flox;Ptf1acreERT2 (KPPtf1a) mice. H & E staining, demonstrating globular morphology of lesions. Scale bar, 100 μm. Representative of five mice.
Extended Data Fig. 4 Exophytic and endophytic neoplasia in KrasG12D;p53flox/flox models and in human pancreas.
a–c, Endophytic and exophytic lesions induced by p53 deletion with KrasG12D activation upon Pdx1–Cre-induced whole-pancreatic recombination (in KPC mice). b, Three-dimensional view of a pancreatic region of a three-week old mouse with endophytic (rectangle labelled 1) and exophytic (rectangle labelled 2) deformations. Scale bar, 150 μm. Panels labelled 1 and 2 provide higher-magnification images of the indicated areas in b. Scale bars, 50 μm. In panel 1, arrowheads demarcate invaginations typical of endophytic growth. In panel 2, a dotted line marks a morphologically normal small-calibre duct in contact with a globular, exophytic lesion. Representative of six mice. c, H & E staining for exophytic (left) and endophytic (right) lesions in the KPC model. Scale bars, 100 μm. Representative of six mice. d, e, Exophytic and endophytic lesions induced by p53 deletion with KrasG12D activation in pancreatic ducts (KPCk19 mice). e, Three-dimensional projection of exophytic (left) and endophytic (right) lesion shapes in KPCk19 mice. Scale bars, 100 μm. Representative of three mice. f, H & E staining of tissue sections from background pancreas of a patient presenting with pancreatic ductal adenocarcinoma. Left, exophytic lesion. Right, endophytic lesion. Scale bars, 100 μm. Representative of four patients.
Extended Data Fig. 5 Characterization of exophytic and endophytic neoplasia biology.
a, Proliferation of exophytic and endophytic lesions of KFCk19 mice as indicated by Ki67 staining. Scale bar, 100 μm. Representative of three mice. b, Stromal composition of KFCk19 exophytic and endophytic lesions, three weeks after recombination and recruitment of cancer-associated fibroblasts as demonstrated by staining for Pdgfrβ, nestin and smooth muscle actin (SMA). For staining comparisons between endophytic and exophytic lesions, lesions in the same tissue section are shown. Scale bars, 100 μm. Insets show magnified views of the area indicated in the main panel. Scale bars, 10 μm. Representative of four mice. c, Staining for human cancer-associated fibroblast markers PDGFRβ and SMA in background pancreatic tissue of a patient with pancreatic ductal adenocarcinoma. Examples of a non-dysplastic duct, an exophytic lesion and an endophytic lesion from the same tissue section are shown. Scale bars, 100 μm. Insets show magnified views of the area indicated in the main panel. Scale bars, 20 μm. One patient. d, Tumour cell epithelial-to-mesenchymal transition in advanced KFCk19 exophytic and endophytic lesions, eight weeks after recombination. Scale bars, 50 μm. Indicated areas are magnified on the right. Scale bars, 15 μm. Cdh1 staining marks epithelial cells, vimentin (Vim) staining indicates mesenchymal character and tdTomato identifies tumour-traced cells. Representative of three mice. e, Quantification of epithelial-to-mesenchymal transition in d as the number of tdTomato-traced, Cdh1−, Vim+ cells per lesion area. Exophytic, n = 29 lesions; endophytic n = 26 lesions. Data are mean ± s.d., ∗∗∗∗P < 0.0001 (two-sided Mann–Whitney test).
Extended Data Fig. 6 Cortical alterations in transformed cells.
a, Schematic showing cell orientation and cell cortex organization. b, Scatter plot of apical–basal pMLC2 intensities per cell, from endophytic and exophytic lesions in KFCk19 mice. Wild type, 106 cells; transformed, 124 cells. c, Basal and apical pMLC2 intensities were extracted from the maxima of the intensity profiles of each cell from exophytic lesions (Fig. 2i) (wild type, 35 cells; transformed, 45 cells). Data are mean ± s.d. NS, not significant (P = 0.057), ∗∗∗∗P < 0.0001 (two-sided Mann–Whitney test). d, Ratio of apical to basal pMLC2 intensity in late-stage exophytic and endophytic lesions, eight weeks after recombination (in KFCk19 mice). Endophytic, 110 cells; exophytic, 138 cells. Data are mean ± s.d. NS, not significant (P = 0.9538) (two-sided Mann–Whitney test). e, MLC2 distribution in transformed and wild-type cells of KFCk19 mice. Left, immunofluorescence staining for MLC2, Cdh1 and EYFP. Scale bar, 10 μm. Right, Ratio of apical to basal MLC2 intensity. Wild type, 119 cells; transformed, 139 cells. Data are mean ± s.d., NS, not significant, P = 0.7722 (two-sided Mann–Whitney test). f, Cortactin distribution in transformed and wild-type cells of KFCk19 mice. Left, immunofluorescence staining for cortactin, Cdh1 and EYFP. Scale bar, 10 μm. Right, ratio of apical to basal cortactin intensity. Wild type, 152 cells; transformed, 137 cells. Data are mean ± s.d. ∗∗∗∗P < 0.0001 (two-sided Mann–Whitney test). g, pMLC2 distribution in the KPC model. Left, immunofluorescence staining for pMLC2 and Krt19. Scale bar, 10 μm. Right, Basal–apical pMLC2 intensity profile, measured as shown in Fig. 2h. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. (157 cells). h, F-actin distribution in the KPC model. Immunofluorescence staining for F-actin (phalloidin) and Cdh1 on cryo-sectioned pancreata from KPC mice or wild-type littermates. Scale bar, 10 μm. Quantifications are shown in Fig. 2k. Wild type, 4 mice; transformed, 3 mice. i, j, pMLC2 distribution in the KPPtf1a model of acinar cell transformation. i, Immunofluorescence staining for pMLC2, Krt19 and tdTomato. Scale bars, 10 μm. Left, normal duct; middle, normal Krt19-negative acinus; right, transformed Krt19-positive tdTomato-traced cells. Asterisk indicates lumen. Representative of three mice. j, Basal–apical pMLC2 intensity profiles, measured as shown in Fig. 2h. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. (normal duct, 142 cells; normal acinus, 76 cells; transformed, 127 cells). k, Ratio of apical to basal F-actin, phosphorylated focal adhesion kinase (pFAK) and vinculin (Vnc) intensities in wild-type and transformed cells of KFCk19 mice. F-actin, 57 wild-type cells, 93 transformed cells; Vnc, 42 wild-type cells, 42 transformed cells; pFAK, 36 wild-type cells, 36 transformed cells. Data are mean ± s.d. ∗∗∗∗P < 0.0001 (two-sided Mann–Whitney test). l, Expression of integrins in transformed cells relative to wild-type duct-cell neighbours in KFCk19 mice. Itga2, 57 wild-type cells, 57 transformed cells; Itga6, 33 wild-type cells, 33 transformed cells; Itgb1, 30 wild-type cells, 30 transformed cells. Data are mean ± s.d. ∗∗∗∗P < 0.0001 (two-sided Mann–Whitney test).
Extended Data Fig. 7 Role of oncogenic Kras signalling in the pMLC2 distribution of transformed epithelial cells.
a–d, pMLC2 distribution in wild-type organoids after phosphatase inhibition. a–c, Immunostaining for pMLC2 and Cdh1. Scale bars, 10 μm. Representative of two experiments with three wild-type organoid lines. a, DMSO control. b, 2 μM okadaic acid treatment. c, 5 μM tautomycetin treatment. d, Ratio of apical to basal pMLC2 intensity of wild-type organoids after treatment with DMSO, okadaic acid (OA) or tautomycetin (TM). DMSO, 104 cells; okadaic acid, 70 cells; tautomycetin, 131 cells. Data are mean ± s.d. ∗∗∗∗P < 0.0001 (two-sided Mann–Whitney test). e, pMLC2 distribution in KC mice. Immunostaining for pMLC2 and Cdh1. Scale bar, 10 μm. Representative of two mice. f, Basal–apical pMLC2 intensity profile of KC cells (e), measured as shown in Fig. 2h. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. of 219 cells. g–j, pMLC2 distribution in KPC organoids after MEK inhibition. g, h, Immunostaining for pMLC2 and Cdh1. Scale bars, 20 μm. Representative of three experiments with three KPC organoid lines. g, DMSO control. h, 8 μM U0126 treatment. i, Basal–apical pMLC2 intensity profiles of DMSO or U0126-treated organoids, measured as shown in Fig. 2h. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. (DMSO, 105 cells; U0126, 133 cells). j, Ratio of apical to basal pMLC2 intensity of KPC organoids after DMSO or U0126 treatment. DMSO, 105 cells; U0126, 133 cells. Data are mean ± s.d. ∗∗∗∗P < 0.0001 (two-sided Mann–Whitney test). k, l, Immunostaining for pMLC2 and Cdh1. Scale bars, 20 μm. k, DMSO control. l, 5 μM ROCK inhibitor (H1152) treatment. Representative of two experiments with three KPC organoid lines. m, Basal–apical pMLC2 intensity profiles of DMSO- or H1152-treated organoids, measured as shown in Fig. 2h. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. (DMSO, 59 cells; H1152, 38 cells). n, Ratio of apical to basal pMLC2 intensity of KPC organoids after DMSO or H1152 treatment. DMSO, 60 cells; H1152, 37 cells. Data are mean ± s.d. NS, not significant, P = 0.5517 (two-sided Mann–Whitney test).
Extended Data Fig. 8 Formulation of ductal transformation in the 3D vertex model and the effect of tension change.
a, Number of circumscribing cells per duct diameter (113 ducts, 8 mice). b, Relative deformation as a function of diameter (mean ± s.e.m. from n = 10 simulations), for simulations with tension changes derived from exophytic (pink) and endophytic lesions (green). Both inputs produce deformations in good agreement with experimental observations (blue). c, Simulation of hyperproliferation without mechanical changes is not sufficient to explain the transition between exophytic and endophytic lesions (dots indicate mean ± s.e.m. from n = 10 simulations). Experimental data from Fig. 3d are shown for comparison. Simulations were carried out as in Fig. 3d, except that mechanical parameters in transformed cells were not modified. d, Classification accuracy, defined as the fraction of exophytic and endophytic lesions that can be predicted on the basis of duct diameter, as a function of duct diameter. The accuracy is defined for each diameter (d) as (TP + TN)/(TP + FP + TN + FN), in which TP (true positive) and FP (false positive) denote the number of exophytic and endophytic deformations occurring below diameter d, and TN (true negative) and FN (false negative) denote the number of endophytic and exophytic deformations occurring above diameter d. The diameter of maximal accuracy at three weeks is used to find the location of the transition. e, Immunofluorescence staining for pMLC2, Ki67, DBA and EYFP showing pMLC2 distribution in hyperproliferating cells and wild-type duct-cell neighbours of FCk19 mice. Scale bars, 10 μm. Representative of six mice. f, Basal–apical pMLC2 pixel intensity profiles of normal and hyperproliferating cells. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. Twenty-eight ducts (6 mice), n = 64 Fbw7flox/flox cells, n = 93 wild-type cells. g, Immunofluorescence staining for ItgA2, Ki67, DBA and EYFP showing lack of basal integrin overexpression in hyperproliferating cells and wild-type duct-cell neighbours of FCk19 mice. Scale bars, 10 μm. Representative of three mice. h, Quantification of basal Itga2 localization in hyperproliferative cells relative to wild-type duct-cell neighbours. (n = 52 wild-type cells, 51 Fbw7flox/flox cells). Data are mean ± s.d., *P = 0.0274 (two-sided Mann–Whitney test).
Extended Data Fig. 9 Histological differentiation of benign and malignant ductal reactions.
a, Left to right, H & E stain of normal pancreas, FCk19 pancreas (hyperproliferative ducts), acute caerulein-induced pancreatitis and three-week-old KPC mice. b, Ki67 staining demonstrating proliferation in FCk19 ducts, ductal structures of acute pancreatitis and early transformation (in KPC mice). c, Staining for pMLC2 showing apical–basal redistribution of pMLC2 in transformed ductal lesions (in KPC mice) but not in normal duct cells (left), FCk19 ducts and reactive ducts. d, Itga2 is absent from the cellular membrane in normal duct cells (left) and FCk19 ducts and reactive ducts, but highly abundant in transformed ductal lesions (KPC). Scale bars, 100 μm (main panels), 20 μm (inset panels). All stainings are representative of six mice (normal pancreas), four mice (FCk19 and acute pancreatitis) or three mice (KPC).
Extended Data Fig. 10 Continuum theory of early lesion morphogenesis and pMLC2 distribution in lung airways and hepatic ducts.
a, We consider a continuum theory of tissue mechanics, in which the tissue is represented by a thin layer. The tissue initially has the shape of a cylinder, and we consider—for simplicity—deformations that are invariant along the longitudinal axis in cylindrical coordinates. The tissue has a bending elasticity and an area stretch elasticity that resists its deformation. In addition, the transformed region is subjected to a spontaneous bending-moment difference (\(\Delta {\bar{\zeta }}_{c}\)), compared to the wild-type tissue. The spontaneous bending moment arises from the difference between the tissue basal and apical surface tension (Tb and Ta, respectively). In the transformed tissue, the apical and basal surface tension (\({T}_{{\rm{a}}}^{{\rm{tf}}}\) and \({T}_{{\rm{b}}}^{{\rm{tf}}}\), respectively) differ from their values in the wild-type tissue (Ta and Tb). b, Two effects drive tissue deformation: tissue growth due to transformed cell division and growth leading to an increase in the radius of the cylindrical tissue, while the spontaneous bending-moment difference drives an inward invagination. The balance of these two effects on the transformed tissue indentation defines a threshold radius at which the indentation of the transformed tissue along the axis of symmetry vanishes. c, Calculated deformed tissue cross-sections after the introduction of a region of transformed cells, in the limit of small deformations. Blue line, deformed shape; red dotted line, original shape; the transformed cells are in the upper region. Nc is the number of cells in a tissue cross-section before cell transformation. Other parameters: \(\frac{\Delta {\bar{\zeta }}_{{\rm{c}}}{l}_{0}}{\kappa }=0.39\), Nt = 3 transformed cells in a cross-section. d, Phase diagram of direction of tumour deformation, in the limit of small deformations and small transformed region. R is the cylinder radius,\(\Delta {\bar{\zeta }}_{{\rm{c}}}\) the spontaneous bending-moment difference in the transformed tissue, and κ the bending modulus of the tissue. Schematic examples of tissue cross-sections undergoing inward (blue area) and outward (white area) deformations are shown. e, pMLC2 distribution in lung airways. Left, immunostaining for pMLC2 and Cdh1 in KFCk19 transformed and wild-type epithelium. Star marks pMLC2high myofibroblasts located below the epithelium. Scale bars, 20 μm. Right, Basal–apical pMLC2 intensity profiles, measured as shown in Fig. 2h. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. (wild type, 167 cells; transformed, 66 cells). f, pMLC2 distribution in hepatic ducts. Left, immunostaining for pMLC2 and Cdh1 in KFCk19 transformed and wild-type epithelium. Scale bars, 20 μm. Right, Basal–apical pMLC2 intensity profiles, measured as shown in Fig. 2h. Single-cell profiles were normalized to cellular average and aligned in length. Data are mean ± s.e.m. (wild type, 134 cells; transformed, 284 cells).
Supplementary information
Supplementary Information
This file contains Supplementary Modelling Procedures. 3D vertex model for epithelial mechanics and a continuum theory of transformed epithelium deformation in a cylindrical tissue.
Supplementary Table
This file contains Supplementary Table 1: Human research participants. Description of patients undergoing surgery for pancreatic neoplasia, who kindly consented to donate their samples for this study.
Video 1: Normal pancreatic ductal system.
Detail of a tdTomato-stained (red) normal pancreas from a R26-tdTomato; Hnf1b-CreERt2 mouse showing intricate arborized ducts of varying calibres. Representative of 5 mice.
Video 2: Exophytic neoplasia.
Exophytic lesion of a KFCk19 pancreas stained for Krt19 (white) and EYFP (red). Representative of 7 mice.
Video 3: Endophytic neoplasia.
Endophytic lesion of a KFCk19 pancreas stained for Krt19 (white) and EYFP (red). Representative of 7 mice.
Video 4: KFE acinar-derived lesion.
Lesion of a KFE pancreas stained for Krt19 (white) and tdTomato (red). Note connection to a normal duct. Representative of 3 mice.
Video 5: KPE acinar-derived lesion.
Lesion of a KPE pancreas stained for Krt19 (white) and tdTomato (red). Note connection to a normal duct. Representative of 4 mice.
Source data
Rights and permissions
About this article
Cite this article
Messal, H.A., Alt, S., Ferreira, R.M.M. et al. Tissue curvature and apicobasal mechanical tension imbalance instruct cancer morphogenesis. Nature 566, 126–130 (2019). https://doi.org/10.1038/s41586-019-0891-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-019-0891-2
This article is cited by
-
Beyond genetics: driving cancer with the tumour microenvironment behind the wheel
Nature Reviews Cancer (2024)
-
How multiscale curvature couples forces to cellular functions
Nature Reviews Physics (2024)
-
Homeotic compartment curvature and tension control spatiotemporal folding dynamics
Nature Communications (2023)
-
Improving the prognosis of pancreatic cancer: insights from epidemiology, genomic alterations, and therapeutic challenges
Frontiers of Medicine (2023)
-
S100 family proteins are linked to organoid morphology and EMT in pancreatic cancer
Cell Death & Differentiation (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.