Abstract
Barrier tissue dysfunction is a fundamental feature of chronic human inflammatory diseases1. Specialized subsets of epithelial cells—including secretory and ciliated cells—differentiate from basal stem cells to collectively protect the upper airway2,3,4. Allergic inflammation can develop from persistent activation5 of type 2 immunity6 in the upper airway, resulting in chronic rhinosinusitis, which ranges in severity from rhinitis to severe nasal polyps7. Basal cell hyperplasia is a hallmark of severe disease7,8,9, but it is not known how these progenitor cells2,10,11 contribute to clinical presentation and barrier tissue dysfunction in humans. Here we profile primary human surgical chronic rhinosinusitis samples (18,036 cells, n = 12) that span the disease spectrum using Seq-Well for massively parallel single-cell RNA sequencing12, report transcriptomes for human respiratory epithelial, immune and stromal cell types and subsets from a type 2 inflammatory disease, and map key mediators. By comparison with nasal scrapings (18,704 cells, n = 9), we define signatures of core, healthy, inflamed and polyp secretory cells. We reveal marked differences between the epithelial compartments of the non-polyp and polyp cellular ecosystems, identifying and validating a global reduction in cellular diversity of polyps characterized by basal cell hyperplasia, concomitant decreases in glandular cells, and phenotypic shifts in secretory cell antimicrobial expression. We detect an aberrant basal progenitor differentiation trajectory in polyps, and propose cell-intrinsic13, epigenetic14,15 and extrinsic factors11,16,17 that lock polyp basal cells into this uncommitted state. Finally, we functionally demonstrate that ex vivo cultured basal cells retain intrinsic memory of IL-4/IL-13 exposure, and test the potential for clinical blockade of the IL-4 receptor α-subunit to modify basal and secretory cell states in vivo. Overall, we find that reduced epithelial diversity stemming from functional shifts in basal cells is a key characteristic of type 2 immune-mediated barrier tissue dysfunction. Our results demonstrate that epithelial stem cells may contribute to the persistence of human disease by serving as repositories for allergic memories.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Schleimer, R. P. & Berdnikovs, S. Etiology of epithelial barrier dysfunction in patients with type 2 inflammatory diseases. J. Allergy Clin. Immunol. 139, 1752–1761 (2017).
Hogan, B. L. et al. Repair and regeneration of the respiratory system: complexity, plasticity, and mechanisms of lung stem cell function. Cell Stem Cell 15, 123–138 (2014).
Whitsett, J. A. & Alenghat, T. Respiratory epithelisal cells orchestrate pulmonary innate immunity. Nat. Immunol. 16, 27–35 (2015).
Iwasaki, A., Foxman, E. F. & Molony, R. D. Early local immune defences in the respiratory tract. Nat. Rev. Immunol. 17, 7–20 (2017).
Holtzman, M. J., Byers, D. E., Alexander-Brett, J. & Wang, X. The role of airway epithelial cells and innate immune cells in chronic respiratory disease. Nat. Rev. Immunol. 14, 686–698 (2014).
Iwasaki, A. & Medzhitov, R. Control of adaptive immunity by the innate immune system. Nat. Immunol. 16, 343–353 (2015).
Schleimer, R. P. Immunopathogenesis of chronic rhinosinusitis and nasal polyposis. Annu. Rev. Pathol. 12, 331–357 (2017).
Zhao, L. et al. Increase of poorly proliferated p63+/Ki67+ basal cells forming multiple layers in the aberrant remodeled epithelium in nasal polyps. Allergy 72, 975–984 (2017).
Hansel, F. K. Clinical and histopathological studies of the nose and sinuses in allergy. J. Allergy 1, 43–70 (1929).
Rock, J. R. et al. Basal cells as stem cells of the mouse trachea and human airway epithelium. Proc. Natl Acad. Sci. USA 106, 12771–12775 (2009).
Karin, M. & Clevers, H. Reparative inflammation takes charge of tissue regeneration. Nature 529, 307–315 (2016).
Gierahn, T. M. et al. Seq-Well: portable, low-cost RNA sequencing of single cells at high throughput. Nat. Methods 14, 395–398 (2017).
Naik, S. et al. Inflammatory memory sensitizes skin epithelial stem cells to tissue damage. Nature 550, 475–480 (2017).
Netea, M. G. et al. Trained immunity: a program of innate immune memory in health and disease. Science 352, aaf1098 (2016).
Rochman, M. et al. Neurotrophic tyrosine kinase receptor 1 is a direct transcriptional and epigenetic target of IL-13 involved in allergic inflammation. Mucosal Immunol. 8, 785–798 (2015).
von Moltke, J., Ji, M., Liang, H. E. & Locksley, R. M. Tuft-cell-derived IL-25 regulates an intestinal ILC2-epithelial response circuit. Nature 529, 221–225 (2016).
Lindemans, C. A. et al. Interleukin-22 promotes intestinal-stem-cell-mediated epithelial regeneration. Nature 528, 560–564 (2015).
Cheng, L. E. & Locksley, R. M. Allergic inflammation–innately homeostatic. Cold Spring Harb. Perspect. Biol. 7, a016352 (2014).
Palm, N. W., Rosenstein, R. K. & Medzhitov, R. Allergic host defences. Nature 484, 465–472 (2012).
Gieseck, R. L. III, Wilson, M. S. & Wynn, T. A. Type 2 immunity in tissue repair and fibrosis. Nat. Rev. Immunol. 18, 62–76 (2017).
von Andrian, U. H. & Mackay, C. R. T-cell function and migration. Two sides of the same coin. N. Engl. J. Med. 343, 1020–1034 (2000).
Allakhverdi, Z. et al. Thymic stromal lymphopoietin is released by human epithelial cells in response to microbes, trauma, or inflammation and potently activates mast cells. J. Exp. Med. 204, 253–258 (2007).
Wambre, E. et al. A phenotypically and functionally distinct human TH2 cell subpopulation is associated with allergic disorders. Sci. Transl. Med. 9 (2017).
Portelli, M. A., Hodge, E. & Sayers, I. Genetic risk factors for the development of allergic disease identified by genome-wide association. Clin. Exp. Allergy 45, 21–31 (2015).
Zuo, W. L. et al. Ontogeny and biology of human small airway epithelial club cells. Am. J. Respir. Crit. Care Med. (2018).
Boscke, R. et al. Wnt signaling in chronic rhinosinusitis with nasal polyps. Am. J. Respir. Cell Mol. Biol. 56, 575–584 (2017).
Nusse, R. & Clevers, H. Wnt/β-catenin signaling, disease, and emerging therapeutic modalities. Cell 169, 985–999 (2017).
Ostuni, R. et al. Latent enhancers activated by stimulation in differentiated cells. Cell 152, 157–171 (2013).
Lambrecht, B. N. & Hammad, H. The immunology of the allergy epidemic and the hygiene hypothesis. Nat. Immunol. 18, 1076–1083 (2017).
Beyaz, S. et al. High-fat diet enhances stemness and tumorigenicity of intestinal progenitors. Nature 531, 53–58 (2016).
Meltzer, E. O. et al. Rhinosinusitis: establishing definitions for clinical research and patient care. J. Allergy Clin. Immunol. 114, 155–212 (2004).
Dhariwal, J. et al. Mucosal type 2 innate lymphoid cells are a key component of the allergic response to aeroallergens. Am. J. Respir. Crit. Care Med. 195, 1586–1596 (2017).
Proud, D., Sanders, S. P. & Wiehler, S. Human rhinovirus infection induces airway epithelial cell production of human β-defensin 2 both in vitro and in vivo. J. Immunol. 172, 4637–4645 (2004).
Pipkorn, U. & Karlsson, G. Methods for obtaining specimens from the nasal mucosa for morphological and biochemical analysis. Eur. Respir. J. 1, 856–862 (1988).
Wenzel, S. et al. Dupilumab in persistent asthma with elevated eosinophil levels. N. Engl. J. Med. 368, 2455–2466 (2013).
Beck, L. A. et al. Dupilumab treatment in adults with moderate-to-severe atopic dermatitis. N. Engl. J. Med. 371, 130–139 (2014).
Bachert, C. et al. Effect of subcutaneous dupilumab on nasal polyp burden in patients with chronic sinusitis and nasal polyposis: a randomized clinical trial. J. Am. Med. Assoc. 315, 469–479 (2016).
Dwyer, D. F., Barrett, N. A., Austen, K. F. & Immunological Genome Project Consortium. Expression profiling of constitutive mast cells reveals a unique identity within the immune system. Nat. Immunol. 17, 878–887 (2016).
Macosko, E. Z. et al. Highly parallel genome-wide expression profiling of individual cells using nanoliter droplets. Cell 161, 1202–1214 (2015).
Satija, R., Farrell, J. A., Gennert, D., Schier, A. F. & Regev, A. Spatial reconstruction of single-cell gene expression data. Nat. Biotechnol. 33, 495–502 (2015).
Poposki, J. A. et al. Group 2 innate lymphoid cells are elevated and activated in chronic rhinosinusitis with nasal polyps. Immun. Inflamm. Dis. 5, 233–243 (2017).
Butler, A., Hoffman, P., Smibert, P., Papalexi, E. & Satija, R. Integrating single-cell transcriptomic data across different conditions, technologies, and species. Nat. Biotechnol. 36, 411–420 (2018).
McDavid, A. et al. Data exploration, quality control and testing in single-cell qPCR-based gene expression experiments. Bioinformatics 29, 461–467 (2013).
Hackett, N. R. et al. The human airway epithelial basal cell transcriptome. PLoS One 6, e18378 (2011).
Giovannini-Chami, L. et al. Distinct epithelial gene expression phenotypes in childhood respiratory allergy. Eur. Respir. J. 39, 1197–1205 (2012).
Naeem, S., Thompson, L. J., Lawler, S. P., Lawton, J. H. & Woodfin, R. M. Declining biodiversity can alter the performance of ecosystems. Nature 368, 734–737 (1994).
Simpson, E. H. Measurement of diversity. Nature 163, 688 (1949).
Trombetta, J. J. et al. Preparation of single-cell RNA-seq libraries for next generation sequencing. Curr. Protoc. Mol. Biol. 107, 4.22.1–4.22.17 (2014).
Dobin, A. et al. STAR: ultrafast universal RNA-seq aligner. Bioinformatics 29, 15–21 (2013).
Li, B. & Dewey, C. N. RSEM: accurate transcript quantification from RNA-seq data with or without a reference genome. BMC Bioinformatics 12, 323 (2011).
Love, M. I., Huber, W. & Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 15, 550 (2014).
Olender, T. et al. The human olfactory transcriptome. BMC Genomics 17, 619 (2016).
Wang, W. et al. Transcriptome analysis reveals distinct gene expression profiles in eosinophilic and noneosinophilic chronic rhinosinusitis with nasal polyps. Sci. Rep. 6, 26604 (2016).
Haghverdi, L., Buttner, M., Wolf, F. A., Buettner, F. & Theis, F. J. Diffusion pseudotime robustly reconstructs lineage branching. Nat. Methods 13, 845–848 (2016).
Buenrostro, J. D. et al. Single-cell chromatin accessibility reveals principles of regulatory variation. Nature 523, 486–490 (2015).
Corces, M. R. et al. An improved ATAC-seq protocol reduces background and enables interrogation of frozen tissues. Nat. Methods 14, 959–962 (2017).
Heinz, S. et al. Simple combinations of lineage-determining transcription factors prime cis-regulatory elements required for macrophage and B cell identities. Mol. Cell 38, 576–589 (2010).
Fulcher, M. L., Gabriel, S., Burns, K. A., Yankaskas, J. R. & Randell, S. H. Well-differentiated human airway epithelial cell cultures. Methods Mol. Med. 107, 183–206 (2005).
Mead, B. E. et al. Harnessing single-cell genomics to improve the physiological fidelity of organoid-derived cell types. BMC Biol. 16, 62 (2018).
Gosselin, D. et al. An environment-dependent transcriptional network specifies human microglia identity. Science 356, eaal3222 (2017).
Acknowledgements
We thank S.L. Carroll for technical support with Seq-Well experiments; H. Raff for RNA extraction; J. Lai for histology; A. Chicoine of the Brigham and Women’s Human Immunology Flow Core for assistance with isolating cells; L. Ludwig, J. Hammelman and J. Buenrostro for advice on reagents and analysis for ATAC-seq; D. Lingwood, U.H. von Andrian, B. Walker, S. Pillai, N. Yosef, S. Rakoff-Nahoum, S. Beyaz, C. Borges, M.B. Cole, N. Yosef, R. Satija and C. Bingle for discussions and comments on the manuscript; Shalek Laboratory members for experimental and computational advice; and M. Morrison for administrative support. A.K.S. was supported by the Searle Scholars Program, the Beckman Young Investigator Program, the Pew-Stewart Scholars, a Sloan Fellowship in Chemistry, NIH grants 1DP2OD020839, 2U19AI089992, 1U54CA217377, P01AI039671, 5U24AI118672, 2RM1HG006193, 1R33CA202820, 2R01HL095791, 1R01AI138546, 1R01HL126554, 1R01DA046277, 2R01HL095791, and Bill and Melinda Gates Foundation grants OPP1139972 and BMGF OPP1116944; N.A.B. by NIH R01HL120952 and Steven and Judy Kaye Young Innovators Award; T.M.L. by NIH R01HL128241; J.A.B. by NIH U19AI095219, R01AI078908, R01AI136041, R01HLI136209; D.F.D. by T32AI007306 (to J.A.B.); K.M.B. by NIH AADCRC Opportunity Fund Award U19AI070535; and K.N.C by NIH K23AI118804. S.K.N. was supported by NIH 2R01GM081871-09 to B.B. Support was also provided from the Koch Institute Support (core) Grant P30-CA14051 from the NCI, and Ragon Institute NIH-funded Centers for AIDS Research (P30 AI060354, Harvard University Center for AIDS Research), supported by NIH co-funding and participating Institutes and Centers: NIAID, NCI, NICHD, NHLBI, NIDA, NIMH, NIA, FIC, and OAR. J.O.M. is a HHMI Damon Runyon Cancer Research Foundation Fellow (DRG-2274-16), and thanks S. Montanes-Ordovas for encouraging him to work on human allergic disease.
Reviewer information
Nature thanks R. Schleimer and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
J.O.-M., D.F.D., T.M.L., J.A.B., N.A.B. and A.K.S. designed the study. N.B. performed surgeries. J.O.-M., D.F.D., C.D., M.V., K.M.B., K.N.C. and E.Y. collected patient samples and performed single-cell experiments. J.O.-M., M.V., D.F.D. and E.Y. performed in vitro experiments. M.H.W. and T.K.H provided the Seq-Well platform and expertise. H.R.K. and E.Y. performed histologic analyses. B.B. provided supervision and analysed epigenetic experiments. J.O.-M., D.F.D., S.K.N. and S.W.K. analysed data. J.O.-M., D.F.D., S.K.N., N.A.B. and A.K.S. interpreted data. J.O.-M., D.F.D., N.A.B. and A.K.S. wrote the manuscript with input from all authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Consistency of cell capture and identification in surgical EthSin scRNA-seq patient cohort.
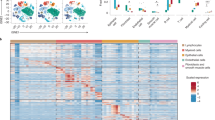
a, Number of unique molecular identifiers (nUMI) and genes identified, and fraction of reads mapping to mitochondrial or ribosomal genes across recovered cell types: 3,222 basal cells, 4,362 apical cells, 2,192 glandular cells, 498 ciliated cells, 835 T cells, 2,976 plasma cells, 1,724 fibroblasts, 1,143 endothelial cells, 811 myeloid cells and 273 mast cells. b, nUMI and genes identified, and fraction of reads mapping to mitochondrial or ribosomal genes across patient samples: 789 polyp 1 cells, 1,309 polyp 2 cells, 1,153 polyp 3 cells, 913 polyp 4 cells, 1,219 polyp 5 cells, 1,141 polyp 6A cells, 1,334 polyp 6B cells, 1,314 polyp 7 cells, 1,286 polyp 8 cells, 1,481 polyp 9 cells, 2,988 polyp 11 cells, 3,109 polyp 12 cells. c, t-SNE plot as in Fig. 1b coloured by cell types across all patients and then separated by sample: 18,036 single cells (n = 12 samples). d, The percentage of each cell type recovered within each sample. e, Select marker gene overlays displaying binned count-based UMI-collapsed expression level (log(scaled UMI + 1)) on a t-SNE plot from Fig. 1b for key cell types identified (see Supplementary Table 3 for full gene lists); AUC 0.998 to 0.7 for all markers displayed.
Extended Data Fig. 2 Top marker genes for cell types by scRNA-seq and bulk tissue RNA-seq from EthSin recovers expected T2I and eosinophilic modules.
a, Row-normalized heat map of the top 10 marker genes identified by ROC test (AUC > 0.73 for all) over all cell types (Fig. 1b, c) with select genes displayed on y axis and cells on x axis (see Supplementary Table 3 for full gene lists); maximum 500 cells per type. b, An overlay of CLC (a pathognomonic gene for eosinophils) displaying binned count-based expression level (log(scaled UMI + 1)) amongst myeloid cells. 811 myeloid cells from n = 12 samples. c, A row-normalized and row-clustered heat map over the top 100 positively and negatively differentially-expressed genes (50 in each direction) in bulk tissue RNA-seq of 27 samples from non-polyp (n = 10) and polyp (n = 17) tissue with select genes displayed. DESeq2 Wald test, all P < 9.03 × 10−5 for genes displayed, corrected for multiple comparisons by Benjamini procedure, samples ordered as in Fig. 3g (see Supplementary Table 4 for full gene list and associated statistics). d, The top differentially regulated pathways identified by ingenuity pathway analysis (see Methods) over the top 1,000 differentially expressed genes, as determined by P < 0.05 corrected for multiple comparisons by Benjamini procedure, across polyp and non-polyp tissue. e, Predicted upstream regulators based on differentially expressed gene modules in polyp tissue relative to non-polyp determined using ingenuity pathway analysis (see Methods).
Extended Data Fig. 3 Sub-clustering of myeloid, fibroblast and endothelial cell types from the EthSin T2I inflammatory ecosystem.
a, t-SNE plot of 811 myeloid cells (n = 6 non-polyp, n = 6 polyp samples), coloured by clusters identified through shared nearest neighbour (SNN) analysis (Supplementary Table 3; Methods), from CRS-EthSin; select marker gene overlays displaying count-based (UMI-collapsed) expression level (log(scaled UMI + 1)) on a t-SNE plot (see Supplementary Table 3 for full gene lists; genes identified by ROC test with AUC 0.689 for S100A8, 0.763 for CD1C, 0.927 for C1QC); a clustered correlation matrix of marker genes identified in single-cell data from myeloid cells; and violin plots for the expression value (log(scaled UMI + 1)) of selected markers of myeloid activation state. b, t-SNE plot of 1,724 fibroblasts (n = 6 non-polyp, n = 6 polyp samples), coloured by clusters identified through shared nearest neighbour (SNN) analysis (Supplementary Table 3; Methods), from CRS-EthSin; select marker gene overlays displaying count-based (UMI-collapsed) expression level (log(scaled UMI + 1)) on a t-SNE plot (see Supplementary Table 3 for full gene lists; genes identified by ROC test with AUC 0.691 for CTGF, 0.683 for CXCL12, 0.726 for MYH11); and a clustered correlation matrix of marker genes identified in single-cell data from fibroblasts. Note, clusters 4 and 5 are likely to represent doublets with epithelial cells and endothelial cells, respectively. Although we exclude these clusters from further formal analyses, we note that there may be interesting biology within pairs of cells that are found to interact more frequently than by chance. c, t-SNE plot of 1,143 endothelial cells (n = 6 non-polyp, n = 6 polyp samples), coloured by clusters identified through shared nearest neighbour (SNN) analysis (Supplementary Table 3; Methods), from CRS-EthSin; select marker gene overlays displaying count-based (UMI-collapsed) expression level (log(scaled UMI + 1)) on a t-SNE plot (see Supplementary Table 3 for full gene lists; genes identified via ROC test with AUC 0.742 for SELE, 0.706 for PODXL, 0.822 for PLAT); and a clustered correlation matrix of marker genes identified in single-cell data from endothelial cells.
Extended Data Fig. 4 Mapping T2I mediators within EthSin non-polyp or polyp ecosystems and the identities of T cells.
a, Dot plots of chemokines and lipid mediators with known roles in T2I mapped onto cell types divided by non-polyp or polyp disease state. Dot size represents fraction of cells within that type expressing the gene, and colour intensity represents binned (log(scaled UMI + 1)) gene expression amongst expressing cells (related to Fig. 1d). b, Dot plot of inducers and effectors of T2I mapped onto cell types divided by non-polyp or polyp disease state. Dot size represents fraction of cells within that type expressing the gene, and colour intensity represents binned (log(scaled UMI + 1)) gene expression amongst expressing cells (related to Fig. 1d). c, t-SNE plot of re-clustered T cells with select gene overlays displaying binned count-based expression level (log(scaled UMI + 1)) for Th2A-specific genes (top row) and canonical T cell markers (bottom row); 835 T cells from n = 6 non-polyp and n = 6 polyp samples. d, Violin plot of five identified T cell clusters scored for expression of T cell receptor complex genes (for example, TRAC and CD3E, see Methods, Supplementary Table 4). Dots represent individual cells; 835 total T cells. e, Dot plot of inducers and effectors of Type 1 immunity across all cell types (note that IL17F was not detected). f, Dot plot of select GWAS risk alleles41 for allergic disease, mapped onto cell types. Dot size represents fraction of cells within that type expressing the gene, and colour intensity represents binned (log(scaled UMI + 1)) gene expression amongst expressing cells (related to Fig. 1d).
Extended Data Fig. 5 Relationship of EthSin epithelial cell clusters and secretory/glandular distinctions.
a, A phylogenetic tree based on the average cell from each cluster of epithelial cell clusters in gene-space. b, Violin plot of expression contribution to a cell’s transcriptome of basal cell genes (see Methods and Supplementary Table 4) across all epithelial cells. Cluster 12, 794 cells; cluster 8, 924 cells; cluster 2, 1,504 cells; cluster 1, 1,561 cells; cluster 0, 1,600 cells; cluster 4, 1,201 cells; cluster 13, 725 cells; cluster 3, 1,467 cells; cluster 16, 498 cells; Mann–Whitney U-test, with Bonferroni correction, P < 1.76 × 10−15, cluster 12, cluster 8 or cluster 2 versus the mean score of basal/apical epithelial cells; P = 0.5392, cluster 1 versus the mean score. c, Canonical correlation analysis (CCA) displaying our cell type annotations for basal and apical cells derived through clustering and biological curation alongside CCA clusters in t-SNE space; 7,584 basal and apical cells. d, Violin plots for the count-based expression level (log(scaled UMI + 1)) of selected marker genes for each identified epithelial cell subset; cell numbers as in b. e, Row-normalized heat map of the top marker genes identified by ROC test (AUC > 0.6) within each cell type for each cell cluster with genes displayed on y axis and cluster annotations on x axis (see Supplementary Table 3 for full gene lists). f, Select overlays on clusters 0 and 4 (differentiating/secretory) and 13 (glandular) displaying binned count-based expression level (log(scaled UMI + 1)) in t-SNE space for canonical goblet (MUC5B, MUC5AC, SPDEF, FOXA3) and secretory (SCGB1A1) genes; 3,526 cells. g, A clustered correlation matrix of glandular, goblet, and secretory cell genes. Pearson’s abs(r) > 0.038 is significant (P < 0.05) based on asymptotic P values.
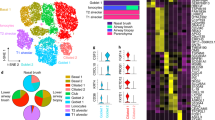
Extended Data Fig. 6 Glandular cell subsets, their relationship to apical secretory cells, and immune cells recovered through nasal scrapings.
a, t-SNE plots of 5,928 single epithelial cells (n = 6 non-polyp samples) and 4,346 single epithelial cells (n = 6 polyp samples) coloured by clusters identified through (left) shared nearest neighbour (SNN) analysis and (right) original biological curation of cell types (Supplementary Table 3; Methods) as illustrated in Fig. 2a. Note, cluster colours in left panels of each disease are not comparable but curated clusters in panels are, and glandular cells are highlighted for subsetting in next panel. b, Violin plots for the count-based expression level (log(scaled UMI + 1)) of selected marker genes identified through marker discovery (ROC test) for each subset of glandular cells; 2,114 total cells (cluster 1, 791 cells; LCN2 cluster, 709 cells; SERPINB3 cluster, 283 cells; MUC5B cluster, 209 cells; PRB1 cluster, 183 cells) with representation of every non-polyp patient in each cluster of cells (for example, no cluster is unique to one patient) and AUC metric 0.800 for LCN2, 0.736 for SERPINB3, 0.985 for MUC5B, 0.973 for BPIFB2, and 0.908 for PRB1. c, Samples were acquired through the two distinct methods of nasal scraping and ethmoid sinus surgical intervention. This allowed for sampling of healthy tissue from InfTurb (scraping, top left), CRS-EthSin-non-polyp tissue (surgery, top middle), CRS-EthSin-polyp tissue (surgery, top right), InfTurb of polyp-bearing individuals (scraping, top right) and CRS-EthSin-polyp tissue accessible for scraping (scraping, top right). Bottom panels, anatomy of the nasal turbinates (healthy and CRS polyp) and ethmoid sinus (CRS non-polyp and CRS polyp) where samples were acquired, highlighting the depth of cells recovered from each site related to Fig. 2. Healthy tissue is annotated with basal and apical cell types, including sub-mucosal glands. d, Left, t-SNE plot of 18,704 single cells from nasal scrapings (n = 9 samples) coloured by clusters identified through shared nearest neighbour (SNN) analysis (Supplementary Table 3; Methods). Middle, t-SNE plot coloured by cell types identified through marker discovery (ROC test) and biological curation of identified clusters (Supplementary Table 3; Methods). Right, t-SNE plot coloured by disease and tissue of origin from healthy InfTurb (7,603 cells; n = 3 samples), polyp-bearing patient InfTurb (2,298 cells; n = 4 samples) and polyp scraping directly from EthSin-polyp (8,803 cells; n = 2 samples), with adjacent select marker gene overlays displaying count-based UMI-collapsed expression level (log(scaled UMI + 1)) for apical epithelial (KRT8) and haematopoietic (PTPRC) genes. e, Select marker gene overlays displaying count-based UMI-collapsed expression level (log(scaled UMI + 1)) on a t-SNE plot from a for key cell types identified (see Supplementary Table 3 for full gene lists); area under the curve (AUC) 0.946 to 0.705 for all markers displayed. f, Violin plots for the count-based expression level (log(scaled UMI + 1)) for key differentially expressed genes using ROC test within myeloid cells across disease states and tissues identified (Methods); 137 cells, n = 3 healthy inferior turbinate; 157 cells, n = 4 polyp inferior turbinate; 210 cells, n = 2 polyp ethmoid sinus samples; AUC 0.67 for TXNRD1, 0.615 for RALA, 0.647 for TLR2, 0.619 for RIPK2, 0.747 for C1QA, 0.674 for FGL2.
Extended Data Fig. 7 Changes in cellular composition between EthSin-non-polyp and EthSin-polyp tissue by scRNA-seq and flow cytometric gating and histological strategy for quantification and isolation of basal cells.
a, The frequency of each cell type recovered amongst all cells within each patient sample (n = 6 non-polyp, n = 6 polyp) grouped by disease state. Two-sided t-test; apical, P = 0.0003; glandular, P < 0.0001; ciliated, P = 0.0047; plasma cell, P = 0.00014; myeloid, P = 0.0098; mast cell, P = 0.00018; all non-polyp versus polyp with Holm–Sidak correction for multiple comparisons. Data are mean ± s.e.m. b, The frequency of basal cells amongst epithelial cells captured in scRNA-seq data displayed for each sample and coloured by non-polyp or polyp designation. c, t-SNE plots with each patient’s cells clustered independently over a common list of most variable genes identified from all epithelial cells and with clustering parameters set constant to 12 principal components and resolution set to 1.4; minimum 789 cells in each plot; see Extended Data Fig. 1b and Supplementary Table 3 for specific cell numbers. d, Simpson’s index of diversity, an indication of the total richness present within an ecosystem, over epithelial cell clusters identified in c, calculated for each patient; n = 6 non-polyp and n = 6 polyp samples. Two-tailed t-test, P = 0.0384. Data are mean ± s.e.m. e, Correlation of Simpson’s index of diversity calculated over epithelial cells against the ranked order of samples based on clinical pathological evaluation; n = 6 non-polyp and n = 6 polyp samples; r = 0.6824, P = 0.009. f, Simpson’s index of diversity over stromal and immune cell types and total cells, calculated for each sample (n = 6 non-polyp and n = 6 polyp). Points represent individual samples. Two-tailed t-test, P = 0.0015 (stromal and immune), P = 0.0145 (total cells), non-polp versus polyp. Data are mean ± s.e.m. g, Reproduced from Fig. 2a: t-SNE plot of 10,274 epithelial cells, coloured by clusters identified through SNN, with adjacent colour bars representing related cell clusters, and overlays displaying binned count-based expression level (log(scaled UMI + 1)) of selected genes used to negatively (CD45, EPCAM, THY1) and positively (NGFR, ITGA6, PDPN) identify basal cells. h, Full flow cytometric gating strategy for quantification and isolation of basal cells from non-polyp and polyp tissue (related to Fig. 3c). i, Representative histology (5× magnification) of the glandular area detected in haematoxylin and eosin stained tissue sections from non-polyp or polyp patients; quantification in Fig. 3e. j, Representative immunofluorescence of p63+ cells (basal cell marker) relative to isotype control; quantification in Fig. 3d. Scale bar, 100 μm. k, Basal cell fraction of transcripts from bulk tissue RNA-seq data of our own dataset (related to Fig. 3g, h) and two GEO datasets containing healthy and healthy/polyp nasal mucosa biopsies. Our data: n = 10 non-polyp samples, n = 17 polyp samples. Reference data: n = 6 healthy, n = 6 polyp samples. Two-tailed t-test, P = 0.0465 (our data) and P = 0.0040 (GEO data). Data are mean ± s.e.m. l, Secretory cell fraction of transcripts from bulk tissue RNA-seq data of our own dataset (related to Fig. 3g, h) and two GEO datasets containing healthy and healthy/polyp nasal mucosa biopsies. Our data, n = 10 non-polyp samples, n = 17 polyp samples; reference data, n = 6 healthy, n = 6 polyp samples. Two-tailed t-test, P = 0.0465 (our data) and P = 0.0040 (GEO data). Data are mean ± s.e.m.
Extended Data Fig. 8 Epithelial cytokine signatures from CRS-EthSin tissue demonstrate T2I pattern, discovery of gene modules in the fibroblast niche which correlate with basal cell hyperplasia, and differential expression within myeloid and endothelial cells by polyp status.
a, Violin plots of IL-4- or IL-13-uniquely induced gene signatures in respiratory epithelial cell clusters or grouped by disease state presented as expression contribution to a cell’s transcriptome (see Methods, Fig. 4b for shared genes, and Supplementary Table 4). Cluster 12, 794 cells; cluster 8, 924 cells; cluster 2, 1,504 cells; cluster 1, 1,561 cells; cluster 0, 1,600 cells; cluster 4, 1,201 cells; cluster 13, 725 cells; cluster 3, 1,467 cells; cluster 16, 498 cells. Mann–Whitney U-test, P < 2.2 × 10−16, 0.305 IL-4 effect size (polyp versus non-polyp) and −0.448 IL-13 effect size (polyp versus non-polyp). b, Violin plots of IFN-α- or IFN-γ-induced gene signatures in respiratory epithelial cell clusters or grouped by disease state presented as expression contribution to a cell’s transcriptome (see Methods, and Supplementary Table 4); cell numbers as in a. Mann–Whitney U-test, P = 4.98 × 10−6, −0.156 IFN-α effect size (polyp versus non-polyp). Mann–Whitney U-test, P < 2.2 × 10−16, 0.161 IFN-γ effect size (polyp versus non-polyp). c, Selected genes detected in fibroblasts from single-cell data which correlate with the samples ranked by basal cell frequency detected within each ecosystem. Non-polyp, n = 6; polyp, n = 6. All genes used: Spearman correlation, abs(r) > 0.7651, P < 0.0037. To determine genes correlated in specific cell types (for example, fibroblasts) with the frequency of basal cells present in a cellular ecosystem, we correlated the average log-normalized single-cell count data for each gene to the rank of samples determined by increasing frequency of basal cells in each ecosystem (8.2% to 19.1% for non-polyp and 27.9% to 70.1% for polyp samples, Extended Data Fig. 7b). d, A clustered correlation matrix of genes identified as per c in single-cell data from fibroblasts; Pearson’s abs(r) > 0.048 is significant (P < 0.05) based on asymptotic P values. e, Row-normalized heat map for myeloid cells from ethmoid sinus with select genes displayed on the y axis, including a core myeloid signature (ROC test myeloid cells versus rest of cells, AUC > 0.8), and genes differentially expressed (bimodal test) by disease state, with disease-state annotations on x axis. Bimodal test, all non-core genes P < 0.0002 or less with Bonferroni correction for multiple hypothesis testing based on number of genes tested. f, Row-normalized heat map for endothelial cells from ethmoid sinus with select genes displayed on y axis including a core basal signature (ROC test endothelial cells versus rest of cells, AUC > 0.75), and genes differentially expressed (bimodal test) by disease state, with disease-state annotations on x axis. Bimodal test, all non-core genes P < 2.43 × 10−6 or less with Bonferroni correction for multiple hypothesis testing based on number of genes tested.
Extended Data Fig. 9 Pseudotime analysis on basal and differentiating/secretory cell clusters from EthSin, transcriptional motif enrichments in non-polyp and polyp basal cells, and the identity of cell types in air–liquid interface cultures.
a, Pseudotime analysis using diffusion mapping (see Methods) of selected clusters of epithelial cells, here displaying diffusion pseudotime (related to Fig. 4d). Clusters 8/1/4, 3,516 cells; clusters 12/2/0, 4,064 cells. n = 6 non-polyp, n = 6 polyp samples. Diffusion map and diffusion coefficients (DC) are calculated over the set of basal and apical marker genes identified in Fig. 1a (see Supplementary Table 3). b, The top 60 negatively correlated genes expressed in non-polyp cells with pseudotime trajectory and Pearson correlation values for genes in polyp cells also displayed; differential correlation coefficient analysis using Fisher’s z-statistic, accounting for number of cells in each group (specific genes highlighted, all >2z; full results including Bonferroni corrected P values in Supplementary Table 3). c, Correlation matrices (row and column clustered) of the normalized read counts per sample in motif-associated peaks for non-polyp or polyp samples. Pearson correlation, n = 3 non-polyp, n = 7 polyp. d, A column-normalized heat map (row and column clustered) for the fraction of peaks with a motif corresponding to accessibility of the respective transcription factor displayed by patient. n = 3 non-polyp, n = 7 polyp. e, IGV tracks for ATF3 and KLF5 based on peaks detected and averaged by non-polyp and polyp samples from ATAC-seq profiling. f, IGV tracks for S100A9 and MUC4 based on peaks detected and averaged by non-polyp and polyp samples from ATAC-seq profiling. g, Violin plots for the count-based expression level (log(scaled UMI + 1)) for key marker genes using ROC test across cell types identified in Fig. 5a, Supplementary Table 3. 1,345 basal; 6,420 secretory; 6,381 hybrid; and 2,027 ciliated cells from n = 2 non-polyp and n = 2 polyp patients. AUC = 0.943 (KRT5), 0.667 (TP63), 0.644 (LYPD2), <0.55 (SPDEF), <0.55 (KRT8), 0.602 (BPIFA1), 0.813 (PIFO), 0.73 (FOXJ1). h, Row-normalized heat map for ALI secretory cells (subsampled to 300 cells per donor) as in Fig. 2f of the top in vivo secretory marker genes identified by ROC test (AUC > 0.662) with select genes displayed on y axis including a core secretory signature (ROC test, secretory cells versus rest of cells), and then within secretory cells, ROC test was used to identify marker genes within each disease/location category; and basal-cell derived annotations on x axis (see Supplementary Table 3 for full gene lists, all AUC > 0.65 for markers displayed in Fig. 2f). i, Quantification of flow cytometry for the ratio of basal to Epcamhi cells (gating as in Extended Data Fig. 7h) from ALI cultures at 21 days, stimulated with the indicated doses of IL-13. Points represent individual biological replicates; n = 6 non-polyp, n = 5 polyp samples for each dose. Two-way ANOVA; not significant between disease groups at any dose tested; Two-way ANOVA, P = 0.0224 for IL-13 dose. Data are mean ± s.e.m. j, Expression levels for CTGF (log2 expression value of log-normalized count data) in basal cells from non-polyp or polyp individuals across doses of cytokines displayed. n = 4 samples each dose. Two-way ANOVA P < 0.0260 for CTGF; all conditions non-polyp versus polyp except 0.1 ng ml−1 IL-4 dose for CTGF.
Extended Data Fig. 10 In vivo blockade with an anti-IL-4Rα monoclonal antibody shifts secretory cell state towards healthy-associated genes.
a, Left, t-SNE plot of 8,764 single cells (related to Fig. 5e) from the nasal polyps of an individual treated with dupilumab (IL-4Rα monoclonal antibody) (1 patient, sampled at n = 3 time points), coloured by clusters identified through SNN analysis (Supplementary Table 3; Methods); middle, t-SNE plot coloured by time point and tissue of origin from polyp pre-dupilumab scraping (5,731 cells), from polyp post-dupilumab scraping (647 cells), and polyp post-dupilumab surgical sample (2,386 cells); right, t-SNE plot coloured by cell types identified through marker discovery (ROC test) and biological curation of identified clusters (Supplementary Table 3; Methods). b, Select cell-type specific score overlays for cell types indicated in original core dataset (see Supplementary Table 3 for full gene list). c, Row-normalized heat map for myeloid cells of the top marker genes identified by ROC test (AUC > 0.8) with select genes displayed on y axis including a core myeloid signature (ROC test myeloid cells versus rest of cells), and then genes found to be differentially expressed from Fig. 5f in basal cells, and treatment annotations on x axis. Bimodal test. *, differential genes in both basal cells and myeloid cells pre- versus post-treatment (P < 0.003 or less with Bonferroni correction for multiple hypothesis testing based on number of genes tested). d, Violin plots for basal cells (200 cells pre-dupilumab and 151 cells post-dupilumab, noted in a) for the count-based expression level (log(scaled UMI + 1)), except where indicated for gene scores, fraction of transcriptome and z-score (see Methods, Supplementary Table 4 for gene set used) for key basal cell genes for selected biological processes, or from the baseline upregulated gene set from polyp basal cells in vitro (Fig. 5c). Differential expression testing for decreased expression post-treatment using bimodal test not significant except where indicated (*P < 0.00087 or less with Bonferroni correction for multiple hypothesis testing based on number of genes tested; see Supplementary Table 3 for full list). Basal in vitro score pre versus post: two-tailed t-test, P < 3.897 × 10−15, effect size 0.822. e, t-SNE plot of 4,486 single cells (related to Figs. 2e, 5e) from the inferior turbinate or nasal polyps of an anti-IL-4Rα (dupilumab) treated individual (n = 4 samples) coloured by time point and tissue of origin (left) from inferior turbinate pre-dupilumab scraping (643 cells), from inferior turbinate post-dupilumab scraping (1,596 cells), polyp pre-dupilumab scraping (1,600 cells), and polyp post-dupilumab scraping (647 cells). t-SNE plot coloured by cell types (right) identified through marker discovery (ROC test) and biological curation of identified clusters (Supplementary Table 3; Methods); black outline indicates cells considered in g. f, Select deconvolution score overlays for cell types indicated in original core dataset (see Supplementary Table 3 for full gene list). g, Violin plot for the gene set score over Wnt pathway (z-score) and expression contribution to a cell’s transcriptome over IFN-α- and IL-4/IL-13-commonly induced gene signature in secretory cells grouped as in e and sub-sampled to a maximum of 150 cells from each disease or location category from inferior turbinate pre-dupilumab scraping (150 cells), from inferior turbinate post-dupilumab scraping (23 cells), polyp pre-dupilumab scraping (150 cells) and polyp post-dupilumab scraping (38 cells) (see Methods, Supplementary Table 3, Supplementary Table 4 for gene lists used). Two-tailed t-test; Wnt score pre versus post polyp tissue, effect size 1.02, P = 1.091 × 10−14; Wnt score pre versus post inferior turbinate tissue, effect size −0.17, P = 0.3706; IL-4/IL-13 score pre versus post polyp tissue, effect size 1.17, P < 2.2 × 10−16; IL-4/IL-13 score pre versus post inferior turbinate tissue, effect size −0.17, P = 0.163; IFN-α score pre versus post polyp tissue, effect size −1.25, P = 4.254 × 10−5; IFN-α score pre versus post inferior turbinate tissue, effect size −0.304, P = 0.2766. *P < 7.81 × 10−6 or less between pre- and post-treated polyp, differential expression testing for decreased expression post-treatment using bimodal test. h, Violin plots of secretory cells grouped as in e and sub-sampled to a maximum of 150 cells from each disease or location category from inferior turbinate pre-dupilumab scraping (150 cells), inferior turbinate post-dupilumab scraping (23 cells), polyp pre-dupilumab scraping (150 cells) and polyp post-dupilumab scraping (38 cells) for the count-based expression level (log(scaled UMI + 1)) and for secretory cell genes from the gene set used in Fig. 2f affected by treatment within anatomical regions indicated by heading. *P < 6.36 × 10−5 or less except KLF5 (P = 0.0033) and FOSB (P = 0.0053), differential expression testing for decreased expression post-treatment using bimodal test with Bonferroni correction for multiple hypothesis testing based on number of genes tested, see Supplementary Table 3 for all genes tested.
Supplementary information
Supplementary Information
This file contains a Supplementary Discussion which includes the peer-reviewed elements which provide further details and support for specific areas referenced in the main text.
Supplementary Data
This file contains the R Script which shows the loading cells-by-genes matrix from Supplementary Table 2 into R and initializing Seurat object as illustrated in Fig. 1 following workflow in Methods.
Supplementary Tables
This file contains Supplementary Tables 1-12 and a Supplementary Tables Guide.
Rights and permissions
About this article
Cite this article
Ordovas-Montanes, J., Dwyer, D.F., Nyquist, S.K. et al. Allergic inflammatory memory in human respiratory epithelial progenitor cells. Nature 560, 649–654 (2018). https://doi.org/10.1038/s41586-018-0449-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-018-0449-8
This article is cited by
-
Bridging tissue repair and epithelial carcinogenesis: epigenetic memory and field cancerization
Cell Death & Differentiation (2024)
-
Single-cell RNA sequencing reveals the epithelial cell, fibroblast, and key gene alterations in chronic rhinosinusitis with nasal polyps
Scientific Reports (2024)
-
Human apical-out nasal organoids reveal an essential role of matrix metalloproteinases in airway epithelial differentiation
Nature Communications (2024)
-
Physiological and immunological barriers in the lung
Seminars in Immunopathology (2024)
-
Simple, low-cost, and well-performing method, the outgrowth technique, for the isolation of cells from nasal polyps
BMC Molecular and Cell Biology (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.