Abstract
The observation that BRCA1- and BRCA2-deficient cells are sensitive to inhibitors of poly(ADP–ribose) polymerase (PARP) has spurred the development of cancer therapies that use these inhibitors to target deficiencies in homologous recombination1. The cytotoxicity of PARP inhibitors depends on PARP trapping, the formation of non-covalent protein–DNA adducts composed of inhibited PARP1 bound to DNA lesions of unclear origins1,2,3,4. To address the nature of such lesions and the cellular consequences of PARP trapping, we undertook three CRISPR (clustered regularly interspersed palindromic repeats) screens to identify genes and pathways that mediate cellular resistance to olaparib, a clinically approved PARP inhibitor1. Here we present a high-confidence set of 73 genes, which when mutated cause increased sensitivity to PARP inhibitors. In addition to an expected enrichment for genes related to homologous recombination, we discovered that mutations in all three genes encoding ribonuclease H2 sensitized cells to PARP inhibition. We establish that the underlying cause of the PARP-inhibitor hypersensitivity of cells deficient in ribonuclease H2 is impaired ribonucleotide excision repair5. Embedded ribonucleotides, which are abundant in the genome of cells deficient in ribonucleotide excision repair, are substrates for cleavage by topoisomerase 1, resulting in PARP-trapping lesions that impede DNA replication and endanger genome integrity. We conclude that genomic ribonucleotides are a hitherto unappreciated source of PARP-trapping DNA lesions, and that the frequent deletion of RNASEH2B in metastatic prostate cancer and chronic lymphocytic leukaemia could provide an opportunity to exploit these findings therapeutically.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Lord, C. J. & Ashworth, A. PARP inhibitors: synthetic lethality in the clinic. Science 355, 1152–1158 (2017).
Pommier, Y., O’Connor, M. J. & de Bono, J. Laying a trap to kill cancer cells: PARP inhibitors and their mechanisms of action. Sci. Transl. Med. 8, 362ps17 (2016).
Hopkins, T. A. et al. Mechanistic dissection of PARP1 trapping and the impact on in vivo tolerability and efficacy of PARP inhibitors. Mol. Cancer Res. 13, 1465–1477 (2015).
Murai, J. et al. Trapping of PARP1 and PARP2 by clinical PARP inhibitors. Cancer Res. 72, 5588–5599 (2012).
Cerritelli, S. M. & Crouch, R. J. The balancing act of ribonucleotides in DNA. Trends Biochem. Sci. 41, 434–445 (2016).
Elstrodt, F. et al. BRCA1 mutation analysis of 41 human breast cancer cell lines reveals three new deleterious mutants. Cancer Res. 66, 41–45 (2006).
Daemen, A. et al. Cross-platform pathway-based analysis identifies markers of response to the PARP inhibitor olaparib. Breast Cancer Res. Treat. 135, 505–517 (2012).
Wang, G. et al. Identifying drug–gene interactions from CRISPR knockout screens with drugZ. Preprint at https://www.biorxiv.org/content/early/2017/12/12/232736 (2017).
Ohle, C. et al. Transient RNA–DNA hybrids are required for efficient double-strand break repair. Cell 167, 1001–1013. e7 (2016).
Pierce, A. J., Johnson, R. D., Thompson, L. H. & Jasin, M. XRCC3 promotes homology-directed repair of DNA damage in mammalian cells. Genes Dev. 13, 2633–2638 (1999).
Potenski, C. J., Niu, H., Sung, P. & Klein, H. L. Avoidance of ribonucleotide-induced mutations by RNase H2 and Srs2–Exo1 mechanisms. Nature 511, 251–254 (2014).
Pizzi, S. et al. Reduction of hRNase H2 activity in Aicardi–Goutières syndrome cells leads to replication stress and genome instability. Hum. Mol. Genet. 24, 649–658 (2015).
Reijns, M. A. et al. Enzymatic removal of ribonucleotides from DNA is essential for mammalian genome integrity and development. Cell 149, 1008–1022 (2012).
Hiller, B. et al. Mammalian RNase H2 removes ribonucleotides from DNA to maintain genome integrity. J. Exp. Med. 209, 1419–1426 (2012).
Reijns, M. A. & Jackson, A. P. Ribonuclease H2 in health and disease. Biochem. Soc. Trans. 42, 717–725 (2014).
Chon, H. et al. RNase H2 roles in genome integrity revealed by unlinking its activities. Nucleic Acids Res. 41, 3130–3143 (2013).
Kim, N. et al. Mutagenic processing of ribonucleotides in DNA by yeast topoisomerase I. Science 332, 1561–1564 (2011).
Sparks, J. L. & Burgers, P. M. Error-free and mutagenic processing of topoisomerase 1-provoked damage at genomic ribonucleotides. EMBO J. 34, 1259–1269 (2015).
Williams, J. S. et al. Topoisomerase 1-mediated removal of ribonucleotides from nascent leading-strand DNA. Mol. Cell 49, 1010–1015 (2013).
Sekiguchi, J. & Shuman, S. Site-specific ribonuclease activity of eukaryotic DNA topoisomerase I. Mol. Cell 1, 89–97 (1997).
Pommier, Y., Sun, Y., Huang, S. N. & Nitiss, J. L. Roles of eukaryotic topoisomerases in transcription, replication and genomic stability. Nat. Rev. Mol. Cell Biol. 17, 703–721 (2016).
Huang, S. N., Williams, J. S., Arana, M. E., Kunkel, T. A. & Pommier, Y. Topoisomerase I-mediated cleavage at unrepaired ribonucleotides generates DNA double-strand breaks. EMBO J. 36, 361–373 (2017).
Kipps, T. J. et al. Chronic lymphocytic leukaemia. Nat. Rev. Dis. Primers 3, 16096 (2017).
Klein, U. et al. The DLEU2/miR-15a/16-1 cluster controls B cell proliferation and its deletion leads to chronic lymphocytic leukemia. Cancer Cell 17, 28–40 (2010).
Cancer Genome Atlas Research Network. The molecular taxonomy of primary prostate cancer. Cell 163, 1011–1025 (2015).
Mu, P. et al. SOX2 promotes lineage plasticity and antiandrogen resistance in TP53- and RB1-deficient prostate cancer. Science 355, 84–88 (2017).
Ku, S. Y. et al. Rb1 and Trp53 cooperate to suppress prostate cancer lineage plasticity, metastasis, and antiandrogen resistance. Science 355, 78–83 (2017).
Armenia, J. et al. The long tail of oncogenic drivers in prostate cancer. Nat. Genet. 50, 645–651 (2018).
Bunz, F. et al. Requirement for p53 and p21 to sustain G2 arrest after DNA damage. Science 282, 1497–1501 (1998).
Hart, T. et al. High-resolution CRISPR screens reveal fitness genes and genotype-specific cancer liabilities. Cell 163, 1515–1526 (2015).
Swift, S., Lorens, J., Achacoso, P. & Nolan, G. P. Rapid production of retroviruses for efficient gene delivery to mammalian cells using 293T cell-based systems. Curr Protoc Immunol 31, 10.17.14–10.17.29 (2001).
Reijns, M. A. et al. The structure of the human RNase H2 complex defines key interaction interfaces relevant to enzyme function and human disease. J. Biol. Chem. 286, 10530–10539 (2011).
Ran, F. A. et al. Genome engineering using the CRISPR–Cas9 system. Nat. Protocols 8, 2281–2308 (2013).
Sanjana, N. E., Shalem, O. & Zhang, F. Improved vectors and genome-wide libraries for CRISPR screening. Nat. Methods 11, 783–784 (2014).
Solier, S. et al. Genome-wide analysis of novel splice variants induced by topoisomerase I poisoning shows preferential occurrence in genes encoding splicing factors. Cancer Res. 70, 8055–8065 (2010).
Naughton, C. et al. Transcription forms and remodels supercoiling domains unfolding large-scale chromatin structures. Nat. Struct. Mol. Biol. 20, 387–395 (2013).
Helmrich, A., Ballarino, M. & Tora, L. Collisions between replication and transcription complexes cause common fragile site instability at the longest human genes. Mol. Cell 44, 966–977 (2011).
Puc, J. et al. Ligand-dependent enhancer activation regulated by topoisomerase-I activity. Cell 160, 367–380 (2015).
Harley, M. E. et al. TRAIP promotes DNA damage response during genome replication and is mutated in primordial dwarfism. Nat. Genet. 48, 36–43 (2016).
Brinkman, E. K., Chen, T., Amendola, M. & van Steensel, B. Easy quantitative assessment of genome editing by sequence trace decomposition. Nucleic Acids Res. 42, e168 (2014).
Sakaue-Sawano, A. et al. Visualizing spatiotemporal dynamics of multicellular cell-cycle progression. Cell 132, 487–498 (2008).
Li, W. et al. MAGeCK enables robust identification of essential genes from genome-scale CRISPR/Cas9 knockout screens. Genome Biol. 15, 554 (2014).
Mi, H., Muruganujan, A. & Thomas, P. D. PANTHER in 2013: modeling the evolution of gene function, and other gene attributes, in the context of phylogenetic trees. Nucleic Acids Res. 41, D377–D386 (2013).
Reynolds, J. J. et al. Mutations in DONSON disrupt replication fork stability and cause microcephalic dwarfism. Nat. Genet. 49, 537–549 (2017).
Escribano-Díaz, C. et al. A cell cycle-dependent regulatory circuit composed of 53BP1-RIF1 and BRCA1-CtIP controls DNA repair pathway choice. Mol. Cell 49, 872–883 (2013).
Pascutti, M. F. et al. IL-21 and CD40L signals from autologous T cells can induce antigen-independent proliferation of CLL cells. Blood 122, 3010–3019 (2013).
Robinson, D. et al. Integrative clinical genomics of advanced prostate cancer. Cell 161, 1215–1228 (2015).
Murai, J. et al. Stereospecific PARP trapping by BMN 673 and comparison with olaparib and rucaparib. Mol. Cancer Ther. 13, 433–443 (2014).
Acknowledgements
We thank Y. Pommier and N. Huang for discussions and communication of unpublished results; R. Szilard for critical reading of the manuscript; R. Greenberg for HeLa DR-GFP cells; the IGMM Imaging and Flow Cytometry facilities for assistance and T. Heffernan and N. Feng for providing talazoparib. M.Z. is a Banting postdoctoral fellow. O.M. is supported by an EMBO Long-Term Fellowship (ALTF 7-2015), the European Commission FP7 (Marie Curie Actions, LTFCOFUND2013, GA-2013-609409) and the Swiss National Science Foundation (P2ZHP3_158709). Work in the laboratory of A.P.J. was supported by the Medical Research Council (MRC, U127580972); Work in the laboratory of T.S. was supported by Bloodwise (14031). Work in the laboratories of S.A. and J.M. was supported by grants from the Canadian Cancer Society (#705045; to S.A.) and CIHR (MOP- 142375; to J.M.). Work in the laboratory of J.d.B. was supported by the Movember Foundation, Prostate Cancer UK, the US Department of Defense, the Prostate Cancer Foundation, Stand Up To Cancer, Cancer Research UK, and the UK Department of Health through an Experimental Cancer Medicine Centre grant and work in the laboratory of V.G.B. was supported by Cancer Research UK (grants C157/A25140 and C157/A15703). D.D. is the Thomas Kierans Chair in Mechanisms of Cancer Development and a Canada Research Chair (Tier I) in the Molecular Mechanisms of Genome Integrity. Work in the laboratory of D.D. was funded through CIHR grant FDN143343, Canadian Cancer Society (CCS grants #70389 and #705644), as well as a Grant-in-Aid from the Krembil Foundation.
Reviewer information
Nature thanks A. Chabes, M. Tarsounas and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
M.Z. performed the initial CRISPR screens with the help of M.A., A.M., M.Ch., S.A. and J.M.; T.H. analysed the data; M.Z. and O.M. performed suppressor screens and A.M. helped with data analysis. Unless otherwise stated, M.Z. and O.M., with input from M.A.M.R., performed all additional experiments and data analysis. M.A.M.R. performed biochemical characterization of RER-deficient RNase H2, and together with Ž.T. and A.F. contributed to the generation of HeLa and HCT116 RNASEH2AKO cell lines. A.A., under the supervision of T.S., conducted ex vivo CLL studies and CGH arrays. S.P. and P.M. clinically characterized CLL patients and provided CLL blood samples. R.C. performed MLPA assays. W.Y., M.Cl. and M.B.L., under the supervision of J.d.B., analysed copy-number alterations (CNAs) in the RB1–RNASEH2B region in CRPCs. M.M. and O.M., under the supervision of V.G.B., conducted xenograft experiments. A.P.J. and D.D. designed and directed the study. D.D. and A.P.J. wrote the manuscript with help of M.Z., O.M. and M.A.M.R. and all authors reviewed it.
Corresponding authors
Ethics declarations
Competing interests
D.D. and T.H. are advisors to Repare Therapeutics.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 CRISPR screens for determinants of PARPi sensitivity.
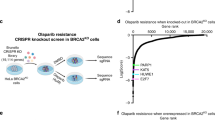
This figure is related to Fig. 1. a, Cas9 immunoblot of WCEs from parental HeLa, RPE1-hTERT and SUM149PT cells and clones stably transduced with a lentiviral Flag–Cas9–2A–Blast construct. Tubulin was used as a loading control. The immunoblot is representative of two biologically independent experiments. b, Validation of CRISPR–Cas9 gene editing efficiency in Cas9-expressing HeLa, RPE1-hTERT and SUM149PT clones. Cell proliferation was monitored after transduction with a control sgRNA construct (sgLacZ) or sgRNAs targeting essential genes PSMD1, PSMB2 and EIF3D30. Solid circles, individual values. Data are mean ± s.d. from three technical replicates normalized to sgLacZ. c, Gene Ontology terms significantly (P < 0.05, binomial test with Bonferroni correction) enriched among hits from olaparib screens common to at least two cell lines. Enrichment was analysed using PANTHER. d, esyN network analysis of interactions between hits common to at least two cell lines. Node size corresponds to mean DrugZ score across cell lines; 77 out of 155 genes are mapped on the network.
Extended Data Fig. 2 RNase H2 deficiency leads to PARPi sensitivity.
This figure is related to Fig. 2a, b. a, CRISPR-mediated inactivation of RNASEH2A or RNASEH2B in the cell lines used in this manuscript. WCEs of indicated cell lines and genotypes were processed for immunoblotting using antibodies against RNASEH2A, RNASEH2B or RNASEH2C. Vinculin, tubulin and GAPDH were used as loading controls. Representative immunoblots of at least two biologically independent experiments. b–d, Abolished RNase H2 enzymatic activity and increased levels of genome-embedded ribonucleotides in RNASEH2AKO cells. b, Analysis of total nucleic acids from wild-type and RNASEH2AKO HeLa cells treated with recombinant RNase H2 and separated by alkaline agarose gel electrophoresis. Ribonucleotide-containing genomic DNA from RNASEH2AKO HeLa cells is nicked and therefore has increased electrophoretic mobility13. Data are representative of three biologically independent experiments. c, Densitometric quantification of the alkaline gel shown in b. d, Cleavage of an RNase H2-specific double-stranded DNA oligonucleotide with a single incorporated ribonucleotide (DRD:DNA; ribonucleotide position is shown in red) by wild-type and RNASEH2AKO WCEs of the indicated cell types was measured using a fluorescence quenching-based assay32. Data are individual values (open circles) with the mean (red lines) of three biologically independent experiments. e–l, RNase H2 deficiency leads to PARPi sensitivity in multiple cell types. e–g, Clonogenic survival assays of the indicated cell lines treated with the indicated PARPi. Data are mean ± s.d. from three biologically independent experiments normalized to untreated cells. Solid lines show a nonlinear least-squares fit of the data to a three-parameter dose–response model. h, EC50 values for olaparib (left) and talazoparib (right) in the indicated cell lines as determined by nonlinear least-squares fitting of the data in e–g and Fig. 2a, b. Data are EC50 values ± 95% confidence intervals. i–l, Increased apoptosis in RNASEH2AKO HeLa, Cas9 RNASEH2BKO SUM149PT and RNASEH2AKO HCT116 cells following PARPi treatment. i, Cleaved caspase-3 immunofluorescence and flow cytometry profiles of untreated and talazoparib-treated wild-type and RNASEH2AKO HeLa. FSC, forward scatter. j–l, Percentages of cleaved caspase-3+(caspase-3+) cells of the indicated genotypes treated with the indicated PARPi. Data are individual values (coloured symbols) with the mean (solid lines) of three biologically independent experiments. Insets and outsets, levels of cleaved caspase-3+ cells without PARPi treatment. Red lines, mean of three biologically independent experiments. P values are from unpaired two-tailed t-tests. In a, d, g, l, RNASEH2AKO HCT116 cells were transduced either with an empty vector (+EV) or a full-length RNASEH2A expression construct (+WT).
Extended Data Fig. 3 Functional homologous recombination, increased replication-associated DNA damage and synthetic lethality with the loss of BRCA1 or BRCA2 in RNase H2-deficient cells.
This figure is related to Fig. 2. a–d, Homologous recombination is not affected by the inactivation of RNase H2. a, Micrographs of wild-type and RNASEH2AKO RPE1-hTERT Cas9 TP53KO and cells exposed to 3 Gy of X-rays (IR) and assessed using γ-H2AX and RAD51 immunofluorescence 4 h later. Images are representative of three biologically independent experiments. b. Quantification of the experiment in a at the indicated time points after irradiation, plotted as a percentage of cells with more than five γ-H2AX and RAD51 colocalizing foci. Data are individual values (open circles) and the mean (red lines) from three biologically independent experiments. P values, unpaired two-tailed t-test. c, Quantitative image-based cytometry (QIBC) plots of DR-GFP experiments in Fig. 2e. Each point shows the mean GFP and RNASEH2A immunofluorescence intensities per nucleus of mock- or I-SceI-transfected HeLa DR-GFP cells transduced with indicated Cas9 sgRNA constructs (EV = empty vector). Dashed lines separate RNASEH2A+ and RNASEH2A− and GFP+ and GFP− cell populations. Data are representative of three biologically independent experiments. d, Quantification of RNASEH2A+ cells in DR-GFP experiments shown in c and Fig. 2e as determined by QIBC. Data are individual values (open circles) and the mean (red lines) of three biologically independent experiments. e–h, Replication-dependent endogenous DNA damage in RNase H2-deficient cells. e, Micrographs for experiments quantified in Fig. 2g. γ-H2AX immunofluorescence in EdU+ and EdU− wild-type and RNASEH2AKO HeLa cells. Scale bars, 5 μm. f, Quantification of γ-H2AX foci per nucleus in experiments shown in e and Fig. 2g. Dots, foci number in individual nuclei; red lines, mean from three biologically independent experiments. g, h, Wild-type and RNASEH2AKO HeLa cells were treated with aphidicolin and EdU as indicated in the schematic (g, top), and immunostained with γ-H2AX antibodies. Mean number of foci per EdU+ nucleus in each experiment (g, open circles) or the number of foci in individual EdU+ nuclei (h, dots) were quantified. Red lines are the mean from three biologically independent experiments; at least 100 cells were analysed per sample in each experiment. P value, unpaired two-tailed t-test. i, j, Increased poly(ADP-ribosylation) of PARP1 in G1 as well as in S/G2/M phases in RNASEH2AKO cells. i, FACS plots of wild-type and RNASEH2AKO HeLa cells expressing the FUCCI cell cycle reporters mKO2-Cdt1 and mAG-Geminin41. Data are representative of two biologically independent experiments. j, PARP1 immunoprecipitates from WCEs of FUCCI-sorted G1 or S/G2/M wild-type and RNASEH2AKO HeLa cells, probed with the indicated antibodies. Images are representative of two biologically independent experiments. Tubulin was used as a loading control. Densitometric quantification of PAR signals normalized to immunoprecipitated PARP1 is shown as fold changes from wild-type to RNASEH2AKO cells. k–o, Inactivation of RNase H2 in BRCA1- or BRCA2-deficient backgrounds results in synthetic lethality. k, BRCA1 and BRCA2 expression, respectively, in wild-type and BRCA1KO RPE1-hTERT TP53KO cells (top) or wild-type and BRCA2KO DLD-1 cells (bottom). WCEs were processed for immunoblotting with the indicated antibodies. Tubulin and KAP1 were used as loading controls. Immunoblots are representative of at least two biologically independent experiments. l, RNase H2 levels in cells used in m–o and Fig. 2i. Cells were transduced with the indicated sgRNA vectors and processed for RNASEH2A immunofluorescence. Each point represents mean RNASEH2A intensity per nucleus as measured by QIBC (n = 1 experiment). At least 2,000 cells were analysed per sample. Percentages of RNASEH2A+ cells in individual samples are shown above each plot. m, Clonogenic survival assays quantified in Fig. 2i. Images are representative of three biologically independent experiments. n, o, Synthetic lethality after inactivation of RNASEH2A or RNASEH2B in BRCA2-deficient cells. Clonogenic survival of wild-type and BRCA2KO DLD-1 cells was assessed after transduction with indicated Cas9 sgRNA vectors. n, Representative images of three biologically independent experiments. o, Quantification of the experiments shown in n. Data are individual values (open circles) with the mean (red lines) of three biologically independent experiments. P values are from an unpaired two-tailed t-test.
Extended Data Fig. 4 A separation-of-function mutant of RNase H2.
This figure is related to Fig. 2j. RNASEH2A(P40D/Y210A) is a separation-of-function mutant that cannot excise single DNA-embedded ribonucleotides, but cleaves RNA–DNA heteroduplexes (similar to the yeast rnh201-P45D-Y219A mutant16). a, Schematic depicting enzymatic activity against two different RNase H2 substrates (DRD–DNA, double-stranded DNA with an embedded ribonucleotide, or RNA–DNA hybrids) in cell lines used in b–d and Fig. 2j. Wild-type and RNASEH2AKO cells were transduced with either an empty vector or the indicated RNASEH2A constructs. b, Complementation of HeLa RNASEH2AKO cells with Flag-tagged RNASEH2A variants restores RNase H2 complex protein levels. WCEs from wild-type and RNASEH2AKO HeLa and RNASEH2AKO cells stably expressing the indicated lentiviral constructs were processed for immunoblotting with the indicated antibodies. Vinculin was used as a loading control. Asterisk indicates a non-specific band. Immunoblots are representative of three biologically independent experiments. c, d, Complementation of HeLa RNASEH2AKO cells with wild-type RNASEH2A, but not with the D34A/D169A (catalytically dead) or P40D/Y210A (separation-of-function) mutants, rescues increased levels of genome-embedded ribonucleotides. c, Total nucleic acids from the cell lines shown in a, b were treated with recombinant RNase H2 and separated by alkaline agarose gel electrophoresis. Image is representative of four experiments. d, Densitometric quantification of alkaline gel shown in c. e, Purified human RNase H2 complexes consisting of RNASEH2B, RNASEH2C and RNASEH2A wild type, P40D/Y210A or D34A/D169A subunits separated by SDS–PAGE and stained with Coomassie blue. One experiment was performed. f–k, RNase H2 activity assays with fluorescein-labelled RNA–DNA substrate (f) or double-stranded DNA with a single incorporated ribonucleotide (DRD–DNA) (g) and increasing amounts of recombinant wild-type, P40D/Y210A or D34A/D169A RNase H2. Products were separated by polyacrylamide gel electrophoresis and detected by fluorescence imaging. Images are representative of three biologically independent experiments. h, k, Quantification of gels from f, g. Product signal is plotted relative to substrate signal per lane. Data are mean ± s.d. from three biologically independent experiments.
Extended Data Fig. 5 PARP1 trapping is the underlying cause of PARPi sensitivity in RNase H2-deficient cells
This figure is related to Fig. 3a–c. a, Schematic representation of CRISPR screens for suppressors of talazoparib sensitivity in RNase H2-deficient cells. Cas9-expressing cells were transduced with the TKOv1 library, talazoparib was added on day 6 (t6; HeLa, 20 nM; RPE1-hTERT, 50 nM) and cells were cultured in its presence until day 18 (t18). Cells were subcultured once at day 12 (RPE1) or 13 (HeLa). sgRNA representations in the initial (t6) and final (t18) populations were quantified by next-generation sequencing. Gene knockouts that were enriched at day 18 over day 6 were identified by MAGeCK42. b, CRISPR-mediated inactivation of RNASEH2A and/or PARP1 in cell lines used in c–e and Fig. 3b. WCEs were processed for immunoblotting with the indicated antibodies. KAP1 was used as a loading control. Immunoblots are representative of two biologically independent experiments. c–e, Loss of PARP1 restores PARPi-resistance in RNASEH2AKO cells. c, Percentage of cleaved caspase-3+ HeLa cells of indicated genotypes with or without olaparib treatment measured by flow cytometry (FACS). Data are individual values (open circles) with the mean (red lines) of three biologically independent experiments. P value is from an unpaired two-tailed t-test. d, e, Clonogenic survival assays with HeLa (d) and RPE1-hTERT (e) cells of the indicated genotypes treated with olaparib (left) or talazoparib (right). Data are mean ± s.d. from three biologically independent experiments. Solid lines show a nonlinear least-squares fit to a three-parameter dose–response model. f. Trapping activity of PARPi correlates with the ability to induce apoptosis in RNASEH2AKO cells. Quantification of cleaved caspase-3+ wild-type and RNASEH2AKO HeLa cells without treatment or treated with the indicated PARPi. Data are individual values with the mean (black lines) of three biologically independent experiments. Note that PARP-trapping activity decreases as follows: talazoparib > olaparib > veliparib4,48. g, PARPi-induced S-phase arrest in RNASEH2AKO cells is alleviated in the absence of PARP1. Top, schematic of talazoparib and EdU treatment. Bottom, EdU (pseudocolor plots) and DNA content (histograms) FACS profiles of untreated and talazoparib-treated wild-type, PARP1KO, RNASEH2AKO and PARP1KORNASEH2AKO HeLa cells. DNA content was determined by propidium iodide (PI) staining. Data are representative of three biologically independent experiments. h, Quantification of mean γ-H2AX intensities in experiments shown in Fig. 3c. Data are individual values (open circles) with the mean (red lines) of three biologically independent experiments. At least 10,000 cells were analysed per sample in each experiment.
Extended Data Fig. 6 TOP1-mediated cleavage at genome-embedded ribonucleotides leads to PARPi sensitivity in RER-deficient cells.
This figure is related to Fig. 3d–g. a, Reduced endogenous DNA damage in TOP1-depleted RNASEH2AKO cells. Quantification of γ-H2AX foci per nucleus in the experiments shown in Fig. 3e, f. Dots, foci number in individual nuclei; red lines, mean of five biologically independent experiments. b–i, TOP1 depletion alleviates PARPi-induced apoptosis and S-phase arrest in HeLa RNASEH2AKO cells (b–e) and in RNASEH2A(P40D Y210A) separation-of-function mutant cells (f–h). b, Cleaved caspase-3 FACS plots for experiments quantified in Fig. 3g. Data are representative of three biologically independent experiments. c, Wild-type and RNASEH2AKO HeLa cells were transfected with non-targeting (siCTRL-SP) or TOP1-targeting (siTOP1-SP) SMARTpool siRNAs. WCEs analysed by immunoblotting with antibodies to TOP1 and actin (loading control). Images are representative of three biologically independent experiments. d, FACS plots of cleaved caspase-3 in wild-type and RNASEH2AKO HeLa cells transfected with siCTRL-SP or siTOP1-SP after talazoparib treatment. e, Quantification of the experiment shown in d. f, RNASEH2AKO HeLa cells stably expressing the indicated Flag-tagged constructs were transfected with non-targeting (siCTRL) or TOP1-targeting (siTOP1) siRNAs. WCEs were analysed by immunoblotting with TOP1, Flag and actin (loading control) antibodies. Immunoblots are representative of three biologically independent experiments. g, FACS plots of cleaved caspase-3 in RNASEH2AKO HeLa cells transfected with siCTRL or siTOP1 and expressing wild-type RNASEH2A or the P40D/Y210A mutant. Data are representative of three biologically independent experiments. h, Quantification of the experiment shown in g. Data in e, h, are mean ± s.d. from three biologically independent experiments normalized to untreated cells. At least 10,000 cells were analysed per sample in each experiment. P values are from an unpaired two-tailed t-test. i, Cell cycle profiles, before and after talazoparib treatment, of wild-type and RNASEH2AKO HeLa cells transfected with the indicated siRNAs. DNA content was assessed by propidium iodide staining and FACS. Data are representative of three biologically independent experiments.
Extended Data Fig. 7 Frequent collateral loss of RNASEH2B in CLL and metastatic CRPC.
This figure is related to Fig. 4a–c. a, b, MLPA analysis (a) and CGH array profiles for chromosome 13q (b) of representative CLL samples carrying two wild-type RNASEH2B alleles (top), a monoallelic RNASEH2B deletion (middle) or biallelic deletion (bottom). a, For MLPA analysis, genomic DNA from reference and experimental samples was analysed using probes targeting control loci and individual RNASEH2B exons (exon 1–11). The MLPA ratio was calculated per probe and normalized to control probes and reference samples. Error bars indicate s.d. of the mean from eight control probes for each sample. Dashed lines indicate the threshold set for diploid copy number. b, For each CGH array profile the y-axes of the top and bottom plots indicate copy number probe intensity (logR ratio) and the x-axes mark the position on chromosome 13 represented by the ideogram (middle). An enlargement of the frequently deleted 13q14.2–14.3 region, including the miRNA-15A/16-1 gene cluster and the RNASEH2B gene, is shown in the bottom plot. One experiment was performed. c, RNASEH2B is frequently co-deleted with RB1 in CRPC. Copy number alterations (CNA) in the RB1–RNASEH2B region in CRPC (n = 226 cases) are shown. Horizontal lines represent the CNA profile for individual CRPC samples (dark blue, homozygous loss; light blue, heterozygous loss; grey, no change; pink, copy number gain (CNA 3–4); red, copy number amplification (CNA > 4); white, insufficient data to determine CNA). Samples are clustered on the basis of RNASEH2B gene status. CNA frequencies for RNASEH2B and the RB1–RNASEH2B region without a copy number breakpoint are shown on the right.
Extended Data Fig. 8 PARPi sensitivity in RNase H2-deficient primary CLL cells and mouse xenograft tumours.
This figure is related to Fig. 4. a, b, Proliferating cells, and not quiescent cells, are the major population of viable cells in ex vivo cultured primary CLL patient samples irrespective of treatment group. Quantification of absolute (a) and relative (b) quiescent and proliferating cell numbers as determined by FACS analysis of the primary CLL samples used in Fig. 4b, c. Wild-type RNASEH2B, n = 8 individual samples; monoallelic deletion, n = 4 individual samples; biallelic deletion, n = 9 individual samples. Data are mean ± s.d. from three technical replicates. FACS gating strategy for stimulated peripheral blood lymphocytes (PBLs) from CLL patients is shown in Supplementary Fig. 2. c, RNase H2-deficient primary CLL cells have reduced survival when cultured with olaparib. Data are the mean of individual samples ± s.e.m. (n = 3 biologically independent CLL samples per group, each analysed in technical triplicates). P value from a two-way ANOVA. d, Talazoparib selectively inhibits the growth of RNASEH2AKO xenograft tumours. RNASEH2AKO cells complemented either with empty vector or wild-type RNASEH2A were injected subcutaneously into bilateral flanks of CD-1 nude mice. Mice were randomized to either vehicle or talazoparib (0.333 mg kg−1) treatment groups (eight animals per group) and tumour volumes were measured twice weekly. Data are mean ± s.e.m. P values are from two-way ANOVA under the null hypothesis that talazoparib does not suppress the tumour growth.
Extended Data Fig. 9 RNase H2-deficient cells are more sensitive to PARPi than DNA polymerase β mutants.
a, Schematic of the POLBΔ188–190 CRISPR mutation. The Mg2+-coordinating aspartate residues (D190, D192 and D256, red triangles) are highlighted in the domain structure of the human DNA polymerase β protein. The sgRNA target site and antibody epitope are indicated by black lines. b, WCEs from parental RPE1-hTERT Cas9 TP53KO cells and two POLBΔ188–190 clones were processed for immunoblotting with DNA polymerase β and tubulin (loading control) antibodies. Immunoblots are representative of two biologically independent experiments. c, The POLBΔ188–190 mutation impairs base excision repair. Wild-type or POLBΔ188–190 RPE1-hTERT Cas9 TP53KO cells were exposed to different concentrations of MMS for 24 h, and then grown in drug-free medium for an additional 48 h. Cell viability was determined using the Cell Titer Glo assay. d, Sensitivity of wild-type, RNASEH2AKO and POLBΔ188–190 RPE1-hTERT Cas9 TP53KO cells to indicated talazoparib concentrations in clonogenic survival assays. Data in c, d are mean ± s.d. from three biologically independent experiments normalized to untreated cells. Solid lines show a nonlinear least-squares fit to a three-parameter dose–response model.
Supplementary information
Supplementary Figures
This file contains Supplementary Figures 1-2. Supplementary Figure 1 contains the unprocessed images of immunoblots presented in the main and Extended Data Figures. Supplementary Figure 2 contains an overview of gating strategies for flow cytometry experiments shown in the main and Extended Data Figures.
Supplementary Table 1
Results of CRISPR screens for PARP inhibitor sensitizers. Tab 1 contains a list of high-confidence hits in each cell line (FDR ≤ 0.01 + FDR ≤ 0.1 in ≥ 2 cell lines, calculated by DrugZ) in screens shown in Fig 1 and ED Fig 1. Tab 2 contains source data for Venn diagram shown in Fig 1b,a list of cell line-specific hits and hits overlapping in ≥ 2 cell lines. Tab 3 contains gene-level DrugZ results including: sumZ, sum of sgRNA-level DrugZ scores for each gene; numObs, number of sgRNAs / gene across screen replicates; normZ, normalized sumZ score; pval, P value; rank, ranking of genes based on normZ; FDR, false discovery rate. See the main text, methods and ref. 8 for details.
Supplementary Table 2
Results of CRISPR screens for suppressors of PARP inhibitor sensitivity in RNASEH2A-KO cells. Gene-level MAGeCK results for screens shown in Fig 3a and ED Fig 5a. The data include: depletion (neg) and enrichment (pos) score, P-value, FDR, rank and number of analyzed sgRNAs (goodsgrna). See main text, Methods and Ref. 33 for details.
Supplementary Table 3
Source data for mouse xenograft experiments in Fig 4d and ED Fig 8d. Tumour measurements in individual mice (mean of tumour sizes at each flank) at indicated time points with mean and s.e.m. n = 8 independent animals per group.
Rights and permissions
About this article
Cite this article
Zimmermann, M., Murina, O., Reijns, M.A.M. et al. CRISPR screens identify genomic ribonucleotides as a source of PARP-trapping lesions. Nature 559, 285–289 (2018). https://doi.org/10.1038/s41586-018-0291-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-018-0291-z
This article is cited by
-
RTF2 controls replication repriming and ribonucleotide excision at the replisome
Nature Communications (2024)
-
The chemotherapeutic drug CX-5461 is a potent mutagen in cultured human cells
Nature Genetics (2024)
-
Genome-wide CRISPR screens identify novel regulators of wild-type and mutant p53 stability
Molecular Systems Biology (2024)
-
PARP inhibitor exerts an anti-tumor effect via LMO2 and synergizes with cisplatin in natural killer/T cell lymphoma
BMC Medicine (2023)
-
C16orf72/HAPSTR1/TAPR1 functions with BRCA1/Senataxin to modulate replication-associated R-loops and confer resistance to PARP disruption
Nature Communications (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.